Highlights
- The estimated BAC of more than half of male and female lifetime hangover negative drinkers was below 80 mg%.
- Approximately 5% of drinkers registering estimated BAC’s beyond 80 mg% claim to be lifetime hangover negative.
- Biological and psychological hypotheses are proposed to explain why heavy drinkers may be lifetime hangover negative.
Abstract
Background
Resistance to alcohol hangover may be a risk factor for alcohol use disorder. Previous research to establish the prevalence of hangover resistance in a drinking population has either not used comparable intoxication levels or has considered hangover resistance over a limited time frame. The purpose of this study was to examine the prevalence of lifetime hangover negative (LHN) drinkers across comparable eBAC values ranging from 0 to 500 mg/dl.
Methods
Students at an eastern Canadian university were surveyed about their heaviest drinking episode in the past month and indicated whether they had ever experienced a hangover in their lifetime (LHN) and, if they had, the hangover severity they experienced the next day. eBACs were calculated and the percentage of LHN drinkers was computed at each 10 mg/dl eBAC increment from 0 to 500 mg/dl.
Results
Most LHN drinkers (58% female, 71% male) had an eBAC on their heaviest drinking occasion below 80 mg/dl. Above eBACs of 80 mg/dl, 5.8% of female and 5.1% of male drinkers were lifetime hangover negative.
Conclusions
The results suggest that only a small percentage of heavy drinkers lay claim to being lifetime hangover negative.
Keywords
Hangover;Alcohol;Prevalence;Hangover resistance;BAC
1. Introduction
Alcohol hangovers are the unpleasant symptoms experienced the day after alcohol consumption. These symptoms, such as headache, sleepiness, and concentration problems can last up to 20 h after drinking (Verster et al., 2010). The presence and severity of hangover symptoms differ however, both between and within drinkers (Penning, McKinney, & Verster, 2012). Furthermore, a number of drinkers report not experiencing hangovers (Howland et al., 2008 ; Howland et al., 2008).
Little research has been conducted to estimate the prevalence of drinkers who do not experience a hangover. The latter is important however, since it has been suggested that hangover resistant drinkers may be at increased risk of continuing harmful drinking behavior because they do not experience the day after punishment (Piasecki et al., 2010 ; Rohsenow et al., 2012). Cameron and French (2015) have also reported that lower perceptions of hangover severity the morning after drinking are associated with stronger beliefs that one is safe to drive; by extension, those drinkers who do not experience hangover symptoms may perceive themselves as safe to drive when they are not. Despite these beliefs, which are also reported by professional drivers (Verster, van der Maarel, McKinney, Olivier & de Haan, 2014), research has shown that driving is significantly impaired during alcohol hangover (Verster, Bervoets, et al., 2014).
Howland, Rohsenow and Edwards (2008) reviewed the little research that has provided data about hangover resistance and found that “despite variations in study design, populations, and time referents, there was striking consistency in the proportion of exposed populations who report not experiencing hangover” (p. 43). In summarizing data from survey and experimental studies, Howland, Rohsenow and Edwards reported that, on average, 23% of drinkers appear to be hangover resistant.
There are, however, several limitations in the studies reviewed by Howland, Rohsenow and Edwards (2008). First, in experimental studies, generally a pre-set dosage of alcohol was consumed, within a set short period of time, to achieve a desired peak blood alcohol concentration (BAC). Given ethical constraints, this peak BAC was generally around 100–120 mg/dl (e.g., Chapman, 1970 ; Howland et al., 2008), which is lower than observed in real life drinking sessions (Hesse and Tutenges, 2010; Jones, 2010 ; Verster et al., 2013). Second, it is unclear what is meant by the term ‘hangover resistance’ from studies in which the time frame under consideration is limited. There is a difference between having experienced a hangover in ones lifetime (lifetime hangover positive; LHP) but not experiencing one following a particular drinking episode or within a limited time period (e.g. 1, 2, 5 years) and never having experienced a hangover across a lifetime of drinking (lifetime hangover negative; LHN). These two types of hangover resistance were not differentiated in the studies reviewed by Howland, Rohsenow and Edwards (2008) but are important, as the absence of negative after-effects of alcohol may differentially affect the frequency and volume of future alcohol consumption in LHN and LHP drinkers (Huntley et al., 2015), which could, hypothetically, differentially alter the risk for future alcohol use disorders.
