Summary
Objective
The aim of this study was to compare the surgical outcome of fasciocutaneous V–Y advancement flap and limberg transposition flap used to treat recurrent sacrococcygeal PSD.
Methods
A total of 58 patients with recurrent pilonidal sinus who underwent surgery were evaluated retrospectively between January 2008 to December 2013. Fasciocutaneous V–Y advancement flap was performed in 25 patients (Group VYF), and limberg transposition flap repair was performed in 33 patients (Group LTF). Patient demographics, operative and postoperative outcomes were recorded then retrospectively analyzed.
Results
The mean age (p = 0.69), sex ratio (p = 0.48), and concomitant diseases (p = 0.98) were not statistically different when compared the VYF with LTF groups. Mean operative time was 55 ± 19 min for the LTF group and 75 ± 25 min for the VYF group (p = 0.01). When length of hospital stay were compared, there was a significant difference between the groups (p = 0.01). Return to work was carryed out after a mean of 23 ± 1.1 days in VYF group and 16.7 ± 1.2 days in LTF group, which is significantly different (p < 0.0004). Between the groups, there was no significantly different regarding surgical complication and recurrent rate. Only one recurrence (4%) was found in VYF group.
Conclusion
Limberg transposition flap may be use in recurrent cases of PSD, because of the lower recurrence rate and less hospital stay time, early return to work. Most important advantage of fasciocutaneous V–Y advancement flap is the ability to close larger defects in recurrent cases.
Keywords
fasciocutaneous V–Y advancement flap;limberg transposition flap;recurrent sacrococcygeal pilonidal sinus disease
1. Introduction
Sacrococcygeal pilonidal sinus disease (PSD) is a common chronic inflammation of the natal cleft and is mainly seen in young adults.1 Authors of some earlier works regarded the condition as congenital.2 Recently, it has become widely accepted that the condition is acquired,1 and thought to originate from hair follicles.3
Although many surgical procedures have been tried, the best surgical method remains controversial because of high recurrence rates. The recurrence rate after a surgical treatment of complex PSD varies from 3% to 46%.4 The procedure should treat the patients with short hospital stay, and allow early return to normal activities by reducing pain and discomfort. With flap surgery, the resulting defective area after wide excision is filled with fasciocutaneous tissue, and its superiority to primary closure has been reported in many papers.5; 6 ; 7 Recently, fasciocutaneous V–Y advancement flap (VYF) and Limberg transposition flap (LTF) are the most popular treatment alternatives.8 ; 9 In our center, the VYF and LTF have been used to reconstruct the defect following the radical excision of recurrent pilonidal sinus in more than 95% of patients.
This retrospective study was designed to compare the surgical outcome of VYF and LTF used to treat recurrent PSD.
2. Method
2.1. Patients
From January 2008 to December 2013, 64 patients underwent flap surgery for recurrent PSD in the Department of General Surgery at Erciyes University School of Medicine. The data were collected after receiving the approval of the ethics committee. A statement of informed consent was obtained from all patients before the operation. The patients who had incomplete records (n = 3) and concurrent abscess formation (n = 3) were excluded from the study. The remaining 58 PSD patients who underwent flap surgery comprised the study group and were evaluated retrospectively. Fasciocutaneous VYF was performed in 25 patients (group VYF), and LTF repair was performed in 33 patients (group LTF).
The biochemical and hematological study results at admission, time from onset of symptoms to presentation, number of previous surgical intervention, and outcomes, including morbidity, length of hospital stay, and recurrence, were all recorded.
The data including age, gender, body mass index, operative time, hospital stay, and intraoperative and postoperative results were analyzed retrospectively, and were compared between the groups.
2.2. Diagnosis
The diagnosis of recurrent PSD was made based on clinical features. All specimens were evaluated using routine pathological tests.
2.3. Preoperative preparation
Hair of the gluteal and sacral regions was shaved before the operation. Preoperative bowel preparation was not used. In all cases, prophylactic antibiotics were used at the time of induction of anesthesia. Patients with purulent discharge and with acute pilonidal abscess were not operated on immediately. These patients were treated by drainage and antibiotics. Definitive surgical procedure was performed on these patients after healing of the acute infection and inflammation. When the defect volume is bigger or with the presence of paramedian sinus localization, the surgeons principally considered the technique of VYF in the treatment of recurrent PSD. LTF was considered principally in the case of smaller defect volume or median sinus localization.
