Summary
Objective
To investigate the safe displacement range of the foramen of Monro (FM) during single burr hole rigid endoscopic third ventriculostomy (ETV) and endoscopic tumor biopsy (ETB).
Methods
Eleven patients who received ETV/ETB for third ventricular and pineal region tumor were reviewed. The burr-hole location, the size, and the virtual displacement of FM were measured using neuronavigation software.
Results
Hydrocephalus was resolved, and no subsequent cerebrospinal fluid (CSF) shunting was required in all cases. Histological diagnosis was established in 11 patients. Ten cases received instrumental cognitive and memory assessment postoperatively. The results were within the normal range for eight cases. The mean burr-hole location was 1.7 cm anterior to coronal suture and 3 cm from the midline. The mean diameters of FM measured on the axial, coronal, sagittal, and views were 5.7, 7.8, and 5.6 mm, respectively. The mean virtual displacements of the FM were 1.9 ± 2.0 mm (range = 0–4.8) for ETV and 2.4 ± 2.1 mm (range = 0–5.5) for ETB. The maximum displacements were 4.8 mm anteriorly for ETV and 5.5 mm posteriorly for ETB.
Conclusion
Single burr hole rigid ETV/ETB is likely to be safe within maximum FM displacements of 4.8 mm anterior for ETV and 5.5 mm posterior for ETB. Preoperative trajectory planning using neuronavigation software is recommended.
Keywords
endoscopic biopsy;endoscopy;hydrocephalus;neuronavigation;pineal region tumor;third ventricular tumor;third ventriculostomy
1. Introduction
Posterior third ventricle and pineal region tumors are heterogenic in histology, including germ cell tumors, pineal tumors, astrocytic tumors, and cystic lesions. Consequently, the corresponding therapy and prognosis are also different. By contrast, the clinical findings are quite consistent – approximately 90% of these patients present obstructive hydrocephalus and features of raised intracranial pressure (ICP).1 Therefore, endoscopic third ventriculostomy (ETV) and endoscopic tumor biopsy (ETB) is the choice for initial management to relieve the hydrocephalus and establish the histological diagnosis.1; 2; 3; 4; 5; 6; 7; 8; 9; 10; 11; 12; 13; 14; 15; 16; 17; 18; 19 ; 20 Treatment of the tumor can be planned afterwards, such as chemotherapy, radiotherapy, or surgical excision. One of the complications of ETV or ETV/ETB is possible injury to the structure around the foramen of Monro (FM), especially the fornix, resulting in memory impairment related to the movement of the endoscope during the procedure.2; 6; 21; 22; 23; 24; 25; 26; 27; 28; 29; 30; 31 ; 32 Apart from in-depth knowledge of the related anatomy and mastering the neuroendoscopic technique, trajectory planning of ETV and ETB is very important in order to minimize the tissue displacement of the FM, thus avoiding injury to the structure around. In this study, using neuronavigation software, we measured the virtual displacement of FM during a single burr hole rigid ETV and ETB procedure. We also correlated the range of displacement with the clinical outcome, including the memory function. We believe that this range will serve as a useful reference for choosing a safe method to perform ETV/ETB, such as single versus two burr hole methods.
2. Patients and methods
2.1. Patients
All patients with posterior third ventricle and pineal region tumors and who underwent ETV and ETB in both institutes of the authors between 2001 and 2008 were reviewed.
2.2. Methods
The clinical presentation, image findings, surgical procedure, pathological diagnosis, subsequent treatment, and clinical outcomes were reviewed. Instrumental assessments including the Mini-Mental State Examination (MMSE), and Rivermead Behavioral Memory Test (RBMT)33 were performed in 2008 to evaluate the cognitive and memory functions.
2.2.1. Endoscopic technique
All procedures were performed with the patients under general anesthesia and in a supine position. A precoronal burr hole with a diameter of 14 mm was made at the mid-pupillary line. A rigid 30°-view neuroendoscope of 3.5 mm × 5.0 mm in diameter with two working channels (Storz, Munich, Germany) was introduced into the lateral ventricle. The cerebrospinal fluid (CSF) specimen was collected. Then, the endoscope was advanced into the third ventricle through the FM. With the 30° view facing anteriorly, ETV was performed in the midline between the mammillary bodies and the infundibular recess in the standard manner. After ETV, the endoscope was directed to the posterior part of the third ventricle with the 30° view facing posteriorly. Tumor biopsy was performed using cup biopsy forceps. Any bleeding of the biopsy site was controlled by irrigation with or without diathermy cauterization. On completion of the procedure, the endoscope was withdrawn slowly. Structures around the FM including the fornix were inspected. Finally, a catheter was inserted into the ventricle for ICP monitoring postoperatively.
