Summary
Objective
The study presents a matched-pair analysis of robot-assisted laparoscopic partial nephrectomy (RALPN) versus radiofrequency ablation (RFA) to compare the perioperative incidence of complications and chronic kidney disease (CKD).
Methods
All 46 RFA and 206 RALPN cases from June 2005 to December 2011 were retrospectively reviewed from the medical records and were matched 1:1 based on propensity scores by sex, tumor size, tumor laterality of kidney, tumor location within the kidney, and clinical T stage. Hilar vessel clamping was performed in all RALPN patients. The estimated glomerular filtration rate was used to define the CKD of < 60 mL/minute/1.73 m2 by the Modification of Diet in Renal Disease equation. All patients with baseline CKD or solitary kidney were excluded prior to the matching analysis. The complication was noted with modified Clavien grades ≥ 3. Statistical analysis was performed to compare the perioperative incidence of complications and CKD.
Results
A total of 27 matched pairs of RFA and RALPN patients were enrolled for analyzing CKD and perioperative complications. The better general conditions, higher estimated blood loss and transfusion rates, and longer operative time and hospital stay were observed significantly in RALPN patients (p < 0.05). Matched analysis demonstrated that the incidences of both perioperative complications (p = 0.434) and of CKD (p = 0.500) were not significantly different. No complication higher than Grade 4 was detected in either group.
Conclusion
Despite the intraoperative renal ischemia and invasiveness of the procedure associated with RALPN, the incidence of perioperative complication and of CKD developing rates were statistically similar.
Keywords
ablation techniques;renal cell carcinoma;laparoscopy;nephrectomy;pulsed radiofrequency ablation treatment
1. Introduction
In the past number of decades, radical nephrectomy (RN) was still considered the gold standard for the treatment of renal cell carcinoma (RCC). However, many patients deemed unsuitable for RN owing to their underlying preoperative conditions such as solitary kidney, renal insufficiency, and high-risk comorbidities underwent other minimally invasive nephron-sparing procedures such as ablative therapy or partial nephrectomy (PN).
Many reports showed that PN yielded not only comparable 5- and 10-year survival rates to RN, but also better clinical outcomes especially in patients with high-risk comorbidities or with selected RCCs for preserving the postoperative renal function.1 ; 2 To reduce the procedural complications, and to spare renal function and prevent chronic kidney disease (CKD), radiofrequency ablation (RFA) therapy has demonstrated comparable clinical and oncologic outcomes in select patients with small RCCs during short- and long-term follow-ups.3 ; 4 Robot-assisted laparoscopic partial nephrectomy (RALPN) also showed similar surgical and renal preserving outcomes to the open surgery.5
No study as yet has evaluated RALPN compared to RFA using comparable patient groups equally matched in terms of age, sex, tumor location, tumor laterality, and clinical T stage. This study presented a propensity-matched pair analysis of RALPN and RFA performed by a heterogeneous group of surgeons and radiologists in two hospitals to compare the incidences of perioperative (peri-) complications and of CKD between RALPN and RFA as a nephron-sparing procedure.
2. Materials and methods
The Institutional Review Boards of the participating institutions (Seoul National University Hospital, Seoul, Korea; Seoul National University Bundang Hospital, Seoul, Korea, B 1202/145-102) approved the retrospective review of the medical records of patients with a single renal mass without LN invasion nor metastasis managed by either RFA or RALPN decided under the surgeons' and patients' preferences and patients' general performance states between June 2005 to December 2011.
The overall inclusion criteria for RFA and RALPN included patients aged over 19 years, a newly developed solid renal mass smaller than approximately 4 cm with RCC confirmation via computerized tomography scan or magnetic resonance images, and with a normal contralateral kidney. The specific inclusion criteria for RFA were patients: (1) who refused the recommended surgery (otherwise conventional surgery was first chosen for the treatment) and had small tumors that were easy to access using RFA, (2) who were unable to undergo surgery because of underlying diseases, and (3) in whom renal function preservation was paramount. The exclusion criteria included any advanced states of RCC whether it indicated positive lymph nodes or metastasis, and any patients with baseline serum creatinine level > 1.4 ng/dL or solitary kidney or calculated an estimated glomerular filtration rate (eGFR) < 60 mL/minute/1.72 m2, which was calculated according to the Modification of Diet in Renal Disease (MDRD) formula:
|
|
(1) |
(if female) by considering serum creatinine, sex, and age. A total of 60 RFAs were performed in 41 patients and 206 RALPNs were performed in 203 patients. All RALPNs and RFAs were performed by a heterogeneous group of six experienced surgeons in PN and two experienced radiologists in ablation therapy.
