Abstract
Background
Transradial artery (TRA) left heart catheterization is an increasingly used technique for both diagnostic and interventional coronary procedures. This study evaluates the incidence of access site complications in the current interventional era.
Methods and results
A total of 507 procedures were performed under standardized conditions. Each procedure was performed using high levels of anticoagulation, hydrophilic sheaths, and short post-procedural compression times. Vascular complications were assessed one day after TRA catheterization using Duplex sonography and classified according to the necessity of additional medical intervention. A simple questionnaire helped identifying upper extremity neurologic or motor complications. Vascular complications were detected in 12 patients (2.36%): radial artery occlusion was detected in 9 patients (1.77%), 1 patient developed an AV-fistula (0.19%), and 2 patients had pseudoaneurysms (0.38%). None of the patients required specialized medical or surgical intervention. Under our procedural conditions, small radial artery diameter was the only significant predictor for the development of post-procedural vascular complications (2.11 ± 0.42 mm vs 2.52 ± 0.39 mm, p = 0.001). None of the previously reported risk factors, namely, advanced renal failure, diabetes, acuteness/complexity of procedure, or sheath and catheter size significantly influenced the rate of vascular complications. No major hematoma or local neurologic or motor complications were identified.
Conclusions
Using current techniques and materials, we report a very low rate of local complications associated with TRA catheterization.
Keywords
Coronary angiography;Transradial catheterization;Radial artery occlusion;Access site complications
1. Introduction
Transradial artery (TRA) left heart catheterization is an increasingly used technique for both diagnostic and interventional coronary procedures due to a low incidence of major access site related complications (e.g. bleeding) [1]; [2]; [3] ; [4]. Additional advantages of TRA catheterization include improved patient comfort and early ambulation, which may shorten the length of hospital stay and reduce healthcare costs [1] ; [4]. However, complications due to TRA cardiac catheterization have been reported and are related to the small diameter of the radial artery, the tendency of the radial artery to spasm, and anatomic anomalies.
One of the most common complications after TRA catheterization is radial artery occlusion (RAO), however, this is usually asymptomatic due to the redundancy of the hand circulation [5]. Since the TRA route has been adopted as standard for cardiac catheterization in some European countries, as well as in Japan, and China [6], recognizing the complications of TRA catheterization is of importance as they may impact the ability to perform repeat TRA catheterizations, the use of the vessel as a potential bypass graft, and the creation of a vascular shunt if permanent dialysis is ever needed [7]. RAO can be identified using plethysmography or Doppler ultrasonography. It has been estimated to affect from 1.5% to up to even 30.5% of the patients that had a TRA catheterization [5]; [8]; [9] ; [10]. RAO starts as a thrombotic occlusion of the artery lumen [11], and in many cases the radial artery recanalizes spontaneously [8]; [12]; [13] ; [14]; however propagation to arterial lumen fibrosis is possible [7] ; [15].
Several factors that predispose patients to develop RAO have been described. Among some of the procedure-related factors are prolonged cannulation times [16], intensity of anticoagulation [13] ; [17], hypotension during compression, and complete vessel occlusion during post-procedural care [18] ; [19]. Patient- and disease- related factors that may predispose to the development of RAO include diabetes [8]; [12] ; [19], peripheral arterial disease [14], smoking [10], low body weight [8], and small radial artery diameter [8]; [12] ; [18]. The radial artery diameter is thought to be most important relative to the size of sheath and the catheter. With a radial artery diameter to sheath diameter ratio of < 1, a higher incidence of RAO has been reported [8]; [12] ; [20]. This may explain why some studies reported that RAO was observed more frequently in women, who generally have radial arteries of smaller diameter and a greater predisposition to vessel spasm [8]; [14] ; [21].
In addition to the development of RAO, other vascular complications of TRA catheterization include minor hematoma [10] ; [22], artery perforation [23], endothelial dysfunction [7] ; [15], and pseudoaneurysm [14]. Complications such as arteriovenous fistulas (AV-fistula) and radial artery avulsion during sheath removal [14], as well as minor nerve damage and complex regional pain syndrome of the upper limb are rare [24]; [25] ; [26]. A few instances of hand ischemia have been reported [16]; [27]; [28] ; [29].
The wide range of rates of complication may be secondary to differences in the experience of the interventional cardiologist as well as differences in technical equipment, anticoagulation strategy, post-procedural care, and methods used to assess for RAO. The goal of this study was to evaluate, in the current era of anticoagulation, sheath and catheter techniques, the incidence of RAO and other vascular complications in an institution, which performs a high volume of TRA cardiac catheterizations and has standardized post-procedural care. To increase the sensitivity of detection, both clinical examination and Duplex ultrasound were used. Additionally, this study determined the incidence of upper extremity neurologic and motor complications in patients post TRA catheterization. Factors potentially involved in the development of vascular and upper extremity neurologic or motor complications were also investigated.
2. Methods
2.1. Patients
This single center, observational study was performed in accordance with the Declaration of Helsinki and was reviewed by the Ethics Committee of the Medical Practitioner Board, Thüringen, Germany.
Consecutive patients of both sexes, undergoing diagnostic and/or therapeutic TRA cardiac catheterizations between February and July 2015, were enrolled. Patients with stable coronary artery disease and with acute coronary syndrome (ACS) were both studied. The included patients had to be older than 18 years of age, had to give informed consent, and had to have intact, palpable radial pulses. Patients with known chronic RAO, absent radial artery pulse, or upper extremity lymphedema were excluded.
Patients were asked to give permission to use their data in accord with current German Data Protection Policy.
