Highlights
- The status of CDKN2A provides epigenetic/genetic information for the cancer patient.
- The correlation of p16INK4a and related biomarkers should be considered for prognosis of cancers.
- Epigenetic/genetic modulation of changes in CDKN2A might be a promising cancer preventive/therapeutic strategy.
Abstract
Aberrant gene silencing is highly associated with altered cell cycle regulation during carcinogenesis. In particular, silencing of the CDKN2A tumor suppressor gene, which encodes the p16INK4a protein, has a causal link with several different types of cancers. The p16INK4a protein plays an executional role in cell cycle and senescence through the regulation of the cyclin-dependent kinase (CDK) 4/6 and cyclin D complexes. Several genetic and epigenetic aberrations of CDKN2A lead to enhanced tumorigenesis and metastasis with recurrence of cancer and poor prognosis. In these cases, the restoration of genetic and epigenetic reactivation of CDKN2A is a practical approach for the prevention and therapy of cancer. This review highlights the genetic status of CDKN2A as a prognostic and predictive biomarker in various cancers.
Keywords
CDKN2A ; p16INK4a ; Genetic alterations ; Epigenetic alterations ; Cancer
1. Introduction
Cancer comprises a collection of complex genetic and epigenetic diseases that arise through multistep processes (Tallen and Riabowol, 2014 ). Tumor cells acquire common properties, including unlimited proliferation potential, self-sufficiency in growth signaling, neovascularization for nutrient and oxygen supply, and resistance to anti-proliferative and apoptotic stimuli (Hanahan and Weinberg, 2011 ). In resting cells, the cell cycle is strictly managed by a set of regulatory proteins that control the various cell cycle checkpoints (Collado et al., 2007 and Collins et al., 1997 ). This cell cycle machinery is often deregulated in cancer as a consequence of the silencing of various tumor suppressor genes (Collins et al., 1997 and Tallen and Riabowol, 2014 ). In fact, loss of tumor suppressor genes and their encoded proteins through deletion, inactivating mutations, epigenetic silencing or post-translational modification results in tumorigenesis. The progression of the mammalian cell cycle from G1 to mitosis is regulated by various cyclin proteins and their catalytic subunits referred to as cyclin-dependent kinases (CDKs) (Nabel, 2002 ). A family of cyclin–CDK inhibitor proteins (CDIs), which bind and inactivate the CDKs, has been isolated. This family includes the p16INK4a , p21CIP1 , p27KIP1 , and associated proteins p15INK4b , p18INK4c , p19INK4d and p57KIP2 (Nabel, 2002 ). These proteins potentially act as tumor suppressors and their inactivation corresponds with human carcinogenesis.
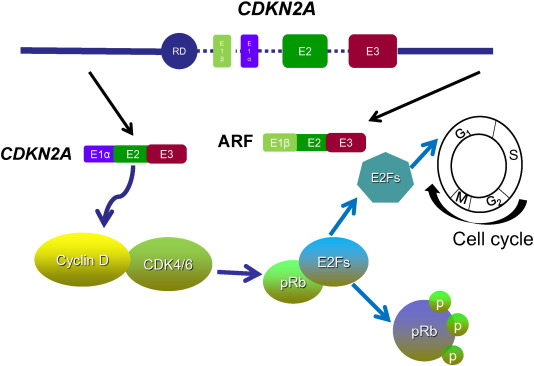
One of the tumor suppressor proteins that is inactivated in cancer is the p16INK4a protein, which is encoded by the cyclin-dependent kinase inhibitor 2A (CDKN2A ) or multiple tumor suppressor 1 (MTS1 ) gene ( Fig. 1 ) (Witcher and Emerson, 2009 ). The CDKN2A gene is located within the frequently deleted chromosomal region 9 of p21 ( Gil and Peters, 2006 ). This gene (8.5 kb full length) contains two introns and three exons and encodes the p16INK4a protein. The p16INK4a protein is a protein consisting of 156 amino acids with a molecular weight of 16 kDa and is a negative regulator of the cell cycle (Serrano et al., 1993 ). In addition to p16INK4a , CDKN2A encodes a completely unrelated tumor suppressor protein, alternate open reading frame (ARF or p19Arf in mice), which interacts with the p53 regulatory protein, mouse double minute 2 homolog (MDM2) (Pomerantz et al., 1998 ). The simple tandem arrangement is complicated by the presence of an additional exon 1β, which is transcribed from its own promoter. The resulting RNA incorporates exons 2 and 3, but specifies a distinct protein because the exons are translated by an alternative reading frame. Thus, while exons 2 and 3 are shared by the two mRNAs, they encode different protein products, p16INK4a and ARF (Quelle et al., 1995 ). The specific binding of the p16INK4a protein to CDK4 or CDK6 induces an allosteric conformational change in these proteins and inhibits the formation of the complex between CDK4 or 6 and cyclin D (Serrano et al., 1993 ). The lack of this complex formation maintains the retinoblastoma protein (Rb) in its hypo-phosphorylated and growth-suppressive states. This leads to the induction of G1 phase cell cycle arrest through the formation of the Rb/E2Fs-repressive complex (Fig. 1 ) (Weinberg, 1995 ). The loss of p16INK4a is increasingly common with advancing stages of various neoplasms, suggesting that p16INK4a inactivation may contribute to cancer progression. The frequent inactivation of p16INK4a induced by homozygous deletion or promoter hyper-methylation and point mutation has been observed in various cancers (Table 1 ).
|
|
|
Fig. 1. Schematic structure of the INK4a /ARF locus and the role of p16INK4a in cells. CDKN2A is produced by alternative splicing of E1, E2 and E3. The p16INK4a protein binds to the cyclin D and CDK4/6 complexes and inhibits the activation of the transcription factor, E2F1, which induces proteins to move from the G1 phase to S phase in the cell cycle. |
| Cancer types | Status of alteration | Frequency (%) | Reference |
|---|---|---|---|
| Gastric lymphoma | Promoter hyper-methylation | 29.7% (11/37) | Huang et al. (2007 ) |
| Burkitts lymphoma | Promoter hyper-methylation | 72.5% (37/51) | Robaina et al. (2015 ) |
| Skin cancer | Promoter hyper-methylation, histone modification | 50–70%, 80–90% | Chen et al. (2012a ) |
| Melanoma | Promoter hyper-methylation | 25.9% (15/58) | Kostaki et al. (2014 ) |
| Histone modification | Sarkar et al. (2015 ) | ||
| Promoter hyper-methylation, non-synonymous mutation | 25% (15/59), 16% (9/56) | Jonsson et al. (2010 ) | |
| Head and neck squamous cell carcinoma | Mutation/promoter hyper-methylation | 57% (138/243) | Chung et al. (2015 ) |
| Promoter hyper-methylation | 54.5% (6/11 cell line) and 66.7% (20/30) | El-Naggar et al. (1997 ) | |
| Oral cancer | Promoter hyper-methylation | 60% (6/10) | Asokan et al. (2014 ) |
| Pancreatic adenocarcinoma | Mutation | 11.8% (2/17) | Salo-Mullen et al. (2015 ) |
| Promoter hyper-methylation | 24.6% (14/57) | Jiao et al. (2007 ) | |
| Non-small cell Lung cancer (NSCLC) | Homozygous deletion (HD)/mutation/promoter hyper-methylation | 53%/13%/33% in cell lines | Tam et al. (2013 ) |
| Mutation/frameshift/HD | 19% (12/63) | Marchetti et al. (1997 ) | |
| Esophageal squamous cell carcinoma | Loss of heterozygocity (LOH)/mutation | 13% (5/38)/6% (4/67) | Kuwabara et al. (2011 ) |
| Promoter hyper-methylation | 81.7% (210/257) | Chen et al. (2012b ) | |
| Deletion | 20% (22/106) | Qureshi et al. (2012 ) | |
| Gastric cancer | Hyper-methylation | 81.6% (40/49, EBVaGC), 33.3% (15/45, EBVnGC) | He et al. (2015 ) |
| Colorectal cancer | Promoter hyper-methylation | 11.9% (34/285) | Kim et al. (2010 ) |
| Promoter hyper-methylation | 17.1% (87/497) | Rajendran et al. (2015 ) | |
| Epithelial ovarian caricnoma | Promoter hyper-methylation | 43% (58/134) | Bhagat et al. (2014 ) |
| Prostate cancer | Expression of ANRIL, CBX7, and EZH2 | Yap et al. (2010 ) | |
| Promoter hyper-methylation | 47.6% (10/21) | Ameri et al. (2011 ) |
Epigenetic alterations are suggested to regulate gene expression without affecting the base sequence. These modifications include genomic DNA-methylation, histone modifications, chromatin remodeling and miRNA/non-coding RNA-induced regulation of gene expression (Hauptman and Glavac, 2013 , Portela and Esteller, 2010 and Sarkar et al., 2015 ). The polycomb group (PcG ) genes, first identified in Drosophila melanogaster , encode the highly conserved PcG proteins, which form two large macromolecular complexes classified as polycomb repressive complex-1 (PRC1) and -2 (PRC2). The PRC1 complex consists of B lymphoma Mo-MLV insertion region 1 homolog (BMI1), mPh1/2, Pc/chromobox (CBX) and RING1A/B, and sustains silencing of chromatin. The mammalian PRC1 might harbor specificity against selecting one of the multiple Pc/CBX homologs. The PRC2 complex is composed of embryonic ectoderm development (EED), suppressor of zeste (SUZ)12 and enhancer of zeste homolog (EZH)1/2, and initiates repression of target genes by di- and trimethylation of lysine 27 of histone H3 (H3K27me2 and H3K27me3) ( Bracken et al., 2007 and Cao et al., 2002 ). Thus, activation of PRC1 and PRC2 induces gene silencing through histone modification ultimately affecting the chromatin structures. Long non-coding RNAs are transcripts longer than 200 nucleotides and lack protein-coding capacity. These RNAs might play a major role in programming the epigenome by cooperating and coordinating with the PcG complexes to impose chromatin states in a dynamic manner (Aguilo et al., 2011 ). The purpose of this mini-review is to shed light on the molecular mechanisms of genetic and epigenetic changes in p16INK4a and the implications in carcinogenesis.