The RFA was impedance-based and performed percutaneously using a single probe, under ultrasonic (US) and fluoroscopic guidance. A 17-gauge internally cooled tip radiofrequency (RF) electrode (Cool-tip; Radionics, Burlington, MA, USA) with a 3-cm tip was placed near the targeted tumor under US guidance. The electrode tip location was verified with different projections to ensure the juxtapositioning of the tip and the renal pelvis without perforation. RF energy was applied at the maximal allowable output (140 W) for 12 minutes per tumor, at a target temperature of 105°C. The applied current, power output, and impedance were continuously monitored during RF ablation, and these parameters were recorded automatically using Real Time Graphics Software version 2.0 (Radionics).
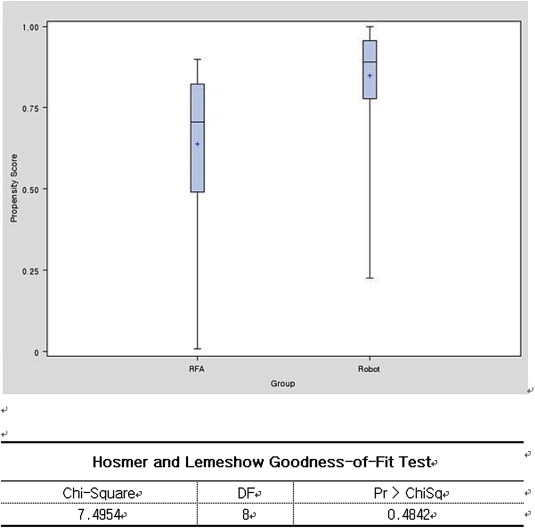
Patients were matched for age, sex, tumor size, clinical T stage, tumor location, and renal laterality, using optimal matching based on propensity scores (Fig. 1). Matching the propensity scores of the smallest absolute distance across all matched pairs was used to compare individually pairwise matching between RFA and RALPN, and the bigger RALPN group was used as a control.6 ; 7 A follow-up protocol after RALPN and RFA was performed according to a consistent protocol with postoperative follow-up of the European Association of Urology guidelines in all patients including renal functional measurements with eGFR-MDRD, which were made prior to the surgery and at 4–6 weeks, 3 months, 6 months, and 12 months post-surgery, semiannually until the 5th year, and annually thereafter.8
|
|
|
Figure 1. Box-plot of propensity scores between RFA and RALPN groups. This plot describes the demographics of RFA and RALPN groups after they were matched based on propensity scores. RALPN = robot-assisted laparoscopic partial nephrectomy; RFA = radiofrequency ablation. |
To evaluate the incidence rate of developing perioperative complications and CKD, different matching pairs of enrollment were used. The matching variables of tumor location and kidney laterality were divided into endophytic, exophytic, mesophytic, and hilar categories, and into right and left. All renal tumor images were classified according to the RENAL nephrometry score, which consists of the following parameters: R (radius), E (exophytic/endophytic), N (nearness), A (anterior/posterior), and L (location), as described previously.9 The clinical T stage was used according to the classification of the International Union Against Cancer/American Joint Committee on Cancer, 2009. Other clinicopathologic data and related variables to CKD and perioperative complications were evaluated between the two groups.
The primary clinical outcomes were perioperative complications, and renal function. Perioperative complications were graded using the modified Clavien classification,10 which was validated for PN11 and ablation therapy.12 A perioperative complication was defined as any major complication classified as Clavien grade ≥ 3 after either RFA or RALPN within 1 month. Functional outcome was based on an eGFR-MDRD, and CKD is defined as eGFR < 60 mL/minute/1.73 m2.
Group differences in continuous and categorical data were compared using the independent t test or Wilcoxon signed rank sum test, and chi-square or Fishers exact tests, respectively. Intrapersonal changes in eGFR were assessed using paired t tests. The propensity score was calculated with an SAS macro after modeling logistic regression and McNemar test, and using the penalized maximum likelihood ratio to compare between the two groups. All analyses were performed with the SAS statistical software (SAS system for Windows, version 9.2; SAS institute, Cary, NC, USA). A p value < 0.05 was considered statistically significant.
