Abstract
The aim of the present study was to document the knowledge of traditional Siddha medical practitioners from Thiruvarur district in Tamil Nadu, India, and to quantitatively analyze the data to identify some useful leads of medicinal plants and to screening the phytocomounds. Field study was carried out for a period of 1 year in Thiruvarur district of Tamil Nadu. The ethnomedicinal information were collected from Siddha medical practitioners. The collected data were analyzed through quantitative analysis. The molecular docking studies were performed three marketed drugs and eleven different medicinal plant compounds against HBeAg using Schrodinger suite. A total of 33 species of plants distributed in 22 genera belonging to 22 families were identified as commonly used ethno medicinal plants by traditional Siddha practitioners in Thiruvarur. An interesting point in molecular docking study is that luteolin is an effective inhibitor for the inhibition of HBV when compared to commercial drugs. Traditional Siddha medical practitioner and remarkable medicinal plant knowledge and uses were documented for the study area.
Keywords
Siddha practitioners ; Phytocompounds ; Hepatitis B virus
Introduction
Plants have played a very important role in human life for a long time, supplying basic needs such as food, clothing, medicine, and housing. Information about the art of using herbs is a legacy passed from one generation to another. Studies dealing with the relationship between humans and plants are placed in the field of science called Ethnobotany. Khajoei Nasab and Khosravi (2014) reported that ethnobotany surveys include interviewing local people, use of the available data in the literature, and the folklore of each region. The goal of ethnobotany is to protect and to pass the valuable and useful traditional knowledge to future generations. Uncontrolled harvest of medicinal plants by people has increased the risk of extinction of many species and subsequently the loss of local knowledge as how to use them.
India is the second largest country in the world with over one billion people with diverse socio-cultural backgrounds. It accounts for 16% of the worlds population and holds 21% of the worlds global burden of diseases. The impact of traditional systems of medicine in the public healthcare system of India is substantially high and medicine is intimately interwoven with religiosity and ethnicity (Broom et al., 2009 ). The first written Siddha medical text ‘Thirumanthiram’ dates back around 6th–7th century A. D. and the Siddha medicine as it now exists both in theory and practice, began in Tamil Nadu around the16th century, but elements of healing practices which became part of Siddha medicine including those they hold in common with Ayurveda, came from an earlier period as evidenced by the concepts for good health in Thirukural, collection of Tamil poems that dates around 450–550 A.D. (Zysk, 2008 ). The Government of India has been supporting and running colleges to teach Siddha system of medicine. But the comparatively feeble institutionalization of Siddha medicine is brought out by the figures for January 2005, which fixes the ratio of registered nonqualified/qualified practitioners at 7.71:2.29, whereas for Ayurveda, it was 2.27:7.73 ( WHO, 2007 ). These traditionally trained practitioners are accused of ignorance and of practicing a false medicine by those who avoid their treatment as well as by Siddha doctors who lay claim to the true medical knowledge ( Sebastia, 2011 ).
According to the WHO, worldwide around two billion people are infected with the hepatitis B virus and 6,000,000 peoples die each year due to its consequences. In India, approximately 80 million people affected in hepatitis B virus, which results in around 2,400,000 deaths annually due to complications from the disease. Hepatitis means inflammation of the liver. It is caused by several mechanisms, including certain infectious agents. Viral hepatitis is caused by different type of viruses such as hepatitis A, B, C, D, and E. The two commonly used vaccines, namely pegylated interferon and ribavirin, are now being used in combination than separately, which shows higher rate of response. But this treatment shows side effects such as hemolytic anemia, renal failure, etc (Balavignesh et al., 2013 ). The aim of the present study was to document and to quantitatively analyze the knowledge of traditional Siddha medical practitioners from Thiruvarur district in Tamil Nadu, India, on medicinal plants and to screening the better drug candidates against hepatitis B virus through in silico methods.
Materials and Methods
Geographical Location
Thiruvarur is located at 9.28°N 79.3°E. The town is bounded by Sukumar river in the north, Valaiyar river in the south, while the Odambokki river flows through the center. The town has an average elevation of 3 m (9.8 ft) from the sea level. The municipality covers an area of 10.47 km2 (4.04 sq. mi). The town along with the district receives an annual rainfall of 1260 mm (50 in.). The town experiences tropical climate during summer, from March to May. The proximity to sea results in high humidity throughout the year and peaks 70% from August to May. The town has a plain terrain of alluvial soil consisting of sand, silt, and clay. Vennar and Vettar, the tributaries of river Cauvery, are the major water bodies around the town. Surface water canals contribute 89% to irrigation, while the rest 11% is accounted by dug wells and tube wells. Paddy is the major crop while the others being black gram, green gram, ground nut and gingely.
Investigation Sites and Selection of Traditional Siddha Practitioners
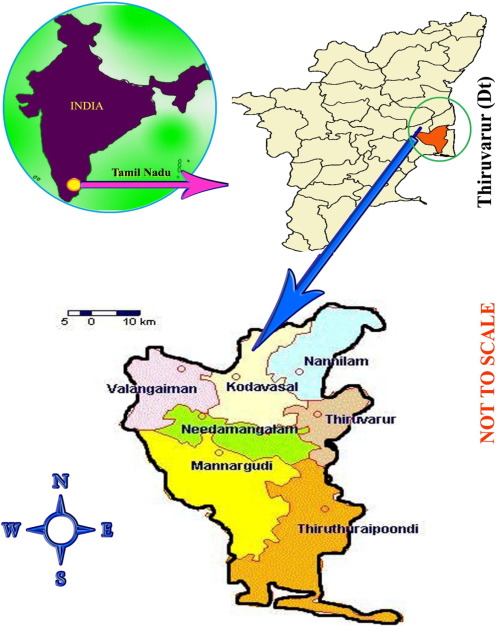
The study area was investigated to get information from local traditional practitioners having practical knowledge of medicinal plants, who were interviewed in Thiruvarur district of 7 taluks (Kudavasal, Mannarkudi, Nannilam, Needamangalam, Thiruthuraipoondi, Thiruvarur, and Valangaiman) during June 2014–April 2015. In 2011, Thiruvarur had a population of 1,264,277 of which male and female were 626,693 and 637,584, respectively. Scheduled castes and scheduled tribes accounted for 14.35% and .66% of the population, respectively (Fig. 1 ). Methods of selecting informants depended upon the distribution of traditional practitioners having sound knowledge. They were requested to collect specimens of the plants they know or to show the plant species on site. These informants were traditional practitioners themselves or had tradition of healing in their families and had knowledge of the medicinal use of the plants. The wealth of medicinal plant knowledge among the people of this district is based on hundreds of years of beliefs and observations. Totally, 87 informants were selected. Of them, 56 men and 31 women between the ages of 18–84 years were included to get ethnomedicinal information through direct interviews or oral conversation (Table 1 ).
