Abstract
Discoveries from basic science research in the last decade have brought significant progress in knowledge of pathophysiologic processes of allergic diseases, with a compelling impact on understanding of the natural history, risk prediction, treatment selection or mechanism-specific prevention strategies. The view of the pathophysiology of allergic diseases developed from a mechanistic approach, with a focus on symptoms and organ function, to the recognition of a complex network of immunological pathways. Several subtypes of inflammation and complex immune-regulatory networks and the reasons for their failure are now described, that open the way for the development of new diagnostic tools and innovative targeted-treatments. An endotype is a subtype of a disease condition, which is defined by a distinct pathophysiological mechanism, whereas a disease phenotype defines any observable characteristic of a disease without any implication of a mechanism. Another key word linked to disease endotyping is biomarker that is measured and evaluated to examine any biological or pathogenic processes, including response to a therapeutic intervention. These three keywords will be discussed more and more in the future with the upcoming efforts to revolutionize patient care in the direction of precision medicine and precision health. The understanding of disease endotypes based on pathophysiological principles and their validation across clinically meaningful outcomes in asthma, allergic rhinitis, chronic rhinosinusitis, atopic dermatitis and food allergy will be crucial for the success of precision medicine as a new approach to patient management.
Keywords
Allergic diseases; Asthma; Biomarkers; Endotypes; Precision medicine
Abbreviations
AD, atopic dermatitis; AHR, airway hyperreactivity; AR, allergic rhinitis; BAL, bronchoalveolar lavage; Bcl-2, B-cell lymphoma 2 protein; BNA, Bayesian Network Analysis; CCL, CC chemokine ligand; CGBN, Conditional Gaussian Bayesian Network; CD, cluster of differentiation; CLP, chitinase-like proteins; COPD, chronic obstructive lung disease; CpG, 5′—Cytosine—phosphate—Guanine—3′; CRS, chronic rhinosinusitis; CRTH2, chemokine receptor homologous molecule expressed on Th2 lymphocytes; CXCL, CXC chemokine ligand; CXCR2, CXC chemokine receptor 2; eNO, exhaled nitric oxide; FA, food allergy; FDA, Food and Drug Administration; Gal, galectin; GATA, gamma-amino-n-butyrate transaminase; G-CSF, granulocyte colony-stimulating factor; GM-CSF, granulocyte-macrophage colony-stimulating factor; ICAM, intercellular adhesion molecule; Ig, immunoglobulin; IL, interleukin; ILC, innate lymphoid cell; IFN, interferon; LCA, latent class analysis; LIGHT, tumor necrosis factor superfamily member 14; MAIT, mucosal associated invariant T cell; MARS, multivariate regression splines; MAP-kinase, mitogen-activated protein kinases; MMP, matrix metalloproteinase; MUC, mucin; NF, nerve fibers; NGF, nerve growth factor; NK, natural killer; NNCS, non-neuronal cholinergic system; NP, nasal polyps; ORA, over-representation analyses; PGE2, prostaglandin E2; PGP, proline-glycine-proline; PPIN, protein–protein interaction network; RAR, retinoic acid receptor; ROC, receiver operating characteristic curves; RUNX, Runt-related transcription factor X; S1P, sphingosine 1-phosphate; SCORAD, scoring atopic dermatitis; SNP, single-nucleotide polymorphism; SR, steroid resistant; SS, steroid sensitive; TDA, topological data analysis; TGF, transforming growth factor; Th, T helper; TNF, tumor necrosis factor; Treg, T regulatory cell; TSLP, thymic stromal lymphopoietin; VCAM, vascular endothelial cellular adhesion molecule; YKL-40, chitinase-3-like protein 1
The concept of endotypes, phenotypes, biomarkers and precision medicine
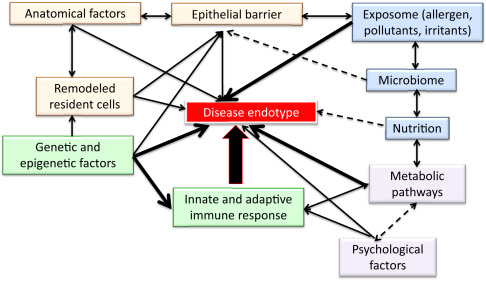
The three key words endotype, phenotype and biomarker will be one of the main topics of research on the way of building blocks of precision medicine and precision health.1, 2 and 3 The word “endotype” uncovers molecular mechanisms underlying observable disease characteristics known as “phenotype”.4 and 5 Assigning unique mechanisms and biomarkers for each endotype is crucial for the validity of the endotype.5 and 6 So far only few (if any) valid endotypes have been identified in allergic disease, all with therapeutic implications. To further elaborate on the definition of an endotype one must recognize that one major pathogenic pathway such as type 2 immune response is highly complex, including several determinants with nonlinear dynamic interactions (Fig. 1) and heterogeneous, since not all determinants are present in all patients or, in a given patient, at all time points.6 and 7 We therefore must embrace the concept of a “complex endotype” consisting of several subendotypes as opposed to an endotype that encompasses a single molecular mechanism. 7
|
|
|
Fig. 1. Factors that affect a disease endotype in allergic diseases. For precision medicine in allergic disease, more mechanistic approaches are needed, based on an integrated understanding of the individual patients biological mechanisms, including the interplay between the immune response and the exposome, infections and microbiome, genetics, epigenetics, psychosocial factors, nutrition, anatomical factors and metabolic pathways. |
Epigenetics and endotypes of allergy and asthma
Epigenetic programming during early life influences is crucial for the development of the endotypes of allergic diseases. Increased knowledge on developmental endotypes addressing disease inception and progression are needed for the outset of early prevention and disease modifying strategies. Crucial determining factors for complex immune regulation and barrier function include respiratory infections, microbiome, and nutrition. Epigenetic mechanisms link gene regulation to environmental influences and developmental trajectories.8 Developmental programming induced by the intrauterine environment (cigarette smoke, nutrition, and stress) affects the fetus and its germ line, with intergenerational epigenetic effects. Developmental programming can be transmitted across generations (trans-generational effects) and cannot be anymore attributed to direct environmental exposure.
Several time-dependent DNA methylation signatures associated with allergic disease developmental endotypes are described. The Tucson Infant Immune Study identified in cord blood mononuclear cells 589 differentially methylated regions associated with childhood asthma. These regions mapped to genes that cluster in immunoregulatory and pro-inflammatory pathways.9 Examination of the methylome of children with or without food sensitization at birth and 12 months revealed a novel 92-CpG signature in CD4 T cells, enriched in genes encoding MAP kinase signaling molecules, distinguishing children who developed clinical food allergy by age 12 months. This signature was stable from birth until 12 months of age, suggesting that the children bearing that signature were on an epigenetic path to disease already at birth.10 DNA methylation could mechanistically explain the effect of season of birth on allergy. In a subset of participants from the Isle of Wight birth cohort autumn birth increased risk of eczema, relative to spring birth. Methylation status of 92 CpGs showed association with season of birth. Results were validated in the Prevention and Incidence of Asthma and Mite Allergy (PIAMA) cohort and showed significantly more CpGs with the same directionality than expected by chance, and four were statistically significant. Season-associated methylation was enriched among networks relating to development, the cell cycle, and apoptosis. Twenty CpGs were nominally associated with allergic outcomes. Season-associated methylation was absent in newborns, suggesting it appears postnatal.11 DNA methylation marks involved in T-cell maturation (RUNX3), type 2 immune response (IL4), and oxidative stress (catalase) were associated with allergic asthma in the inner city study.12 In monozygotic twin pairs with discordance for asthma symptoms methylomic markers in peripheral blood differentiate remitting and persisting asthma.13 Peripheral blood readily detectable DNA methylomic biomarkers outperformed allergen-specific IgE and skin prick tests for predicting food challenge outcomes.14
Biomarkers, precision medicine and endotypes
Biomarkers, or biological markers, are measurable indicators used to examine any aspects of health or disease. Any type of analyses can be a biomarker and may provide information about the pathophysiology of an underlying disease, the course of an illness, and/or the response to treatment. They are expected to inform us if a disease is present or absent, define its severity, provide information about its progression, serve to select most effective treatment, and/or serve as guidance about the affected individuals survival. Biomarkers are used at present to predict treatment response and very few to forecast disease risk and progression. It should be noted that most biomarkers are currently suited only for research settings and still need to be validated and qualified.15, 16 and 17 Steps towards biomarker qualification are clearly delineated by regulators lead by the FDA.18 At present, biomarkers are not sufficiently specific to select the endotype specifically responding to a targeted treatment. For example, blood eosinophils predict response to anti-IL-4/IL-13, anti-IL-5, and anti-IgE antibodies, as well as CRTH2 antagonists and the clinician will face a challenge of how best to treat severe asthma patients with high blood eosinophils.3 and 17
Precision medicine represents a novel approach, embracing four key features: personalized care based on molecular, immunologic and functional endotyping of the disease, with participation of the patient in the decision making process of therapeutic actions, and considering predictive and preventive aspects of the treatment.1, 2, 3, 19 and 20 Asthma, allergic rhinitis (AR), chronic rhinosinusitis (CRS), food allergy (FA) and atopic dermatitis (AD) are ideally suited for precision medicine, because they represent an umbrella of different diseases that partially share biological mechanisms (endotypes) and present similar visible properties (phenotypes) that require an individualized approach for a better selection of treatment responders, risk prediction and design of disease-modifying strategies.3, 16 and 20 The precision in the clinic needs four main components: an improved disease taxonomy is a current unmet need because none of the disease endotypes in allergic diseases are included in the existing taxonomies; full patient monitoring using novel digital technology and the concept of endotypes and novel biomarkers is a must; improved understanding and common usage of disease phenotypes, endotypes and biomarkers preferentially at the point of care; and finally biomarker and endotype-linked patient care and usage of precision therapies.1
