Abstract
Objective
The aim of this study was to introduce the results of a novel mini-invasive operative technique comprising mini-incision release, “pie-crusting” lengthening of the quadriceps extensor, and arthroscopic lysis in severe arthrofibrotic knees.
Methods
From 2010 to 2014, 17 patients (12 males and 5 females with a mean age of 44 years (range, 19–62 years)) with severely arthrofibrotic knees were treated with this operative technique. The mean follow-up duration was 23 months. The knee range of motion (ROM) was assessed with a goniometer. The functional outcomes were evaluated according to the Hospital for Special Surgery (HSS) score and Judets criteria.
Results
The ROM significantly improved from 29.7° (range, 7°–56°) preoperatively to 127° (range, 120°–136°) at the final follow-up in all patients (p < 0.001). According to Judets criteria, all patients achieved excellent results (ROM > 100°). The HSS score was improved from 70 points (range, 60–85 points) preoperatively to 91 points (range, 84–98 points) (p < 0.001) at the final follow-up. No extension lag, skin necrosis, quadriceps weakness, wound dehiscence or quadriceps tendon rupture occurred.
Conclusions
Mini-invasive quadricepsplasty-associated arthroscopic lysis and manipulation of the knee in flexion is simple and easy and should be considered as a legitimate treatment for arthrofibrosis of the knee.
Keywords
Arthrofibrosis of the knee ; Quadricepsplasty ; Mini-invasive ; Pie-crusting
Introduction
Arthrofibrosis of the knee is a common complication, usually caused by trauma or surgery, that results in the loss of knee motion. Severely arthrofibrotic knee may result in significant functional impairment. Despite it has been reported widely, the treatment of a severely arthrofibrotic knee represents a dilemma faced by orthopedic surgeons. Many methods have been introduced to treat arthrofibrotic knees, including two classical procedures, Thompson quadricepsplasty and Judet quadricepsplasty, and their modifications.1 ; 2 ; 3 ; 4 ; 5 These traditional procedures require extensive exposure and have a high rate of associated complications, such as extension lag, skin necrosis, recurrent adhesion, and wound dehiscence.1 ; 6 ; 7 ; 8 ; 9 ; 10 Additionally, although a number of new treatment techniques exist, their outcomes remain suboptimal.11 ; 12 ; 13 Thus, there is no consensus regarding the ideal treatment strategy has been reached. The purpose of this study was to introduce a mini-invasive operative technique and to report the treatment outcomes of 17 consecutively treated severely arthrofibrotic knees.
Patients and methods
The present retrospective study comprised 17 knees in 17 patients who were admitted to the Central Hospital of Lishui City and Dous Traumatology Hospital of Jinyun County, Zhejiang Province, China between Nov 2010 and May 2014 with postoperative arthrofibrosis of the knee resulting from femoral and periarticular knee fractures and anterior cruciate ligament injury. The study was approved by the research committee of our institute. The study group comprised 12 males and 5 females with a mean age of 44 years (range, 19–62 years) (Table 1 ). Causative factors for arthrofibrosis included a mid-shaft femoral fracture in 4 patients, a distal femoral fracture in 7 patients, a tibial plateau fracture in 2 patients, a femoral shaft fracture associated with an ipsilateral patellar fracture in 1 patient, a tibial eminence anterior cruciate ligament avulsion fracture in 2 patients, and a patellar fracture in 1 patient (Table 1 ). All patients received early surgery after trauma. All patients failed a controlled nonoperative regimen of physical therapy, which lasted for a period of 1–5 months, and manipulation under anesthesia. Patients with any of the following were excluded from the study: distal femoral deformity, patellar fusion to the anterior aspect of the femur, weakness of the quadriceps muscles secondary to neurological deficit, and interruption of the knee extensor mechanism. The criteria of Judet were used to access clinical outcomes.
