Abstract
Clear-cell sarcoma is a rare and malignant soft tissue tumor most commonly located at the distal end of extremities and rarely at the trunk. Data on the clinical features of the tumor is limited, complicating the analysis of prognosis and establishment of treatment protocols.
In our study, we present a case diagnosed with clear-cell sarcoma in his right scapula and treated with tumor resection and chemotherapy, combination of dacarbazine, pharmorubicin and cisplatin. The patient died due to multiple organ failure eight months after operation. Early diagnosis, attentive care, and extended surgical resection combined with adjuvant therapy is of essence in treatment of clear-cell sarcoma.
Keywords
Clear cell sarcoma ; Giant ; Scapular
Clear cell sarcoma (CCS) is a malignant soft tissue tumor with rare incidence. Enzinger reported and explored the histogenesis of CCS in 1965.1 Generally, CCS ranges from 2 cm to 7 cm in diameter and locates at distal end of extremities and rarely at trunk. Only one case of scapula intrusion has been reported so far with diameter around 4.5 cm,2 and this patient’s tumor is the largest one occurring at joint. The clinical features of CCS have only been described to a very limited extent, which significantly inhibits analysis of prognosis and establishment of treatment principle.
Here we report a CCS case with incidence site at right scapula. The patient with giant CCS at right scapular was admitted to our hospital in 2011. After scapula artificial shoulder arthroplasty and ten days of chemotherapy, right scapular mass, right submaxillary lymphadenectasis, ascites and pulmonary metastasis were observed six months post operation. Multiple organ failure caused the death of patient eight months post operation.
Case report
The patient was a 63 years old male. He was admitted to our hospital because “the right scapular pain had been felt for 7 months, and an enclosed mass had been found on the right scapular for more than 4 months” on February 18, 2011. The patient had felt a sense of pain in the right shoulder since July 2010, mainly nocturnal pain, aggravated while moving. He had been treated as “frozen shoulder” for several weeks before transfer. However, relief of symptoms was not observed. The size of painful mass at right scapular had been described as “increasing” since October 2010.
Physical examination indicated that a mass with size of 15 cm × 10 cm × 10 cm in the right scapular region, without surface swelling and with moderate skin temperature. The mass was hard, tender, difficult to push away, and the enlarged left supraclavicular lymph nodes could be felt.
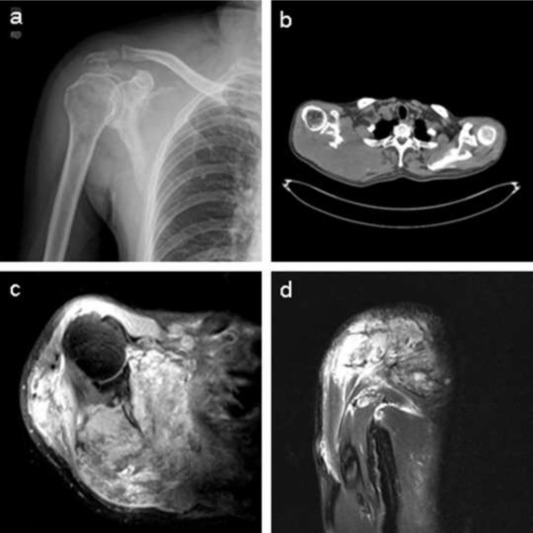
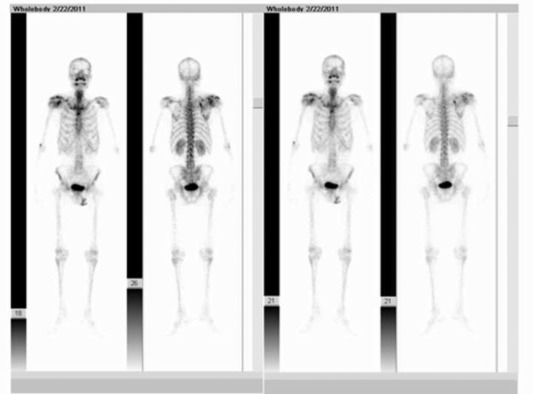
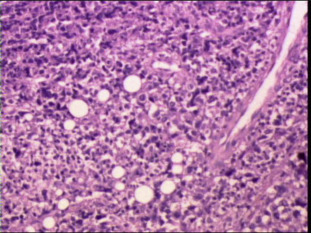
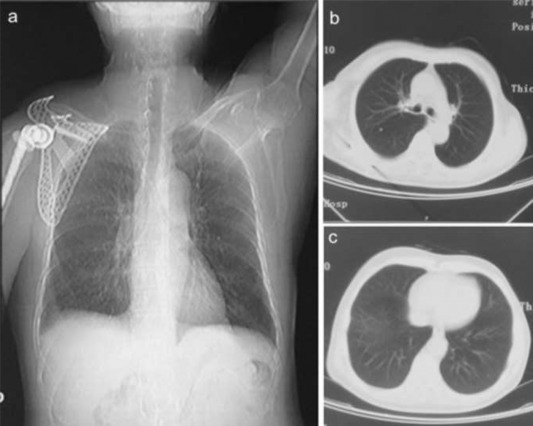
Laboratory tests showed that the serum concentration of CEA reached 17.64 ng/ml. Imaging: X-ray (Fig. 1 a) showed the destruction of the right scapula, and a shadow of soft tissue mass in right scapular region; CT (Fig. 1 b) showed right scapula destructed, surrounded by irregular low-density mass shadow. MRI (Fig. 1 c, d) showed a shadow of soft tissue mass inside of right shoulder, two rounded nodule below the right clavicle, considering as a malignant tumor of the right scapula, right subclavian lymph node metastasis. Emission computed tomography (ECT) showed high metabolism activity in the right scapula, right shoulder and right clavicle bone (Fig. 2 ). Preoperative needle biopsy report: clear cell sarcoma (Fig. 3 ); immunohistochemical staining: PCK (−), LCA (−), Melanoma (−), Syn (+), desmin (−), S-100 (+), CD68 (±), vimentin (+).