Longitudinal follow-up of clinical and molecular profiles is essential to confirm the validity of an endotype.21 Participants in the Childhood Asthma Management Program (CAMP) study were evaluated 9 and 14 years after they ended the trial. Differences in clinical characteristics observed between subjects assigned to different phenotypic clusters persisted into young adulthood and were associated with differences in molecular signatures for atopy and asthma control.22
New bioinformatics tools to define endotypes
Several new approaches are used nowadays to define an endotype, including more accessible tools for human immunophenotyping, specific targeted immune therapies and the application of omics and new statistical tools. Gene expression profiling of airway samples introduced the definition of the type-2 asthma endotype.23 Novel biomarkers of Th2 inflammation are being identified in easily accessible non-invasive samples such as serum, exhaled air, nasal brushing, urine and sputum.24, 25 and 26 Transcriptomic endotypes of asthma based on common patterns of gene expression in the sputum and blood were recently described in a cohort of children with asthma and were associated with near-fatal, severe, and milder asthma.27
There is a shift from investigator-imposed subjective disease clustering (hypothesis driven) to data-driven disease endotyping (hypothesis generating). New statistical tools such as supervised analysis, Latent Class Analysis (LCA), Bayesian Network Analysis (BNA), Topological Data Analysis (TDA) and several types of Network Analysis become available. From these tools, supervised analysis with receiver operating characteristic (ROC) curves and regression trees can find the best predictor from a set of continuous variables,28 LCA is used to reduce the dimensionality of the data sets and to group variables into patterns,29 BNA helps to explore associations between parameters,30 while TDA can identify multidimensional endotypes.31 In a recent study ROC curves identified IL-13 and IL-5 as best predictors for blood eosinophilia, followed by EDN and exhaled NO. In the regression tree model, blood eosinophilia was best predicted by IL-5. The next important variables were EDN and eNO.21 The application of LCA integrating sputum supernatant eicosanoids with quantitative assessment of sputum cells revealed four distinct asthma classes differing in eicosanoid pathways.32 In severe asthma, TDA identified six novel clinic-patho-biological clusters of underlying disease mechanisms, with elevated mast cell mediators tryptase, chymase, and carboxypeptidase A3.33 BNA separated clinical features from intricately connected inflammatory pathways highlighting the expression of YKL-40 in patients with neutrophilic inflammation and the expression of MMPs in patients with severe asthma.34 Apparently, generalized usage of these tools will help to better understand the complex pathophysiology and complex endotypes.
Data-driven models are another type of unbiased approach for characterization of endotypes. Multivariate regression splines (MARS) is a robust nonparametric modeling approach that outperforms other approaches including linear regression modeling, classification trees.35 Non-parametric MARS modeling approach yields highly accurate classifiers of inflammatory endotypes in asthma, exceeding all other machine-learning approaches tested.36 Clinical biomarkers and blood gene expression collected from a stratified, cross-sectional study of asthmatic and non-asthmatic children enrolled into The Mechanistic Indicators of Childhood Asthma (MICA) study were used to construct a data-driven model. The model proved the interplay between innate and adaptive immune responses, with a dominant role for adaptive immunity in one group, innate immunity two other groups and a mixed contribution in the forth group. Metabolic syndrome-induced systemic inflammation was an associated factor in three of the four asthma endotypes. This study suggested underlying mechanisms linking obesity and asthma through systemic inflammation and common genetic background. The context provided by the clinical biomarker data was essential in interpreting gene expression patterns and identifying putative endotypes, which emphasizes the importance of integrated approaches when studying complex diseases.37 In an adult asthma study metabolomic data, genome-wide genotype, gene expression, and methylation data were used to construct a Conditional Gaussian Bayesian Network (CGBN). Integrative and metabolic pathway over-representation analyses (ORA) identified enrichment of known biological pathways within the strongest molecular determinants. The CGBN model based on four SNPs and two metabolites could predict asthma control with an AUC of 95%. Integrative ORA identified 17 significantly enriched pathways related to cellular immune response, interferon signaling, and cytokine-related signaling. Arachidonic acid, prostaglandin E2 (PGE2) and sphingosine 1-phosphate (S1P), in addition to six genes appeared to drive the pathway results.38 Protein–protein interaction network (PPIN) provides a new framework to detect genes for different stages of asthma. By investigating the proteins in stage-specific interactions, the study demonstrated that they are more likely related to asthma, and the functional enrichment analysis indicated that the pathways enriched in the differential interactions are related to the progress of asthma.39
Creation, harmonization and merging of large datasets will enable the validation of endotypes on a population level. Ideally, these large datasets would integrate existing clinical and “omics” data (e.g., genomic, proteomic, lipidomic, and microbiomic). The use of harmonized terminology for patient characteristics and outcomes, of standardized protocols and open access to repositories for biospecimen collection are of critical importance.
Type 2 immune response driven complex endotype
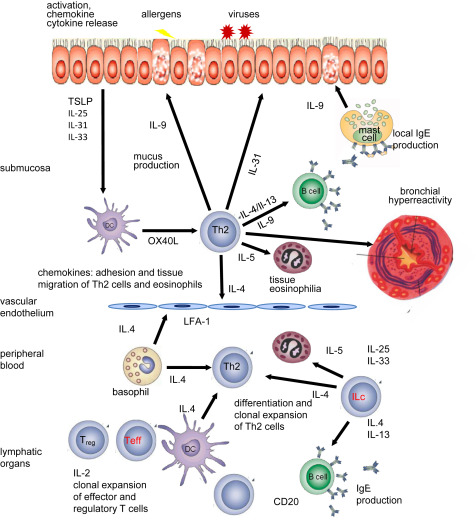
Generally, it is considered that a type 2 immune response underlines atopic asthma and allergic rhinitis, as a fundament for the united airways disease concept.3 and 40 Type 2 immune response involves Th2 cells, type 2 B cells, group 2 innate lymphoid cells (ILC), a small fraction of IL-4 secreting NK cells, IL-4 secreting NK-T cells, basophils, eosinophils and mast cells and their major cytokines. From a complex network of cytokines, IL-4, IL-5, IL-9 and IL-13 are mainly secreted from the immune system cells and IL-25, IL-31, IL-33 and TSLP from tissue cells, particularly epithelial cells41 (Fig. 2). Both the innate and the acquired immune response contribute to type 2 immune response endotypes. Th1/Th17 inflammatory cells and non-allergic mechanisms such as environmental factors, psycho-social stress, activation of metabolic pathways, resident cells in the remodeled phenotype or epithelial barrier dysfunction further modulate the profile of type 2-driven inflammation.42, 43, 44, 45 and 46 In addition, type 2-driven inflammation is characterized by a high cellular plasticity that enables the cells to adapt to a specific inflammatory milieu. Several sub-endotypes might exist within the type 2 immune response complex endotype such as the IL-5-high, IL-13-high or IgE-high endotype7 and their preponderance differs between allergic diseases (Fig. 3).7
|
|
|
Fig. 2. The complex network of type 2 immune response. Activation of the epithelial cells and release of IL-25, IL-31, IL-33 and TSLP contribute to type 2 responses of T cells and innate lymphoid cells. These cytokines play a role in the production of allergen-specific IgE, eosinophilia, permissiveness of endothelium for the recruitment of inflammatory cells to inflamed tissues, production of mucus and decreased threshold of contraction of smooth muscles. |
|
|
|
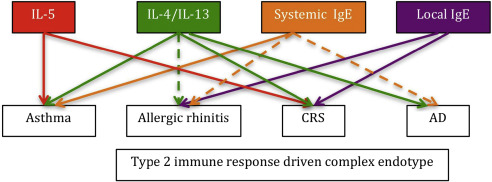
Fig. 3. The complex type 2 immune response driven endotype consists of several individual pathways with different preponderance in major allergic diseases. The IL-5 pathway is a therapeutic target in asthma validated in major phase III clinical trials leading to regulatory approval of mepolizumab for severe asthma and was targeted in a proof of concept study in CRS with NP. The IL-4/IL-13 pathway seems similarly important for asthma, CRS with NP and AD: targeted intervention with dupilumab significantly reduced symptom burden. Targeting systemic IgE is a well validated intervention in allergic asthma and new anti-IgE monoclonal antibodies are under clinical development. Anti-IgE treatment seemed less rewarding in AD. Local IgE production is a key pathogenic event driving the inflammation process both in AR and CRS. Up to now no targeted interventions were tested for AR as a primary disease phenotype. Continuous line: type 2 immune response endotypes with a beneficial response to targeted treatment and/or strong evidence for involvement in disease pathogenesis. Dashed line: evidence relating to disease pathogenesis. CRS, chronic rhinosinusitis; AD, atopic dermatitis. |
In asthma, the type 2 immune response endotype has been related to response to inhaled corticosteroids3 and 47 and to disease outcomes, such as exacerbations.48 and 49 For asthma many targeted treatments are in various stages of clinical development for patients with type 2 immune response-driven inflammation: anti-IL-4/IL-13,50 and 51 anti-IL-4,52 anti-IL-5,53, 54 and 55 and anti-IgE antibodies,56 and 57 as well as CRTH2 antagonists58, 59 and 60 and an endotype driven approach guided by biomarkers such as blood or sputum eosinophilia or serum periostin seems to predict treatment response.
