Keywords
Pulmonary vein thrombus;64-MDCT;Completely occluding small thrombus;Warfarin
1. Introduction
Stroke is an increasing health problem throughout the world in the elderly populations and has become one of the major causes of mortality. The onset of ischemic stroke is sudden and can result in either temporary or permanent brain damage. Additionally, stroke is an important contributor to dementia and age-related cognitive decline and is frequently associated with permanent disability and impaired quality of life [1]. Although conventional risk factors such as hypertension account for a significant proportion of stroke risk, the influence of many other factors remains unclear [2].
Stroke risk modification and stroke prevention are major focal points in health care. Primary and secondary stroke prevention strategies differ according to stroke subtype; however, there is no direct method to evaluate the efficiency of anticoagulants. In 2015, Marcucci R. asked whether we can estimate the resistance of antiplatelet drugs [3], to which I responded that a 64-slice multidetector computed tomography (64-MDCT) may estimate the resistance of antiplatelet drugs by means of estimating the size of a pulmonary vein thrombus in elderly patients with chest pain [4].
Pulmonary vein thromboses are thought to be rare. Pulmonary vein thromboses that cause a transient ischemic attack (TIA) or stroke have only been reported in association with underlying lung neoplasia [5], previous pulmonary transplant or lobectomy [6] and pulmonary arteriovenous malformations or fistulae [7].
Since 2012, I have published several cases of pulmonary vein thromboses in elderly patients without these conditions, such as lung cancer and lung surgery, using 64-MDCT, which can evaluate coronary artery stenosis and the pulmonary vein thrombi (8,9) simultaneously. It was reported that a small pulmonary vein thrombus might originate from a larger pulmonary vein thrombus [8]. Recently, I reported that nearly all left atrial thrombi are alleged to arise from a pulmonary vein thrombus [9].
Warfarin, the predominant anticoagulant in clinical use, has been shown to reduce AF-related stroke by 64% in a large meta-analysis [10]. Although I reported that warfarin and dabigatran dissolved a large pulmonary vein thrombus that was not completely occluded, it is unclear whether warfarin and dabigatran could dissolve a small thrombus that completely occluded the pulmonary vein. However, the direct effects of warfarin therapy on a completely occluded small thrombus in a small pulmonary vein have not been thoroughly characterized.
2. Case reports
2.1. Case 1
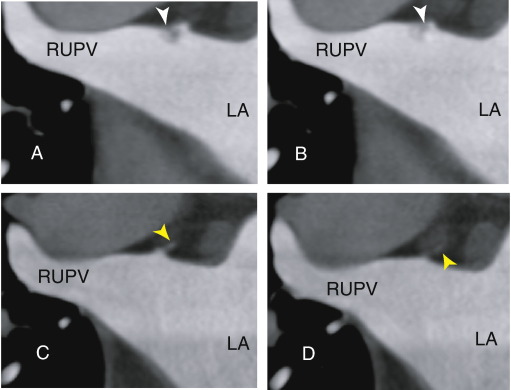
A 77-year-old male with a lacuna infarction in the pons was referred to our hospital to evaluate a source of cerebral infarction. He had no atrial fibrillation (AF). He was treated with aspirin (82 mg once daily), and no previous treatment with warfarin or NOACs had been implemented. A 64-MDCT scan showed a 3 to 4 mm thrombus at the proximal side of the right upper pulmonary vein (Fig. 1A and B; axial). After 2 months of warfarin therapy, the thrombus disappeared (Fig. 1C and D; axial). Concurrently, a fine vessel could be identified at the base of the eliminated thrombus, indicating that warfarin dissolved a completely occluded thrombus.
