Abstract
Aim
To explore the role of the Australian breast care nurse in the provision of information and support to women with breast cancer, with a focus on the differences experienced depending on geographic work context.
Design
A cross-sectional study.
Methods
This study conducted in 2013, involved surveying BCNs currently working in Australia, using a newly developed self-report online survey.
Results
Fifty breast care nurses completed the survey, 40% from major cities, 42% from inner regional Australia and 18% from outer regional, remote and very remote Australia. Patterns of service indicated higher caseloads in urban areas, with fewer kilometres served. Breast care nurses in outer regional, remote and very remote areas were less likely to work in multi-disciplinary teams and more likely to spend longer consulting with patients. Breast care nurses reported they undertook roles matching the competency standards related to the provision of education, information and support; however, there were barriers to fulfilling competencies including knowledge based limitations, time constraints and servicing large geographical areas.
Conclusions
This was the first Australian study to describe the role of the breast care nurse nationally and the first study to investigate breast care nurses perceived ability to meet a selection of the Australian Specialist Breast Nurse Competency Standards. Important differences were found according to the geographical location of breast care nurses.
Introduction
Breast cancer is the second most common cancer in the world and the most frequent cancer among women worldwide (Ferlay et al. 2013). Consistent with worldwide prevalence, breast cancer is the most common cancer amongst Australian women with incidence continuing to increase (Australian Institute of Health and Welfare (AIHW) 2012). Best practice for care of Australians with breast cancer involves health professionals working collaboratively in multidisciplinary teams aiming to meet the multiple health needs of patients (National Breast Cancer Centre and National Cancer Control Initiative 2003, National Breast Cancer Centre 2005a,b). As a member of the multidisciplinary team, the specialist breast care nurse (BCN) was introduced in Australia in the mid-1990s to facilitate better continuity of care and psychosocial support (Jones et al. 2010) for people undergoing treatment for breast cancer. Specialist breast care nursing has evolved over the past twenty years not only in Australia, but in Canada, Europe, the UK and the US (Eicher et al. 2012).
In the Australian context, the BCN role involves assisting people with breast cancer across all stages of the continuum of care, including diagnosis, treatment, rehabilitation and palliative care by providing clinical care, information, education, psychological and emotional support, and taking an active role in the co-ordination of care (National Breast Cancer Centre 2005b). Further, the BCN model of practice is defined as a specialist practice, therefore requiring a higher level of knowledge and skill in the care of women with breast cancer (National Breast Cancer Centre 2005b). Usual requirements include experience in oncology nursing and the recommended minimum education such as a Bachelor of Nursing and a Post Graduate Diploma of Breast Care Nursing (Yates et al. 2007). The scope of specialist breast nursing practice is defined as occurring in the context of a model of care that enables the nurse to work collaboratively with patients contributing to patient-centred care, while also working collaboratively within the multi-disciplinary team (National Breast Cancer Centre 2005b).
The consensus view is that BCNs are valued highly by their patients (Eicher et al. 2006, Halkett et al. 2006, Jones et al. 2010, Reed et al. 2010). However, despite advances in healthcare initiatives including the introduction of BCNs, women with breast cancer still have high unmet support needs. Several studies have found that many women do not have adequate information about their disease and treatment, nor receive enough practical and emotional support from health professionals (McGrath et al. 1999, Girgis et al. 2000, Raupach & Hiller 2002, Davis et al. 2004, Vivar & McQueen 2005, Aranda et al. 2006, Lawler et al. 2011). Historically, addressing these needs for rural or remote Australian women has proven more difficult because cancer service capabilities in Australia are restricted by many factors including challenges in attracting and retaining a sufficiently skilled workforce and servicing large geographical areas (National Breast Cancer Centre 2001, Health Workforce Australia 2013). For example, in Australia, the large geographical mass means that a women living in the rural town of Richmond, Queensland, would need to travel 500 km to reach the closest regional hospital offering cancer treatment services. Further, to have their treatment in the closest metropolitan city, they would need to travel 1584 km to Brisbane, Queensland.
Background
In Australia, BCNs are either employed by the McGrath Foundation or by public or private healthcare providers. In 2013, at the time of this study, there were no existing statistics on BCNs working in Australia; however, it was estimated that there were around 400, with 84 of these being employed by the McGrath Foundation (McGrath Foundation 2013, Paynter 2013).