2. Genetic alterations of CDKN2A in various cancers
The changes in CDKN2A /p16INK4a status are highly variable depending on the type of cancer. The following section describes the mechanisms of p16INK4a inactivation in various cancers (Table 1 ; Fig. 2 ).
|
|
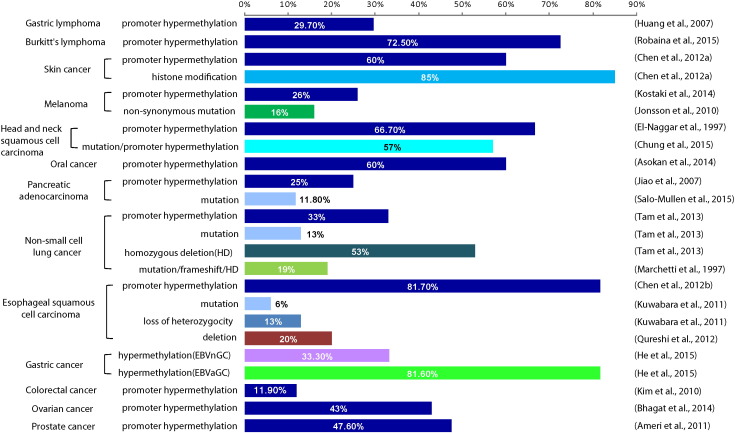
|
Fig. 2. Frequency of CDKN2A alterations in various cancer types. Based on the types of aberrant CDKN2A , the bars represent the percentage of changes reported. |
2.1. Lymphoma
Several studies have demonstrated that promoter hyper-methylation leads to the loss of p16INK4a expression in lymphoma. Gastric lymphoma is an extra-nodal non-Hodgkins lymphoma and is associated with 2–8% of all gastric cancers (Alevizos et al., 2012 ). Huang et al. reported that 26.5% (13 of 49) of primary gastric lymphomas exhibited hyper-methylation of the CDKN2A promoter, suggesting that expression of p16INK4a is a clinical risk factor for gastric lymphoma (Huang et al., 2007 ). Burkitts lymphoma is a common subtype of B-cell non-Hodgkins lymphoma in children and adolescents (Molyneux et al., 2012 ). A recent analysis of 51 Burkitts lymphoma tumor samples revealed that methylation of the CDKN2A promoter occurred in 72.5% of the samples and nuclear expression of the p16INK4a protein remained undetectable in about 41% of the samples (Robaina et al., 2015 ). In this study, CDKN2A promoter methylation was detected in 32 patient samples (80%) at stage III/IV of the cancer ( Robaina et al., 2015 ).
2.2. Skin cancer and melanoma
Solar ultraviolet (UV) radiation is the most common risk factor for the initiation and promotion of melanoma and non-melanoma skin carcinogenesis (de Gruijl, 1999 ). The CDKN2A gene is a melanoma susceptibility gene and its mutations are present in 20 to 40% of familial and 2 to 3% of sporadic melanomas ( Kostaki et al., 2014 ). The inactivation of CDKN2A in skin cancer involves histone modifications as well as DNA methylation. Chronic exposure of HaCaT skin keratinocytes to UVA radiation has been reported to cause 80 to 90% histone methylation (H3K4m3) and 50 to 70% DNA methylation in the CDKN2A promoter region ( Chen et al., 2012a ). Deletion of p16INK4a has also been detected in 50% of melanomas and its inactivation by point mutations occurs in about 9% of cases, which correlates with an increased risk of metastases and disease progression. Methylation of the CDKN2A gene promoter occurs in about 5 to 19% of sporadic melanomas, whereas promoter methylation of the gene was found in 27 to 33% of melanoma metastases ( Kostaki et al., 2014 ). In cutaneous melanoma metastases, the CDKN2A promoter is hyper-methylated in about 25% (15/59) of cases and non-synonymous mutation of the gene was observed in about 16% (9/56) of cases examined ( Jonsson et al., 2010 ).
ANRIL (antisense noncoding RNA in the INK4 locus) mediates a cis-acting silencing mechanism. ANRIL binds with PRC1 at the RNA-binding domains of CBX7 and methylates the CDKN2A promoter region at H3K27, which inhibits CDKN2A gene expression ( Sarkar et al., 2015 , Yap et al., 2010 and Sato et al., 2010 ).
2.3. Head and neck cancer
Head and neck squamous cell carcinoma (HNSCC) is a heterogeneous disease that arises in the areas of the nasal and oral cavities, pharynx and larynx. Although HNSCC can be caused by infection with human papilloma virus (HPV) (Bishop et al., 2013 ), approximately 90% of HPV-negative HNSCC tumors exhibit low expression of CDKN2A. This is largely due to mutations, loss of heterozygosity, and DNA hyper-methylation of the gene ( Veganzones et al., 2015 ). In one study, 57% of HPV-negative HNSCC from the TCGA (The Cancer Genome Atlas ) dataset was due to mutation or loss of the CDKN2A gene ( Chung et al., 2015 ). In primary HNSCC with deficient expression of CDKN2A , 66.7% (20/30) of the tumors exhibited DNA methylation of the CDKN2A promoter. The number of methylations was found to be 4 methylations at exon 1, 7 at exon 2 and 9 each at exons 1 and 2 ( El-Naggar et al., 1997 ).
Oral cancer includes a group of neoplasms affecting any region of the oral cavity, pharyngeal regions and salivary glands. More than 90% of all oral neoplasms are oral squamous cell carcinomas (OSCCs) (Markopoulos, 2012 ). Genetic alterations in OSCC might activate mutations or methylation of cell cycle regulatory genes, thereby promoting cell survival and proliferation (Al-Kaabi et al., 2014 ). In OSCC patients, hyper-methylation of the CDKN2A promoter was observed 60% of the time and oral leukoplakia patients also exhibited 60% hyper-methylation in the CDKN2A promoter ( Asokan et al., 2014 ).
2.4. Pancreatic cancer
Because of their severe metastatic potential, pancreatic tumors are the most aggressive types of cancer. Expression of CDKN2A has been reported to be aberrant in ~ 95% of pancreatic adenocarcinomas, and approximately 15% of those (El-Naggar et al., 1997 ) and 24.6% in another study (Jiao et al., 2007 ) were attributed to promoter hyper-methylation. The CDKN2A gene is abnormally methylated in 27% of pancreatic cancer cell lines ( Moore et al., 2001 ). In addition, the mutation of CDKN2A occurred 11.8% of the time in hereditary pancreatic cancer patients ( Salo-Mullen et al., 2015 ).
2.5. Lung cancer
Lung cancer is the leading cause of cancer death and most patients with lung cancer suffer from non-small cell lung cancer (NSCLC) (Siegel et al., 2015 ). Alterations in CDKN2A were examined in 63 NSCLCs samples of which 30 samples were primary resected NSCLCs with metastatic involvement of thoracic lymph nodes and 33 NSCLCs were without lymph node metastases ( Marchetti et al., 1997 ). The analysis revealed that 6 NSCLC tumor samples had somatic aberrations of the CDKN2A gene, including 4 mutations, 1 frame-shift and 1 homozygous deletion ( Marchetti et al., 1997 ). These alterations of CDKN2A were significantly associated with lymph node metastasis of NSCLC. Further analysis of 40 NSCLC adenocarcinoma cell lines revealed that CDKN2A was inactivated in 75% (30/40) of cases including 16 homozygous deletions, 10 methylations and 4 mutations ( Tam et al., 2013 ). In another study, alteration of CDKN2A in NSCLC adenocarcinoma tissue samples was noted as 38% (17/45) and included 10 homozygous deletions, 4 methylations and 3 mutations ( Tam et al., 2013 ).
2.6. Esophageal cancer
Esophageal cancer is the 6th leading cause of cancer death worldwide (Zhang, 2013 ). Esophageal squamous cell carcinoma (ESCC) is more common in the developing world and arises from the epithelial cells. The promoter region of CDKN2A was highly methylated in tissue samples from Chinese subjects (81.7% or 210/257) ( Chen et al., 2012b ). Among 38 Japanese ESCC samples examined, 13% showed a loss of heterozygosity of the CDKN2A gene and 67 tumors showed 6% with CDKN2A mutations ( Kuwabara et al., 2011 ). A novel 7 base pair (TCCAGCC) deletion in 22 of 106 (~ 20%) esophageal tumor samples was observed in exon 2 of CDKN2A ( Qureshi et al., 2012 ). An in silico study revealed that the deletion of these 7 base pairs resulted in premature termination and caused instability of the p16INK4a /CDK6 complex (Qureshi et al., 2012 ).