Separating LHN from LHP drinkers can be easily achieved by asking participants whether or not they have ever experienced a hangover in their lifetime. However, in estimating the prevalence of lifetime hangover resistance, this simple binary is insufficient as it does not take level of intoxication into account. For example, using a large Dutch survey, Verster et al. (2013) constructed a frequency distribution of the number of past-year hangover resistant drinkers relative to the total number of drinkers at each 10 mg/dl (mg%) estimated BAC (eBAC) value ranging from 0 to 500 mg%. In addition, they computed a cumulative frequency distribution of the proportion of past-year hangover resistant drinkers above and below each 10 mg% eBAC increment to examine how past-year hangover resistant drinkers were distributed across the eBAC spectrum. In total, 32.1% of the drinkers in their study reported not experiencing a hangover in the past year, however more than half of them were distributed at eBAC levels below 80 mg%, the threshold used in a number of countries to determine impaired driving. For drinkers whose eBAC met or exceeded 200 mg%, only 8.1% reported not experiencing a hangover in the past year—substantially lower than the 23% reported by Howland, Rohsenow and Edwards (2008).
Although Verster et al. (2013) were able to show how hangover resistant drinkers were distributed across the continuum of eBAC values, hangover resistance over a 12 month period is not equivalent to hangover resistance over a lifetime of drinking (LHN). Therefore, the purpose of the present study was to examine the frequency distribution and cumulative frequency of LHN drinkers across a continuum of eBAC values ranging from 0 to 500 mg% in a population of university drinkers. Based on Verster et al. we hypothesized that half or more of the LHN drinkers would be distributed at eBAC levels below 80 mg%. Furthermore, as it is conceivable that a proportion of the past-year hangover resistant drinkers in the frequency distribution created by Verster et al. may have experienced a hangover at some point in their lifetime, it was hypothesized that the cumulative frequency of LHN drinkers above 80 and 200 mg% in the present study would be lower than that reported by Verster et al. These aims were achieved through the use of survey data collected from students at an eastern Canadian university.
2. Materials and methods
2.1. Subjects & procedure
As part of an ongoing larger project examining monthly patterns of alcohol consumption and alcohol related harms in university students, full-time students at Acadia University (an eastern Canadian university) were invited by email to anonymously complete an online drinking survey about their experiences involving alcohol. The Acadia University Research Ethics Board provided ethical approval for the project. During each three month long academic term, the full-time student population was divided into three groups stratified on the basis of sex, year of study, and degree program. A day following the end of each month within an academic term, one of these groups was sent an email inviting them to complete an anonymous drinking survey online so that, by the end of the third month of each academic term, each full-time student had received an invitation to complete the survey. The email provided students with a hyperlink to the survey URL. Students provided informed consent by clicking on the URL hyperlink, which took them to the survey website. Twenty-four hours following the invitation email students received a reminder email, and 24 h following the reminder email students received a third email thanking those who had completed the survey and reminding students to complete the survey for a final time. The survey was closed at the end of the day following the final reminder. Students who completed the survey had the option to enter into a draw for one of two $50 gift certificates by clicking on a URL hyperlink that directed them to a separate website.
2.2. Survey
The survey asked students about their experiences involving alcohol during the previous month, including details about their typical pattern of drinking (frequency, quantity & duration) and their highest volume drinking episode (quantity, duration & hangover severity). Data for the heaviest rather than a typical drinking episode was chosen as the unit of analysis in the present study because we wanted to know the highest BAC after which LHN drinkers report not experiencing a hangover, as claims of lifetime hangover resistance gain credibility at higher levels of intoxication. Regarding students' heaviest drinking episode, they were asked, “In the past month, what is the largest number of drinks you recall consuming?” and “On that day, over how many hours did you drink?” Students were then asked to rate their hangover severity the next day on a single item hangover question (Rohsenow et al., 2007) that asked, “How would you rate your hangover the next day?” Seven response options were provided: I have never experienced a hangover, 0 (Absent), 1 (Mild), 2, 3 (Moderate), 4, and 5 (Severe); students selecting ‘I have never experienced a hangover’ were labelled LHN whereas students selecting ‘0 (Absent)’ and students with a hangover severity rating greater than zero were labelled LHP.
