Abstract
This study investigated the combined efficacy of docosahexaenoic acid (DHA) and Panax ginseng extract for treating Alzheimer's disease (AD). Single-target therapies aimed at clearing amyloid-beta (Aβ) have been largely unsuccessful, shifting attention toward multi-target approaches; among the most promising are DHA and Panax ginseng. Although DHA shows strong efficacy in AD prevention, once neurodegeneration has taken hold, blood-brain barrier (BBB) damage impairs its transport into the brain. Ginseng may counteract this by strengthening the BBB through the Wnt/β-catenin (BAR-1 ortholog in Caenorhabditis elegans) pathway and preventing DHA oxidation via its antioxidant properties, thereby enhancing delivery where it exerts neuroprotective effects. Based on these complementary mechanisms, the present study evaluated whether combined treatment confers benefits beyond either treatment alone using CL2355 (transgenic AD model) and N2 (wild-type) Caenorhabditis elegans. Five experimental groups were compared: two untreated controls (wild-type; AD model) and three AD model groups receiving DHA (5 mM), ginsenoside (10 μg/mL), or both. Treatment effects were assessed through paralysis (mobility), chemotaxis (neurological function), and population growth (reproduction) assays. The combined treatment reduced paralysis by 40% relative to untreated AD worms and 10% beyond either treatment alone, while significantly improving chemotactic function (p<0.01). These results suggest combined treatment holds potential as a multi-target therapeutic strategy, possibly by enhancing DHA absorption by the neurological system and/or targeting AD pathology through compounding mechanisms, though this study cannot distinguish between the two. These promising findings warrant further research using higher-order AD models or assays measuring nervous system DHA absorption.
1.0 Introduction
Alzheimer’s disease (AD) is a neurodegenerative disease and the leading cause of dementia, accounting for 75% of cases [1]. As of 2014, AD affects more than 35.6 million people worldwide, a number estimated to quadruple by 2050. AD impairs language recognition and cognitive function by damaging the neocortex and hippocampus, reducing life expectancy, and increasing physical impairment in the elderly [2, 1]. Although the etiology of AD remains incompletely understood, current research is primarily based on a theory attributing its cause to abnormal accumulation of amyloid-beta (Aβ) aggregates, which results in neuroinflammation and subsequent neurodegeneration [3, 4, 5, 6].
Currently, FDA-approved AD treatments target cholinergic and glutamatergic systems [7]. Cholinesterase inhibitors (CHEIs) reduce the breakdown of acetylcholine but are unable to halt disease progression or reverse damage [2]. NMDA receptor antagonists represent another therapeutic class. NMDA receptors play a critical role in synaptic transmission and plasticity underlying learning and memory, but their excessive activation by glutamate leads to Ca²⁺ overload and neuronal death, a process implicated in AD pathogenesis [8]. Memantine, the only clinically approved NMDA antagonist for AD, selectively blocks this pathological overactivation while preserving normal synaptic signaling. However, like CHEIs, it provides only symptomatic relief and cannot prevent further AD progression [9, 10, 11].
More broadly, drugs that solely target Aβ, which theoretically halt disease progression and potentially reverse existing damage, have repeatedly failed to pass Stage 3 trials. Over the years, hundreds of therapies have been proposed and developed to clear Aβ; Yet none, with the exception of Donanemab, has improved clinical outcomes to a significant extent. However, Donanemab is effective only in the early stages of AD, carries a risk of brain swelling, and costs approximately $32,000 per year, placing it out of reach for many patients [13]. These persistent limitations have shifted attention toward multi-target therapeutics, drugs that target pathology through numerous mechanisms, to better address the multifactorial etiology of AD [14]. The present study evaluated the efficacy of the combined treatment of two established multitarget AD therapies, DHA and Panax Ginseng extract, to assess their potential for synergistic effects, such as increased bioavailability, and contribute to the search for more accessible therapies.
Omega-3 fatty acids (ω-3FAs)
DHA is the predominant omega-3 fatty acid (ω-3FA) in the brain [15]. Dietary ω-3FA supplementation, particularly at moderate or high doses, shows promise for slowing AD progression and restoring executive and hippocampal function, with studies reporting up to ~64% reduction in AD risk [16, 17, 18]. These outcomes can be largely attributed to ω-3FAs multi-target free radical scavenging, anti-inflammatory, BBB-strengthening, antiapoptotic, and neurotrophic properties [19, 20]. Upon metabolism, ω-3FAs generate specialized pro-resolving mediators that facilitate BBB repair and enhance clearance of Aβ and fibrinogens [21, 22]. Furthermore, Mfsd2a, the primary DHA transporter at the BBB, plays an integral role in barrier and pericyte health but declines with age and cognitive decline. However, maintaining a high ω-3FA index, especially before significant neurodegeneration has occurred, offsets this progression [23, 20]. Unfortunately, Epidemiological data indicate that U.S. ω-3FA intake is largely inadequate (~0.1–0.2 g DHA/EPA per day), leading many researchers to argue ω-3FA deficiency to be a leading driver of AD prevalence [24, 17].
Beyond targeting hallmark AD pathology (Aβ plaques, neurofibrillary tangles), ω-3FAs may attenuate cognitive and motor decline through additional mechanisms. A systematic review of eleven studies (n=698) found that ω-3FA supplementation substantially increased serum brain-derived neurotrophic factor (BDNF) levels at moderate or high doses [25]. BDNF is a neurotrophin critical for synaptic formation and maintenance, with established roles in learning, memory, emotion, sensory integration, motor function, executive function, and stress response—all of which are impaired with AD [26, 27]. Additionally, AD patients exhibit reduced BDNF levels, an association that may both result from and exacerbate disease progression, though whether the relationship is causal remains an area of active investigation [28, 29].
ω-3FAs also possess potent anti-neuroinflammatory properties. In the aging brain, misfolded proteins, primarily Aβ aggregates and neurofibrillary tangles (NFTs), trigger innate immune responses in microglia, initiating a neurodegenerative cascade [33]. ApoE-4, a major genetic risk factor for AD, further amplifies this process by upregulating glial activation (relative to ApoE-2 or ApoE-3) through lipid modulation [30]. Although ω-3FAs have been extensively studied for their anti-inflammatory effects in cardiology and metabolic health [31], recent evidence demonstrates that dietary ω-3FAs also traverse the BBB and reduce neuroinflammation directly. In a randomized controlled trial of 33 mild AD patients, six months of DHA-based ω-3FA supplementation (2.3 g) reduced phosphorylated tau and lowered neuroinflammatory biomarkers, including interleukin-1 and interleukin-6 [32].
Panax ginseng
Panax ginseng, a perennial plant of the Araliaceae family, has been used in East Asian medicine since approximately 1500 CE and is among the earliest herbal medicines applied to the treatment of dementia and neurological disorders [7, 34]. Ginsenosides, the primary bioactive compounds isolated from Panax ginseng, exhibit multi-target neuroprotective properties relevant to AD: anticholinesterase activity; increased neuroplasticity; Aβ and tau clearance; anti-inflammatory and antioxidant activity; anti-apoptotic effects; alleviation of insulin resistance; and BBB strengthening [34, 35]. Multiple human trials support ginseng’s efficacy in AD prevention and amelioration [36], and researchers have emphasized the need for further investigation into ginseng-based drug combinations [34].