Like many nurses who work in advanced practice roles or specialized practice areas, Australian BCNs practice in a variety settings (Yates et al. 2007), with a range of expectations for the role, leading to lack of role clarity (Eicher et al. 2006, Lowe et al. 2011). Previous research shows there is some doubt about whether all Australian women with breast cancer have adequate access to a BCN (Campbell et al. 2006, Eley & Rogers-Clark 2012). Furthermore, there has been debate about the smaller caseload of BCNs in rural and remote areas, suggesting the role of the BCN in these settings is unsustainable (National Breast Cancer Centre and National Cancer Control Initiative 2003).
The research literature about Australian BCNs consists of predominantly exploratory, single site studies conducted primarily in metropolitan areas (Ahern & Gardner 2015) indicating a need for further research to investigate differing BCN roles in varying geographical and practice contexts. This study was designed in response to this finding and, therefore, explores the role of the Australian BCN in providing information and support to women diagnosed with breast cancer, with a particular focus on reporting the differences experienced in varying geographic work contexts. The research questions addressed are:
- What role differences occur between rural/remote and urban BCNs in Australia?
- How does the self-report role of an Australian BCN compare with Australian Specialist Breast Care Nurse Competency Standards relating to the provision of education, information and support?
The study
An online survey, known as the Breast Care Nurse Survey was developed for this study and issued using a cross-sectional design. Ethical approval was granted by the Australian Catholic University Human Research Ethics Committee (approval number 2013 196N). Participants were BCNs currently working in Australia recruited using snowball sampling. Of the 60 participants who began the survey, 50 completed it, giving a completion rate of 83%. Consent was indicated by submission of a completed survey and this was explained in the participant information.
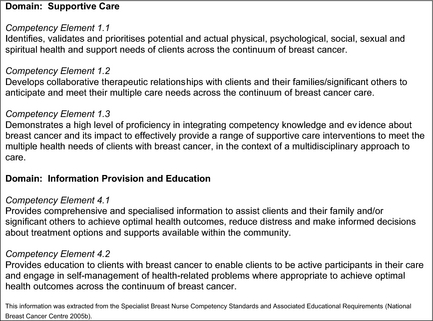
A literature search revealed no suitable pre-existing survey instrument. Therefore, a new survey instrument was developed, consisting of 59 structured items and allowance for 26 open-ended responses, divided into three sections. Section 1 (13 items) collected demographic information about participants. Section 2 (20 items) collected primarily interval and ratio data about caseloads, consults and multi-disciplinary team involvement. Section 3 (26 structured items with Likert scales and allowance for additional free text) was based on the Specialist Breast Nurse Competency Standards. In this section, the performance criteria for Specialist Breast Nurse Competency Standards 1·1, 1·2, 1·3, 4·1 and 4·2 (see Figure 1) were used as a framework for generating items to explore the breadth of the BCN role in the provision of education, information and support, and the perceived barriers to undertaking each of the performance criteria. Details of development, face validity and reliability of the survey are being prepared for publication separately.
|
|
|
Figure 1. Specialist breast nurse competency standards used to guide Section Three of the Breast Care Nurse Survey. |
All data were stored electronically in password protected files. Detailed address data were collected to identify the geographic location of each participant; however, names of participants were not collected. Collection of Internet Protocol (IP) address of each participant was a default process of the online survey software. However, steps were taken to ensure that confidentiality and privacy were maintained by first deleting all IP addresses from the database and identifying each record by a unique number. Second, an Australian Bureau of Statistics (ABS) Remoteness Area (RA) code was manually allocated to the physical residential/workplace address of each participant to identify their geographical location (Australian Bureau of Statistics, 2013a). These RA codes were consistent with the latest available information from the ABS and were allocated using an address coding tool on the ABS website (Australian Bureau of Statistics, 2013b). Once the RA code was allocated, all other information relating to place of residence was deleted from the database to protect the identity of participants.
Structured items collected both nominal and ordinal data and were analysed using descriptive statistics with SPSS Statistics software, version 20·0 (IBM Corp 2011). Categories where cell numbers were small were combined. For example, number of years working as a BCN was collapsed from five categories down to three. Thematic analysis was applied to open-ended questions, where responses were used to add richness to the quantitative data.