|
|
|
Fig. 1. Investigation sites. |
| Age | NI | % Informants |
|---|---|---|
| 28–37 | 8 | 9.19% |
| 38–44 | 21 | 24.13% |
| 45–57 | 23 | 26.43% |
| 58–69 | 17 | 19.54% |
| 70–77 | 13 | 14.94% |
| 78–84 | 9 | 10.34% |
| Gender | ||
| Men | 66 | 75.86% |
| Women | 21 | 24.14% |
| Experience | ||
| < 5 years | 16 | 18.39% |
| 8–11 years | 30 | 34.48% |
| 12–19 years | 27 | 31.03% |
| 20 years above | 14 | 16.09% |
| Main occupation | ||
| Self-employed | 17 | 19.54% |
| Agriculture | 25 | 28.73% |
| Homemade practitioners | 21 | 24.13% |
| Clinical practitioners | 24 | 25.28% |
Preservation of Plant Specimens
Standard method was followed with record to collection of plant materials, drying, mounting, preparation, and preservation of plant specimens (Jain, 1964 ). Voucher specimens of medicinal plants in triplicate were collected, prepared, and identified. Plants with their correct nomenclature were arranged alphabetically by family name, vernacular name, ethnomedicinal uses and applications. The identification and nomenclature of the listed plants were based on the Flora of Presidency of Madras (Gamble, 1935 ) and the Flora of Tamil Nadu Carnatic (Matthew, 1983 ). They were later verified at Botanical Survey of India, Southern Circle, Coimbatore, India.
Quantitative Analysis
Relative Frequency Citation (RFC)
This index used here is the relative frequency of citation (RFC). This index is obtained by dividing the number of informants mentioning a useful species (FC or frequency of citation), by the total number of informants in the survey (N). RFC value varies from 0 (when nobody refers to a plant as a useful one) to 1 (when all the informants mentioning it as useful) (Tardio and Pardo-de Santayana, 2008 ). RFC index, which does not consider the use-category (UR or use-report is a single record for use of a plant mentioned by an individual) and RFC calculated by the following formula:
|
|
Use value (UV)
The use value (UV) demonstrates the relative importance of plants known locally. It was calculated using the following formula (Gazzaneo et al., 2005 ):
|
|
where Ui is the number of uses mentioned by each informant for a given species and N is the total number of informants.
Relative Importance
The relative importance (RI) of plant species cited by the informants is calculated as follows (Kadir et al., 2012 ): RI = PP + AC, where PP = the number of pharmacological properties (reported specific ailments) attributed to a species divided by the maximum number of properties attributed to the most resourceful species (species with the highest number of properties). AC = the number of ailment categories treated by a given species divided by the maximum number of ailment categories treated by the most resourceful species. A value of 2 is the highest possible value for relative importance (RI) indicating the most versatile species with the greatest number of medicinal properties (Oliveira et al., 2010 ).
Calculation of Informant Agreement Ratio (IAR)
The importance of the individual species was estimated by calculating the IAR (Trotter and Logan, 1986 ) for each species. IAR was calculated using the following formula:
|
|
where nr is the total number of citations registered for species s and na is the number of illness categories that are treated with this species. These values range between zero (when the number of illness categories equals the number of citations) and one (whereby all the participants agree upon the exclusive use of the species for the particular illness) (Thomas et al., 2009 ).
Computational Methods with Glide Version 6.3
All computational studies were carried out using Glide version 6.3, installed in a single machine running on Intel Core i7 Duo processor with 1 GB RAM and 275 GB hard disk with Black Dell inspiron version 7.0 as the operating system.
Preparation of Protein Target Structure
The X-ray crystal structure of hepatitis B virus e-antigen enzyme is obtained from the Protein Data Bank. After selection, protein preparation wizard of Schrodinger suite has been used to prepare protein. All water molecules were removed, HET numbers are removed, missing side chains were added, hydrogen atoms are added to the proteins, and all atom force field (OPSL-2001) charges and atom types were assigned. Preparation and refinement were done running ProteinPrep job on the structure in a standard procedure. Optimize and Minimized the protein were performed until the average root mean square deviation of non-hydrogen atoms reached 0.3 Å.
Identification and Validation of Binding Site (SiteMap)
The SiteMap was used to locate the ligand binding sites over the protein molecule. The SiteMap helps for the ligand to interact with amino acid residues from protein molecule.
Ligand Preparation
These twelve natural compounds were selected from medicinal plants; these ligands were used in our molecular docking studies. These twelve compounds were sketched from Schrödinger Suit (Maestro 10.5 version) and the commercial compound was retrieved from the ChemSpider database. The compounds were prepared with the help of LigPrep (2.3) module (Ligprep, Version 2.3, 2009 ), the drawn ligands were geometry optimized by using the optimized potentials for liquid simulations-2005 (OPLS-2005) force field with the steepest descent followed by truncated Newton conjugate gradient protocol. Partial atomic charges were computed using the OPLS-2005 force field. The LigPrep is a utility in Schrodinger software suite that combines tools for generating 3D structures from 1D (Smiles) and 2D (SDF) representation, searching for tautomers and steric isomers and geometry minimization of ligands.
Results
Demographic Profile of the Siddha Practitioners
Demographic characteristics of respondents were determined and recorded through face-to-face interviews. The number of practitioners between the age groups 45–57 was high when compared to the other groups. The percentage of practitioners with an experience lower than 5 years was only 18.39%. There was uneven distribution in the male–female ratio. Nearly 24.13% of the practitioners were homemade medicine in study area. 25.28% of the practitioners were practicing it only as a clinical practitioner (Table 1 ). Regarding the demography of the informants, both dominated middle-aged healers and non-dominated other workers were documented in our studies. As indicated, there was high male–female ratio; womens role as a traditional medical practitioner was less than the male practitioner. Still, it remains a male-exclusive domain. Even in several previous works with traditional medical practitioners in India the same fact was recorded. Mati and De Boer (2011) conducted a study in Kurdish markets and reported that women occupied a major of part consumers while men occupied a major portion of the sellers of traditional medicine. But as far as our study is concerned, a major portion of women involved in traditional medicine perform their service as birth attendants. Though the general figure showed that a major portion of the healers were uneducated or poorly educated, cattle drovers, many of the young practitioners hold a degree/diploma. Some of the practitioners also refer the patients to biomedical doctors/technician stores, who view their health status and they are able to read and understand the reports of some basic lab tests such as blood glucose levels. Some of them are also collecting these reports as proof of efficacy of their treatment. A major portion of the practitioners practice this medicine as a part-time job. The consultation charges usually ranged between INR11–51,and in some cases, it was free.