2.4. Surgery
The patients were operated on under general (n = 42) or spinal (n = 16) anesthesia, and placed in the prone jackknife position. The buttocks were laterally retracted with adhesive tapes. The sacrococcygeal area was washed with 10% povidone-iodine solution. The extension of the sinus was determined by methylene-blue injection into the sinus tract. The sinus localization was defined as median or paramedian, and recorded. Excision of all sinus tracts, fistula borders, and scar tissues was carried out deep to the postsacral fascia and surrounding undamaged fibrolipomatous tissues. The postsacral defect was then filled with saline until the fluid overflowed. The volume of the remaining saline in the defect cavity was again measured by a syringe, and defined as the defect volume.
In the VYF group, the defect was closed by a unilateral or bilateral VYF, as described previously by Papp et al.10 In group LTF, after removing the specimen, the Limberg fasciocutaneous flap was prepared by extending the incision down to and through the right or left gluteus maximus fascia.11
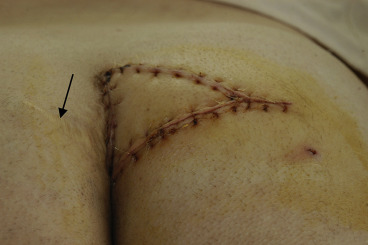
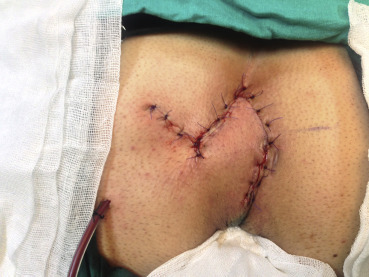
In both groups, the wound was closed in two layers, and approximation of the fascial layer and subcutaneous tissues was performed with polyglycolic-acid sutures. The skin was closed with interrupted nonabsorbable monofilament sutures or steel skin staplers (Figure 1 ; Figure 2). Suction drains were applied in all patients.
|
|
|
Figure 1. Fasciocutaneous V–Y advancement flap. |
|
|
|
Figure 2. Limberg transposition flap. |
2.5. Follow-up
All patients were released for mobilization on the 2nd postoperative day. The suction drains were removed when a daily drainage below 20 mL was obtained. In general, the patients were discharged on the 3rd or 4th postoperative day. The sutures were removed on the 10th postoperative day. The patients were advised to avoid pressure on the operated site for 10–15 days postoperatively. All cases were examined twice during the first 2 weeks, and once at the end of 1, 3, and 6 months after the operation, and yearly thereafter.
2.6. Statistical analysis
Differences among the groups were compared using Chi-square tests and Mann–Whitney U tests. The data were analyzed with the SPSS software package (version 13.0; SPSS, Inc., Chicago, IL, USA). The significance was set at p < 0.05.
3. Results
The surgical procedures and patient demographics are shown in Table 1. The mean age (p = 0.69), gender ratio (p = 0.48), and body mass index (p = 0.1) of the patients were not statistically different between the LTF and VYF groups. Concomitant disease was more frequent in the LTF group (28%), but this difference was not statistically significant when compared to the VYF group (24.2%) (p = 0.98). Twenty-nine patients were treated previously by simple excision with primary closure, while seventeen underwent the Karydakis technique, six patients the rhomboid-flap technique, four patients the VYF, and the remaining two the open method (wide excision and healed by secondary intention). Thirty-seven patients presented with their first recurrence, eighteen patients with their second recurrence, and three patients with their third recurrence.
| Group VYF (n = 25) | Group LTF (n = 33) | p | |
|---|---|---|---|
| Age (y) | 29.3 ± 9.3 (17–46) | 31.9 ± 8.9 (19–48) | 0.69a |
| Gender ratio (male/female) | 21/4 (84/16)% | 24/9 (73/27)% | 0.48 |
| Body mass index | 26.6 ± 0.7 | 25 ± 0.6 | 0.1 |
| Concomitant disease | 0.98 | ||
| Cardiac | 2 (8%) | 3 (9%) | |
| Respiratory | 3 (12%) | 3 (9%) | |
| Diabetes mellitus | 2 (8%) | 2 (6%) |
Values are mean ± standard deviation (range) and n (%).