2.2. TRA catheterization procedure
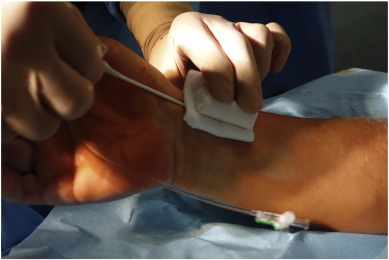
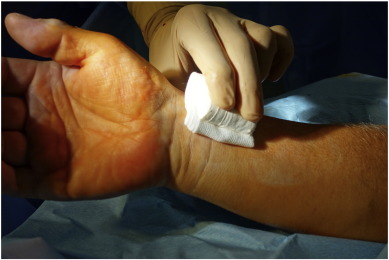
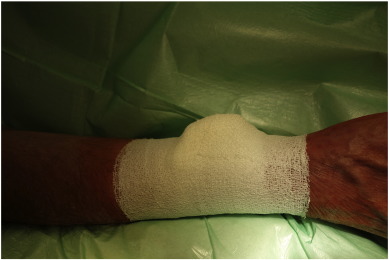
After sterile preparation and local anesthesia with 2% lidocaine, the right radial artery was cannulated using a modified Seldinger technique, puncturing the anterior vessel wall. Only 5Fr and 6Fr hydrophilic sheaths (Radifocus® Introducer II, Terumo, Japan), or in some cases 7.5Fr (for CTO and rotablation) sheathless guiding catheters (Asahi Intecc, Aichi, Japan) were used. After sheath insertion, 0.3 mg to 0.5 mg nitroglycerin and 2500–5000 IU heparin were injected gradually through the sheath into the radial artery. During the procedure, the doses of nitroglycerin, antithrombotic drugs (aspirin, P2Y12, or GPIIb/IIIa inhibitors) and heparin were adjusted depending on the type of procedure, bodyweight, and previous anticoagulation profile of the patient in keeping with current guidelines. ACT measurements were performed as needed. Immediately after completion of the procedure and radial sheath removal a sterile folded cotton pad was put on the puncture side. On top of this, a hand-rolled- cotton pad was affixed with tape and then tightened with a cohesive elastic bandage (Peha-haft®, Hartmann, Germany) (Supplementary Fig.1, Supplementary Fig. 2 ; Supplementary Fig. 3 Supplementary Data). After 3 h, the tight bandage was completely removed and then another Peha-haft bandage was affixed loosely until the morning. Patients were completely mobile during this period. Each patient received between 20 and 60 mg enoxaparin, adjusted according to bodyweight and previous anticoagulation profile, 5 to 10 h post-procedure.
2.3. Extraction of patient data from records
The following information were prospectively extracted from the patient records: anthropometric data, current medications, past medical history (focused on cardiac, renal, and upper extremity orthopedic disorders), as well as procedure related such as indication for the current catheterization, history of prior transradial cardiac catheterizations, and any associated complications, medication, sheaths and catheters used during the current procedure. From the laboratory studies routinely made prior to cardiac catheterization, glomerular filtration rate (GFR calculated according to CKD-EPI) were recorded. For subjects taking oral anticoagulants (OACs), the type and time of the last dose were recorded.
2.4. Hematoma examination
The presence of any hematoma on the arm used for TRA catheterization was recorded and classified according to the necessity of additional medical intervention.
2.5. Ultrasound examination of the radial artery
Radial artery patency was verified in each patient by Duplex ultrasonography. Pulse-wave Doppler, plus the standard B-mode and color flow Doppler were performed using a portable MicroMaxx SonoSite ultrasound system (Sonosite Inc., Bothell, WA, United States) with a 7.5 MHz transducer. The procedure was performed the following morning, 10 to 27 h after TRA cardiac catheterization depending on the time of the procedure. First, the presence of a palpable pulse was tested. Then the distal radial artery was visualized in longitudinal scan. To avoid measuring artefacts, the transducer was kept at a 60° angle to the artery, and all measurements were performed by a single investigator. Peak systolic flow was measured proximal and distal to the puncture site. Normal blood flow was indicated by a triphasic or biphasic flow. To exclude the possibility of a proximal occlusion, blood flow was assessed up to the brachial artery bifurcation.
2.6. Neurological and motor assessment
A simple questionnaire directed at helping to identify pain, unusual sensitivity, or limitations in the use of the hand that could correlate to an upper extremity neurologic or motor complication post-TRA catheterization was administered to the patient. The questionnaire was completed prior to the ultrasound examination.
2.7. Statistical analysis
Descriptive data were provided for all patients. Mean, standard deviation, median, minimum and maximum were used to characterize metric variables. Categorical variables were described using absolute frequencies and 95% confidence intervals (CI). Odds ratios (OR) were calculated to quantify the association of a given variable with post-procedural radial artery complications. Fishers exact test was used to test the null hypothesis that a categorical variable was not associated with complications. The Mann-Whitney-U Test was used to test whether patients with versus patients without complications differed in a metric variable, respectively. The number of patients with vascular complications that needed additional medical attention was too low for a meaningful multivariate analysis. Statistical relevance was accepted with a two-sided p < 0.05.
3. Results
During the study we followed 481 (507 procedures) out of 490 patients (520 procedures), 9 patients being lost due to unsuccessful first catheterization attempt and use of an alternative access site. Out of 481 patients, 25 patients had more than one intervention. Due to unfavorable anatomy, vasospasm development, or unsuccessful puncture in 19 procedures (3.6%) an alternative access site was used (for 14 patients the contralateral radial site and for 5 patients the femoral site), and 2 patients received no further catheterization during the current study. Thus, only 7 patients out of 490 (1.4%) could not receive a transradial cathetherization.