The preoperative magnetic resonance imaging (MRI) and postoperative computed tomography (CT) images were fused using neuronavigation software (BrainLAB iPlan Cranial 2.6, Heimstetten, Germany) for three-dimensional reconstruction and analysis. The axial plane was aligned to the anterior–posterior commission plane. Two trajectories were drawn from the center of the actual burr hole to the site of ETV at the floor of the third ventricle and to the site of tumor biopsy (Figs. 1 and 2). At the level of FM using the probe view (i.e., to view perpendicular to the trajectory), the distance between the edge of the foramen and the trajectory was measured as the distance of virtual displacement (Figs. 3 and 4). The location of the actual burr hole was measured in terms of distances from the midline and the coronal suture, and also the angle between the trajectory and the orbitomeatal (OM) line. The size of the FM on preoperative MRI was measured in its maximal extension size on axial, coronal, and sagittal images.
|
|
|
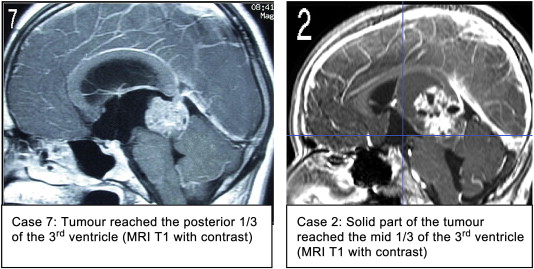
Figure 1. MRI images of the tumor location with respect to the third ventricle. |
|
|
|
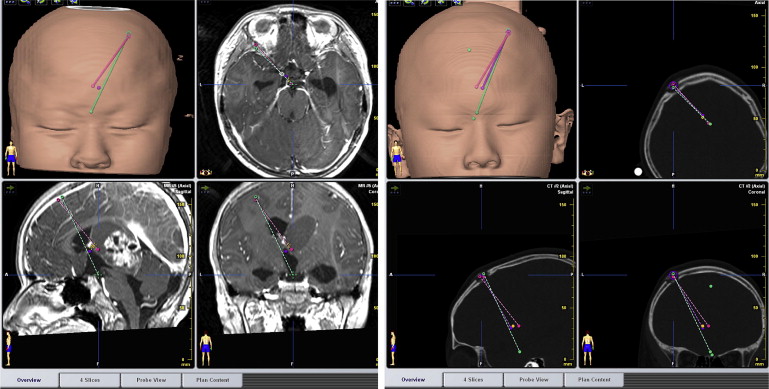
Figure 2. ETV and ETB trajectory reconstruction: The preoperative MRI image and postoperative CT images were fused together. The trajectories were drawn from the burr hole to the sites of the ETV and ETB in the three-dimensional reconstruction images. CT = computed tomography; ETB = endoscopic tumor biopsy; ETV = endoscopic third ventriculostomy; MRI = magnetic resonance imaging. |
|
|
|
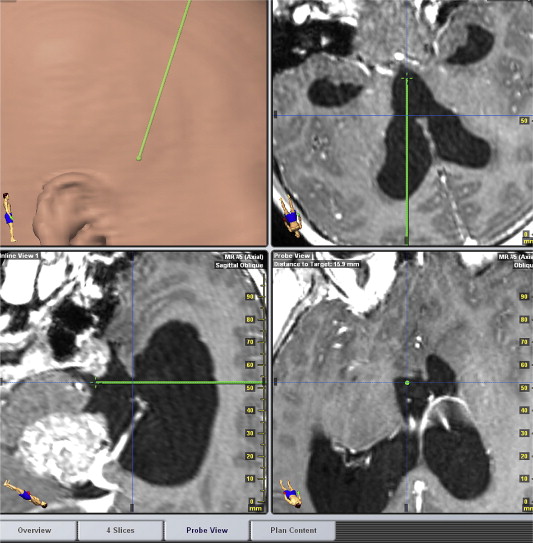
Figure 3. Measurement of the virtual displacement for endoscopic third ventriculostomy in neuronavigation software (probe view): Case 3, displacement = 0 mm. |
|
|
|
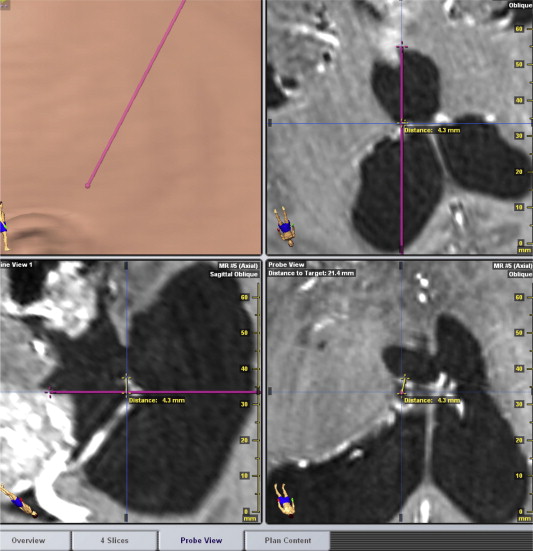
Figure 4. Measurement of the virtual displacement for endoscopic tumor biopsy in neuronavigation software (probe view): Case 3, displacement = 4.3 mm. |
3. Results
Between 2001 and 2008, 11 patients (8 males and 3 females, age: from 11 to 74 years, mean age: 29 years) had underwent ETV/ETB for third ventricle and pineal region tumors with obstructive hydrocephalus (Table 1). In one case, ETV was attempted only because the anatomy of the anterior part of the floor of the third ventricle was unclear because of the disseminated tumor (Case 1). The follow-up period was from 6 months to 7 years. All the cases were screened using MRI or CT imaging during the follow-up period. The majority of the tumors were in the posterior one-third of the third ventricle (Table 1, Fig. 1). The histological diagnosis revealed six germ cell tumors (5 germinomas and 1 immature teratoma), one atypical teratoid rhabdoid tumor (AT/RT), one pineocytoma, and two pilocytic astrocytomas. In one case, the pathological report revealed fibrous tissue only (Case 11).