LTF = Limberg transposition flap; VYF = fasciocutaneous V–Y advancement flap.
a. Mann–Whitney U test.
The duration of the presenting disease varied from 8 months to 6 years after the previous operation, but we did not find a significant relationship between the duration of symptoms and the type of surgical procedure required (p > 0.05). The most common complaints were spontaneous purulent discharge and sacrococcygeal pain after a physical activity, or a period of prolonged sitting and swelling in the two groups (88%). The most common physical-examination findings were holes in the natal cleft with purulent discharge (100%).
The operative and postoperative outcomes are summarized in Table 2. The mean operative time was 55 minutes ± 19 minutes (range, 40–90 minutes) in the LTF group, and 75 minutes ± 25 minutes (range, 55–105 minutes) in the VYF group (p = 0.01). In the VYF group, bilateral V–Y plasty was performed in 19 patients, and unilateral V–Y plasty in 14 patients. The operation time was not statistically different in the unilateral V–Y plasty and LTF groups (p = 0.24). The defect volume was 22 mL ± 1.3 mL in the LTF group, and 30.6 mL ± 1.5 mL in the VYF group (p < 0.0001). The rate of paramedian sinus localization was more frequent in the VYF group than in the LTF group [18/25 (72%) vs. 10/33 (30.3%)]. The most frequent postoperative medical complications were urinary retention (12.1%) and atelectasis (6.9%). In the LTF group, eight surgical complications occurred in seven (28.0%) patients, and in the VYF group, 13 complications occurred in 11 (33.3%) patients. When compared, the complication rates were not significantly different (p = 0.76; Table 2). The most frequent surgical complication was maceration. All the macerations were detected on the lower part of the incision left on the intergluteal sulcus. Wound infections and partial wound dehiscences appeared subsequent the maceration. The seroma rates in the LTF and VYF groups were 8.0% (two patients) and 9.0% (three patients), respectively. These patients were treated by aspiration without opening the wound. The patients with partial wound dehiscence were treated with local wound care, and improved in a month. Return to work was carried out after a mean of 23 days ± 1.1 days in the VYF group, and 16.7 days ± 1.2 days in the LTF group, which are significantly different (p < 0.0004).
| Group VYF (n = 25) | Group LTF (n = 33) | p | |
|---|---|---|---|
| Operative time (min) | 75 ± 25 (55–105) | 55 ± 19 (40–90) | 0.01 |
| Medical complications | 1.00 | ||
| Dysrhythmia | 1 (4%) | 0 (0) | |
| Atelectasis | 2 (8%) | 2 (6%) | |
| Urinary retention | 3 (12%) | 4 (12%) | |
| Surgical complications | 0.76 | ||
| Wound infection | 2 (8%) | 1 (3%) | 0.57 |
| Maceration | 2 (8%) | 4 (12%) | 0.68 |
| Seroma | 2 (8%) | 3 (9%) | 1.00 |
| Minimal flap-tip necrosis | 1 (4%) | 3 (9%) | 0.62 |
| Partial wound dehiscence | 1 (4%) | 2 (6%) | 1.00 |
| Sinus localization Median & paramedian | 7 & 18 | 23 & 10 | 0.001 |
| Defect volume (mL) | 30.6 ± 1.5 (20–45) | 22 ± 1.3 (15–40) | <0.0001 |
| Amount of drainage (mL) | 25 (15–45) | 30 (15–50) | 0.54 |
| Time for drain removal (d) | 2 (1–3) | 2 (1–4) | 1.00 |
| Duration of hospital stay (d) | 5.8 ± 0.9 (4–11) | 4.3 ± 0.8 (3–7) | 0.01 |
| Duration of follow-up (mo) | 26 (6–44) | 28 (6–50) | 0.52 |
| Recurrence | 1 (4%) | 0 (0%) | 0.43 |
| Return to work (d) | 23 ± 1.1 | 16.7 ± 1.2 | 0.0004 |
Values are mean ± standard deviation (range) and median (range), or n (%).
LTF = Limberg transposition flap; VYF = fasciocutaneous V–Y advancement flap.