3. Results
During a median follow-up of 14.6 months, 27 paired cases of RFA and of RALPN were matched to evaluate the incidence of complications and the renal function for developing postoperative incidence of CKD. Among the 54 cases, two RALPN patients and two RFA patients died—three from cancer-related and one from noncancer-related causes—at a median follow-up of 6.5 months after the treatment. For patients with RALPN, hilar vessel clamping was performed in all cases with a mean warm ischemic time of 20.4 (standard deviation ± 6.9) minutes (Table 1).
| Variables | RALPN (n = 27) | RFA (n = 27) | p |
|---|---|---|---|
| Age (y) | 60.33 ± 15.61 | 58.67 ± 11.60 | 0.627 a |
| Sex (male/female) | 19 (70.4)/8 (29.6) | 22 (81.5)/5 (18.5) | 0.549 b |
| Body mass index (kg/m2) | 25.9 ± 3.4 | 26.6 ± 3.1 | 0.127 |
| Diabetes | 4 (14.8) | 5 (18.5) | > 0.99 c |
| Hypertension | 16 (59.3) | 11 (40.7) | 0.101 c |
| ASA score | 1.0 ± 0.2 | 1.6 ± 0.5 | < 0.001 |
| 1 | 26 | 14 | |
| 2 | 1 | 13 | |
| Follow-up duration (mo) | 10.9 ± 7.0 | 16.7 ± 10.5 | 0.068 |
| Preop. Cr (mg/dL) | 0.9 ± 0.2 | 1.2 ± 0.2 | < 0.001 |
| Preop. Hb (mg/dL) | 14.2 ± 1.2 | 13.0 ± 1.7 | 0.003 |
| Preop. eGFR (mL/min/1.73 m2) | 86.7 ± 14.1 | 84.0 ± 23.5 | 0.049 |
| Tumor size | 1.77 ± 0.96 | 1.8 ± 0.81 | 0.928 a |
| Laterality | 0.267 b | ||
| 1: left | 16 (59.3) | 11 (40.7) | |
| 2: right | 11 (40.7) | 16 (29.3) | |
| Location | 0.462 b | ||
| 1: exophytic | 13 (50.0) | 13 (50.0) | |
| 2: mesophytic | 4 (15.3) | 2 (7.7) | |
| 3: endophytic | 8 (30.8) | 8 (30.8) | |
| 4: hilar | 1 (3.9) | 3 (11.5) | |
| RENAL score (sum) | 6.5 ± 1.7 | 6.3 ± 1.6 | 0.748 |
| R | 1.1 ± 0.2 | 1.1 ± 0.3 | 0.973 |
| E | 2.1 ± 0.8 | 2.0 ± 0.7 | 0.671 |
| N | 1.8 ± 0.9 | 1.8 ± 1.0 | 0.832 |
| A | 0.5 ± 0.5 | 0.8 ± 0.4 | 0.086 |
| L | 1.6 ± 0.7 | 1.4 ± 0.7 | 0.591 |
| Tumor distance to collecting system or sinus (mm) | 9.0 ± 6.3 | 7.5 ± 6.8 | 0.462 |
| Clinical T stage | 0.513 b | ||
| T1 | 22 (81.5) | 23 (85.2) | |
| T2 | 0 | 0 | |
| T3 | 5 (18.5) | 4 (14.8) | |
| Total operative time (min) | 167.9 ± 66.0 | NA | NA |
| Warm ischemic time (min) | 20.4 ± 6.9 | NA | NA |
| Safety margin (mm) | 3.9 ± 3.1 | NA | NA |
| Estimated blood loss (mL) | 162.0 ± 119.2 | NA | NA |
| Transfusion | 1 (3.7) | 0 | > 0.99 c |
| Histology | 27 (100) | 5 (18.5) | < 0.003 c |
| Clear cell | 19 (70.1) | 2 (5.4) | |
| Papillary | 4 (14.8) | 1 (3.7) | |
| Chromophobe | 1 (3.7) | 0 | |
| Angiomyolipoma | 1 (3.7) | 0 | |
| Oncocytoma | 2 (5.4) | 2 (5.4) | |
| Hospital stay (d) | 6.2 ± 1.5 | 3.0 ± 2.2 | < 0.001 |
| Postop. Hb (mg/dl) | 13.3 ± 1.3 | 12.5 ± 1.5 | 0.084 |
| Postop. eGFR (mL/min/1.73 m2) | 80.5 ± 16.5 | 81.3 ± 27.8 | 0.303 |
| Postop. Cr change (mg/dl) | 0.02 ± 0.21 | 0.03 ± 0.41 | 0.912 |
| eGFR change (mL/min/1.73 m2) d | 6.2 ± 2.4 | 2.8 ± 0.7 | 0.049 |
| Postop. CKD | 1 (3.7) | 3 (11.1) | 0.500 b |
| Complication | 3 (11.1) | 4 (14.8) | 0.434 e |
| Pyelo/pyonephritis | 0 | 1 (3.7) | |
| Hydronephrosis | 0 | 1 (3.7) | |
| Wound | 1 (3.7) | 0 | |
| Bleeding | 2 (7.4) | 0 | |
| Urine leak | 0 | 2 (7.4) | |
| Tumor recurrence | 2 (7.4) | 1 (3.7) | 0.669 |
| Death | 0.764 | ||
| Cancer-related cause | 2 (7.4) | 1 (3.7) | |
| Noncancer-related cause | 0 | 1 (3.7) |
Data are presented as n (%) or mean ± SD.
