Summary
Ureteric strictures are common and can be due to benign or malignant causes. Various surgical treatments can be used from minimally invasive endoscopic retrograde JJ stent insertion, balloon dilatation, ureterolithotomy, to open surgical exploration and repair. Memokath 051 stent is a metallic stent designed for long-term ureteral stenting in the management of ureteral strictures. The insertion of this device is usually a straightforward procedure performed endoscopically in a retrograde fashion via cystoscopy. However, this procedure can be difficult in complicated scenarios when the bladder has been removed with neoureteral reimplantations or high-grade strictures. Here, we report a case of Memokath stent insertion complicated by placement difficulties in a lady with ileal conduit due to previous ovarian cancer complicated by vesicovaginal fistula, who presented with malignant stricture of the ureteroileal anastomosis. We describe a simple yet effective antegrade technique to precisely reposition the malpositioned Memokath stent, along with illustrations.
Keywords
antegrade;Memokath stent;ureteroileal stricture
1. Introduction
Benign or malignant stricture formation at the ureteroileal junction postileal conduit diversion surgery is not uncommon. This may lead to hydronephrosis and consequently kidney loss. Stent placement offers a viable option in the management of ureteroileal junction stricture. However, long-term management of ureteral obstruction using double J stents is associated with well-recognized complications. To overcome this associated morbidity, permanent metallic stents such as Memokath 051 stent were introduced. We report our experience and the challenges encountered in stenting a gynecological related malignant stricture of the ureteroileal anastomosis, using Memokath 051 stent. We used an antegrade over-the-wire method to reposition the irretrievable malpositioned Memokath 051 stent.
2. Case report
A 64-year-old lady was diagnosed to have locally advanced ovarian carcinoma 5 years prior to presentation. She had undergone debulking surgery with colostomy as well as ileal conduit diversion surgery. She had also undergone two courses of chemotherapy, and was also treated with fulguration that entailed tissue ablation using high-frequency electric sparks. Despite the aggressive treatment of the disease, she developed tumor recurrence that caused right hydronephrosis and hydroureter. Endoscopic examination performed via the ileal conduit showed a 5-cm stricture of the ureteroileal junction caused by tumor infiltration. Balloon dilatation of the malignant stricture was performed, but there was still persistent contrast hold-up seen in the right collecting system. Subsequently, antegrade stenting of the malignant stricture was performed using a 6F double J stent. Unfortunately, there was recurrent distal migration of the double J stent into the conduit, requiring repeated repositioning of the stent under fluoroscopic guidance in the radiology department.
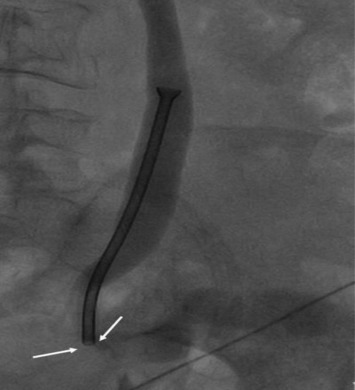
Subsequently, a decision was made by the urology team to replace the double J stent with a Memokath 051 stent (PNN A/S, Hornbaek, Denmark) endoscopically, via fluoroscopic guidance. The Memokath stent used was 10 cm in length with a 10.5 F inner lumen size and 20 F expanded lumen size at the funnel. The procedure was performed under general anesthesia, with the patient placed in a supine position, and with preoperative antibiotics coverage. A conduitoscopy was performed using a cystoscope, and it showed a tumor at the anastomotic site with the tip of the double J stent in situ. Biopsies of the tumor were performed, and the double J stent was partially pulled out. Subsequently, a guidewire was threaded up into the right pelvicalyceal system via the indwelling double J stent. After the removal of the double J stent and prior to the Memokath stent insertion, over the guidewire, the malignant stricture was dilated with serial ureteric dilators and Memokath sheath. However, because of the unfavorable angulation of the ureteroileal junction and inaccurate assessment of stricture length, the stent was suboptimally positioned. Following warm saline deployment, the distal end of the stent was noted to be lying above the stricture ( Fig. 1). Attempts to retrieve the stent failed, as the endoscope could not be passed across the malignant stricture.
