Abstract
Background
We retrospectively investigated our hypothesis that pre-percutaneous coronary intervention (PCI) procedural therapeutic hypothermia may have clinical advantages in patients with a profound cardiogenic shock complicating anterior ST-segment elevation myocardial infarction (STEMI).
Methods
Of 483 consecutive patients treated with PCI for a first anterior STEMI including 31 patients with aborted sudden cardiac arrest between 2009 and 2013, a total of 37 consecutive patients with an anterior STEMI complicated with profound cardiogenic shock defined as the presence of hyperlactic acidemia (serum levels of lactate > 4 mmol/L) with mechanical circulatory support were identified. An impaired myocardial tissue-level reperfusion (angiographic myocardial blush grade 0 or 1) and in-hospital mortality were evaluated in accordance with the presence or absence of pre-PCI procedural therapeutic hypothermia.
Results
Thirteen patients were treated with pre-PCI procedural therapeutic hypothermia and 24 were not inducted with therapeutic hypothermia. Five patients with and 18 without pre-PCI procedural therapeutic hypothermia impaired myocardial tissue-level reperfusion (38% vs. 75%, p = 0.037). A total of 26 patients with in-hospital death (overall in-hospital mortality 70%) were composed of 6 with and 20 without therapeutic hypothermia (in-hospital mortality 46% vs. 83%, p = 0.028). A multivariate analysis demonstrated a significant association of pre-PCI procedural therapeutic hypothermia (p = 0.021) with in-hospital survival benefit. Adverse events associated with therapeutic hypothermia were not found in 12 patients who completed this treatment.
Conclusions
The present study may imply a crucial possibility of clinical benefits of pre-PCI procedural therapeutic hypothermia in patients with a cardiogenic shock complicating anterior STEMI.
Keywords
Cardiogenic shock;Myocardial infarction;Therapeutic hypothermia;Revascularization;Reperfusion injury;In-hospital mortality
1. Introduction
A complication of cardiogenic shock remains a leading cause of death not showing any improvements in in-hospital mortality in patients with a ST-segment elevation myocardial infarction (STEMI) despite early prompt percutaneous coronary intervention (PCI) with mechanical circulatory support [1]; [2]; [3]; [4] ; [5]. The fatal clinical features of a cardiogenic shock complicating STEMI are mainly composed of systemic microcirculatory and cellular distress resulting in a development of multi-organ dysfunction syndromes [6]. Recently we demonstrated a possible role of exaggerated inflammation in the pathogenesis of excessive systemic as well as myocardial tissue-level mal-perfusion in those treated with PCI for a cardiogenic shock complicating STEMI [7].
Therapeutic hypothermia is widely available and has become an established standard of care for patients with post-cardiac arrest syndromes [8]. Feasibility of using therapeutic hypothermia in combination with emergency PCI in patients with STEMI with post-cardiac arrest syndromes had also been recognized [9]; [10] ; [11]. One of the main features to provide clinical benefits of therapeutic hypothermia has been proposed to limit a systemic ischemia–reperfusion injury mediated through attenuating widespread systemic inflammatory response in those with post-cardiac arrest syndromes [12] ; [13]. If so, the clinical advantages of therapeutic hypothermia may exist in those with a cardiogenic shock complicating STEMI who presented exaggerated inflammation.
In the present study, to address our hypothesis that therapeutic hypothermia preceding PCI may provide clinical benefits in patients with a cardiogenic shock complicating STEMI, we retrospectively analyzed clinical features of the 37 consecutive patients with a profound cardiogenic shock complicating STEMI.