|
|
|
Fig. 1. (A, B) Axial images showing a thrombus (3 to 4 mm) within the right upper pulmonary vein (arrowhead) before warfarin therapy. (C, D) Axial images showing the distinguished thrombus within the right upper pulmonary vein after 2 months of warfarin therapy. Simultaneously, a small vessel appeared at the base of the eliminated thrombus (yellow arrowhead). RUPV: right upper pulmonary vein, LA: left atrium. |
2.2. Case 2
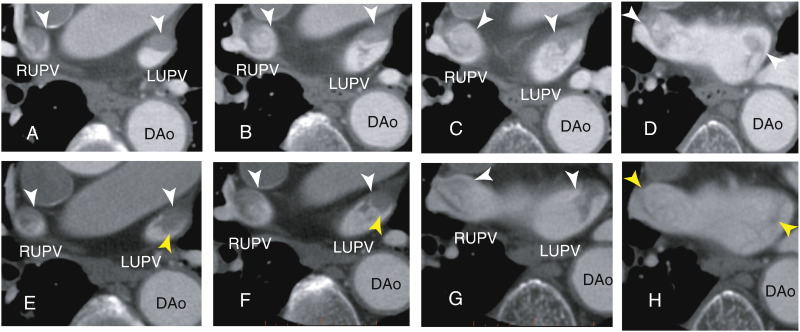
A 74-year-old male with AF was referred to our hospital for the evaluation of an LAA thrombus. No previous treatment with warfarin had been performed because the patient rejected the therapy. The patient had no symptoms of lung cancer or cerebral infarction. The chest roentgenogram showed no lung cancer. Large thrombi were detected in the right upper pulmonary vein, the left upper pulmonary vein and the left atrium (LA), as shown in axial (Fig. 1A to D) images as the defect of an enhancement by a 64-MDCT scan. The merge of a thrombus was sharp (Fig. 1A and B), and part of the thrombus could be observed in the LA (Fig. 1D). After 3 months of warfarin therapy, the size of the thrombi did not appear to change significantly; however, the shape of the thrombi appeared to change (Fig. 2E to G). In Fig. 2E and F, the sharp borderline became vague. In Fig. 2H, the size of the thrombi in LA appeared to be reduced, which is depicted as “lines.” During the warfarin therapy, the patient had no symptoms of systemic thrombosis such as cerebral infarction.
|
|
|
Fig. 2. Axial images showing thrombi within the right upper and the left upper pulmonary veins (white arrowheads). The right upper and the left upper pulmonary veins present with enlarged defects because of large thrombi (Fig. 2A). The left upper pulmonary vein demonstrated the sharp merge of enhancement (Fig. 2A and 2B), whereas the merge of the thrombi in left atrium was vague (Fig. 2C and 2D). After 3 months of warfarin therapy, the size of the thrombi did not change significantly, but the shape of the thrombi was altered (Fig. 2E to 2G). In Fig. 2E and Fig. 2F, the sharp borderline disappeared and became rather vague (yellow arrowhead). In Fig. 2H, the image size of thrombi in the LA decreased, which is shown as “lines” (yellow arrowheads). DAo: descending aorta, LUPV: left upper pulmonary vein, RUPV: right upper pulmonary vein. |
3. Discussion
In the first case, warfarin dissolved a small, completely occluded thrombus in the small pulmonary vein after 2 months of therapy. In the second case, warfarin did not significantly dissolve a large thrombus in the pulmonary vein by 3-month therapy; however, the thrombus in the left atrium decreased in size. Additionally, the shape of the thrombus changed slightly; prior to the warfarin treatment, the merge of the thrombus in the left upper pulmonary vein was sharp; after 3 months of warfarin therapy, the merge of the thrombus became vague, suggesting that warfarin gradually dissolved the thrombus. One reason why the thrombus in the left atrium dissolved might be the high volume of warfarin-treated blood flow. The use of 64-MDCT scans could assess the thrombus in the pulmonary vein and the left atrium. This is the first case study to demonstrate not only the dissolution of a small thrombus in the pulmonary vein, but the appearance of the small vessel after warfarin therapy at the original thrombus site, which might be the root of the dissolved thrombus. I have reported that nearly all of a left atrial thrombus was rooted from a pulmonary vein thrombus [8]. In another case, the round thrombus in the right upper pulmonary vein had a small thrombus in the small vessel, which connected to the thrombus as a root [9].