|
|
|
Figure 1. Right nephrostogram showing a Memokath 051 stent in a dilated ureter. The distal tip of the stent is located just above the stricture (arrows). |
The opinion of an interventional radiologist was sought, and an attempt to salvage the Memokath 051 stent was initiated. A decision was made to reposition the stent via an antegrade approach. To gain access into the collecting system, the lower pole calyx of the right kidney was punctured under ultrasound guidance, and a 10-cm 9F sheath (Terumo, Terumo Interventional Systems, Somerset, New Jersey) was inserted. Under fluoroscopy guidance, through the sheath, and via a 5F Bern catheter (Boston Scientific, Boston Scientific Peripheral Interventions, Natick, Massachusetts), a 150-cm hydrophilic-coated guidewire (Terumo) was maneuvered intraluminally across the Memokath 051 stent, and from there on across the malignant stricture. The Terumo guidewire was then exchanged for a 150-cm stiff Amplatz guidewire (Boston Scientific), which was further advanced along the ileal conduit and through the ileostomy. The emerged guidewire was then retrieved and secured. Subsequently, a 25-cm 9F dilator (Dispomedica, Dispomedica GmbH, Hamburg, Germany), was passed antegradely, over the guidewire into the collecting system. The dilator was advanced until its tip became engaged with the upper end of the Memokath 051 stent. Then by pulling on both ends of the guidewire — thus applying traction on the guidewire — the dilator was further advanced or pushed manually, resulting in the forward movement of the stent. The stent was slowly pushed until it crossed the malignant stricture (Fig. 2). There was no need for instillation of cold saline in this process. The ensuing nephrostogram showed free flow of contrast from the right collecting system into the ileal conduit. At the end of procedure, a 6F pigtail nephrostomy tube was left in the pelvicalyceal system for temporary drainage. After a few days, the pigtail tube was blocked to allow complete internal drainage through the stent and was later removed after a contrast study performed 1 week later showed that the Memokath 051 stent was still in place and appeared to be functioning well (Fig. 3). The degree of hydronephrosis and hydroureter had also improved in the follow-up computed tomography examination of the abdomen and pelvis performed 6 weeks later.
|
|
|
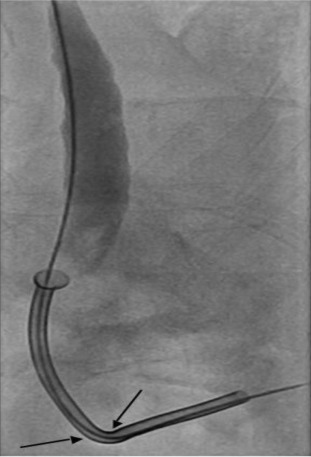
Figure 2. Successful repositioning of Memokath 051 stent across the stricture (arrows). |
|
|
|
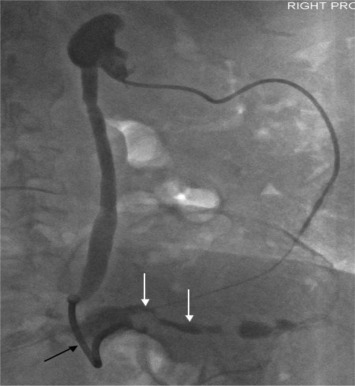
Figure 3. Nephrostogram performed a week after the procedure shows free flow of contrast into the ileal conduit. Memokath 051 stent is still in place. |
3. Discussion
Ileal conduit diversion may be complicated by benign or malignant stricture formation at the ureteroileal junction, which may subsequently lead to obstruction. This complication can be managed by dilating the stricture using a balloon or placing a double J stent across the stricture.1 A double J stent is a specially designed flexible plastic tube with a “pigtail” or curl at each end. In the case of ileal conduit ureteric stricture, the proximal curl end of the double J stent is placed in the renal pelvis and the other end is placed in the ileal conduit, acting as anchors to hold the stent in place. However, double J stent placement also has well-recognized complications such as stent migration, encrustation, sepsis, hematuria, pain, reflux, fragmentation, and dislodgement.2 As illustrated by this case, the patient had recurrent double J stent migration that required repeated repositioning of the stent under fluoroscopic guidance.