2. Methods
2.1. Study patients (Fig. 1)
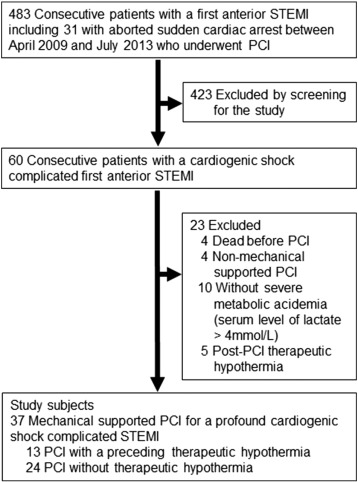
From a total of 483 consecutive patients treated with PCI for a first anterior STEMI including 31 patients with aborted sudden cardiac arrest between April 2009 and July 2013, 60 patients with cardiogenic shock including some with aborted sudden cardiac arrest were screened by the medical staff for inclusion in this study. The eligibility criteria were as follows; 1) clinical manifestations of profound cardiogenic shock on hospital admission or sustained more than 30 min after successful resuscitation, so called post-resuscitation shock [14], which revealed a systolic blood pressure of less than 90 mm Hg or a mean blood pressure less than 70 mm Hg despite high-dose inotrope infusion, clinical signs of respiratory distress with pulmonary congestion, impaired end-organ perfusion such as cool extremities, perspiration, prostration and so necessitates mechanical circulatory support such as intra-aortic balloon pumping and/or percutaneous cardio-pulmonary bypass with mechanical ventilation [15]. 2) A proof of severe abnormality in tissue oxygen metabolism defined by a presence of arterial blood levels of lactate over 4 mmol/L (i.e. severe metabolic acidemia) on hospital admission or 30 min after resuscitation [16]; [17] ; [18]. 3) Therapeutic hypothermia preceded PCI, if applied. According to these eligibility criteria, 23 patients were excluded because 4 were dead before PCI, 4 had unnecessary mechanical circulatory support, 10 had less severe metabolic acidemia, and 5 had post-PCI procedural therapeutic hypothermia. Finally 37 patients (28 men, 70 ± 13 years) with severe metabolic acidemia and that underwent PCI with mechanical circulatory support for a cardiogenic shock complicating first anterior STEMI were recruited in this study. Of those, 13 patients were treated with pre-PCI procedural therapeutic hypothermia and 24 were not inducted with therapeutic hypothermia. Our study patients were coincided with the recent recommendation of the cardioprotection study in STEMI such as anterior STEMI and pre-PCI procedural therapeutic intervention [19]. All patients or an immediate family member provided written, informed consent to attend our clinical investigation at the time of hospital admission. The study protocol was approved by our institutional review board.
|
|
|
Fig. 1. Flowchart of selection of study population. STEMI denotes ST-segment elevation myocardial infarction, PCI, percutaneous coronary intervention. |
2.2. Therapeutic hypothermia
Of the 13 patients treated with therapeutic hypothermia, 11 were resuscitated from ventricular fibrillation and/or pulseless ventricular tachycardia, and 2 were initiated with therapeutic hypothermia to protect brain damages from mal-perfusion due to a critical shock state at the discretion of the physician in charge. Of those with therapeutic hypothermia, 9 patients underwent endovascular cooling using a heat exchanger with the Capiox® percutaneous cardio-pulmonary bypass system (Termo Inc., Tokyo, Japan) and 4 underwent surface cooling using the Arctic Sun® temperature management system (Medivance Corp, Louisville, CO) in accordance with our protocol for treatment with therapeutic hypothermia. Briefly, all patients were sedated during the induction and maintained with therapeutic hypothermia with mechanical ventilation achieving arterial oxyhemoglobin saturation > 94% with a minimum concentration of FiO2 and monitored the core temperature using a pulmonary artery or urinary catheter with a temperature sensor in the usual manner. With the rapid infusion of ice-cold, isotonic, non-glucose-containing fluid (30 mL/kg), patients were rapidly cooled to 34 °C. After maintaining therapeutic hypothermia for 12–24 h, rewarming was started by 0.5 °C every 12 h to 36 °C under feedback from a continuous measurement of core temperature to the cooling devices.
2.3. PCI procedure
PCI with coronary stent deployment was performed with the conventional technique to eliminate occlusion or sub-occlusion of the left main and/or proximal left anterior descending coronary artery. Dual anti-platelet drug therapy with aspirin and either clopidogrel or ticlopidine but not glycoprotein IIb/IIIa inhibitors was initiated in all patients. Deployment of stent with pre-dilatation or directly and also use of an aspiration catheter to retrieve culprit coronary thrombus was up to the physician in charge. Because of refractory hemodynamic instability, an intra-aortic balloon counterpulsation and/or percutaneous cardio-pulmonary bypass were inducted before PCI in all the patients. The mean time from hospital arrival to PCI was 50 ± 48 min (median 33 min).