Demographic questions pertinent to the present research included students' sex, age, height and weight. Information about height and weight was obtained to compute estimated blood alcohol concentration (eBAC). eBAC (in mg/dl, or mg%) was computed separately for males and females using the formulas provided by Seidl, Jensen and Alt (2000, p. 74). For males, eBAC was obtained by the formula: 1000 ∗ ((#drinks ∗ 13.6 g alcohol) / (weight in kg ∗ (0.31608 − (0.004821 ∗ weight in kg) + (0.004632 ∗ height in cm)) / 10 − (#hours ∗ 0.017)); for females, eBAC was obtained with the formula: 1000 ∗ ((#drinks ∗ 13.6 g alcohol) / (weight in kg ∗ (0.31223 − (0.006446 ∗ weight in kg) + (0.004466 ∗ height in cm)) / 10 − (#hours ∗ 0.017)). In each formula, the number of drinks was multiplied by 13.6 as this value corresponds to the volume of alcohol (in grams) contained in a standard drink in Canada. An elimination rate of 0.017 g% per hour was selected as it represents the midpoint in Jones' (2010) suggested range of elimination rates of alcohol from blood. Each formula was multiplied by 1000 to convert BAC values from g/dl to mg/dl. eBAC values represent blood alcohol concentrations for the time point at which students reported their drinking episode had ended. Thus, an eBAC of zero means that a drinking episode was sufficiently long for the alcohol a student had consumed to be metabolized. For inclusion in the analyses, students were required to have provided data about their heaviest drinking episode (quantity, duration & hangover severity), sex, height and weight as well as background information, including their age and their typical drinking pattern (frequency, quantity & duration). Missing data resulted in case wise deletion.
2.3. Statistical analysis
Data collected over six academic terms from September 2013 to March 2016 were combined to produce a dataset with the greatest number of observations of LHN drinkers. Computed eBAC values from 0 to 300 mg% were organized into 10 mg% increments by combining values within a range of − 5 and + 4.9 mg% around each increment (e.g., an eBAC of 80 mg% included computed eBACs within the range of 75 to 84.9 mg%). eBAC values from 300 to 500 mg% were organized into 50 mg% increments due to the increasing scarcity of data points beyond 300 mg%. A frequency distribution was created by dividing the number of LHN drinkers by the total number of drinkers at each eBAC increment from 0 to 500 mg%. A cumulative frequency distribution was constructed to examine the proportion of LHN relative to the total number of drinkers above each eBAC increment.
3. Results
Over the six academic terms, 5540 of 20,887 students completed the anonymous online survey for an overall response rate of 26.5% (female response rate = 33.5%; male response rate = 16.8%). A two-tailed binomial test showed that the proportion of female v male respondents (4060 v 1480 or 73.3% v 26.7%) differed significantly from the student population (58% female v 42% male), causing the sample to be overrepresented by female and underrepresented by male responses, z = 23.16, p < 0.0001 (Siegel & Castellan, 1988). Therefore, female and male data were analyzed separately. Data provided by nondrinkers were removed, as were observations with missing data. The final samples included observations from 3046 female (95% confidence interval = 1.25%) and 1158 male drinkers (95% confidence interval = 2.32%).
A general description of the typical drinking pattern within female and male samples is provided in Table 1.
| Female | Male | |||
|---|---|---|---|---|
| M | SD | M | SD | |
| Age | 20.0 | 1.8 | 20.2 | 2.0 |
| Height (cm) | 166.3 | 7.4 | 180.9 | 6.9 |
| Weight (kg) | 64.7 | 12.7 | 81.6 | 16.5 |
| Typical weekly drinking frequency (days/week) | 1.3 | 0.9 | 1.7 | 1.2 |
| Typical weekly alcohol consumption (g/week) | 83.2 | 79.6 | 154.7 | 151.7 |
| Typical drinking day | ||||
| Alcohol consumed (g) | 60.7 | 30.6 | 85.8 | 48.8 |
| Consumption duration (h) | 3.66 | 1.80 | 4.37 | 2.15 |
| eBAC (mg/dl) | 90 | 66 | 71 | 60 |
| Heaviest drinking day | ||||
| Alcohol consumed (g) | 89.1 | 46.3 | 132.8 | 67.7 |
| Consumption duration (h) | 4.58 | 2.52 | 5.56 | 3.11 |
| eBAC (mg/dl) | 144 | 96 | 124 | 83 |
| Hangover Severity rating | 1.61 | 1.52 | 1.56 | 1.48 |
Note: Alcohol is expressed in grams rather than standard drinks because of the diversity of standard drink sizes worldwide (e.g., Canada 13.6 g, U.S.A. 14 g, the Netherlands 10 g; see Kalinowski & Humphreys, 2016).