| Case | Gender | Age (yr) | Initial diagnosis | Treatment | ROM (deg) | HSS (points) | |||
|---|---|---|---|---|---|---|---|---|---|
| Preo | Immediately | Final | Preo | Final | |||||
| 1 | M | 44 | Distal femoral fracture | Open reduction and internal fixation, plate | 2–28 | 0–120 | 0–125 | 66 | 89 |
| 2 | M | 55 | Anterior cruciate ligament avulsion fracture from tibia | Open reduction and internal fixation, cerclage wire | 0–42 | 0–127 | 0–130 | 72 | 90 |
| 3 | M | 61 | Patella fracture | 7–26 | 2–131 | 2–123 | 65 | 85 | |
| 4 | M | 46 | Tibial plateau fracture | Open reduction and internal fixation, plate | 0–50 | 0–124 | 0–127 | 80 | 93 |
| 5 | M | 62 | Mid-shaft femoral fracture | Open reduction and internal fixation, plate | 0–18 | 0–130 | 0–132 | 62 | 95 |
| 6 | M | 37 | Distal femoral fracture | Open reduction and internal fixation, plate | 9–34 | 4–121 | 3–124 | 71 | 88 |
| 7 | M | 52 | Distal femoral fracture | Open reduction and internal fixation, plate | 0–20 | 0–132 | 0–130 | 84 | 94 |
| 8 | M | 41 | Tibial plateau fracture | Open reduction and internal fixation, plate | 0–10 | 0–124 | 0–120 | 63 | 90 |
| 9 | M | 53 | Distal femoral fracture | Open reduction and internal fixation, plate | 0–12 | 0–127 | 0–123 | 64 | 93 |
| 10 | M | 24 | Mid-shaft femoral fracture | Open reduction and internal fixation, plate | 3–29 | 0–125 | 0–129 | 77 | 98 |
| 11 | M | 45 | Femoral shaft fracture associated with an ipsilateral patellar fracture | Open reduction and internal fixation, plate and cerclage wire | 5–30 | 0–130 | 0–129 | 68 | 87 |
| 12 | M | 46 | Mid-shaft femoral fracture | Open reduction and internal fixation, plate | 4–49 | 0–126 | 0–125 | 82 | 96 |
| 13 | F | 44 | Distal femoral fracture | Open reduction and internal fixation, plate | 6–38 | 1–121 | 0–124 | 61 | 94 |
| 14 | F | 19 | Anterior cruciate ligament avulsion fracture from tibia | Open reduction and internal fixation, cerclage wire | 0–21 | 0–121 | 0–130 | 62 | 90 |
| 15 | F | 43 | Distal femoral fracture | Open reduction and internal fixation, plate | 2–9 | 0–120 | 0–128 | 60 | 84 |
| 16 | F | 38 | Mid-shaft femoral fracture | Open reduction and internal fixation, plate | 0–56 | 0–131 | 0–136 | 85 | 92 |
| 17 | F | 37 | Distal femoral fracture | Open reduction and internal fixation, plate | 15–33 | 2–127 | 2–124 | 77 | 95 |
Preo – preoperatively; Immediately – immediate postoperatively; Final – the final follow-up.
Surgical technique
The surgical procedure is sequential and comprises three states: mini-incision release, “pie-crusting” lengthening of the quadriceps extensor, and arthroscopic lysis of the arthrofibrotic knee, and manipulation of the knee in flexion after each state. The operative procedure is performed under epidural or general anesthesia, with the patient in a supine position. Tourniquet use is optional; a tourniquet is placed proximally around the thigh but is not inflated in the first two stages unless troublesome bleeding occurs.