Different Plant Families Recorded
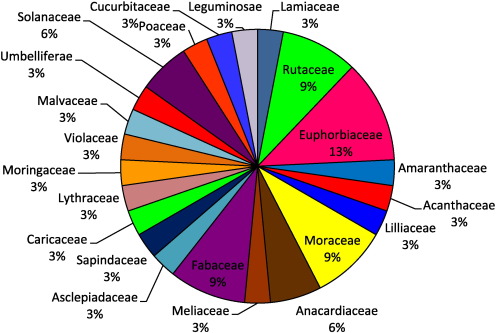
The plants used for medicinal purposes in the region are presented in Table 2 with relevant information. As a result of study, 33 medicinal plant species belonging to 22 families were found in the research area. The most presented families are Euphorbiaceae (each 4 species) followed by Fabaceae, Moraceae and Rutaceae (each 3 species), Anacardiaceae and Solanaceae (each 2 species), and others (16 species) (Fig. 2 ). Among the families, Euphorbiaceae, Fabaceae, Moraceae, and Rutaceae, which were most dominant in this study, are consistently in other ethnobotanical studies (Ayyanar and Ignacimuthu, 2011 , Prabhu et al., 2014 and Morvin Yabesh et al., 2014 ; Kim and Song, 2014 ), which can be attributed to their having a wide range of bio-active ingredients (Gazzaneo et al., 2005 ). Euphorbiaceae is also known to have the highest number species, more than any other plant family in the world (Marles and Farnsworth, 1995 ).
| No. | Plant name and voucher number | Family | Practitioner and vernacular name | Parts used | Ailment categories with number of informants | Preparations | UR and FC | RFC | Use value | RI | IAR |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. | Aegle mermelos L. PHC-2019 | Rutaceae | Vila maram | Fruit Fruit | NA:18 (Nerves throne) PB:27 (Insect bite) | Paste Paste | 45/51 | 0.586 | 0.517 | 0.535 | 0.977 |
| 2. | Acalypha indica L. PHC-2025 | Euphorbiaceae | Kuppaimeni | Leaves Leaves Leaves | PB: 4 (Scorpion sting) DID: 7 (Scabies) GIA: 6 (To kill intestinal worms) | Paste Paste Paste | 17/43 | 0.492 | 0.195 | 0.803 | 0.875 |
| 3. | Achyranthes aspera L. PHC-2031 | Amarathanceae | Nayuruvi | Seed Whole plant Seed Root Leaves Leaves Leaves Leaves | RSD:15 (Cough) GUA:24 (Stone formation) GH:23 (Body strength) PB:10 (Scorpion bite) DID:11 (Wounds) HA:23(Hepatitis B viral infection FVR:16 (Fever) GH:17 (Body refresh) | Powder Juice Powder Juice Paste Juice Paste Juice | 139/87 | 1.000 | 1.597 | 2.000 | 0.949 |
| 4. | Adhatoda vasica Nees. PHC-2036 | Acanthaceae | Adathodai | Leaves Leaves Leaves | ED:5 (Diabetes) RSD:6 (Cough) FVR:1 (Fever) | Paste Juice Paste | 12/23 | 0.264 | 0.137 | 0.803 | 0.818 |
| 5. | Allium cepa L. PHC-2020 | Liliaceae | Vengayam | Bulb Leaves Bulb | ED:11 (Diabetes) AA:13 (Erectile of sex organ) PB:8 (Scorpion bite) | Paste Raw Raw | 32/41 | 0.471 | 0.367 | 0.803 | 0.935 |
| 6. | Azadirachta indica A. Juss. PHC-2026 | Meliaceae | Vaembu | Young bark Bark Leaves Leaves Leaves Flower Seed | SMSD:12 (Rheumatism) DID:13 (Scabies) DID:21 (Small pox) FVR:11 (Scarlet fever) ED:19 (Diabetes) GIA: 17 (To kill intestinal warms) HC: 23 (To kill insect) | Paste Paste Paste Juice Juice Juice Paste | 116/86 | 0.988 | 1.333 | 1.772 | 0.947 |
| 7. | Cajanus cajan (L.) PHC-2030 Millsp | Fabaceae | Ilanthai | Fruits | AA:10 (Increase sperm production) | Raw | 10/25 | 0.287 | 0.114 | 0.267 | 1.000 |
| 8. | Calotropis procera PHC-2032 | Asclepiadaceae | Erukku | Latex Root Root | DID:12 (Abscess) PB:7 (Scorpion sting) PB: 9 (Dog bite) | Raw Paste Paste | 28/43 | 0.494 | 0.321 | 0.660 | 0.925 |
| 9. | Cardiospermum halicacabum L. PHC-2035 | Sapindaceae | Mudakkathan | Leaves Leaves | SMSD:13 (Rheumatism) GIA:9 (Gastric problem) | Decoction Juice | 22/38 | 0.321 | 0.252 | 0.535 | 0.952 |
| 10. | Carica papaya L. PHC-2040 | Caricaceae | Pappali | Fruits Latex Leaves | GA:3 (Easy delivery) DA:7 (Tooth ache) FVR:7 (Viral fever) OA:4 (Eye ache) | Raw Raw Decoction Raw | 21/33 | 0.379 | 0.241 | 0.827 | 0.850 |
| 11. | Citrus'aurantifolia* (Christm.) Swingle. PHC-2044 | Rutaceae | Elumitchai | Fruit Leaves | NA:16 (Cure head ache) RSD:18 (Cold and control vomit) | Raw Raw | 34/23 | 0.264 | 0.390 | 0.535 | 0.969 |
| 12. | Coccinia grandis Wight & Arn. PHC-2044 | Cucurbitaceae | Kovai | Fruits | ED:14 (Diabetes) | Raw | 14/19 | 0.218 | 0.160 | 0.267 | 1.000 |
| 13. | Cynodon dactylon (L.) Pers. PHC-2027 | Poaceae | Arugampul | Leaves Leaves | GIA:5 (Motion problem) GH:11 (Blood purification) ED:3 (Diabetes) | Juice Juice Paste | 19/27 | 0.310 | 0.218 | 0.803 | 0.888 |
| 14. | Coriandrum sativum L. PHC-2021 | Umbelliferae | Koththamalli | Leaves Seed Leaves Leaves | GIA:6 (Indigestion and vomiting) AA: 3 (Avoid stone formation) DID: 8 (Epilepsy) GIA: 9 (Control bloody diarrhea) | Paste Powder Paste Paste | 26/29 | 0.333 | 0.298 | 0.267 | 0.880 |
| 15. | Euphorbia hirta L. PHC-2036 | Euphorbiaceae | Amman pacharasi | Leaves | DID:16 (Swellings) | Juice | 16/24 | 0.275 | 0.183 | 0.267 | 1.000 |
| 16. | Hypanthus enneaspermus (L.) F. Muell PHC-2043 | Violaceae | Orithal thamarai | Whole plant | AA:17 (Increase sperm production) | Powder | 17/22 | 0.252 | 0.195 | 0.660 | 1.000 |
| 17. | Ficus benghalensis L. PHC-2027 | Moraceae | Alamaram | Seed Lateral root | AA:12 (Increase sperm production) DCA:7 (Teeth strength and control blood leaking of teeth) | Powder Raw | 19/21 | 0.241 | 0.218 | 0.660 | 0.944 |
| 18. | Ficus racemosa L. PHC-2033 | Moraceae | Aththi | Fruit Fruit Fruit | AA:9 (Sperm production) GA:6 (Easy delivery) GA:15 (Lactation) | Raw Raw Raw | 30/47 | 0.540 | 0.344 | 0.660 | 0.931 |
| 19. | Ficus religiosa L. PHC-2037 | Moraceae | Arasamaram | Leaves Leaves Fruit | DID:17 (Cuts) DID: Wounds AA:11 (Sperm production) | Paste Powder Powder | 28/29 | 0.333 | 0.321 | 0.660 | 0.962 |