In chronic rhinosinusitis (CRS) with nasal polyposis (NP) there is good evidence for a type 2 immune response driven endotype.61 The eosinophilic pathway driven by IL-5 is prominent, together with local IgE production and innate immune response activation, such as ILC type 2 cells. Tissue eosinophilia and evidence of eosinophil activation are closely associated with remodeling features of CRS, associated mucosal damage and clinical symptoms.62 A recent study evaluating the inflammatory endotypes of CRS using partition-based clustering showed several IL-5-positive clusters: a group with moderate IL-5 concentrations, a mixed CRS with and without nasal polyposis (NP) and increased asthma phenotype, and a group with high IL-5 levels, an almost exclusive NP phenotype with strongly increased asthma prevalence. In the IL-5 high group, two clusters demonstrated the highest concentrations of IgE and asthma prevalence, with all samples expressing Staphylococcus aureus enterotoxin-specific IgE. 63 Both anti IL-5 and anti IgE targeted interventions showed clinical efficacy in CRS with NP. 64 and 65 The IL-4/IL-13 pathway seems similar important for CRS with NP: targeted intervention with dupilumab on top of nasal steroids for 16 weeks significantly reduced the NP burden.66
Type 2 immune response in AD covers the whole disease spectrum from background inflammation in non-lesional skin to acute disease flares and to chronic disease, peaking during acute flares.67, 68 and 69 IL-4/IL-13 seems to be key drivers since targeted treatment with dupilumab improved significantly the clinical responses and the AD gene signature in a dose-dependent manner.70, 71 and 72 Anti IgE treatment seemed less rewarding in AD, although a subgroup of responders can be identified by the absence of filaggrin mutations and altered lipid metabolite profiles with high levels of various glycerophospholipids.73
Non-type 2 immune response driven complex endotype
Non-eosinophilic asthma is a well-documented asthma phenotype. Studies in large cohorts, such as the SARP (Severe Asthma Research Program) cohort, identified neutrophilic inflammation through induced sputum as an important hallmark of a distinct cluster of patients with moderate to severe asthma.74 More recent studies evaluating the molecular signature of the Th2 genes23 or using unsupervised hierarchical clustering of gene expression profiles in asthma75 reinforce the reality of non-eosinophilic asthma. In CRS with NP unsupervised cluster analysis showed a distinct cluster characterized by neutrophilic inflammation76 and Th1/Th17 polarization was described for NP sampled from Asian patients.77 Age-related decline in neutrophil inflammation was related to better postoperative results in elderly patients with non-eosinophilic NP.78 Th22- and Th1-driven inflammation is prominent in patients with the chronic form of AD.67, 68 and 69
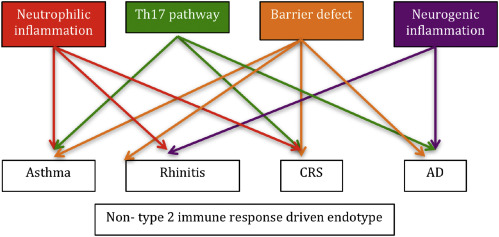
Several data sets support the relevance of multiple non-type 2-driven molecular sub-endotypes in allergic diseases related to neutrophilic inflammation, Th17 pathway activation, tissue remodeling and barrier defects, neurogenic inflammation with chemosensory dysfunction (Fig. 4).
|
|
|
Fig. 4. Multiple non-type 2-driven molecular sub-endotypes in major allergic diseases. Growing evidence supports a role for a dysregulated innate immune response promoting neutrophilic inflammation in asthma, rhinitis and CRS. The IL-17 pathway has been related to disease severity in asthma, CRS and AD. Tissue remodeling and barrier defects are major players modulating the non type-2 immune response in asthma and CRS, while barrier defect is central for all disease phenotypes. The neurogenic inflammation pathway appears of particular importance in rhinitis and AD. |
Neutrophilic inflammation
Two major mechanisms leading to non type 2 inflammation have been postulated: the dysregulated innate immune response, including neutrophil intrinsic abnormalities and the activation of the IL-17-dependent pathway.79 In addition, type 1 immune response, metabolic or epigenetic factors, or the activation of the epithelial-mesenchymal trophic unit that may lead to extensive remodeling without any inflammation have been identified as modulators. The endotyping of the non-type 2 allergic diseases lags well behind type 2 immune response, and until now, no endotype-driven interventions have been proven to be effective.
Growing evidence supports a role for a dysregulated innate immune response in neutrophilic asthma, with altered gene expression of Toll like receptors and increased expression of genes from the IL-1β and TNF-α/nuclear factor-κB pathways,80 phenotype switch and enhanced neutrophil chemotaxis and survival in the airways, impairment in anti-inflammatory mechanisms and in pathogen recognition and destruction processes and increased protease activity. The signature of non-eosinophilic asthma includes three genes involved in innate immune response: IL-1β, alkaline phosphatase tissue-nonspecific isozyme and CXCR2.81
In an experimental model of Th1/neutrophil-predominant asthma, TNFα reduced the responsiveness to steroids and neutralization of TNFα using etanercept restored glucocorticoid sensitivity.82 Recently, the TNF superfamily member, LIGHT, has been implicated as a mediator in asthmatic airway inflammation. Human bronchial epithelial cells express the receptor for LIGHT, the lymphotoxin β receptor (LTβR) and upon stimulation with LIGHT release IL-6, oncostatin M, MCP-1, growth-regulated protein α and IL-8.83
In non-eosinophilic asthma blood neutrophils release significantly higher levels of IL-8 at rest. Microarrays demonstrated expression profiles that were significantly distinct from eosinophilic asthma: 317 genes were significantly altered in resting neutrophils, including genes related to cell motility and regulation of apoptosis.84 Persistent elevation of airway neutrophils due to impaired efferocytosis was also described. Galectin-3 (gal-3) is significantly reduced in neutrophilic asthma compared with eosinophilic and paucigranulocytic asthma. In addition, patients with neutrophilic asthma have impairment in anti-inflammatory ratio of gal-3/gal-3 binding protein and IL-1RA/IL-1β.85
Altered pathogen recognition and destruction processes are present with macrophage efferocytosis impaired in non-eosinophilic asthma to a similar degree as in COPD.86 A low number of neutrophils or the presence of a type of neutrophils with compromised antimicrobial activity was related to the formation of biofilms in CRS.87
The increased activity of neutrophil elastase is in direct correlation with the levels of interleukin-8 and neutrophils.88 In a subset of chronic obstructive lung disease (COPD) patients the tripeptide matrikine proline-glycine-proline (PGP) seems to play a role. Azithromycin and roflumilast have been shown to reduce acute exacerbations of COPD and recent evidence has linked both of these agents to modulation of the PGP/neutrophil pathway in concert with this exacerbation reduction, thus supporting the PGP/neutrophil pathway as a new target for the neutrophilic airway inflammation.89
IL-17 and neutrophilic endotype
Through the induction of cytokines and chemokines IL-17 is a major driving force for the recruitment of neutrophil granulocytes in the lungs and their activation directly through CXCL8 production or indirectly by inducing the production of IL-6, G-CSF and GM-CSF, IL-8, CXCL1, and CXCL5 by airway epithelial cells. Although Th17 cells represent a core source of IL-17, a newly identified population of innate lymphoid cells (ILCs) is also able to produce IL-17.90 and 91 IL-17 – producing ILC3s express CC chemokine receptor 6, produce IL-17 and sometimes IL-22, and are central to the development of asthma in obese mice. Increased numbers of this subset of cells have been found in the bronchoalveolar lavage (BAL) fluid of obese individuals with severe asthma.92
A likely role of IL-17 in neutrophilic asthma is suggested by the significant association between IL-17 and other diseases with underlying neutrophilic inflammation, such as psoriasis, and by the efficiency of IL-17-targeted therapies in these diseases.93 The link between neutrophilic inflammation and Th17 immunity is well established in mouse models of asthma, where it has been linked to the development of airway hyperreactivity (AHR) and remodeling.94 and 95 Human data are accumulating, however a cause and effect relationship between IL-17 production and neutrophilic asthma has not been demonstrated and targeted intervention with brodalumab (an anti IL-17 receptor monoclonal antibody) did not show a significant treatment effect.96 A strong correlation between IL-17 and neutrophils was established in induced sputum and blood.97 and 98 IL-17 has been linked to remodeling, AHR, asthma severity and inflammation.99, 100 and 101 In the Clinical Asthma Research Association cohort study, patients with non-allergic asthma showed very distinctly IL-17-shifted proinflammatory immunity, promoting neutrophil inflammation and less functional Treg cells. In parallel, expressions of anti-inflammatory IL-37, proline-serine-threonine phosphatase-interacting protein 2, the neutrophil-associated genes CD93, triggering receptor expressed on myeloid cells 1, and regulator of G-protein signaling 13 were increased.102 In a recent study however Th17 cells and γδ17 cells were not associated with asthma, even in the severe neutrophilic forms. Instead, mucosal associated invariant T (MAIT)-cell frequencies were strikingly reduced in asthma compared with health, both in sputum and in bronchial biopsies, especially in severe asthma where BAL regulatory T cells were also reduced.34