Evidence from animal models corroborates these findings. In transgenic AD mice, fermented ginseng extract ameliorated memory dysfunction concurrent with reduced Aβ42 brain accumulation [37]. Red, black, and white ginseng extracts inhibit acetylcholinesterase and reduce hippocampal Aβ oligomer-induced memory impairment [38]. In the present study, ginseng was administered as Korean red ginseng, which contains the highest concentration of ginsenosides among ginseng preparations. Korean red ginseng treatment has demonstrated improved frontal lobe function via quantitative electroencephalography [39], and its cognitive benefits have been sustained for over two years in AD patients [40].
Blood-brain barrier (BBB) and nutrient transport
On a fundamental level, ApoE in the brain serves as a regulator of astrocytes and glial cells, helping to modulate inflammation and thus the brain’s ability to fight pathogens and repair. At the beginning of human history, ApoE-4 existed as the sole isoform. Alternate isoforms that are less inflammatory by comparison, ApoE-2 and ApoE-3, appeared in the presence of a more glucose-based diet facilitated by agriculture. Although ApoE-4 was highly evolutionarily advantageous before the advent of modern medicine, it now poses a leading risk factor for AD pathogenesis, raising AD risk by up to 15-fold in double allele cohorts [41, 42].
Multiple mechanisms underpin ApoE-4’s contribution to AD risk. ApoE-4 binds to receptor LRP1, which is responsible for Aβ clearance, thereby elevating Aβ oligomer levels by up to 2.7-fold [43]. This binding also triggers the release of MMP-9 and cyclophilin A, which further degrade the BBB and render the brain vulnerable to neurotoxic bloodstream proteins, including plasminogen, auto-antibodies, albumin, and fibrinogen, that trigger a cascade of neuroinflammation.
The BBB’s role in ω-3FA transport is directly relevant to this study [44, 45, 21]. Although ω-3FA supplementation shows strong preventive efficacy, contradictory results in post-onset cohorts impede broader clinical recommendations. In a randomized controlled trial of 174 patients with mild to moderate AD, moderate-dose ω-3FAs failed to improve cognitive outcomes relative to placebo over six months [46]. While the short study duration likely played a role, existing BBB damage in the AD patients may also be a contributing factor. When the BBB becomes compromised, the brain’s ability to uptake of DHA drastically deteriorates because the amount of DHA transporters, Mfsd2a, sharply decreases. Although the brains of young adults readily uptake ω-3FAs regardless of ApoE status, older adults, especially those with ApoE-4 and/or AD, show significantly reduced uptake [16]. A separate trial confirmed this pattern: DHA supplementation was significantly less effective at mitigating AD symptoms in ApoE-4 carriers compared to ApoE-3 carriers [47].
Several approaches have been proposed to increase ω-3FA bioavailability in the brain, including co-administration with antioxidants and polyphenols. For instance, combining ω-3FAs with carotenoid and vitamin E improved cognitive outcomes in otherwise healthy older adults—an effect attributed to antioxidant-enhanced bioavailability [18]. However, ginseng may offer even greater synergistic potential. Ginsenoside Rg1 directly activates the Wnt/β-catenin pathway, the transcriptional regulator of Mfsd2a, thereby upregulating DHA transport across the BBB [48]. Additionally, ginseng may halt broader BBB degradation through inhibition of MMP-9, an enzyme that downregulates Mfsd2a in ApoE-4 carriers, and by crossing the BBB to reduce the neuroinflammation at the center of the neurodegenerative cascade [49, 52]. Preliminary studies in C. elegans further suggest that ginseng modulates lipid metabolism and extends healthspan by upregulating ω-3FA (in the form of lipoic acid) metabolic signaling pathways; though whether this effect translates to DHA is unclear [50, 51]. Together, these findings suggest that ginseng may increase DHA absorption by the brain, thus bypassing the primary limitation of ω-3FA treatment for patients who have already developed AD.
Caenorhabditis elegans
Caenorhabditis elegans is a widely used model organism for AD research due to its cellular simplicity, genetic amenability, low cost, and substantial homology with humans—83% of its proteome has human homologous genes [53, 54]. Its nervous system of 302 neurons enables mechanisms to be traced at the level of individual neurons, and its 2–3 week lifespan allows observation of neurodegeneration across an entire adult life [55, 56]. Previous studies have utilized the organism’s transparent body for in vivo visualization of neuronal death and protein aggregation [55]. Although previous research has tested ginseng and ω-3FAs separately in C. elegans AD models, the combination of both treatments has not been investigated.
Previous research
To date, no AD studies have combined ω-3FAs (DHA, ALA, or EPA) with ginseng. However, two studies in other contexts provide relevant precedent. A double-blind randomized controlled trial found that ω-3FAs combined with ginseng and green tea catechins significantly improved cognitive test performance and increased activation in relevant brain regions via fMRI [57]. A later study in children with ADHD found that the combination significantly alleviated symptoms beyond the sole use of either treatment, possibly indicating a synergistic effect [58]. However, these studies did not investigate the potential connection between ginseng and increased ω-3FA absorption in the brain.
Research question & hypothesis
The present study researched the efficacy of a combination of Docosahexaenoic acid (DHA) and Panax Ginseng extract for the treatment of Alzheimer's Disease (AD). Based on both the comprehensive mechanisms the combined treatment addresses and the potential for ginseng to enhance DHA absorption in the nervous system, this study hypothesizes that a combination of ginseng extract and DHA would confer benefits in alleviating Aβ toxicity in CL2355 (transgenic AD model) beyond those of either treatment alone. Operationally, this translates to a higher percentage of unparalyzed worms following temperature upshift, greater population growth, and a higher chemotaxis index (attraction to a chemical stimulus)
2.0 Materials and Methods
Creating M9 buffer
Using a top loading balance, 1.5 g of KH2PO4, 3 g of Na2HPO4, and 2.5 g of NaCl was dissolved in a 500 mL of distilled water in a graduated cylinder. The solution was then sealed with aluminum foil and autoclaved for 20 minutes. Next, 1 mL of 1 M MgSO4 was added to the solution. The final solution was stored at room temperature and sterilized using an autoclave prior to each use.
Creating ginsenoside stock solution (10 mg/ml)
Five grams of ginseng extract was measured using a top loading balance. Next, 50 mL of distilled water was measured into a graduated cylinder, mixing it with the ginseng extract in the graduated cylinder until fully dissolved. The solution was then autoclaved at 120°C for 2 hours before being transferred to the test tube and stored in a dark and cool environment. If necessary, the solution was repeatedly mixed before each use.
Creating Omega-3 stock solution (500 mM)
Utilizing a top-loading balance 8.2g of DHA omega-3 was measured in an Erlenmeyer flask using a top-loading balance. In a graduated cylinder, 50 mL of sterilized M9 solution was measured. Using 1.5 mL Tween 80, the measured omega-3 was dissolved. The water and fatty acid emulsion was transferred into a vial and vortexed until fully homogeneous. Then, the stock solution was stored in a light blocking tinted vial and placed in a dark and cool environment until its usage. Before each use, a vortex was used to ensure a homogeneous mixture of the treatment.
Creating Nematode Growth Media (NGM) agar plates
The C. elegans were cultured in the Nematode Growth Media (NGM) agar plates with various concentrations of the tested treatments. The Petri dishes were labeled by group names per distinct treatment concentrations and strains according to Table 1. The NGM (provided by Carolina Biological) in solid form was melted into liquid form for usage. First, the bottle was uncapped about halfway to release steam and pressure. The NGM agar was then added into the microwave for 30 seconds in intervals of 15 seconds, checking each time until adequately melted (alternatively a water bath at approximately 100℃ was used if time permitted). Gloves were used when taking the agar out of the microwave, properly shaking it to ensure no solids remain (agar should be a dark-yellow liquid). Then, the agar was allowed to cool for a few minutes with caution of re-solidification in cases of excessive cooling.