| Case no. | Sex | Age at ETV/ETB (years) | Formal education (years) | Presentation | Tumor location in the third ventricle | Tumor size (height × width × AP, mm) | Tumor origin | Pathology | Hydrocephalus severity | Subsequent tumor treatment | Subsequent CSF shunt | Postoperative complication | Follow-up and outcome | MMSE (normal ≥ 25/30) | RBMT (normal ≥ 16/24) |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1a | F | 10 | 4 | Hypopituitorism | Mid. 1/3 | 25 × 11 × 10 | Suprasellar | Germinoma | Mild | CT, RT | No | None | 6 months | 30 | 24 |
| 2 | M | 11 | 5 | Vomiting, headache | Mid. 1/3 | 38 × 38 × 32 | Thalamus | Teratoma, immatured | Moderate | Craniotomy CT, RT | No | None | 1 year | 30 | 17 |
| 3 | M | 17 | 11 | Diplopia, unsteady gait, vomiting | Post. 1/3 | 43 × 29 × 37 | Pineal region | Germinoma | Severe | CT, RT | No | None | 18 months | 29 | 21 |
| 4 | M | 17 | 11 | Headache | Post. 1/3 | 36 × 33 × 35 | Pineal region | Pilocytic astrocytoma | Severe | Craniotomy CT, RT | No | None | 18 months | 27 | 20 |
| 5b | M | 19 | 12 | Headache, vomiting | Post. 1/3 | 12 × 11 × 20 | Pineal region | Germinoma | Moderate | CT, RT | No | Yes | 1 year | 30 | 24 |
| 6 | M | 20 | 12 | Headache, diplopia, vomiting, unsteady gait | Mid. 1/3 | 28 × 29 × 28 | Pineal region | AT/RT | Moderate | Craniotomy CT, RT | No | None | 2 years | 22 | 3 |
| 7 | M | 22 | 15 | Headache | Post. 1/3 | 22 × 26 × 30 | Pineal region | Germinoma | Severe | RT | No | None | 2 years | 29 | 22 |
| 8 | M | 24 | 12 | Headache | Post. 1/3 | 17 × 14 × 18 | Pineal region | Germinoma | Moderate | RT | No | None | 6 years | 29 | 19 |
| 9 | F | 35 | 12 | Headache | Post. 1/3 | 20 × 20 × 22 | Pineal region | Pilocytic astrocytoma | Moderate | Craniotomy CT, RT | No | None | 7 years | 25 | 18 |
| 10c | M | 41 | N/A | Headache | Post. 1/3 | 20 × 16 × 18 | Pineal region | Pineocytoma | Moderate | RT | No | None | 1 year | N/A | N/A |
| 11d | F | 74 | 6 | Unsteady gait | Post. 1/3 | 51 × 44 × 43 | Pineal region | Fiber tissue | Severe | Observation | No | None | 8 years | 10 | 0 |
AT/RT = atypical teratoid rhabdoid tumor; CSF = cerebrospinal fluid; CT = chemotherapy; ETB = endoscopic tumor biopsy; ETV = endoscopic third ventriculostomy; MMSE = Mini-Mental State Examination; RBMT = Rivermead Behavioral Memory Test; RT = radiotherapy; M = male; F = female.
a. Case 1: ETV was attempted only because the anatomy of the anterior part of the floor of the third ventricle was unclear due to the disseminated tumor.
b. Case 5: Intraventricular hemorrhage on Day 2 postoperatively after the removal of the external ventricular drain.
c. Case 10: The patient died 1 year later due to hemorrhagic stroke that was unrelated to the operation.
d. The tumor remained static in size, as observed in computed tomography imaging, at 7 years after ETB.