Th17 cells are resistant to glucocorticoid-induced apoptosis and cytokine suppression, at least in part due to high levels of BCL-2.103 These findings support a role of Th17 cells in steroid-resistant (SR) endotypes of asthma, chronic rhinosinusitis or atopic dermatitis. The IL-17 pathway was related to decreased corticosteroid sensitivity, also a characteristic of neutrophilic asthma.104 Patients with SR asthma produced significantly increased IL-17A and IFN-γ levels compared to steroid sensitive (SS) asthma. Production of IL-17A was inversely and production of IL-13 was positively associated with the clinical response to prednisolone. Oral calcitriol significantly improved dexamethasone-induced IL-10 production in vitro while suppressing dexamethasone-induced IL-17A production. This effect mirrored the previously demonstrated improvement in clinical response to oral glucocorticoids in calcitriol-treated patients with SR asthma. These data identify immunologic pathways that likely underpin the beneficial clinical effects of calcitriol in patients with SR asthma and suggest strategies for identifying vitamin D responders in asthma.105
Inflammatory cell expression of IL-9 and IL-17C is increased in CRS, especially in association with NP, asthma and atopy.106 Th17 cytokines (IL-17, IL-22, and IL-26) have been shown to induce a significant disruption of the epithelial barrier, in contrast to the application of interferons and of Th1 or Th2 cytokines who did not affect the mucosal barrier function.107 IL-17 receptor B levels are increased in immune cells of patients with NPs compared to controls and IL-25 expression is up-regulated in NP mucosa from patients with CRS with NPs compared with control subjects and those with CRS without NPs. IL-25 mRNA expression positively correlated with the expression of T-box transcription factor, RAR-related orphan receptor C, GATA3, eosinophil cationic protein, TGF-β1, and TGF-β2. In the murine NP model IL-25 was also more abundant compared with controls mice, and similar correlations with inflammatory markers were observed. Anti-IL-25 treatment reduced the number of polyps, mucosal edema thickness, collagen deposition, infiltration with inflammatory cells, and expression of IL-4 and IFN-γ, CCL11, CXCL2, ICAM 1 and VCAM 1.108
Th17 cells are increased in both skin52, 53 and 54 and blood of patients with AD.109 In a mouse model of AD deficiency of filaggrin appeared to be a driver of increased peripheral levels of Th17 cells. The authors hypothesized that this increase must be acquired as peripheral Th17 cells were found only in adult mice indicating involvement of exogenous factors.110
Neurogenic inflammation
Neurogenic rhinitis is a particular endotype characterized by a relative overexpression of transient receptor potential channels on trigeminal nerves and high concentrations of substance P and neurokinins and is linked to gustatory rhinitis, rhinitis of the elderly, and idiopathic rhinitis with nasal hyperreactivity.111 The serum level of the nerve growth factor (NGF) is significantly higher in AD compared to controls, and correlates with the severity of itch, erythema, scale/xerosis and eosinophil count.112 There is increased expression of NGF in the lesional compared to non-lesional AD and the number of mast cell-nerve fibers (NF) contacts correlates with SCORAD and itch in lesional skin. Nicotinic acetylcholine receptor α7 mRNA, a marker for the non-neuronal cholinergic system (NNCS) was significantly lower in lesional AD skin at baseline. After the stress test NF numbers dropped in lesional AD as did their contacts with mast cells and NGF + NF now correlated with SCORAD and mast cell-NF contacts with itch in non-lesional skin. At the same time, expression of secreted mammal Ly-6/urokinase-type plasminogen activator receptor-related levels (a marker for NNCS activation) increased in lesional AD skin.113
The mixed type 2/Th17 endotype
The mixed Th17/Th2 endotype is not rare in asthma, CRS or AD. Th2 cells can differentiate into dual-positive Th2/Th17 cells114 and these cells were identified in the BAL fluid of asthmatic patients and related to glucocorticoid resistance in vitro and airway obstruction and hyperreactivity.43 In CRS IL-25 receptor (IL-17RB)-expressing Th2 effector cells were identified in NP tissue but not the healthy nasal mucosa or periphery, while abundant IL-17-producing T cells were observed in both healthy nasal mucosal and polyp populations, thus suggesting that the Th17 response might be important in healthy nasal mucosal immune homeostasis and the NP inflammation and remodeling occurs within the mixed endotype.115 A non-type 2 immune response mixing Th1, Th17 and Th22 driven inflammation and epithelial dysfunction is also described for AD in non-lesional skin and in the chronic remitting-relapsing form of the disease.67, 68 and 69
The relationship between Th17 and type 2 immune response is highly complex. An interesting model suggests that IL-17 produced by γδ T cells and by Th17 cells in response to injured epithelium enhances the production of IL-4 and IL-13 from ILC2 and Th2 cells, which acts as a negative feedback loop shutting down further IL-17 production and neutrophilia.116 Conversely, IL-4 and IL-13 may amplify Th17 responses by up-regulating CD209a expression on dendritic cells.117 When the type 2 response fails to fully suppress the IL-17 response, or further promotes it, excessive tissue damage can occur. Understanding what regulates the IL-17–IL-4/13 feedback loops will provide invaluable insight into situations in which IL-17 exacerbates type 2 inflammation.
In a cross-sectional study of asthmatics of varying severity endo-bronchial tissue gene expression analysis revealed three major patient clusters: Th2-high, Th17-high, and Th2/17-low. In individual patient samples, Th2-high and Th17-high patterns were mutually exclusive and their gene signatures were inversely correlated and differentially regulated by IL-13 and IL-17A. This dichotomous pattern was further investigated in a preclinical model of allergen-induced asthma. Neutralization of IL-4 and/or IL-13 resulted in increased Th17 cells and neutrophilic inflammation in the lung. Neutralization of both IL-13 and IL-17 protected mice from eosinophilia, mucus hyperplasia, and airway hyperreactivity and abolished the neutrophilic inflammation, suggesting that combination therapies targeting both pathways may maximize therapeutic efficacy across a patient population with a mixed Th2/Th17 endotype.118
Chitinases and chitinase-like proteins (CLPs) may be an important link between type 2 immunity and IL-17. Acting as danger-associated molecular patterns CLPs release IL-1 with IL-17 production by innate γδ T cells, which in turn drives a type 2 response. Subsequently type 2 cytokines induce even more CLP expression, which likely further contribute to repair. Additionally, CLPs can promote Th2 differentiation and suppress IFNγ, further promoting type 2 immunity.119 Furthermore neutrophils can switch to an N2 phenotype, contributing to the pool of IL-13, which in addition to IL-4, promotes activation of macrophages limiting further injury and promoting repair.120 IL-33 is a co-factor that cooperates with IL-17A to exacerbate AHR by enhancing neutrophilic inflammation via CXCR2 signaling. Furthermore, CXCR2 signaling derived Th2 responses are enhanced.118 In patients with CRS with NP IL-25 and IL-33 interact locally with IL-17RB+ST2+ polyp T cells to augment Th2 responses.115 IL-17 significantly increases MUC5B mucin expression, while IL-13 additionally induces significant goblet cell hyperplasia and MUC5AC mucin expression in CRS with NP. IFN-γ and IL-13 both significantly reduce ciliated cell differentiation and ciliary beat frequency.121
Unmet needs and perspectives
To emphasize the importance of endotyping of diseases, discovery of biomarkers, it will be good to quote a pioneer in precision medicine, Sir John Bell, Professor of Medicine at Oxford University, and Chairman of the Office for the Strategic Coordination of Health Research: “The best example of precision medicine in my opinion does not come from cancer, it comes from asthma. For this condition, we have gone more than 20 years without a new drug, because the disease was not defined very well.” (http://www.pharmafile.com/news/.) As said, successful management of patients with severe asthma and allergic diseases continues to be a major unmet need. One of the barriers to successful management is the heterogeneity of the diseases with different phenotypes and endotypes. A revised paradigm for disease management, that entails categorization of patients via use of endotypes and multiomic biomarkers for prescribing targeted therapy, will replace the “one size fits all” approach to allergic diseases. The success of cytokine inhibition defining the hierarchical position of distinct cytokines in allergic diseases pathogenesis with the description of meaningful clinical endotypes hold the promise to transform the therapeutic landscape in allergic diseases in a precision based fashion.
