Summary
Background
Laparoendoscopic single-site surgery (LESS) has emerged as a result of a search for “pain-less” and “scar-less” surgery. Laparoendoscopic single-site cholecystectomy (LESS-C) is probably the most common application in general surgery, although it harbors certain limitations. It was proposed that the da Vinci Single-Site (Si) robotic system may overcome some of the difficulties experienced during LESS, providing three dimensional views and the ability to work in a right-handed fashion. Thirty-six robotic single port cholecystectomies (R-LESS-C) performed with the da Vinci Si robotic system are evaluated in this paper
Materials and methods
R-LESS-C performed in 36 patients were reviewed. The data related to the perioperative period (i.e., anesthesia time, operation time, docking time, and console time) was recorded prospectively, whereas the hospitalization period, postoperative visual analogue scale (VAS) pain scores were collected retrospectively.
Results
A total number of 36 patients, with a mean age of 40.1 years (21–64 years), underwent R-LESS-C. There were five men and 31 women. The mean anesthesia and operation times were 79.3 minutes (45–130 minutes) and 61.8 minutes (34–110 minutes), respectively. The mean docking time was 9.8 minutes (4–30 minutes) and the mean console time was 24.9 minutes (7–60 minutes). The mean hospital stay was 1.05 days (1–2 days) and the mean pain score (VAS) was 3.6 (2–8) in the first 24 hours. Incisional hernia was recorded in one patient.
Conclusion
R-LESS-C can be performed reliably with acceptable operative times and safety. The da Vinci Si robotic system may ease LESS-C. Two issues should be considered for routine use: expensive resources are needed and the incidence of incisional hernia may increase.
Keywords
da Vinci Single-Site robotic system;laparoendoscopic single site cholecystectomy (LESS-C);laparoendoscopic single site surgery (LESS);robotic single port cholecystectomy (R-LESS-C)
1. Introduction
Laparoendoscopic procedures have been widely used since the 1980s and have become an intrinsic component of general surgery practice. The attempts to reduce the number and size of ports, with the assumption of less pain and less scar, contributed to the rise of laparoendoscopic single-site surgery (LESS).
LESS has been used in various procedures in general surgery, urology,1; 2 ; 3 gynecology,4 ; 5 and transplantation surgery.6 ; 7 Simple procedures like appendectomy8; 9 ; 10 and cholecystectomy11; 12; 13; 14; 15; 16 ; 17 have been performed with LESS, as well as more complicated ones, like antireflux surgery,18 right hemicolectomy,19 and total mesorectal resection.20
Laparoscopic cholecystectomy is one of the most common procedures in general surgery practice and has been accepted as the gold standard for the treatment of gallbladder stones. The first single incision laparoscopic cholecystectomy via the transumbilical approach was done by Navarra in 199721 and there has been an accelerated accrual of literature about this technique in recent years. Although promising results have been reported,11; 12 ; 15 a single port approach has significant limitations mainly associated with instrumentation and proper triangulation.17; 22; 23; 24; 25 ; 26 The problem mostly encountered is a difficulty in traction of the gallbladder and maintenance of the critical view. Crowding and conflict of the hand instruments may hinder fine dissection. The surgeon has to re-coordinate his eyes and hands to work in a cross handed fashion. The da Vinci Single-Site (Si) robotic system (Intuitive Surgical, Sunnyvale, CA, USA) has been developed and proposed to overcome these problems and to improve surgical outcome. To our knowledge, there are a few reports regarding the use of this system in small groups of patients.27; 28; 29 ; 30 In the present series, experiences in 36 patients who underwent robotic single port cholecystectomy (R-LESS-C) are discussed.
2. Materials and methods
Patients who were referred to the general surgery clinic for elective cholecystectomy and who wanted to undergo R-LESS-C, with their own consent, were accepted as candidates for robotic single port surgery. The exclusion criteria were: (1) acute cholecystitis, cholangitis, or common bile duct stones; (2) biliary pancreatitis; (3) cirrhosis; (4) bleeding disorders; (5) suspicious or proven malignancy; (6) American Society of Anesthesiologists (ASA) score > 2; (7) patients with a history of previous abdominal operation other than cesarean section; (8) patients who were mentally ill; (9) patients who were pregnant; and (10) patients who rejected R-LESS-C or signing the informed consent. All patients were informed about the innovative nature of this approach and no proven benefit of this approach was offered. Not all of the patients meeting the criteria above underwent R-LESS-C. The final decision was made at the discretion of the surgeon. All patients signed the informed consent for R-LESS-C prior to the operation.