Half of the NGM agar was dedicated to ginseng groups by transferring them to a separate graduated cylinder. A 1000x dilution of ginsenoside solution (0.18 mL) was performed using 180 mL of NGM agar as the solvent. Then, the agar was poured into the Petri dish very quickly, covering the lid of the Petri dish and tapping the bottle to avoid possible contamination. The aforementioned procedure was repeated for all Petri dishes with a waiting time of 15-20 minutes until agar solidified in each dish prior to refrigerator storage for 24 hours before usage (keeping the Petri dish upside down to prevent condensation from falling on the agar).
Each plate was then spotted with E. coli OP50 grown for 24 hours in LB Media. Upon transferring, plates were dried for an additional 24 hours. The previously made omega-3 stock solution was diluted from 1mL to 5 mM with sterilized water to a final volume of 100 mL (100x dilution). Then, a dispersion of 0.1 mL of DHA omega-3 aliquot to the solidified and spotted NGM in Groups CL -G/+O, and CL +G/+O was done using a sterilized spreader. Upon administration of treatment in each Petri dish, the mediums were allowed to dry for another 24 hours.
Table 1: Experimental Setup
| Group Name | C. elegans strain | DHA Omega-3 (mM) | Ginsenoside (μg/ml) |
| WT | N2 (wild type) | 0 | 0 |
| CL -G/-O | CL2355 (AD) | 0 | 0 |
| CL -G/+O | CL2355 (AD) | 5 | 0 |
| CL +G/-O | CL2355 (AD) | 0 | 10 |
| CL +G/+O | CL2355 (AD) | 5 | 10 |
Toothpick technique C. elegans Transfer
A blunt dissecting probe, acting as a pick for C. elegans transfer, was sterilized on a flame. A bead of OP50 was collected from an empty place to make the point sticky. Gently touch the worm selected using the OP50 coated probe. When the worm disappeared, it was on the probe. The worms were placed on the destination place by gently rolling the probe's tip until it became free. The worm was zoomed in on using the microscope to ensure that it was not damaged after the transfer and only the selected worm or egg was transferred.
Creating bacteria agar
The table was cleaned before beginning and preparing the materials for the study, with researchers following standard safety procedures. A weighing paper was folded to make it easier to handle. On a weighing boat on a scale, 17.5 g of premix LB Agar powder was weighed. This powder was transferred to an Erlenmeyer flask and distilled water was added until reaching a final volume of 500 mL. The bottle cap and the top were sealed with aluminum foil tightly. The solution was then autoclaved in the liquid setting for 20 minutes. Following the autoclaving, the agar was cooled to about 55℃. A thin layer of LB agar was poured into each Petri dish, ensuring the liquid was properly and evenly spread. After putting on the lid of the Petri dishes, each plate was left to cool down until solidification. After 24 hours of the solidification process, the dish was flipped to avoid the condensation falling onto the agar. After this, the plates were placed in plastic bags in the refrigerator at 4℃.
Bacterial aseptic technique
E. coli OP50 (Source: https://cgc.umn.edu/strain/OP50) was used to feed C. elegans strains CL2355 (Sourced: https://cgc.umn.edu/strain/CL2355) and N2 (Sourced: https://cgc.umn.edu/strain/N2) and placed in all Petri dishes. A rubber tube was connected to the valve of the gas and the valve of a Bunsen burner. Once the gas ignited, a match was lit and placed over the gas. The inoculation loop was sterilized by passing the tip and the neck of the inoculation loop through the flame. After the inoculation loop cooled, it was used to scoop the agar from a bacterial colony. The bacteria were streaked across the surface of a new Petri dish, ensuring that there was no excessive pressure put on the agar to refrain from breaking it. After, the lid was placed back on to the Petri dish and flipped upside down in the incubator to ensure that the accumulated condensation does not fall on the agar. Following two days of the Petri dishes being incubated, parafilm was wrapped around the sides of the Petri dish and placed into the fridge to store for later use. Before and after each process, diluted bleach was used to sterilize all surfaces.
Spotting Petri dishes with E. coli OP50
A 0.5 cm x 0.5 cm square chunk of agar with E. coli OP50 was cut using forceps or other sterilized metal. Sterilized forceps were used to grab a piece of agar. The agar was placed into the middle of the premade NGM plates. Each chunk was gently placed into its respective Petri dish. Before and after cutting and transferring each chunk, disinfectant tools were used to prevent contamination.
Conducting the paralysis assay
After 48 hours of C. elegans culturing, the temperature was either adjusted to 27℃ (for Trial 1) or 30℃ (for Trial 2). To ensure that the plates reached the temperature at the same time, the plates were not stacked on each other. After 24 hours of temperature upshift, the scoring of paralysis was performed for every two hours until all nematodes were paralyzed. Paralyzed nematodes were transferred to a part of the plate that was not spotted to refrain from scoring them again. In C. elegans, the head of nematodes is last to become paralyzed while the tail is first, restricting its movement. The C. elegans were considered paralyzed when they were unable to move, excluding its head. Nematodes that rarely voluntarily move were poked using a worm picker. If C. elegans did not show full movement, they were considered paralyzed.
Testing for Population Growth
A 24 well plate’s first column was labeled “WT”, the second column “CL -G/-O”, the third column “CL -G/+O”, the fourth column “CL +G/-O”, and the fifth column “CL +G/+O”. Four wells were used for each group. First, 1.0 mL of ginsenoside NGM was poured into the columns of CL +G/-O and CL +G/+O. Then, 0.1 mL of DHA omega-3 aliquot was pipetted to the solidified and spotted NGM in the columns CL -G/+O and CL +G/+O. Then, C. elegans were chunked into each column containing NGM. Every day for one week, the amount of C. elegans was recorded under a compound microscope. For Trial 1 of the assay, 10 μL ginseng was spread on top of the NGM for the treatment groups that required it. For Trial 2, ginseng was diluted into the NGM following the previous procedure.
Conducting the Chemotaxis Index Assay
Seven days before conducting the chemotaxis, C. elegans from each group were transferred to similar treatment plates to allow the C. elegans to culture. These plates were regarded as the treatment plates. Two days before the chemotaxis, a marker was used to divide each of 5 NGM Petri dishes into 4 equal quadrants, and a circle was created from the origin with a 1 cm radius. Then, another circle was created from the origin with a 2 cm radius. 10 µL of E. coli, acting as an attractant, was pipetted onto quadrant 1 and quadrant 3 of the chemotaxis plate. These 5 Petri dishes with the absence of treatment were regarded as the chemotaxis plates.
A micropipette was used to pipette 2 mL M9 on the treatment plates. The treatment plate was gently angled to cover all surface area to ensure that all nematodes were cleansed. A pipette was used to pipette 1 mL of the previously made worm solution in a microcentrifuge tube. The solution was centrifuged for 6,600 rpm for 10 seconds. After the centrifugation, the remaining M9 was removed. One mL M9 was pipetted in the centrifuge tube and the tube was turned to ensure that all nematodes were cleansed. The process was repeated three times. After, the volume of the supernatant was reduced to 100 μl and centrifuged for another 10 seconds. A pipette was used to transfer 2 μl of nematodes onto the chemotaxis plates.