2.7. Gastric cancer
Gastric (stomach) cancer develops in the lining of the stomach. In a meta-analysis of Chinese gastric cancer patients, hyper-methylation of the CDKN2A promoter was recorded as 43.3% of the median average (28.3–64.4%), and was significantly correlated with CDKN2A promoter methylation and carcinogenesis ( Peng et al., 2014 and Wang et al., 2014 ). Infection with the Epstein-Barr virus (EBV) is one risk factor for gastric cancer. EBV-associated gastric carcinoma (EBVaGC) accounts for approximately 8–10% of all gastric carcinomas (Liang et al., 2014 ). Hyper-methylation of the CDKN2A promoter was detected in 81.6% and 33.3% of the EBVaGC and EBVnGC (EBV-negative gastric carcinomas), respectively ( He et al., 2015 ). These findings suggest that a high level of CDKN2A promoter methylation is a risk factor for developing EBV-associated gastric cancers. Another important etiologic factor for gastric carcinogenesis is Helicobacter pylori (H. pylori ) infection. Matsusaka et al. demonstrated that H. Pylori infection promotes CDKN2A DNA methylation from 21.3% to 45.0%, which correlates with poor tumor differentiation, increased lymph node metastasis, and lower survival rates of gastric cancer patients ( Matsusaka et al., 2014 and Qu et al., 2013 ).
2.8. Colorectal cancer
The development of colorectal cancer involves genetic and epigenetic changes of several tumor suppressor genes, including CDKN2A ( Chan et al., 2002 ). Similar to other cancers, the CDKN2A gene is silenced through promoter hyper-methylation during the course of colorectal cancer pathogenesis ( Kim et al., 2010 ). Kim et al. reported that promoter methylation of CDKN2A occurred in 11.9% of 285 sporadic colorectal cancer patients. Among these CDKN2A hyper-methylated cancer patients, 10.6% of 264 patients exhibited microsatellites with low frequency, whereas 28.6% of 21 patients showed microsatellites with high frequency ( Kim et al., 2010 ). In another study, CDKN2A promoter methylation occurred in 17.1% of 497 patients and its regulation was highly associated with poor survival in stage II and III colorectal cancer patients treated with adjuvant fluoropyrimidine ( Lee et al., 2015 ). The prognostic value of concurrent methylation of the CDKN2A promoter was associated with gender variation and was significant only in male patients ( Lee et al., 2015 ).
2.9. Ovarian cancer
Ovarian cancer is the most common form of gynecological cancer and a leading cause of cancer-related mortality among women (Jayson et al., 2014 ). This cancer is diagnosed usually at an advanced stage and has a high rate of recurrence (Hennessy et al., 2009 ). In a recent study, Bhagat et al. demonstrated that the frequency of CDKN2A promoter methylation was 43% in 134 invasive cancer cases including 22% of 23 low malignancy patient tumors and 42% of 26 benign cases ( Bhagat et al., 2014 ). Down-regulation of CDKN2A mRNA expression and hyper-methylation of the CDKN2A promoter are significantly associated.
2.10. Prostate cancer
Prostate cancer presents mostly as adenocarcinomas and is the second leading cause of cancer death in men (Siegel et al., 2015 ). Silencing of the CDKN2A gene plays a critical role in prostate cancer progression. Methylation of the CDKN2A promoter has been reported to occur in 47.6% of 21 patients with poor prognosis ( Ameri et al., 2011 ). Epigenetically, ANRIL and H3K2me are involved and alternatively bind with CBX7 of PRC1, thereby repressing CDKN2A gene transcription ( Yap et al., 2010 ).
2.11. Renal cell carcinoma
Accumulation of various genetic aberrations, including the CDKN2A gene, underlies the development of renal cell carcinomas ( Dulaimi et al., 2004 ). Evaluation of the methylation status of the promoter CpG island of CDKN2A and immunohistochemical detection of the p16INK4a -encoded protein in 57 patients with renal carcinomas revealed that the CDKN2A gene was hyper-methylated in 22.9% of patients and none of them expressed the p16INK4a protein product (Vidaurreta et al., 2008 ). The lack of p16INK4a protein expression was detected in 52.9% of the tumors, suggesting the involvement of another genetic alteration or post-transcriptional modification of the protein (Vidaurreta et al., 2008 ).
3. Molecular switches associated with p16INK4a aberrations
The inactivation of CDKN2A in cancer is neither an isolated event nor does it appear to have a direct link with carcinogen exposure ( Table 2 ). Analysis of the current literature reveals that promoter methylation of CDKN2A is not associated with HPV infection, which is a cause of head and neck squamous cell carcinomas ( Chung et al., 2015 ). However, the epigenetic changes in CDKN2A are associated with simultaneous genetic or epigenetic alterations in other cancer-related oncogenes or tumor suppressor genes ( Veganzones et al., 2015 , Chung et al., 2015 , Kostaki et al., 2014 , Tam et al., 2013 , Wilson et al., 2010 and Jonsson et al., 2010 ). Thus, the study of the concordance between p16INK4a inactivation with other tumor-related genetic/epigenetic lesions could provide new avenues for developing anticancer therapies. Tam et al. have demonstrated that mutations of the epidermal growth factor receptor (EGFR ) and KRAS are major oncogenic drivers in the pathogenesis of lung adenocarcinomas. The mutation of EGFR is reportedly associated with CDKN2A homozygous deletion or mutation, whereas KRAS mutation is related to hyper-methylation of the CDKN2A promoter ( Tam et al., 2013 ). However, changes in STK11 (also known as LKB1 ), a gene frequently mutated in lung adenocarcinomas, have no impact on CDKN2A inactivation mechanisms ( Tam et al., 2013 ). Veganzones and colleagues investigated the frequency of simultaneous methylation of CDKN2A and hMLH1 , a gene that encodes a DNA repair enzyme, in colorectal cancer patients with microsatellite instability (MSI) ( Veganzones et al., 2015 ). The outcome of the analysis of 51 samples of MSI-positive sporadic colorectal cancer was expressed by a new variable referred to as combined methylation of CDKN2A and hMLH1 (CMETH2 ). Results indicated that 17 of 51 patients (33.3%) tested positive for CMETH2 expression, which was associated with poorly differentiated tumors in proximal locations. The clinic-pathological implication of CMETH2 was reflected in the overall survival of patients with distal tumors ( Veganzones et al., 2015 ).
| Genes/Factors | Cancer types | Note | Reference |
|---|---|---|---|
| HPV | Head and neck squamous cell carcinoma | CDKN2A alteration in non-HPV-cancer | Chung et al. (2015 ) |
| EGFR | Lung adenocarcinoma | CDKN2A homozygous deletion or mutation is correlated with EGFR mutation | Tam et al. (2013 ) |
| KRAS | Hypermethylation of CDKN2A promoter is correlated with KRAS mutation | ||
| hMLH1 (human mutL homolog 1) | Colorectal cancer (microsatellite instability) | Hypermethylation of both CDKN2A and hMLH1 is 33.3% (17/51) | Veganzones et al. (2015 ) |
| SETDB1 | (Sporadic cutaneous) Melanoma | Cytoplasmic SETDB1 expression correlates with higher frequency of CDKN2A methylation and p16INK4A expression | Kostaki et al. (2014 ) |
| NRAS | Cutaneous melanoma | NRAS-mutated tumors have CDKN2A promoter methylation (52%, 12/23) | Jonsson et al. (2010 ) |
| SNF5 | – | Inactivation of H3K27 tri-methylation of CDKN2A by EZH2 in deficient SNF5 | Wilson et al. (2010 ) |
Histone modification, especially histone 3-lysine-9 methylation (H3K9) is a common mechanism of transcriptional repression of gene expression (Yoruker et al., 2012 ). SETDB1, which belongs to the family of SET domain histone methyltransferases including Suv39H, EZH2 and G9a, contains a highly conserved motif of 150-amino acids and is involved in the modulations of chromatin structure (Yang et al., 2002 ). The SETDB1 protein structure contains a CpG DNA methyl-binding domain, which regulates H3K9 methylation activity (Ceol et al., 2011 ). The CpG island methylation of the CDKN2A gene promoter and expression of SETDB1 in sporadic cutaneous melanomas are highly correlated with histologic prognostic parameters ( Kostaki et al., 2014 ). Methylation of the CDKN2A promoter is associated with 52% (12/23) of NRAS -mutated cutaneous melanomas compared with BRAF -mutated (7%, 2/27) tumors ( Jonsson et al., 2010 ). EZH2, a histone methyltransferase and a catalytic subunit of the PRC2 polycomb repressor, mediates gene silencing by tri-methylating H3K27 of various target gene promoters ( Bracken et al., 2007 and Cao et al., 2002 ). SNF5, one of the core subunits of Brahma-associated factor (BAF) chromatin remodeler complexes, down-regulates EZH2 transcription (Wilson et al., 2010 ). Thus, the loss of SNF5 function leads to increased EZH2 expression, thereby repressing the expression of CDKN2A through the tri-methylation of H3K27 in the CDKN2A promoter region ( Wilson et al., 2010 ).