The precision medicine initiative recently announced the need to move the field of precision medicine more rapidly into clinical care. As currently structured, it will primarily fund efforts in cancer genomics with longer-term goals of advancing precision medicine to all areas of health. This focused effort provides scientists, clinicians, and patients within the allergy community an opportunity to work together boldly to advance clinical care; the community needs to be aware and engaged in the process as it progresses.
To move beyond a select few genes/drugs, the successful adoption of pharmacogenomics into routine clinical care and development of computational approaches and tools to effectively integrate multidomain data (such as cognitive IT-systems) are urgently needed for the development of newly targeted treatments. Real-time databases for molecular profiling data could become a pragmatic solution to several knowledge management problems in the practice and science of precision medicine. “Interventional informatics” approach can substantially improve human health and wellness through the use of data-driven interventions at the point of care of broader population levels. The collaborative medicine approach with open access to research databases worldwide will speed the discovery of new targets.
Conclusion
The endotype driven approach implementing multiomics, biomarkers and computation approaches to big data analysis is slowly making its way into the precision management of allergic diseases.
Several disease complex endotypes can be identified for asthma, AR, CRS and AD. Sub-endotypes exist within complex endotype umbrella, and their preponderance differs between allergic diseases. Both the innate and the acquired immune response contribute to type 2 and non type-2 immune response endotypes and non-allergic mechanisms such as environmental factors, psycho-social stress, activation of metabolic pathways, resident cells in the remodeled phenotype or epithelial barrier dysfunction further modulate the profile of the inflammation.
The recent focus on precision medicine opens new opportunities for the allergy community to advance in the clinical care of allergic patients in a cost-efficient and equitable way.
Conflict of interest
CAA received research funding from Allergopharma AG. IA has no conflict of interest.
Acknowledgments
Ioana Agache wrote the review as part of the preparation for the research project PN-II-RU-TE-2014-4-2303.
Cezmi A. Akdiss research is supported by Swiss National Foundation grant no: 310030_156823.
References
- 1 C.A. Akdis, Z. Ballas; Precision medicine & precision health: building blocks to foster a revolutionary healthcare model; J Allergy Clin Immunol, 137 (2016), pp. 1359–1361
- 2 S. Galli; Toward precision medicine and health: promises opportunities and challenges in allergic diseases; J Allergy Clin Immunol, 137 (2016), pp. 1289–1300
- 3 A. Muraro, R.F. Lemanske, P.W. Hellings, C.A. Akdis, T. Bieber, T.B. Casale, et al.; Precision medicine in patients with allergic diseases: airway diseases and atopic dermatitis—PRACTALL document of the European Academy of Allergy and Clinical Immunology and the American Academy of Allergy, Asthma & Immunology; J Allergy Clin Immunol, 137 (2016), pp. 1347–1358
- 4 J. Lötvall, C.A. Akdis, L.B. Bacharier, L. Bjermer, T.B. Casale, A. Custovic, et al.; Asthma endotypes: a new approach to classification of disease entities within the asthma syndrome; J Allergy Clin Immunol, 127 (2011), pp. 355–360
- 5 I. Agache, C. Akdis, M. Jutel, J.C. Virchow; Untangling asthma phenotypes and endotypes; Allergy, 67 (2012), pp. 835–846
- 6 I. Agache; From phenotypes to endotypes to asthma treatment; Curr Opin Allergy Clin Immunol, 13 (2013), pp. 249–256
- 7 I. Agache, K. Sugita, H. Morita, M. Akdis, C.A. Akdis; The complex type 2 endotype in allergy and asthma: from laboratory to bedside; Curr Allergy Asthma Rep, 15 (2015), p. 29
- 8 A. DeVries, D. Vercelli; Early predictors of asthma and allergy in children: the role of epigenetics; Curr Opin Allergy Clin Immunol, 15 (2015), pp. 435–439
- 9 A. DeVries, G. Wlasiuk, S.J. Miller, A. Bosco, D.A. Stern, J. Nicodemus-Johnson, et al.; Neonatal epigenetic predictors of childhood asthma map to immunoregulatory and pro-inflammatory pathways [abstract]; Am J Respir Crit Care Med, 191 (2015), p. A3524
- 10 D. Martino, J.E. Joo, A. Sexton-Oates, T. Dang, K. Allen, R. Saffery, et al.; Epigenome wide association study reveals longitudinally stable DNA methylation differences in CD4þ T cells from children with IgE-mediated food allergy; Epigenetics, 9 (2014), pp. 998–1006
- 11 G.A. Lockett, N. Soto-Ramírez, M.A. Ray, T.M. Everson, C.J. Xu, V.K. Patil, et al.; Association of season of birth with DNA methylation and allergic disease; Allergy (2016) http://dx.doi.org/10.1111/all.12882
- 12 I.V. Yang, B.S. Pedersen, A. Liu, G.T. O'Connor, S.J. Teach, M. Kattan, et al.; DNA methylation and childhood asthma in the inner city; J Allergy Clin Immunol, 136 (2015), pp. 69–80
- 13 T.M. Murphy, C.C. Wong, L. Arseneault, J. Burrage, R. Macdonald, E. Hannon, et al.; Methylomic markers of persistent childhood asthma: a longitudinal study of asthma-discordant monozygotic twins; Clin Epigenetics, 7 (2015), p. 130
- 14 D. Martino, T. Dang, A. Sexton-Oates, S. Prescott, M.L. Tang, S. Dharmage, et al.; Blood DNA methylation biomarkers predict clinical reactivity in food-sensitized infants; J Allergy Clin Immunol, 135 (2015), pp. 1319–1328
- 15 J.A. Wagner; Overview of biomarkers and surrogate endpoints in drug development; Dis Markers, 18 (2002), pp. 41–46
- 16 J.A. Wagner, S.A. Williams, C.J. Webster; Biomarkers and surrogate end points for fit-for-purpose development and regulatory evaluation of new drugs; Clin Pharmacol Ther, 81 (2007), pp. 104–107
- 17 A. Berry, W.W. Busse; Biomarkers in asthma; has their time come to direct treatment?; J Allergy Clin Immunol, 137 (2016), pp. 1317–1324
- 18 F.M. Goodsaid, F.W. Frueh, W. Mattes; Strategic paths for biomarker qualification; Toxicology, 245 (2008), pp. 219–223
- 19 A. Muraro, W.J. Fokkens, S. Pietikainen, D. Borrelli, I. Agache, J. Bousquet, et al.; European symposium on precision medicine in allergy and airways diseases: report of the European Union Parliament Symposium (October 14, 2015); Allergy (2015) http://dx.doi.org/10.1111/all.12819
- 20 J.L. Jameson, D.L. Longo; Precision medicine – personalized, problematic, and promising; N Engl J Med, 372 (2015), pp. 2229–2234
- 21 I. Agache, D.L. Strasser, A. Klenk, C. Agache, H. Farine, C. Ciobanu, et al.; Serum IL-5 and IL-13 consistently serve as the best predictors for the blood eosinophilia phenotype in adult asthmatics; Allergy (2016) http://dx.doi.org/10.1111/all.12906
- 22 J.A. Howrylak, M. Moll, S.T. Weiss, B.A. Raby, W. Wu, E.P. Xing; Gene expression profiling of asthma phenotypes demonstrates molecular signatures of atopy and asthma control; J Allergy Clin Immunol (2016) http://dx.doi.org/10.1016/j.jaci.2015.09.058
- 23 P.G. Woodruff, B. Modrek, D.F. Choy, G. Jia, A.R. Abbas, Ellwanger, et al.; T-helper type 2-driven inflammation defines major subphenotypes of asthma; Am J Respir Crit Care Med, 180 (2009), pp. 388–395