Results
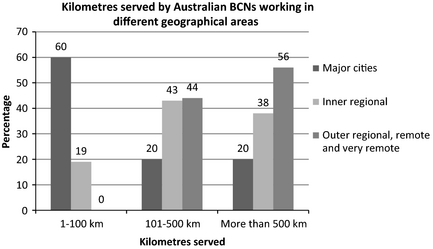
Fifty BCNs completed the survey. Respondents working in major Australian cities comprised 40% (n = 20) of the total sample. Forty-two per cent (n = 21) worked in inner regional Australia, with the remaining 18% (n = 9) working in outer regional, remote or very remote Australia. Respondents worked in a variety of healthcare settings. Figure 2 shows kilometres served by BCNs working in different geographic areas.
|
|
|
Figure 2. Kilometres served by Australian BCNs working in different geographical areas. |
Breast care nurse education, experience and qualifications
The majority of respondents had worked fewer than 6 years as a BCN (64%, n = 32) and this pattern was consistent regardless of geographic location (Table 1). Forty per cent of respondents were employed full time. Most BCNs employed in major cities worked between 3 and 5 days per week (80%, n = 16) in contrast to less than half of those employed in outer regional, remote or very remote areas. Overall, BCNs in outer regional, remote and very remote areas also reported being less highly qualified.
| Characteristic | Total n = 50 | Major Cities n = 20 | Inner Regional n = 21 | Outer regional, remote or very remote n = 9 | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | |
| Years working as BCN | ||||||||
| 0-5 years | 32 | 64 | 13 | 65 | 12 | 57 | 7 | 78 |
| 6-10 years | 11 | 22 | 2 | 10 | 7 | 33 | 2 | 22 |
| More than 10 years | 7 | 14 | 5 | 25 | 2 | 10 | 0 | 0 |
| Employment basis | ||||||||
| Full time | 20 | 40 | 8 | 40 | 9 | 43 | 3 | 33 |
| Part time | 30 | 60 | 12 | 60 | 12 | 57 | 6 | 67 |
| Percentage of work week as BCN | ||||||||
| 0·5-2·5 days per week | 16 | 32 | 4 | 20 | 7 | 33 | 5 | 56 |
| 3-5 days per week | 34 | 68 | 16 | 80 | 14 | 67 | 4 | 44 |
| Highest Qualification | ||||||||
| Hospital Trained, Bachelor of Nursing | 5 | 10 | 2 | 10 | 0 | 0 | 3 | 33 |
| Graduate Certificate, Graduate Diploma, Master of Nursing, PhD | 45 | 90 | 18 | 90 | 21 | 100 | 6 | 67 |
| Hold BCN Qualificationa | ||||||||
| Yes | 42 | 84 | 17 | 85 | 18 | 86 | 7 | 78 |
| No | 8 | 16 | 3 | 15 | 3 | 14 | 2 | 22 |
|
a Not all of these qualifications are tertiary level. | ||||||||
Current patient and consult characteristics
Higher caseloads and higher percentages of patients newly diagnosed with breast cancer were seen in major cities and inner regional areas (Table 2). Results indicate that BCNs in outer regional, remote and very remote areas were more likely to continue to follow patients from diagnosis through to and after completion of adjuvant treatment, than BCNs in major cities. Ninety percent of all BCNs reported seeing patients within one week of diagnosis, with 64% reporting consulting patients at least weekly within the first month of diagnosis. No BCNs reported spending less than 20 minutes each consult with breast cancer patients and BCNs in outer regional, remote and very remote areas were more likely to spend an hour or more consulting with patients.
| Characteristic | Total n = 50 | Major cities n = 20 | Inner regional n = 21 | Outer regional, remote and very remote n = 9 | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | |
| Case load | ||||||||
| 0-50 patients | 26 | 52 | 11 | 55 | 8 | 38 | 7 | 78 |
| 51-100 patients | 12 | 24 | 3 | 15 | 8 | 38 | 1 | 11 |
| More than 100 patients | 12 | 24 | 6 | 30 | 5 | 24 | 1 | 11 |
| Newly diagnosed breast cancer patients per month | ||||||||
| 1-10 patients | 35 | 70 | 10 | 50 | 16 | 76 | 9 | 100 |
| 11-20 patients | 11 | 22 | 6 | 30 | 5 | 24 | 0 | 0 |
| More than 20 patients | 4 | 8 | 4 | 20 | 0 | 0 | 0 | 0 |
| When patients are seen | ||||||||
| At diagnosis | 44 | 88 | 18 | 90 | 18 | 86 | 8 | 89 |
| Pre-operatively | 45 | 90 | 16 | 80 | 20 | 95 | 9 | 100 |
| Post-operatively | 46 | 92 | 17 | 85 | 20 | 95 | 9 | 100 |