4. Epigenetic induction of CDKN2A
Reactivation of silenced CDKN2A or the inhibition of epigenetic repression of the gene could be a rational strategy for the prevention or treatment of various cancers. While epigenetic silencing of CDKN2A is caused by DNA hyper-methylation and histone modification ( Bracken et al., 2007 , Cao et al., 2002 and Collado et al., 2007 ), restoration of p16INK4a transcriptional activation can be achieved by a set of intracellular regulatory genes as well as a series of small molecule epigenetic modifiers (Table 3 , Fig. 3 and Fig. 4 ) ( Crea et al., 2009 , Feng et al., 2009 , Hassler et al., 2012 , Kollmann et al., 2011 , Li et al., 2013a , Majid et al., 2008 , Nandakumar et al., 2011 , Valdez et al., 2015 and Zhang and Tong, 2014 ).
| Inducer | Mechanisms | Cancer types | References | |
|---|---|---|---|---|
| Genes | FOXA1 | EZH2 inhibition | Breast cancer and prostate cancer | Zhang and Tong (2014) , Li et al. (2013a ) |
| Si-ZBP-89 | HDAC3 inhibition | NCI-460 human lung cancer cells | Feng et al. (2009 ) | |
| Jmjd3 | Histone demethylation | Neurofibroma Schwann cells | (Gomez-Sanchez et al. (2013 ) | |
| Mutant UHRF1 | H3K9me3 inhibition | Nady et al. (2011 ) | ||
| c-JUN | Protect DNA methylation | Kollmann et al. (2011 ) | ||
| Compounds | Genistein | Induction of histone acetyl transferase (HAT) | Prostate cancer | Majid et al. (2008 ) |
| Modification of histone and Inhibition of binding BMI1 and c-MYC to CDKN2A promoter | Breast cancer | Li et al. (2013b ) | ||
| Sulforaphane (SFN) | HDAC3 inhibition by induction of Nrf2 | Colon cancer | Rajendran et al. (2015 ) | |
| EGCG | DNA demethylation and histone acetylation | Skin cancer cell | Nandakumar et al. (2011 ) | |
| TSA | HBP1 transcription factor acetylation | Wang et al.1 (2012 ) | ||
| EGCG and TSA | DNA demethylation | Lymphoma | Wu et al. (2013 ) | |
| TSA and 5-aza-2′- deoxycytidine | DNA demethylation | Epstein–Barr virus-associated gastric cancer cells | He et al. (2015 ) | |
| 5-aza-2′- deoxycytidine | DNA demethylation | Large cell lymphoma | Hassler et al. (2012 ) | |
| 5-aza-2′- deoxycytidine and irinotecan | DNA demethylation | Colorectal cancer cells | Crea et al., (2009 ) | |
| Cladribine, clofarabine | DNA demethylation | Acute myeloid leukemia | Valdez et al. (2015 ) | |
| Doxorubicin, FUMI (5-fluorouracil + mitomycin C) | DNA demethylation | Breast cancer | Klajic et al. (2014 ) |
|
|
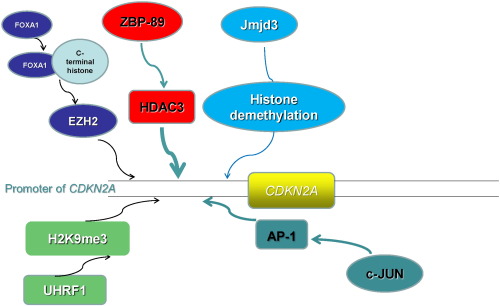
|
Fig. 3. The epigenetic induction of p16INK4a by regulatory genes. FOXA1, Si-ZBP-89, Jmjd3, Mutant UHRF1 and c-JUN induce p16INK4a protein expression by re-activation of the CDKN2A promoter. |
|
|
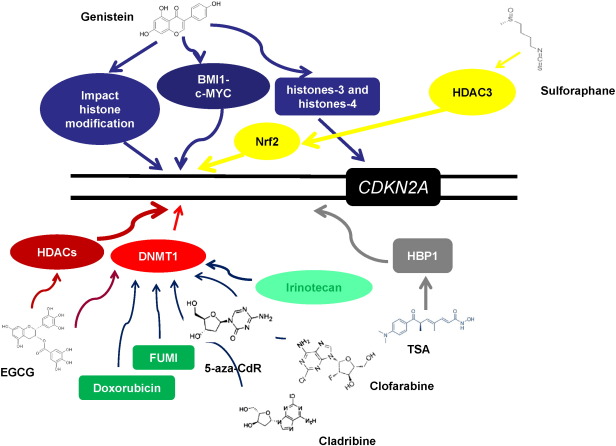
|
Fig. 4. The epigenetic induction of p16INK4a by reagents. Phytochemicals such as genistein, SFN and EGCG and synthetic chemicals, TSA, 5-aza-2′-deoxycytidine, irinotecan, cladribine, clofarabine, doxorubicin, FUMI (5-fluorouracil + mitomycin C) and combinations reactivate p16INK4a protein expression by prohibiting alterations in the CDKN2A promoter. |
4.1. Induction of CDKN2A by regulatory genes
The FOXA1 (Forkhead box A1) protein is a transcription factor that regulates the expression of p16INK4a (Li et al., 2013a and Zhang and Tong, 2014 ). In hormone-dependent cancers, such as breast and prostate cancers, the expression of FOXA1 is positively correlated with the expression of p16INK4a , but inhibits the expression of EZH2, which is a component of PRC2 and an epigenetic repressor of CDKN2A ( Nanni et al., 2006 ). FOXA1 directly binds to the C-terminal histone-binding motif and inhibits EZH2 methyltransferase activity, thereby inducing the expression of p16INK4a and suppressing cancer cell growth (Zhang and Tong, 2014 ).
ZBP-89, a four-zinc finger transcription factor, plays a role in the regulation of target genes by binding to the GC-rich DNA elements (Wu et al., 2007 ). ZBP-89 directly recruits histone deacetylase-3 (HDAC3) to the CDKN2A promoter and represses the expression CDKN2A by histone hypo-acetylation ( Feng et al., 2009 ). Therefore knockdown of ZBP-89 (ZBP-89i) by a specific small interfering RNA vector induced the expression of p16INK4a and cell senescence in NCI-H460 human lung cancer cells by promoting histone acetylation (Feng et al., 2009 ).
Jmjd3 (jumonji domin containing 3) is a histone lysine demethylase, which especially works to remove the tri-methylation of histone H3 at lysine 27. Jmjd3 induces expression of p16INK4a and senescence of Schwann cells under the conditions of nerve regeneration and tumorigenic stimulation (Gomez-Sanchez et al., 2013 ). The UHRF1 (ubiquitin-like plant homeobox domain (PHD) and RING finger containing 1) protein interacts with DNA methyltransferase 1 (DNMT1) and recognizes hemi-methylated CpG dinucleotides through its SRA (SET- and RING-associated domain) region (Bostick et al., 2007 ). The aromatic cage mutant of tandem tudor domain (TTD, 124–285 aa) within UHRF1 cannot bind to H2K9me3 and therefore induces the expression of p16INK4a (Nady et al., 2011 ).
The c-Jun protein is a component of activator protein (AP)-1 and a common regulator of cell cycle components and was reported to have a direct role in regulating gene transcription of e.g. , p53 and cyclin D1. Although JunB, as a tumor enhancer, reportedly inhibits promoter methylation of Cdk6 in BCR-ABL-induced leukemia ( Ott et al., 2007 ), binding of c-Jun to the promoter region shows a protective function and prevents methylation and silencing of these genes. Because the promoter region of the CDKN2A gene includes binding sites for AP-1, c-Jun can inhibit methylation of the CDKN2A promoter ( Kollmann et al., 2011 )
4.2. Induction of p16INK4a by reagents
A number of natural and synthetic small molecule modifiers of epigenetic regulation of gene expression have been identified (Fig. 4 ). Many of these small molecules are capable of restoring the expression of p16INK4a in various cancers. Genistein, an isoflavone present in soybean, is a cancer chemopreventive agent that inhibits cell proliferation and induces apoptosis (Gullett et al., 2010 ). Li et al. reported that genistein represses early breast tumorigenesis through epigenetic regulation of CDKN2A by impacting histone modifications as well as by recruiting the BMI1-c-MYC complex to the regulatory region in the CDKN2A promoter ( Li et al., 2013b ). In prostate cancer, treatment with genistein increased acetylated histones 3 and 4 of the CDKN2A transcription start sites ( Majid et al., 2008 ). Thus, soybean products containing genistein might be useful in preventing breast and prostate cancer through transcriptional activation of CDKN2A by modulating its epigenetic silencing ( Li et al., 2013b and Majid et al., 2008 ). Sulforaphane, a major component of broccoli and other cruciferous vegetables, is an inducer of nuclear factor erythroid 2 (NF-E2)-related factor 2 (Nrf2), which regulates the transcriptional activation of a battery of genes encoding various phase 2 detoxification enzymes ( Fahey et al., 1997 and Kensler et al., 2013 ). Rajendran et al. reported that Nrf2 wildtype mice showed a higher incidence of colon tumors than Nrf2 heterozygous (Nrf2+/− ) mice when treated with 1,2-dimethylhydrazine. Tumors from wildtype mice exhibited higher HDAC3 levels globally and deregulated p16INK4a levels locally. Treatment with sulforaphane markedly reduced the tumor burden in wildtype mice but not in Nrf2+/− mice. Sulforaphane, an inhibitor of HDAC3, a repressor of p16INK4a , induced p16INK4a expression and reduced the tumor burden in this model (Rajendran et al., 2015 ).
Epigallocatechin-3-gallate (EGCG), a main polyphenol component of green tea, stimulated expression of p16INK4a by inhibiting DNA methylation and increasing histone acetylation in the CDKN2A promoter of human skin cancer cells ( Nandakumar et al., 2011 ). Trichostatin A (TSA) is an HDAC4 inhibitor that elevated the acetylation of HBP1 (K419), a member homologous to the sequence-specific high mobility group (HMG) family of transcription factors, and increased the expression of p16INK4a , thereby inducing apoptosis and differentiation (Wang et al., 2012 ). The combination treatment with inhibitors of DNMTs and HDACs might be a representative therapeutic strategy in cancer. Treatment of CA46 lymphoma cells with EGCG (24 μg/ml) or the combination treatment of EGCG (6 μg/ml) and TSA (15 ng/ml) resulted in lower proliferative indices when compared to the other groups. Co-treatment with EGCG and TSA decreased the DNA methylation of CDKN2A , which coincided with increased CDKN2A mRNA and protein expression. Thus, EGCG and TSA synergistically induced CDKN2A expression by reducing promoter methylation, which might decrease CA46 lymphoma cell proliferation ( Wu et al., 2013 ).