3.1. Local vascular complications
Vascular complications that needed further medical investigation were detected in 12 patients with an overall incidence of 2.36%. RAO was detected in 9 patients (1.77%), whereas 1 patient developed an AV-fistula (0.19%), and 2 patients developed pseudoaneurysm (0.38%). Of note, 7 patients with RAO were clinically asymptomatic, 1 patient had no radial pulse, and 1 patient had increased pain with the application of compression (Table 1). Five of these patients developed a minor hematoma. None of the patients needed surgery or special medical intervention. In the case of the patients with pseudoaneurysm, 1 patient developed a hematoma and moderate pain and 1 patient was asymptomatic. In both cases, with targeted compression, the pseudoaneurysm closed after 1 and 5 days, respectively. Clinically, only the patient with AV-fistula had signs of dysfunction characterized by increased pain, limited wrist motion and very large hematoma. However, no further clinical intervention was required in this case. Interestingly, in 11 out of 12 patients who developed vascular complications, the radial artery pulse was still palpable, three of them having retrograde arterial blood flow at the wrist level confirmed by ultrasound.
| Patient | Complication type | Pulse | Retrograde flow | Hematoma | Pain | Limitations in movement |
|---|---|---|---|---|---|---|
| 1 | AV-fistula | + | − | + | + | + |
| 2 | Pseudoaneurysm | + | − | − | − | − |
| 3 | Pseudoaneurysm | + | − | + | + | + |
| 4 | RAO | + | − | − | − | − |
| 5 | RAO | + | − | − | − | − |
| 6 | RAO | + | + | − | − | − |
| 7 | RAO | + | + | + | − | − |
| 8 | RAO | + | − | − | − | − |
| 9 | RAO | + | − | + | − | − |
| 10 | RAO | + | + | + | − | − |
| 11 | RAO | + | − | + | + | + |
| 12 | RAO | − | − | + | − | − |
Patient characteristics and procedural data of patients with and without vascular complications are listed in Table 2 (metric parameters) and Table 3 (categorical parameters) and were compared with regard to possible risk factors. Small radial artery diameter was a strong predictor of development of post-procedural vascular complications (2.11 ± 0.42 mm in patients with vascular complications vs. 2.52 ± 0.39 mm, p = 0.001), whereas other factors such as multimorbidity (severe chronic kidney disease, diabetes), acuteness and complexity of the procedure, sheath and catheter size, or use of OACs on the intervention day, had no statistically significant effect on the rate of vascular complications.
| Vascular complications | n | Mean | SD | Median | Min-Max | OR (95%-CI) p-Value⁎ | |
|---|---|---|---|---|---|---|---|
| Age (years) | − | 495 | 67.5 | 10.7 | 70.0 | 24.0–91.0 | 1.03 (0.97–1.08) |
| + | 12 | 70.5 | 10.3 | 73.5 | 50.0–84.0 | p = 0.310 | |
| BMI | − | 495 | 28.8 | 5.2 | 28.0 | 16.0–59.0 | 1.01 (0.90–1.12) |
| + | 12 | 28.9 | 5.3 | 29.2 | 22.6–36.9 | p = 0.922 | |
| GFR (ml/min/1.7m2) | − | 495 | 70.2 | 21.8 | 73.0 | 7.0–118.0 | 0.98 (0.96–1.01) |
| + | 12 | 60.9 | 21.8 | 58.5 | 31.0–96.0 | p = 0.131 | |
| Duration (min) | − | 495 | 32.9 | 25.4 | 24.0 | 4.0–186.0 | 1.00 (0.98–1.03) |
| + | 12 | 34.3 | 18.0 | 33.5 | 8.0–61.0 | p = 0.448 | |
| Diameter (mm) | − | 495 | 25.2 | 3.9 | 25.0 | 14.0–36.0 | 0.77 (0.67–0.89) |
| [× 10] | + | 12 | 21.1 | 4.2 | 20.5 | 16.0–30.0 | p = 0.001 |
⁎. p-Value Mann-Whitney-U test.
