Summary
Background
Undescended testes is one of the most common congenital abnormalities in boys. In cases of impalpable testes, ultrasound is often used to find the testis, which frequently provides false-negative results. Recently, laparoscopy has become popular in the management of impalpable testes.
Methods
Retrospective study of all children with impalpable testes presenting for laparoscopy between August 2007 and July 2011 who had undergone ultrasound examinations without localizing the testes was conducted and the role of laparoscopy in diagnosing impalpable testes was evaluated.
Results
Twenty-three patients presented with impalpable testes for laparoscopy. All patients underwent ultrasound examinations in which the testes could not be identified. Of the 23 patients, Five patients were found to have palpable testes in the superficial inguinal pouch under anesthesia and proceeded to conventional open exploration during which the testes were brought into the scrotum. Eighteen patients were found to have impalpable testes in an evaluation under anesthesia (EUA) and proceeded to laparoscopy. Twelve patients were found to have intra-abdominal testes and underwent laparoscopic-assisted orchidopexy. Three patients underwent a two-stage Fowler-Stephens procedure, and two patients with “vanishing” testes with the vas and atrophic vessels entering a closed internal ring proceeded to open exploration and orchidectomy for atrophic testes. In addition, a teenager with atrophic testes underwent laparoscopic orchidectomy.
Conclusions
Laparoscopy is superior to ultrasound in the management of impalpable testes when high-resolution ultrasound is not available during the diagnostic process, with respect to both the sensitivity of localizing the testis and being more time and cost effective.
Keywords
undescended testis;impalpable testis;ultrasound;laparoscopy
1. Introduction
Undescended testes in boys is a very common congenital abnormality in which one or both testes do not reach the bottom of the scrotum prior to birth. The incidence of the condition is 3–5% among all boys at birth, and decreases to 0.8–1% after 6 months of age.1; 2; 3; 4; 5; 6; 7; 8; 9; 10; 11 ; 12 The classification of undescended testes includes suprascrotal, intracanalicular, intra-abdominal, and ectopic types,6 ; 13 whereas the classification of impalpable testes includes intra-abdominal, intracanalicular, vanishing testis, and agenesis testis types.14 The diagnostic tools used to detect undescended testes include physical examinations, radiologic examinations, hormonal examinations, and laparoscopic examinations.1; 4; 10; 15; 16; 17 ; 18 When the testes cannot be detected by physical examination, ultrasound is the most favored tool among the radiologic examinations because it is the least invasive procedure and does not scare children, whereas other radiologic examinations require anesthetic procedures and the associated risk of radiation. Ultrasound is also a fast and simple procedure to perform. Despite its advantages, ultrasound provides the lowest sensitivity results in localizing impalpable testes,2; 4; 6; 8; 18; 19 ; 20 unless high-resolution ultrasound is used, which achieves similar outcomes as computed tomography scans.1 ; 6 However, high-resolution ultrasound is not widely available in most centers in developing countries. The lack of equipment sometimes leads to misdiagnosis and misleads the parents into not taking further action and assuming that the testes had not formed.
Males with undescended testes have a lower sperm count, poorer quality sperm, and lower fertility rate, compared to males whose testicles descend normally; the rate of subfertility increases with bilateral involvement and increasing age at the time of orchidopexy.1 ; 4 Based on the results of testicular biopsies performed at the time of orchidopexy, the germ cell density decreases over time, beginning as early as 1 year of age.4 Fertility is directly related to the age at orchidopexy with a success rate as high as 87.5% if the surgery is performed before 2 years of age and as low as 14% if the surgery is performed at 13 years of age or older; however, these figures may be influenced by the distribution of unilateral and bilateral cases.2
Undescended testes are not a life-threatening disease. Therefore, most parents try to avoid any invasive procedures they believe are unnecessary. However, the long-term risk of testicular cancer has been well documented in males with a history of undescended testes, particularly if surgical correction is performed after 1 year of age.1; 2; 4; 6; 7; 8; 11 ; 12 Hence, making a correct diagnosis is essential to ensure that the patient receives proper treatment at the appropriate time to reduce the risk of testicular cancer.