| 20. | Lawsonia inermis L. PHC-2028 | Lythraceae | Maruthani | Leaves Bark | HC:29 (Hair growth and natural hair colouring) GA:7 (Gonorrhoea) | Paste | 36/32 | 0.367 | 0.333 | 0.666 | 0.971 |
| 21. | Glycyrrhiza glabra L. PHC-2045 | Leguminosae | Athimathuram | Whole plant | HA: 19 (HBV infection) | Paste | 19/24 | 0.275 | 0.218 | 0.267 | 1.000 |
| 22. | Mangifera indica L. PHC-2038 | Anacardiaceae | Maa maram | Leaves Fruits Leaves | GIA:4 (Intestinal warms) GA: 3 (Pregnancy) OA: 1 (Tumour) | Juice Raw Paste | 8/11 | 0.126 | 0.091 | 0.803 | 0.714 |
| 23. | Moringa oleifera L. PHC-2022 | Moringaceae | Murungai | Leaves Flower Bark | GH:7 (Increase immune power) AA:5 (Sperm production) GA:13 (Venereal disease) | Paste Juice Paste | 25/31 | 0.356 | 0.287 | 0.803 | 0.916 |
| 24. | Murraya koengii Spreng. PHC-2041 | Rutaceae | Karuveppilai | Leaves | HC:16 (Hair growth and Hair strength) | Paste | 16/19 | 0.218 | 0.183 | 0.392 | 0.960 |
| 25. | Ocimum sanctum L. PHC-2043 | Lamiaceae | Thulasi | Leaves Leaves | GH:9 (Body Refresh) AA: 17 (Affected sperm counting) | Paste Raw | 26/51 | 0.586 | 0.298 | 0.535 | 0.960 |
| 26. | Odina wodier Roxb. FL PHC-2034 | Anacardiaceae | Othiya maram | Bark Bark Bark | GA:11 (Venereal disease) DID:14 (Inflammation) GH:3 (Remove body pain) | Juice Paste Juice | 28/61 | 0.701 | 0.321 | 0.803 | 0.925 |
| 27. | Phyllanthus amarus L. PHC-2028 | Euphorbiaceae | Keela nelli | Leaves Leaves Seed Seed | DID:19 (Scabies) HA:27(Hepatitis B viral infection) GH:22 (Increase immune system) DID:12 (Wound) | Paste Juice Raw Raw | 80/87 | 1.000 | 0.919 | 0.928 | 0.962 |
| 28. | Phyllanthus emblica L. PHC-2042 | Euphorbiaceae | Nelli | Fruit Fruit Fruit | HC:5 (Hair growth) GH:11 (Increase immune system and body strength) HEM:7 (Hepatitis B viral infection) | Juice Juice Juice | 23/33 | 0.379 | 0.264 | 0.803 | 0.909 |
| 29. | Pongamia glabra Vent. PHC-2039 | Fabaceae | Pungan | Leaves Seed | DID:5 (Avoid microbes infection) GIA:6 (Control child dysentery (Maantham)) | Paste Raw | 11/16 | 0.183 | 0.126 | 0.535 | 0.900 |
| 30. | Solanum nigrum SW. PHC-2023 | Solanaceae | Manaththakkali | Leaves Whole plant Root Whole plant | RSD: 24 (Cough) HEM: 17 (Piles) ED:27 (Diabetes) HA:18 (Hepatitis B viral infection) | Paste Juice Juice Juice | 86/57 | 0.655 | 0.988 | 0.928 | 0.964 |
| 31. | Solanum trilobatum L. PHC-2035 | Solanaceae | Thuthuvalai | Leaves | GIA:24 (Easy delivery) | Paste | 31/42 | 0.482 | 0.356 | 0.267 | 1.000 |
| 32. | Tectona grandis L. PHC-2029 | Fabaceae | Thaekku | Leaves | DID:18 (Dandruff) | Paste | 18/20 | 0.229 | 0.206 | 0.267 | 1.000 |
| 33. | Thespesia populneae Cat. PHC-2024 | Malvaceae | Poovarasu | Leaves Seed | DID:23 (Swelling) DID:11 (Skin disease) | Paste Paste | 34/39 | 0.448 | 0.390 | 0.392 | 0.969 |
UR : use report, FC : frequency citation, RFC : relative frequency citation, RI : relative importance, IAR : informant agreement remedies.
|
|
|
Fig. 2. Percentage of plant families used. |
Plant Parts Used for Traditional Siddha Medicine
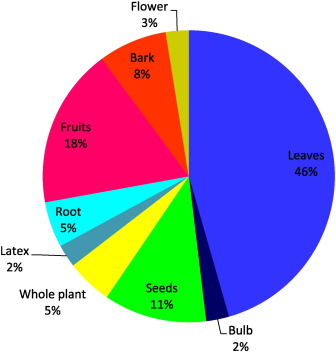
The most frequently used plant parts were leaves (46%), followed by fruits (18%), seed (11%), bark (8%), whole plant and root (5%), flower (3%), and bulb and latex (2%) (Fig. 3 ). All over the world, tribal communities use leaves for the preparation of herbal medicine (Ullah et al., 2013 , Vijayakumar et al., 2015 , Prabhu et al., 2014 and Morvin Yabesh et al., 2014 ). The leaf is the major site for photosynthesis, or in other words, it is metabolically the most active part of the plant. As a result, various biogenetic pathways take place to produce secondary metabolites which contribute toward its medicinal value (Balick and Cox, 1996 and Ghorbani, 2005 ). Moreover, collection and the mode of preparation of medicine from leaves is much easier than other parts of the plant, which makes them the first choice for use (Giday et al., 2009 and Telefo et al., 2011 ).
|
|
|
Fig. 3. Percentage of plant parts used. |
Mode of Preparations and Application
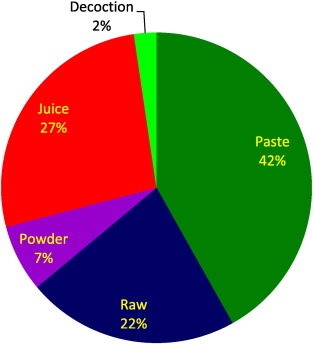
There are various methods of preparation and application for different types of ailments and they have various preparation forms like paste (42%), juice (27%), raw (22%), powder (7%), and decoction (2%). Among the methods of preparation, decoction (28%) and powder (24%) are the methods mostly used for the remedies (Fig. 4 ). Medicinal plant is mostly prepared in paste from the Siddha medical practitioners. According to the informants, preparation of paste for the treatment of ailments is a common method of the tribal communities in a global level ( Amri and Kisangau, 2012 , Giday et al., 2009 and Ullah et al., 2013 ). The paste is prepared by grinding the fresh or dried plant parts with oil or water. In some cases, the processing involves drying of the plant material followed by grinding into fine powder. The juice is taken as orally along with water or milk or honey. Raw is taken as raw plant parts orally. Decoction is obtained by boiling the plant parts in water until the volume of water is reduced to required amount.
|
|
|
Fig. 4. Percentage of preparations. |
Quantitative Analysis
Relative Frequency Citation
This means that this species has been mentioned by all informants and is the most recognized plant in the region. Also, because of the highest values of these species, they have the most diverse uses. Achyranthes aspera , Phyllanthus amarus , and Solanum nigrum were ranked first by RFC, respectively ( Table. 2 ).