| n | Vascular complications | Ratio (%) 95%-CI | OR (95%-CI) | p-Value⁎ | ||
|---|---|---|---|---|---|---|
| Gender | M | 327 | 6 | 1.8 (0.7–4.0) | Ref | |
| F | 180 | 6 | 3.3 (1.2–7.1) | 1.84 (0.58–5.82) | 0.361 | |
| Age (years) | < 60 | 130 | 2 | 1.5 (0.2–5.4) | Ref | |
| 61–75 | 258 | 6 | 2.3 (0.9–5.0) | 1.52 (0.30–7.68) | 0.723 | |
| > 75 | 119 | 4 | 3.4 (0.9–8.4) | 2.23 (0.40–12.46) | 0.430 | |
| Smoking | − | 396 | 10 | 2.5 (1.2–4.6) | Ref | |
| + | 111 | 2 | 1.8 (0.2–6.4) | 0.71 (0.15–3.29) | 1.000 | |
| Diabetes | − | 306 | 7 | 2.3 (0.9–4.7) | Ref | |
| + | 201 | 5 | 2.5 (0.8–5.7) | 1.09 (0.34–3.49) | 1.000 | |
| Coronary disease | None | 59 | 1 | 1.7 (0.0–9.1) | Ref | |
| Coronary atherosclerosis | 124 | 1 | 0.8 (0.0–4.4) | 0.47 (0.03–7.75) | 0.542 | |
| 1-Vessel | 101 | 5 | 5.0 (1.6–11.2) | 3.02 (0.34–26.88) | 0.415 | |
| 2-Vessel | 120 | 3 | 2.5 (0.5–7.1) | 1.49 (0.15–14.72) | 1.000 | |
| 3-Vessel | 103 | 2 | 1.9 (0.2–6.8) | 1.15 (0.10–13.04) | 1.000 | |
| Heparin (IU) | < 5000 | 20 | 0 | 0 (0.0–16.8) | − | |
| 5000 | 309 | 10 | 3.2 (1.6–5.9) | − | 1.000 | |
| > 5000 | 178 | 2 | 1.1 (0.1–4.0) | − | 1.000 | |
| Oral anticogulant | No OAC | 407 | 8 | 2.0 (0.9–3.8) | Ref | |
| No OACPD | 52 | 1 | 1.9 (0.0–10.3) | 0.98 (0.12–8.00) | 1.000 | |
| OAC | 48 | 3 | 6.3 (1.3–17.2) | 3.33 (0.85–13.07) | 0.099 | |
| Procedure a) | Elective | 483 | 10 | 2.1 (1.0–3.8) | Ref | |
| emergency | 24 | 2 | 8.3 (1.0–27.0) | 4.30 (0.88–20.98) | 0.106 | |
| Procedure b) | Diagnostic | 299 | 6 | 2.0 (0.7–4.3) | Ref | |
| Intervention | 208 | 6 | 2.9 (1.1–6.2) | 1.45 (0.46–4.57) | 0.562 | |
| Sheath size (Fr) | 5 | 283 | 6 | 2.1 (0.8–4.6) | Ref | |
| 6 | 224 | 6 | 2.7 (1.0–5.7) | 1.27 (0.40–4.00) | 0.772 | |
| Sheath number | 1 | 427 | 10 | 2.3 (1.1–4.3) | Ref | |
| 2 | 80 | 2 | 2.5 (0.3–8.7) | 1.07 (0.23–4.98) | 1.000 | |
| Previous procedures | None | 343 | 9 | 2.6 (1.2–4.9) | Ref | |
| 1 | 122 | 1 | 0.8 (0.0–4.5) | 0.31 (0.04–2.46) | 0.466 | |
| ≥ 2 | 42 | 2 | 4.8 (0.6–16.2) | 1.86 (0.39–8.92) | 0.342 | |
| Catheter size (Fr) | ≤ 5 | 313 | 7 | 2.2 (0.9–4.6) | Ref | |
| > 5 | 194 | 5 | 2.6 (0.8–5.9) | 1.16 (0.36–3.70) | 0.774 | |
| Catheter number | 1 | 114 | 3 | 2.6 (0.5–7.5) | Ref | |
| 2 | 212 | 2 | 0.9 (0.1–3.4) | 0.35 (0.06–2.15) | 0.348 | |
| 3 | 112 | 4 | 3.6 (1.0–8.9) | 1.37 (0.30–6.29) | 0.720 | |
| ≥ 4 | 69 | 3 | 4.3 (0.9–12.2) | 1.68 (0.33–8.63) | 0.674 |
⁎. p-Value Fishers exact test.
The most common local vascular complication was a minor hematoma mostly localized at the puncture site. All factors that significantly contributed to the development of minor access site complications are found in Table 4 (metric parameters) and Table 5 (categorical parameters). Minor hematoma developed in 169 patients (33%) and was associated with increased age 70.6 ± 10.4 years vs 66.1 ± 10.5 years (p < 0.001), female gender (OR 2.22, 95%-Cl 1.51–3.28, p < 0.001), impaired renal function with GFR of 65.8 ± 20.8 ml/min/1.7 m2 vs. 72.2 ± 22.1 ml/min/1.7 m2 (p < 0.001), coronary artery disease (OR 2.12, 95%-Cl 1.02–4.40, p = 0.042), as well as procedural settings as interventional procedures (OR 2.29, 95%-Cl 1.56–3.36, p < 0.001), longer procedural duration (36.8 ± 25.3 min vs 31 ± 2.1 min, p = 0.005), increased size and number of radial sheaths (OR 1.67, 95%-Cl 1.15–2.43, p = 0.008 and OR 2.17, 95%-Cl 1.33–3.55, p = 0.002, respectively), catheter size (OR 2.21, 95%-Cl 1.50–3.24, p < 0.001), and high intra-procedural heparinization (OR 4.95, 95%-Cl 1.36–17.98, p = 0.008).
| Complication | n | Mean | SD | Median | Min-Max | OR (95%-CI) p-Value⁎ | |
|---|---|---|---|---|---|---|---|
| Hematoma | |||||||
| Age (years) | − | 338 | 66.1 | 10.5 | 67.0 | 32.0–89.0 | 1.04 (1.02–1.06) |
| + | 169 | 70.6 | 10.4 | 73.0 | 24.0–91.0 | p < 0.001 | |
| GFR (ml/min/1.7m2) | − | 338 | 72.2 | 22.1 | 74.0 | 7.0–118.0 | 0.99 (0.98–1.00) |
| + | 169 | 65.8 | 20.8 | 67.0 | 10.0–107.0 | p < 0.001 | |
| Duration (min) | − | 338 | 31.0 | 25.1 | 23.0 | 5.0–186.0 | 1.01 (1.00–1.02) |
| + | 169 | 36.8 | 25.3 | 30.0 | 4.0–143.0 | p = 0.005 | |
| Pain | |||||||
| Diameter (mm) | − | 475 | 25.2 | 3.9 | 25.0 | 14.0–36.0 | 0.92 (0.84–1.01) |
| [× 10] | + | 32 | 23.9 | 4.5 | 23.0 | 17.0–36.0 | p = 0.018 |
⁎. p-Value Mann-Whitney-U test.