| During adjuvant chemotherapy/radiotherapy | 43 | 86 | 15 | 75 | 19 | 90 | 9 | 100 |
| After completion of adjuvant treatment | 43 | 86 | 14 | 70 | 20 | 95 | 9 | 100 |
| How soon consults occur after diagnosis | ||||||||
| At diagnosis | 14 | 28 | 9 | 45 | 3 | 14 | 2 | 22 |
| Within one or two days | 14 | 28 | 3 | 15 | 9 | 43 | 2 | 22 |
| Within one week | 17 | 34 | 6 | 30 | 6 | 29 | 5 | 56 |
| More than a week | 5 | 10 | 2 | 10 | 3 | 14 | 0 | 0 |
| Regularity of consults within the first month of diagnosis | ||||||||
| Never | 2 | 4 | 2 | 10 | 0 | 0 | 0 | 0 |
| Daily | 2 | 4 | 1 | 5 | 1 | 5 | 0 | 0 |
| At least once per week | 32 | 64 | 11 | 55 | 14 | 67 | 7 | 78 |
| Once a fortnight | 2 | 4 | 1 | 5 | 1 | 5 | 0 | 0 |
| Once per month | 1 | 2 | 0 | 0 | 1 | 5 | 0 | 0 |
| As needed | 17 | 34 | 8 | 40 | 5 | 24 | 4 | 44 |
| Time allocated to a consult | ||||||||
| Up to 20 minutes | 0 | 0 | 0 | 0 | 0 | 0 | 0 | 0 |
| 21-30 minutes | 21 | 42 | 13 | 65 | 7 | 33 | 1 | 11 |
| Up to 1 hour | 25 | 50 | 6 | 30 | 12 | 57 | 7 | 78 |
| More than one hour | 4 | 8 | 1 | 5 | 2 | 10 | 1 | 11 |
Consult methods and multi-disciplinary team involvement
Regardless of geographic location, BCNs mostly used face-to-face and telephone consultations, only spending 10% of their working week using electronic consultations. Those working in geographically distant areas report less likelihood of involvement in multidisciplinary teams (MDTs). Overall, the majority of BCNs reported spending up to 30% of their working week in MDT meetings and most of these reported feeling encouraged to share their views in MDT meetings (Table 3).
| Characteristic Measured | Total n = 50 | Major cities n = 20 | Inner regional n = 21 | Outer regional, remote and very remote n = 9 | ||||
|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | |
| Face-to-face consults (n = 50) | ||||||||
| Up to 50% | 31 | 62 | 7 | 35 | 16 | 76 | 8 | 89 |
| More than 50% | 19 | 38 | 13 | 65 | 5 | 24 | 1 | 11 |
| Telephone consults (n = 50) | ||||||||
| Up to 50% | 33 | 66 | 17 | 85 | 12 | 57 | 4 | 33 |
| More than 50% | 17 | 34 | 3 | 15 | 9 | 43 | 5 | 56 |
| Electronic communication consults (n = 50) | ||||||||
| Up to 10% | 47 | 94 | 19 | 95 | 21 | 100 | 7 | 77 |
| More than 10% | 3 | 6 | 1 | 5 | 0 | 0 | 2 | 22 |
| Do you work in a MDT? (n = 50) | ||||||||
| Yes | 44 | 88 | 19 | 95 | 19 | 91 | 6 | 67 |
| No | 6 | 12 | 1 | 5 | 1 | 9 | 3 | 33 |
| If yes | ||||||||
| What percentage of your week is spent in MDTMs? (n = 44) | ||||||||
| Up to 30% | 32 | 73 | 11 | 58 | 17 | 89 | 4 | 67 |
| 31-60% | 9 | 20 | 6 | 32 | 1 | 5 | 2 | 33 |
| More than 60% | 3 | 7 | 2 | 11 | 1 | 5 | 0 | 0 |
| Are you encouraged to share your view in MDTs about patient care? (n = 43) | ||||||||
| Yes, always | 23 | 53 | 11 | 58 | 10 | 56 | 2 | 33 |
| Yes, but only if I have been working with the patient | 10 | 23 | 5 | 26 | 3 | 17 | 2 | 33 |
| No, but I feel free to share my view | 10 | 23 | 3 | 16 | 5 | 28 | 2 | 33 |
Respondents reported regularly undertaking the performance criteria embedded in competency standards 1·1, 1·2, 1·3, 4·1 and 4·2 (National Breast Cancer Centre 2005b). Analysis of relationships using cross tabulation between responses and years' experience revealed those with more than 5 years' experience were more likely to reporting to ‘always’ undertake performance criteria in 22 out of the 26 criteria listed. Relationships between responses and level of education revealed those with post-graduate education were more likely to report ‘always’ undertaking performance criteria in 19 out of the 26 criteria listed. Notably, much lower percentages of BCNs perceived an ability to ‘always’ undertake performance criteria 1·1c, than was reported in any of the other performance criteria listed and these percentages were equivalent regardless of levels of experience and education.
