Abstract
Aim
Etiology and pathophysiology of chronic internal disease was unknown until last days. This article challenges that two clinical trials have discovered the origin of chronic prostate diseases.
Methods
The hypothesis of the chronic internal diseases cause due to pathological activity of capillaries with emerging micro-focus of hypothermia, a continuous trigger for disease development in any affected organ, was declared in the US patent “Therapeutic Device and Method”, i.e. thermobalancing therapy (TT) and therapeutic device. Two clinical trials before and 6 months after TT for chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS) and benign prostatic hyperplasia (BPH) with the device, namely Dr. Allens therapeutic device (DATD) confirmed the effectiveness of TT. This device was used as mono-therapy for 124 patients with BPH and 45 men with CP/CPPS.
Results
Compared to controls, the TT groups showed significant improvements from baseline to endpoint. TT in men with BPH decreased urinary symptoms and PV, increased Qmax and improved quality of life index (QoL). At the same time, another clinical trial on TT in men with CP/CPPS has demonstrated decrease of pain score and PV mL, improvement of QoL and increase of Qmax mL/sec.
Conclusions
The long-term application of the source of emitted body heat with DATD, i.e. TT, to the projection of affected prostate removes “micro-focus” of hypothermia at the capillary level that improves blood circulation in the organ and its function. Thus this article shows that the underlying cause for different chronic internal diseases, such as BPH and CP/CPPS is the same and is positioned at the microvascular level. More studies with thermobalancing therapy needed.
Keywords
Origin of diseases ; Chronic prostatitis ; CP/CPPS ; Benign prostatic hyperplasia ; BPH ; Therapeutic device ; Thermobalancing therapy ; BPH cause ; CP/CPPS cause
Introduction
Chronic diseases are poorly defined problems, for instance investigations on chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS) have usually focused on peripheral-end-organ mechanisms, such as inflammatory or infective conditions, however, the potential etiologies and pathogenesis for CP/CPPS still remains unclear (Liao et al., 2016 ). Absence of knowledge of the pathogenesis of benign prostate hyperplasia (BPH) makes investigators look for its development in several mechanisms including increased intra-abdominal pressure, altered endocrine status, increased sympathetic nervous activity, increased inflammation process, and oxidative stress (Parikesit et al., 2016 ).
For many years has been suggested that in CP/CPPS pathogenesis has been proposed immunological, neurological, endocrine, or psychological basis (Cho and Min, 2015 ). In the last decade the cause of CP/CPPS has been also considered from the view of vascular dysfunction (Shoskes et al., 2011 ), chronic ischemia in the prostate tissue (Kogan et al., 2011 ), and increased pressure in the prostate gland (Mehik et al., 2003 ). The same situation was seen with the etiology of BPH, where the metabolic syndrome (MetS) (Demir et al., 2009 ), inflammation (Bostanci et al., 2013 ) and hormones (Bhasin et al., 2003 ) were discussed, and recent investigation found the vascular factor in pathogenesis of BPH (Saito et al., 2014 ).
It has been suggested that all chronic internal diseases, including BPH and CP/CPPS, originate at the capillary level. This conclusion is based on 2 functional physiological properties of capillaries that are activated by a trigger, thereby leading to violation of the microcirculation along with emergence of a focus on hypothermia, which in itself becomes a continuous trigger leading to chronic disease. Thus it was proposed that continuous application of a natural source of energy could treat the chronic disorder and thermobalancing therapy (TT) with therapeutic device (DATD) were created (Allen and Adjani, 2016 ).
The use TT with DATD for the treatment of LUTS and BPH led to a marked improvement and symptomatic relief (Allen and Aghajanyan, 2015 ). Furthermore, TT with DATD has shown to be effective for CP/CPPS (Allen and Aghajanyan, 2016a ). The symptoms' improvement in men with BPH and CP/CPPS after using TT can be explained by positive changes in the prostate gland. So, it can be suggested that pathological capillary activity plays the crucial role in the etiology and pathophysiology of these prostate diseases.