The cumulative frequency of LHN drinkers at the eBAC increments of 50 mg%, 80 mg%, 110 mg% and 200 mg% are shown in Table 2. These eBAC values correspond to the two most common internationally recognized legal limits establishing impaired driving, the commonly held peak BAC needed to develop a hangover (Rohsenow et al., 2012 ; Verster et al., 2010), and the highest eBAC value described by Verster et al. (2013).
| eBAC (mg%) | Female LHN drinkers | Male LHN drinkers |
|---|---|---|
| 50 | 45.5% (135/295) | 63.9% (85/133) |
| 80 | 58.0% (171/295) | 71.4% (95/133) |
| 110 | 69.8% (206/295) | 81.9% (109/133) |
| 200 | 89.8% (265/295) | 92.5% (123/133) |
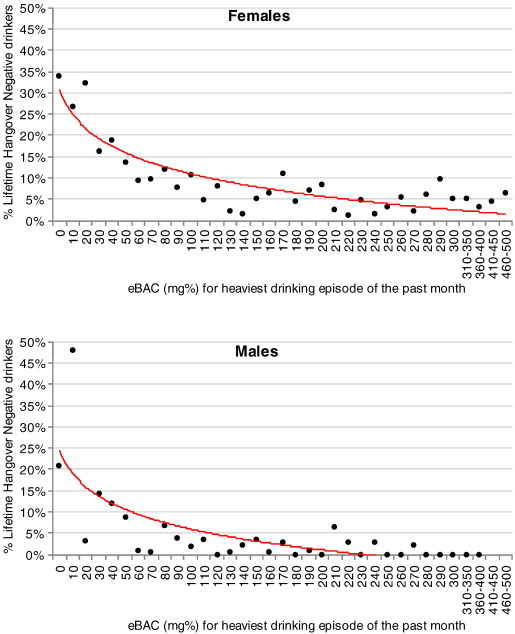
The frequency distributions for female and male LHN drinkers across the eBAC continuum are shown in Fig. 1. An independent samples t-test for unequal variances showed that the eBAC values were significantly higher in the female than male sample, t (2389.02) = 6.38, p < 0.001, signaling that eBACs in the female sample were distributed over higher values than in the male sample (see Table 1). The data show that a significantly greater percentage of female and male LHN drinkers fell within eBAC increments below (female = 58%; male = 71.4%) than above 80 mg% (female = 42%; male = 28.6%), χ2(1) = 7.65, p < 0.01 (Siegel & Castellan, 1988).
|
|
|
Fig. 1. Number of lifetime hangover negative drinkers relative to the number of drinkers (expressed as a %) within each eBAC increment from 0 to 500 mg of alcohol per 100 ml of blood (mg%). |
When considering only the subset of drinkers with eBACs above 80 mg%, the proportion of this subset who claimed to be LHN was 5.8% (124/2140) of female and 5.1% (38/739) of male drinkers; when the smaller subset of drinkers with eBACs above 200 mg% was considered, the prevalence of lifetime hangover resistance was 4.2% (30/722) and 4.6% (10/216) for female and male drinkers, respectively.
4. Discussion
Within the full sample of drinkers, over half of male and female LHN drinkers were distributed at eBAC increments below 80 mg%, which supports the first hypothesis. Furthermore, consistent with Verster et al. (2013), only a small percentage of LHN drinkers were distributed at eBACs > 200 mg%. These results support and extend the findings of Verster et al. by examining LHN vs. past-year hangover negative drinkers, and by providing separate distribution profiles for females and males. Combined, the results of both studies show that the majority of hangover negative drinkers (both past-year and lifetime) cluster at low eBACs, with a small minority of hangover negative drinkers distributing themselves at high eBACs.