Pre- and post-procedural culprit epicardial coronary flow was evaluated by Thrombolysis in Myocardial Infarction (TIMI) flow grade from 0 to 3, with the highest grade indicating normal coronary reflow [20]. Myocardial tissue-level reperfusion was evaluated by angiographic myocardial blush grade from 0 to 3, with the highest grade indicating normal myocardial tissue-level reperfusion [21]. Impaired myocardial tissue-level reperfusion was defined by the presence of post-PCI procedural angiographic myocardial blush grade 0 or 1 under the mechanical and pharmacological circulatory supports.
2.4. Clinical assessments
The degree of myocardial tissue-level reperfusion and in-hospital mortality were evaluated to address whether there are any clinical benefits in those treated with pre-PCI procedural therapeutic hypothermia for a profound cardiogenic shock complicating anterior STEMI. The adverse effects of therapeutic hypothermia such as PCI related major bleeding, refractory infection, and electrolyte abnormality often related to dysrhythmias were also evaluated [8].
2.5. Statistical analysis
Continuous variables are presented as mean ± SD. To compare variables between patients with and without therapeutic hypothermia, p values were obtained by Students t-test or the Mann–Whitney test for continuous variables or the chi-square test for categorical variables. The 30-day in-hospital mortality was evaluated by the Kaplan–Meier analysis with the Log-rank and the Breslow–Gehan–Wilcoxon tests, in accordance with the presence or absence of pre-PCI procedural therapeutic hypothermia. The Cox proportional hazard model was used to assess an association of myocardial tissue-level reperfusion with all-cause in-hospital death. Logistic regression analysis was performed to identify variables that were independently associated with in-hospital survival. Statistical significance was set at p values of < 0.05.
3. Results
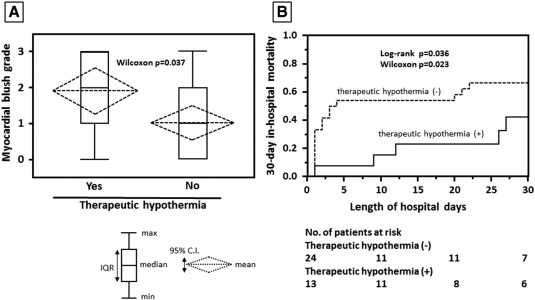
Demographic characteristics of the present study revealed a mean age of 70 ± 14 years, 65% male, 41% hypertension, and 49% diabetes mellitus. Time periods from hospital admission to PCI were 44 ± 39 min and mean length of hospital stay was 28 ± 35 days. Patients with and without therapeutic hypothermia showed no differences in vital signs and a severity of metabolic acidosis upon hospital admission (Table 1). Those with therapeutic hypothermia were mostly resuscitated with induction of therapeutic hypothermia before PCI, and so relatively spent time from hospital admission to PCI. All of the 13 patients with therapeutic hypothermia had achieved the target core temperature of 34 °C before PCI. The characteristics of coronary angiogram and PCI procedures were not different between those with and without therapeutic hypothermia except for the high prevalence of the use of percutaneous cardio-pulmonary bypass in those with therapeutic hypothermia. Despite a similar achievement of post-PCI procedural TIMI flow grade III, an incidence of angiographic myocardial blush grade 0 and/or 1 was significantly different between those with and without therapeutic hypothermia (Fig. 2A). A total of 26 patients were in-hospital dead, thereby overall in-hospital mortality was 70%. In detail, one patient with therapeutic hypothermia and 8 without hypothermia were dead within 24 h after hospital admission (8% vs. 33%, p = 0.063), and 6 patients with and 20 without therapeutic hypothermia were finally in-hospital dead (46% vs. 83%, p = 0.028). As shown in Fig. 2B, the 30-day in-hospital survival curve was significantly different in accordance with the presence or absence of pre-PCI procedural therapeutic hypothermia. In the Cox proportional hazard model, post-PCI procedural angiographic myocardial blush grade 0 or 1 was highly associated with in-hospital death (hazard ratio, 5.614; 95% confidence interval, 2.095–19.491, p = 0.003). The logistic multivariate analysis demonstrated pre-PCI procedural therapeutic hypothermia as a potent contributor to in-hospital survival benefits (Table 2). There were no adverse events related with therapeutic hypothermia in 12 patients who completed this treatment (Table 3).