Methods
Ethical Approval of the Study Protocol
The Ethics Committee of Yerevan State Medical University approved the study protocol, and all participants provided written informed consent to be included in the study.
Study Design
Two clinical controlled studies undertaken in 2013–2015 that measured: International Prostate Symptom Score–Quality of Life (I-PSS) in 124 men with BPH and National Institute of Health Chronic Prostatitis Symptom Index (NIH-CPSI) in 45 men with CP/CPPS, and also prostate volume (PV mL), and maximum urinary flow rate (Qmax mL/sec). The parameters were compared between groups: treatment groups, which underwent TT, and control groups, which did not have such treatment.
Participants
Over a 2-year period, 45 men (age < 55 years) with CP/CPPS (NIH category III) and 124 men with BPH were selected for a clinical trial at the Department of Urology of Yerevan State Medical University. Patients were selected in conjunction with urologists.
Evaluation
Baseline evaluations were a full physical examination, medical history, digital rectal examination, serum biochemistry, measurement of prostate-specific antigen and electrolytes, urinalysis, and renal function tests. Evaluations were made at baseline and 6 months after treatment.
Endpoints
Primary endpoints were changes in urinary symptoms, pain and QoL score and secondary endpoints were changes in PV and Qmax after 6 months of treatment.
Statistical Analyses
The independent-samples t -test and paired-samples t -test are suitable only for interval and ratio data, so the Wilcoxon signed-rank test was employed. P < 0.05 was considered significant. Statistical analyses were carried out using SPSS v22 (IBM, Armonk, NY, USA).
DATD
Men who met the inclusion criteria of the study had TT using DATD. The latter was attached to the coccyx area of the patient. In April 2010, DATD was registered at the Medicines and Healthcare Products Regulatory Agency as a class-1 medical device. Thermobalancing alternative treatment with DATD provides a method of treating an affected prostate gland by application of a special mixture of waxes (thermoelement) topically upon its projection. This thermoelement can accumulate the emitted body heat, and thus turn into a source of energy itself. In this way, DATD applies the thermoelement tightly to the skin, thereby overcoming the skin barrier and spreading heat energy toward the prostate gland.
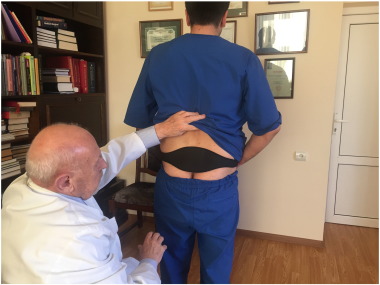
The thermoelement accumulates the body heat and acts as the heat source for the prostate. The neoprene belt keeps the thermoelement in close contact with the skin and prevents heat dissipation (Fig. 1 ).
|
|
|
Fig. 1. DATD tightly attaches thermoelement to the skin in the coccyx area. |
Results
Pain Score in 45 Men With CP/CPPS
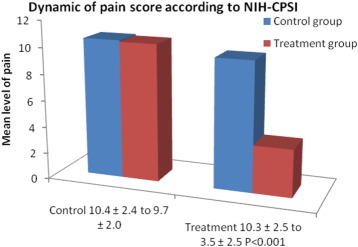
Fig. 2 shows the changes in pain score in CP/CPPS patients at the beginning and at the end of the study. In the control group, the mean pain score decreased slightly from 10.49 to 9.71 at the end of the study period, whereas in the treatment group the mean pain score decreased from 10.38 to 3.58 with a P value < 0.001.
|
|
|
Fig. 2. Pain score in 45 men with CP/CPPS according to the National Institute of Health-Chronic Prostatitis Symptom Index (NIH-CPSI) before and after thermobalancing therapy and in the control group. |
Prostate Volume in 45 Men With CP/CPPS
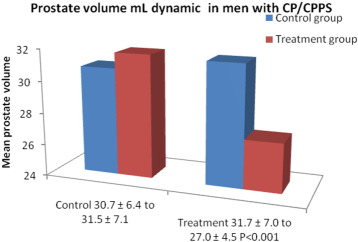
Fig. 3 shows the changes in PV in CP/CPPS patients at the beginning and end of the study. In the control group, the mean prostate volume increased from 30.77 ± 6.44 to 31.58 ± 7.14 mL at the end of the study period, whereas in the treatment group, the mean PV decreased from 31.75 ± 7.01 to 27.07 ± 4.52 mL with a P value < 0.001.