The operative data, including anesthesia time, operation time, docking time, and console time, was collected prospectively. Anesthesia time was recorded from the induction of the anesthesia until the recovery of the patient from anesthesia. Operation time was recorded from incision to wound closure. The postoperative pain scores according to the visual analogue scale (VAS) were collected retrospectively from a computerized database system by an independent nurse at the time of the study. The study was approved by the Ethical Review Board of Acıbadem University.
2.1. Surgical procedure
Patients received general anesthesia and a single dose of prophylactic cephazolin sodium intravenously. Antithrombotic prophylaxis was not used in any of the patients.
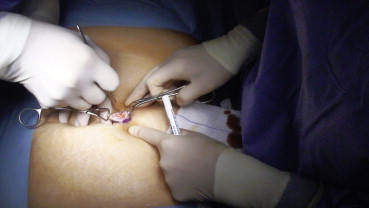
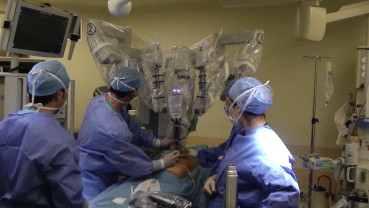
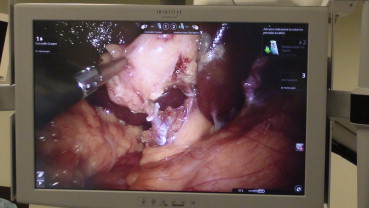
R-LESS-C was performed with the da Vinci Si System (Intuitive Surgical). The patient was placed in a supine position. A 2.5 cm incision through the umbilicus was made and dissection was carried down to the fascia (Fig. 1). Subcutaneous flaps were made without transection of the umbilical stalk. The peritoneal cavity was intruded under direct vision with an open technique. The da Vinci Single-Site Port (Intuitive Surgical) was placed and a pneumoperitoneum was produced with 13–15 mmHg intra-abdominal pressure. The patient was placed in a reverse Trendelenburg position with a 10–15° inclination and tilted to the left side. The robotic system was brought over the right shoulder of the patient (Fig. 2). After the introduction of the camera system, curved trocars were placed under direct vision and docking was done. After the docking procedure, the fundus of the gallbladder was retracted cephalad towards the patients right shoulder via the assistant instrument. No suture retraction technique was used for any patient. The surgeon started the operation at the console after a safe retraction and visualization of the Calots triangle. The cystic duct and cystic artery were dissected carefully and clipped, followed by bisection (Fig. 3).
|
|
|
Figure 1. Incision in the umbilicus for the port. |
|
|
|
Figure 2. Docking of the robotic system. |
|
|
|
Figure 3. Clipping of the cystic artery and the cystic duct. |
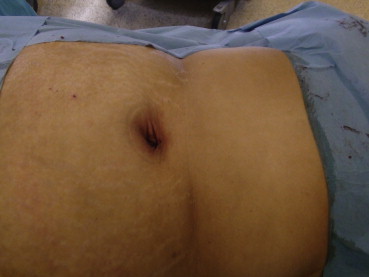
Cholecystectomy was performed in a retrograde fashion. After bleeding control, the specimen was removed through the umbilicus with the port. The fascial defect and the skin incision were closed with absorbable sutures (Fig. 4).
|
|
|
Figure 4. Closure of the single port incision. |
2.2. Postoperative care
Pain management was done with metamizole sodium routinely in all patients and nonsteroidal anti-inflammatory agents were ordered according to the patients demand. Narcotic analgesics were not used. Pain scores according to visual analogue scale (VAS) were recorded by the attending nurse in the computer-based system every 2 hours. The highest pain score that had been recorded was considered for the analysis of pain in this study.
3. Results
A total of 36 patients with a mean age of 40.1 years (21–64 years) underwent R-LESS-C. There were five men and 31 women. The mean anesthesia time was 79.3 minutes (45–130 minutes). The mean operative time was 61.8 minutes (34–110 minutes), the mean docking time was 9.8 minutes (4–30 minutes), and the mean console time was 24.9 minutes (7–60 minutes). The mean length of hospital stay was 1.05 days (1–2 days) and the mean pain score (VAS) was 3.6 (2–8). In three patients, the pain score (VAS) was 8; two of these patients stayed in hospital for 2 days because of mobilization difficulty. The major complaint in these patients was pain at the umbilical wound.