The amounts of drainage observed in the patients in the LTF and VYF groups were not statistically different. Drains were removed on the 1st–4th (median: 2) postoperative days. The mean durations of hospital stay were 4.3 days and 5.8 days in the LTF and VYF groups, respectively. The follow-up ranged from 12 months to 50 months. During the follow-up period, only one recurrence (4%) was found in VYF group. There was no recurrence in LTF groups. Again, Fasciocutaneous V−Y advancement flap was used to treat recurrent one patient.
4. Discussion
Our results show that either VYF or LTF is a good treatment option for recurrent PSD, because of the great surgical outcomes. We think that LTF can be used in both primary and secondary cases of complicated PSD, with a lower recurrence rate and less hospital stay time.
Many treatment methods have been proposed, but no one method has been widely accepted yet. The ideal operation for PSD should cause minimal pain, shorten hospital stay, allow a speedy resumption of normal activities, and has a low recurrence rate.12
The surgical treatment of PSD involves excision and primary closure, excision and lay open, marsupialization, and excision and flap closure. Because of the high recurrence rates due to continuing natal cleft with both excision and primary closure or lay open, a considerable controversy exists about the optimal treatment.12; 13; 14 ; 15 Similarly, half of our eligible patients with recurrent PSD were previously treated by simple excision with primary closure.
The use of VYF and LTF has received growing attention in the surgical treatment of primary and recurrent PSD.6; 7; 8; 9; 16; 17 ; 18 Unilaterally or bilaterally, VYF may be used for closure of defects after excision of wide or recurring PSD.7 ; 18 Fasciocutaneous VYFs need less dissection and mobilization, and naturally lower seroma incidence when compared with LTF.19 Other advantages of VYF are tension-free closure, rapid and nonproblematic wound healing, less postoperative pain, and total obliteration of dead spaces. This technique results in a prolonged hospital stay and requires a longer operating time.20 In our study, the operating time and hospital stay were longer in VYF than in LTF. LTF is associated with wound infection, seroma, wound separation, flap necrosis, and recurrence rates of 0.8–7.6%, 1.5–5.2%, 0–4.1%, 0–3%, and 1.2–4.9%, respectively, in the literature. Our results were consistent with previous reports.5; 6; 13; 21 ; 22
In the literature, the rates of wound infection, seroma, and wound separation after VYF were reported to be 0–10.2%, 0–4.6%, and 0–10.2%, respectively.7; 20 ; 23 Our VYF results correlate well with previous reports. In our patients, the most frequent surgical complications were maceration, seroma, and minimal necrosis in the VYF group, and maceration, seroma, and wound infection in the LTF group. Although we routinely used suction drains, the seroma rates in the VYF group were 9.0% (three patients), and in the LTF group were 8.0% (two patients). In all five patients, suction drain was removed on the 1st postoperative day for early discharge from the hospital. They were treated by aspiration without opening the wound, and stayed a long time in the hospital (median: 9 days in the VYF group, 7 days in the LTF group). We believe that suction drains are necessary with both VYF and LTF treatments, especially in obese patients and wide dissection areas, and drains should not be removed during the early postoperative period. Conversely, Mentes et al24 suggested that closed suction drain is not necessary after the Limberg flap operation. Maceration was the most frequent complication in both groups. Wound infections and wound dehiscences were other frequent complications. LTF repairs not only flatten the natal cleft, but also displace the incision scar from the midline. Therefore, skin maceration and debris accumulation are eliminated.25 The prevention of maceration may be important for the development of other complications and recurrences. In the VYF group, the patients with minimal flap-tip necrosis were treated with debridement and local wound care, and improved in a short time period. In the LTF group, flap-tip necrosis was determined in only one patient. According to this technique, tissues can become near without tension, which reduces wound dehiscence and postoperative pain, and provides early return to work and a shorter hospital stay with low recurrence rate, as shown in another study as well as in ours.19
Recurrence rate is the most important criterion in determining the success of a surgical technique in a localized disease. Lee et al26 suggested primary closure be used in the treatment of the primary disease, but the recurrences should be treated by flap reconstruction. Lieto et al27 used sinus excision with the flap-reconstruction technique in a study of 55 patients with recurrent disease, only one patient (1.8%) demonstrated recurrence. El-Khadrawy et al18 used sinus excision with the rhomboid-transposition-flap technique in a study of 60 patients with recurrent disease, six patients (1.8%) demonstrated recurrence. In the present study, recurrence was not observed in the LTF group. Recently, Demiryilmaz et al17 operated on 45 patients with primary and recurrent pilonidal sinus, with a median follow-up time of 25 months, and recurrence was not found. Unalp et al28 compared the LTF with the VYF, and found that there were no significant differences in terms of complications between the two techniques. They suggested that, if the defect is to be reconstructed with a flap in patients with PSD, reconstruction with Limberg flap should be preferred over reconstruction with V–Y flap by virtue of its lower rate of recurrence. We often performed VYF in patients treated for recurrent PSD, especially those with a larger volume defect and paramedian sinus localization, and LTF in cases of smaller volume defect and median sinus localization in our clinic during the study period. The operative results and recurrence rates were similar between the groups. Therefore, we suggest VYF may be a better alternative for closure of defects after a wide excision if the defect is bigger, or with the presence of paramedian sinus localization in the treatment of PSD, as suggested in a previous report.8 In the literature, the rates of recurrence after VYF were reported to be 0–11.1%, which is comparable to our study findings.19; 24; 28 ; 29
The main limitation of our study was its retrospective nature. Another limitation of our study was the lack of additional parameters, such as pain scores and degree of patient satisfaction.