|
|
|
Fig. 3. Prostate volume in mL in 45 men with CP/CPPS before and after thermobalancing therapy and in the control group. |
Urinary Symptoms in 124 Men With BPH
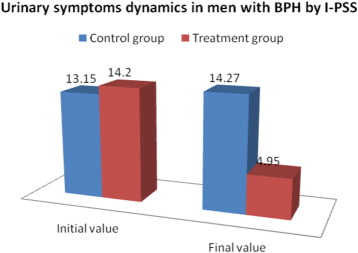
According to Fig. 4 in the control group, the mean urinary symptoms I-PSS score increased from 13.45 ± 3.254 to 14.35 ± 3.396 whereas, in the treatment group, it decreased from 14.33 ± 3.399 to 4.73 ± 2.754 at the end of the observation period, a significance level of P < 0.001.
|
|
|
Fig. 4. The dynamics of urinary symptoms in 124 men with BPH before and after thermobalancing therapy and in the control group by the International Prostate Symptom Score (I-PSS). |
Prostate Volume in 124 Men With BPH
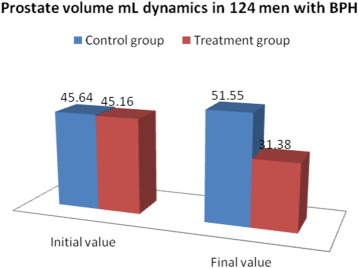
According to Fig. 5 in the control group, the mean PV increased from 45.54 mL to 50.85 mL whereas, in the treatment group, it decreased from 45.19 mL to 31.86 mL, at a significance level of P < 0.001.
|
|
|
Fig. 5. The changes in prostate volume mL in 124 men with BPH before and after thermobalancing therapy and in the control group. |
Discussion
These outcomes suggest that TT is effective for CP/CPPS and BPH. Hence, DATD decreased pain score in patient with CP/CPPS and urinary symptoms in patient with BPH significantly whereas, in the absence of treatment, the symptoms even worsened. Hence, DATD reduced PV significantly in men with CP/CPPS and BPH whereas, in the control groups, PV increased. We suggest that reduce in the prostate size is connected with improvement of blood circulation in the prostate gland. Thus the thermobalancing technique is effective by influencing the cause of both internal diseases. None of the patients who received TT had adverse effects. Furthermore, DATD is a one-time purchase, thus TT is overall cost effective.
Both studies were not randomized. Having a “placebo” or “sham” group as controls could have provided more statistical rigor with regard to outcomes. However, men with CP/CPPS have psychological problems, and pain syndrome associates with diminished QoL (Chung and Lin, 2013 ; Krsmanovic et al ., 2014 ). The similar problems are in men with BPH who suffer from depression and anxiety, their health-related QoL is considered poor (Martin et al ., 2015 ; Pinto et al ., 2016 ). 6-month may consider as a short period of time for taking tablets/placebo but too long for using something attached to the body. Therefore, proposing that men with CP/CPPS and BPH should wear a “placebo belt” for 6 months that does not alleviate symptoms would be very difficult. Usually, patients with CP/CPPS and BPH felt symptom relief within weeks of wearing DATD, so they used the device as required.
DATD applies natural thermoelement in close contact with the body in the projection of the prostate gland maintaining the accumulated temperature for a long period, spreading the energy toward the prostate gland and acting on “micro-focus” of hypothermia and ischemia elements, thereby relieving continuous pressure from the prostate tissue and resolving chronic pelvic pain (Aghajanyan and Allen, 2016 ), and reducing urinary symptoms in men with BPH (Allen and Aghajanyan, 2016b ).