Use Value
The most commonly used species was Achyranthes aspera with 139 use reports by 87 informants, giving the highest use value of 1.577,which is a new claim in the treatment of hepatitis B viral infection. Followed by Azadirachta indica , with 116 use reports by 87 informants giving the highest value (1.333); Solanum nigrum with 86 use reports by 87 informants with UV of 0.988, attributed to its use in the treatment of various diseases, and it is well recognized by all the informants as having hepatoprotective power. Generally, these plants were frequently used by traditional Siddha medical practitioners in Radhapuram taluk, Tamil Nadu, India ( Chellppandian et al., 2012 ) and local health care practices of Sikkim (Badola and Pradhan, 2013 ), India, for treatment of various diseases.
The very low use value of Solanum torvum , Nerium oleander , and Passiflora foetida , which is reported by only one informant with a UV of 0.12, of which Passiflora foetida was a new claim and also used in headache; others are regularly using this plant in the treatment of body cooling and ear ache. Similar were supported (Chellaiah et al., 2006; Itharat and Ooraikul, 2007 and Seyid et al., 2013 ).
Vijayakumar et al. (2015) reported that plants in the study area lead to their low use value as in the case of Nelliyampathy hills of Kerala, India. In the present study, plants reported with low use value (16 use reports by 87 informants with a UV of 0.183) were Mangifera indica (8 use reports by 87 informants) followed by Cajanus cajan (10 use reports by 87 informants with a UV of 0.114), Pongamia glabra (11 use reports by 87 informants with a UV of), Adathoda vasica (12 use reports by 87 informants with a UV of 0.137), Coccinia grandis (14 use reports by 87 informants with a UV of 0.184), and Euphorbia hirta , which has a very low UV of 0.186 among the traditional Siddha medical practitioners as treatment for cough, fever, swellings, and diabetes and increase sperm production.
Relative Importance
The collected ethnomedicinal plants possessed a number of pharmacological properties (Variers, 1993; Khare, 2007 ). The plants with the greatest number of illness treated and ailment categories were found to be Achyranthes aspera (2.000) followed by Azadirachta indica (1.339). Moreover, the high relative importance (RI) value of Achyranthes aspera (RI = 2.00) reported might be an indication of its high availability and affordability in the study area (Table 2 ). The plant with more number of pharmacological properties (PP) were Achyranthes aspera (8 PP), so they have a normalized PP value of 1.000 (8/8). Achyranthes aspera was employed to treat eight ailment categories and had a normalized AC value of 1.00 (7/7).
According to Morvin Yabesh et al. (2014) , Achyranthes aspera was recognized as the most resourceful taxa since it was mentioned by most of the informants among the traditional healers in Silent Valley of Kerala, India. Azadiractha indica resourceful taxa were used against hyperdipsia, eczema, leucoderma, intermittent, and fever and as spermicidal by the village peoples of Thoppampatti, Dindigul district, Tamil Nadu, India ( Sivasankari et al., 2014 ). Many of the most versatile species reported in this study were similar for some neighboring indigenous communities in India ( Ayyanar and Ignacimuthu, 2011 , Pandikumar et al., 2011 , Morvin Yabesh et al., 2014 and Vijayakumar et al., 2015 ).
Informant Agreement Remedies
Also, the high index of agreement on remedies (IAR) values documented for 5 medicinal plant species in the current study implies that all informants agree upon the exclusive use of the medicinal animal species for a particular ailment condition. Moreover, the significantly high IAR values of easily available medicinal plant species, for instance, Coccinia indica (1.000), Glycyrrhiza glabra (1.000), Lawsonia inermis (1.000), Murraya koenigii (1.000), and Tectona grandis (1.000) recorded in the present study, indicate the need to document the traditional knowledge over their usage in order to prevent the loss of such traditional knowledge ( Table 2 ). Similarly, it is reported that for IAR value in Tamil Nadu hair care, Tectona grandis had high number of citations and high IAR value indicating that it had been recommended only for the treatment of dandruff, and Glycyrrhiza glabra had a high number of citations and high IAR value, indicating that it had been recommended only for cough. In liver ailments, Coccinia grandis had a high number of citations, had a high IAR value, indicating that it had been recommended only for the treatment of diabetes ( Silambarasan and Ayyanar, 2015 and Chellppandian et al., 2012 ).
The medicinal herbs were collected by local people living in the study area on daily payment basis from local Siddha medical practitioners without any consideration of age and size of the plants, resulting in depletion of their natural resources in the area. However, with the migration of young people to search for better jobs in cities, the collection of plant is slowly declining. It is very important that the emphasis should be on organized cultivation, which will involve and provide jobs for the local community, which is virtually absent at present.
Molecular Docking Study
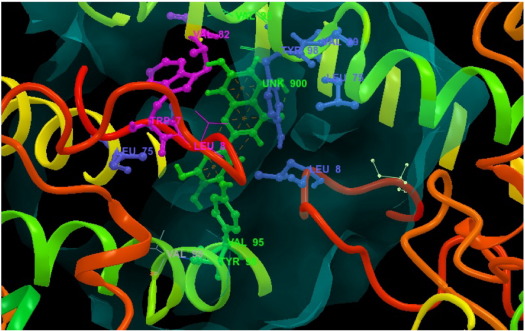
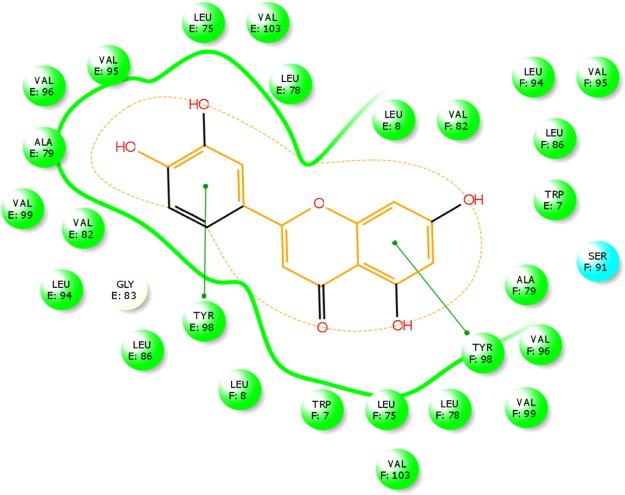
Molecular docking was performed between the bioactive compounds of ethnomedicinal plant and hepatitis B virus e-antigen enzyme (Fig. 5 and Fig. 6 ). The 3-D structure of the HBeAg was provided; five ligand binding sites are evaluated. The bioactive compounds recognized the first site as a major active binding site for the molecular docking (Fig. 7 ). The above target protein (HBeAg) and ligands (bioactive compounds) were geometrically optimized. All the ligand molecules were docked against the active sites of the target protein using Glide software. The docking results were presented in the form of glide docking score in negative values (Table 3 ). In the docking studies, higher negative values represent high binding affinity between the receptor and ligand molecules, indicating the higher efficiency of the bioactive compounds.