| n | Complication | Ratio(%) 95%-CI | OR (95%-CI) | p-Value⁎ | ||
|---|---|---|---|---|---|---|
| Hematoma | ||||||
| Gender | M | 327 | 88 | 26.9 (22.2–32.1) | Ref | |
| F | 180 | 81 | 45.0 (37.6–52.6) | 2.22 (1.51–3.28) | < 0.001 | |
| Age (years) | < 60 | 130 | 26 | 20.0 (13.5–27.9) | Ref | |
| 61–75 | 258 | 87 | 33.7 (28.0–39.8) | 2.04 (1.23–3.38) | 0.006 | |
| > 75 | 119 | 56 | 47.1 (37.8–56.4) | 3.56 (1.98–6.39) | < 0.001 | |
| Coronary disease | None | 59 | 13 | 22.0 (12.3–34.7) | Ref | |
| Coronary arteriosclerosis | 124 | 36 | 29.0 (21.2–37.9) | 1.45 (0.70–3.01) | 0.374 | |
| 1-Vessel | 101 | 36 | 35.6 (26.4–45.8) | 1.96 (0.93–4.14) | 0.078 | |
| 2-Vessel | 120 | 45 | 37.5 (28.8–46.8) | 2.12 (1.02–4.40) | 0.042 | |
| 3-Vessel | 103 | 39 | 37.9 (28.5–48.0) | 2.16 (1.02–4.54) | 0.054 | |
| Heparin (IU) | < 5000 | 20 | 3 | 15.0 (3.2–37.9) | Ref | |
| 5000 | 309 | 83 | 26.9 (22.0–32.2) | 2.08 (0.59–7.32) | 0.303 | |
| > 5000 | 178 | 83 | 46.6 (39.1–54.2) | 4.95 (1.36–17.98) | 0.008 | |
| Procedure | Diagnostic | 299 | 77 | 25.8 (20.9–31.1) | Ref | |
| Intervention | 208 | 92 | 44.2 (37.4–51.3) | 2.29 (1.56–3.36) | < 0.001 | |
| Sheath size (Fr) | 5 | 283 | 80 | 28.3 (23.1–33.9) | Ref | |
| 6 | 224 | 89 | 39.7 (33.3–46.5) | 1.67 (1.15–2.43) | 0.008 | |
| Sheath number | 1 | 427 | 130 | 30.4 (26.1–35.1) | Ref | |
| 2 | 80 | 39 | 48.8 (37.4–60.2) | 2.17 (1.33–3.55) | 0.002 | |
| Catheter size (Fr) | ≤ 5 | 313 | 83 | 26.5 (21.7–31.8) | Ref | |
| > 5 | 194 | 86 | 44.3 (37.2–51.6) | 2.21 (1.50–3.24) | < 0.001 | |
| Pain | ||||||
| Gender | M | 327 | 14 | 4.3 (2.4–7.1) | Ref | |
| F | 180 | 18 | 10.0 (6.0–15.3) | 2.48 (1.20–5.15) | 0.013 | |
| Swelling | ||||||
| Gender | M | 327 | 7 | 2.1 (0.9–4.4) | Ref | |
| F | 180 | 14 | 7.8 (4.3–12.7) | 3.86 (1.51–9.83) | 0.004 | |
| Sheath size (Fr) | 5 | 283 | 7 | 2.5 (1.0–5.0) | Ref | |
| 6 | 224 | 14 | 6.3 (3.5–10.3) | 2.63 (1.04–6.66) | 0.043 | |
⁎. p-Value Fishers exact test.
3.2. Local motor and/or neurologic complications
There were no major local, post-interventional motor or neurologic complications. In 32 post-procedural questionnaires (6.3%) patients reported pain in the arm on the following day. However, they did not need any additional medical intervention. Pain was reported by 10% of the women and 4.3% of the men participating in the study (OR 2.48, 95% CI 1.20–5.15, p = 0.013) and was associated with a small radial artery diameter (2.39 ± 0.45 mm vs 2.5 ± 0.39 mm, p = 0.018). Transient post-procedural hand/arm swelling was observed in 21 patients (4.1%), most likely due to the temporary tight post-procedural compression. Swelling developed in 7.8% of women and 2.1% of men (OR 3.86, 95% CI 1.51–9.86, p = 0.004) and was associated with the use of 6Fr size radial sheath (OR 2.63, 95% CI 1.04–6.66, p = 0.043).
Motor limitations developed in 8 patients (1.6%) and were mostly correlated with swelling of the arm due to tight post-procedural compression. Additionally, 11 patients (2.2%) reported formication in the hand and 4 patients (0.8%) felt the hand to be warmer than usual.
4. Discussion
In many cardiac catheterization centers, TRA catheterization is preferred over transfemoral catheterization due to its lower incidence of post-interventional complications, especially bleeding [1]; [2]; [3] ; [4]. However, concerns regarding unknown or potentially high rates of access site complications still generate debate.
