Dear Editor,
With an increase in health consciousness, the intake of food supplements such as multivitamins, multi-minerals, and herbal products has become widespread in the general population.1 However, little is known about the adverse effects of food supplement intake including supplement-induced pneumonia (SIP).2 and 3 We herein describe a case in which black garlic, a popular herbal food supplement, induced pneumonia.
Case report
A 77-year-old female was admitted to our hospital with dyspnoea and coughing in March 2014. She had hypertension and had been taking amlodipine for more than 10 years without any side effects. She had no history of smoking, allergies, or respiratory disorders. Around 3 weeks prior to hospitalization, she began taking black garlic. One week after first taking it, she started suffering from dyspnoea and coughing.
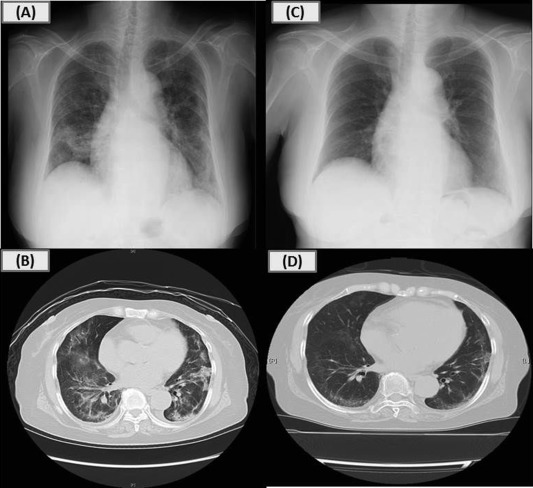
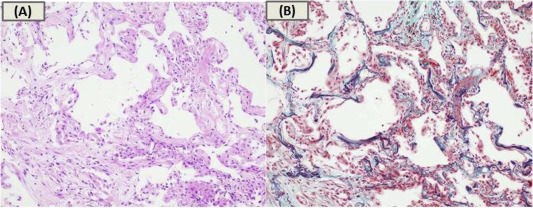
Her physical examination on admission showed bilateral fine crackles with oxygen saturation of 92% on room air, but no fever. Chest radiograph showed bilateral infiltrates (Fig. 1A). Chest CT scan revealed bilateral reticulo-nodular shadows with ground glass opacity (Fig. 1B). Respiratory function test showed moderate restriction with a vital capacity of 1.30 L (%predicted of 60.7%) and a forced expiratory volume in 1 s of 1.23 L (%predicted of 79.9%). Blood test results demonstrated elevated C-reactive protein of 6.69 mg/dL (normal range <0.3 mg/dL), sialylated carbohydrate antigen KL-6 of 585 U/mL (normal range <500 U/mL), and surfactant protein-D (SP-D) of 135 ng/mL (normal range <110 ng/mL). The patients white blood cell counts and proportion of eosinophils were normal. Autoimmune antibodies and specific IgE to garlic were negative. Meropenem and Azithromycin were administered for suspected atypical pneumonia, but were ineffective. Bronchoscopy was conducted in order to make a definite diagnosis. Bronchoalveolar lavage fluid analysis revealed an increased number of total cells and lymphocytes (total cell counts, 34.8 × 104/mlBALF; alveolar macrophages, 17.1%; lymphocytes, 76.1%; neutrophils, 5.0%; eosinophils, 1.8%; CD4/CD8 ratio, 1.3), whereas no malignant cells and microorganisms including fungi and Pneumocystis jirovecii were detected. Transbronchial lung biopsies showed organising exudates, alveolar wall thickening, and lymphocyte infiltrates without granulomas, suggesting organising pneumonia ( Fig. 2).
|
|
|
Fig. 1. Chest X-rays and CT scans on admission and after treatment. Chest radiograph on admission showing bilateral infiltrates predominantly in the middle and lower lung fields (A); Chest CT on admission showing bilateral reticulo-nodular shadows, thickening of bronchovascular bundles, and curvilinear shadow with ground glass opacity predominantly in the middle and lower lung lobes (B); Chest radiograph after 3 weeks of steroid treatment showed significant improvement (C, D). |
|
|
|
Fig. 2. Histological findings obtained from transbronchial biopsy. Histological findings obtained from transbronchial biopsy showed organising exudates, alveolar wall thickening, and lymphocyte infiltrates without granulomas and atypical lymphocytes (A: Haematoxylin-eosin stain, B: Elastica-masson stain). |
On the basis of her clinical, radiological, and pathological findings along with the recent intake of black garlic, we suspected black garlic-induced pneumonia. Therefore, a drug-induced lymphocyte stimulation test (DLST) for both black and raw garlic was performed. The results were positive with stimulation indices of 306% (black garlic) and 197% (raw garlic), which are 175% and 170% in a healthy subject, respectively (normal reaction <180%). Finally, the patient was diagnosed as having black garlic-induced pneumonia.