There were four events in 36 procedures. In one patient, desufflation of the abdominal cavity occurred after completion of cholecystectomy and bleeding control became troublesome. In another patient the clip-applier stuck, so that moving or removing the instrument became impossible. Technical support was needed to move the robotic instrument. In one patient, because of the hindrance of the anatomy and adhesions, an additional 5 mm trocar was placed. This incision was then used for non-suction draining. Docking was done twice in another patient because of difficulty in visualization of Calots triangle; the sum of the two docking procedures was 30 minutes. There were no conversions to conventional laparoscopic or open surgery. No major complications were recorded, such as bleeding, perforation of the gallbladder, injury of the common bile duct, or other organ injury. None of the patients needed perioperative or postoperative cholangiography or endoscopic retrograde cholangiopancreatography for retained bile duct stones. At follow-up, one patient developed an incisional hernia in the port site 7 months after R-LESS cholecystectomy. The patient underwent laparoscopic hernia repair.
4. Discussion
Despite the increased practice of laparoendoscopic single-site cholecystectomy (LESS-C) and accrual of the data, it is too early to proclaim LESS-C as the new gold standard in the management of gallstone disease. Although LESS-C has been reported to be safe and acceptable by several studies,11; 12 ; 15 there is still a significant concern with possible increased rates of complications, mainly bile duct injury.22; 27 ; 31 There is still an ongoing search for optimal instruments and optimal techniques, because of the limitations of the technique. The main issue in single port laparoscopic surgery is to restore the “critical view” for safe dissection with effective traction. Several techniques have been used for traction, such as suturing the bladder fundus with a Keith needle16 ; 32 or mini hook.25 ; 33 Flexible instruments and camera systems designed for single port surgery provide limited utility in overcoming this problem. There is conflict between the hand instruments that interfere with tissue manipulation and fine movements. The surgeon has to change his/her mindset to work in a cross handed manner, which leads to exhaustion. Additionally, the mentioned problems are likely to increase the operative time.
Robotic technology for single site surgery was designed to overcome these problems. The curved trocars of the robotic system were designed to diminish the triangulation problem and four access cannula in the trocar eliminates the need for percutaneous suture retraction.27 ; 29 The dexterity of the EndoWrist (working in a right handed fashion) eases the surgeons maneuvers and prevents the “sword fighting”; a three-dimensional high-definition view provides an additional advantage.
However, the da Vinci Si robotic system, as every new technology, has its own limitations: the robotic system is a considerable size, which limits the space in the operating room for the circulating staff, and the arms of the robot limit the access of the bedside assistant.27 ; 29 The insertion of long and curved trocars should be done under direct vision, in order to avoid unwanted intra-abdominal injury. The robotic instruments are semi-flexible and not articulated. The instruments have a limited range of motion in a limited surgical area. The system must be properly docked in order to establish the critical view in a small working field of not more than approximately 10 cm in three dimensions. In one patient in our series, the system was undocked and re-docked to provide the view for secure dissection.
The loss of tactile stimulation necessitates a certain experience to avoid undesirable tissue trauma. The movement of the arms of the robotic system can produce extensive traction in the umbilical wound, despite the port system. The unexpectedly higher pain scores in three patients in our series may be the result of excessive traction at the umbilical wound. Kroh et al27 reported partial tearing of the multichannel trocar in two patients, in addition to significant loss of pneumoperitoneum in three patients, which necessitated reinsertion of the trocar after undocking of the robot. This was attributed to reverse Trendelenburg positioning for patients with thicker abdominal walls. We did not experience any dislodgement of the four channel trocar in our series, but there were two events that should be noted. In one patient after completion of cholecystectomy, a significant loss of pneumoperitoneum occurred and bleeding control of the gallbladder bed could not be managed by robotic equipment. Hand instruments for single port laparoscopic cholecystectomy were used to control bleeding. In another patient, the robotic system stuck and it was impossible to move or remove the robotic instruments. Significant and professional technical support was needed to move the hand instrument. This increased the anesthesia and operation time. The surgery was accomplished successfully without any hazardous event.
Robotic single-site surgery necessitates special education of the operating team, attending nurse, circulating staff, and the anesthesiologist.
The cost of the R-LESS-C is not considered as a measure in the present study; however, it is obvious that the system is more expensive than conventional laparoscopy. The da Vinci Si platform costs an additional $150,000 over the robotic system. The robotic instruments cost $1330 for each cholecystectomy procedure. R-LESS-C requires higher expenses; it is thought that these could not compensate for hospitalization time or analgesic use.