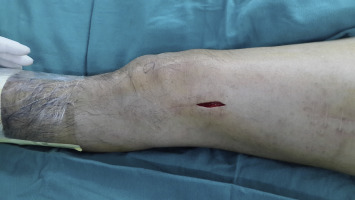
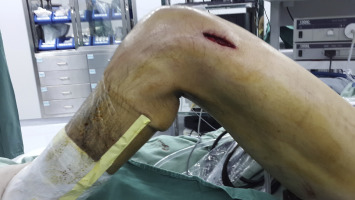
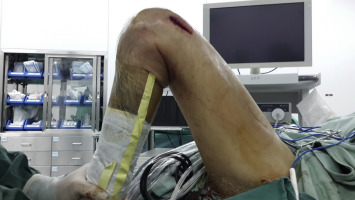
As previously described by Wang et al,11 ; 12 ; 13 the first stage, mini-incision release, consists of releasing the quadriceps extensor, suprapatellar pouch, lateral patellar retinaculum, patellofemoral joint space, and the vastus medialis expansion. A 5-cm longitudinal anterolateral skin incision is made starting from the superolateral corner of the patella and extending 5 cm proximally (Fig. 1 skin incision). After the quadriceps extensor and the suprapatellar pouch released from the femur using a periosteal elevator, a blunt curved dissection scissor is used to incise the lateral patellar retinaculum along the lateral border of the patella and patellar tendon percutaneously, and to separate the adhesions within the patellofemoral joint space, and to incise the medial and lower part of the vastus medialis expansion using an inside-out technique. At this time, the first stage is completed, and the maximum flexion of the knee is examined by gentle manipulation and remains unsatisfactory due to quadriceps extensor contracture (Fig. 2 ROM before pie-crusting). The skin incisions are bilaterally retracted with right-angled retractors, and the rectus femoris and vastus intermedius adhesive tendons are appropriately exposed with the knee extended, requiring further management.
|
|
|
Fig. 1. Skin incision. |
|
|
|
Fig. 2. ROM before pie-crusting. |
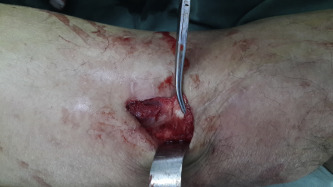
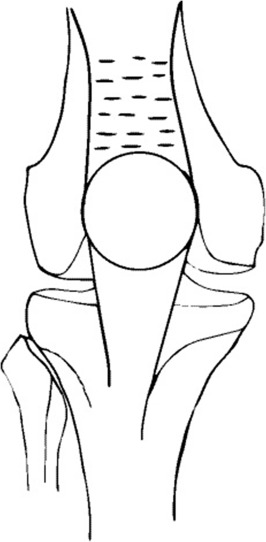
The second stage involves “pie-crusting” lengthening of the quadriceps extensor. Pie-crusting of the tendons is performed by poking an 11-blade scalpel straight through the tendons, distally to proximally (Fig. 3 pie-crusting). The cuts begin at the patellar insertion of the tendons, the length of the cuts and the interval between two cuts are approximately 6 mm and 5 mm respectively. Several staggered rows of cuts are made depending on the contracture severity, and the longitudinal fibers of the bilateral tendon edges are not cut to prevent tendon tears (Fig. 4 schematic diagram of pie-crusting). Manipulation of the knee in flexion is periodically attempted throughout the pie-crusting procedure to assess the arc of knee flexion, and the quadriceps extensor is gradually lengthened. Pie-crusting is considered complete once the flexion is 120° (Fig. 5 ROM after pie-crusting), and the skin is closed without closure of the fascia or muscle.
|
|
|
Fig. 3. Pie-crusting, make several staggered rows of cuts in the tendon. |
|
|
|
Fig. 4. Schematic diagram of pie-crusting: the cuts begin at the patellar insertion of the tendons, and the interval between two cuts is approximately 5 mm. |
|
|
|
Fig. 5. ROM after pie-crusting. |
The third stage comprises arthroscopic lysis of the arthrofibrotic knee. After inflating the tourniquet, standard anterolateral and anteromedial portals are established. A blunt trocar is easily passed into the previously restored suprapatellar pouch. The arthroscope is inserted, and the joint is routinely inspected. Any adhesions of the suprapatellar pouch, medial and lateral gutters, intercondylar area, intercondylar notch, and anterior interval are debrided. Gentle manipulation is performed in flexion after adhesion lysis; the arc of knee flexion should reach more than 120°.