After the 60 minute cleansing period, the nematodes were used. A micropipette was used to transport 2 μL of the nematode solution from the centrifuged solution to the center of the chemotaxis plate, or the intersection of the perpendicular lines drawn. Immediately after, a recording device was set directed towards the chemotaxis plates in a compound microscope, and a 60 minute video was recorded. After 60 minutes, the chemotaxis plates with the nematodes were placed in an incubator with a controlled temperature of 4 °C. The number of nematodes that passed through the circle with a 1 cm radius and moved towards the attractant zone or control zone and the time it took was recorded in Microsoft Excel corresponding with their respective quadrants. The process was repeated, replacing the treatment solution with sole control treatment. This Petri dish was regarded as the control plate. The chemotaxis assay was performed in quadruplicate.
Safety
Proper lab safety, including wearing gloves, goggles, and tied hair during the experimentation process, was fulfilled especially when conducting bacterial works. The tabletop working area was cleansed with a diluted bleach solution before and after experimentation along with the sterilization of all instruments at the end of the trial period. All Petri plates were sealed with parafilm during experimentation and autoclaved at 120 ℃ and 100 kPa for 20 minutes as part of the disposal procedure. Tools in contact with cultures were also soaked in 10% bleach and sterilized with heat as a segment of the disposing process. Hands were washed after any bacterial work or assay procedure. Three days of safety training specifically for bacterial works and the presence of experienced supervisors were ensured whilst dealing with microorganisms and the flame or gas of a Bunsen burner required for sterilization.
Three days of safety training specifically for bacterial works and the presence of experienced supervisors were ensured while dealing with microorganisms and the flame or gas of a Bunsen burner required for sterilization of tools. Most substances utilized in the study possessed a biosafety level BSL-1 and deemed “not hazardous” under the criteria of the federal OSHA Hazard Communication Standard 29CFR 1910.1200, and Regulation (EC) No 1272/2008 (GHS). Nonetheless, substances specifically can be dangerous when ingested, inhaled, or especially in cases of in contact with eyes (skin contact and inhalation do not pose serious harm unless it is done excessively or if the researcher feels unwell after exposure) so precautionary safety such as protective gloves, clothing, and above all else eye protection was adhered to.
Data Analysis
Data was collected, stored, and analyzed using Microsoft Excel. Data was then shown using scatter plots and bar graphs in which the x values were time in hours, time in days, and group names and the y values were not paralyzed C. elegans as a percentage, number of C. elegans, and chemotaxis index. The median paralysis time was conducted using a Kaplan–Meier survival analysis. In the paralysis assay, the number of non-paralyzed C. elegans on each plate was converted into a percentage. The standard mean of error was calculated and represented as error bars added using Microsoft Excel. To calculate significance, one-way ANOVA followed by Tukey HSD was done using https://astatsa.com/OneWay_Anova_with_TukeyHSD/. Significance was determined using p-values in which a p-value less than 0.05 was considered significant. Chemotaxis index was determined using the following formula:
CI = (number of worms in attractant zone - number of worms in control zone)/total number of scored worms
Results
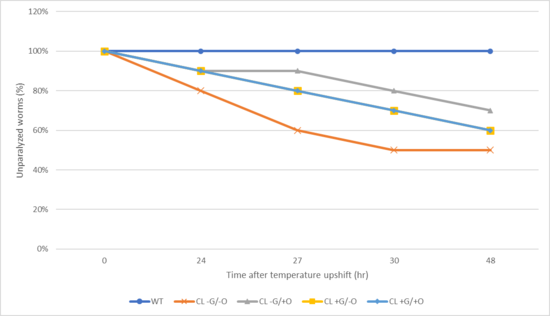
In the C. elegans strain CL2355, as the temperature rises, Aꞵ peptide production increases in nematode muscles, leading to paralysis. CL-G/-O (the negative control group) had the lowest percentage of unparalyzed worms 48 hours after the temperature upshift. CL -G/+O had the highest percentage of unparalyzed worms compared with the negative control group, at 70% 48 hours after the temperature upshift. Additionally, CL +G/-O and CL +G/+O showed similar effects, with the percentage of unparalyzed worms remaining identical over time. Throughout the assay, all treatment groups exhibited a higher percentage of unparalyzed nematodes, indicating alleviation of the effects of Aβ aggregation. The wild-type C. elegans (WT) does not produce Aꞵ peptides, so the nematodes did not exhibit paralysis following a temperature upshift.
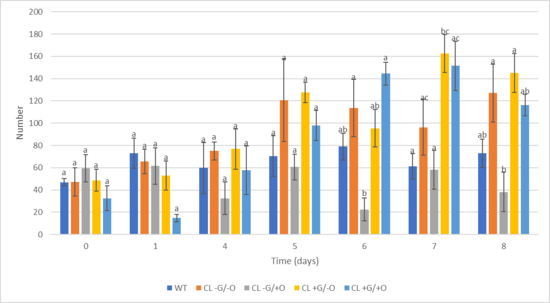
Figure 2 shows population growth throughout the whole assay, with CL +G/-O and CL +G/+O showing higher populations compared to WT from Day 5. At Day 6, CL +G/+O (combined treatments) had a statistically significantly higher population than the CL -G/+O group. Similarly, at Day 7, CL +G/-O had statistically higher growth than WT along with Day 8, demonstrating a significantly higher population compared to CL -G/+O.
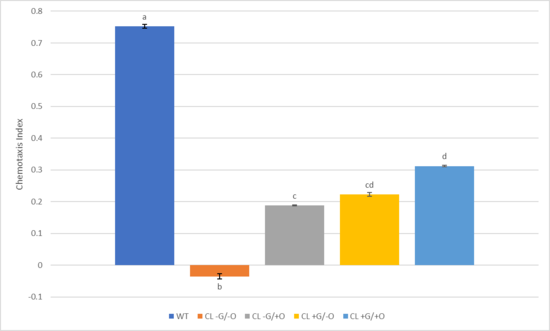
The results shown in Figure 3 indicate that WT (N2 wildtype) had the greatest chemotaxis index compared to all other groups. CL -G/-O, the negative control group, had the lowest chemotaxis index, which was statistically significant when compared to the CL -G/+O group, CL +G/-O, and CL +G/+O. Out of the groups expressing Aꞵ peptides, CL +G/+O had the greatest chemotaxis index, with statistical significance when compared to CL -G/-O and CL -G/+O. The CL +G/-O group had the next greatest chemotaxis index (0.222), followed by CL -G/+O (0.188).
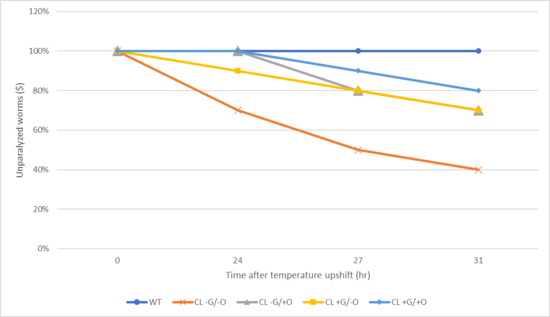
The results of Figure 4 are consistent with that of Trial 1 in which all treatment groups had a higher percentage of unparalyzed C. elegans compared to CL -G/-O. WT had the lowest percentage of unparalyzed worms throughout the trial, except at Hour 0. Among all treatment groups with C. elegans exhibiting Aβ aggregation, CL +G/+O (combined treatment) had the highest percentage of unparalyzed C. elegans (80%) at 31 hours following the temperature upshift. The CL-G/+O and CL+G/-O groups both had 70% unparalyzed C. elegans 31 hours after a temperature upshift. Therefore, treatment with sole ginseng, sole omega-3, and a combination of ginseng and omega-3 all showed alleviation of Aβ aggregation effects, with the combination treatment exhibiting the greatest effect in Trial 2 of the paralysis assay.