- 24 N. Meyer, J.W. Dallinga, S.J. Nuss, E.J. Moonen, J.J. van Berkel, C. Akdis, et al.; Defining adult asthma endotypes by clinical features and patterns of volatile organic compounds in exhaled air; Respir Res, 15 (2014), p. 136
- 25 N. Meyer, S.J. Nuss, T. Rothe, A. Siebenhüner, C.A. Akdis, G. Menz; Differential serum protein markers and the clinical severity of asthma; J Asthma Allergy, 7 (2014), pp. 67–75
- 26 M.C. Peters, Z.K. Mekonnen, S. Yuan, N.R. Bhakta, P.G. Woodruff, J.V. Fahy; Measures of gene expression in sputum cells can identify TH2-high and TH2-low subtypes of asthma; J Allergy Clin Immunol, 133 (2014), pp. 388–394
- 27 X. Yan, J.H. Chu, J. Gomez, M. Koenigs, C. Holm, X. He, et al.; Noninvasive analysis of the sputum transcriptome discriminates clinical phenotypes of asthma; Am J Respir Crit Care Med, 191 (2015), pp. 1116–1125
- 28 C.R. Williams-DeVane, D.M. Reif, E.C. Hubal, P.R. Bushel, E.E. Hudgens, J.E. Gallagher, et al.; Decision tree-based method for integrating gene expression, demographic, and clinical data to determine disease endotypes; BMC Syst Biol, 7 (2013), p. 119
- 29 J. Hagenaars, A. McCutcheon (Eds.), Applied Latent Class Analysis, Cambridge University Press, Cambridge (2002), p. 454
- 30 D. Pe'er; Bayesian network analysis of signaling networks: a primer; Sci STKE, 2005 (2005), p. pl4
- 31 M. Altaf-Ul-Amin, T. Katsuragi, T. Sato, S. Kanaya; A glimpse to background and characteristics of major molecular biological networks; Biomed Res Int, 2015 (2015), p. 540297
- 32 L. Mastalerz, N. Celejewska-Wójcik, K. Wójcik, A. Gielicz, A. Ćmiel, M. Ignacak, et al.; Induced sputum supernatant bioactive lipid mediators can identify subtypes of asthma; Clin Exp Allergy, 45 (2015), pp. 1779–1789
- 33 T. Hinks, X. Zhou, K. Staples, B. Dimitrov, A. Manta, T. Petrossian, et al.; Multidimensional endotypes of asthma: topological data analysis of cross-sectional clinical, pathological, and immunological data; Lancet, 385 (Suppl. 1) (2015), p. S42
- 34 T.S. Hinks, T. Brown, L.C. Lau, H. Rupani, C. Barber, S. Elliott, et al.; Multidimensional endotyping in patients with severe asthma reveals inflammatory heterogeneity in matrix metalloproteinases and chitinase 3-like protein 1; J Allergy Clin Immunol (2016) http://dx.doi.org/10.1016/j.jaci.2015.11.020
- 35 J.H. Friedman; Multivariate adaptive regression splines; Ann Stat, 19 (1991), pp. 1–67
- 36 A.R. Brasier, S. Victor, H. Ju, W.W. Busse, D. Curran-Everett, E. Bleecker, et al.; Predicting intermediate phenotypes in asthma using bronchoalveolar lavage-derived cytokines; Clin Transl Sci, 3 (2010), pp. 147–157
- 37 B.J. George, D.M. Reif, J.E. Gallagher, C.R. Williams-DeVane, B.L. Heidenfelder, E.E. Hudgens, et al.; Data-driven asthma endotypes defined from blood biomarker and gene expression data; PLoS One, 10 (2015), p. e0117445
- 38 M.J. McGeachie, A. Dahlin, W. Qiu, D.C. Croteau-Chonka, J. Savage, A.C. Wu, et al.; The metabolomics of asthma control: a promising link between genetics and disease; Immun Inflamm Dis, 3 (2015), pp. 224–238
- 39 F. Yang, X. Yu, L. Wang, L. Liu, X. Xu, X. Zheng, et al.; Identify asthma genes across three phases based on protein-protein interaction network; IET Syst Biol, 9 (2015), pp. 135–140
- 40 A.N. Greiner, P.W. Hellings, G. Rotiroti, G.K. Scadding; Allergic rhinitis; Lancet, 378 (2011), pp. 2112–2122
- 41 Akdis CA. The underlying mechanisms in allergy (overview). EAACI Global Atlas of Allergy. http://www.eaaci.org/resources/scientific-output/global-atlas-of-allergy.html.
- 42 R.H. Dougherty, S.S. Sidhu, K. Raman, M. Solon, O.D. Solberg, G.H. Caughey, et al.; Accumulation of intraepithelial mast cells with a unique protease phenotype in T(H)2-high asthma; J Allergy Clin Immunol, 125 (2010), pp. 1046–1053
- 43 C. Irvin, I. Zafar, J. Good, D. Rollins, C. Christianson, M.M. Gorska, et al.; Increased frequency of dual-positive TH2/TH17 cells in bronchoalveolar lavage fluid characterizes a population of patients with severe asthma; J Allergy Clin Immunol, 134 (2014), pp. 1175–1186
- 44 J.W. Steinke, L. Liu, P. Huyett, J. Negri, S.C. Payne, L. Borish; Prominent role of IFN-γ in patients with aspirin-exacerbated respiratory disease; J Allergy Clin Immunol, 132 (2013), pp. 856–865 e1-3
- 45 G.S. Marijsse, S.F. Seys, A.-S. Schelpe, E. Dilissen, P. Goeminne, L.J. Dupont, et al.; Obese individuals with asthma preferentially have a high IL-5/IL-17A/IL-25 sputum inflammatory pattern; Am J Respir Crit Care Med, 189 (2014), pp. 1284–1285
- 46 H. Hammad, B.N. Lambrecht; Barrier epithelial cells and the control of type 2 immunity; Immunity, 43 (2015), pp. 29–40
- 47 R.H. Green, C.E. Brightling, G. Woltmann, D. Parker, A.J. Wardlaw, I.D. Pavord; Analysis of induced sputum in adults with asthma: identification of subgroup with isolated sputum neutrophilia and poor response to inhaled corticosteroids; Thorax, 57 (2002), pp. 875–879
- 48 P. Haldar, C.E. Brightling, B. Hargadon, S. Gupta, W. Monteiro, A. Sousa, et al.; Mepolizumab and exacerbations of refractory eosinophilic asthma; N Engl J Med, 360 (2009), pp. 973–984
- 49 P. Nair, M.M. Pizzichini, M. Kjarsgaard, M.D. Inman, A. Efthimiadis, E. Pizzichini, et al.; Mepolizumab for prednisone-dependent asthma with sputum eosinophilia; N Engl J Med, 360 (2009), pp. 985–993
- 50 J. Corren, R.F. Lemanske, N.A. Hanania, P.E. Korenblat, M.V. Parsey, J.R. Arron, et al.; Lebrikizumab treatment in adults with asthma; N Engl J Med, 365 (2011), pp. 1088–1098
- 51 N.A. Hanania, M. Noonan, J. Corren, P. Korenblat, Y. Zheng, S.K. Fischer, et al.; Lebrikizumab in moderate-to-severe asthma: pooled data from two randomised placebo-controlled studies; Thorax, 70 (2015), pp. 748–756
- 52 S. Wenzel, L. Ford, D. Pearlman, S. Spector, L. Sher, F. Skobieranda, et al.; Dupilumab in persistent asthma with elevated eosinophil levels; N Engl J Med, 368 (2013), pp. 2455–2466
- 53 I.D. Pavord, S. Korn, P. Howarth, E.R. Bleecker, R. Buhl, O.N. Keene, et al.; Mepolizumab for severe eosinophilic asthma (DREAM): a multicentre, double-blind, placebo-controlled trial; Lancet, 380 (2012), pp. 651–659
- 54 H.G. Ortega, M.C. Liu, I.D. Pavord, G.G. Brusselle, J.M. FitzGerald, A. Chetta, MENSA Investigators, et al.; Mepolizumab treatment in patients with severe eosinophilic asthma; N Engl J Med, 371 (2014), pp. 1198–1207
- 55 J. Corren, S. Weinstein, L. Janka, J. Zangrilli, M. Garin; Phase 3 study of reslizumab in patients with poorly controlled asthma: effects across a broad range of eosinophil counts; Chest (2016) http://dx.doi.org/10.1016/j.chest.2016.03.018
- 56 N.A. Hanania, S. Wenzel, K. Rosén, H.J. Hsieh, S. Mosesova, D.F. Choy, et al.; Exploring the effects of omalizumab in allergic asthma: an analysis of biomarkers in the EXTRA study; Am J Respir Crit Care Med, 187 (2013), pp. 804–811
- 57 M. Humbert, W. Busse, N.A. Hanania, P.J. Lowe, J. Canvin, V.J. Erpenbeck, et al.; Omalizumab in asthma: an update on recent developments; J Allergy Clin Immunol Pract, 2 (2014), pp. 525–536
- 58 I.P. Hall, A.V. Fowler, A. Gupta, K. Tetzlaff, M.C. Nivens, M. Sarno, et al.; Efficacy of BI 671800, an oral CRTH2 antagonist, in poorly controlled asthma as sole controller and in the presence of inhaled corticosteroid treatment; Pulm Pharmacol Ther, 32 (2015), pp. 37–44