Laparoscopy has become widely used to diagnose impalpable testes since 1976 when Cortesi et al15 initially described it. Using laparoscopy, the testes can be clearly identified and localized, and treatment can be administered immediately after making a diagnosis. Therefore, the risk of misdiagnosing agenesis testis in impalpable testes is reduced, which then reduces the risk of testicular cancer over the long term.
2. Patients and methods
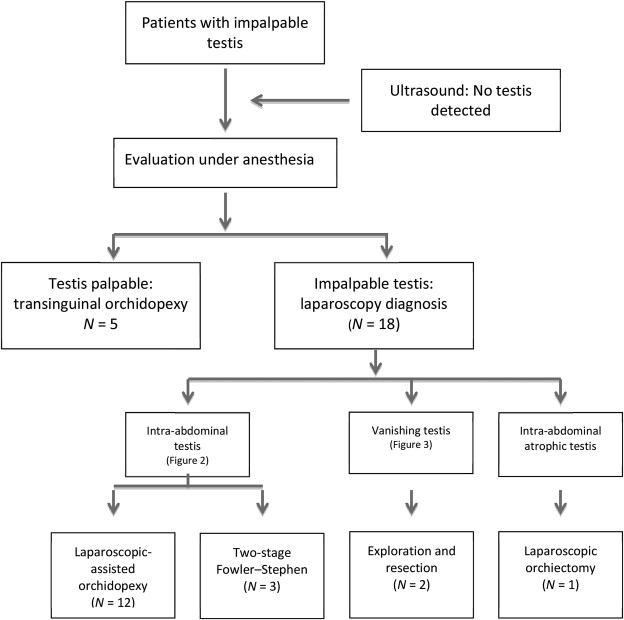
The diagnosis of impalpable testis in patients who were referred to Universiti Kebangsaan Malaysia (UKM) Hospital Pediatric Surgery Outpatient Clinic in Kuala Lumpur, Malaysia between August 2007 and July 2011 was confirmed by physical examinations (Fig. 1). Based on the UKM Clinical Pathway Guidelines, the patients were eligible for an evaluation under anesthesia and proceeded to open orchidopexy if the testes were palpable, or they underwent diagnostic laparoscopy and then proceeded to the appropriate surgery. If intra-abdominal testes were detected, the testes were evaluated with respect to whether they could be brought down into the scrotum without tension by bringing the testis to the contralateral side. If there was no tension, the procedure was continued with laparoscopic-assisted orchidopexy. If there was tension, the procedure was continued with the two-stage Fowler–Stephens technique.1 If remnants of the testes were present or if the vas deferens and vessels entered the inguinal canal, the procedure was continued with exploration and orchidectomy of the atrophic testis. If the testes were found to be atrophic intra-abdominally, a laparoscopic orchidectomy was performed.
|
|
|
Figure 1. Impalpable testis management algorithm used at Universiti Kebangsaan Malaysia Hospital (Kuala Lumpur, Malaysia) and the number of patients treated between August 2007 and December 2011. |
3. Results
Prior to being referred to the UKM Hospital Pediatric Surgery Outpatient Department, 23 patients with impalpable testes presented for laparoscopy after having undergone ultrasound. No testes were identified on ultrasound examinations. Five patients had palpable testes in the superficial inguinal pouch under anesthesia, and proceeded to conventional open exploration during which the testes were brought into the scrotum without tension. Eighteen (18/23) patients had impalpable testes in an evaluation under anesthesia (EUA) and proceeded to laparoscopy. Twelve patients had intra-abdominal testes and underwent laparoscopic-assisted orchidopexy (Fig. 2). Three patients underwent the two-stage Fowler–Stephens procedure. Two patients with vanishing testes with the vas deferens and atrophic vessels entering a closed internal ring proceeded to open exploration and orchidectomy for atrophic testes (Fig. 3). In addition, a teenager with atrophic testes underwent laparoscopic orchidectomy.