| Pre-PCI procedural therapeutic hypothermia | p value | ||
|---|---|---|---|
| Yes (n = 13) | No (n = 24) | ||
| Age, year | 65 ± 12 | 69 ± 13 | 0.098 |
| Male sex, no (%) | 11 (85) | 13 (54) | 0.133 |
| Body mass index, kg/m2 | 24 ± 4 | 22 ± 3 | 0.110 |
| Systolic blood pressure, mm Hg | 88 ± 32 | 92 ± 18 | 0.679 |
| Diastolic blood pressure, mm Hg | 47 ± 18 | 49 ± 13 | 0.768 |
| Heart rate, beats/min | 95 ± 31 | 94 ± 28 | 0.969 |
| Shock index, beats/min/mm Hg | 1.22 ± 0.82 | 1.06 ± 0.39 | 0.540 |
| Creatine kinase-MB on admission, IU/L | 67 ± 153 | 60 ± 68 | 0.894 |
| Hypertension, no (%) | 6 (46) | 9 (38) | 0.865 |
| Dyslipidemia, no (%) | 3 (23) | 3 (13) | 0.705 |
| Current smoking, no (%) | 7 (54) | 6 (25) | 0.160 |
| Diabetes mellitus, no (%) | 3 (23) | 15 (63) | 0.051 |
| Arterial blood pH | 7.16 ± 0.19 | 7.24 ± 0.16 | 0.188 |
| PaO2, mm Hg | 198 ± 154 | 128 ± 92 | 0.154 |
| PaCO2, mm Hg | 48 ± 23 | 38 ± 15 | 0.202 |
| Arterial blood bicarbonate, mmol/L | 16.9 ± 3.1 | 16.5 ± 4.4 | 0.693 |
| Arterial blood lactate, mmol/L | 8.76 ± 4.33 | 7.17 ± 3.58 | 0.280 |
| Base excess, mmol/L | − 11.7 ± 3.6 | − 11.4 ± 5.6 | 0.813 |
| Arterial blood glucose, mg/dL | 291 ± 48 | 293 ± 116 | 0.946 |
| White blood cell counts, x103/μL | 13.1 ± 5.7 | 13.3 ± 4.4 | 0.896 |
| Hemoglobin, g/dL | 12.6 ± 2.4 | 12.3 ± 2.4 | 0.678 |
| Serum creatinine, mg/dL | 1.53 ± 1.35 | 1.53 ± 0.85 | 0.998 |
| Serum sodium, mmol/L | 138 ± 3 | 136 ± 5 | 0.394 |
| Serum potassium, mmol/L | 4.1 ± 0.8 | 4.3 ± 0.6 | 0.447 |
| Resuscitation before PCI, no (%) | 11 (85) | 12 (50) | 0.025 |
| Time from symptom onset to hospital admission, min | 22 ± 23 | 81 ± 77 | 0.002 |
| Time from hospital admission to induction of therapeutic hypothermia, min | 19 ± 8 | – | – |
| Time from hospital admission to target temperature, min | 83 ± 66 | – | – |
| Time from hospital admission to PCI, min | 85 ± 67 | 46 ± 21 | 0.060 |
| Left main trunk as the infarct-related coronary artery, no (%) | 6 (46) | 6 (25) | 0.189 |
| Multi-vessel coronary artery diseases, no (%) | 8 (62) | 17 (71) | 0.716 |
| Pre-PCI procedural TIMI flow grade 0, no (%) | 7 (54) | 20 (83) | 0.121 |
| Post-PCI procedural TIMI flow grade 3, no (%) | 9 (69) | 15 (63) | 0.953 |
| Thrombus aspiration, no (%) | 8 (62) | 12 (50) | 0.737 |
| Intra-aortic balloon counterpulsation, no (%) | 13 (100) | 24 (100) | 0.999 < |
| Percutaneous cardio-pulmonary bypass, no (%) | 9 (69) | 6 (25) | 0.022 |
Plus–minus values are mean ± SD. PCI denotes percutaneous coronary intervention, STEMI ST-segment elevation myocardial infarction, pH potential hydrogen, PaO2 partial pressure of oxygen, PaCO2 partial pressure of carbon dioxide and TIMI thrombolysis in myocardial infarction.