We believe that either VYF or LTF is a good alternative for the treatment of recurrent PSD, because of the excellent surgical outcomes. LTF can be used in both primary and secondary cases of complicated PSD, because of the lower recurrence rate and reduced hospital stay time, and so earlier return to work. Despite the risk of flap-tip necrosis and longer operative and hospital stay time, VYF has advantages, like ability to close larger defects in recurrent cases. Our findings are based on a retrospective study; in the future, a randomized controlled trial should be conducted to compare the surgical outcome of VYF and LTF procedures for recurrent PSD.
References
- 1 T.G. Allen-Mersh; Pilonidal sinus: finding the right tract for treatment; Br J Surg, 77 (1990), pp. 123–132
- 2 J.W. Chamberlain, G.F. Vawter; The congenital origin of pilonidal sinus; J Pediatr Surg, 9 (1974), pp. 441–444
- 3 J.U. Bascom; Pilonidal disease: long-term results of follicle removal; Dis Colon Rectum, 23 (1983), pp. 800–807
- 4 A. Shafik; Electrocauterization in the treatment of pilonidal sinus; Int Surg, 81 (1996), pp. 83–84
- 5 C. Daphan, M.H. Tekelioglu, C. Sayilgan; Limberg flap repair for pilonidal sinus disease; Dis Colon Rectum, 47 (2004), pp. 233–237
- 6 B.B. Mentes, S. Leventoglu, A. Cihan, E. Tatlicioglu, M. Akin, M. Oguz; Modified Limberg transposition flap for sacrococcygeal pilonidal sinus; Surg Today, 34 (2004), pp. 419–423
- 7 T. Schoeller, G. Wechselberger, A. Otto, C. Papp; Definite surgical treatment of complicated recurrent pilonidal disease with a modified fasciocutaneous V-Y advancement flap; Surgery, 121 (1997), pp. 258–263
- 8 H. Berkem, S. Topaloglu, H. Ozel, F.M. Avsar, Y. Yildiz, B.C. Yuksel; V-Y advancement flap closures for complicated pilonidal sinus disease; Int J Colorectal Dis, 20 (2005), pp. 343–348
- 9 K. Topgul, E. Ozdemir, K. Kilic, H. Gökbayir, Z. Ferahköşe; Long-term results of Limberg flap procedure for treatment of pilonidal sinus; Dis Colon Rectum, 46 (2003), pp. 1545–1548
- 10 C.H. Papp, E. Zanon, K. Hasenöhrl; Der fasciocutane VY-lappen zur deckung von decubitalulcera; Der Chirurg, 59 (1988), pp. 287–290
- 11 A.S. Azab, M.S. Kamal, R.A. Saad, K.A. Abou al Atta, N.A. Ali; Radical cure of pilonidal sinus by transposition rhomboid flap; Br J Surg, 71 (1984), pp. 154–155
- 12 D. Doll, E. Matevossian, K. Wietelmann, T. Evers, M. Kriner, S. Petersen; Family history of pilonidal sinus predisposes to earlier onset of disease and a 50% long-term recurrence rate; Dis Colon Rectum, 52 (2009), pp. 1610–1615
- 13 O.F. Akinci, A. Coskun, A. Uzunköy; Simple and effective surgical treatment of pilonidal sinus: asymmetric excision and primary closure using suction drain and subcuticular skin closure; Dis Colon Rectum, 43 (2000), pp. 701–706 discussion 706–707