Figure 5 shows that WT had the highest population number throughout the assay. All groups exhibiting Aβ aggregation had significantly lower populations than WT on Days 8 and 9. CL-G/-O (the negative control group) decreased in population number as the assay progressed. Within the groups exhibiting Aβ aggregation, CL +G/+O (combined treatments) displayed the highest population throughout the whole trial, other than Day 5.
Discussion
The results of this study generally support the hypothesis that a combined treatment of Panax ginseng extract and DHA confers an additive or synergistic effect in alleviating Aβ toxicity. In Trial 2, the combined treatment (CL +G/+O) displayed 40% and 10% lower rates of paralysis relative to untreated CL2355 (CL -G/-O) and sole treatment groups, respectively. In C. elegans models of AD, paralysis typically occurs without visible deposition of Aβ plaques; thus, reduced paralysis rates, as observed in the present study, indicate clearance of Aβ oligomers and/or attenuation of their deleterious effects [59].
This mechanism aligns with the increasingly influential Aβ Oligomer Hypothesis. Although the amyloid cascade theory proposed in 1992 served as the guiding framework of AD etiology, many researchers have since deviated from or modified this hypothesis, forming distinct schools of thought, each backed by extensive research, including BBB breakdown, mitochondrial dysfunction, and the Aβ oligomer hypothesis [60, 61, 62]. The latter identifies soluble Aβ oligomers, rather than insoluble plaques, as the key neurotoxic species driving neuroinflammation, neuronal damage, and ultimately AD pathogenesis.
Currently, Donanemab is the only drug that the FDA has approved to treat AD via Aβ clearance. Researchers attribute Donanemab's relative effectiveness to its ability to specifically target neurotoxic forms of Aβ, including oligomers, unlike treatments that indiscriminately target harmless or even protective Aβ species [12]. However, with the drug currently costing $32,000 per year and proving effective only in the early stages of AD, widespread clinical adoption remains limited [13]. As the combined treatment of ginseng and DHA similarly appears to target neurotoxic Aβ species, it may serve as a more accessible alternative with multi-target benefits extending beyond Aβ clearance alone.
The paralysis assay was followed by a chemotaxis assay to evaluate whether Aβ attenuation translates to broader improvements in neurological function. The chemotaxis assay integrates sensory perception, motor output, learning, and memory, making it a comprehensive marker of neurotoxicity. CL2355 produces Aβ pan-neuronally through the synaptobrevin ortholog (snb-1) promoter, leading to deficits in serotonin sensitivity, neuronal function, and chemotaxis. The combined treatment produced the greatest improvement in chemotactic ability among Aβ-expressing groups (0.312), significantly outperforming the untreated control (p<0.01). Ginseng alone (0.223) and DHA alone (0.188) showed comparable intermediate effects, both significantly higher than the untreated control (-0.035) but significantly lower than the combined treatment (Fig. 3). These findings suggest that the combined treatment exerts a neuroprotective effect that extends beyond motor function, partially restoring complex neurological processes.
The combined treatment had marginal effects on population growth compared to CL -G/-O (Fig. 5). However, as incomplete sterility is a characteristic of the CL2355 strain and some AD strains exhibit normal reproduction, it remains unclear whether impaired reproduction in CL2355 is directly attributable to Aβ pathology.
Collectively, these findings support the original hypothesis that combined treatment would more effectively alleviate AD symptoms in C. elegans, as groups receiving the combination demonstrated lower rates of paralysis and significantly higher chemotaxis scores than either treatment alone.
Limitations and Future Research
Treatment Delivery Method
Trial 1 of the paralysis assay (Fig. 1) produced results contradicting Trial 2 (Fig. 4): the combined treatment (30% reduction in paralysis) performed worse than DHA alone (40% reduction). These inconsistencies reduce the validity of the findings and warrant additional replication with more rigorous methodology. However, this discrepancy may also have arisen from the ginseng delivery method. In Trial 1, ginseng was infused within NGM agar rather than spread across the surface (the delivery method used for DHA), an approach intended to control treatment volume and prevent ginsenoside denaturation upon contact with the Tween-80 used to emulsify DHA. Given that the results in ginseng-administered groups contradicted prior research and that Trial 1 employed a highly unconventional delivery method, agar infusion likely impeded ginseng absorption. Trial 2, therefore, adopted surface spreading consistent with prior research, yielding markedly improved efficacy in both the ginseng-only and combined treatment groups (30% and 40% paralysis reduction, respectively, compared to 10% each in Trial 1). Future studies using this treatment combination should exclusively utilize surface spreading and, preferably, identify alternatives to Tween-80.
C. elegans Strain
The CL2355 strain was selected for its prior use in chemotaxis research [59]. However, CL2355 demonstrates temperature-induced pan-neuronal Aβ expression in which heat increases but does not solely determine Aβ production [63]. For paralysis assays, the CL4176 strain—which exhibits strictly temperature-dependent Aβ expression—is more suitable and extensively used [59]. Future research should use both strains in combination to address this limitation.
Statistical Power
For both paralysis trials, statistical significance (p<0.05) could not be determined due to each group having only a single replicate (n=10/group). Although this design was formulated in alignment with some prior research, the absence of replication limits the conclusions that can be drawn. Future research should perform paralysis assays in triplicate and subject results to ANOVA to enable rigorous statistical analysis.
Population Assay
Similar to paralysis, the results of the population assay (Fig. 2 & Fig. 5) also notably differed between trials. Trial 1 was subject to the same ginseng delivery limitation and was further confounded by inconsistent food availability, as OP50 spotted on agar may have been depleted over the course of the trial. Additionally, the CL -G/+O group became contaminated around Day 4, introducing another confounding variable. Critically, Trial 1 produced results in which the wild-type group (normal reproduction) exhibited a lower population than CL -G/-O (incomplete sterility, no treatment) — an outcome inconsistent with established findings. The combination of these known confounders and biologically incoherent results renders Trial 1 of the population assay virtually null. Trial 2 addressed these issues through surface spreading, consistent feeding, and more rigorous sterilization, producing results consistent with prior research [59]. Future replications should ensure consistent feeding throughout the experimental duration.
Chemotaxis Assay
The chemotaxis assay presents its own limitations. Previous research recommends using young adult C. elegans for chemotaxis analysis, as chemosensory neurons undergo intermediate changes at the L4 stage [64, 65]. Although bleach synchronization is standard practice for controlling life stages, it was not implemented in this study due to laboratory equipment constraints. Variance in life stages was minimized through relatively high sample sizes per quadrant. Additionally, sodium azide (the standard anesthetic used to immobilize C. elegans upon entering a quadrant) was not used due to its high volatility and risk of rapid dermal absorption. To mimic the results of anesthetics, a 60-minute video recording was used to track the first quadrant entered by each nematode, and scored worms were transferred to prevent rescoring.
C. elegans as an AD Model
C. elegans as a model of AD possesses notable limitations. The organism lacks several features central to AD pathology, including the APOE gene, a BBB, complex mammalian neurophysiology (hippocampus, cortex, BDNF signaling), tau phosphorylation (in Aβ-expressing models), and a human-like microbiome [55]. These absences are directly relevant to the mechanisms proposed in this study. For instance, ginseng’s ability to ameliorate cognitive defects in mouse AD models depends partly on restoring lactobacillus dominance—a mechanism absent in C. elegans [66]. More critically, BBB-mediated mechanisms inferred to underlie ginseng’s enhancement of DHA transport to the brain, a central part of the original hypothesis, cannot be rigorously tested in an organism lacking a BBB. Similarly, although C. elegans possess an analog to Wnt/β-catenin (a pathway activated by ginsenosides), they lack the Mfsd2a transporters that Wnt/β-catenin produces, which significantly undermines the ability for the present study’s findings to corroborate the notion that ginseng enhances DHA absorption [55].