Although warfarin was unable to intercalate into the large thrombus, the treatment was successful in dissolving the merge of the large thrombus. However, when the thrombus is small, warfarin could dissolve the thrombus as shown in the first case, which was illustrated using 64-MDCT scans. It is thus important to recognize the capabilities of 64-MDCT scans in treating pulmonary vein thrombi.
When the pulmonary vein or a branch of the pulmonary vein is completely occluded by a thrombus, the blood flow decreases, which causes hypoxic, undernourished tissue as well as a reduced temperature. Hypoxia activates hypoxia inducible factors (HIFs), and malnourishment induces the expression of metal-regulatory transcription factor-1 (MTF-1) and nuclear respiratory factor-1 and -2 (NRF-1, -2). Low tissue temperature may modulate heat shock protein (HSP) expression by unknown mechanism(s). These transcription factors can cause epigenetic changes in associated cells. Abnormal function of HSP, which is caused by pulmonary vein thrombosis, may play roles in elderly patients with pulmonary diseases such as lung cancer, chronic obstructive pulmonary disease or atrial fibrillation (AF). According to this manuscript, warfarin dissolved the completely occluded thrombus in the fine pulmonary vein. I have reported that dabigatran was able to almost entirely dissolve a pulmonary vein thrombus. Although warfarin and dabigatran have been used clinically in patients with AF and have been shown to dissolve a pulmonary vein thrombus to some extent, there is little evidence that such treatment cured the AF, indicating that the recovery of arterial blood flow does not cure the induced epigenetic changes of the associated cells. More studies are required to obtain insight into novel therapies to cure AF after dissolving a completely occluded thrombus in the pulmonary vein.
Conflict of interest
The author report no relationships that could be construed as a conflict of interest.
References
- [1] A.D. Lopez, C.D. Mathers, M. Ezzati, D.T. Jamison, C.J. Murray; Global and regional burden of disease and risk factors, 2001: systematic analysis of population health data; Lancet, 367 (2006), pp. 1747–1757
- [2] R.L. Sacco, J.H. Ellenberg, J.P. Mohr, T.K. Tatemichi, D.B. Hier, T.R. Price, et al.; Infarcts of undetermined cause: the NINCDS Stroke Data Bank; Ann Neurol, 25 (1989), pp. 382–390
- [3] R. Marcucci; Resistance to antiplatelet drugs. Can it be assessed?; Int J Cardiol (2015) https://doi.org/10.1016/j.ijcme.2014.10.012
- [4] H. Takeuchi; 64-slice multidetector computed tomography may assess resistance of antiplatelet drugs; Int J Cardiol (2015) https://doi.org/10.1016/j.ijcme.2015.03.001
- [5] S. Schwalm, R.P. Ward, K.T. Spencer; Transient ischemic attack in a patient with pulmonary vein thrombosis after left upper lobectomy for squamous cell lung cancer; J Am Soc Echocardiogr, 17 (2004), pp. 487–488
- [6] M.P. Reilly, T.J. Plappert, S.E. Wiegers; Cerebrovascular emboli related to pulmonary venous thrombosis after lung transplantation; J Am Soc Echocardiogr, 11 (1998), pp. 299–302
- [7] R. Cohen, L. Cabanes, C. Burckel, D. Duboc, E. Touze; Pulmonary arteriovenous fistulae thrombosis responsible for recurrent stroke; J Neurol Neurosurg Psychiatry, 77 (2006), pp. 707–708
- [8] H. Takeuchi; Nearly all left atrial thrombi may be extended from pulmonary vein thrombi; IJC Heart Vasculature (2015) https://doi.org/10.1016/j.ijcha.2015.01.013
- [9] H. Takeuchi; A long and narrow pulmonary vein thrombus attached to the wall of pulmonary vein; IJC Heart Vasculature (2015) https://doi.org/10.1016/j.ijcha.2015.02.011
- [10] R.G. Hart, L.A. Pearce, M.I. Aguilar; Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation; Ann Intern Med, 146 (2007), pp. 857–867
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?