- 59 Z. Diamant, P.N. Sidharta, D. Singh, B.J. O'Connor, R. Zuiker, B.R. Leaker, et al.; Setipiprant, a selective CRTH2 antagonist, reduces allergen-induced airway responses in allergic asthmatics; Clin Exp Allergy, 44 (2014), pp. 1044–1052
- 60 R. Pettipher, M.G. Hunter, C.M. Perkins, L.P. Collins, T. Lewis, M. Baillet, et al.; Heightened response of eosinophilic asthmatic patients to the CRTH2 antagonist OC000459; Allergy, 69 (2014), pp. 1223–1232
- 61 C.A. Akdis, C. Bachert, C. Cingi, M.S. Dykewicz, P.W. Hellings, R.M. Naclerio, et al.; Endotypes and phenotypes of chronic rhinosinusitis: a PRACTALL document of the European Academy of Allergy and Clinical Immunology and the American Academy of Allergy, Asthma & Immunology; J Allergy Clin Immunol, 131 (2013), pp. 1479–1490
- 62 H.P. Barham, J.L. Osborn, K. Snidvongs, N. Mrad, R. Sacks, R.J. Harvey; Remodeling changes of the upper airway with chronic rhinosinusitis; Int Forum Allergy Rhinol, 5 (2015), pp. 565–572
- 63 P. Tomassen, G. Vandeplas, T. Van Zele, L.O. Cardell, J. Arebro, H. Olze, et al.; Inflammatory endotypes of chronic rhinosinusitis based on cluster analysis of biomarkers; J Allergy Clin Immunol (2016) http://dx.doi.org/10.1016/j.jaci.2015.12.1324
- 64 P. Gevaert, N. Van Bruaene, T. Cattaert, K. Van Steen, T. Van Zele, F. Acke, et al.; Mepolizumab, a humanized anti–IL-5 mAb, as a treatment option for severe nasal polyposis; J Allergy Clin Immunol, 128 (2011), pp. 989–995
- 65 P. Gevaert, L. Calus, T. Van Zele, K. Blomme, N. De Ruyck, W. Bauters, et al.; Omalizumab is effective in allergic and nonallergic patients with nasal polyps and asthma; J Allergy Clin Immunol, 131 (2013), pp. 110–116
- 66 C. Bachert, L. Mannent, R.M. Naclerio, J. Mullol, B.J. Ferguson, P. Gevaert, et al.; Effect of subcutaneous dupilumab on nasal polyp burden in patients with chronic sinusitis and nasal polyposis: a randomized clinical trial; JAMA, 315 (2016), pp. 469–479
- 67 S. Noda, M. Suárez-Fariñas, B. Ungar, S.J. Kim, C. de Guzman Strong, H. Xu, et al.; The Asian atopic dermatitis phenotype combines features of atopic dermatitis and psoriasis with increased TH17 polarization; J Allergy Clin Immunol, 136 (2015), pp. 1254–1264
- 68 T. Czarnowicki, J. Gonzalez, A. Shemer, D. Malajian, H. Xu, X. Zheng, et al.; Severe atopic dermatitis is characterized by selective expansion of circulating TH2/TC2 and TH22/TC22, but not TH17/TC17, cells within the skin-homing T-cell population; J Allergy Clin Immunol, 136 (2015), pp. 104–115
- 69 T. Czarnowicki, H. Esaki, J. Gonzalez, D. Malajian, A. Shemer, S. Noda, et al.; Early pediatric atopic dermatitis shows only a cutaneous lymphocyte antigen (CLA)(+) TH2/TH1 cell imbalance, whereas adults acquire CLA(+) TH22/TC22 cell subsets; J Allergy Clin Immunol, 136 (2015), pp. 941–951
- 70 L.A. Beck, D. Thaçi, J.D. Hamilton, N.M. Graham, T. Bieber, R. Rocklin, et al.; Dupilumab treatment in adults with moderate-to-severe atopic dermatitis; N Engl J Med, 371 (2014), pp. 130–139
- 71 D. Thaçi, E.L. Simpson, L.A. Beck, T. Bieber, A. Blauvelt, K. Papp, et al.; Efficacy and safety of dupilumab in adults with moderate-to-severe atopic dermatitis inadequately controlled by topical treatments: a randomised, placebo-controlled, dose-ranging phase 2b trial; Lancet, 387 (2016), pp. 40–52
- 72 J.D. Hamilton, M. Suárez-Fariñas, N. Dhingra, I. Cardinale, X. Li, A. Kostic, et al.; Dupilumab improves the molecular signature in skin of patients with moderate-to-severe atopic dermatitis; J Allergy Clin Immunol, 134 (2014), pp. 1293–1300
- 73 M. Hotze, H. Baurecht, E. Rodríguez, N. Chapman-Rothe, M. Ollert, R. Fölster-Holst, et al.; Increased efficacy of omalizumab in atopic dermatitis patients with wild-type filaggrin status and higher serum levels of phosphatidylcholines; Allergy, 69 (2014), pp. 132–135
- 74 W.C. Moore, D.A. Meyers, S.E. Wenzel, W.G. Teague, H. Li, X. Li, National Heart, Lung, and Blood Institutes Severe Asthma Research Program, et al.; Identification of asthma phenotypes using cluster analysis in the Severe Asthma Research Program; Am J Respir Crit Care Med, 181 (2010), pp. 315–323
- 75 K.J. Baines, J.L. Simpson, L.G. Wood, R.J. Scott, P.G. Gibson; Transcriptional phenotypes of asthma defined by gene expression profiling of induced sputum samples; J Allergy Clin Immunol, 127 (2011), pp. 153–160
- 76 H. Lou, Y. Meng, Y. Piao, N. Zhang, C. Bachert, C. Wang, et al.; Cellular phenotyping of chronic rhinosinusitis with nasal polyps; Rhinology (2016 Jan 9) [Epub ahead of print]
- 77 N. Zhang, T. Van Zele, C. Perez-Novo, N. Van Bruaene, G. Holtappels, N. DeRuyck, et al.; Different types of T-effector cells orchestrate mucosal inflammation in chronic sinus disease; J Allergy Clin Immunol, 122 (2008), pp. 961–968
- 78 D.W. Kim, D.K. Kim, A. Jo, H.R. Jin, K.M. Eun, J.H. Mo, et al.; Age-related decline of neutrophilic inflammation is associated with better postoperative prognosis in non-eosinophilic nasal polyps; PLoS One, 11 (2016), p. e0148442
- 79 I. Agache; Non-eosinophilic asthma endotypes; Curr Treat Options Allergy, 2 (2015), pp. 257–267
- 80 J.L. Simpson, T.V. Grissell, J. Douwes, R.J. Scott, M.J. Boyle, P.G. Gibson; Innate immune activation in neutrophilic asthma and bronchiectasis; Thorax, 62 (2007), pp. 211–218
- 81 K.J. Baines, J.L. Simpson, L.G. Wood, R.J. Scott, N.L. Fibbens, H. Powell, et al.; Sputum gene expression signature of 6 biomarkers discriminates asthma inflammatory phenotypes; J Allergy Clin Immunol, 133 (2014), pp. 997–1007
- 82 L. Dejager, K. Dendoncker, M. Eggermont, J. Souffriau, F. Van Hauwermeiren, M. Willart, et al.; Neutralizing TNFα restores glucocorticoid sensitivity in a mouse model of neutrophilic airway inflammation; Mucosal Immunol, 8 (2015), pp. 1212–1225
- 83 Y. Mikami, H. Matsuzaki, M. Horie, S. Noguchi, T. Jo, O. Narumoto, et al.; Lymphotoxin β receptor signaling induces IL-8 production in human bronchial epithelial cells; PLoS One, 9 (2014), p. e114791
- 84 K.J. Baines, J.L. Simpson, N.A. Bowden, R.J. Scott, P.G. Gibson; Differential gene expression and cytokine production from neutrophils in asthma phenotypes; Eur Respir J, 35 (2010), pp. 522–531
- 85 P. Gao, P.G. Gibson, K.J. Baines, I.A. Yang, J.W. Upham, P.N. Reynolds, et al.; Anti-inflammatory deficiencies in neutrophilic asthma: reduced galectin-3 and IL-1RA/IL-1ß; Respir Res, 16 (2015), p. 5
- 86 J.L. Simpson, P.G. Gibson, I.A. Yang, J. Upham, A. James, P.N. Reynolds, et al.; Impaired macrophage phagocytosis in non-eosinophilic asthma; Clin Exp Allergy, 43 (2013), pp. 29–35
- 87 J. Marcinkiewicz, P. Stręk, M. Strus, R. Głowacki, M. Ciszek-Lenda, K. Zagórska-Świeży, et al.; Staphylococcus epidermidis and biofilm-associated neutrophils in chronic rhinosinusitis. A pilot study; Int J Exp Pathol, 96 (2015), pp. 378–386
- 88 J.L. Simpson, R.J. Scott, M.J. Boyle, P.G. Gibson; Differential proteolytic enzyme activity in eosinophilic and neutrophilic asthma; Am J Resp Crit Care Med, 172 (2005), pp. 559–565
- 89 D.W. Russell, J.M. Wells, J.E. Blalock; Disease phenotyping in chronic obstructive pulmonary disease: the neutrophilic endotype; Curr Opin Pulm Med, 22 (2016), pp. 91–99
- 90 C. Nembrini, B.J. Marsland, M. Kopf; IL-17-producing T cells in lung immunity and inflammation; J Allergy Clin Immunol, 123 (2009), pp. 986–994