Previous studies report a wide range of vascular complication rates from 1.5% to 30.5% [5]; [8]; [9] ; [10]. Using current techniques and materials, we report here a very low access site vascular complication rate (2.36%) within 24 h after TRA catheterization. This is due in part to our extensive experience of selecting materials for compression and of testing different sheaths and catheters. Importantly, we have also standardized our procedural and post-procedural regimens so that there has been an optimal adjustment of parameters known to influence the rate of complication development, particularly the degree of anticoagulation, reduction of tight compression time to 3 h, and post-procedural administration of enoxaparin. Under our conditions, the only significant risk factor for the development of vascular complications was radial artery diameter. In this study, patients with radial artery diameters < 2.1 mm had a higher rate of post-procedural complications. Renal failure and the acuteness of the procedure may also play a secondary role in the development of complications, but were not statistically significant here. Interestingly, anticoagulation, sheath and catheter size and complexity of procedure did not influence at all the vascular complications rate. Spaulding et al. (1996) have shown that a significant decrease in the incidence of RAO correlated with more aggressive anticoagulation; whereas, other studies have shown no effect or only protective trends when > 2500 IU heparin was used [9]; [13] ; [22]. This is in agreement with our study in which we observe no influence of heparin on vascular complication development rate when > 2500 IU is used. However, Kelm et al. (2002) have shown an increased risk for developing AV-fistula at the femoral access site when > 12.500 IU heparin or when warfarin was used. This might suggest an upper limit to the beneficial effects of anticoagulation [30]. Our anticoagulation regimen is standardized and consists of procedural anticoagulation with 2500–12,500 IU heparin depending on the type of procedure, bodyweight, and previous anticoagulation profile of the patient, followed by post-procedural anticoagulation with 20–60 mg enoxaparin. However, our results suggest that supplementation with OACs on the catheterization day do not influence the rate of vascular complications. The important role of sheath and catheter size in the development of access site complications was described by several studies [8]; [12]; [14] ; [20]. Under our procedural conditions, sheath and catheter size did not affect the incidence of vascular complications, similar to the findings reported by Markovic et al. [22]. In addition to optimal anticoagulation, we used the more recent generation of hydrophilic, polymer-coated sheaths, which are reported to reduce the incidence of radial artery spasm, reduce shear stress to the vessel wall by requiring less force to remove than identical uncoated sheaths, and are associated with less discomfort for the patient [31] ; [32]. As alluded to above, of critical importance in the reduction of access site vascular complication rate was also the post-procedural care. Thus, the tight compression time in our department is only 3 h and is followed by light compression until the next morning. This not only prevented the occlusion of radial artery as previously reported [18] ; [19], but also allowed patients to remain mobile. This eliminated the discomfort caused by commercial TR bands and pulse plethysmography, which additionally demand patient cooperation.
It is important to note that only 1 out of 12 patients who developed vascular complications did not have a palpable pulse and that only 1 patient could be identified with an AV-fistula based on clinical examination (symptoms, palpation, and auscultation). Thus, 4 patients were totally asymptomatic, and 6 patients had clinical symptoms similar to patients without radial artery injury. Thus, under typical conditions, only two of these 12 patients would have received a Duplex ultrasound investigation. Thus, it is easy to appreciate the difficulties in quantifying a vascular complication rate if no ultrasound analysis is used and could explain the broad range of reported complication rates. The implication of this finding is very important since early identification of pseudoaneurysms and AV fistulas is critical for their management, and repeated transradial catheterization in patients with RAO can be avoided. Thus, we recommend routine clinical examination and use of Duplex ultrasound as part of post-procedural care, or, if not possible, at least when one of the following is present: subjective clinical symptoms reported by the patient (pain, motor impairment, hand/arm swelling), absence of pulse, bruits heard on auscultation, or minor hematoma.
The most common complication documented in our settings was minor hematoma. Minor hematomas and transient post-procedural hand swelling were recorded in 33% and 4.1% of the patients, respectively. Thus, we documented a higher incidence of hematoma than previously reported [10] ; [33]. However, a direct comparison is difficult since in these prior studies hematoma development was investigated in a follow-up 30 days post-procedure and minor hematoma was defined as the need for 1 U of blood or modification of antiplatelet therapy. None of our patients required blood transfusions or alterations of their medication regimen since all of the hematomas recorded here were minor bruises that resolved spontaneously. Increased age, female gender, impaired renal function, coronary artery disease, and procedural factors such as interventions, longer procedural duration, stronger heparinization, increased size and number of radial sheaths, and increased catheter size were identified as risk factors for developing hematoma. Using a standardized radial approach and similar criteria for defining minor hematoma as in the present study, Markovic et al. (2015) observed minor hematoma in 16% of patients. However, this did not correlate with sheath size, need for secondary compression, or use of dual antiplatelet therapy or oral anticoagulation, possibly due to the smaller sample size used in that study.
Finally, we did not observe any major local neurologic or motor complications. Pain was reported by 6.3% of the patients, was more frequent in women, and was associated with a smaller radial artery diameter. None of the patients needed additional medical care or analgesic drugs. Similarly, transient post-procedural hand/arm swelling was identified in 4.1% of the patients, being more frequent in women and when 6Fr radial sheaths were used. Few instances of motor limitations (1.6%), hand paresthesias (2.2%), and hyperthermic perception of the “injured” arm (0.8%) were also reported.
In summary, our results suggest that the overall upper extremity vascular and neurological complication rate of TRA catheterization is quite low and that the complications are not severe. We did find that small radial artery diameter was associated with an increased rate of vascular complications and with the development of minor neurologic and/or motor complications. This should perhaps be kept in mind when patients with a smaller body habitus undergo TRA left heart catheterization.