|
|
|
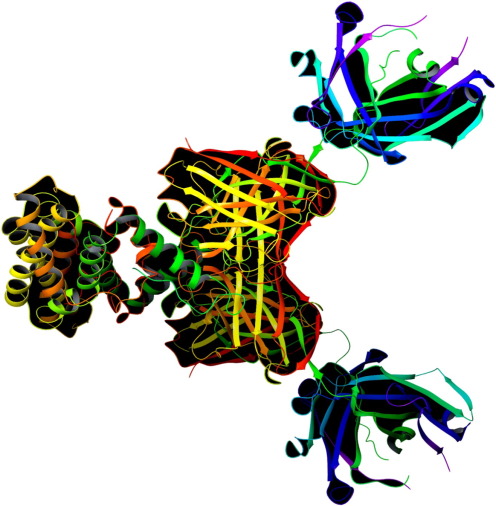
Fig. 5. 3D structure of 3V6Z receptor. |
|
|
|
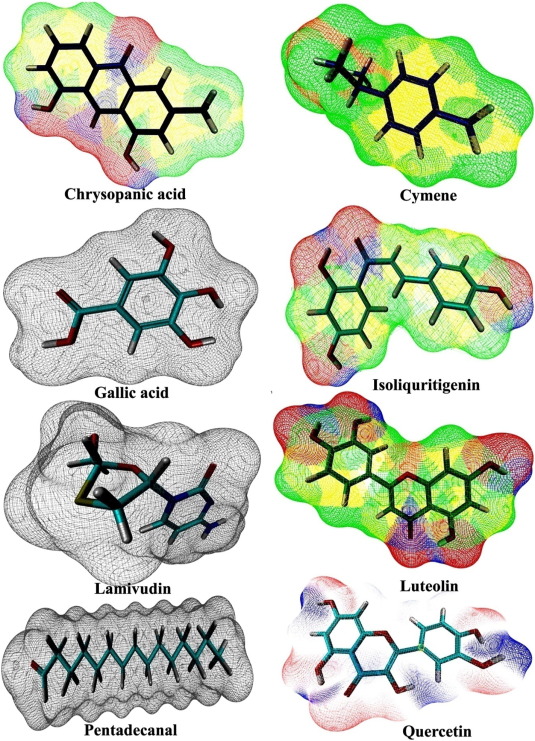
Fig. 6. 3D structure of some phytocompounds and commercial drug model with Schrodinger suite. |
|
|
|
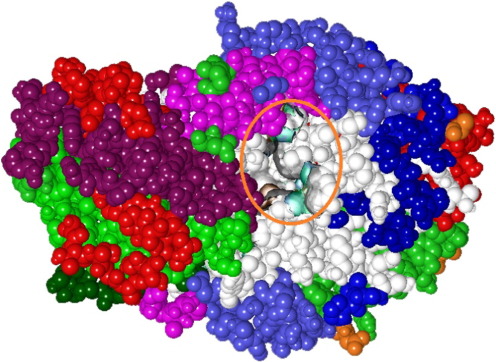
Fig. 7. Active binding site of 3V6Z receptor. |
| S. no. | Phytocompounds | Docking scores |
|---|---|---|
| 1. | Luteolin | − 8.08747 |
| 2. | Glabrene | − 7.77192 |
| 3. | Isoliquiritigenin | − 7.57663 |
| 4. | Chrysophanic acid | − 7.03012 |
| 5. | Cymene | − 6.98227 |
| 6. | Cyclosativene | − 6.86796 |
| 7. | Sabinene | − 6.694 |
| 9. | Querceitin | − 6.62595 |
| 10. | Sabinene | − 6.37937 |
| 11. | Methyl eugenol | − 6.04532 |
| 12. | Gallic acid | − 5.22005 |
Molecular docking enables a scientist to virtually screen a number of candidate compounds based on their docking score with a target molecule. In the present study, phytocompounds have been docked against HBeAg target. Binding energies of the protein (target)-ligand (drug) interactions are important to describe how fit the drug binds to the target macromolecule. Twelve phytocompounds (luteolin, glabrene, isoliquritigenenin, chrysopanic acid, cymene, cyclosativene, sabinene, quercetin, sabinene, methyl eugenol, gallic acid, and transaconitic acid) and three commercial drugs (lamivudine, tenofovir and ribivirin) were selected for the docking studies.
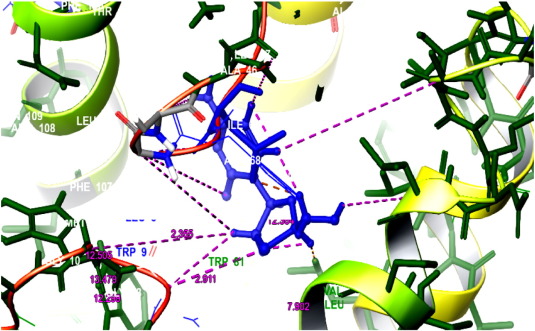
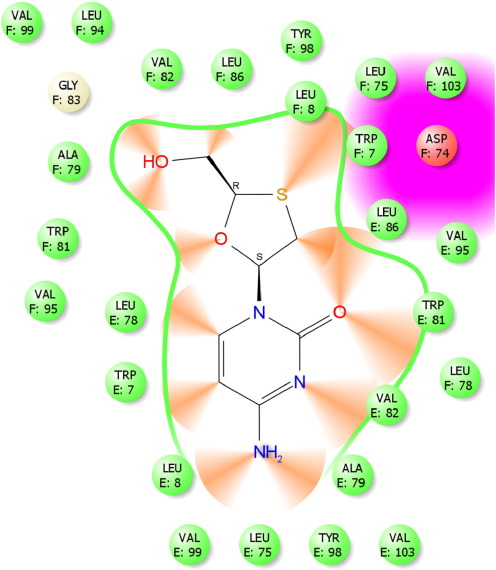
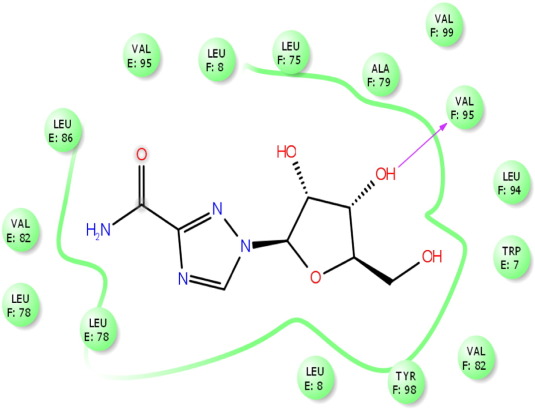
An interesting point in this study is that luteolin (− 8.087), glabrene (− 7.772), isoliquritigenenin (− 7.577), chrysopanic acid (− 7.03), cymene (− 6.982), cyclosativene (− 6.868), sabinene (− 6.379), quercitin (− 6.626), sabinene (− 6.379), methyl eugenol (− 6.045), gallic acid (− 5.220), and transaconitic acid (− 3.884) dock into the binding pockets of HBeAg protein. The analysis of docking score showed the best results than commercial drugs. Specifically, luteolin (− 8.087), glabrene (− 7.772), isoliquritigenenin (− 7.577), chrysopanic acid (− 7.03), cymene (− 6.982), cyclosativene (− 6.868), and sabinene (− 6.379), the effective inhibitors for the inhibition of HBV, were compared to the commercial drugs (i.e, lamivudine (− 6.113), tenofovir (− 6.074), and ribivirin (− 5.041)). The commercial drugs had the very lowest value compared to phytocompounds (Table 3 and Table 4 ). Out of 15 ligands, luteolin showed the highest glide score of − 8.087 with ligand and amino acid residues (Fig. 8 and Fig. 8a ). During docking, luteolin showed two pi-pi stacking bonding between the ligand molecule and the amino acid residues of the receptor showing a perfect binding (Fig. 9 ). The commercial drug lamivudine showed the lowest glide score of − 6.113 with ligand and amino acid residues (Fig. 10 and Fig. 10a ). This docking studies commercial drug of ribivirin showed one H bond interaction bonding between the ligand molecule and the amino acid residues of the receptor showing a perfect binding (Fig. 11 ). Among the 12 bioactive compounds and 3 commercial drugs, luteolin was identified as the most suitable drug for hepatitis B virus. Thus, it is evident that the plant parts of Glycyrrhiza glabra , Phyllanthus amarus , Phyllanthus embilica , and Solanum nigrum exhibit anti-hepatitis nature. Similarly, Omprakash et al. (2011) reported that phytocompounds were found to be best docking with hepatitis B virus. It can be observed that the binding energy decreases and increases after the ligand is docked with energy minimized structure of 1QGT protein. The present study also confirmed these reports.
| S. no. | Commercial drug | Docking score |
|---|---|---|
| 1. | Lamivudine | − 6.11301 |
| 2. | Tenofovir | − 6.07362 |
| 3. | Rivirin | − 5.041 |
|
|
|
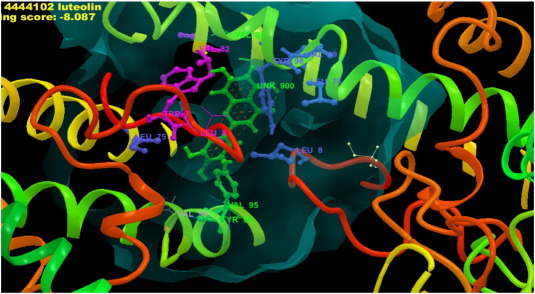
Fig. 8. Luteolin interacted with 3V6Z receptor. |
|
|
|
Fig. 8a. A portion enlarged. |
|
|
|
Fig. 9. Amino acid residues from luteolin interaction. |
|
|
|
Fig. 10. Lamivudine interacted with 3V6Z enzyme. |
|
|
|
Fig. 10a. Amino acid residues from lamivudine interaction. |
|
|
|
Fig. 11. Amino acid residues from ribivirin interaction. |
Conclusion