In an attempt to improve upon existing double J stents, metallic versions were introduced such as the thermo-expandable Memokath 051 stent. Memokath 051 stent is a nickel–titanium alloy spiral stent that has a thermosensitive “shape memory” property that allows easy stent insertion and removal.3 It is designed for long-term ureteral stenting in the management of malignant or benign ureteric strictures as well as an alternative for selected patients with noncurable ureteral obstruction.4 ; 5 Studies on the use of Memokath 051 stent for malignant and benign ureteric strictures revealed a low rate of encrustation (<10%) and stent migration (<20%).6 ; 7 If factors such as 3–6-monthly indwelling double J stent change and its associated comorbidities are taken into consideration, Memokath 051 stent offers a higher financial advantage and a better quality of life.3
In most of the patients, the insertion and removal of Memokath 051 stent are straightforward, taking only about 20–50 minutes.5 However, the procedure can be difficult or impossible in patients with retroperitoneal fibrosis and postirradiation strictures.6 In the presented case, the stent insertion was done retrogradely via the ileal conduit using a flexible cystoscope, and under fluoroscopic guidance. Technically, there were considerable difficulties and challenges encountered during the insertion. The difficulties arose because of the following reasons: first, acute angulation of the axis of the conduit and ureter; second, tumor at the ureteroileal anastomosis causing high resistance in advancing the stent up the ureter; and third, inaccurate assessment of the upper and lower ends of the stricture when using the fluoroscopic technique in positioning the stent. These factors had resulted in unsatisfactory positioning of the Memokath 051 stent in our case.
Usually, the migrated or poorly positioned Memokath 051 stent can be removed, repositioned, and replaced via flexible endoscopy.8 However, in this case, because the stent could not be retrieved endoscopically, repositioning was performed via a percutaneous antegrade approach. The most challenging part of the procedure was passing the guidewire into the stent and from there on traversing the tight malignant stricture. Fortunately, cannulation and passage of guidewire into the stent was facilitated by the stents funnel shaped tip. Theoretically, a balloon catheter could be used to advance the stent antegradely; however, we chose a rather unconventional device, a 25-cm 9F dilator, to push the stent because of its ideal length, shaft stiffness, tapered tip, and its significantly low cost. The dilators tapered tip and shaft stiffness provide optimal anchoring and stability needed to advance the stent. Because of the severe narrowing and acute angle of the anastomosis, advancing the stent would have been an arduous task if traction had not been applied to the guidewire. To avoid buckling at the stricture when advancing the stent, we applied tension to the guidewire by pulling it at both ends, enabling it to function as a monorail for the stent to be guided along. This technique improved the stricture angle, hence allowing a straighter path for the stent to be advanced over the guidewire. Although this “body floss” technique is not new in the field of radiology, its application in repositioning Memokath 051 stent has not been described in previous English-language literatures.
In summary, Memokath 051 stent is a cost-effective alternative to double J stent, which is prone to migration especially in the case of ureteroileal diversion. However, irretrievable malpositioned Memokath 051 stent, especially in malignant ureteroileal strictures, can be a problem to the urologists. As described in this case, we used a simple monorail technique to reposition the stent antegradely. This indeed provides a viable option in the management of Memokath 051 stent migration.
References
- 1 P. Pappas, K. Stravodimos, T. Kapetanakis, et al.; Ureterointestinal strictures following Bricker ileal conduit: management via a percutaneous approach; Int Urol Nephrol, 40 (2008), pp. 621–627
- 2 I. Singh; Indwelling JJ ureteral stents—a current perspective and review of literature; Ind J Surg, 65 (2003), pp. 405–412
- 3 D. Staios, I. Shergill, A. Thwaini, I. Junaid, N. Buchholz; The Memokath™ stent; Expert Rev Med Devices, 4 (2007), pp. 99–101
- 4 B. Kulkarni; A new thermo-expandable shape-memory nickel–titanium alloy stent for the management of ureteric strictures; BJU Int, 83 (1999), pp. 755–759
- 5 A. Papatsoris, N. Buchholz; A novel thermo-expandable ureteral metal stent for the minimally invasive management of ureteral strictures; J Endourol, 24 (2010), pp. 487–491
- 6 P. Klarskov, J. Nordling, J. Nielsen; Experience with Memokath 051 ureteral stent; Scand J Urol Nephrol, 39 (2005), pp. 169–172
- 7 M. Arya, H. Mostafid, H.R. Patel, M.J. Kellet, T. Philp; The self-expanding metallic ureteric stent in the long-term management of benign ureteric strictures; BJU Int, 88 (2001), pp. 339–342
- 8 K.A. Siddique, P. Zammit, N. Bafaloukas, S. Albanis, N.P. Buchholz; Repositioning and removal of an intra-renal migrated ureteric Memokath® stent; Urol Int, 77 (2006), pp. 297–300
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?