No CSF shunting was required subsequent to the EVT for all the cases. After the biopsy, four cases received craniotomy for tumor excision. Six cases received chemotherapy and/or radiotherapy without further operation. Case 11 with histological diagnosis of fibrous tissue was under observation. Follow-up imaging of this case at 8 years after the biopsy revealed that the tumor size remained static. None of the cases developed acute amnesia postoperatively. One patient (Case 5) had intraventricular hemorrhage on postoperative Day 2 after the removal of the ICP monitoring catheter. In this case, injury to the massa intermedia was observed by the endoscope during the biopsy procedure. The intraventricular hemorrhage was managed conservatively and the patient recovered well. One case died 1 year later due to hemorrhagic stroke unrelated to the ETV/ETB operation (Case 10).
The outcome was evaluated using MMSE and RBMT at 6 months to 7 years postoperatively. The results were within normal range in eight out of 10 patients. There were two cases (Cases 6 and 11) with low MMSE and RBMT scores, suggesting global impairment rather than selective memory deficit. Case 6 had a 3 × 3 × 4 cm AT/RT in the pineal region extending upward above the tentorium and toward the left side. Neurobehavioral Cognitive Status Examination (NCSE) was used to evaluate his cognitive status after ETV/ETB before the subsequent tumour excision.
The results were normal including the memory. Unfortunately, he encountered extensive intraventricular hemorrhage during the tumor excision via a left occipital interhemispheric transtentorial approach. On Glasgow Coma Scale examination, he was unable to obey commands until 17 days postoperatively. However, NCSE assessment at 7 weeks after the tumor excision showed impaired time orientation, naming, construction ability and memory. We believe that the extensive surgery in pineal region and surgical complications are the factors that contributed to the decline in his cognitive status. Case 11 is a woman who presented at 74 years of age. The MMSE and RBMT examinations were done at the age of 82 years, revealing dementia. Case 10 died 1 year after biopsy; therefore was excluded from the assessment.
The mean distances from the center of the burr hole were 17 mm (standard deviation (SD) = 6.8, range = 5–29 mm) anterior to the coronal suture and 30 mm (SD = 6.8, range = 18–37 mm) to midline. The mean angles were 58° (SD = 58, range = 50–63°) between the ETV trajectory and the OM line and 46° (SD = 3.9, range = 39–53°) between the ETB trajectory and the OM line. The mean angle between the two trajectories was 14° (SD = 4.2, range = 10–22°). The mean diameters of the FM were 5.7 mm (SD = 1.4, range = 4.4–8.8 mm) on the axial image, 7.8 mm (SD = 1.9, range = 5.5–12.4 mm) on the coronal image, and 5.6 mm (SD = 1.3, range = 4.3–7.7 mm) on the sagittal image. The mean virtual displacements of FM were 1.9 mm (SD = 2, range = 0–4.8 mm) for ETV and 2.4 mm (SD = 2.2, range = 0–5.5 mm) for ETB (Table 2). The maximum displacements were 4.8 mm anterior for ETV and 5.5 mm posterior for ETB.
| Case no. | FM size (mm) axial/coronal/sagittala | FM displacement (mm) | OM–ETV trajectory angle (°) | OM-ETB trajectory angle (°) | ETV–ETB trajectory angle (°) | Burr-hole location (mm) | ||
|---|---|---|---|---|---|---|---|---|
| Anterior | Posterior | From coronal suture | From midline | |||||
| 1 | 4.0/6.0/4.0 | 0 | 0 | 60 | 50 | 10 | 15 | 20 |
| 2 | 4.8/7.2/4.8 | 0 | 0 | 63 | 53 | 10 | 5 | 35 |
| 3 | 8.8/12.4/7.7 | 0 | 2.2 | 57 | 47 | 10 | 19 | 31 |
| 4 | 5.6/7.2/6.1 | 3.1 | 0 | 63 | 42 | 21 | 15 | 36 |
| 5 | 4.4/5.5/4.3 | 4.8 | 4.7 | 63 | 47 | 16 | 20 | 18 |
| 6 | 6.5/8.8/7.6 | 3.8 | 0 | 60 | 48 | 12 | 12 | 37 |
| 7 | 6.1/8.9/5.8 | 2.1 | 3.5 | 60 | 49 | 11 | 18 | 30 |
| 8 | 5/6.7/4.7 | 0 | 5.5 | 55 | 43 | 22 | 20 | 37 |
| 9 | 4.8/6.2/4.9 | 4.6 | 2.8 | 58 | 45 | 13 | 22 | 35 |
| 10 | 6.5/7.5/6.7 | 2.4 | 4.4 | 53 | 39 | 14 | 29 | 31 |
| 11 | 6.6/9/4.7 | 0 | 3.1 | 50 | 46 | 14 | 7 | 24 |
| Mean (SD) | 5.7(1.4)/7.8(1.9)/5.6(1.3) | 1.9 (2.0) | 2.4 (2.1) | 58.1 (4.3) | 46.3 (3.9) | 13.9 (4.2) | 16.6 (6.8) | 30.4 (6.8) |
ETB = endoscopic tumor biopsy; ETV = endoscopic third ventriculostomy; FM = foramen of Monro; OM = orbitomeatal line.