There is no single port or conventional laparoscopic cholecystectomy arm in this study, but R-LESS-C requires greater operation and anesthesia times, although the console time is comparable with conventional laparoscopic surgery. The main reason for this is the longer preparation time of the patient by the anesthesiologist and the surgical team. The operation time in this series is comparable with previous reports.27; 28 ; 29 We are running a prospective randomized controlled trial that was approved by the Ethical Review Board of Acıbadem University, to compare R-LESS cholecystectomy with LESS cholecystectomy in our hospital.
We suggest that robotic single-site surgery is safe by means of complications in selected patients with uncomplicated gallbladder disease and can be performed in acceptable operation times, despite its own limitations.
In summary, the da Vinci Si robotic system meets expectations by means of preventing a conflict of instruments and establishing the “critical view”. The dexterity of the hand instruments and the three-dimensional view facilitate the fine movements of the surgeon. Further experience of both the surgeon and the operating team may help to decrease the operation time. The major disadvantages are the higher costs and significant increase in operating room resources, which prevent the justification for routine use. Suspicion regarding an increased risk of incisional hernias compared to conventional four port laparoscopic cholecystectomy persists, until long term follow up is achieved. Robotic technology may provide advantages in more complex abdominal procedures, with refinement of techniques and equipment. Further clinical trials in large series of patients are needed to confirm these potential advantages and evaluate the reproducibility.
References
- 1 L. Wang, B. Liu, Z. Wu, et al.; Comparison of single-surgeon series of transperitoneal laparoendoscopic single-site surgery and standard laparoscopic adrenalectomy; Urology, 79 (2012), pp. 577–583
- 2 J.E. Humphrey, D. Canes; Transumbilical laparoendoscopic single-site surgery in urology; Int J Urol, 19 (2012), pp. 416–428
- 3 F. Greco, D. Veneziano, S. Wagner, et al.; Laparoendoscopic single-site radical nephrectomy for renal cancer: technique and surgical outcomes; Eur Urol, 62 (2012), pp. 168–174
- 4 J.M. Wenger, J.B. Dubuisson, P. Dallenbach; Laparoendoscopic single-site supracervical hysterectomy with endocervical resection; J Minim Invasive Gynecol, 19 (2012), pp. 217–219
- 5 F. Fanfani, C. Rossitto, M.L. Gagliardi, et al.; Total laparoendoscopic single-site surgery (LESS) hysterectomy in low-risk early endometrial cancer: a pilot study; Surg Endosc, 26 (2012), pp. 41–46
- 6 H.J. Choi, Y.K. You, G.H. Na, et al.; Single-port laparoscopy assisted donor right hepatectomy in living donor liver transplantation: sensible approach or unnecessary hindrance?; Transplant Proc, 44 (2012), pp. 347–352
- 7 C. Afaneh, M.J. Aull, E. Gimenez, et al.; Comparison of laparoendoscopic single-site donor nephrectomy and conventional laparoscopic donor nephrectomy: donor and recipient outcomes; Urology, 78 (2011), pp. 1332–1337
- 8 S.D. St Peter, O.O. Adibe, D. Juang, et al.; Single incision versus standard 3-port laparoscopic appendectomy: a prospective randomized trial; Ann Surg, 254 (2011), pp. 586–590
- 9 R. Vilallonga, U. Barbaros, A. Nada, et al.; Single-port transumbilical laparoscopic appendectomy: a preliminary multicentric comparative study in 87 patients with acute appendicitis; Minim Invasive Surg (2012), p. 492409 https://doi.org/10.1155/2012/492409
- 10 E.M. Knott, A.C. Gasior, G.W. Holcomb 3rd, D.J. Ostlie, S.D. St Peter; Impact of body habitus on single-site laparoscopic appendectomy for nonperforated appendicitis: subset analysis from a prospective randomized trial; J Laparoendosc Adv Surg Tech A, 22 (2012), pp. 404–407
- 11 S.E. Hodgett, J.M. Hernandez, C.A. Morton, et al.; Laparoendoscopic single-site (LESS) cholecystectomy; J Gastrointest Surg, 13 (2009), pp. 188–192