A suction drain is inserted to prevent hemarthrosis, and a bulk compressive dressing is applied using an elastic bandage wrapping from foot to thigh.
Postoperative protocol
Edema is controlled by cryotherapy using icepacks. Oral and intravenous analgesics are used for postoperative pain control. Aggressive physical therapy, comprising active-assisted knee flexion exercises, continuous passive motion, resistive quadriceps exercises, and isometric quadriceps exercises, is initiated on the first postoperative day and is continued throughout the hospital stay, and is performed 3 times a day to achieve the maximum ROM. Full weight-bearing exercise is encouraged after surgery. The postoperative hospital stay is less than 10 days. Outpatient physical therapy carried out every week, is continued after discharge for 6 weeks. Active-assisted knee flexion exercises and full weight-bearing exercise are emphasized in this stage.
Statistical analysis
Pre-operative, immediate postoperative and final follow-up knee flexion and HSS knee scores were compared using a paired t test. P values < 0.05 were considered statistically significant. The SPSS software package (SPSS for windows, Release 13.0; SPSS, Chicago, Illinois) was used for the statistical analysis.
Results
This study included 17 knees in 17 patients. All patients were followed up for 8–50 months, with an average of 23 months.
Motion
The knee ROM was assessed with a goniometer. The degree of knee flexion increased from 32.8° (range, 10°–56°) preoperatively to 126.2° (range, 120°–133°) immediately postoperatively (p < 0.001), followed by a slight increase to an average of 127.4° (range, 120°–136°) (p < 0.001) in the follow-up period. Moreover, the extension loss was improved from 3.1° (range, 0°–15°) preoperatively to 0.4° (range, 0°–3°) at the final follow-up. The ROM significantly improved in all patients from 29.7° (range, 7°–56°) preoperatively to 127° (range, 120°–136°) (p < 0.001) at the final follow-up, as demonstrated in Table 1 . The preoperative and at the last follow-up ROM (Fig. 6 ROM at the final follow-up) of the patient presented in the figures were 0°–18° and 0°–132°.
|
|
|
Fig. 6. ROM at the final follow-up. |
Functional outcomes
Functional outcomes were evaluated according to the HSS score and Judets criteria. Preoperatively, the HSS score was low, at 70 points (range, 60–85 points); at the last follow-up, the score had significantly improved to 91 points (range, 84–98 points) (p < 0.001) ( Table 1 ). According to Judets criteria, all patients achieved excellent results (ROM > 100°). Quadriceps muscle power was graded as 5/5 in all patients.
Complications
None of the patients showed extension lag immediately after surgery or at the last follow-up, and none suffered from skin necrosis, quadriceps weakness, wound dehiscence or quadriceps tendon rupture.
Discussion
Arthrofibrosis of the knee is a devastating consequence of periarticular knee fractures, trauma and surgery that results in the loss of knee motion, which impedes normal walking, sitting and stair climbing and causes a noticeable and intolerable limp.14 The mechanisms of motion loss include vastus intermedius fibrosis, suprapatellar adhesions, patellar-femoral adhesions, and rectus femoris shortening, as well as fibrosis and shortening of the aponeurotic expansions of the vastus medialis and vastus lateralis and their adherence to femoral condyles.1
A number of surgical strategies to treat arthrofibrosis of the knee have been introduced, ranging from traditional quadricepsplasty, represented by the Thompson quadricepsplasty, the Judet quadricepsplasty and their modifications, to arthroscopic arthrolysis, arthroscopically assisted percutaneous quadricepsplasty, mini-invasive quadricepsplasty associated with arthroscopic release, as well as some new techniques.1 ; 2 ; 4 ; 11 ; 12 ; 13 ; 15 ; 16 ; 17 However, no consensus regarding the ideal treatment strategy has been reached.