|
|
|
Fig. 1. (a), X-ray images show right scapula and that distal clavicle is destructed by tumor. (b), CT images show that right scapula is destructed and surrounded by irregular low-density mass shadow. (c), (d), MRI images show a shadow of soft tissue mass inside of right shoulder and two subclavian lymph nodes metastasis sites. |
|
|
|
Fig. 2. ECT showed high metabolism activity in the right scapula, right shoulder and right clavicle bone. |
|
|
|
Fig. 3. Histological features. The optical image shows that tumor cells are nested and in shape of polygon or spindle, with nuclear vacuolization and prominent nucleoli (HE × 100). |
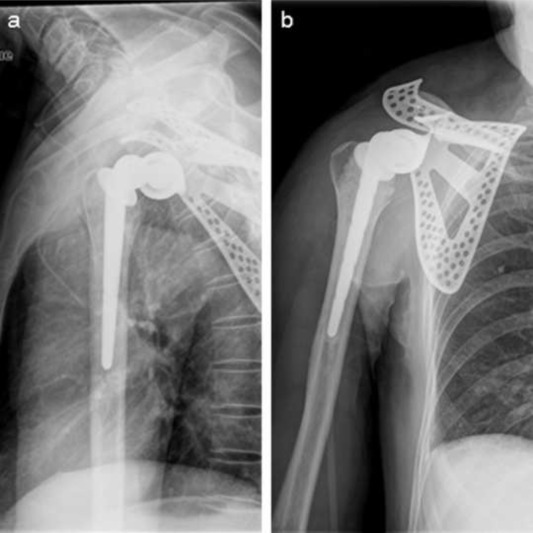
An artificial total shoulder was customized, and the operation of the right scapular tumor resection and tumor type with to wholly the scapula artificial shoulder arthroplasty and lesions lymph node including the pathological lymph node below right subclavian and above left supraclavicular dissection had been performed in March 2011 (Fig. 4 a, b). To achieve full exposure of scapular and tumor, scapular notch was implemented, approximately 2 cm of the distal end of right clavicle excised. Then the original tumor and the 3 cm area surrounding it together with whole right acromioclavicular joint was removed, followed by fixing biceps long head tendon to stump of clavicle and prosthesis installment. After discharge from our hospital, ten days of chemotherapy, combination of dacarbazine, pharmorubicin and cisplatin, was applied in patient in May 2011 in another hospital and given up due to anorexia and vomit. Right scapular mass, right submaxillary lymphadenectasis, and ascites were observed. Nodules in superior lobe of right lung and inferior lobe of left lung were observed in CT results (Fig. 5 a, b, c) which suggested potential pulmonary metastases in September 2011. Multiple organ failure caused the death of patient in November 2011.
|
|
|
Fig. 4. Postoperative X-ray test. Images show that shoulder joint prosthesis is well placed. |
|
|
|
Fig. 5. CT images show nodules in superior lobe of right lung and inferior lobe of left lung. |
The patient, s wife was informed that data from the case would be submitted for publication and gave her consent.
Discussion
The incidence of CCS is rare, accounting for 1% of soft tissue sarcomas, and the main symptom is localized pain. Generally, CCS ranges in size from 2 cm to 7 cm. The preoperative diagnosis of CCS is difficult because the diagnosis must rely on pathological examination and immunohistochemistry assays. The CCS is characterized with poor prognosis, high rate of local recurrence and metastasis, and poor 5-year survival rate. Lymph node metastasis is frequently observed in CCS at early stage. In this case, left supraclavicular lymphadenectasis had been found in preoperative physical examination, MRI result showed possible right subclavian lymph nodes metastasis and pathological examination post surgery confirmed the lymph node metastasis. The description of this case is in line with the characteristics of the CCS.