ASA = American Society of Anesthesiologists score; CKD = chronic kidney disease; Cr = creatinine; GFR = glomerular filtration rate (MDRD); NA = not available; Preop. = preoperative; Postop. = postoperative; RALPN = robot-assisted laparoscopic partial nephrectomy; RFA = radiofrequency ablation.
a. Paired t test.
b. McNemar test.
c. Fishers exact test.
d. eGFR change is the estimated glomerular filtration change between before and after operation or procedure.
e. Conditional logistic regression analysis.
For comparison of baseline and posttreatment clinical parameters between RALPN and RFA, univariate analysis revealed that baseline general performance states with serum creatinine, hemoglobin, eGFR, and American Society of Anesthesiologists score were significantly better in RALPN and that post-eGFR change and hospital stay were significantly lower and shorter in RFA (p < 0.05, Table 1). Other operative parameters of RALPN were noncomparable to those of RFA with greater mean estimated blood loss (162.0 ± 119.4 mL), longer operative time (167.9 ± 66.0 minutes), and higher transfusion rate (3.7%). Biopsy prior to RFA was performed in only 18 (66.6%) cases, and five (18.5%) cases confirmed the cell histology.
Among the 27 RFA matched patients, CKD developed in three patients (11.1%) with a mean eGFR change from 84.0 (± 23.5) mL/minute/1.73 m2 to 81.3 (± 27.8) mL/minute/1.73 m2 after 6 months, representing a mean eGFR difference of 2.8 (± 0.7) mL/minute/1.73 m2. For 27 RALPN patients, CKD developed in one patient (3.7%), and the mean eGFR decreased from 86.7 (± 14.1) mL/minute/1.73 m2 to 80.5 (± 16.5) mL/minute/1.73 m2, with a mean eGFR difference of 6.2 (± 2.4) mL/minute/1.73 m2. Propensity-matched analysis demonstrated that the incidences of CKD were not significantly different between RFA and RALPN (p = 0.500; Table 2).
| Group | Total | p | ||
|---|---|---|---|---|
| RALPN | RFA | |||
| CKD incidence | ||||
| Non-CKD | 26 (96.3) | 24 (92.6) | 50 | 0.500 a |
| CKD | 1 (3.7) | 3 (11.1) | 4 | |
| Complication incidence | ||||
| No complication | 24 (88.9) | 23 (85.2) | 47 | 0.434 a |
| With complication | 3 (11.1) | 4 (14.8) | 7 | |
Data are presented as n (%).
CKD = chronic kidney disease; RALPN = robot-assisted laparoscopic partial nephrectomy; RFA = radiofrequency ablation.
a. McNemar test.
For perioperative complications, no major complication of Grade 4 was detected in either group; however, four (14.8%) patients developed complications in RFA and three (11.1%) patients did so in RALPN, in which the incidences of major complications of Grade ≥ 3 were not significantly different in the matched analysis (p = 0.434; Table 2). The complications in RFA consisted of two urinary leaks necessitating the intervential insertion of percutaneous drainage, one flank pain with moderate hydronephrosis that resolved after the insertion of a ureteral stent, and one severe pyonephritis managed by RN after the failure of medical management. According to the modified Clavien classification, there were three Grade 3a (8.0%) and one Grade 3b (2.6%) complications. For complications in the RALPN group, there was one infected wound problem that resolved after surgical therapy (3.7%, Grade 3a), and two prolonged bleeding cases necessitating two transfusions with radiologic intervential embolizations for pseudoaneurysm (7.4%, Grade 3a).