To understand the etiology of chronic prostatitis lifestyle factors were investigated on a large number of men but no associations were observed between major lifestyle factors (obesity, smoking, and hypertension) and CP/CPPS (Zhang et al., 2015 ). Russo with colleagues declare that LUTS due to BPH may be considered as a complex disorder that can be discovered in the earlier stage. Therefore the counteraction of previous metabolic alterations should be the first aid for BPH. Thus the next challenges of urologists should be development of new target therapies for men who are at risk of LUTS due to BPH (Russo and Cimino, 2015 ). Presented clinical trials underline that TT is an effective independent treatment for CP/CPPS and BPH because treats the underlying cause of these chronic diseases (Allen and Aghajanyan, 2016c ).
Conclusions
The initiating cause for development of chronic diseases, including prostatitis and BPH, may differ and comprise from immunological, neurological, endocrine, inflammatory, metabolic or psychological factors but the trigger for the progress of chronic disease hides at the capillary level, i.e., constriction with an emergent focus of hypothermia in the tissue. As was shown by clinical trials, this phenomenon leads to spontaneous expansion of capillaries that increases pressure in the prostate gland provoking repeated constrictions. This “micro-focus” of hypothermia and, consequently, ischemia, sets up a vicious cycle of spontaneous growth of capillaries and continuous pressure in prostate-gland tissue that leads to CP/CPPS and BPH. By terminating “micro-focus” of hypothermia with DATD microcirculation within the prostate improves. Thus TT acts on the etiology of chronic disease in patients with the chronic prostate problems.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not for-profit sectors.
Conflict of Interest Statement
The author declares that there is no conflict of interest.
References
- Aghajanyan and Allen, 2016 I.G. Aghajanyan, S. Allen; Positive response to thermobalancing therapy enabled by therapeutic device in men with non-malignant prostate diseases: BPH and chronic prostatitis; Diseases, 4 (2016), p. 18
- Allen and Adjani, 2016 Allen S, Adjani A Therapeutic Device and Method, United States Patent and Trademark Office, 2016, Patent No: US 9,408,744 B2, https://www.google.com/patents/US9408744 .
- Allen and Aghajanyan, 2015 S. Allen, I.G. Aghajanyan; Benign prostatic hyperplasia treatment with new physiotherapeutic device; Urol. J., 12 (5) (2015), pp. 2371–2376 (Nov 14)
- Allen and Aghajanyan, 2016a S. Allen, I. Aghajanyan; Effect of thermobalancing therapy on chronic prostatitis and chronic pelvic pain syndrome; J. Clin. Urol., 20 (2016), pp. 1–8 http://dx.doi.org/10.1177/2051415816671036 (Sept)
- Allen and Aghajanyan, 2016b S. Allen, I.G. Aghajanyan; Thermobalancing conservative treatment for moderate-to-low-degree lower urinary tract symptoms (LUTS) secondary to prostate enlargement; Cogent Med., 3 (1) (2016), p. 1195067 http://dx.doi.org/10.1080/2331205X.2016.1195067
- Allen and Aghajanyan, 2016c S. Allen, I.G. Aghajanyan; Use of thermobalancing therapy in ageing male with benign prostatic hyperplasia with a focus on etiology and pathophysiology; Aging Male (2016), pp. 1–5 http://dx.doi.org/10.1080/13685538.2016.1247151
- Bhasin et al., 2003 S. Bhasin, A.B. Singh, R.P. Mac, et al.; Managing the risks of prostate disease during testosterone replacement therapy in older men: recommendations for a standardized monitoring plan; J. Androl., 24 (3) (2003), pp. 299–311