|
|
|
Fig. 2. A. Distribution of post-PCI procedural myocardial blush grade. IQR denotes interquartile range, C.I., confidence interval. B. The 30-day in-hospital mortality in the study population. |
| Variable | Standard error | Odds ratio | 95% confidence interval | p value |
|---|---|---|---|---|
| Time from symptom onset to hospital admission | 0.007 | 0.998 | 0.984–1.013 | 0.739 |
| Percutaneous cardio-pulmonary bypass | 0.602 | 0.157 | 0.007–1.208 | 0.079 |
| Pre-PCI therapeutic hypothermia | 0.642 | 19.397 | 2.144–471.541 | 0.006 |
PCI denotes percutaneous coronary intervention.
| Pre-PCI procedural therapeutic hypothermia | |||
|---|---|---|---|
| Baseline | 24 h later | p value | |
| Systolic blood pressure, mm Hg | 107 ± 24 | 115 ± 16 | 0.423 |
| Diastolic blood pressure, mm Hg | 60 ± 17 | 61 ± 8 | 0.915 |
| Heart rate, beats/min | 88 ± 28 | 84 ± 16 | 0.766 |
| Arterial blood pH | 7.09 ± 0.17 | 7.42 ± 0.12 | 0.001 |
| PaO2, mm Hg | 193 ± 137 | 158 ± 73 | 0.503 |
| PaCO2, mm Hg | 55 ± 22 | 41 ± 12 | 0.103 |
| Arterial blood bicarbonate, mmol/L | 17.7 ± 2.4 | 24.4 ± 1.4 | 0.001 |
| Arterial blood lactate, mmol/L | 9.12 ± 3.40 | 2.96 ± 1.50 | 0.001 |
| Base excess, mmol/L | − 12.0 ± 4.1 | 0.28 ± 2.42 | 0.001 |
| White blood cell counts, x103/μL | 13.6 ± 6.3 | 14.1 ± 6.1 | 0.858 |
| Serum creatinine, mg/dL | 1.61 ± 1.39 | 1.49 ± 1.52 | 0.849 |
| Serum sodium, mmol/L | 137 ± 4 | 138 ± 3 | 0.757 |
| Serum potassium, mmol/L | 4.1 ± 0.9 | 3.9 ± 0.7 | 0.539 |
Plus–minus values are mean ± SD. PCI denotes percutaneous coronary intervention, STEMI ST-segment elevation myocardial infarction, pH potential hydrogen, PaO2 partial pressure of oxygen and PaCO2 partial pressure of carbon dioxide.
4. Discussion
In the present study, we found 1) a crucial difference in the prevalence of impaired myocardial tissue-level reperfusion and in-hospital mortality in accordance with the presence or absence of pre-PCI procedural therapeutic hypothermia in patients with a profound cardiogenic shock complicating anterior STEMI. 2) A pivotal association between impaired myocardial tissue-level reperfusion and in-hospital mortality in those with profound cardiogenic shock. 3) Therapeutic hypothermia did not cause any serious disadvantages in those who completed this treatment in the setting of a profound cardiogenic shock complicating STEMI. Thus, the present findings may provide a great possibility that pre-PCI procedural therapeutic hypothermia would ameliorate in-hospital clinical features in patients with a profound cardiogenic shock complicating anterior STEMI.
As shown in previous studies, in-hospital death is mainly caused by a high incidence of severe multi-organ dysfunction syndromes within a couple of days after the onset of cardiogenic shock in those with STEMI [5] ; [6]. Importantly, fatal clinical outcomes in a cardiogenic shock complicating STEMI were associated with the widespread systemic inflammatory response syndrome showing high serum levels of interleukin-6 [22] ; [23], high scores of either Acute Physiology and Chronic Health Evaluation II [24] or Simplified Acute Physiology Score II [25], but no less associated with cardiac dysfunction itself [5]. Metabolic crisis showing high serum levels of lactate or high base deficit was also recognized as one of the strongest predictors of fatal outcomes in patients with a cardiogenic shock complicating STEMI [5] ; [26]. In view of the rapid development of severe multi-organ dysfunction syndromes with systemic inflammatory response syndrome in those with a cardiogenic shock complicating STEMI, we postulate to restore systemic homeostasis via the regulation of exaggerated systemic inflammation as one of the goals of treatment in those with critical cardiogenic shock [6] ; [27].