a. The MRI axial image is aligned to anterior-posterior commissure plane.
4. Discussion
The majority of patients with third ventricular and pineal region tumors present with acute symptoms of raised ICP because of obstructive hydrocephalus caused by the tumor. By contrast, tumors in this region are variable, and a substantial proportion of them are sensitive to chemotherapy or radiotherapy without the need of aggressive surgery. In 1994, Grunert, Perneczky, and Resch34 reported a series of 12 cases that had undergone endoscopic procedures through the FM. In 3 cases, either at the same time or in a second procedure, an ETV through the FM was performed in addition to ETV. Since then, many studies on ETV/ETB have been published for posterior third ventricle and pineal region tumors with obstructive hydrocephalus as initial management.1; 2; 3; 4; 5; 6; 7; 8; 9; 10; 11; 12; 13; 14; 15; 16; 17; 18; 19 ; 20 Through ETV/ETB, the following three objectives are achieved by one-step surgery: (1) CSF collection for tumor marker and cytological analysis; (2) definitive treatment of obstructive hydrocephalus by third ventriculostomy to relieve the raised ICP; (3) tumor biopsy for histological diagnosis, thus guiding the further treatment of the tumor.
However, working inside the third ventricle with the endoscope through the FM poses a risk of injury to the structures around the FM, especially the fornix resulting in memory deficit. Although the incidence of post-operative memory deficit is low, it persists throughout the literature, either in ETV/ETB or ETV alone series.2; 6; 21; 22; 23; 24; 25; 26; 27; 28; 30; 31 ; 32 For ETV alone, the postoperative complication of permanent memory disorders was 0.17%.24 For ETV/ETB, in 1997, Ferrer and colleagues reported that one out of four cases had short-term memory loss lasting for 2 weeks.2 The incidence of this complication became significantly lower in the later reports. In 2001, Pople and colleagues reported one case out of 18 cases with temporary amnesia postoperatively.6 In 2011, Mohanty and colleagues reported eight cases had forniceal contusion out of a series of 87 cases. Among these eight cases, the contusion were mild in seven and significant in one.28 Although the postoperative memory deficit in most of the reported cases was transient or mild, severe complication did occur sometimes. Benabarre and colleagues reported that a case developed memory impairment after ETV for slit ventricle syndrome.22 Longitudinal neuropsychological evaluations for more than 1 year revealed severe immediate memory deficit as well as difficulties in planning and consolidation of newly learned information. Damage to the right fornix was noted intraoperatively and confirmed by postoperative MRI. In another case report by Bonanni and colleagues, a patient developed deep amnesia and bulimia immediately after ETV and ETB.23 Psychological evaluation at 4 months postoperatively revealed normal IQ but poorly performed memory tasks. The memory deficit persisted when examined at 9 months and 1 year postoperatively. Postoperative MRI showed a complete section of the column of the right fornix, partial lesion of the right septal nuclei, and atrophy of mammillary bodies.
To avoid injury to the fornix and adjacent structures, two alternative methods have been adopted: [1] flexible scope2; 4; 6; 8; 9; 11; 12; 13; 14; 17; 34 ; 35; [2] two burr holes for different trajectories.4; 5; 6; 7; 10; 11; 16; 19 ; 20 The flexible scope has the advantages of wider visualization range and operation field than those of the rigid scope. However, it requires more experience to master its orientation. Its optic resolution is not as good as the rigid scope. In addition, the size of the biopsy specimen is smaller than that used in the rigid scope. The two burr-hole method is effective in avoiding the movement of the rigid neuroendoscope at the FM. However, it requires two trajectories, which will generate more trauma and increase chances of infection in the brain parenchyma. The anterior burr hole may also cause cosmetic disadvantages.7
Single burr-hole rigid ETV/ETB remain the choice of many neurosurgeons.1; 15; 18 ; 28 Four factors are important regarding the risk of damaging the fornix: (1) the size of FM; (2) the location of the tumor; (3) the trajectory, which is determined by the location of the burr hole; and (4) the size and view angle of the neuroendoscope. The chances of injury are higher when the foramen is smaller and the tumor is located more posteriorly. An optimal burr-hole location can minimize the movement of the endoscope at the level of the FM by a trajectory from the burr hole to the FM, where further anterior movement for ETV and posterior movement for ETB are equally distributed.