Nevertheless, C. elegans remains valuable for rapid preclinical screening. Its short lifespan and genetic versatility (e.g., temperature-induced Aβ secretion) make it well-suited for initial evaluation of novel treatments [55]. Although C. elegans lacks mammalian-specific genes such as BDNF, it retains the majority of evolutionarily conserved genes, such as those involved in klotho production, whose expression is upregulated by ginseng [67, 68]. Moreover, being the first to evaluate DHA treatment in a C. elegans AD model, the present study expands the literature on C. elegans and establishes a foundation for future research. Nevertheless, these strengths and weaknesses underscore the importance of progressing to higher-order organisms given promising results. To further leverage the C. elegans model, future studies should test the combined treatment on tau-expressing and gene-knockout strains to elucidate underlying mechanisms. Western blot analysis using anti-Aβ 6E10 and anti-oligomer A11 antibodies should also be performed to confirm that the combined treatment specifically targets Aβ oligomers.
Synergistic or Compounding? An Area of Future Research
Despite the combined treatment outperforming either treatment alone on all tested measures, this study cannot definitively determine whether these effects result from compounding mechanisms of each treatment or from ginseng enhancing DHA absorption. The compounding interpretation is compelling: ginseng and DHA both ameliorate AD symptoms and Aβ toxicity through overlapping and distinct mechanisms. Both treatments reduce neuroinflammation, sometimes through shared pathways (e.g., NF-κB inhibition); but ginseng additionally acts through the Nrf2/ARE pathway, while DHA uniquely produces specialized pro-resolving mediators [9, 69]. The combined treatment therefore casts a wider net, tackling AD pathology from more angles than either treatment alone.
Alternatively, the promising outcomes may also reflect ginseng increasing DHA absorption by the nervous system through mechanisms such as the Wnt/β-catenin pathway and antioxidant protection against DHA oxidation [34, 18]. The present study identifies this relationship between ginseng and DHA absorption as a gap in the current literature. Although unavailable to researchers of the present study, future investigations using C. elegans can should assess the amount of DHA absorbed; Some options include using lipophilic dyes, Gas Chromatography-Mass Spectrometry, or monitoring the expression of fat-related genes [70].
Conclusion
This study provides promising preliminary evidence that a combined treatment of Panax ginseng extract and DHA alleviates AD pathology more effectively than either treatment alone. The combined treatment appears to ameliorate Aβ oligomer toxicity, as suggested by the paralysis assay, and partially restore complex neurological function, as suggested by the chemotaxis assay. However, limitations including the model organism, confounding variables, and insufficient statistical power for certain assays underscore the preliminary nature of these findings. Moreover, this study could not determine whether the observed benefits arose from complementary mechanisms of the two treatments or from ginseng enhancing DHA absorption in the nervous system. Beyond its empirical findings, this study advances a mechanistic hypothesis that ginsenosides may enhance DHA bioavailability via the Wnt/β-catenin pathway and antioxidant protection, which, if validated in future research, could reframe the clinical utility of DHA supplementation in post-onset AD where BBB damage currently limits efficacy. Lastly, as the first study to evaluate DHA treatment in a C. elegans AD model, the present work demonstrates that DHA's established neuroprotective effects in mammalian models are reproducible in C. elegans model of AD. Given the growing global burden of AD and the prohibitive cost and limited efficacy of current treatments, accessible multi-target treatments warrant urgent investigation. Next steps should include directly measuring whether ginseng increases DHA absorption, achievable in C. elegans through lipophilic dye tracking or gas chromatography-mass spectrometry, followed by progression to higher-order AD models such as APP/PS1 mice.
References
[1] Qiu C, Kivipelto M and Von Strauss E 2009 Epidemiology of Alzheimer’s disease: occurrence, determinants, and strategies toward intervention Dialogues in Clinical Neuroscience 11 111–28
[2] Sharma K 2019 Cholinesterase inhibitors as Alzheimer’s therapeutics (Review) Mol Med Rep 20 1479–87
[3] Sadigh-Eteghad S, Sabermarouf B, Majdi A, Talebi M, Farhoudi M and Mahmoudi J 2015 Amyloid-beta: a crucial factor in Alzheimer’s disease Med Princ Pract 24 1–10
[4] Deng X, Zhao S, Liu X, Han L, Wang R, Hao H, Jiao Y, Han S and Bai C 2020 Polygala tenuifolia : a source for anti-Alzheimer’s disease drugs Pharmaceutical Biology 58 410–6
[5] Bredesen D E 2016 Inhalational Alzheimer’s disease: an unrecognized—and treatable—epidemic Aging (Albany NY) 8 304–13
[6] Soni D and Galluci L 2023 The Causes and Effects of Alzheimer’s Disease J Stud Res 12
[7] Kim H-J, Jung S-W, Kim S-Y, Cho I-H, Kim H-C, Rhim H, Kim M and Nah S-Y 2018 Panax ginseng as an adjuvant treatment for Alzheimer’s disease Journal of Ginseng Research 42 401–11
[8] Mark L P, Prost R W, Ulmer J L, Smith M M, Daniels D L, Strottmann J M, Brown W D and Hacein-Bey L 2001 Pictorial review of glutamate excitotoxicity: fundamental concepts for neuroimaging AJNR Am J Neuroradiol 22 1813–24
[9] Liu J, Chang L, Song Y, Li H and Wu Y 2019 The Role of NMDA Receptors in Alzheimer’s Disease Front. Neurosci. 13
[10] Paoletti P 2011 Molecular basis of NMDA receptor functional diversity European Journal of Neuroscience 33 1351–65
[11] Kodis E J, Choi S, Swanson E, Ferreira G and Bloom G S 2018 N-methyl-D-aspartate receptor–mediated calcium influx connects amyloid-β oligomers to ectopic neuronal cell cycle reentry in Alzheimer’s disease Alzheimer’s & Dementia 14 1302–12
[12] Rashad A, Rasool A, Shaheryar M, Sarfraz A, Sarfraz Z, Robles-Velasco K and Cherrez-Ojeda I 2022 Donanemab for Alzheimer’s Disease: A Systematic Review of Clinical Trials Healthcare (Basel) 11 32