She was asked to stop taking black garlic and treated with 3 days of methylprednisolone (1 g/day) followed subsequently by oral prednisolone (40 mg/day) because of her aggravating respiratory condition. After the initiation of treatment, chest radiographs showed significant improvement (Fig. 1C,D). In terms of blood abnormalities, SP-D recovered to normal within 9 days while KL-6 showed a transient increase at day 18 and then returned to normal at day 36. She was instructed not to take any kinds of garlic and discharged. At the outpatient clinic, oral prednisolone was tapered and stopped over 9 months. No recurrence has been observed up to the present.
Discussion
To the best of our knowledge, this is the first report of black garlic-induced pneumonia. Black garlic is a type of caramelised garlic supplement made by heating whole bulbs of raw garlic in a pot under humid and unfermented conditions for one month (Maillard reaction). No food additives are used over the course of this process. Under this circumstance, it abounds in amino acid components such as s-allyl cysteine, which have strong antioxidant effects.4 This patient had been taking a clove of black garlic itself every day for 3 weeks for her health, and subsequently developed pneumonia.
Recently, many supplements such as multivitamins, multi-minerals, and herbal products are available with no serious side effects mentioned on the label.1, 2 and 3 Thus, it is difficult to doubt supplements could induce pneumonia. Additionally, the lack of peculiar tests makes it difficult to diagnose SIP. However, once SIP is suspected, the suspected causative agent must be immediately withdrawn in order not to develop life-threatening pulmonary infiltrate such as acute respiratory distress syndrome. A provocation test would be the best way to confirm a causative agent,5 but it may lead to critical condition and thus the application is limited.6 For this reason, DLST is frequently performed as a surrogate marker for adverse drug reaction.6 and 7
In this case, the positive DLST result subsequently to a history of taking black garlic provided a clue to diagnose black garlic induced-pneumonia. The mechanism of drug including supplements induced lung disorders has been recognized as either an immunological reaction or a cytotoxic effect.6 The positive DLST for black garlic could suggest a delayed type of immunoreaction rather than cytotoxic reaction.
Pathological finding in this case showed organising pneumonia pattern. Accordingly, SP-D and KL-6 as markers of interstitial lung diseases were high over the course of treatment. However, SP-D rather than KL-6 returned to normal quickly, which is similar to a previous report.8 This reaction could be explained by the shorter half-life and smaller molecular weight of SP-D. Thus, SP-D could be a sensitive marker for predicting the response to steroid treatment in SIP.
In conclusion, we described a first case of black garlic-induced pneumonia. DLST in addition to careful interviews may provide useful information on diagnosing SIP. Furthermore, SP-D rather than KL-6 could be a useful marker to monitor therapeutic effect in SIP. The accumulation of case-based reports sheds light on further understanding of SIP.
Conflict of interest
The authors have no conflict of interest to declare.
References
- 1 B.B. Timbo, M.P. Ross, P.V. McCarthy, C.T. Lin; Dietary supplements in a national survey: prevalence of use and reports of adverse events; J Am Diet Assoc, 106 (2006), pp. 1966–1974
- 2 K.E. Mar, P. Sen, K. Tan, R. Krishnan, K. Ratkalkar; Bronchiolitis obliterans organizing pneumonia associated with massive L-tryptophan ingestion; Chest, 104 (1993), pp. 1924–1926
- 3 R.S. Lai, A.A. Chiang, M.T. Wu, J.S. Wang, N.S. Lai, J.Y. Lu, et al.; Outbreak of bronchiolitis obliterans associated with consumption of Sauropus androgynus in Taiwan; Lancet, 348 (1996), pp. 83–85
- 4 Y.M. Lee, O.C. Gweon, Y.J. Seo, J. Im, M.J. Kang, M.J. Kim, et al.; Antioxidant effect of garlic and aged black garlic in animal model of type 2 diabetes mellitus; Nutr Res Pract, 3 (2009), pp. 156–161
- 5 Y. Suzuki, S. Miwa, M. Shirai, H. Ohba, M. Murakami, K. Fujita, et al.; Drug lymphocyte stimulation test in the diagnosis of adverse reactions to antituberculosis drugs; Chest, 134 (2008), pp. 1027–1032
- 6 O. Matsuno; Drug-induced interstitial lung disease: mechanisms and best diagnostic approaches; Respir Res, 13 (2012), p. 39
- 7 W.J. Pichler, J. Tilch; The lymphocyte transformation test in the diagnosis of drug hypersensitivity; Allergy, 59 (2004), pp. 809–820
- 8 H. Kitajima, H. Takahashi, K. Harada, A. Kanai, S. Inomata, H. Taniguchi, et al.; Gefitinib-induced interstitial lung disease showing improvement after cessation: disassociation of serum markers; Respirology, 11 (2006), pp. 217–220
Document information
Published on 05/04/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?