Therapeutic hypothermia is widely available and has become an established standard of care for patients with post-cardiac arrest syndromes [28]. Non-randomized trials have also reported the feasibility of combination of therapeutic hypothermia with PCI in the setting of STEMI [11]. The clinical benefits of therapeutic hypothermia in the prevention of a systemic ischemia–reperfusion injury as well as systemic inflammatory response in those with post-cardiac arrest syndromes have been proposed by several potential mechanisms such as enhancing cellular membrane integrity through preserved adenosine triphosphate with a reduction in metabolic demand and glucose consumption [29], prevention of mitochondrial damages via the inhibition of calcium-induced mitochondrial permeability transition pore [30], and an improvement in microcirculation [31]. Furthermore, a reduction in reactive oxygen species [32] and suppression of pro-inflammatory mediators [13] during therapeutic hypothermia may be of great benefit to ameliorate systemic and also myocardial tissue-level ischemia–reperfusion injury [12]. Recently a clinical feasibility and also advantages of pre-PCI procedural therapeutic hypothermia in those with STEMI had been reported [33]. A couple of studies also reported feasibility in therapeutic hypothermia in patients with STEMI complicated with cardiogenic shock [34]; [35] ; [36]. In the present study, we found a crucial possibility of pre-PCI procedural therapeutic hypothermia for a decrease in an incidence of impaired myocardial tissue-level reperfusion and an improvement in in-hospital survival rate in those with a profound cardiogenic shock complicated anterior STEMI. Thus, we believe that a systemic therapeutic hypothermia prior to coronary reperfusion must be the promising challenges to overcome systemic microcirculatory and cellular distress syndrome in this critical disorder. Future investigations warrant a validation of pre-PCI procedural therapeutic hypothermia as a potential strategy in patients with a profound cardiogenic shock complicating STEMI.
5. Study limitations
We have several limitations to putting an accurate interpretation of our findings in the present study. First, this was a retrospective study with a small number of study subjects. There was a demographic bias in the study patients because those treated with therapeutic hypothermia were mostly resuscitated before PCI. So, our findings did not have power to conclude the clinical benefits of pre-PCI procedural therapeutic hypothermia. Future large prospective clinical studies need to confirm the results of this study. Second, although our analysis did not find any disadvantage such as serious arrhythmia, infection, bleeding, etc. during therapeutic hypothermia in the setting of profound cardiogenic shock, the optimal temperature and duration for therapeutic hypothermia in those with a profound cardiogenic shock complicating STEMI are still unknown [37]. Third, because cardiogenic shock has a wide clinical spectrum from mild to profound, there is also a caution to translate the present study into a whole range of those with cardiogenic shock.
6. Conclusions
The present study may provide a pivotal insight into the possibility of clinical benefits of pre-PCI procedural therapeutic hypothermia in patients with a profound cardiogenic shock complicating anterior STEMI.
Funding
This study is currently supported in part by Japan Keirin Association (25-1-089) and the Japanese Research Promotion Society for Cardiovascular Disease (H-5-2014).
Disclosure
The authors declare that there is no conflict of interest.
Acknowledgments
We are deeply indebted to Mariko Ishizaki, for her expert contribution in preparing the manuscript.