Many studies have addressed the importance of planning the trajectory.1; 6; 15; 18; 20; 28 ; 34 The principle is to have a trajectory from the burr hole to the FM where further anterior movement for ETV and posterior movement for ETB are equally distributed. However, equally distributing the endoscope movement only implies minimizing the entire range of the movement. It does not mean that the movement is within a safe range of the surrounding structure.
In our series with one burr hole using a 30° view and 3.5 × 5 mm diameter rigid scope, the virtual displacements of FM ranged from 0 mm to 4.8 mm for ETV and from 0 mm to 5.5 mm for ETB. The corresponding mean burr-hole location is 1.7 cm anterior to the coronal suture and 3 cm from the midline. Within this range, there was no injury to the fornix observed intraoperatively and no postoperative acute amnesia observed clinically. In the late postoperative stage, the results of MMSE and RBMT were within the normal range except for three cases because of individual reasons. Therefore, we conclude that the maximum displacements of 4.8 mm anteriorly for ETV and 5.5 mm posteriorly for ETB are likely to be a safe range.
However, we realize that the result of displacement measured virtually may not be exactly the same as the actual displacement during the operation. The difference can be due to the following reasons: [1] During the ETV and ETB operation, because the tilting forward or backward of the endoscope, the axle center of the endoscope may slightly shift forward and backward at the entry point of the burr hole. Thus, the actual displacement of FM may be less than the virtual measurement using the center of the burr hole as the axle center of endoscope tilting. For a burr hole with a diameter of 14 mm, the forward and backward shifting of the endoscope at the entry point will decrease the displacement to around 1.6 mm at the level of FM. [2] Using a 3.5 × 5.0 mm rigid endoscope for ETV and ETB, the virtual FM displacement should add 2.5 mm in addition to the measurement of trajectory line at the level of FM as the radius of the long axis of the endoscope. This measurement would be more close to actual displacement of FM if the ETV and ETB trajectories were measured using the intraoperative navigation images.
Knaus and colleagues18 studied the virtual endoscopic movement quantitatively using neuronavigation software. Among the 15 cases, 11 cases received ETV/ETB in the third ventricle. The ranges of tissue shift at the level of FM were 1.9 ± 2 mm for ETV and 2.4 ± 4 mm for ETB. These results are very similar to our results. By contrast, other than SD, the range of displacement is not provided in the study. We believe that the maximum value of tissue shift is also important as a consideration for a safe range of displacement.
In fact, we have analyzed the trajectory postoperatively and started the preoperative planning of the optimal trajectory for some of the cases before the retrospective review of the result. The choice of our burr-hole location is based on review of the literature as well as our own experience. We now routinely plan the optimal trajectory before the operation for ETV/ETB.
There was one case with the massa intermedia injured by the endoscope during ETB. In this case, the third ventricle was only mildly dilated, and the tumor was in the posterior one-third of the third ventricle. In the navigation software analysis, the massa intermedia was encountered by the ETB trajectory and the injury could be anticipated preoperatively. To avoid the injury, a two burr-hole method or flexible scope should be considered. Many studies have shown that the selection of single or two burr holes and rigid or flexible scope should be tailored according to an individual case as well as the surgeons experience.4; 6; 9; 10; 12; 14; 16; 17; 20; 34 ; 35 The result of our study will provide a useful reference for preoperative planning.
From this retrospective study conducted from 2001 to 2008, we conclude that measuring the possible range of FM preoperation will guide us to perform the surgery more safely. Therefore, we have used it as a safe reference to assist preoperative planning since then. We expect that further studies need to be conducted to prospectively validate this result.
We have also provided the size of FM in patients with obstructive hydrocephalus. The normal size of the FM is 5.4 + 1.2 mm × 2.7 + 0.9 mm.36 In our series with tumor in the posterior third ventricle and pineal region, the mean diameters are 5.7 mm (SD 1.4, range 4.4–8.8 mm) on axial image, 7.8 mm (SD 1.9, range 5.5–12.4 mm) on the coronal image, and 5.6 mm (SD 1.3, range 4.3–7.7 mm) on the sagittal image. We believe that this is also important information for reference.
5. Limitations of the study
Our study has several limitations: the series is small, and it is a retrospective study. There is no preoperative cognitive and memory assessment to compare with the postoperative result. One of the reasons is that many patients presented with raised ICP and impaired consciousness. Emergency operation was often required, and it was not feasible to conduct routine preoperative cognitive assessment.