Whereas less than half of LHN drinkers were distributed across eBAC increments above 80 mg%, the small number of LHN v total drinkers at comparable levels of intoxication, i.e., at eBAC increments > 80 mg%, showed that few drinkers at high eBACs are lifetime hangover negative. Compared to the frequency distribution of past-year hangover resistant drinkers across eBACs from 0 to 500 mg% reported by Verster et al. (2013), the prevalence of lifetime hangover resistance in the present study was consistently lower, which supports our second hypothesis. Furthermore, Verster et al. reported that above eBACs of 200 mg%, 8.1% of drinkers claimed not to have had a hangover in the past year; in the present study we found 4.2% and 4.6% of female and male drinkers, respectively, to be LHN beyond this level. One explanation for the reduced prevalence of LHN drinkers in the present study is that some proportion of the past-year hangover resistant drinkers in the Verster et al. study may have experienced a hangover at some point in their drinking history so that the prevalence of past-year hangover resistance in their study would have included some combination of LHN and LHP drinkers. A second explanation may be a difference in sampling methods. In the present study a number of datasets were combined in order to maximize the number of observations of lifetime hangover resistance; Verster et al.s dataset was made up of independent observations. A dataset containing a mixture of independent and dependent observations may introduce sampling bias compared to a dataset made up entirely of independent observations.
Nonetheless, expanding the range of eBAC values over which hangover resistance is considered reveals a much smaller proportion of the drinking population who have never experienced the negative after-effects of heavy alcohol consumption than reported by Howland, Rohsenow and Edwards (2008). Interestingly, a calculation of undifferentiated hangover resistance (LHN & LHP combined) for eBAC increments spanning 100–120 mg% to replicate the target BAC range reported by Howland, Rohsenow, Allensworth-Davies et al. (2008) found that, in our dataset, 25.7% (105/409) of female and 30.1% (41/136) of male drinkers within this narrow eBAC range reported not experiencing a hangover. Compared to the hangover resistance rate of 23% reported by Howland, Rohsenow, Allensworth-Davies et al., the lower prevalence rate reported in the present study and by Verster et al. (2013) may simply be a function of separating LHN from LHP drinkers, and expanding the eBAC range being considered.
Knowing with greater precision the proportion of drinkers who are lifetime hangover negative is important because elucidating the characteristics of this small subset of drinkers versus those at equivalent intoxication levels who do have hangovers may help the field in its search to understand the pathology of alcohol hangover. There is little scientific research into hangover immune drinkers. This is, however, a strange group, as they do not suffer from hangover symptoms that the vast majority of drinkers do, despite consuming similar large quantities of alcohol.
Having established that the prevalence of lifetime hangover resistance is small at eBACs above 80 mg%, the question can be asked, why have some heavy drinkers never experienced a hangover? We forward two hypotheses. The first hypothesis we identify as a biological hypothesis, which states that perhaps the biological processes involved in the metabolism of alcohol in LHN drinkers are different than in drinkers who experience hangovers, and this difference prevents LHN drinkers from experiencing hangover symptoms. Examining the physiological mechanisms at play in returning the body to equilibrium following heavy consumption of alcohol in LHN v LHP drinkers may shed light into the biology of hangover. The second hypothesis we identify as a psychological hypothesis, which suggests that the biological processes involved in the metabolism of alcohol are the same for all drinkers but that LHN drinkers are simply less sensitive to their effects. Examining the psychological experience associated with the bodys return to equilibrium following heavy consumption of alcohol in LHN v LHP drinkers may shed light into the psychology of hangover, especially as it relates to the propensity to drive when it may not be safe to do so ( Cameron & French, 2015). Schuckit (1998) has shown that both biological and psychological processes come into play for drinkers who are less sensitive to the acute intoxicating effects of alcohol. Low level of response to alcohol is related to heavier drinking and is a good predictor of developing a subsequent alcohol use disorder (Schuckit & Smith, 2013), especially in drinkers with a family history of alcohol problems. However, Schuckit and colleagues did not examine how low level of response to alcohol might extend to hangover. Rohsenow et al. (2012) found that hangover insensitivity correlated with low level of response to alcohol during an alcohol challenge to a target BAC of 120 mg% and suggested that “these two types of insensitivity are related” (p. 273). As hangover insensitivity is also associated with consuming higher volumes of alcohol, at least in the short term (Huntley et al., 2015), the relationship between lifetime hangover resistance—the ultimate in hangover insensitivity—and risk for developing alcohol use disorders awaits future study.