4. Discussion
During the past few decades, open PN was considered the established treatment for RCCs < 4 cm in size with comparable clinico-oncologic outcomes to RN and with better preservation of the renal function, thus preventing postoperative CKD.1 ; 2 Many studies reported that RALPN was superior to open PN in terms of intraoperative blood loss and length of hospital stay. Its renal functional change was proven to be not different from that of PN.5 ; 13
As the advanced diagnostic imaging techniques had led to a marked diagnostic increase of small renal masses with no evidence of metastasis in patients with multiple comorbidities or with a solitary kidney, the rate of PN might increase the risk of surgery for these patients. These facts helped to introduce alternative thermal ablation techniques such as RFA, which are reserved for carefully selected high-surgical-risk patients with renal masses smaller than approximately 4 cm, reportedly without compromising the oncologic outcomes to PN (like the results of this study), in that the similar tumor recurrence and insignificant difference of cancer-related death rates happened all in patients with Stage 3a RCC (Table 1).4 ; 14 And the reasons behind the better preservation of renal function in RFA compared with PN were attributable to ischemic injury during hilar clamping for perfusion and reperfusion injuries, invasive surgical resection or electrocauterization of the renal parenchyma as well as tumors, and increased intraoperative bleeding loss in PN.15 These speculations on the reduction of postoperative renal function being greater than that observed in RFA were also easily applied to RAPLN. However, no comparison of RALPN and RFA has been carried out, and no reports have been presented on this topic to date. Therefore, this study marks the first effort to compare the renal function and the incidence of developing CKD, as well as perioperative complication(s) between RALPN and RFA. To compare these two procedures, it was important to consider the characteristics of tumors as well as the patients' demographic data so that the two study populations would be evenly matched in terms of age, sex, tumor size, clinical T stage, and its renal laterality and locations within the kidney.
This study demonstrated that RFA and RALPN matched patients had almost no serious postoperative reductions in eGFR that would be sufficient to cause postoperative CKD. Therefore, the incidence of CKD after the treatment was not statistically different between the two groups (RFA 3/27 vs. RALPN 1/27, p = 0.500). This finding was similar to that in other reports, wherein the difference in CKD incidence was observed between PN and thermal ablation. 3 ; 16
As regards the predisposing characteristics of four patients who developed CKD after the treatment, they were younger than 65 (range 36–65) years and all were staged T1a (tumor size range 0.9–2 cm), they had the same sex ratio (2 males and 2 females), and they had good Eastern Cooperative Oncology Group status (2 Grade 0, and 2 Grade 1 with diabetes (DM) and hypertension (HTN)). Their renal tumors were located more in the left side than in the right side (3:1), and two were endophytic tumors and the other two were exophytic tumors. Their eGFRs were between 60.7 mL/minute/1.73 m2 and 89.4 mL/minute/1.73 m2 prior to the treatment, and between 55.0 mL/minute/1.73 m2 and 59.3 ml/minute/1.73 m2 after the treatment. All the predisposing factors of CKD including age, sex, underlying diseases, and tumor locations and sizes showed no significant findings owing to the limited number of CKD patients in this study.
Other interesting findings were observed in changes of eGFR. First, in spite of the insignificant differences in terms of developing CKD, the change differences of eGFR between baseline and after treatment were significant after 6 months, and the decrease of eGFR in RALPN was greater than that in RFA [6.2 ± 2.4 mL/minute/1.73 m2 (RALPN) vs. 2.8 ± 0.7 (RFA) mL/minute/1.73 m2, p = 0.049]. This meant that RFA resulted in less kidney functional deterioration compared with RALPN. This result might be explained by previously suggested explanations—ischemic injury during the clamping procedure, cauterizing injury, and resected volume of renal parenchyma in PN. In this study, the warm ischemic time in RALPN was 20.4 ± 6.9 minutes, which was less than a reportedly tolerable time of 28 minutes for renal ischemic injury, so that the effect of ischemic injury might not be negatively great on renal function. Nevertheless, our results showed a significant decrease of renal function after RALPN compared with that after RFA in consideration of post-eGFR change.
Although this is the first comparison report dealing with the renal function and perioperative complications of RALPN and RFA, similar previous comparative studies between PN and thermal ablation have been reported, in which RFA performed better in preserving renal function and PN negatively affected renal function more than RFA did in small RCCs.14; 15 ; 17 Another recent retrospective study that compared RALPN and cryoablation in a large number of patients during long-term follow-up showed that RALPN offers significantly better renal preservation than cryoablation.18 However, these studies did not match RCC patients for age, sex, or tumor size, location, laterality, and stage. Without considering tumor size and location, comparisons of surgery and ablative therapy are difficult. Previous studies compared different and widely ranging tumor sizes that were treated by surgery versus varied and smaller-sized tumors treated with ablative therapy.17 ; 18 Therefore, it was not surprising that their results are different from ours.