|
|
|
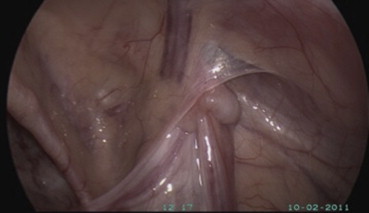
Figure 2. Intra-abdominal testis. The testis is located at the outer ring of the inguinal canal. |
|
|
|
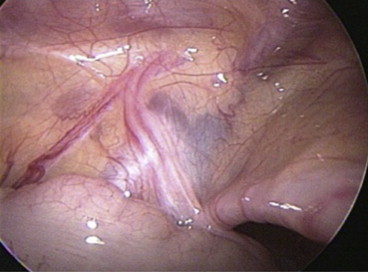
Figure 3. Vanishing testis. The vas deferens and vessels enter the inguinal canal. |
4. Discussion
Failure to locate the testes, interpreting this finding as indicating that no testes had formed, and diagnosing the patient with agenesis testis is a relief to some parents as this diagnosis has no operative risks and no cancer risks because of undescended testes, and saves money due to the lack of the need for surgery. However, should a misdiagnosis occur, and the testes actually exists somewhere in the abdomen, then the future risk of testicular cancer and infertility must be considered. Therefore, meticulous examinations using sensitive and detailed diagnostic tools should be conducted to detect the testes or remnants and to prevent the risk of testicular cancer in the future.
Ultrasound is an operator-dependent diagnostic tool that provides insensitive results, as many studies prove.4; 8; 18; 19 ; 20 High-resolution ultrasound offers similar sensitivity as computed tomography, although this modality is unavailable in most centers in developing countries. The experience of the ultrasound operator has an important role in the efficacy of the ultrasound examination. Magnetic resonance imaging is more sensitive than ultrasound and does not have the risk of radiation or require intravascular contrast injection; however, it has disadvantages such as a long scanning time and the presence of motion artifacts during the examination.20
Laparoscopy has become widely used to diagnose impalpable testes since 1976 when Cortesi et al15 first reported its use. Laparoscopy provides the ability to visualize directly the testes or remnants, detect agenesis of the testes, and evaluate the possibility of bringing the testes into the scrotum without tension. If no testes are present, tracking to the distal part of the vas deferens and the vascular area is possible using direct visualization with the laparoscopy camera to detect whether the testes are atrophic, contain remnants, or simply do not exist. Therefore, a diagnosis can be determined without hesitation.
If the testes are detected on ultrasound examination, the patient must be considered for surgery. The delay between diagnosis and surgery may allow the parents to change their minds regarding the operation, thereby increasing the patients risk of testicular cancer in the future. This is a common situation because the parents believe that there is no danger because the child appears healthy and is not in a life-threatening situation.
If the testes are not detected on ultrasound, the patient must undergo an evaluation under anesthesia to obtain greater relaxation of the muscles, thereby making palpation more effective.17 An evaluation under anesthesia is performed in an operating theater. Therefore, if the testes are palpable, open orchidopexy can be performed immediately. If the testes are not palpable, the laparoscopic diagnostic procedure is continued with the appropriate procedure, depending on the results obtained from the examination. For example, the patient may receive laparoscopic-assisted orchidopexy, laparoscopic orchidectomy, the Fowler–Stephens procedure, or exploration and excision of the remnants of the testes. The operation may be terminated because of findings of agenesis testis.
Whether surgery is performed, patients can be diagnosed in one stage using diagnostic laparoscopic procedures, which makes the procedure more time- and cost-effective. For these reasons, laparoscopy is superior to ultrasound.
This study showed that laparoscopy can be used to find testes that are not detected on ultrasound. It addresses the problems associated with impalpable testes in one stage. Our results support the findings of Elder19 who concluded: “ultrasonography is unnecessary in boys with a nonpalpable testis, because it rarely if ever localizes a true nonpalpable testis, and it does not alter the surgical approach in these patients.” In a 2011 review article, Tasian and Copp9 also concluded: “ultrasound does not reliably localize non-palpable testis and does not rule out an intra-abdominal testis. Eliminating the use of ultrasound will not change the management of non-palpable cryptorchidism but will decrease health care expenditures.”