- Bostanci et al., 2013 Y. Bostanci, A. Kazzazi, S. Momtahen, J. Laze; Djavan B correlation between benign prostatic hyperplasia and inflammation; Curr. Opin. Urol., 23 (2013), pp. 5–10
- Cho and Min, 2015 I.C. Cho, S.K. Min; Proposed new pathophysiology of chronic prostatitis/chronic pelvic pain syndrome; Urogenit. Tract Infect., 10-2 (2015), pp. 92–101
- Chung and Lin, 2013 S.D. Chung, H.C. Lin; Association between chronic prostatitis/chronic pelvic pain syndrome and anxiety disorder: a population-based study; PLoS One, 8 (2013), p. e64630
- Demir et al., 2009 O. Demir, K. Akgul, Z. Akar, O. Cakmak, I. Ozdemir, A. Bolukbasi, E. Can, B.H. Gumus; Association between severity of lower urinary tract symptoms, erectile dysfunction and metabolic syndrome; Aging Male, 12 (1) (2009), pp. 29–34 http://dx.doi.org/10.1080/13685530902777425 (Mar)
- Kogan et al., 2011 M.I. Kogan, I.I. Belousov, A.S. Bolotskov; Arterial blood flow in the prostate in the syndrome of chronic pelvic pain/chronic prostatitis; Urologiia, 3 (2011), pp. 22–28
- Krsmanovic et al., 2014 A. Krsmanovic, D.A. Tripp, J.C. Nickel, et al.; Psychosocial mechanisms of the pain and quality of life relationship for chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS); Can. Urol. Assoc. J., 8 (2014), pp. 403–408
- Liao et al., 2016 C.-H. Liao, H.-C. Lin, C.-Y. Huang; Chronic prostatitis/chronic pelvic pain syndrome is associated with irritable bowel syndrome: a population-based study; Sci. Rep., 6 (2016), p. 26939 26939 http://dx.doi.org/10.1038/srep 26939
- Martin et al., 2015 S. Martin, A. Vincent, A.W. Taylor, et al.; Lower urinary tract symptoms, depression, anxiety and systemic inflammatory factors in men: a population-based cohort study; PLoS One, 10 (10) (2015), p. e0137903 (Oct 7)
- Mehik et al., 2003 A. Mehik, M.J. Leskinen, P. Hellström; Mechanisms of pain in chronic pelvic pain syndrome: influence of prostatic inflammation; World J. Urol., 21-2 (2003), pp. 90–94
- Parikesit et al., 2016 D. Parikesit, C.A. Mochtar, R. Umbas, A.R. Hamid; The impact of obesity towards prostate diseases; Prostate Int., 4 (1) (2016), pp. 1–6 http://dx.doi.org/10.1016/j.prnil.2015.08.001 (Mar)
- Pinto et al., 2016 J.D. Pinto, H.G. He, S. Chan, W. Wang; Health-related quality of life and psychological well-being in men with benign prostatic hyperplasia: an integrative review; Jpn. J. Nurs. Sci. (2016) http://dx.doi.org/10.1111/jjns.12115
- Russo et al., 2015 G.I. Russo, S. Cimino, G. Morgia; Benign prostatic hyperplasia and metabolic syndrome: the expanding evidences of a new disease of aging male; Aging Male, 18 (3) (2015), pp. 133–134 http://dx.doi.org/10.3109/13685538.2015.1028353
- Saito et al., 2014 M. Saito, P. Tsounapi, R. Oikawa, et al.; Prostatic ischemia induces ventral prostatic hyperplasia in the SHR; possible mechanism of development of BPH; Sci. Rep. (2014) http://dx.doi.org/10.1038/srep03822
- Shoskes et al., 2011 D.A. Shoskes, D. Prots, J. Karns, J. Horhn, A.S. Shoskes; Greater endothelial dysfunction and arterial stiffness in men with vhronic prostatitis/chronic pelvic pain syndrome — a possible link to cardiovascular disease; J. Urol., 186 (2011), p. 907
- Zhang et al., 2015 R. Zhang, S. Sutcliffe, E. Giovannucci, et al.; Lifestyle and risk of chronic prostatitis/chronic pelvic pain syndrome in a cohort of United States male health professionals; J. Urol., 194-5 (2015), pp. 1295–1300
Document information
Published on 27/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?