5. Conclusions
In this prospective ultrasound-based study, we report a very low rate of local post-procedural vascular complications, no major hematoma, and no major local neurologic or motor complications associated with TRA cardiac catheterization at our high volume center using current techniques and guidelines. We found that a radial artery diameter of < 2.1 mm was a risk factor for local vascular complications. Other risk factors found in earlier studies, such as renal failure, diabetes, emergent catheterization, sheath size, and oral anticoagulation were at most trends here.
These findings suggest that TRA left heart catheterization in the current interventional era is a very safe procedure.
6. Limitations of the study
There are limitations in the design of this study. This is a single center prospective study so one cannot exclude the possibility of a bias. No ultrasound measurements were performed before the TRA catheterization, thus the status of the radial artery pre- and post-catheterization could not be compared. Ultrasound measurements were done 10–27 h post-catheterization and no later follow-up was done. Thus, we cannot comment on recanalization of the occluded artery at a later time point or exclude the possibility of the development of later complications. The inability or refusal of some patients hospitalized in the intensive care unit to give consent for participation in the study also may have led to a lower number of acutely treated patients being included in the study. Finally, given that we had a very low number of complications, the statistical power may have been too limited to demonstrate some associations that actually exist.
The following are the supplementary data related to this article.
|
|
|
Supplementary Fig.1. Post-procedural sheath removal. |
|
|
|
Supplementary Fig. 2. Self-made roll made from a cotton pad. |
|
|
|
Supplementary Fig. 3. Cotton pad fixed with a cohesive elastic bandage. |
Funding
This study was supported by HELIOS Kliniken GmbH, Grant-ID: 000113.
Conflict of interest statement
All authors state that there is no conflict of interest.
Acknowledgments
This study was supported by HELIOS Kliniken GmbH, Grant-ID: 000113. Statistics were performed by Ms. Hiltrud Niggemann, www.p-wert.de.
References
- [1] S.S. Jolly, S. Amlani, M. Hamon, S. Yusuf, S.R. Mehta; Radial versus femoral access for coronary angiography or intervention and the impact on major bleeding and ischemic events: a systematic review and meta-analysis of randomized trials; Am. Heart J., 157 (2009), pp. 132–140
- [2] M. Valgimigli, A. Gagnor, P. Calabró, E. Frigoli, S. Leonardi, T. Zaro, et al.; Radial versus femoral access in patients with acute coronary syndromes undergoing invasive management: a randomised multicentre trial; Lancet, 385 (2015), pp. 2465–2476
- [3] P. Agostoni, G.G.L. Biondi-Zoccai, M.L. De Benedictis, S. Rigattieri, M. Turri, M. Anselmi, et al.; Radial versus femoral approach for percutaneous coronary diagnostic and interventional procedures: systematic overview and meta-analysis of randomized trials; J. Am. Coll. Cardiol., 44 (2004), pp. 349–356
- [4] M.D. Mitchell, J.A. Hong, B.Y. Lee, C.A. Umscheid, S.M. Bartsch, C.W. Don; Systematic review and cost-benefit analysis of radial artery access for coronary angiography and intervention; Circ. Cardiovasc. Qual. Outcomes, 5 (2012), pp. 454–462
- [5] J. Slawin, P. Kubler, A. Szczepanski, J. Piatek, M. Stepkowski, K. Reczuch; Radial artery occlusion after percutaneous coronary interventions—an underestimated issue; Postepy Kardiol. Interwencyjnej, 9 (2013), pp. 353–361
- [6] Bertrand OF, S.V. Rao, S. Pancholy, S.S. Jolly, J. Rodés-Cabau, É. Larose, et al.; Transradial approach for coronary angiography and interventions: results of the First International Transradial Practice Survey; JACC Cardiovasc. Interv., 3 (2010), pp. 1022–1031
- [7] J.M. Burstein, D. Gidrewicz, S.J. Hutchison, K. Holmes, S. Jolly, W.J. Cantor; Impact of radial artery cannulation for coronary angiography and angioplasty on radial artery function; Am. J. Cardiol., 99 (2007), pp. 457–459
- [8] N. Garg, B.K. Madan, R. Khanna, A. Sinha, A. Kapoor, S. Tewari, et al.; Incidence and predictors of radial artery occlusion after transradial coronary angioplasty: Doppler-guided follow-up study; J. Invasive Cardiol., 27 (2015), pp. 106–112
- [9] G. Hahalis, I. Xathopoulou, G. Tsigkas, G. Almpanis, I. Christodoulou, N. Grapsas, et al.; A comparison of low versus standard heparin dose for prevention of forearm artery occlusion after 5 French coronary angiography; Int. J. Cardiol., 187 (2015), pp. 404–410
- [10] D.A. Jia, Y.J. Zhou, D.M. Shi, Y.Y. Liu, J.L. Wang, X.L. Liu, et al.; Incidence and predictors of radial artery spasm during transradial coronary angiography and intervention; Chin. Med. J., 123 (2010), pp. 843–847
- [11] A.R. Zankl, M. Andrassy, C. Volz, B. Ivandic, U. Krumsdorf, H.A. Katus, et al.; Radial artery thrombosis following transradial coronary angiography: incidence and rationale for treatment of symptomatic patients with low-molecular-weight heparins; Clin. Res. Cardiol., 99 (2010), pp. 841–847
