Abstract
Perforation of the mesenteric small bowel is an uncommon cause of acute abdomen in the emergency department. Early diagnosis is difficult owing to unspecific clinical presentations. The most common causes of perforation are tumor, trauma, Crohns disease, ischemia, and foreign body ingestion. Currently, computed tomography (CT) is often the initial modality used to assess patients with acute abdomen, and the excellent anatomic details it provides, including segmental bowel wall thickening, mesenteric air bubbles, and fatty infiltration, may help the clinician to diagnose earlier and with greater ease. Here, we present a case of acute abdomen diagnosed as small bowel perforation due to unintentional fish bone ingestion using multidetector CT. The multiplanar reconstruction images from multidetector CT helped locate the perforation site before surgical intervention.
Keywords
Fish bone ; Foreign body ingestion ; Small intestinal perforation
Introduction
Bowel perforation caused by a foreign body has various clinical manifestations. Larger objects are usually retained in the esophagus and stomach, which allows endoscopic diagnosis and possibly even removal. Small bowel perforations are usually caused by sharp and pointed objects [1] . Preoperative diagnosis is difficult because ingestion is usually unintentional [1] ; [2] . Diagnosis largely depends on patient history and physical examination along with any radiographic findings, but it remains very challenging. Computed tomography (CT) findings in these cases usually include thickened intestinal segments and air bubbles near the perforation site as well as a clearly identifiable calcified foreign body [2] ; [3] ; [4] ; [5] .
Case Report
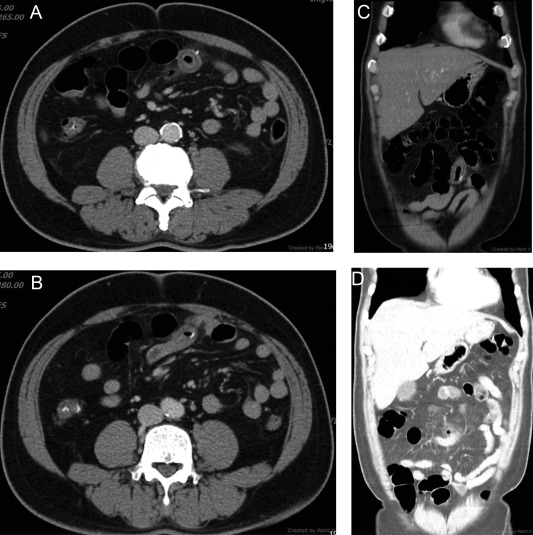
A 54-year-old man presented to the emergency department with worsening lower abdominal pain and anorexia ongoing for 3 days, but without diarrhea or emesis. Upon physical examination, there was local and rebound tenderness over the periumbilical and right lower quadrant areas of the abdomen. Laboratory tests revealed increased inflammatory markers, including a white blood cell count of 13.7 × 103 /μL (90% neutrophils) and a C-reactive protein level of 250 mg/L. An abdominal radiograph in the supine position was obtained but proved unremarkable. The patient was referred for an abdominal ultrasonography (US) where bowel wall thickening was noticed, but it was free of ascites. CT of the abdomen with contrast media demonstrated segmental small bowel wall thickening, adjacent mesenteric fatty stranding, and gas bubble retention. Nearby, one high-density pin-like material penetrating the bowel wall was found (Figure 1 ). Foreign body-induced small bowel perforation was conclusively diagnosed. Based on the patient’s dietary history and the shape of the foreign body, a fish bone was suspected as the cause.
|
|
|
Figure 1. Multidetector computed tomography of the abdomen. (A, B) Axial images demonstrated segmental small bowel wall thickening with fatty infiltration and one radiopaque pin-like lesion penetrating the bowel wall; (C) multiplanar reformation images demonstrate segmental small bowel wall thickening with fatty infiltration; (D) lung window image demonstrates free gas bubbles. |
An emergency surgical intervention—exploratory laparotomy—was performed after the diagnosis was made. One fish bone, measuring 2.2 cm in length, was detected at the site, 110 cm proximal to the ileocecal valve, with a local mesenteric abscess. Segmental resection of the ileum, about 10 cm in length, and reperitonization with debridement of the abscess coating near the bowel wall were performed.
Discussion
Accidental ingestion of a foreign body is common in clinical practice, but it rarely causes gastrointestinal perforation. The majority of foreign bodies pass through the feces, but 1%, especially those with sharper edges and elongated shapes such as fish or chicken bones, may cause perforation [1] ; [2] . The most common sites of perforation include the less fixed segments or those with acute angulation or small lumen, such as the ileal, ileocecal, and rectosigmoid segments. It is a challenge to make an early diagnosis because of the nonspecific clinical presentations. Fortunately, our case presented with an acute abdomen with elevated inflammation markers, and thus CT of the abdomen was arranged immediately, allowing for rapid diagnosis. CT is the diagnostic modality of choice for small gastrointestinal perforations. It provides subtle and definitive anatomical information, including segmental bowel wall thickening (> 8 mm in the stomach, > 3 mm in the jejunum and ileum, and > 5 mm in the colon and rectum) [5] even when close to extraluminal gas bubbles, adjacent mesenteric fatty infiltration, and retained foreign bodies [3] ; [4] ; [5] . The use of modern multidetector CT, with both axial images and multiplanar reformations, allows for better visualization of the whole abdomen and also better specificity in locating the perforation site. The overall accuracy rate when diagnosing the site of the perforation is > 80% [2] .
However, some cases might have contraindications for CT; therefore, US can be used as an alternative mode of imaging. Several advantages of US are its high flexibility, repeatability, low price, lack of radiation burden, and the possibility of a more clinical approach that combines real-time imaging with palpation. US can also be useful in pediatric cases in identifying the location of an ingested foreign body that has not yet been passed to the feces and where surgical removal might be needed [6] . Small intestinal perforation should always be considered when diagnosing cases of acute abdomen presenting at emergency departments. Owing to its high accuracy, CT, especially multidetector CT, is the modality of choice in diagnosing the perforation site.
Conflicts of interest
All authors declare no conflicts of interest.
References
- [1] A.P. Madrona, J.A.F. Hernandez, M.C. Prats, J.R. Riquelme, P.P. Paricio; Intestinal perforation by foreign bodies; Eur J Surg, 166 (2000), pp. 307–309
- [2] R. Zissin, A. Osadchy, G. Gayer; Abdominal CT findings in small bowel perforation; Br J Radio, 82 (2009), pp. 162–171
- [3] B.K.P. Goh, Y.M. Tan, S.E. Lin, P.K.H. Chow, F.K. Cheah, L.P.J. Ooi, et al.; CT in the preoperative diagnosis of fish bone perforation of the gastrointestinal tract; AJR Am J Roentgenol, 187 (2006), pp. 710–714
- [4] J. Hines, J. Rosenblat, D.R. Duncan, B. Friedman, D.S. Katz; Perforation of the mesenteric small bowel: Etiologies and CT findings; Emerg Radiol, 20 (2013), pp. 155–161
- [5] R. Cianci, V. Bianco, G. Esposito, A.D. Pizzi, A. Filippone; MDCT imaging of gastrointestinal tract perforation due to foreign body ingestion; R. Luigia, P. Antonio (Eds.), Imaging of alimentary tract perforation, Springer International Publishing, Switzerland (2015), pp. 79–84
- [6] W.K. Chau, J.Y. Wang, S.S.M. Wu; Ultrasonic detection of an intraabdominal foreign body; J Clin Ultrasound, 13 (1985), pp. 130–131
Document information
Published on 15/05/17
Submitted on 15/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?