- 14 C. Soll, D. Hahnloser, D. Dindo, P.A. Clavien, F. Hetzer; A novel approach for treatment of sacrococcygeal pilonidal sinus: less is more; Int J Colorectal Dis, 23 (2008), pp. 177–180
- 15 M. Kement, M. Oncel, N. Kurt, L. Kaptanoglu; Sinus excision for the treatment of limited chronic pilonidal disease: results after a medium-term follow-up; Dis Colon Rectum, 49 (2006), pp. 1758–1762
- 16 J. Bascom; Skin flaps for pilonidal disease; Ann Plast Surg, 41 (1998), p. 338
- 17 I. Demiryilmaz, I. Yilmaz, K. Peker, et al.; Application of fasciocutaneous V-Y advancement flap in primary and recurrent sacrococcygeal pilonidal sinus disease; Med Sci Monit, 20 (2014), pp. 1263–1266
- 18 O. el-Khadrawy, M. Hashish, K. Ismail, H. Shalaby; Outcome of the rhomboid flap for recurrent pilonidal disease; World J Surg, 33 (2009), pp. 1064–1068
- 19 F. Altintoprak, E. Dikicier, Y. Arslan, T. Ozkececi, G. Akbulut, O.N. Dilek; Comparision of the Limberg flap with the V-Y flap technique in the treatment of pilonidal disease; J Korean Surg Soc, 85 (2013), pp. 63–67
- 20 G. Milito, F. Cortese, C.U. Casciani; Rhomboid flap procedure for pilonidal sinus: results from 67 cases; Int J Colorectal Dis, 13 (1998), pp. 113–117
- 21 K. Topgül, E. Ozdemir, K. Kilic, H. Gökbayir, Z. Ferahköşe; Long-term results of Limberg procedure for treatment of pilonidal sinus: a report of 200 cases; Dis Colon Rectum, 46 (2003), pp. 1545–1548
- 22 M.Z. Sabuncuoglu, A. Sabuncuoglu, O. Dandin, et al.; Eyedrop-shaped, modified Limberg transposition flap in the treatment of pilonidal sinus disease; Asian J Surg, 38 (2015), pp. 161–167
- 23 T.Z. Nursal, A. Ezer, K. Calişkan, N. Törer, S. Belli, G. Moray; Prospective randomized suture controlled trial comparing V-Y advancement flap with primary methods in pilonidal disease; Am J Surg, 199 (2010), pp. 170–177
- 24 O. Mentes, M. Bagci, T. Bilgin, O. Ozgul, M. Ozdemir; Limberg flap procedure for pilonidal sinus disease: results of 353 patients; Langenbecks Arch Surg, 393 (2008), pp. 185–189
- 25 R. Eryilmaz, M. Sahin, O. Alimoglu, F. Dasiran; Surgical treatment of sacrococcygeal pilonidal sinus with the Limberg transposition flap; Surgery, 134 (2003), pp. 745–749
- 26 P.J. Lee, S. Raniga, D.K. Biyani, A.J. Watson, I.G. Faragher, F.A. Frizelle; Sacrococcygeal pilonidal disease; Colorectal Dis, 10 (2008), pp. 639–650
- 27 E. Lieto, P. Castellano, M. Pinto, A. Zamboli, C. Pignatelli, G. Galizia; Dufourmentel rhomboid flap in the radical treatment of primary and recurrent sacrococcygeal pilonidal disease; Dis Colon Rectum, 53 (2010), pp. 1061–1068
- 28 H.R. Unalp, H. Derici, E. Kamer, O. Nazli, M.A. Onal; Lower recurrence rate for Limberg vs. V-Y flap for pilonidal sinus; Dis Colon Rectum, 50 (2007), pp. 1436–1444
- 29 O.N. Dylek, M. Bekereciodlu; Role of simple V-Y advancement flap in the treatment of complicated pilonidal sinus; Eur J Surg, 164 (1998), pp. 961–964
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?