[13] Sims J R, Zimmer J A, Evans C D, Lu M, Ardayfio P, Sparks J, Wessels A M, Shcherbinin S, Wang H, Monkul Nery E S, Collins E C, Solomon P, Salloway S, Apostolova L G, Hansson O, Ritchie C, Brooks D A, Mintun M, Skovronsky D M, and TRAILBLAZER-ALZ 2 Investigators 2023 Donanemab in Early Symptomatic Alzheimer Disease: The TRAILBLAZER-ALZ 2 Randomized Clinical Trial JAMA 330 512–27
[14] Maramai S, Benchekroun M, Gabr M T and Yahiaoui S 2020 Multitarget Therapeutic Strategies for Alzheimer’s Disease: Review on Emerging Target Combinations BioMed Research International 2020 5120230
[15] Dighriri I M, Alsubaie A M, Hakami F M, Hamithi D M, Alshekh M M, Khobrani F A, Dalak F E, Hakami A A, Alsueaadi E H, Alsaawi L S, Alshammari S F, Alqahtani A S, Alawi I A, Aljuaid A A and Tawhari M Q 2022 Effects of Omega-3 Polyunsaturated Fatty Acids on Brain Functions: A Systematic Review Cureus
[16] Arellanes I C, Choe N, Solomon V, He X, Kavin B, Martinez A E, Kono N, Buennagel D P, Hazra N, Kim G, D’Orazio L M, McCleary C, Sagare A, Zlokovic B V, Hodis H N, Mack W J, Chui H C, Harrington M G, Braskie M N, Schneider L S and Yassine H N 2020 Brain delivery of supplemental docosahexaenoic acid (DHA): A randomized placebo-controlled clinical trial eBioMedicine 59
[17] Wei B-Z, Li L, Dong C-W, Tan C-C, Alzheimer’s Disease Neuroimaging Initiative and Xu W 2023 The Relationship of Omega-3 Fatty Acids with Dementia and Cognitive Decline: Evidence from Prospective Cohort Studies of Supplementation, Dietary Intake, and Blood Markers Am J Clin Nutr 117 1096–109
[18] Power R, Nolan J M, Prado-Cabrero A, Roche W, Coen R, Power T and Mulcahy R 2022 Omega-3 fatty acid, carotenoid and vitamin E supplementation improves working memory in older adults: A randomised clinical trial Clinical Nutrition 41 405–14
[19] Ajith T A 2018 A Recent Update on the Effects of Omega-3 Fatty Acids in Alzheimer’s Disease Current Clinical Pharmacology 13 252–60
[20] Patrick R P 2019 Role of phosphatidylcholine-DHA in preventing APOE4-associated Alzheimer’s disease FASEB J 33 1554–64
[21] Valente M, Dentoni M, Bellizzi F, Kuris F and Gigli G L 2022 Specialized Pro-Resolving Mediators in Neuroinflammation: Overview of Studies and Perspectives of Clinical Applications Molecules 27 4836
[22] Francos-Quijorna I, Santos-Nogueira E, Gronert K, Sullivan A B, Kopp M A, Brommer B, David S, Schwab J M and López-Vales R 2017 Maresin 1 Promotes Inflammatory Resolution, Neuroprotection, and Functional Neurological Recovery After Spinal Cord Injury J. Neurosci. 37 11731–43
[23] Yang A C, Stevens M Y, Chen M B, Lee D P, Stähli D, Gate D, Contrepois K, Chen W, Iram T, Zhang L, Vest R T, Chaney A, Lehallier B, Olsson N, du Bois H, Hsieh R, Cropper H C, Berdnik D, Li L, Wang E Y, Traber G M, Bertozzi C R, Luo J, Snyder M P, Elias J E, Quake S R, James M L and Wyss-Coray T 2020 Physiological blood-brain transport is impaired with age by a shift in transcytosis Nature 583 425–30
[24] Kris-Etherton P, Taylor D S, Yu-Poth S, Huth P, Moriarty K, Fishell V, Hargrove R L, Zhao G and Etherton T D 2000 Polyunsaturated fatty acids in the food chain in the United States12 The American Journal of Clinical Nutrition 71 179S-188S
[25] Ziaei S, Mohammadi S, Hasani M, Morvaridi M, Belančić A, Daneshzad E, Saleh S A K, Adly H M and Heshmati J 2024 A systematic review and meta-analysis of the omega-3 fatty acids effects on brain-derived neurotrophic factor (BDNF) Nutr Neurosci 27 715–25
[26] Brown S P, Mathur B N, Olsen S R, Luppi P-H, Bickford M E and Citri A 2017 New Breakthroughs in Understanding the Role of Functional Interactions between the Neocortex and the Claustrum J. Neurosci. 37 10877–81
[27] Miranda M, Morici J F, Zanoni M B and Bekinschtein P 2019 Brain-Derived Neurotrophic Factor: A Key Molecule for Memory in the Healthy and the Pathological Brain Front. Cell. Neurosci. 13
[28] Zhang Z, Liu X, Schroeder J P, Chan C-B, Song M, Yu S P, Weinshenker D and Ye K 2014 7,8-dihydroxyflavone prevents synaptic loss and memory deficits in a mouse model of Alzheimer’s disease Neuropsychopharmacology 39 638–50
[29] Weinstein G, Beiser A S, Choi S H, Preis S R, Chen T C, Vorgas D, Au R, Pikula A, Wolf P A, DeStefano A L, Vasan R S and Seshadri S 2014 Serum brain-derived neurotrophic factor and the risk for dementia: the Framingham Heart Study JAMA Neurol 71 55–61
[30] Parhizkar S and Holtzman D M 2022 APOE mediated neuroinflammation and neurodegeneration in Alzheimer’s disease Seminars in Immunology 59 101594
[31] Wierenga K A and Pestka J J 2021 Omega-3 Fatty Acids And Inflammation - You Are What You Eat! Front Young Minds 9 601068
[32] Freund Levi Y, Vedin I, Cederholm T, Basun H, Faxén Irving G, Eriksdotter M, Hjorth E, Schultzberg M, Vessby B, Wahlund L-O, Salem Jr N and Palmblad J 2014 Transfer of omega-3 fatty acids across the blood–brain barrier after dietary supplementation with a docosahexaenoic acid-rich omega-3 fatty acid preparation in patients with Alzheimer’s disease: the OmegAD study Journal of Internal Medicine 275 428–36
[33] Heneka M T, Carson M J, El Khoury J, Landreth G E, Brosseron F, Feinstein D L, Jacobs A H, Wyss-Coray T, Vitorica J, Ransohoff R M, Herrup K, Frautschy S A, Finsen B, Brown G C, Verkhratsky A, Yamanaka K, Koistinaho J, Latz E, Halle A, Petzold G C and Kummer M P 2015 Neuroinflammation in Alzheimer’s disease The Lancet Neurology 14 388–405
[34] Wang Z, Zhang Z, Liu J, Guo M and Li H 2023 Panax Ginseng in the treatment of Alzheimer’s disease and vascular dementia Journal of Ginseng Research 47 506–14
[35] Zhang S, Liu F, Li J, Jing C, Lu J, Chen X, Wang D, Cao D, Zhao D and Sun L 2023 A 4.7-kDa polysaccharide from Panax ginseng suppresses Aβ pathology via mitophagy activation in cross-species Alzheimer’s disease models Biomedicine & Pharmacotherapy 167 115442
[36] Lee B C, Choe Y M, Suh G-H, Choi I-G, Kim H S, Hwang J, Yi D, Jhoo J H and Kim J W 2023 Ginseng intake and Alzheimer disease-specific cognition in older adults according to apolipoprotein ε4 allele status Front. Aging Neurosci. 15
[37] Kim J, Kim S H, Lee D-S, Lee D-J, Kim S-H, Chung S and Yang H O 2013 Effects of fermented ginseng on memory impairment and β-amyloid reduction in Alzheimer’s disease experimental models J Ginseng Res 37 100–7
[38] Lee M R, Yun B S, In O H and Sung C K 2011 Comparative Study of Korean White, Red, and Black Ginseng Extract on Cholinesterase Inhibitory Activity and Cholinergic Function J Ginseng Res 35 421–8