A remarkable traditional medicinal plants knowledge, practice, and preparation were documented from the study area. This is the first study which quantifies the use of medicinal plants by the traditional Siddha medical practitioners in this area. In the present findings, it is well documented that the compounds luteolin, glabrene, isoliquritigenenin, chrysopanic acid, cymene, cyclosativene, sabinene, quercetin, and sabinene play a part in the management of HBV and also exhibited good docking profiles and can be considered safe for development into a commercial drug, thereby justifying the in silico methods and traditional claim. These compounds could be a better candidate to treat HBV. In this way, we have compiled significant baseline data regarding indigenous knowledge about the medicinal plants for treating HBV, which are now ready to be further investigated pharmacologically, which would lead to natural drug discovery and development.
Acknowledgments
The authors are grateful to the SERB/F/8339/2914-15 for providing financial assistant in this project. We specially express our thanks to the management of A.V.V.M. Sri Pushpam College (Autonomous), Poondi, for providing them necessary facilities and support to carry out this work.
References
- Amri and Kisangau, 2012 E. Amri, D. Kisangau; Ethnomedicinal study of plants used in villages around Kimboza Forest Reserve in Morogoro, Tanzania; J. Ethnobiol. Ethnomed., 8 (2012), p. 1
- Ayyanar and Ignacimuthu, 2011 M. Ayyanar, S. Ignacimuthu; Ethnobotanical survey of medicinal plants commonly used by Kani tribals in Tirunelveli hills of Western Ghats, India; J. Ethnopharmacol., 134 (2011), pp. 851–864
- Badola and Pradhan, 2013 H.K. Badola, B.K. Pradhan; Plants used in healthcare practices by Limboo tribe in South-West of Khangchendzonga Biosphere Reserve, Sikkim, India; Indian J. Tradit. Knowl., 12 (3) (2013), pp. 355–369
- Balavignesh et al., 2013 V. Balavignesh, E. Srinivasan, N.G. Ramesh Babu, N. Saravanan; Molecular docking study ON NS5B polymerase of hepatitis c virus by screening of volatile compounds from Acacia concinna and ADMET prediction ; Int. J. Pharm. Life Sci., 4 (4) (2013), pp. 2548–2558
- Balick and Cox, 1996 M. Balick, P. Cox; Plants culture and people; Scientific American Network New York (1996)
- Broom et al., 2009 A. Broom, A. Doron, P. Tove; The in equalities of medical pluralism: hierarchies of health, the politics of tradition and the economies of care in Indian oncology; Soc. Sci. Med., 69 (2009), pp. 698–706
- Chellppandian et al., 2012 M. Chellppandian, S. Mutheeswaran, P. Pandikumar, V. Duraipandiyan, S. Ignacimuthu; Quantitative ethnobotany of traditional Siddha medicinal practitioners from Radhapuram taluk of Tirunelveli District, Tamilnadu, India; J. Ethnopharmacol., 143 (2012), pp. 540–547
- Gamble, 1935 J.S. Gamble; The Flora of the Presidency of Madras; Adlard & Son, Ltd., London (1935)
- Gazzaneo et al., 2005 L.R.S. Gazzaneo, R.F.P. Lucena, U.P. Albuquerque; Knowledge and use of medicinal plants by local specialists in a region of Atlantic Forest in the state of Pernambuco; J. Ethnobiol. Ethnomed., 1 (2005), p. 9
- Ghorbani, 2005 A. Ghorbani; Studies on pharmaceutical ethno botany in the region of Turkmen Sahra North of Iran (Part 1): general results; J. Ethnopharmacol., 102 (2005), pp. 58–68
- Giday et al., 2009 M. Giday, Z. Asfaw, Z. Woldu; Medicinal plants of the Meinit ethnic group of Ethiopia: an ethnobotanical study; J. Ethnopharmacol., 124 (2009), pp. 513–521
- Itharat and Ooraikul, 2007 A. Itharat, B. Ooraikul; Research of Thai medicinal plants for cancer treatment; Adv. Med. Plant Res. (2007), pp. 287–317
- Jain, 1964 S.K. Jain; The role of botanist in folklore research; Folklore, 5 (1964), pp. 145–150
- Kadir et al., 2012 M.F. Kadir, M.S.B. Sayeed, M.M.K. Mia; Ethnopharmacological survey of medicinal plants used by the indigenous and tribal people in Rangamati Bangladesh; J. Ethnopharmacol., 144 (2012), pp. 627–637
- Khajoei Nasab and Khosravi, 2014 F. Khajoei Nasab, A.R. Khosravi; Ethnobotanical study of medicinal plants of Sirjan in Kerman Province, Iran; J. Ethnopharmacol., 154 (2014), pp. 190–197
- Khare, 2007 C.P. Khare; Indian Medicinal Plants, An Illustrated Dictionary; Springer Science Business Media LLC, 233 Spring street, New York, NY 10013, USA (2007), p. 836
- Kim and Song, 2014 H. Kim, M.J. Song; Analysis of traditional knowledge about medicinal plants utilized in communities of Jirisan Park (Korea); J. Ethnopharmacol., 153 (2014), pp. 85–89
- Ligprep, Version 2.3, 2009 Ligprep, Version 2.3; Schrodinger, LLC, New York (2009)