A second interesting finding from our results was that some improvement of eGFR after the operation or procedures was observed in both groups [RFA, 9/27 (33.3%); RALPN 10/27 (37%); data not shown in tables]. The observation that eGFR did not decrease after the treatment was speculative because the procedural insult to the small treatment area was insufficient to cause renal function deterioration after the procedure, and the remnant parenchyma of the affected kidney and the contralateral normal kidney were stimulated to compensate for decreased renal function by expressing multiple mediators.19 ; 20 Additionally, the local hypoxia-inducing effect of tumor on the juxtaposed renal parenchyma disappeared after tumor removal or ablation. The disappearance of tumor inflammatory immune responses enabled renal function to restore normoxia by erythrocytosis of RCC21 and several inflammatory immune mediators.22
Another attendant objective in our study was the comparison of major complication rates between RFA and RALPN, conclusively resulting in similar complication rates and grades [RFA 4/27 (14.8%) vs. RALPN 3/27 (11.1%), 4 RFA Grade 3a vs. 3 RALPN with 2 Grade 3a and 1 Grade 3b, respectively; p > 0.05]. Our results were consistent with other analyses that compared ablative therapy with PN, as they also showed similar complication rates in both groups. 15 ; 23 Some reports showed RALPN to be superior to PN of small RCCs in terms of clinicopathological outcomes including perioperative complications.5 However, our results on enrolled cases selected after matching important baseline clinical parameters to propensity scores demonstrated no statistical superiority of RALPN over RFA, but similarity in perioperative complication.
For the relationship with complication(s) and multiple treatments in the same patient, three RFA patients (11.1%) had more than two procedural histories because of multiple tumors. However, no perioperative complication occurred in those RFA patients, although it had been reported that multiple procedures correlated with the incidence of perioperative complication due to multiple ablations of normal renal tissue including the tumor tissue.24 ; 25
The complication rate of RFA in this study appeared relatively high compared to that of other reports (incidence 9.3–11.0%, and grade ≥3, 4.3–6.6%),24 ; 25 whereas the incidence rate of RALPN complication with two bleeding and one wound dehiscence was relatively similar to that in previous reports (5–12%).5 One suggested explanation for the high incidence rate of RFA complication was that the RFA used in this study was performed percutaneously under US and fluoroscopic guidance rather than under computerized tomographic (CT) guidance, which was the option used in other previous studies. CT-guided RFA is known to yield better results, with higher accuracy in the treatment of small renal tumors, thereby resulting in lower complication rates.26
Discussion of the high incidence rate and specific complications after RFA was carried out in this study. Two urinomas from urinary leakages occurred, necessitating percutaneous drainage, and one urinary obstruction with hydronephrosis owing to mild stricture in the collecting system required insertion of a ureteral stent that resolved completely after its removal after 2 weeks. Urinomas usually resolve with ureteral stenting, whereas strictures in the collecting system may require further endopyelotomy or reconstructive surgery after ureteral stenting.27 These complications were well known complications in RFA because of the locations of the tumors near the pelvocalyceal system (or ureteropelvic junction), such that the thermal injury with coagulation necrosis in the pelvocalyceal system results in either urine leakage or stricture formation causing hydronephrosis.28 One patient among the three suggested patients had a tumor near the pelvocalyceal system, but he was selected for RFA because he was unable to undergo other surgeries requiring general anesthesia owing to an underlying comorbidity. For such cases, although RFA has been used to treat small renal tumors of any size and any location even in the central hilum and renal sinus near the major vessels,29 considerable care should be exercised when treating tumors especially those lying in continuity with the collecting system of renal hilum and major vessels, for which RFA is not highly recommended.30
Another possibility of urine leakage in this study might be related to the 17-gauge Cooltip probe used in our RFA procedure. The 17G single probe Cooltip might leave a large bore hole in the tumor, making leaks more likely compared with the 25G tines used in the array-type probes. However, to prevent urinary leakage from occurring after the RFA, some form of preprocedural management such as ureteral stenting might be helpful to avoid complications of the urinary system in some high-risk patients. Therefore, it is important to establish a close collaboration between the urologist and the interventional radiologist in such high-risk patients with small renal tumors.