5-Aza-2′-dexoycytidine (5-aza-CdR, decitabine, Dacogen®) is a DNMT inhibitor, which has been approved by the Food and Drug Administration (FDA) for the treatment of myelodysplastic syndrome, a hematological malignancy (Scandura et al., 2011 ). Treatment of anaplastic large cell lymphoma cells with 5-aza-CdR resulted in the inhibition of proliferation through G1 phase cell cycle arrest in vitro and in vivo through re-expression of p16INK4a (Hassler et al., 2012 ). Furthermore, combination treatment with TSA and 5-aza-CdR exerted synergic cell growth inhibition and apoptosis in EBV-associated gastric carcinoma through the induction of CDKN2A by inhibiting methylation ( He et al., 2015 ). On the other hand, co-treatment with 5-aza-CdR and irinotecan, a topoisomerase-1 inhibitor, caused a more sensitive cytotoxic effect in p53 -mutated colon cancer cells, such as HT-29, SW620, and WiDr cells ( Crea et al., 2009 ). The synergistic effect of 5-aza-CdR and irinotecan was significantly associated with topoisomerase I up-regulation by 5-aza-CdR, and combined to induce CDKN2A expression through promoter demethylation as well as Sp1 up-regulation. Expression of p16INK4a enhanced cell cycle arrest after irinotecan treatment (Crea et al., 2009 ).
Cladribine and clofarabine are second-generation analogues of 2′-deoxyadenosine. Fludarabine (Fludara) and Busulfan (Myeran) and are cell cycle non-specific alkylating antineoplastic agents. Although both cladribine and clofarabine induced p16INK4a expression, cladribine was effective at a lower concentration compared to clofarabine (Valdez et al., 2015 ). The combination of cladribine or clofarabine with fludarabin and busulfan caused synergic cytotoxicity in acute myeloid leukemia. Moreover, the addition of panobinostat, an HDAC inhibitor, and 5-aza-CdR with these combinations also enhanced cytotoxicity. Inclusion of panobiostat and 5-aza-CdR increased histone modifications and DNA demethylation, and increased the levels of the p16INK4a , p15INK4b and p21Waf1/Cip1 proteins (Valdez et al., 2015 ).
Treatment with doxorubicin and FUMI (5-fluorouracil and mitomycin C) in breast cancer resulted in demethylation of the CDKN2A promoter by 19.3% and 9.1%, respectively ( Klajic et al., 2014 ). The CDKN2A gene was differentially methylated before/after treatment with doxorubicin and before/after treatment between responders. Lower levels of methylation were observed after treatment in the responder groups. Also, CDKN2A methylation levels among the non-responders were significantly changed ( Klajic et al., 2014 ).
5. Conclusion
A high frequency of genetic and epigenetic alterations (e.g. , promoter hyper-methylation, homozygous deletion or mutation) in the CDKN2A gene has been observed in human cancer cell lines derived from various tumor types. However, a significantly lower frequency of CDKN2A abnormalities has been reported in fresh, non-cultured primary tumors and cell lines. Therefore, regulation of CDKN2A abnormalities will have benefits for the cancer prevention and/or therapy.
Outstanding questions
Besides genetic and epigenetic aberrations, the regulation of gene expression is also associated with the status of many other proteins, such as p53, BRAF, ataxia talengectia mutated (ATM), phosphatase and tensin homolog deleted at chromosome 10 (PTEN), KRAS and phosphatidylinositol 3-kinase (PI3-K) as well as the components of the CDKN2A promoter, such as the PRC1 and PRC2 complexes and long noncoding RNAs. HPV, a small DNA virus (major types HPV-16 and HPV-18) expresses E6 and E7 oncoproteins and is linked causally to most cervical cancers that show a high expression of p16INK4a ( Kobalka et al., 2015 , Munger et al., 2013 , Pauck et al., 2014 and Nehls et al., 2008 ). The E6 and E7 oncoproteins directly block p53 and pRb tumor suppressors resulting in the accumulation of p16INK4a , which is upstream of p53 and pRb ( Dyson et al., 1989 and Scheffner et al., 1993 ). HPV-infection-associated cervical cancer also mediates the high expression of p16INK4a by epigenetic modulation of the CDKN2A upstream promoter ( Nehls et al., 2008 and Mclaughlin-Drubin et al., 2013 ). Thus in HPV-infection-associated cancer, we should consider the p16INK4a as a biomarker in an opposite manner than what is generally expected. Although smoking and/or drinking is a risk factor for lung, head and neck, and pancreatic cancers ( Gillison et al., 2012 , Jiao et al., 2007 and Tam et al., 2013 ), meaningful correlations of p16INK4a expression with smoking or drinking are not yet supported by strong evidence ( Jiao et al., 2007 , Gillison et al., 2012 and Tam et al., 2013 ). Because p16INK4a is a critical regulator of cell proliferation and is inactivated during the course of tumorigenesis, methods for restoration of p16INK4a function could provide good therapeutic strategies. To achieve this goal, the focus has been directed toward understanding the molecular mechanisms, especially genetic and epigenetic changes that lead to p16INK4a inactivation in cancer, and developing small molecule modifiers of these mechanistic switches. For example, ZBP-89 can induce the expression of p16INK4a (Zhang et al., 2010 ). Likewise, FOXA1 and jmjd3 enhance CDKN2A expression by direct transcriptional activation and promoter di-methylation, respectively. Thus, discovery of small molecule activators of ZBP-89, jmjd3 or FOXA1 might be a future research goal for developing novel anticancer therapies. On the other hand, factors that repress CDKN2A gene expression, such as SETDB1, EZH2, or PcB proteins, could be potential therapeutic targets to induce p16INK4a functionality and tumor suppression. Although several natural and synthetic compounds, such as genistein, sulforaphane, EGCG and 5-aza-CdR have been shown to intervene against the epigenetic silencing of CDKN2A , mechanism-based development of p16INK4a activators warrants further studies.
Search strategy and selection criteria
This review was prepared by searching in PubMed with querying key words: p16INK4a , epigenetics, alteration, gene alteration, gene silencing, cancer, promoter alteration and induction of p16INK4a . The search was conducted for research articles including clinical reports up to 28 December 2015 and we especially summarized research articles in each cancer type.
Financial support
This work was supported by grant funding from the National Institutes of HealthCA166011 , CA187027 and CA196639 , The Hormel Foundation and Henan Provincial Government, China . Funders had no role in producing this manuscript.
Disclosure of potential conflicts of interests
No potential conflicts of interest are disclosed.
Authors' contribution
RZ contributed to the literature search and collection of articles, assisted with designing the figures and writing; BYC contributed to the design and organization of the manuscript; MHL did most of the original writing; AMB did all the editing and confirmation of references and accurate information; ZD supervised the studies and allocated the funding.
Acknowledgements
We wish to thank Dr. Joydeb Kumar Kundu for helpful comments on the manuscript.