Traditional quadricepsplasty is associated with increased surgical injury and serious complications, such as skin necrosis, wound dehiscence, postoperative extremity edema, severe pain, and extension lag caused by disruption of the knee extensor mechanism.4 ; 10 ; 15 Arthroscopic arthrolysis, even aided by percutaneous quadricepsplasty, fails to lengthen the knee extensor and to achieve sufficient ROM.16 ; 18 ; 19 ; 20 Mini-invasive quadricepsplasty associated with arthroscopic release has been reported by Wang et al (2006) and Liu et al (2011).11 ; 12 Wangs quadricepsplasty strategy integrally transects the quadriceps tendon to lengthen the quadriceps tendon and constrains early rehabilitation exercise, resulting in extension lag. Lius procedure produces a long range (approximately 9–15 cm) of transections, mini-tears and sliding of the quadriceps extensor in coronal plane; this procedure results in no extension lag, but its ROM < 125° is considered to be inadequate for completing daily living activities and for squatting.14 Recently, Wen et al introduced their percutaneous quadriceps tendon pie-crusting technique.17 But it requires a large parapatellar medial incision and is performed by making serried punctures on the quadriceps tendon, resulting in an early decrease in quadriceps strength due to quadriceps muscle injury but not in extension lag. Hence, various problems continue to limit the present techniques. The functional results and some complications of the traditional and arthroscopy assisted techniques are showed in Table 2 . Compare to them, our technique show better results.
| Technique | Functional results (Judets criteria) | Complications | |||||
|---|---|---|---|---|---|---|---|
| Excellent | Good | Fair | Poor | Extension lag | Skin necrosis | Rupture of the quadriceps tendon | |
| Thompson | 22.5% | 67.5% | 5% | 5% | ✓ | ✓ | ✓ |
| Judet | 38.10% | 42.86% | 19.05% | ✓ | ✓ | ✓ | |
| Wang | 72.73% | 22.73% | 4.54% | ✓ | |||
| Liu | 85.71% | 14.29% | |||||
Judets criteria for the surgical results is as follows: excellent: ROM > 100°; good: ROM, 80°–100°; Fair: ROM, 50°–80°; and poor: ROM < 50°.
According to the aforementioned protocols developed by previous authors, proper quadricepsplasty is essential to obtain adequate ROM, mini-invasive quadricepsplasty is effective to lengthen the knee extensor, and disastrous postoperative extension lag may ensue from excessive disruption of the knee extensor mechanism. Thus, to achieve appropriate ROM improvement and to prevent extension lag, the quadricepsplasty procedure requires not only less invasion but also minimal disturbance of the knee extensor mechanism. Furthermore, in addition to a successful operation, an aggressive rehabilitation regimen is indispensable to achieve a satisfactory outcome.
The pie-crusting tendon lengthening technique has been successfully used to release tight lateral structures in valgus knees during total knee arthroplasty. Recently, Burge et al (2014) first reported their success in using the pie-crusting technique in a patient with longstanding limited flexion who underwent primary total knee arthroplasty.21 According to the authors, the pie-crusting technique was used without complications in approximately 20 operative procedures, predominantly in revision total knee arthroplasty with arthrofibrosis, and was recommended for treating flexion limitations due to a tight extensor mechanism. Our pie-crusting technique in lengthening of the quadriceps extensor is safe and effective. There was no quadriceps tendon rupture.
To the best of our knowledge, our strategy for treating arthrofibrosis of the knee has not been demonstrated in the literature. In our study, the technique of mini-invasive quadricepsplasty associated with arthroscopic lysis showed satisfactory outcomes, benefiting from the effective lengthening of the fibrotic knee extensor mechanism, with some advantages over the aforementioned protocols.