- 91 S. Yu, H.Y. Kim, Y.-J. Chang, R.H. DeKruyff, D.T. Umetsu; Innate lymphoid cells and asthma; J Allergy Clin Immunol, 133 (2014), pp. 943–950
- 92 H.Y. Kim, H.J. Lee, Y.-J. Chang, M. Pichavant, S.A. Shore, K.A. Fitzgerald, et al.; Interleukin-17-producing innate lymphoid cells and the NLRP3 inflammasome facilitate obesity-associated airway hyperreactivity; Nat Med, 20 (2014), pp. 54–61
- 93 P.J. Mease; Inhibition of interleukin-17, interleukin-23 and the TH17 cell pathway in the treatment of psoriatic arthritis and psoriasis; Curr Opin Rheumatol, 27 (2015), pp. 127–133
- 94 R.H. Wilson, G.S. Whitehead, H. Nakano, M.E. Free, J.K. Kolls, D.N. Cook; Allergic sensitization through the airway primes Th17-dependent neutrophilia and airway hyperresponsiveness; Am J Respir Crit Care Med, 180 (2009), pp. 720–730
- 95 J. Zhao, C.M. Lloyd, A. Noble; Th17 responses in chronic allergic airway inflammation abrogate regulatory T-cell-mediated tolerance an contribute to airway remodeling; Mucosal Immunol, 6 (2013), pp. 335–346
- 96 W.W. Busse, S. Holgate, E. Kerwin, Y. Chon, J. Feng, J. Lin, et al.; Randomized, double-blind, placebo-controlled study of brodalumab, a human anti-IL-17 receptor monoclonal antibody, in moderate to severe asthma; Am J Respir Crit Care Med, 188 (2013), pp. 1294–1302
- 97 D.M. Bullens, E. Truyen, L. Coteur, E. Dilissen, P.W. Hellings, L.J. Dupont, et al.; IL-17 mRNA in sputum of asthmatic patients: linking T cell driven inflammation and granulocytic influx?; Respir Res, 7 (2006), p. 135
- 98 I. Agache, C. Ciobanu, C. Agache, M. Anghel; Increased serum IL-17 is an independent risk factor for severe asthma; Respir Med, 104 (2010), pp. 1131–1137
- 99 S. Molet, Q. Hamid, F. Davoine, E. Nutku, R. Taha, N. Pagé, et al.; IL-17 is increased in asthmatic airways and induces human bronchial fibroblasts to produce cytokines; J Allergy Clin Immunol, 108 (2001), pp. 430–438
- 100 A. Barczyk, W. Pierzchala, E. Sozañska; Interleukin-17 in sputum correlates with airway hyperresponsiveness to methacholine; Respir Med, 97 (2003), pp. 726–733
- 101 J.W. Chien, C.Y. Lin, K.D. Yang, C.H. Lin, J.K. Kao, Y.G. Tsai; Increased IL-17A secreting CD41 T cells, serum IL-17 levels and exhaled nitric oxide are correlated with childhood asthma severity; Clin Exp Allergy, 43 (2013), pp. 1018–1026
- 102 D. Raedler, N. Ballenberger, E. Klucker, A. Böck, R. Otto, O. Prazeres da Costa, et al.; Identification of novel immune phenotypes for allergic and non-allergic childhood asthma; J Allergy Clin Immunol, 135 (2015), pp. 81–91
- 103 J. Banuelos, S. Shin, Y. Cao, B.S. Bochner, L. Morales-Nebreda, G.R. Budinger, et al.; BCL-2 protects human and mouse Th17 cells from glucocorticoid-induced apoptosis; Allergy (2016) http://dx.doi.org/10.1111/all.12840
- 104 A. Gupta, S. Dimeloe, D.F. Richards, E.S. Chambers, C. Black, Z. Urry, et al.; Defective IL-10 expression and in vitro steroid-induced IL-17A in paediatric severe therapy-resistant asthma; Thorax, 69 (2014), pp. 508–515
- 105 E.S. Chambers, A.M. Nanzer, P.E. Pfeffer, D.F. Richards, P.M. Timms, A.R. Martineau, et al.; Distinct endotypes of steroid-resistant asthma characterized by IL-17A(high) and IFN-γ(high) immunophenotypes: potential benefits of calcitriol; J Allergy Clin Immunol, 136 (2015), pp. 628–637
- 106 C.M. Olcott, J.K. Han, T.D. Cunningham, C.B. Franzese; Interleukin-9 and interleukin-17C in chronic rhinosinusitis; Int Forum Allergy Rhinol (2016) http://dx.doi.org/10.1002/alr.21745
- 107 M. Ramezanpour, S. Moraitis, J.L. Smith, P.J. Wormald, S. Vreugde; Th17 cytokines disrupt the airway mucosal barrier in chronic rhinosinusitis; Mediators Inflamm, 2016 (2016), Article 9798206
- 108 H.W. Shin, D.K. Kim, M.H. Park, K.M. Eun, M. Lee, D. So, et al.; IL-25 as a novel therapeutic target in nasal polyps of patients with chronic rhinosinusitis; J Allergy Clin Immunol, 135 (2015), pp. 1476–1485
- 109 L. Ma, H.B. Xue, X.H. Guan, C.M. Shu, F. Wang, J.H. Zhang, et al.; The imbalance of Th17 cells and CD4(+) CD25(high) Foxp3(+) Treg cells in patients with atopic dermatitis; J Eur Acad Dermatol Venereol, 2 (2014), pp. 1079–1086
- 110 C.M. Bonefeld, T.H. Petersen, J. Bandier, C. Agerbeck, A. Linneberg, K. Ross-Hansen, et al.; Epidermal filaggrin deficiency mediates increased systemic Th17 immune response; Br J Dermatol (2016) http://dx.doi.org/10.1111/bjd.14570
- 111 L. Van Gerven, Y.A. Alpizar, M.M. Wouters, V. Hox, E. Hauben, M. Jorissen, et al.; Capsaicin treatment reduces nasal hyperreactivity and transient receptor potential cation channel subfamily V, receptor 1 (TRPV1) overexpression in patients with idiopathic rhinitis; J Allergy Clin Immunol, 133 (2014), pp. 1332–1339
- 112 J. Yamaguchi, M. Aihara, Y. Kobayashi, T. Kambara, Z. Ikezawa; Quantitative analysis of nerve growth factor (NGF) in the atopic dermatitis and psoriasis horny layer and effect of treatment on NGF in atopic dermatitis; J Dermatol Sci, 53 (2009), pp. 48–54
- 113 E.M. Peters, A. Michenko, J. Kupfer, W. Kummer, S. Wiegand, V. Niemeier, et al.; Mental stress in atopic dermatitis–neuronal plasticity and the cholinergic system are affected in atopic dermatitis and in response to acute experimental mental stress in a randomized controlled pilot study; PLoS One, 9 (2014), p. e113552
- 114 L. Cosmi, L. Maggi, V. Santarlasci, M. Capone, E. Cardilicchia, F. Frosali, et al.; Identification of a novel subset of human circulating memory CD4(+) T cells that produce both IL-17A and IL-4; J Allergy Clin Immunol, 125 (2010), pp. 222–230
- 115 E.P. Lam, H.H. Kariyawasam, B.M. Rana, S.R. Durham, A.N. McKenzie, N. Powell, et al.; IL-25/IL-33-responsive TH2 cells characterize nasal polyps with a default TH17 signature in nasal mucosa; J Allergy Clin Immunol (2015) http://dx.doi.org/10.1016/j.jaci.2015.10.019
- 116 S. Nakajima, A. Kitoh, G. Egawa, Y. Natsuaki, S. Nakamizo, C.S. Moniaga, et al.; IL-17A as an inducer for Th2 immune responses in murine atopic dermatitis models; J Invest Dermatol, 134 (2014), pp. 2122–2130
- 117 H.E. Ponichtera, M.G. Shainheit, B.C. Liu, R. Raychowdhury, B.M. Larkin, J.M. Russo, et al.; CD209a expression on dendritic cells is critical for the development of pathogenic Th17 cell responses in murine schistosomiasis; J Immunol, 192 (2014), pp. 4655–4665
- 118 D.F. Choy, K.M. Hart, L.A. Borthwick, A. Shikotra, D.R. Nagarkar, S. Siddiqui, et al.; TH2 and TH17 inflammatory pathways are reciprocally regulated in asthma; Sci Transl Med, 7 (2015) 301ra129
- 119 T.E. Sutherland, N. Logan, D. Rückerl, A.A. Humbles, S.M. Allan, V. Papayannopoulos, et al.; Chitinase-like proteins promote IL-17-mediated neutrophilia in a tradeoff between nematode killing and host damage; Nat Immunol, 15 (2014), pp. 1116–1125
- 120 F. Chen, W. Wu, A. Millman, J.F. Craft, E. Chen, N. Patel, et al.; Neutrophils prime a long-lived effector macrophage phenotype that mediates accelerated helminth expulsion; Nat Immunol, 15 (2014), pp. 938–946
- 121 N. Mizutani, T. Nabe, S. Yoshino; IL-17A promotes the exacerbation of IL-33-induced airway hyperresponsiveness by enhancing neutrophilic inflammation via CXCR2 signaling in mice; J Immunol, 192 (2014), pp. 1372–1384
Document information
Published on 05/04/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?