References
- [1] J.M. Cheng, C.A. den Uil, S.E. Hoeks, et al.; Percutaneous left ventricular assist devices vs. intra-aortic balloon pump counterpulsation for treatment of cardiogenic shock: a meta-analysis of controlled trials; Eur. Heart J., 30 (2009), pp. 2102–2108
- [2] H. Thiele, B. Allam, G. Chatellier, G. Schuler, A. Lafont; Shock in acute myocardial infarction: the Cape Horn for trials?; Eur. Heart J., 31 (2010), pp. 1828–1835
- [3] H. Thiele, U. Zeymer, F.J. Neumann, et al.; Intraaortic balloon support for myocardial infarction with cardiogenic shock; N. Engl. J. Med., 367 (2012), pp. 1287–1296
- [4] D.S. Menees, E.D. Peterson, Y. Wang, et al.; Door-to-balloon time and mortality among patients undergoing primary PCI; N. Engl. J. Med., 369 (2013), pp. 901–909
- [5] K. Werdan, S. Gielen, H. Ebelt, J.S. Hochman; Mechanical circulatory support in cardiogenic shock; Eur. Heart J., 35 (2014), pp. 156–167
- [6] M. Suzuki; Address to critical issues in a cardiogenic shock complicating acute myocardial infarction; P. Wilkonson (Ed.), Myocardial Infarctions: Risk Factors, Emergency Management and Long-term Health Outcomes, NOVA Science Publishers, Inc., New York, NY (2014), pp. 179–192
- [7] M. Suzuki, I. Takamisawa, A. Seki, et al.; Clinical evidence of exaggerated inflammation in patients with a cardiogenic shock complicating ST-segment elevation myocardial infarction; Health, 5 (2013), pp. 1648–1653
- [8] R.W. Neumar, J.P. Nolan, C. Adrie, et al.; Post-cardiac arrest syndrome: epidemiology, pathophysiology, treatment, and prognostication. A consensus statement from the International Liaison Committee on Resuscitation; Circulation, 118 (2008), pp. 2452–2483
- [9] S. Wolfrum, C. Pierau, P.W. Radke, H. Schunkert, V. Kurowski; Mild therapeutic hypothermia in patients after out-of-hospital cardiac arrest due to acute ST-segment elevation myocardial infarction undergoing immediate percutaneous coronary intervention; Crit. Care Med., 36 (2008), pp. 1780–1786
- [10] L.M. Batista, F.O. Lima, J.L. Januzzi Jr., V. Donahue, C. Snydeman, D.M. Greer; Feasibility and safety of combined percutaneous coronary intervention and therapeutic hypothermia following cardiac arrest; Resuscitation, 81 (2010), pp. 398–403
- [11] D. Stub, S. Bernard, S.J. Duffy, D.M. Kaye; Post cardiac arrest syndrome: a review of therapeutic strategies; Circulation, 123 (2011), pp. 1429–1435
- [12] S. Kanemoto, M. Matsubara, M. Noma, et al.; Mild hypothermia to limit myocardial ischemia–reperfusion injury: importance of timing; Ann. Thorac. Surg., 87 (2009), pp. 157–163
- [13] C. Delhaye, M. Mahmoudi, R. Waksman; Hypothermia therapy: neurological and cardiac benefits; J. Am. Coll. Cardiol., 59 (2012), pp. 197–210
- [14] S.D. Mentzelopoulos, S. Malachias, C. Chamos, et al.; Vasopressin, steroids, and epinephrine and neurologically favorable survival after in-hospital cardiac arrest. A randomized clinical trial; JAMA, 310 (2013), pp. 270–279
- [15] B. Kar, S.S. Basra, N.R. Shah, P. Loyalka; Percutaneous circulatory support in cardiogenic shock: interventional bridge to recovery; Circulation, 125 (2012), pp. 1809–1817
- [16] E. Rivers, B. Nguyen, S. Havstad, et al.; Early goal-directed therapy in the treatment of severe sepsis and septic shock; N. Engl. J. Med., 345 (2001), pp. 1368–1377
- [17] J.L. Vincent, D. De Backer; Circulatory shock; N. Engl. J. Med., 369 (2013), pp. 1726–1734
- [18] D.M. Yealy, J.A. Kellum, D.T. Huang, et al.; A randomized trial of protocol-based care for early septic shock; N. Engl. J. Med., 370 (2014), pp. 1683–1693
- [19] L. Schwartz Longacre, R.A. Kloner, A.E. Arai, et al.; New horizons in cardioprotection: recommendations from the 2010 National Heart, Lung, and Blood Institute Workshop; Circulation, 124 (2011), pp. 1172–1179
- [20] W.G. Austen, J.E. Edwards, R.L. Frye, et al.; A reporting system on patients evaluated for coronary artery disease. Report of the Ad Hoc Committee for Grading of Coronary Artery Disease, Council on Cardiovascular Surgery, American Heart Association; Circulation, 51 (1975), pp. 5–40