The main treatment of CCS is surgery.3 During operation, in order to explore the possible invasion of brachial plexus and blood vessels by tumor, pectoralis major deltoid ditch approach was performed and then outside of the 1/3 of the clavicle was exposed. If nerve or blood vessels are invaded by tumor, limb salvage surgery should not be performed. However, based on preoperative MRI results and intraoperative exploration, invasion of nerves and blood vessels by tumor was not observed in this case. Exposure and protection of brachial plexus, axillary artery, particularly musculocutaneous nerve and axillary nerve in operation is critical to reserve full biceps elbow flexion and part of shoulder abduction of patient. The benefit of radical lymph node dissection of CCS is not yet fully understood,4 therefore, selective lymph node dissection was performed in this case. After operation, right elbow, wrist and hand functioned normally, right shoulder remained normal appearance, and the outreach function was partially reserved.
Preoperative and postoperative adjuvant radiotherapy and chemotherapy has become the conventional means of the treatment for malignant tumors, however therapeutic effect of radiotherapy and chemotherapy on CCS is still not clear,5 ; 6 and has side effects, including long treatment cycle, preoperatively rapid growth of tumor, and obvious pain. Therefore, to achieve better surgery tolerance, radiotherapy and chemotherapy was not applied preoperatively. Chemotherapy and radiotherapy were scheduled immediately post-operation, but only chemotherapy was applied one month post-operation for 10 days and terminated due to patients low tolerance to the side effects. In this case, invasion of distal clavicle of right scapula by CCS and lymph node metastasis were observed. The tumor was approximately 15 × 10 × 10 cm in size. Although evaluation of prognosis based on lymph node metastasis and bone invasion is inconclusive, size of CCS acts as a significant factor contributing to prognosis of patients.7 Kawai8 and Ipach9 have revealed that worse prognosis was observed for CCS with diameter greater than 5 cm, and the 5-year and 10-year survival rate was 59% and 41% respectively.7
The patients died eight month post operation as a result of delayed diagnosis, large tumor volume and un-standardized postoperative chemotherapy and radiotherapy. This is consistent with the reported prognosis.
CCS is a rare but highly malignant tumor. Clinically, it should be paid more attention and early diagnosis, surgical extended resection and combined adjuvant therapy are suggested. Due to the poor prognosis, further exploration of advanced diagnosis and treatment approaches for CCS is required.
Conflicts of interest
No conflicts declared.
References
- 1 F.M. Enzinger; Clear-cell sarcoma of tendons and aponeuroses. An analysis of 21 cases; Cancer, 18 (1965), pp. 1163–1174
- 2 C.J. Kazakos, V.G. Galanis, A. Giatromanolaki, D.A. Verettas, E. Sivridis; Clear cell sarcoma of the scapula. A case report and review of the literature; World J Surg Oncol, 4 (2006), p. 48
- 3 X. Liu, H. Zhang, Y. Dong; Primary clear cell sarcoma of humerus: case report; World J Surg Oncol, 9 (2011), p. 163
- 4 D.R. Kuiper, H.J. Hoekstra, R.P. Veth, T. Wobbes; The management of clear cell sarcoma; Eur J Surg Onco, 29 (2003), pp. 568–570
- 5 M. Karita, H. Tsuchiya, N. Yamamoto, T. Shirai, K. Hayashi, H. Nishida; Caffeine-potentiated chemotherapy for clear cell sarcoma: a report of five cases; Int J Clin Oncol, 18 (2013), pp. 33–37
- 6 R.L. Jones, A. Constantinidou, K. Thway, et al.; Chemotherapy in clear cell sarcoma; Med Oncol, 28 (2011), pp. 859–863
- 7 O. Hocar, A. Le Cesne, S. Berissi, et al.; Clear cell sarcoma (malignant melanoma) of soft parts: a clinicopathologic study of 52 cases; Dermatol Res Pract, 2012 (2012), p. 984096
- 8 A. Kawai, A. Hosono, R. Nakayama, et al.; Clear cell sarcoma of tendons and aponeuroses: a study of 75 patients; Cancer, 109 (2007), pp. 109–116
- 9 I. Ipach, F. Mittag, H.G. Kopp, B. Kunze, P. Wolf, T. Kluba; Clear-cell sarcoma of the soft tissue–a rare diagnosis with a fatal outcome; Eur J Cancer Care Engl, 21 (2012), pp. 412–420
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?