[39] Heo J-H, Park M-H and Lee J-H 2016 Effect of Korean Red Ginseng on Cognitive Function and Quantitative EEG in Patients with Alzheimer’s Disease: A Preliminary Study The Journal of Alternative and Complementary Medicine 22 280–5
[40] Heo J-H, Lee S-T, Oh M J, Park H-J, Shim J-Y, Chu K and Kim M 2011 Improvement of Cognitive Deficit in Alzheimer’s Disease Patients by Long Term Treatment with Korean Red Ginseng J Ginseng Res 35 457–61
[41] Belloy M E, Napolioni V and Greicius M D 2019 A Quarter Century of APOE and Alzheimer’s Disease: Progress to Date and the Path Forward Neuron 101 820–38
[42] Yamazaki Y, Zhao N, Caulfield T R, Liu C-C and Bu G 2019 Apolipoprotein E and Alzheimer disease: pathobiology and targeting strategies Nat Rev Neurol 15 501–18
[43] Ba M, Kong M, Li X, Ng K P, Rosa-Neto P and Gauthier S 2016 Is ApoE ɛ 4 a good biomarker for amyloid pathology in late onset Alzheimer’s disease? Transl Neurodegener 5 20
[44] Platt M P, Agalliu D and Cutforth T 2017 Hello from the Other Side: How Autoantibodies Circumvent the Blood–Brain Barrier in Autoimmune Encephalitis Front. Immunol. 8
[45] LeVine S M 2016 Albumin and multiple sclerosis BMC Neurol 16 47
[46] Freund-Levi Y, Eriksdotter-Jönhagen M, Cederholm T, Basun H, Faxén-Irving G, Garlind A, Vedin I, Vessby B, Wahlund L-O and Palmblad J 2006 ω-3 Fatty Acid Treatment in 174 Patients With Mild to Moderate Alzheimer Disease: OmegAD Study: A Randomized Double-blind Trial Arch Neurol 63 1402–8
[47] Quinn J F, Raman R, Thomas R G, Yurko-Mauro K, Nelson E B, Van Dyck C, Galvin J E, Emond J, Jack C R, Weiner M, Shinto L and Aisen P S 2010 Docosahexaenoic acid supplementation and cognitive decline in Alzheimer disease: a randomized trial JAMA 304 1903–11
[48] Xiang Y, Wang S, Wang L, Wang Z, Yao H, Chen L and Wang Y 2019 Effects of Ginsenoside Rg1 Regulating Wnt/ β -Catenin Signaling on Neural Stem Cells to Delay Brain Senescence Stem Cells International 2019 1–12
[49] Gong L, Yin J, Zhang Y, Huang R, Lou Y, Jiang H, Sun L, Jia J and Zeng X 2022 Neuroprotective Mechanisms of Ginsenoside Rb1 in Central Nervous System Diseases Front. Pharmacol. 13
[50] Shi H, Zhao J, Li Y, Li J, Li Y, Zhang J, Qiu Z, Wu C, Qin M, Liu C, Zeng Z, Zhang C and Gao L 2023 Ginsenosides Rg1 regulate lipid metabolism and temperature adaptation in Caenorhabditis elegans Journal of Ginseng Research 47 524–33
[51] Yu X, Li H, Lin D, Guo W, Xu Z, Wang L and Guan S 2021 Ginsenoside Prolongs the Lifespan of C. elegans via Lipid Metabolism and Activating the Stress Response Signaling Pathway International Journal of Molecular Sciences 22
[52] Abbott N J, Patabendige A A, Dolman D E, Yusof S R and Begley D J 2010 Structure and function of the blood-brain barrier Neurobiology of Disease 37 13–25
[53] Sofela S, Sahloul S and Song Y-A 2021 Biophysical analysis of drug efficacy on C. elegans models for neurodegenerative and neuromuscular diseases PLOS ONE 16 e0246496
[54] Lai C H, Chou C Y, Ch’ang L Y, Liu C S and Lin W 2000 Identification of novel human genes evolutionarily conserved in Caenorhabditis elegans by comparative proteomics Genome Research 10 703–713
[55] Alvarez J, Alvarez-Illera P, Santo-Domingo J, Fonteriz R I and Montero M 2022 Modeling Alzheimer’s Disease in Caenorhabditis elegans Biomedicines 10 288
[56] Alexander A G, Marfil V and Li C 2014 Use of Caenorhabditis elegans as a model to study Alzheimer’s disease and other neurodegenerative diseases Front. Genet. 5
[57] Carmichael O T, Pillai S, Shankapal P, McLellan A, Kay D G, Gold B T and Keller J N 2018 A Combination of Essential Fatty Acids, Panax Ginseng Extract, and Green Tea Catechins Modifies Brain fMRI Signals in Healthy Older Adults The Journal of nutrition, health and aging 22 837–46
[58] Lee J, Lee A, Kim J-H, Shin Y M, Kim S-J, Cho W D and Lee S I 2020 Effect of Omega-3 and Korean Red Ginseng on Children with Attention Deficit Hyperactivity Disorder: An Open-Label Pilot Study Clin Psychopharmacol Neurosci 18 75–80
[59] Tangrodchanapong T, Sobhon P and Meemon K 2020 Frondoside A Attenuates Amyloid-β Proteotoxicity in Transgenic Caenorhabditis elegans by Suppressing Its Formation Front. Pharmacol. 11
[60] Bhatia S, Rawal R, Sharma P, Singh T, Singh M and Singh V 2022 Mitochondrial Dysfunction in Alzheimer’s Disease: Opportunities for Drug Development Curr Neuropharmacol 20 675–92
[61] Sweeney M D, Sagare A P and Zlokovic B V 2018 Blood–brain barrier breakdown in Alzheimer disease and other neurodegenerative disorders Nat Rev Neurol 14 133–50
[62] Cline E N, Bicca M A, Viola K L and Klein W L 2018 The Amyloid-β Oligomer Hypothesis: Beginning of the Third Decade Journal of Alzheimer’s Disease 64 S567–610
[63] Anon Strain: CL2355, Genotype: smg-1(cc546) dvIs50 I. - Caenorhabditis Genetics Center (CGC) - College of Biological Sciences
[64] Hart A C 2006 Behavior WormBook: The Online Review of C. elegans Biology [Internet] (WormBook)
[65] Margie O, Palmer C and Chin-Sang I 2013 C. elegans Chemotaxis Assay J Vis Exp 50069
[66] Lee M, Lee S-H, Kim M-S, Ahn K-S and Kim M 2022 Effect of Lactobacillus dominance modified by Korean Red Ginseng on the improvement of Alzheimer’s disease in mice Journal of Ginseng Research 46 464–72
[67] Lim S W, Shin Y J, Luo K, Quan Y, Cui S, Ko E J, Chung B H and Yang C W 2019 Ginseng increases Klotho expression by FoxO3-mediated manganese superoxide dismutase in a mouse model of tacrolimus-induced renal injury Aging (Albany NY) 11 5548–69
[68] Château M-T, Araiz C, Descamps S and Galas S 2010 Klotho interferes with a novel FGF-signalling pathway and insulin/Igf-like signalling to improve longevity and stress resistance in Caenorhabditis elegans Aging (Albany NY) 2 567–81
[69] Chávez-Castillo M, Gotera M P, Duran P, Díaz M P, Nava M, Cano C, Díaz-Camargo E, Cano G, Cano R, Rivera-Porras D and Bermúdez V 2025 Neuroprotective Role of Omega-3 Fatty Acids: Fighting Alzheimer’s Disease Molecules 30
[70] Watts J L 2016 Using Caenorhabditis elegans to Uncover Conserved Functions of Omega-3 and Omega-6 Fatty Acids Journal of Clinical Medicine 5
Document information
Published on 09/03/26
Submitted on 20/02/25
Volume 8, 2026
Licence: CC BY-NC-SA license
Share this document
Keywords
claim authorship
Are you one of the authors of this document?