The current study has some limitations. First, the data were self-reported. This may introduce the well-known limitations of survey research in general, such as recall bias (Davis et al., 2010 ; Del Boca and Darkes, 2003). The eBAC levels presented in this study are based on self-reports of the quantity of alcohol consumed and the duration of drinking occasions whose relationship to actual quantity and duration are unknown. However, the self-reported data are consistent across the six academic terms that were combined to form the dataset for the present study; the similarity of reporting suggests evidence of a reliable phenomenon. Second, the data are not drawn from a random sample but rather from students willing to complete the survey. As such, the proportion of the female student population willing to complete the survey (33.5%) was essentially double the proportion of the male student population (16.5%). Combined with a campus population characterized by a larger proportion of females than males, our dataset is over represented by female respondents. To minimize gender bias the data were analyzed separately for females and males; however, the low response rate of males suggests that the male sample may not accurately represent the population from which it came and should be viewed with caution. Third, the eBAC data are based on drinkers' single heaviest drinking episode during the previous month. The extent to which this drinking occasion represents individuals' lifetime heaviest drinking episode is unknown. A more accurate account of lifetime hangover resistance could be obtained if it were based on drinkers' heaviest lifetime drinking occasion. Fourth, our dataset was limited to young drinkers in a university setting. Whether hangover resistance persists in the LHN drinkers as they age is not known. Longitudinal research that tracks hangover resistance within LHN individuals over time and across a variety of BACs would further clarify the nature and extent of hangover resistance.
Limitations notwithstanding, the ability to separate LHN from LHP drinkers at comparable and especially high levels of intoxication in the present study represents a significant advancement within hangover research. Whereas Howland, Rohsenow and Edwards (2008) reported that, on average, 23% of heavy drinkers were resistant to hangover, the present study—while supporting this finding—has shown that when examined across a wider range of BAC values in only those drinkers who have never experienced a hangover in their lifetime, the prevalence of lifetime hangover resistance was approximately 5%.
Disclosure of interests
Joris Verster has received grants/research support from the Dutch Ministry of Infrastructure and the Environment, Janssen Research and Development, Nutricia, Takeda, and Red Bull and has acted as a consultant for the Canadian Beverage Association, Centraal Bureau Drogisterijbedrijven, Coleman Frost, Danone, Deenox, Eisai, Janssen, Jazz, Purdue, Red Bull, Sanofi-Aventis, Sen-Jam Pharmaceutical, Sepracor, Takeda, Transcept, Trimbos Institute, and Vital Beverages.
The other authors have no conflicts of interest to disclose.
References
- Cameron and French, 2015 E. Cameron, D.P. French; Predicting perceived safety to drive the morning after drinking: The importance of hangover symptoms; Drug and Alcohol Review (2015) https://doi.org/10.1111/dar.12311
- Chapman, 1970 L.F. Chapman; Experimental induction of hangover; Quarterly Journal of Studies on Alcohol, 5 (Supplement) (1970), pp. 67–86
- Davis et al., 2010 C.G. Davis, J. Thake, V. Vilhena; Social desirability biases in self-reported alcohol consumption and harms; Addictive Behaviors, 35 (2010), pp. 302–311 https://doi.org/10.1016/j.addbeh.2009.11.001
- Del Boca and Darkes, 2003 K. Del Boca, J. Darkes; The validity of self-reports of alcohol consumption: State of the science and challenges for research; Addiction, 98 (s2) (2003), pp. 1–12 https://doi.org/10.1046/j.1359-6357.2003.00586.x
- Hesse and Tutenges, 2010 M. Hesse, S. Tutenges; Predictors of alcohol hangover during a week of heavy drinking on holiday; Addiction, 105 (2010), pp. 476–483 https://doi.org/10.1111/j.1360-0443.2009.02816.x