References
- Aguilo et al., 2011 F. Aguilo, M.M. Zhou, M.J. Walsh; Long noncoding RNA, polycomb, and the ghosts haunting INK4b-ARF-INK4a expression; Cancer Res., 71 (2011), pp. 5365–5369
- Alevizos et al., 2012 L. Alevizos, I.P. Gomatos, S. Smparounis, M.M. Konstadoulakis, G. Zografos; Review of the molecular profile and modern prognostic markers for gastric lymphoma: how do they affect clinical practice?; Can. J. Surg., 55 (2012), pp. 117–124
- Al-Kaabi et al., 2014 A. Al-Kaabi, L.W. Van Bockel, A.J. Pothen, S.M. Willems; p16INK4A and p14ARF gene promoter hypermethylation as prognostic biomarker in oral and oropharyngeal squamous cell carcinoma: a review; Dis. Markers, 2014 (2014), p. 260549
- Ameri et al., 2011 A. Ameri, A. Alidoosti, S.Y. Hosseini, M. Parvin, M.H. Emranpour, F. Taslimi, E. Salehi, P. Fadavip; Prognostic value of promoter hypermethylation of retinoic acid receptor beta (RARB) and CDKN2 (p16/MTS1) in prostate cancer; Chin. J. Cancer Res., 23 (2011), pp. 306–311
- Asokan et al., 2014 G.S. Asokan, S. Jeelani, N. Gnanasundaram; Promoter hypermethylation profile of tumour suppressor genes in oral leukoplakia and oral squamous cell carcinoma; J. Clin. Diagn. Res., 8 (2014), pp. ZC09–ZC12
- Bhagat et al., 2014 R. Bhagat, S.S. Kumar, S. Vaderhobli, C.S. Premalata, V.R. Pallavi, G. Ramesh, L. Krishnamoorthy; Epigenetic alteration of p16 and retinoic acid receptor beta genes in the development of epithelial ovarian carcinoma; Tumour Biol., 35 (2014), pp. 9069–9078
- Bishop et al., 2013 J.A. Bishop, T.W. Guo, D.F. Smith, H. Wang, T. Ogawa, S.I. Pai, W.H. Westra; Human papillomavirus-related carcinomas of the sinonasal tract; Am. J. Surg. Pathol., 37 (2013), pp. 185–192
- Bostick et al., 2007 M. Bostick, J.K. Kim, P.O. Esteve, A. Clark, S. Pradhan, S.E. Jacobsen; UHRF1 plays a role in maintaining DNA methylation in mammalian cells; Science, 317 (2007), pp. 1760–1764
- Bracken et al., 2007 A.P. Bracken, D. Kleine-Kohlbrecher, N. Dietrich, D. Pasini, G. Gargiulo, C. Beekman, K. Theilgaard-Monch, S. Minucci, B.T. Porse, J.C. Marine, K.H. Hansen, K. Helin; The Polycomb group proteins bind throughout the INK4A-ARF locus and are disassociated in senescent cells; Genes Dev., 21 (2007), pp. 525–530
- Cancer Genome Atlas, N., 2015 Cancer Genome Atlas, N.; Comprehensive genomic characterization of head and neck squamous cell carcinomas; Nature, 517 (2015), pp. 576–582
- Cao et al., 2002 R. Cao, L. Wang, H. Wang, L. Xia, H. Erdjument-Bromage, P. Tempst, R.S. Jones, Y. Zhang; Role of histone H3 lysine 27 methylation in Polycomb-group silencing; Science, 298 (2002), pp. 1039–1043
- Ceol et al., 2011 C.J. Ceol, Y. Houvras, J. Jane-Valbuena, S. Bilodeau, D.A. Orlando, V. Battisti, L. Fritsch, W.M. Lin, T.J. Hollmann, F. Ferre, C. Bourque, C.J. Burke, L. Turner, A. Uong, L.A. Johnson, R. Beroukhim, C.H. Mermel, M. Loda, S. Ait-Si-Ali, L.A. Garraway, R.A. Young, L.I. Zon; The histone methyltransferase SETDB1 is recurrently amplified in melanoma and accelerates its onset; Nature, 471 (2011), pp. 513–517
- Chan et al., 2002 A.O. Chan, R.R. Broaddus, P.S. Houlihan, J.P. Issa, S.R. Hamilton, A. Rashid; CpG island methylation in aberrant crypt foci of the colorectum; Am. J. Pathol., 160 (2002), pp. 1823–1830
- Chen et al., 2012a I.P. Chen, S. Henning, A. Faust, P. Boukamp, B. Volkmer, R. Greinert; UVA-induced epigenetic regulation of P16(INK4a) in human epidermal keratinocytes and skin tumor derived cells; Photochem. Photobiol. Sci., 11 (2012), pp. 180–190
- Chen et al., 2012b J. Chen, Z.J. Huang, Y.Q. Duan, X.R. Xiao, J.Q. Jiang, R. Zhang; Aberrant DNA methylation of P16, MGMT, and hMLH1 genes in combination with MTHFR C677T genetic polymorphism and folate intake in esophageal squamous cell carcinoma; Asian Pac. J. Cancer Prev., 13 (2012), pp. 5303–5306
- Chung et al., 2015 C.H. Chung, V.B. Guthrie, D.L. Masica, C. Tokheim, H. Kang, J. Richmon, N. Agrawal, C. Fakhry, H. Quon, R.M. Subramaniam, Z. Zuo, T. Seiwert, Z.R. Chalmers, G.M. Frampton, S.M. Ali, R. Yelensky, P.J. Stephens, V.A. Miller, R. Karchin, J.A. Bishop; Genomic alterations in head and neck squamous cell carcinoma determined by cancer gene-targeted sequencing; Ann. Oncol., 26 (2015), pp. 1216–1223
- Collado et al., 2007 M. Collado, M.A. Blasco, M. Serrano; Cellular senescence in cancer and aging; Cell, 130 (2007), pp. 223–233
- Collins et al., 1997 K. Collins, T. Jacks, N.P. Pavletich; The cell cycle and cancer; Proc. Natl. Acad. Sci. U. S. A., 94 (1997), pp. 2776–2778
- Crea et al., 2009 F. Crea, E. Giovannetti, F. Cortesi, V. Mey, S. Nannizzi, M.I. Gallegos Ruiz, S. Ricciardi, M. Del Tacca, G.J. Peters, R. Danesi; Epigenetic mechanisms of irinotecan sensitivity in colorectal cancer cell lines; Mol. Cancer Ther., 8 (2009), pp. 1964–1973
- De Gruijl, 1999 F.R. De Gruijl; Skin cancer and solar UV radiation; Eur. J. Cancer, 35 (1999), pp. 2003–2009
- Dulaimi et al., 2004 E. Dulaimi, I. Ibanez De Caceres, R.G. Uzzo, T. Al-Saleem, R.E. Greenberg, T.J. Polascik, J.S. Babb, W.E. Grizzle, P. Cairns; Promoter hypermethylation profile of kidney cancer; Clin. Cancer Res., 10 (2004), pp. 3972–3979
- Dyson et al., 1989 N. Dyson, P.M. Howley, K. Munger, E. Harlow; The human papilloma virus-16 E7 oncoprotein is able to bind to the retinoblastoma gene product; Science, 243 (1989), pp. 934–937
- El-Naggar et al., 1997 A.K. El-Naggar, S. Lai, G. Clayman, J.K. Lee, M.A. Luna, H. Goepfert, J.G. Batsakis; Methylation, a major mechanism of p16/CDKN2 gene inactivation in head and neck squamous carcinoma; Am. J. Pathol., 151 (1997), pp. 1767–1774
- Fahey et al., 1997 J.W. Fahey, Y. Zhang, P. Talalay; Broccoli sprouts: an exceptionally rich source of inducers of enzymes that protect against chemical carcinogens; Proc. Natl. Acad. Sci. U. S. A., 94 (1997), pp. 10367–10372
- Feng et al., 2009 Y. Feng, X. Wang, L. Xu, H. Pan, S. Zhu, Q. Liang, B. Huang, J. Lu; The transcription factor ZBP-89 suppresses p16 expression through a histone modification mechanism to affect cell senescence; FEBS J., 276 (2009), pp. 4197–4206
- Gil and Peters, 2006 J. Gil, G. Peters; Regulation of the INK4b-ARF-INK4a tumour suppressor locus: all for one or one for all; Nat. Rev. Mol. Cell Biol., 7 (2006), pp. 667–677
- Gillison et al., 2012 M.L. Gillison, Q. Zhang, R. Jordan, W. Xiao, W.H. Westra, A. Trotti, S. Spencer, J. Harris, C.H. Chung, K.K. Ang; Tobacco smoking and increased risk of death and progression for patients with p16-positive and p16-negative oropharyngeal cancer; J. Clin. Oncol., 30 (2012), pp. 2102–2111
- Gomez-Sanchez et al., 2013 J.A. Gomez-Sanchez, C. Gomis-Coloma, C. Morenilla-Palao, G. Peiro, E. Serra, M. Serrano, H. Cabedo; Epigenetic induction of the Ink4a/Arf locus prevents Schwann cell overproliferation during nerve regeneration and after tumorigenic challenge; Brain, 136 (2013), pp. 2262–2278
- Gullett et al., 2010 N.P. Gullett, A.R. Ruhul Amin, S. Bayraktar, J.M. Pezzuto, D.M. Shin, F.R. Khuri, B.B. Aggarwal, Y.J. Surh, O. Kucuk; Cancer prevention with natural compounds; Semin. Oncol., 37 (2010), pp. 258–281
- Hanahan and Weinberg, 2011 D. Hanahan, R.A. Weinberg; Hallmarks of cancer: the next generation; Cell, 144 (2011), pp. 646–674
- Hassler et al., 2012 M.R. Hassler, A. Klisaroska, K. Kollmann, I. Steiner, M. Bilban, A.I. Schiefer, V. Sexl, G. Egger; Antineoplastic activity of the DNA methyltransferase inhibitor 5-aza-2'-deoxycytidine in anaplastic large cell lymphoma; Biochimie, 94 (2012), pp. 2297–2307
- Hauptman and Glavac, 2013 N. Hauptman, D. Glavac; Long non-coding RNA in cancer; Int. J. Mol. Sci., 14 (2013), pp. 4655–4669
- He et al., 2015 D. He, Y.W. Zhang, N.N. Zhang, L. Zhou, J.N. Chen, Y. Jiang, C.K. Shao; Aberrant gene promoter methylation of p16, FHIT, CRBP1, WWOX, and DLC-1 in Epstein-Barr virus-associated gastric carcinomas; Med. Oncol., 32 (2015), p. 92