The last complicated case in RFA was a patient with pyonephritis who underwent nephrectomy, which was related to infection of the affected kidney. The nephrectomy case had multiple underlying comorbidities including diabetes and steroid-induced immune suppression, as a result of which pyelonephritis progressed to pyonephritis despite the medical treatment. Pyelonephritis happened because RFA produces thermal coagulation necrosis and protein denaturation, which can result in inflammation of the affected renal parenchyma.31
Our study has several limitations. This was a retrospective review of a relatively small group of patients with different comorbidities and short-term follow-up. As the follow-up time lengthens, the CKD prevalence might be increasingly affected, because renal function deteriorated over time and one of the most important predisposing factors for CKD was age.1; 3 ; 4 Mukkamala et al32 recently reported the postoperative time-related CKD prevalence in their study. They noted that clinically significant CKD progressed in a small number of patients 5 years after the treatment, but in almost one-half of their patients, it occurred 10 years after the surgery. However, in this study, the prevalence of CKD after 5 years might not be as high as, or even similar to, what one might expect, because many predisposing factors had already been matched. Second, the highly specialized and experienced surgeons and radiologists were composed of a heterogeneous group from two tertiary teaching hospitals to render the skill differences among the professional staff. Third, the evolution of RFA technology over the study period might have resulted in the overestimation of RFA complications and the underestimation of RFA-associated CKD prevalence.
5. Conclusion
Despite intraoperative renal ischemia and the invasiveness of the procedures associated with RALPN, the perioperative complications and CKD developing rates were statistically similar in a propensity-matched control study. However, the study shows that RFA had slightly better renal preservation effects than RALPN in high-risk patients with small RCCs.
References
- 1 S.P. Kim, R.H. Thompson, S.A. Boorjian, et al.; Comparative effectiveness for survival and renal function of partial and radical nephrectomy for localized renal tumors: a systematic review and meta-analysis; J Urol, 188 (2012), pp. 51–57
- 2 C.J. Weight, A.F. Fergany, P.W. Gunn, B.R. Lane, A.C. Novick; The impact of minimally invasive techniques on open partial nephrectomy: a 10-year single institutional experience; J Urol, 180 (2008), pp. 84–88
- 3 K.J. Kiriluk, S.A. Shikanov, G.D. Steinberg, A.L. Shalhav, D.A. Lifshitz; Laparoscopic partial nephrectomy versus laparoscopic ablative therapy: a comparison of surgical and functional outcomes in a matched control study; J Endourol, 25 (2011), pp. 1867–1872
- 4 S.P. Psutka, A.S. Feldman, W.S. McDougal, F.J. McGovern, P. Mueller, D.A. Gervais; Long-term oncologic outcomes after radiofrequency ablation for t1 renal cell carcinoma; Eur Urol, 63 (2013), pp. 486–492
- 5 A. Masson-Lecomte, D.R. Yates, V. Hupertan, et al.; A prospective comparison of the pathologic and surgical outcomes obtained after elective treatment of renal cell carcinoma by open or robot-assisted partial nephrectomy; Urol Oncol, 31 (2013), pp. 924–930
- 6 G. Heinze, M. Ploner; Fixing the nonconvergence bug in logistic regression with SPLUS and SAS; Comput Methods Prog Biomed, 71 (2003), pp. 181–187
- 7 G. Heinze, M. Schemper; A solution to the problem of separation in logistic regression; Stat Med, 21 (2002), pp. 2409–2419
- 8 B. Ljungberg, N.C. Cowan, D.C. Hanbury, et al.; EAU guidelines on renal cell carcinoma: the 2010 update; Eur Urol, 58 (2010), pp. 398–406
- 9 R.M. Hegg, G.D. Schmit, A.N. Kurup, A.J. Weisbrod, S.A. Boorjian, T.D. Atwell; Ultrasound-guided transhepatic radiofrequency ablation of renal tumors: a safe and effective approach; Cardiovasc Intervent Radiol, 37 (2014), pp. 508–512
- 10 D. Dindo, N. Demartines, P.A. Clavien; Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey; Ann Surg, 240 (2004), pp. 205–213