- [12] S. Nagai, S. Abe, T. Sato, K. Hozawa, K. Yuki, K. Hanashima, et al.; Ultrasonic assessment of vascular complications in coronary angiography and angioplasty after transradial approach; Am. J. Cardiol., 83 (1999), pp. 180–186
- [13] P.R. Stella, F. Kiemeneij, G.J. Laarman, D. Odekerken, T. Slagboom, R. van der Wieken; Incidence and outcome of radial artery occlusion following transradial artery coronary angioplasty; Catheter. Cardiovasc. Diagn., 40 (1997), pp. 156–158
- [14] M. Uhlemann, S. Möbius-Winkler, M. Mende, I. Eitel, G. Fuernau, M. Sandri, et al.; The Leipzig prospective vascular ultrasound registry in radial artery catheterization: impact of sheath size on vascular complications; JACC Cardiovasc. Interv., 5 (2012), pp. 36–43
- [15] T. Wakeyama, H. Ogawa, H. Iida, A. Takaki, T. Iwami, M. Mochizuki, et al.; Intima-media thickening of the radial artery after transradial intervention: an intravascular ultrasound study; J. Am. Coll. Cardiol., 41 (2003), pp. 1109–1114
- [16] R.J. Valentine, J.G. Modrall, G.P. Clagett; Hand ischemia after radial artery cannulation; J. Am. Coll. Surg., 201 (2005), pp. 18–22
- [17] C. Spaulding, T. Lefevre, F. Funck, B. Thebault, M. Chauveau, K. Ben Hamda, et al.; Left radial approach for coronary angiography: results of a prospective study; Catheter. Cardiovasc. Diagn., 39 (1996), pp. 365–370
- [18] M. Sanmartin, M. Gomez, J.R. Rumoroso, M. Sadaba, M. Martinez, J.A. Baz, et al.; Interruption of blood flow during compression and radial artery occlusion after transradial catheterization; Catheter. Cardiovasc. Interv., 70 (2007), pp. 185–189
- [19] S.B. Pancholy, Bertrand OF, T. Patel; Comparison of a priori versus provisional heparin therapy on radial artery occlusion after transradial coronary angiography and patent hemostasis (from the PHARAOH Study); Am. J. Cardiol., 110 (2012), pp. 173–176
- [20] S. Saito, H. Ikei, G. Hosokawa, S. Tanaka; Influence of the ratio between radial artery inner diameter and sheath outer diameter on radial artery flow after transradial coronary intervention; Catheter. Cardiovasc. Interv., 46 (1999), pp. 173–178
- [21] A. Tuncez, Z. Kaya, D. Aras, A. Yildiz, E.E. Gul, M. Tekinalp, et al.; Incidence and predictors of radial artery occlusion associated transradial catheterization; Int. J. Med. Sci., 10 (2013), pp. 1715–1719
- [22] S. Markovic, A. Imhof, M. Kunze, W. Rottbauer, J. Wohrle; Standardized radial approach reduces access site complications: a prospective observational registry; Coron. Artery Dis., 26 (2015), pp. 56–59
- [23] T. Patel, S. Shah, K. Sanghavi, S. Pancholy; Management of radial and brachial artery perforations during transradial procedures–a practical approach; J. Invasive Cardiol., 21 (2009), pp. 544–547
- [24] E.J. Cho, J.H. Yang, Y.B. Song; Type II complex regional pain syndrome of the hand resulting from repeated arterial punctures during transradial coronary intervention; Catheter. Cardiovasc. Interv., 82 (2013), pp. E465–E468
- [25] M.Y. Jeong, J.S. Yu, W.B. Chung; Usefulness of thermography in diagnosis of complex regional pain syndrome type I after transradial coronary intervention; J. Invasive Cardiol., 25 (2013), pp. E183–E185
- [26] T.J. Papadimos, J.P. Hofmann; Radial artery thrombosis, palmar arch systolic blood velocities, and chronic regional pain syndrome 1 following transradial cardiac catheterization; Catheter. Cardiovasc. Interv., 57 (2002), pp. 537–540
- [27] M. Ayan, A. Smer, M. Azzouz, A. Abuzaid, A. Mooss; Hand ischemia after transradial coronary angiography: resulting in right ring finger amputation; Cardiovasc. Revasc. Med., 16 (2015), pp. 367–369
- [28] M.K. Lee, I.O. Lee, M.H. Kong, S.K. Han, S.H. Lim; Surgical treatment of digital ischemia occurred after radial artery catheterization; J. Korean Med. Sci., 16 (2001), pp. 375–377
- [29] L.M. Rademakers, G.J. Laarman; Critical hand ischaemia after transradial cardiac catheterisation: an uncommon complication of a common procedure; Neth. Heart J., 20 (2012), pp. 372–375
- [30] M. Kelm, S.M. Perings, T. Jax, T. Lauer, F.C. Schoebel, M.P. Heintzen, et al.; Incidence and clinical outcome of iatrogenic femoral arteriovenous fistulas: Implications for risk stratification and treatment; J. Am. Coll. Cardiol., 40 (2002), pp. 291–297
- [31] F. Kiemeneij, D. Fraser, T. Slagboom, G. Laarman, R. van der Wieken; Hydrophilic coating aids radial sheath withdrawal and reduces patient discomfort following transradial coronary intervention: a randomized double-blind comparison of coated and uncoated sheaths; Catheter. Cardiovasc. Interv., 59 (2003), pp. 161–164
- [32] S. Rathore, R.H. Stables, M. Pauriah, A. Hakeem, J.D. Mills, N.D. Palmer, et al.; Impact of length and hydrophilic coating of the introducer sheath on radial artery spasm during transradial coronary intervention: a randomized study; JACC Cardiovasc. Interv., 3 (2010), pp. 475–483
- [33] S.S. Jolly, S. Yusuf, J. Cairns, K. Niemela, D. Xavier, P. Widimsky, et al.; Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): a randomised, parallel group, multicentre trial; Lancet, 377 (2011), pp. 1409–1420
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?