There are three advantages of our pie-crusting technique of lengthening the quadriceps extensor. The first advantage is maintaining the continuity of the quadriceps extensor that allows aggressive rehabilitation exercise and plays an important role in preventing extension lag. The second advantage is the appropriate lengthening of the quadriceps extensor. During the pie-crusting, the number of staggered rows of cuts is depending on the arc of knee flexion. Once the proper arc of knee flexion is achieved, the pie-crusting ceases. The whole process is controllable and simple, and can prevent excessive lengthening of the quadriceps extensor, which may result in extension lag. The third advantage is high elongation of the quadriceps extensor. When the knee is manipulated in flexion, the cuts are opened like the shape of rhombus. The small interior angle of the rhombus is approximately 40°. According to the arccosine function, the length of the long diagonal of the rhombus is approximately 5.6 mm. Thus, one row of cuts can increase the length of the quadriceps extensor to approximately 5.6 mm, six rows increase approximately 33 mm, and eight rows increase approximately 44 mm.
Based on these advantages, we suppose that the effective elongation reconstructs the mechanical properties of the quadriceps extensor and makes an extensive ROM, the continuity ensures the safety of the quadriceps extensor under the strong tensile stress during the aggressive rehabilitation exercise, and our pie-crusting technique can effectively reconstruct the mechanical properties of the quadriceps extensor without significantly diminishing its mechanical strength. We believe that the immediately postoperatively extensive ROM with the early aggressive rehabilitation exercise is why our results are relatively superior to the others.
In the present series, no incision complications, such as skin necrosis and wound dehiscence (a benefit of the mini-incision), and no extension lag were observed. 7 patients have a decreased ROM in the final follow-up compared with the ROM immediately postoperatively. Thats just because the measurement of the ROM immediately postoperatively is under anesthesia with the muscles relaxed. The aggressive rehabilitation after surgery can be help to minimize loss of the ROM in the final follow-up. We believe that our technique of mini-invasive quadricepsplasty associated arthroscopic lysis is simple and easy and should thus be considered as a legitimate treatment for arthrofibrosis of the knee.
The major limitation in our study is that we excluded patients with distal femoral deformity, patellar fusion to the anterior aspect of the femur, quadriceps muscle weakness secondary to neurological deficit, or knee extensor mechanism interruption. The applicability of our strategy to these patients requires further study.
Conflicts of interest and source of funding
The authors declare no conflicts of interest and source of funding.
References
- 1 T.C. Thompson; Quadricepsplasty; Ann Surg, 121 (1945), pp. 751–754
- 2 J. Judet, R. Judet, J. Lagrange; Technic of liberation of the extensor apparatus in knee stiffness; Mem Acad Chir (Paris), 82 (1956), pp. 944–947
- 3 V.G. Oliveira, L.F. D'Elia, L.E. Tirico, et al.; Judet quadricepsplasty in the treatment of posttraumatic knee rigidity: long-term outcomes of 45 cases; J Trauma (2011) http://dx.doi.org/10.1097/TA.0b013e3182159e0a
