Abstract
We present a 15-year-old female patient with an anaphylactic reaction to a jellyfish sting, sustained while surfing in the Mediterranean Sea. She experienced immediate difficulty in breathing, hoarseness and itching and was taken by ambulance to the emergency department, receiving intramuscular adrenaline on the way. She presented with periorbital swelling and facial edema and improved with systemic steroids and antihistamines. She was discharged 2 days later with allergy service follow up at our institution. This is the first case report documenting anaphylaxis due to Mediterranean jellyfish envenomation.
Keywords
Jellyfish ; Rhopilema nomadica ; Anaphylaxis ; Mediterranean Sea
1. Background
The phylum Cnidaria includes more than 9000 species, of which approximately 100 are known to cause injury to humans. All species possess microscopic cnidaria, which are highly specialized organelles consisting of an encapsulated hollow barbed thread bathed in venom [1] . They are commonly referred to as jelly fish. Rhopilema (R.) nomadica, the nomad jellyfish, is indigenous to the tropical warm waters of the Indian and Pacific Oceans [2] . Since the 1970s it has also been found in Mediterranean Sea, having entered via the Suez Canal. It has now been reported in the Eastern Mediterranean, off the coasts of Israel, Turkey and in the Aegean Sea off the coast of Greece [3] . The beaches of the Mediterranean Sea provide inviting summer leisure resorts for both citizens and tourists in Israel, however in more recent years this pleasure has come with the price of a massive seasonal invasion of this jellyfish [4] .
Envenomation is usually expressed as the immediate appearance of pain, redness and a burning sensation, with a subsequent papulo-vesicular eruption of the involved skin, although delayed skin reactions are also described [1] . Eruptions are due to immediate allergic, acute toxic and persistent inflammatory responses [5] and [6] . In Israel, envenomations are generally self-limited and do not require emergency care, however this year we have seen many children with systemic symptoms, and some have required hospitalization [1] . We report a patient with severe systemic symptoms due to an anaphylactic reaction which manifested after a jellyfish envenomation.
2. Case
A 15 year old female presented to the emergency department of the Dana-Dweck Children’s Hospital with anaphylaxis after being stung by a jellyfish while surfing at a Tel Aviv (Israel) beach. She had recently sustained recurrent jellyfish stings while engaging in this sport (more then five stings over three weeks). She had no history of atopic dermatitis or allergy in the past.
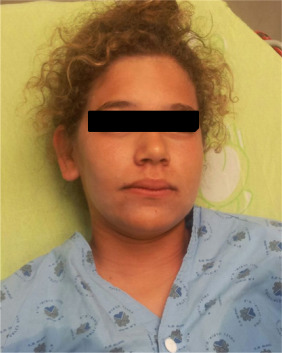
On this occasion, five minutes after being stung on the left arm, she experienced shortness of breath, an itching sensation and hoarseness. She was examined at the beach by a paramedic and was immediately transported to the emergency department receiving intramuscular adrenaline (0.01 mg/kg, 1:1000) on the way. On presentation she manifested mild dyspnea and stridor. Her pulse rate was 90 beats/min, blood pressure 134/79 mm Hg, respiratory rate 20/min and oxygen saturation 100% in room air. She had severe peri-orbital swelling and facial edema (Fig. 1 ), and a vesiculo-urticarial reaction on her left arm at the site of the sting. She received intravenous methylprednisolone (2 mg/kg) and intravenous diphenhydramine with resultant improvement after 15 min (Fig. 2 ). She was hospitalized and treated with ongoing systemic and topical steroids and antihistamines three times a day for two days, as well as magnesium dressings for the arm lesion, that consisted of marked erythema with papulovesicular eruptions. Laboratory results during hospitalization showed no signs of inflammation, normal C-reactive protein, blood count, serum electrolytes and renal function (performed to rule out presence of hemolysis and possible renal injury). She was discharged after two days with a recommendation to attend the allergic clinic at our institution in one month. This clinic recommended continuing treatment with oral antihistamines during the summer time, an Epipen prescription, and allergy prick testing using jellyfish materials. She was encouraged to return for re-testing the following summer after re-exposure to jellyfish envenomation.
|
|
|
Fig. 1. The patient at the presentation. |
|
|
|
Fig. 2. The same patients at discharge. |
3. Discussion
An immune-mediated response to venom may explain some sting related symptoms. Elevated serum anti-sea nettle immunoglobulin (Ig) M, IgG, and IgE may persist for year in patients with exaggerated reactions to stings compared with controls [7] and [8] . Compared with other jellyfish species, envenomation by R. nomadica is mostly mild [2] . Most patients with stings are treated beachside and never require hospitalization. The vast majority of patients with stings who do seek medical care experience severe pain without evidence of systemic poisoning, however severe systemic manifestation can develop [9] . Our patient, whose anaphylactic reaction was aborted by timely intervention, probably reacted on this occasion due to having received multiple stings in the recent past.