With respect to the sensitivity of localizing the testis and being more time- and cost-effective, laparoscopy is superior to ultrasound in the management of impalpable testes when high-resolution ultrasound is unavailable during the diagnostic process.
References
- 1 M.J. Mathers, H. Sperling, H. Rubben, et al.; The undescended testis: diagnosis, treatment and long-term consequences; Dtsch Arztebl Intl, 106 (2009), pp. 527–532
- 2 A.E. MacKinnon; The undescended testis; Indian J Pediatr, 72 (2005), pp. 429–432
- 3 E.M. Ritzén; Undescended testes: a consensus on management; Eur J Endocrinol, 159 (suppl 1) (2008), pp. s87–s90
- 4 S.G. Docimo, R.I. Silver, W. Cromie; The undescended testicle: diagnosis and management; Am Fam Physician, 62 (2000), pp. 2037–2044
- 5 J.M. Hutson, S. Hasthorpe; Abnormalities of testicular descent; Cell Tissue Res, 322 (2005), pp. 155–158
- 6 H.T. Nguyen, F. Coakley, H. Hricak; Cryptorchidism: strategies in detection; Eur Radiol, 9 (1999), pp. 336–343
- 7 C. Foresta, D. Zuccarello, A. Garolla, et al.; Role of hormones, genes, and environment in human cryptorchidism; Endocr Rev, 29 (2008), pp. 560–580
- 8 D. Nugroho, I. Wahyudi, A. Rodjani; Profil pasien undescensus testis di rumah sakit cipto mangunkusumo Jakarta periode 2002–2010; J Indon Med Assoc, 62 (2012), pp. 51–552 [Article in Indonesian]
- 9 G.E. Tasian, H.L. Copp; Diagnosis performance of ultrasound in nonpalpable cryptorchidism: a systematic review and meta-analysis; Pediatrics, 127 (2011), pp. 119–128
- 10 L.A. Baker, S.G. Docimo, I. Surer, et al.; A multi-institutional analysis of laparoscopic orchidopexy; BJU Int, 87 (2001), pp. 484–489
- 11 A. Petterson, L. Richiardi, A. Nordenskjold, et al.; Age at surgery for undescended testis and risk of testicular cancer; N Engl J Med, 356 (2007), pp. 1835–1841
- 12 P.J. Kokorowski, J.C. Routh, D.A. Graham, et al.; Variations in timing of surgery among boys who underwent orchidopexy for cryptorchidism; Pediatrics, 126 (2010), pp. e576–e582
- 13 W.W. Hack, R.W. Meijer, S.D. Bos, et al.; A new clinical classification for undescended testis; Scand J Urol Nephrol, 37 (2003), pp. 43–47
- 14 R.G. Moore, C.A. Peters, S.B. Bauer, et al.; Laparoscopic evaluation of the nonpalpable testis—a prospective assessment of accuracy; J Urol, 151 (1994), pp. 728–731
- 15 N. Cortesi, P. Ferrari, E. Zambarda, et al.; Diagnosis of bilateral abdominal cryptorchidism by laparoscopy; Endoscopy, 8 (1976), pp. 33–34
- 16 J.E.S. Scott; Laparoscopy as an aid in the diagnosis and management of the impalpable testis; J Pediatr Surg, 17 (1982), pp. 14–16
- 17 K.K. Patil, J.S.A. Green, P.G. Duffy; Laparoscopy for impalpable testis; BJU Int, 95 (2005), pp. 704–708
- 18 J.M. Gatti, D.J. Ostlie; The use of laparoscopy in the management of nonpalpable undescended testis; Curr Opin Pediatr, 19 (2007), pp. 349–353
- 19 J.S. Elder; Ultrasonography is unnecessary in evaluating boys with a nonpalpable testis; Pediatrics, 110 (2002), pp. 748–751
- 20 K. Kanemoto, Y. Hayashi, Y. Kojima, et al.; Accuracy of ultrasonography and magnetic resonance imaging in the diagnosis of non-palpable testis; Int J Urol, 12 (2005), pp. 668–672
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?