- Marles and Farnsworth, 1995 R. Marles, N. Farnsworth; Antidiabetic plants and their active constituents; Phytomedicine, 2 (1995), pp. 137–165
- Mati and De Boer, 2011 E. Mati, H.J. De Boer; Trade and commercialization of herbal medicine in the Qaysari Market, Kurdish Autonomous region; Iraq. J. Ethnopharmacol., 133 (2011), pp. 490–510
- Matthew, 1983 K.M. Matthew; The Flora of the Tamil Nadu Carnatic.; The Rapinat Herbarium, 3. St. Josephs College, Tiruchirapalli, India (1983), p. lxxxiv (2154)
- Morvin Yabesh et al., 2014 J.E. Morvin Yabesh, S. Prabhu, S. Vijayakumar; An ethnobotanical study of medicinal plants used by traditional healers in silent valley of kerala, India; J. Ethnopharmacol., 154 (2014), pp. 774–789
- Oliveira et al., 2010 E.S. Oliveira, D.F. Torres, S.E. Brooks, R.R.N. Alves; The medicinal animal markets in the metropolitan region of Natal City, north eastern Brazil; J. Ethnopharmacol., 130 (2010), pp. 54–60
- Omprakash et al., 2011 K.K. Omprakash, B. Vadivukkarasi, R. Rajasekaran, A. Narayana; Insilico studies of antigen-E (hepatits-B) against principal components of 9 medicinal plants; Asian J. Pharm. Clin. Res., 4 (2) (2011), pp. 1–4
- Pandikumar et al., 2011 P. Pandikumar, M. Chellappandian, S. Mutheeswaran, S. Ignacimuthu; Consensus of local knowledge on medicinal plants among traditional healers in Mayiladumparai block of Theni District, Tamil Nadu, India; J. Ethnopharmacol., 134 (2011), pp. 851–864
- Prabhu et al., 2014 S. Prabhu, S. Vijayakumar, J.E. MorvinYabesh, K. Ravichandran, B. Sakthivel; Documentation and quantitative analysis of the local on medicinal plants in Kalrayan hills of Villupuram district, Tamil Nadu, India; J. Ethnopharmacol., 157 (2014), pp. 7–20
- Sebastia, 2011 B. Sebastia; Border crossings of medicines not very sweet: prevent safety or preserve the authenticity?; J. Anthopol. Knowl., 5 (2011), pp. 71–98
- Seyid et al., 2013 A.S. Seyid, A. Ekrem, S. Selami; An ethno botanical study of medicinal plants used by the local people of Alsehir (Manisa) in Turkey; J. Ethnopharmacol., 150 (2013), pp. 860–874
- Silambarasan and Ayyanar, 2015 R. Silambarasan, M. Ayyanar; An ethnobotanical study of medicinal plants in Palamalai region of Eastern Ghats, India; J. Ethnopharmacol., 172 (2015), pp. 162–178
- Sivasankari et al., 2014 B. Sivasankari, N. Anandharaj, P. Gunasekaran; An ethnobotanical study of indigenous knowledge on medicinal plants used the village peoples of Thoppampatti, Dindukal district, Tamilnadu, India; J. Ethnopharmacol., 153 (2014), pp. 408–423
- Tardio and Pardo-de Santayana, 2008 J. Tardio, M. Pardo-de Santayana; Cultural importance indices: a comparative analysis based on the useful wild plants of southern Cantabria (Northern Spain); Econ. Bot., 62 (2008), pp. 24–39
- Telefo et al., 2011 P.B. Telefo, L.L. Lienou, M.D. Yemele, M.C. Lemfack, C. Mouokeu, C.S. Goka, S.R. Tagne, F.P. Moundipa; Ethnopharmacological survey of plants used for the treatment of female infertility in Baham, Cameroon; J. Ethnopharmacol., 136 (2011), pp. 178–187
- Thomas et al., 2009 E. Thomas, I. Vandebroek, S. Sanca, P.V. Damma; Cultural significance of medicinal plant families and species among Quechua farmers in Apillapampa, Bolivia; J. Ethnopharmacol., 122 (2009), pp. 60–67
- Trotter and Logan, 1986 R.T. Trotter, M.H. Logan; Informant consensus: a new approach for identifying potentially effective medicinal plants; N.L. Etkin (Ed.), Plants in Indigenous Medicine and Diet, Behavioural Approaches, Redgrave Publishing Company, Bred ford Hills, New York (1986), pp. 91–112
- Ullah et al., 2013 M. Ullah, M.U. Khan, A. Mahmood, R.N. Malik, M. Hussain, S.M. Wazir, M. Daud, Z.K. Shinwari; An ethnobotanical survey of indigenous medicinal plants in Wana district south Waziristan agency; Pakistan. J. Ethnopharmacol., 150 (2013), pp. 918–924
- Vijayakumar et al., 2015 S. Vijayakumar, J.E. MorvinYabesh, S. Prabhu, R. Manikandan, B. Muralidharan; Quantitative ethnomedicinal study of plants used in the Nelliyampathy hills of Kerala, India; J. Ethnopharmacol., 161 (2015), pp. 238–254
- WHO, 2007 WHO; WHO Country Cooperation Strategy 2006–2011; Supplement on Traditional Medicine, WHO Country Office for India, New Delhi (2007)
- Zysk, 2008 K.G. Zysk; Siddha Medicine in Tamil Nadu; National museets Tranque bar Initiative, København (2008)
Document information
Published on 27/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?