Free text information revealed the most common barriers to undertaking performance criteria were large patient loads, limited time constraints and knowledge base limitations. In the supportive care domain, BCNs working in rural or remote centres reported limited resources and limited access to other healthcare workers and identified geographical distances to main treatment centres as barriers to fulfilling competencies. The existence of ethnic and cultural barriers was also acknowledged, especially by those working in remote and very remote settings.
In the domain of information provision and education, a number of BCNs reported lack of private spaces to address matters needing discretion. Some reported they lacked experience, knowledge, skills and confidence dealing with sensitive matters, but many explained they were increasing their skill and knowledge base through education. Those in geographically isolated areas reported that although ongoing education was available, access was difficult due to factors such as distance, cost and time away from work. Free text responses also revealed the difficulties experienced accessing the MDT due to geographical distance. Additionally, some BCNs reported MDT meetings were held infrequently, leading to barriers in provision of timely advice.
Discussion
Current evidence about the role of the Australian BCN providing information in support to women with breast cancer is lacking (Ahern & Gardner 2015). This study provides insights into the role of the Australian breast care nurse particularly in the context of different geographical locations.
A comparison of BCNs based on geographical location
As the majority of respondents had less than 6 years' experience in their position, assessing the educational needs of this group and providing additional educational support may be required. Access to additional education through continued professional development (CPD) is an important factor regardless of geographical location and ensures that nursing practice is evidence-based, maintains best-practice standards and meets the current needs of communities (Black & Farmer 2013).
Although the ratios of full-time to part-time BCNs were consistent across the three geographical areas, there were major differences in total working hours. Perhaps, like many other rural nursing roles, BCNs working in outer regional, remote and very remote areas may be predominantly part-time in this role and combine the BCN role with other nursing roles, increasing role diversity (Francis & Mills 2011).
The higher caseloads experienced by those working in major cities and inner regional areas may contribute to reduced regularity and duration of consult time. These results support findings of Jones et al. (2010) who noted BCNs in metropolitan areas had a wider range of responsibilities, higher caseloads with the potential for more limited care being provided to patients.
Findings related to length of consultations and regularity with which BCNs see their patients throughout the cancer trajectory suggest that women in outer regional, remote and very remote areas may have higher levels of access to their BCNs and therefore more time and opportunity to receive information and support from their BCN. This reinforces the findings from a previous study that found a statistically significantly higher percentage of women in outer regional, remote and very remote areas reported using the BCN for support than women in major cities and inner regional areas (Ahern et al. 2014). An increase in the number of BCNs available to meet the needs of women in major cities and inner regional areas would decrease caseloads, enabling BCNs in these areas to increase regularity and duration of consultations, potentially improving the levels of BCN support experienced by these women.
Limited use of electronic consultations were surprising considering that Internet-based telemedicine is readily available and regularly used by many health professionals (Fatehi et al. 2014). Increased uptake of the telemedicine model would provide advantages for BCNs and patients alike saving BCN travel time, while allowing patients the convenience of consulting from the privacy of their own home (Sabesan & Piliouras 2009).
BCN perceived ability to undertake competencies consistent with their role
Perceptions of BCNs with more experience and/or higher qualifications associated with higher levels of ability to undertake competencies related to the provision of information and support reinforce once again the benefit of continued professional development, training or education relevant to BCN roles. Importantly, BCN perceptions highlighted a specific area of need to enable them to more confidently meet performance criteria 1·1c. This performance criterion indicates that BCNs are required to routinely assess all clients for psychosocial risk factors and distress at the time of diagnosis and on a regular basis using a systematic evidence-based approach (National Breast Cancer Centre 2005b). Therefore, BCNs may need further education and access to appropriate evidence-based screening tools to assist them to become more confident and competent in addressing psychosocial and psychological needs of patients.
Online courses are one way of delivering CPD to rural and remote nurses through organizations such as CRANAplus and EdCaN (Australian Government 2010, CRANAplus Incorporated 2014). Each offer web-based learning resources useful to rural nurses and within cancer control, but more specific resources for BCNs could be developed. However, through an open forum discussion at a national cancer nurses conference, the point was made that often BCNs fail to take up online education that is offered (Ahern 2014), although the reason behind the lack of uptake are unknown.