- 12 O. Vidal, M. Valentini, J.J. Espert, et al.; Laparoendoscopic single-site cholecystectomy: a safe and reproducible alternative; J Laparoendosc Adv Surg Tech A, 19 (2009), pp. 599–602
- 13 S.R. Philipp, B.W. Miedema, K. Thaler; Single-incision laparoscopic cholecystectomy using conventional instruments: early experience in comparison with the gold standard; J Am Coll Surg, 209 (2009), pp. 632–637
- 14 J.K. Elsey, D.V. Feliciano; Initial experience with single incision laparoscopic cholecystectomy; J Am Coll Surg, 210 (2010), pp. 624–626
- 15 P.G. Curcillo II, Wu As, E.R. Podolsky, et al.; Single-port-access (SPA) cholecystectomy: a multi-institutional report of the first 297 cases; Surg Endosc, 24 (2010), pp. 1854–1860
- 16 S.K. Chang, C.W. Tay, R.A. Bicol, et al.; A case-control study of single-incision versus standard laparoscopic cholecystectomy; World J Surg, 35 (2011), pp. 289–293
- 17 H. Rivas, E. Varela, D. Scott; Single-incision laparoscopic cholecystectomy: initial evaluation of a large series of patients; Surg Endosc, 24 (2010), pp. 1403–1412
- 18 I. Hamzaoglu, T. Karahasanoglu, E. Aytac, A. Karatas, B. Baca; Transumbilical totally laparoscopic single-port Nissen fundoplication: a new method of liver retraction: the Istanbul technique; J Gastrointest Surg, 14 (2010), pp. 1035–1039
- 19 A.G. Chow, S. Purkayastha, E. Zacharakis, P. Paraskeva; Single-incision laparoscopic surgery for right hemicolectomy; Arch Surg, 146 (2011), pp. 183–186
- 20 I. Hamzaoglu, T. Karahasanoglu, B. Baca, et al.; Single-port laparoscopic sphincter-saving mesorectal excision for rectal cancer: report of the first 4 human cases; Arch Surg, 146 (2011), pp. 75–81
- 21 G. Navarra, E. Pozza, S. Occhionorelli, P. Carcoforo, I. Donini; One-wound laparoscopic cholecystectomy; Br J Surg, 84 (1997), p. 695
- 22 E.R. Podolsky, P.G. Curcillo II; Reduced-port surgery: preservation of the critical view in single-port-access cholecystectomy; Surg Endosc, 24 (2010), pp. 3038–3043
- 23 K.E. Roberts, D. Solomon, A.J. Duffy; Single-incision laparoscopic cholecystectomy: A surgeons initial experience with 56 consecutive cases and a review of the literature; J Gastrointest Surg, 14 (2010), pp. 506–510
- 24 J.R. Romanelli, T.B. Roshek, D.C. Lynn, et al.; Single-port laparoscopic cholecystectomy: initial experience; Surg Endosc, 24 (2010), pp. 1374–1379
- 25 Y. Hirano, T. Watanabe, T. Uchida, et al.; Single-incision laparoscopic cholecystectomy: single institution experience and literature review; World J Gastroenterol, 16 (2010), pp. 270–274
- 26 C. Edwards, A. Bradshaw, P. Ahearne, et al.; Single-incision laparoscopic cholecystectomy is feasible: initial experience with 80 cases; Surg Endosc, 24 (2010), pp. 2241–2247
- 27 M. Kroh, K. El-Hayek, S. Rosenblatt, et al.; First human surgery with a novel single-port robotic system: cholecystectomy using the da Vinci Single-Site platform; Surg Endosc, 25 (2011), pp. 3566–3573
- 28 S.M. Wren, M.J. Curet; Single-port robotic cholecystectomy: results from a first human use clinical study of the new da Vinci single-site surgical platform; Arch Surg, 146 (2011), pp. 1122–1127
- 29 P. Morel, M.E. Hagen, P. Bucher, et al.; Robotic single-port cholecystectomy using a new platform: initial clinical experience; J Gastrointest Surg, 15 (2011), pp. 2182–2186
- 30 A. Pietrabissa, F. Sbrana, L. Morelli, et al.; Overcoming the challenges of single-incision cholecystectomy with robotic single-site technology; Arch Surg, 147 (2012), pp. 709–714
- 31 A. Chiruvella, J.M. Sarmiento, J.F. Sweeney, et al.; Iatrogenic combined bile duct and right hepatic artery injury during single-incision laparoscopic cholecystectomy; JSLS, 14 (2010), pp. 268–271
- 32 A. Rawlings, S.E. Hodgett, B.D. Matthews, et al.; Single-incision laparoscopic cholecystectomy: initial experience with critical view of safety dissection and routine intraoperative cholangiography; J Am Coll Surg, 211 (2010), pp. 1–7
- 33 M. Ito, Y. Asano, A. Horiguchi, et al.; Cholecystectomy using single-incision laparoscopic surgery with a new SILS port; J Hepatobiliary Pancreat Sci, 17 (2010), pp. 688–691
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?