The retrospective investigation of cognitive and memory function with MMSE and RBMT at 6 months or longer after the endoscopic procedure tend to overlook reversible impairment at the early postoperative stage, although clinically all patients did not develop acute amnesia. The function of fornix is correlated with not only cognitive function and memory, but also the processing speed and working memory. MMSE and RBMT are not sophisticated enough in identifying deficits in all these functions. We also realize that MMSE and RBMT are mainly used in the population in the age group of 16 years and above. In our series, there were two children with age 10 and 11 years respectively. These weaken the validity of the result.
6. Conclusion
In our series with one burr hole using a 30° view and 3.5 × 5 mm diameter rigid scope, the virtual displacements of FM ranged from 0 mm to 4.8 mm for ETV and from 0 mm to 5.5 mm for ETB. The corresponding mean burr-hole location is 1.7 cm anterior to the coronal suture and 3 cm from the midline. Within this range, there was no injury to the fornix observed intraoperatively and no postoperative acute amnesia observed clinically. In the late postoperative assessment using MMSE and RBMT, the results were within the normal range except for three cases because of individual reasons. Therefore, we conclude that maximum displacements of 4.8 mm anterior for ETV and 5.5 mm posterior for ETB are likely to be a safe range. We highly recommend optimal trajectory planning using neuronavigation software before surgery.
References
- 1 S. Robinson, A.R. Cohen; The role of neuroendoscopy in the treatment of pineal region tumors; Surg Neurol, 48 (1997), pp. 360–365 discussion 365–7
- 2 E. Ferrer, D. Santamarta, G. Garcia-Fructuoso, et al.; Neuroendoscopic management of pineal region tumours; Acta Neurochir (Wien), 139 (1997), pp. 12–20 discussion 20–1
- 3 R.G. Ellenbogen, L.E. Moores; Endoscopic management of a pineal and suprasellar germinoma with associated hydrocephalus: technical case report; Minim Invasive Neurosurg, 40 (1997), pp. 13–15 discussion 16
- 4 S. Oi, M. Kamio, T. Joki, et al.; Neuroendoscopic anatomy and surgery in pineal region tumors: role of neuroendoscopic procedure in the ‘minimally-invasive preferential’ management; J Neurooncol, 54 (2001), pp. 277–286
- 5 S. Oi, M. Shibata, J. Tominaga, et al.; Efficacy of neuroendoscopic procedures in minimally invasive preferential management of pineal region tumors: a prospective study; J Neurosurg, 93 (2000), pp. 245–253
- 6 I.K. Pople, T.C. Athanasiou, D.R. Sandeman, et al.; The role of endoscopic biopsy and third ventriculostomy in the management of pineal region tumours; Br J Neurosurg, 15 (2001), pp. 305–311
- 7 F. Veto, Z. Horvath, T. Doczi; Biportal endoscopic management of third ventricle tumors in patients with occlusive hydrocephalus: technical note; Neurosurgery, 40 (1997), pp. 871–875 discussion 875–877
- 8 D.C. Macarthur, N. Buxton, J. Punt, et al.; The role of neuroendoscopy in the management of brain tumours; Br J Neurosurg, 16 (2002), pp. 465–470
- 9 B. Yamini, D. Refai, C.M. Rubin, et al.; Initial endoscopic management of pineal region tumors and associated hydrocephalus: clinical series and literature review; J Neurosurg, 100 (2004), pp. 437–441
- 10 T. Yurtseven, Y. Ersahin, E. Demirtas, et al.; Neuroendoscopic biopsy for intraventricular tumors; Minim Invasive Neurosurg, 46 (2003), pp. 293–299
- 11 M.F. Chernov, S. Kamikawa, F. Yamane, et al.; Neurofiberscopic biopsy of tumors of the pineal region and posterior third ventricle: indications, technique, complications, and results; Neurosurgery, 59 (2006), pp. 267–277 discussion 267–277
- 12 B. Depreitere, N. Dasi, J. Rutka, et al.; Endoscopic biopsy for intraventricular tumors in children; J Neurosurg, 106 (2007), pp. 340–346
- 13 D.F. O'Brien, C. Hayhurst, B. Pizer, et al.; Outcomes in patients undergoing single-trajectory endoscopic third ventriculostomy and endoscopic biopsy for midline tumors presenting with obstructive hydrocephalus; J Neurosurg, 105 (2006), pp. 219–226