Reported barriers to undertaking the selected competencies included a lack of culturally appropriate resources available to meet the multiple care needs of women with breast cancer. While there are now resources available through the Breast Cancer Network Australia and Cancer Australia, at the time this study was conducted these resources may not have been readily available (Cancer Australia 2012, Breast Cancer Network Australia 2013).
Policy and research implications
Continued professional development (CPD), training and support are recommended for all BCNs (Yates et al. 2007). It is well documented that continued professional development and education of nurses in the rural setting is difficult due to limited resources (Fahey & Monoghan 2005, McCoy 2009, Health Workforce Australia 2013); however, these are critical elements supporting the role and professional practice of BCNs (Francis & Mills 2011, Black & Farmer 2013). Therefore, individual BCNs should commit to CPD offered and employers need to support and fund nurses to undertake CPD through post-graduate study and clinical learning opportunities (Black & Farmer 2013). Ongoing assessment of gaps in the education and training provided to BCNs is recommended for educating bodies, and additionally, the reasons for failure to take up online CPD is an area worthy of further investigation.
The lack of access to and participation for BCNs in outer regional, remote and very remote areas to multi-disciplinary teams compared with their peers in major cities and inner regional areas is consistent with a recent study evaluating the McGrath BCN service which found 47% of rural BCNs participated in MDT meetings (Paynter et al. 2013). Multidisciplinary care benefits both clinicians and patients and it is well recognized that cancer care is most effectively delivered by MDTs (Catt et al. 2005, National Breast Cancer Centre 2005a, Health Workforce Australia 2013). The BCN is positioned between cancer specialists and patients enabling the nurse to advocate for patients and assist in their medical management (Amir et al. 2004), thus the importance of BCN involvement in MDT meetings conducted by the cancer treatment team. Diverse geographical locations make it difficult for face-to-face MDT meetings. However, Internet and videoconferencing software can be used not only for outpatient consultations, but also case discussions between health professionals (Doolittle & Spaulding 2006, Sabesan et al. 2012). Therefore, it is recommended that clinicians seek opportunities to use videoconferencing technologies enabling inclusion of BCNs from all geographical areas in regular MDT meetings. Current availability of and use of videoconferencing technologies by MDTs is an area in need of more research.
Strengths and limitations
Importantly, this is the first study to describe the Australian BCN role nationally and to investigate BCNs' perceived ability to meet the Specialist Breast Nurse Competency Standards relating to the provision of education, information and support (National Breast Cancer Centre 2005b). Limitations include using a newly developed self-report survey tool and a small convenience sample. Further validation of the instrument would be beneficial before it is used in other contexts.
Conclusion
This study reports the differences in characteristics and practice of BCNs working in urban areas and those working in regional, rural and remote areas. Findings suggest BCNs in outer regional, remote and very remote areas require improved support through better access to continued professional development and training, and better inclusion in MDT meetings. Innovative use of web-based resources such as online training and videoconferencing should be investigated and used to achieve improved access to CPD and MDTs for BCNs working in outer regional, remote and very remote areas. For BCNs working in major cities and inner regional areas, an increase in numbers of employed BCNs may decrease caseloads and increase patient contact time. All recommendations have the capacity to improve the professional practice of Australian BCNs and outcomes for women with breast cancer.
Acknowledgements
University supervisors are Prof Anne Gardner and Prof Mary Courtney.
Conflict of interest
There are no conflicts of interest declared.
Author contributions
All authors have agreed on the final version and meet at least one of the following criteria [recommended by the ICMJE (http://www.icmje.org/recommendations/)]:
- substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data;
- drafting the article or revising it critically for important intellectual content.
References
- Ahern T. (2014) The role of the Australian breast care nurse: A self-report online survey. 17th CNSA Winter Congress, 25 July 2014 Cancer Nurses Society Australia, Melbourne, Vic, Australia.
- Ahern T. & Gardner A. (2015) Literature review: an exploration of the role of the Australian breast care nurse in the provision of information and supportive care. Collegian22, 99–108.
- Ahern T., Gardner A. & Courtney M. (2014) Geographical comparisons of information and support needs of Australian women following the primary treatment of breast cancer: a 10 year replication study. Health Expectations [Online]. Available at http://onlinelibrary.wiley.com.ezproxy2.acu.edu.au/doi/10.1111/hex.12242/abstract. (accessed 10 October 2014).
- Amir Z., Scully J. & Borrill C. (2004) The professional role of breast cancer nurses in multi-disciplinary breast cancer care teams. European Journal of Oncology Nursing8, 306–314.