- [21] C.M. Gibson, C.P. Cannon, S.A. Murphy, et al.; Relationship of TIMI myocardial perfusion grade to mortality after administration of thrombolytic drugs; Circulation, 101 (2000), pp. 125–130
- [22] A. Geppert, A. Dorninger, G. Delle-Karth, G. Zorn, G. Heinz, K. Huber; Plasma concentrations of interleukin-6, organ failure, vasopressor support, and successful coronary revascularization in predicting 30-day mortality of patients with cardiogenic shock complicating acute myocardial infarction; Crit. Care Med., 34 (2006), pp. 2035–2042
- [23] R. Andrie, U.M. Becher, R. Frommold, et al.; Interleukin-6 is the strongest predictor of 30-day mortality in patients with cardiogenic shock due to myocardial infarction; Crit. Care, 16 (2012), p. R152
- [24] W.A. Knaus, E.A. Draper, D.P. Wagner, J.E. Zimmerman; APACH II: A severity of disease classification system; Crit. Care Med., 13 (1985), pp. 818–829
- [25] J.R. Le Gall, S. Lemeshow, F. Saulnier; A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study; JAMA, 270 (1993), pp. 2957–2963
- [26] H. Thiele, U. Zeymer, F.J. Neumann, et al.; Intra-aortic balloon counterpulsation in acute myocardial infarction complicated by cardiogenic shock (IABP-SHOCK II): final 12 month results of a randomized, open-label trial; Lancet, 382 (2013), pp. 1638–1645
- [27] M. Suzuki; Acute coronary syndromes as auto-inflammatory disorders; Curr. Pharm. Des., 18 (2012), pp. 4370–4384
- [28] M.F. Hazinski, J.P. Nolan, J.E. Billi, et al.; Part 1: executive summary: 2010 International consensus on cardiopulmonary resuscitation and emergency cardiovascular care science with treatment recommendations; Circulation, 122 (2010), pp. S250–S275
- [29] B.Z. Simkhovich, S.L. Hale, R.A. Kloner; Metabolic mechanism by which mild regional hypothermia preserves ischemic tissue; J. Cardiovasc. Pharmacol. Ther., 9 (2004), pp. 83–90
- [30] R. Tisser, N. Couvreur, B. Ghaleh, et al.; Rapid cooling preserves the ischemic myocardium against mitochondrial damage and left ventricular dysfunction; Cardiovasc. Res., 83 (2009), pp. 345–353
- [31] S. Ye, Y. Weng, S. Sun, et al.; Comparison of the durations of mild therapeutic hypothermia on outcome after cardiopulmonary resuscitation in the rat; Circulation, 125 (2012), pp. 123–129
- [32] I. Khaliulin, S.J. Clarke, H. Lin, J. Parker, M.S. Suleiman, A.P. Halestrap; Temperature preconditioning of isolated rat hearts—a potent cardioprotective mechanism involving a reduction in oxidative stress and inhibition of the mitochondrial permeability transition pore; J. Physiol., 581 (2007), pp. 1147–1161
- [33] D. Erlinge, M. Götberg, I. Lang, et al.; Rapid endovascular catheter core cooling combined with cold saline as an adjunct to percutaneous coronary intervention for the treatment of acute myocardial infarction. The CHILL-MI trial: a randomized controlled study of the use of central venous catheter core cooling combined with cold saline as an adjunct to percutaneous coronary intervention for the treatment of acute myocardial infarction; J. Am. Coll. Cardiol., 63 (2014), pp. 1857–1865
- [34] J. Hovdenes, J.H. Laake, L. Aaberge, H. Haugaa, J.F. Bugge; Therapeutic hypothermia after out-of-hospital cardiac arrest: experiences with patients treated with percutaneous coronary intervention and cardiogenic shock; Acta Anaesthesiol. Scand., 51 (2007), pp. 137–142
- [35] R. Skulec, T. Kovarnik, G. Dostalova, J. Kolar, A. Linhart; Induction of mild hypothermia in cardiac arrest survivors presenting with cardiogenic shock syndrome; Acta Anaesthesiol. Scand., 52 (2008), pp. 188–194
- [36] C. Zobel, C. Adler, A. Kranz, et al.; Mild therapeutic hypothermia in cardiogenic shock syndrome; Crit. Care Med., 40 (2012), pp. 1715–1723
- [37] N. Nielsen, J. Wetterslev, T. Cronberg, et al.; Targeted temperature management at 33 °C versus 36 °C after cardiac arrest; N. Engl. J. Med., 369 (2013), pp. 2197–2206
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?