- Hennessy et al., 2009 B.T. Hennessy, R.L. Coleman, M. Markman; Ovarian cancer; Lancet, 374 (2009), pp. 1371–1382
- Huang et al., 2007 Q. Huang, X. Su, L. Ai, M. Li, C.Y. Fan, L.M. Weiss; Promoter hypermethylation of multiple genes in gastric lymphoma; Leuk. Lymphoma, 48 (2007), pp. 1988–1996
- Jayson et al., 2014 G.C. Jayson, E.C. Kohn, H.C. Kitchener, J.A. Ledermann; Ovarian cancer; Lancet, 384 (2014), pp. 1376–1388
- Jiao et al., 2007 L. Jiao, J. Zhu, M.M. Hassan, D.B. Evans, J.L. Abbruzzese, D. Li; K-ras mutation and p16 and preproenkephalin promoter hypermethylation in plasma DNA of pancreatic cancer patients: in relation to cigarette smoking; Pancreas, 34 (2007), pp. 55–62
- Jonsson et al., 2010 A. Jonsson, R. Tuominen, E. Grafstrom, J. Hansson, S. Egyhazi; High frequency of p16(INK4A) promoter methylation in NRAS-mutated cutaneous melanoma; J. Investig. Dermatol., 130 (2010), pp. 2809–2817
- Kensler et al., 2013 T.W. Kensler, P.A. Egner, A.S. Agyeman, K. Visvanathan, J.D. Groopman, J.G. Chen, T.Y. Chen, J.W. Fahey, P. Talalay; Keap1-nrf2 signaling: a target for cancer prevention by sulforaphane; Top. Curr. Chem., 329 (2013), pp. 163–177
- Kim et al., 2010 J.C. Kim, J.S. Choi, S.A. Roh, D.H. Cho, T.W. Kim, Y.S. Kim; Promoter methylation of specific genes is associated with the phenotype and progression of colorectal adenocarcinomas; Ann. Surg. Oncol., 17 (2010), pp. 1767–1776
- Klajic et al., 2014 J. Klajic, F. Busato, H. Edvardsen, N. Touleimat, T. Fleischer, I. Bukholm, A.L. Borresen-Dale, P.E. Lonning, J. Tost, V.N. Kristensen; DNA methylation status of key cell-cycle regulators such as CDKNA2/p16 and CCNA1 correlates with treatment response to doxorubicin and 5-fluorouracil in locally advanced breast tumors; Clin. Cancer Res., 20 (2014), pp. 6357–6366
- Kobalka et al., 2015 P.J. Kobalka, J.P. Abboud, X. Liao, K. Jones, B.W. Lee, B.S. Korn, D.O. Kikkawa, J.H. Lin; p16INK4A expression is frequently increased in periorbital and ocular squamous lesions; Diagn. Pathol., 10 (2015), p. 175
- Kollmann et al., 2011 K. Kollmann, G. Heller, V. Sexl; c-JUN prevents methylation of p16(INK4a) (and Cdk6): the villain turned bodyguard; Oncotarget, 2 (2011), pp. 422–427
- Kostaki et al., 2014 M. Kostaki, A.D. Manona, I. Stavraka, P. Korkolopoulou, G. Levidou, E.A. Trigka, E. Christofidou, G. Champsas, A.J. Stratigos, A. Katsambas, O. Papadopoulos, C. Piperi, A.G. Papavassiliou; High-frequency p16(INK) (4A) promoter methylation is associated with histone methyltransferase SETDB1 expression in sporadic cutaneous melanoma; Exp. Dermatol., 23 (2014), pp. 332–338
- Kuwabara et al., 2011 T. Kuwabara, T. Hiyama, S. Tanaka, M. Yoshihara, K. Arihiro, K. Chayama; Genetic pathways of multiple esophageal squamous cell carcinomas; Oncol. Rep., 25 (2011), pp. 453–459
- Lee et al., 2015 D.W. Lee, S.W. Han, Y. Cha, Y.Y. Rhee, J.M. Bae, N.Y. Cho, K.H. Lee, T.Y. Kim, D.Y. Oh, S.A. Im, Y.J. Bang, S.Y. Jeong, K.J. Park, G.H. Kang, T.Y. Kim; Different prognostic effect of CpG island methylation according to sex in colorectal cancer patients treated with adjuvant FOLFOX; Clin. Epigenetics, 7 (2015), p. 63
- Li et al., 2013a Q. Li, Y. Zhang, J. Fu, L. Han, L. Xue, C. LV, P. Wang, G. Li, T. Tong; FOXA1 mediates p16(INK4a) activation during cellular senescence; EMBO J., 32 (2013), pp. 858–873
- Li et al., 2013b Y. Li, H. Chen, T.M. Hardy, T.O. Tollefsbol; Epigenetic regulation of multiple tumor-related genes leads to suppression of breast tumorigenesis by dietary genistein; PLoS One, 8 (2013), p. e54369
- Liang et al., 2014 Q. Liang, X. Yao, S. Tang, J. Zhang, T.O. Yau, X. Li, C.M. Tang, W. Kang, R.W. Lung, J.W. Li, T.F. Chan, R. Xing, Y. Lu, K.W. Lo, N. Wong, K.F. To, C. Yu, F.K. Chan, J.J. Sung, J. Yu; Integrative identification of Epstein-Barr virus-associated mutations and epigenetic alterations in gastric cancer; Gastroenterology, 147 (2014) (1350-62 e4)
- Majid et al., 2008 S. Majid, N. Kikuno, J. Nelles, E. Noonan, Y. Tanaka, K. Kawamoto, H. Hirata, L.C. Li, H. Zhao, S.T. Okino, R.F. Place, D. Pookot, R. Dahiya; Genistein induces the p21WAF1/CIP1 and p16INK4a tumor suppressor genes in prostate cancer cells by epigenetic mechanisms involving active chromatin modification; Cancer Res., 68 (2008), pp. 2736–2744
- Marchetti et al., 1997 A. Marchetti, F. Buttitta, S. Pellegrini, G. Bertacca, A. Chella, V. Carnicelli, V. Tognoni, A. Filardo, C.A. Angeletti, G. Bevilacqua; Alterations of P16 (MTS1) in node-positive non-small cell lung carcinomas; J. Pathol., 181 (1997), pp. 178–182
- Markopoulos, 2012 A.K. Markopoulos; Current aspects on oral squamous cell carcinoma; Open Dent. J., 6 (2012), pp. 126–130
- Matsusaka et al., 2014 K. Matsusaka, S. Funata, M. Fukayama, A. Kaneda; DNA methylation in gastric cancer, related to Helicobacter pylori and Epstein-Barr virus; World J. Gastroenterol., 20 (2014), pp. 3916–3926
- Mclaughlin-Drubin et al., 2013 M.E. Mclaughlin-Drubin, D. Park, K. Munger; Tumor suppressor p16INK4A is necessary for survival of cervical carcinoma cell lines; Proc. Natl. Acad. Sci. U. S. A., 110 (2013), pp. 16175–16180
- Molyneux et al., 2012 E.M. Molyneux, R. Rochford, B. Griffin, R. Newton, G. Jackson, G. Menon, C.J. Harrison, T. Israels, S. Bailey; Burkitts lymphoma; Lancet, 379 (2012), pp. 1234–1244
- Moore et al., 2001 P.S. Moore, B. Sipos, S. Orlandini, C. Sorio, F.X. Real, N.R. Lemoine, T. Gress, C. Bassi, G. Kloppel, H. Kalthoff, H. Ungefroren, M. Lohr, A. Scarpa; Genetic profile of 22 pancreatic carcinoma cell lines. Analysis of K-ras, p53, p16 and DPC4/Smad4; Virchows Arch., 439 (2001), pp. 798–802
- Munger et al., 2013 K. Munger, T.K. Gwin, M.E. Mclaughlin-Drubin; p16 in HPV-associated cancers; Oncotarget, 4 (2013), pp. 1864–1865
- Nabel, 2002 E.G. Nabel; CDKs and CKIs: molecular targets for tissue remodelling; Nat. Rev. Drug Discov., 1 (2002), pp. 587–598
- Nady et al., 2011 N. Nady, A. Lemak, J.R. Walker, G.V. Avvakumov, M.S. Kareta, M. Achour, S. Xue, S. Duan, A. Allali-Hassani, X. Zuo, Y.X. Wang, C. Bronner, F. Chedin, C.H. Arrowsmith, S. Dhe-Paganon; Recognition of multivalent histone states associated with heterochromatin by UHRF1 protein; J. Biol. Chem., 286 (2011), pp. 24300–24311
- Nandakumar et al., 2011 V. Nandakumar, M. Vaid, S.K. Katiyar; (−)-Epigallocatechin-3-gallate reactivates silenced tumor suppressor genes, Cip1/p21 and p16INK4a, by reducing DNA methylation and increasing histones acetylation in human skin cancer cells; Carcinogenesis, 32 (2011), pp. 537–544
- Nanni et al., 2006 S. Nanni, C. Priolo, A. Grasselli, M. D'eletto, R. Merola, F. Moretti, M. Gallucci, P. De Carli, S. Sentinelli, A.M. Cianciulli, M. Mottolese, P. Carlini, D. Arcelli, M. Helmer-Citterich, C. Gaetano, M. Loda, A. Pontecorvi, S. Bacchetti, A. Sacchi, A. Farsetti; Epithelial-restricted gene profile of primary cultures from human prostate tumors: a molecular approach to predict clinical behavior of prostate cancer; Mol. Cancer Res., 4 (2006), pp. 79–92
- Nehls et al., 2008 K. Nehls, S. Vinokurova, D. Schmidt, F. Kommoss, M. Reuschenbach, F. Kisseljov, J. Einenkel, M. Von Knebel Doeberitz, N. Wentzensen; p16 methylation does not affect protein expression in cervical carcinogenesis; Eur. J. Cancer, 44 (2008), pp. 2496–2505
- Ott et al., 2007 R.G. Ott, O. Simma, K. Kollmann, E. Weisz, E.M. Zebedin, M. Schorpp-Kistner, G. Heller, S. Zochbauer, E.F. Wagner, M. Freissmuth, V. Sexl; JunB is a gatekeeper for B-lymphoid leukemia; Oncogene, 26 (2007), pp. 4863–4871
- Pauck et al., 2014 A. Pauck, B. Lener, M. Hoell, A. Kaiser, A.M. Kaufmann, W. Zwerschke, P. Jansen-Durr; Depletion of the cdk inhibitor p16INK4a differentially affects proliferation of established cervical carcinoma cells; J. Virol., 88 (2014), pp. 5256–5262