- Aranda S., Schofield P., Weih L., Milne D., Yates P. & Faulkner R. (2006) Meeting the support and information needs of women with advanced breast cancer: a randomised controlled trial. British Journal of Cancer95, 667–673.
- Australian Bureau of Statistics (2013a) Australian Statistical Geography Standard (ASGS) [Online]. Australian Bureau of Statistics. Available at http://www.abs.gov.au/websitedbs/D3310114.nsf/home/Australian+Statistical+Geography+Standard+(ASGS) (accessed 1 July 2013).
- Australian Bureau of Statistics (2013b) Census Home [Online]. Available at http://www.abs.gov.au/websitedbs/censushome.nsf/home/map (accessed 5 May 2013).
- Australian Government (2010) EdCaN: The Australian National Cancer Nursing Education Project [Online]. Retrieved from http://www.edcan.org/ on 16 June 2014.
- Australian Institute of Health and Welfare (AIHW) (2012) Cancer incidence projections, Australia 2011 to 2020. Cancer series no. 66. Cat. no. CAN 62. AIHW, Canberra.
- Black E. & Farmer F. (2013) A review of strategies to support the professional practice of specialist cancer nurses. The Australian Journal of Cancer Nursing14, 22–28.
- Breast Cancer Network Australia (2013) Cultural and Linguistic Diversity at BCNA [Online]. Retrieved from http://www.bcna.org.au/news/2013-09/cultural-and-linguistic-diversity-bcna on 13 June 2014.
- Campbell D., Khan A., Rankin N., Williams P. & Redman S. (2006) Are specialist breast nurses available to Australian women with breast cancer. Cancer Nursing29, 43–48.
- Cancer Australia (2012) My Breast Cancer Journey: A Guide for Aboriginal and Torres Strait Islander women and their families. Cancer Australia, Surry Hills, NSW.
- Catt S., Fallowfield L., Jenkins V., Langridge C. & Cox A. (2005) The informational roles and psychological health of members in 10 oncology multidisciplinary teams in the UK. British Journal of Cancer93, 1092–1097.
- CRANAplus Incorporated (2014) CRANAplus: improving remote health. [Online]. Retrieved from https://crana.org.au/ on 16 June 2014.
- Davis C., Williams P., Parle M., Redman S., Turner J., Davis C., Williams P., Parle M., Redman S. & Turner J. (2004) Assessing the support needs of women with early breast cancer in Australia. Cancer Nursing27, 169–174.
- Doolittle G.C. & Spaulding A. (2006) Providing access to oncology care for rural patients via telemedicine. Journal of Clinical Oncology Practice2, 228–230.
- Eicher M., Marquard S. & Aebi S. (2006) A nurse is a nurse? A systematic review of the effectiveness of specialised nursing in breast cancer. European Journal of Cancer42, 3117–3126.
- Eicher M., Kadmon I., Claassen S., Marquard S., Pennery E., Wengstrom Y. & Fenlon D. (2012) Training breast care nurses throughout Europe: the EONS postbasic curriculum for breast cancer nursing. European Journal of Cancer48, 1257–1262.
- Eley R. & Rogers-Clark C. (2012) Consumer perceptions of the effectiveness of a breast care nurse in providing coordinated care to women with breast cancer in Queensland, Australia. Australian Journal of Advanced Nursing29, 56–61.
- Fahey C.M. & Monoghan J.S. (2005) Australian rural midwives: perspectives on continuing professional development. Rural and Remote Health5, 468. Available at http://www.rrh.org.au/publishedarticles/article_print_468.pdf. (accessed 10 September 2014).
- Fatehi F., Martin-Khan M., Gray L.C. & Russell A.W. (2014) Design of a randomized, non-inferiority trial to evaluate the reliability of videoconferencing for remote consultation of diabetes. Medical Informatics and Decision Making [Online]. Retrieved from http://www.biomedcentral.com/1472-6947/14/11 on 14 November 2014.
- Ferlay J., Soerjomataram I., Ervik M., Dikshit R., Esser S., Mathers C., Rebelo M., Parkin D.M., Forman D. & Bray F. (2013) GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 11 [Online]. International Agency for Research on Cancer, Lyon, France. Retrieved from http://globocan.iarc.fr on 02 April 2014.
- Francis K.L. & Mills J.E. (2011) Sustaining and growing the rural nursing and midwifery workforce: understanding the issues and isolating directions for the future. Collegian18, 55–60.