- Howland et al., 2008 J. Howland, D.J. Rohsenow, D. Allensworth-Davies, J. Greece, A. Almeida, S.J. Minsky, ... J. Hermos; The incidence and severity of hangover the morning after moderate alcohol intoxication; Addiction, 103 (2008), pp. 758–765 https://doi.org/10.1111/j.1360-0443.2008.02181.x
- Howland et al., 2008 J. Howland, D.J. Rohsenow, E.M. Edwards; Are some drinkers resistant to hangover: A literature review; Current Drug Abuse Reviews, 1 (2008), pp. 42–46 https://doi.org/10.2174/1874473710801010042
- Huntley et al., 2015 G. Huntley, H. Treloar, A. Blanchard, P.M. Monti, K.B. Carey, D.J. Rohsenow, R. Miranda Jr.; An event-level investigation of hangovers' relationship to age and drinking; Experimental and Clinical Psychopharmacology, 23 (2015), pp. 314–323 https://doi.org/10.1037/pha0000037
- Jones, 2010 A.W. Jones; Evidence-based survey of the elimination rates of ethanol from blood with applications in forensic casework; Forensic Science International, 200 (2010), pp. 1–20 https://doi.org/10.1016/j.forsciint.2010.02.021
- Kalinowski and Humphreys, 2016 A. Kalinowski, K. Humphreys; Governmental standard drink definitions and low-risk alcohol consumption guidelines in 37 countries; Addiction, 111 (2016), pp. 1293–1298 https://doi.org/10.11111/add.13341
- Penning et al., 2012 R. Penning, A. McKinney, J.C. Verster; Alcohol hangover symptoms and their contribution to overall hangover severity; Alcohol and Alcoholism, 47 (2012), pp. 248–252 https://doi.org/10.1093/alcalc/ags029
- Piasecki et al., 2010 T.M. Piasecki, B.M. Robertson, A.J. Epler; Hangover and risk for alcohol use disorders: Existing evidence and potential mechanisms; Current Drug Abuse Reviews, 3 (2010), pp. 92–102 https://doi.org/10.2174/1874473711003020092
- Rohsenow et al., 2007 D.J. Rohsenow, J. Howland, S.J. Minsky, J. Greece, A. Almeida, T. Roehrs; The acute hangover scale: A new measure of immediate hangover symptoms; Addictive Behaviors, 32 (2007), pp. 1314–1320 https://doi.org/10.1016/j.addbeh.2006.10.001
- Rohsenow et al., 2012 D.J. Rohsenow, J. Howland, M. Winter, C.A. Bliss, C.A. Littlefield, T.C. Heeren, T.V. Calise; Hangover sensitivity after controlled alcohol administration as predictor of post-college drinking; Journal of Abnormal Psychology, 121 (2012), pp. 270–275 https://doi.org/10.1037/a0024706
- Schuckit, 1998 M.A. Schuckit; Biological, psychological and environmental predictors of the alcoholism risk: A longitudinal study; Journal of Studies on Alcohol, 59 (1998), pp. 485–494 https://doi.org/10.15288/jsa.1998.59.485
- Schuckit and Smith, 2013 M.A. Schuckit, T.L. Smith; Stability of scores and correlations with drinking behaviors over 15 years for the self-report of the effects of alcohol questionnaire; Drug and Alcohol Dependence, 128 (2013), pp. 194–199 https://doi.org/10.1016/j.drugalcdep.2012.08.022
- Seidl et al., 2000 S. Seidl, U. Jensen, A. Alt; The calculation of blood ethanol concentrations in males and females; International Journal of Legal Medicine, 114 (2000), pp. 71–77 https://doi.org/10.1007/s004140000154
- Siegel and Castellan, 1988 S. Siegel, N.J. Castellan Jr.; Nonparametric statistics for the behavioral sciences; (2nd ed.)McGraw-Hill, New York, NY (1988)
- Verster et al., 2010 J.C. Verster, R. Stephens, R. Penning, D.J. Rohsenow, J. McGeary, D. Levy, ... on behalf of the Alcohol Hangover Research Group; The Alcohol Hangover Research Group consensus statement on best practice in alcohol hangover research; Current Drug Abuse Reviews, 3 (2010), pp. 116–127 https://doi.org/10.2174/1874473711003020116
- Verster et al., 2013 J.C. Verster, S. de Klerk, A.C. Bervoets, L.D. Kruisselbrink; Can hangover immunity be really claimed; Current Drug Abuse Reviews, 6 (2013), pp. 253–254 https://doi.org/10.2174/187447370604140616120736
- Verster et al., 2014 J.C. Verster, A.C. Bervoets, S. de Klerk, R.A. Vreman, B. Olivier, T. Roth, K.A. Brookhuis; Effects of alcohol hangover on simulated highway driving performance; Psychopharmacology, 231 (2014), pp. 2999–3008 https://doi.org/10.1007/s00213-014-3474-9
- Verster et al., 2014 J.C. Verster, M. van der Maarel, A. McKinney, B. Olivier, L. de Haan; Driving during alcohol hangover among Dutch professional truck drivers; Traffic Injury Prevention, 15 (2014), pp. 434–438 https://doi.org/10.1080/15389588.2013.833329
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?