- 11 M. Waldert, S. Waalkes, T. Klatte, et al.; External validation of the preoperative anatomical classification for prediction of complications related to nephron-sparing surgery; World J Urol, 28 (2010), pp. 531–535
- 12 M.P. Laguna, P. Beemster, V. Kumar, et al.; Perioperative morbidity of laparoscopic cryoablation of small renal masses with ultrathin probes: a European multicentre experience; Eur Urol, 56 (2009), pp. 355–361
- 13 S. Lee, J. Oh, S.K. Hong, S.E. Lee, S.S. Byun; Open versus robot-assisted partial nephrectomy: effect on clinical outcome; J Endourol, 25 (2011), pp. 1181–1185
- 14 H.H. Sung, B.K. Park, C.K. Kim, H.Y. Choi, H.M. Lee; Comparison of percutaneous radiofrequency ablation and open partial nephrectomy for the treatment of size- and location-matched renal masses; Int J Hyperthermia, 28 (2012), pp. 227–234
- 15 G.C. Hui, K. Tuncali, S. Tatli, P.R. Morrison, S.G. Silverman; Comparison of percutaneous and surgical approaches to renal tumor ablation: metaanalysis of effectiveness and complication rates; J Vasc Interv Radiol, 19 (2008), pp. 1311–1320
- 16 C.R. Mitchell, T.D. Atwell, A.J. Weisbrod, et al.; Renal function outcomes in patients treated with partial nephrectomy versus percutaneous ablation for renal tumors in a solitary kidney; J Urol, 186 (2011), pp. 1786–1790
- 17 S.M. Lucas, J.M. Stern, M. Adibi, I.S. Zeltser, J.A. Cadeddu, G.V. Raj; Renal function outcomes in patients treated for renal masses smaller than 4 cm by ablative and extirpative techniques; J Urol, 179 (2008), pp. 75–79
- 18 J. Guillotreau, G.P. Haber, R. Autorino, et al.; Robotic partial nephrectomy versus laparoscopic cryoablation for the small renal mass; Eur Urol, 61 (2012), pp. 899–904
- 19 A.I. Katz, F.G. Toback, M.D. Lindheimer; The role of renal “work” in compensatory kidney growth; Yale J Biol Med, 51 (1978), pp. 331–337
- 20 C. Fleck, H. Braunlich; Kidney function after unilateral nephrectomy; Exp Pathol, 25 (1984), pp. 3–18
- 21 B. Kvarstein, R. Lindemann, W. Mathisen; Renal carcinoma with increased erythropoietin production and secondary polycythemia; Scand J Urol Nephrol, 7 (1973), pp. 178–180
- 22 M. Lahn, P. Fisch, G. Kohler, et al.; Pro-inflammatory and T cell inhibitory cytokines are secreted at high levels in tumor cell cultures of human renal cell carcinoma; Eur Urol, 35 (1999), pp. 70–80
- 23 T. Klatte, J. Mauermann, G. Heinz-Peer, et al.; Perioperative, oncologic, and functional outcomes of laparoscopic renal cryoablation and open partial nephrectomy: a matched pair analysis; J Endourol, 25 (2011), pp. 991–997
- 24 A.Z. Weizer, G.V. Raj, M. O'Connell, C.N. Robertson, R.C. Nelson, T.J. Polascik; Complications after percutaneous radiofrequency ablation of renal tumors; Urology, 66 (2005), pp. 1176–1180
- 25 T.D. Atwell, G.D. Schmit, S.A. Boorjian, et al.; Percutaneous ablation of renal masses measuring 3.0 cm and smaller: comparative local control and complications after radiofrequency ablation and cryoablation; AJR, 200 (2013), pp. 461–466
- 26 A. Boss, S. Clasen, M. Kuczyk, F. Schick, P.L. Pereira; Image-guided radiofrequency ablation of renal cell carcinoma; Eur Radiol, 17 (2007), pp. 725–733
- 27 M.G. Oefelein; Delayed presentation of urinoma after radiofrequency ablation-assisted laparoscopic partial nephrectomy; J Endourol, 20 (2006), pp. 27–30
- 28 E.M. Merkle, S.G. Nour, J.S. Lewin; MR imaging follow-up after percutaneous radiofrequency ablation of renal cell carcinoma: findings in 18 patients during first 6 months; Radiology, 235 (2005), pp. 1065–1071
- 29 B.K. Park, C.K. Kim; Complications of image-guided radiofrequency ablation of renal cell carcinoma: causes, imaging features and prevention methods; Eur Radiol, 19 (2009), pp. 2180–2190
- 30 S. Park, J.A. Cadeddu; Outcomes of radiofrequency ablation for kidney cancer; Cancer Control, 14 (2007), pp. 205–210
- 31 P. Mertyna, M.W. Dewhirst, E. Halpern, W. Goldberg, S.N. Goldberg; Radiofrequency ablation: the effect of distance and baseline temperature on thermal dose required for coagulation; Int J Hyperthermia, 24 (2008), pp. 550–559
- 32 A. Mukkamala, C. He, A.Z. Weizer, et al.; Long-term renal functional outcomes of minimally invasive partial nephrectomy for renal cell carcinoma; Urol Oncol (2014 May 17) pii: S1078-1439(14)00154-9
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?