- Girgis A., Boynes A., Sanson-Fisher R.W. & Burrows S. (2000) Perceived needs of women diagnosed with breast cancer: rural versus urban location. Australian & New Zealand Journal of Public Health24, 166–173.
- Halkett G., Arbon P., Scutter S. & Borg M. (2006) The role of the breast care nurse during treatment for early breast cancer: the patients perspective. Contemporary Nurse23, 46–57.
- Health Workforce Australia (2013) National Cancer Workforce Strategic Framework. Health Workforce Australia, Adelaide, SA.
- IBM CORP (2011) IBM SPSS Statistics for Windows, 20.0 ed. IBM Corp, Armonk, NY.
- Jones L., Leach L., Chambers S. & Occhipinti S. (2010) Scope of practice of the breast care nurse: a comparison of health professional perspectives. European Journal of Oncology Nursing14, 322–327.
- Lawler S., Spathonis K., Masters J., Adams J. & Eakin E. (2011) Follow-up care after breast cancer treatment: experiences and perceptions of service provision and provider interactions in rural Australian women. Supportive Care in Cancer19, 1975–1982.
- Lowe G., Plummer V., O'Brien A.P. & Boyd L. (2011) Time to clarify – the value of advanced practice nursing roles in heatlh care. Journal of Advanced Nursing68, 677–685.
- McCoy C. (2009) Professional development in rural nursing: challenges and opportunities. The Journal of Continuing Education in Nursing40, 128–131.
- McGrath Foundation (2013) McGrath Breast Care Nurses. [Online]. Retrieved from http://www.mcgrathfoundation.com.au/our-nurses on 12 April 2013.
- McGrath P., Patterson C., Yates P., Treloar S., Oldenburg B. & Loos C. (1999) A study of postdiagnosis breast cancer concerns for women living in rural and remote Queensland. Part II: support issues. Australian Journal of Rural Health7, 43–52.
- National Breast Cancer Centre (2001) Clincial practice guidelines for the management of early breast cancer. Available at http://www.nhmrc.gov.au/_files_nhmrc/publications/attachments/cp74.pdf. (accessed 10 May 2013).
- National Breast Cancer Centre (2005a) Multidisciplinary Meetings for Cancer Care: A Guide for Health Service Providers. NBCC, Camperdown, NSW.
- National Breast Cancer Centre (2005b) Specialist Breast Nurse Competency Standards and Associated Educational Requirements. Retrieved from http://canceraustralia.gov.au/sites/default/files/publications/bnc-1-specialist-breast-nurse-competency-standards-associated-educational-requirments_507f8fbd520de.pdf on 01 May 2013.
- National Breast Cancer Centre and National Cancer Control Initiative (2003) Clinical practice guidelines for the psychosocial care of adults with cancer. Retrieved from http://www.nhmrc.gov.au/_files_nhmrc/file/publications/synopses/cp90.pdf on 10 May 2013.
- Paynter H. (2013) RE: Australian Breast Care Nurse Population. Type to AHERN, T.
- Paynter H., Fodero L., Scuteri J., Kerin-Ayres K. & Tink K. (2013) Evaluation of the McGrath Foundations breast cancer nurses initiative. The Australian Journal of Cancer Nursing14, 4–9.
- Raupach J.C.A. & Hiller J.E. (2002) Information and support for women following the primary treatment of breast cancer. Health Expectations5, 289–301.
- Reed E., Scanlon K. & Fenlon D. (2010) A survey of provision of breast care nursing for patients with metastatic breast cancer – implications for the role. European Journal of Oncology Nursing19, 575–580.
- Sabesan S. & Piliouras P. (2009) Disparity in cancer survival between urban and rural patients – how can clinicians help reduce it?Remote and Rural Health9, 1146. Available at http://www.rrh.org.au/publishedarticles/article_print_1146.pdf. (accessed 25 July 2014).
- Sabesan S., Larkins S., Evans R., Varma S., Andrews A., Beuttner P., Brennan S. & Young M. (2012) Telemedicine for rural cancer care in North Queensland: bringing cancer care home. The Australian Journal of Rural Health20, 259–264.
- Vivar C.G. & McQueen A. (2005) Informational and emotional needs of long-term survivors of breast cancer. Journal of Advanced Nursing51, 520–528.
- Yates P., Evans A., Moore A., Heartfield M., Gibson T. & Luxford K. (2007) Competency standards and educational requirements for specialist breast nurses in Australia. Collegian14, 11–15.
Document information
Published on 09/06/17
Submitted on 09/06/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?