- 4 M.H. Ebrahimzadeh, A. Birjandi-Nejad, S. Ghorbani, M.R. Khorasani; A modified Thompson quadricepsplasty for extension contracture resulting from femoral and periarticular knee fractures; J Trauma, 68 (2010), pp. 1471–1475 http://dx.doi.org/10.1097/TA.0b013e3181bdcdec
- 5 V.G. Oliveira, L.F. D'Elia, L.E. Tirico, et al.; Judet quadricepsplasty in the treatment of posttraumatic knee rigidity: long-term outcomes of 45 cases; J Trauma Acute Care Surg, 72 (2012), pp. E77–E80
- 6 E.A. Nicoll; Quadricepsplasty; J Bone Jt Surg Br, 45 (1963), pp. 483–490
- 7 N.A. Ebraheim, R.J. DeTroye, S.R. Saddemi; Results of judet quadricepsplasty; J Orthop Trauma, 7 (1993), pp. 327–330
- 8 J. Bellemans, A. Steenwerckx, K. Brabants, J. Victor, J. Lammens, G. Fabry; The Judet quadricepsplasty: a retrospective analysis of 16 cases; Acta Orthop Belg, 62 (1996), pp. 79–82
- 9 S.B. Hahn, W.S. Lee, D.Y. Han; A modified Thompson quadricepsplasty for the stiff knee; J Bone Jt Surg Br, 82 (2000), pp. 992–995
- 10 A.M. Ali, J. Villafuerte, M. Hashmi, M. Saleh; Judets quadricepsplasty, surgical technique, and results in limb reconstruction; Clin Orthop Relat Res, 415 (2003), pp. 214–220 http://dx.doi.org/10.1097/01.blo.0000093913.26658.9b
- 11 J.H. Wang, J.Z. Zhao, Y.H. He; A new treatment strategy for severe arthrofibrosis of the knee. A review of twenty-two cases; J Bone Jt Surg Am, 88 (2006), pp. 1245–1250 http://dx.doi.org/10.2106/JBJS.E.00646
- 12 K.M. Liu, S. Liu, Z. Cui, X. Han, T. Tang, A. Wang; A less invasive procedure for posttraumatic knee stiffness; Arch Orthop Trauma Surg, 131 (2011), pp. 797–802 http://dx.doi.org/10.1007/s00402-010-1223-z
- 13 H.O. Mayr, A. Stohr; Arthroscopic treatment of arthrofibrosis after ACL reconstruction. Local and generalized arthrofibrosis; Oper Orthop Traumatol, 26 (2014), pp. 7–18 http://dx.doi.org/10.1007/s00064-013-0264-1
- 14 D. Magit, A. Wolff, K. Sutton, M.J. Medvecky; Arthrofibrosis of the knee; J Am Acad Orthop Surg, 15 (2007), pp. 682–694
- 15 D.H. Lee, T.H. Kim, S.J. Jung, E.J. Cha, S.I. Bin; Modified judet quadricepsplasty and Ilizarov frame application for stiff knee after femur fractures; J Orthop Trauma, 24 (2010), pp. 709–715 http://dx.doi.org/10.1097/BOT.0b013e3181c80bb9
- 16 R. Steinfeld, M.E. Torchia; Arthroscopically assisted percutaneous quadricepsplasty: a case report and description of a new technique; Arthroscopy, 14 (1998), pp. 212–214
- 17 H.X. Liu, H. Wen, Y.Z. Hu, H.C. Yu, X.Y. Pan; Percutaneous quadriceps tendon pie-crusting release of extension contracture of the knee; Orthop Traumatol Surg Res, 100 (2014), pp. 333–335 http://dx.doi.org/10.1016/j.otsr.2013.12.023
- 18 N.R. Sprague, R.L. O'Connor, J.M. Fox; Arthroscopic treatment of postoperative knee fibroarthrosis; Clin Orthop Relat Res, 166 (1982), pp. 165–172
- 19 M.S. Dhillon, A.K. Panday, S. Aggarwal, O.N. Nagi; Extra articular arthroscopic release in post-traumatic stiff knees: a prospective study of endoscopic quadriceps and patellar release; Acta Orthop Belg, 71 (2005), pp. 197–203
- 20 C.E. Blanco, H.O. Leon, T.B. Guthrie; Endoscopic quadricepsplasty: a new surgical technique; Arthroscopy, 17 (2001), pp. 504–509 http://dx.doi.org/10.1053/jars.2001.24062
- 21 J.R. Burge, H.B. Sanchez, R.A. Wagner; Quadriceps and patellar tendon pie-crusting as a treatment for limited flexion in total knee arthroplasty; Am J Orthop (Belle Mead NJ), 43 (2014), pp. E83–E88
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?