- 14 Y.Z. Al-Tamimi, D. Bhargava, S. Surash, et al.; Endoscopic biopsy during third ventriculostomy in paediatric pineal region tumours; Childs Nerv Syst, 24 (2008), pp. 1323–1326
- 15 S.V. Roopesh Kumar, A. Mohanty, V. Santosh, et al.; Endoscopic options in management of posterior third ventricular tumors; Childs Nerv Syst, 23 (2007), pp. 1135–1145
- 16 R. Prat, I. Galeano; Endoscopic biopsy of foramen of Monro and third ventricle lesions guided by frameless neuronavigation: usefulness and limitations; Clin Neurol Neurosurg, 111 (2009), pp. 579–582
- 17 E.S. Ahn, L. Goumnerova; Endoscopic biopsy of brain tumors in children: diagnostic success and utility in guiding treatment strategies; J Neurosurg Pediatr, 5 (2010), pp. 255–262
- 18 H. Knaus, S. Matthias, A. Koch, et al.; Single burr hole endoscopic biopsy with third ventriculostomy-measurements and computer-assisted planning; Childs Nerv Syst, 27 (2011), pp. 1233–1241
- 19 S. Chibbaro, F. Di Rocco, O. Makiese, et al.; Neuroendoscopic management of posterior third ventricle and pineal region tumors: technique, limitation, and possible complication avoidance; Neurosurg Rev, 35 (2012), pp. 331–340
- 20 P.F. Morgenstern, N. Osbun, T.H. Schwartz, et al.; Pineal region tumors: an optimal approach for simultaneous endoscopic third ventriculostomy and biopsy; Neurosurg Focus, 30 (2011), p. E3
- 21 J.J. Baskin, K.H. Manwaring, H.L. Rekate; Ventricular shunt removal: the ultimate treatment of the slit ventricle syndrome; J Neurosurg, 88 (1998), pp. 478–484
- 22 A. Benabarre, J. Ibanez, T. Boget, et al.; Neuropsychological and psychiatric complications in endoscopic third ventriculostomy: a clinical case report; J Neurol Neurosurg Psychiatry, 71 (2001), pp. 268–271
- 23 R. Bonanni, G.A. Carlesimo, C. Caltagirone; Amnesia following endoscopic third ventriculostomy: a single case study; Eur Neurol, 51 (2004), pp. 118–120
- 24 T. Bouras, S. Sgouros; Complications of endoscopic third ventriculostomy; J Neurosurg Pediatr, 7 (2011), pp. 643–649
- 25 J.U. Choi, D.S. Kim, S.H. Kim; Endoscopic surgery for obstructive hydrocephalus; Yonsei Med J, 40 (1999), pp. 600–607
- 26 N. Hayashi, H. Murai, S. Ishihara, et al.; Nationwide investigation of the current status of therapeutic neuroendoscopy for ventricular and paraventricular tumors in Japan; J Neurosurg, 115 (2011), pp. 1147–1157
- 27 D. Hellwig, J.A. Grotenhuis, W. Tirakotai, et al.; Endoscopic third ventriculostomy for obstructive hydrocephalus; Neurosurg Rev, 28 (2005), pp. 1–34 discussion 35–38
- 28 A. Mohanty, V. Santosh, B.I. Devi, et al.; Efficacy of simultaneous single-trajectory endoscopic tumor biopsy and endoscopic cerebrospinal fluid diversion procedures in intra- and paraventricular tumors; Neurosurg Focus, 30 (2011), p. E4
- 29 R.P. Naftel, G.T. Reed, A.V. Kulkarni, et al.; Evaluating the Childrens Hospital of Alabama endoscopic third ventriculostomy experience using the Endoscopic Third Ventriculostomy Success Score: an external validation study; J Neurosurg Pediatr, 8 (2011), pp. 494–501
- 30 H.W. Schroeder, W.R. Niendorf, M.R. Gaab; Complications of endoscopic third ventriculostomy; J Neurosurg, 96 (2002), pp. 1032–1040
- 31 C. Teo, S. Rahman, F.A. Boop, et al.; Complications of endoscopic neurosurgery; Childs Nerv Syst, 12 (1996), pp. 248–253 discussion 253
- 32 W. Tirakotai, D.M. Schulte, B.L. Bauer, et al.; Neuroendoscopic surgery of intracranial cysts in adults; Childs Nerv Syst, 20 (2004), pp. 842–851
- 33 B.A. Wilson, L. Clare, A.D. Baddeley; The Rivermead Behavioural Memory Test; (2nd ed.)Pearson Assessment, London (2003)
- 34 P. Grunert, A. Perneczky, K. Resch; Endoscopic procedures through the foramen interventriculare of Monro under stereotactical conditions; Minim Invasive Neurosurg, 37 (1994), pp. 2–8
- 35 P.A. Oppido, A. Fiorindi, L. Benvenuti, et al.; Neuroendoscopic biopsy of ventricular tumors: a multicentric experience; Neurosurg Focus, 30 (2011), p. E2
- 36 Z. Wang, X. Ding, J. Liao, et al.; Anatomical study on the structures of the third ventricle in neuroendoscopic surgery; Chinese J Clin Anat, 21 (2003), pp. 440–442
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?