Jellyfish venoms are mixtures of toxic and antigenic polypeptides [10] . Human response to these compounds may include a local reaction or, more rarely, a systemic syndrome. An immune-mediated response to venom may explain some sting-related symptoms. Elevated serum anti-sea nettle immunoglobulin IgM, IgG, and IgE may persist for years in patients with exaggerated responses to stings, compared with controls [7] and [8] .
Cutaneous eruptions after envenomation may be local, generalized, exaggerated, recurrent, delayed, persistent, or occur at sites distant from the primary sting. Anaphylaxis is a potentially life-threatening manifestation of immediate hypersensitivity. The severity of these reactions varies from mild urticaria to shock and death. Anaphylaxis most commonly involves the pulmonary, circulatory, cutaneous, gastrointestinal, and central neurologic systems. The classic IgE-mediated reaction leading to anaphylaxis after exposure to a foreign substance occurs after prior exposure to a foreign antigen, either in its native state or as a hapten attached to a carrier protein. On re-exposure IgE binds to high-affinity receptors on mast cells and basophil and induces bridging of IgE molecules, degranulation of these cells, and release of various pre-formed and rapidly generated mediators.
Management of a life-threatening anaphylactic reaction requires simultaneous evaluation and management of the airway, breathing, and circulation, as well as the immediate administration of epinephrine. Corticosteroids are frequently recommended because of known efficacy in other allergic diseases. They can be administered as methylprednisolone 1–2 mg/kg IV (maximum 125 mg) or, for mild symptoms, prednisone 0.5–1 mg/kg by mouth (maximum 60–80 mg). H1 -receptor antihistamines such as diphenhydramine (1–1.25 mg/kg intramuscularly or intravenously; maximum 50 mg) are indicated in histamine-mediated allergic reactions.
To confirm allergy to jellyfish, allergic tests such as prick-to-prick testing and immunoblotting for antigens to IgE antibodies using jellyfish materials, can be performed [8] .
The patient we describe is the first reported to experience anaphylaxis following jellyfish envenomation in the Mediterranean. This is a rare complication and may be related to the multiple recent envenomations she had experienced during seaside activities.
Transparency document
Transparency Document.
References
- [1] S. Uri, G. Marina, G. Liubov; Severe delayed cutaneous reaction due to Mediterranean jellyfish (Rhopilema nomadica ) envenomation ; Contact Dermatitis, 52 (5) (2005), pp. 282–283
- [2] R. Silfen, A. Vilan, I. Wohl, A. Leviav; Mediterranean jellyfish (Rhopilema nomadica ) sting ; Burns, 29 (8) (2003), pp. 868–870
- [3] A. Lotan, L. Fishman, E. Zlotkin; Toxin compartmentation and delivery in the Cnidaria: the nematocysts tubule as a multiheaded poisonous arrow; J. Exp. Zool., 275 (6) (1996 15), pp. 444–451
- [4] S. Menahem, P. Shvartzman; Recurrent dermatitis from jellyfish envenomation; Can. Fam. Physician, 40 (1994), pp. 2116–2118
- [5] B. Yoffe, A.M. Baruchin; Mediterranean jellyfish (Rhopilema nomadica ) sting ; Burns, 30 (5) (2004), pp. 503–504
- [6] K.D. Winkel, P. Mirtschin, J. Pearn; Twentieth century toxinology and antivenom development in Australia; Toxicon, 48 (7) (2006), pp. 738–754
- [7] J.W. Burnett, G.J. Calton; Use of IgE antibody determinations in cutaneous Coelenterate envenomations; Cutis, 27 (1) (1981), pp. 50–52
- [8] K. Imamura, D. Tsuruta, A. Tsuchisaka, T. Mori, C. Ohata, M. Furumura, T. Hashimoto; Anaphylaxis caused by ingestion of jellyfish; Eur. J. Dermatol., 23 (3) (2013), pp. 392–395
- [9] J.W. Burnett, G.J. Calton, H.W. Burnett, R.M. Mandojana; Local and systemic reactions from jellyfish stings; Clin. Dermatol., 5 (3) (1987), pp. 14–28 (Review)
- [10] J.W. Burnett, G.J. Calton; Jellyfish envenomation syndromes updated; Ann. Emerg. Med., 16 (9) (1987), pp. 1000–1005
Document information
Published on 12/05/17
Accepted on 12/05/17
Submitted on 12/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?