- Peng et al., 2014 D. Peng, H. Zhang, G. Sun; The relationship between P16 gene promoter methylation and gastric cancer: a meta-analysis based on Chinese patients; J. Cancer Res. Ther., 10 (Suppl) (2014), pp. 292–295
- Pomerantz et al., 1998 J. Pomerantz, N. Schreiber-Agus, N.J. Liegeois, A. Silverman, L. Alland, L. Chin, J. Potes, K. Chen, I. Orlow, H.W. Lee, C. Cordon-Cardo, R.A. Depinho; The Ink4a tumor suppressor gene product, p19Arf, interacts with MDM2 and neutralizes MDM2s inhibition of p53; Cell, 92 (1998), pp. 713–723
- Portela and Esteller, 2010 A. Portela, M. Esteller; Epigenetic modifications and human disease; Nat. Biotechnol., 28 (2010), pp. 1057–1068
- Qu et al., 2013 Y. Qu, S. Dang, P. Hou; Gene methylation in gastric cancer; Clin. Chim. Acta, 424 (2013), pp. 53–65
- Quelle et al., 1995 D.E. Quelle, F. Zindy, R.A. Ashmun, C.J. Sherr; Alternative reading frames of the INK4a tumor suppressor gene encode two unrelated proteins capable of inducing cell cycle arrest; Cell, 83 (1995), pp. 993–1000
- Qureshi et al., 2012 M.A. Qureshi, N. Jan, N.A. Dar, M. Hussain, K.I. Andrabi; A novel p16(INK4A) mutation associated with esophageal squamous cell carcinoma in a high risk population; Biomarkers, 17 (2012), pp. 552–556
- Rajendran et al., 2015 P. Rajendran, W.M. Dashwood, L. Li, Y. Kang, E. Kim, G. Johnson, K.A. Fischer, C.V. Lohr, D.E. Williams, E. Ho, M. Yamamoto, D.A. Lieberman, R.H. Dashwood; Nrf2 status affects tumor growth, HDAC3 gene promoter associations, and the response to sulforaphane in the colon; Clin. Epigenetics, 7 (2015), p. 102
- Robaina et al., 2015 M.C. Robaina, R.S. Faccion, V.O. Arruda, L.M. De Rezende, G.M. Vasconcelos, A.G. Apa, C.E. Bacchi, C.E. Klumb; Quantitative analysis of CDKN2A methylation, mRNA, and p16(INK4a) protein expression in children and adolescents with Burkitt lymphoma: biological and clinical implications; Leuk. Res., 39 (2015), pp. 248–256
- Salo-Mullen et al., 2015 E.E. Salo-Mullen, E.M. O'reilly, D.P. Kelsen, A.M. Ashraf, M.A. Lowery, K.H. Yu, D.L. Reidy, A.S. Epstein, A. Lincoln, A. Saldia, L.M. Jacobs, R. Rau-Murthy, L. Zhang, R.C. Kurtz, L. Saltz, K. Offit, M.E. Robson, Z.K. Stadler; Identification of germline genetic mutations in patients with pancreatic cancer; Cancer (2015)
- Sarkar et al., 2015 D. Sarkar, E.Y. Leung, B.C. Baguley, G.J. Finlay, M.E. Askarian-Amiri; Epigenetic regulation in human melanoma: past and future; Epigenetics, 10 (2015), pp. 103–121
- Sato et al., 2010 K. Sato, H. Nakagawa, A. Tajima, K. Yoshida, I. Inoue; ANRIL is implicated in the regulation of nucleus and potential transcriptional target of E2F1; Oncol. Rep., 24 (2010), pp. 701–707
- Scandura et al., 2011 J.M. Scandura, G.J. Roboz, M. Moh, E. Morawa, F. Brenet, J.R. Bose, L. Villegas, U.S. Gergis, S.A. Mayer, C.M. Ippoliti, T.J. Curcio, E.K. Ritchie, E.J. Feldman; Phase 1 study of epigenetic priming with decitabine prior to standard induction chemotherapy for patients with AML; Blood, 118 (2011), pp. 1472–1480
- Scheffner et al., 1993 M. Scheffner, J.M. Huibregtse, R.D. Vierstra, P.M. Howley; The HPV-16 E6 and E6-AP complex functions as a ubiquitin-protein ligase in the ubiquitination of p53; Cell, 75 (1993), pp. 495–505
- Serrano et al., 1993 M. Serrano, G.J. Hannon, D. Beach; A new regulatory motif in cell-cycle control causing specific inhibition of cyclin D/CDK4; Nature, 366 (1993), pp. 704–707
- Siegel et al., 2015 R.L. Siegel, K.D. Miller, A. Jemal; Cancer statistics, 2015; CA Cancer J. Clin., 65 (2015), pp. 5–29
- Tallen and Riabowol, 2014 G. Tallen, K. Riabowol; Keep-ING balance: tumor suppression by epigenetic regulation; FEBS Lett., 588 (2014), pp. 2728–2742
- Tam et al., 2013 K.W. Tam, W. Zhang, J. Soh, V. Stastny, M. Chen, H. Sun, K. Thu, J.J. Rios, C. Yang, C.N. Marconett, S.A. Selamat, I.A. Laird-Offringa, A. Taguchi, S. Hanash, D. Shames, X. Ma, M.Q. zhang, W.L. Lam, A. Gazdar; CDKN2A/p16 inactivation mechanisms and their relationship to smoke exposure and molecular features in non-small-cell lung cancer; J. Thorac. Oncol., 8 (2013), pp. 1378–1388
- Valdez et al., 2015 B.C. Valdez, Y. Li, D. Murray, J. Ji, Y. Liu, U. Popat, R.E. Champlin, B.S. Andersson; Comparison of the cytotoxicity of cladribine and clofarabine when combined with fludarabine and busulfan in AML cells: enhancement of cytotoxicity with epigenetic modulators; Exp. Hematol., 43 (2015) (448-61 e2)
- Veganzones et al., 2015 S. Veganzones, M.L. Maestro, S. Rafael, V. De La Orden, M. Vidaurreta, B. Mediero, M. Espantaleon, J. Cerdan, E. Diaz-Rubio; Combined methylation of p16 and hMLH1 (CMETH2) discriminates a subpopulation with better prognosis in colorectal cancer patients with microsatellite instability tumors; Tumour Biol., 36 (2015), pp. 3853–3861
- Vidaurreta et al., 2008 M. Vidaurreta, M.L. Maestro, M.T. Sanz-Casla, C. Maestro, S. Rafael, S. Veganzones, J. Moreno, J. Blanco, A. Silmi, M. Arroyo; Inactivation of p16 by CpG hypermethylation in renal cell carcinoma; Urol. Oncol., 26 (2008), pp. 239–245
- Wang et al., 2012 W. Wang, K. Pan, Y. Chen, C. Huang, X. Zhang; The acetylation of transcription factor HBP1 by p300/CBP enhances p16INK4A expression; Nucleic Acids Res., 40 (2012), pp. 981–995
- Wang et al., 2014 H.L. Wang, P.Y. Zhou, P. Liu, Y. Zhang; Role of p16 gene promoter methylation in gastric carcinogenesis: a meta-analysis; Mol. Biol. Rep., 41 (2014), pp. 4481–4492
- Weinberg, 1995 R.A. Weinberg; The retinoblastoma protein and cell cycle control; Cell, 81 (1995), pp. 323–330
- Wilson et al., 2010 B.G. Wilson, X. Wang, X. Shen, E.S. Mckenna, M.E. Lemieux, Y.J. Cho, E.C. Koellhoffer, S.L. Pomeroy, S.H. Orkin, C.W. Roberts; Epigenetic antagonism between polycomb and SWI/SNF complexes during oncogenic transformation; Cancer Cell, 18 (2010), pp. 316–328
- Witcher and Emerson, 2009 M. Witcher, B.M. Emerson; Epigenetic silencing of the p16(INK4a) tumor suppressor is associated with loss of CTCF binding and a chromatin boundary; Mol. Cell, 34 (2009), pp. 271–284
- Wu et al., 2007 Y. Wu, X. Zhang, M. Salmon, Z.E. Zehner; The zinc finger repressor, ZBP-89, recruits histone deacetylase 1 to repress vimentin gene expression; Genes Cells, 12 (2007), pp. 905–918
- Wu et al., 2013 D.S. Wu, J.Z. Shen, A.F. Yu, H.Y. Fu, H.R. Zhou, S.F. Shen; Epigallocatechin-3-gallate and trichostatin A synergistically inhibit human lymphoma cell proliferation through epigenetic modification of p16INK4a; Oncol. Rep., 30 (2013), pp. 2969–2975
- Yang et al., 2002 L. Yang, L. Xia, D.Y. Wu, H. Wang, H.A. Chansky, W.H. Schubach, D.D. Hickstein, Y. Zhang; Molecular cloning of ESET, a novel histone H3-specific methyltransferase that interacts with ERG transcription factor; Oncogene, 21 (2002), pp. 148–152
- Yap et al., 2010 K.L. Yap, S. Li, A.M. Munoz-Cabello, S. Raguz, L. Zeng, S. Mujtaba, J. Gil, M.J. Walsh, M.M. Zhou; Molecular interplay of the noncoding RNA ANRIL and methylated histone H3 lysine 27 by polycomb CBX7 in transcriptional silencing of INK4a; Mol. Cell, 38 (2010), pp. 662–674
- Yoruker et al., 2012 E.E. Yoruker, U. Mert, D. Bugra, S. Yamaner, N. Dalay; Promoter and histone methylation and p16(INK4A) gene expression in colon cancer; Exp. Ther. Med., 4 (2012), pp. 865–870
- Zhang, 2013 Y. Zhang; Epidemiology of esophageal cancer; World J. Gastroenterol., 19 (2013), pp. 5598–5606
- Zhang and Tong, 2014 Y. Zhang, T. Tong; FOXA1 antagonizes EZH2-mediated CDKN2A repression in carcinogenesis; Biochem. Biophys. Res. Commun., 453 (2014), pp. 172–178
- Zhang et al., 2010 C.Z. Zhang, G.G. Chen, P.B. Lai; Transcription factor ZBP-89 in cancer growth and apoptosis; Biochim. Biophys. Acta, 1806 (2010), pp. 36–41
Document information
Published on 06/04/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?