Abstract
Purpose
The aim of this experimental study is to evaluate the efficacy of a novel intraarticular drug in a papain induced osteoarthritis (OA) rat model and compare with the traditional hyaluronat (HA) visco supplementation.
Methods
An early stage OA model was induced by the intra-articular injection of papain enzyme in the right knee joints of 44 Sprague-Dawley rats. Eleven rats (eleven right knees: papain group, 11 left knees: control group) were chosen randomly 28 days after the last injection and sacrificed for verifying OA. The remaining rats (n = 33) were randomly divided into 3 groups. Group 1 was injected 0,2 mL of sterile saline solution (0,9%), group 2 was injected 0,2 mL HA and the group 3 was injected 0,2 mL of HA-CSNAG (hyaluronat, chondritin sulfate, N-acetyl-d -glucosamine) combination in the right knees. Injections were performed on the 35th, the 42nd and the 49th days consecutively. Two weeks after the last injection, all groups were sacrificed to evaluate the severity of OA according to Mankin system.
Results
Early stage of OA was verified regarding total Mankin scores (p < 0.05). There was statistically significant difference between Group 1 and Group 2 (p < 0.05), between Group 1 and Group 3 (p < 0.05) on the 63th day regarding total Mankin scores. Group 3 showed statistically significant improvement in terms of proteoglycan content of matrix when compared to Group 2 (p < 0,05).
Conclusion
HA-CS-NAG compound in hydrogel form is more chondroprotective to rats' cartilage when compared to HA during the early stages of OA.
Keywords
Chondroprotective ; Papain induced osteoarthritis ; Hyaluronic acid ; Mankin score ; Rat
Introduction
Osteoarthritis (OA) is one of the most prevalent and debilitating joint disease associated with reduced quality of life and increased healthcare costs. With respect to recent applications of histopathological and imaging techniques, OA is now considered a heterogeneous chronic disease that may affect all tissues of the synovial joint. A large cascade of events lead to the breakdown and loss of articular cartilage, resulting in the damage of all structures of the joint including subchondral bone change, varying degrees of osteophyte formation, synovitis and adjacent supporting connective tissue elements.1
Available medical therapies, including traditional analgesics and non-steroidal anti-inflammatory drugs (NSAIDs) for OA are ineffective at altering or slowing down the disease progression and rather alleviate the symptoms by reducing pain and improving the joint mobility. Additionally, their chronic use has been limited by their deleterious side effects.2 ; 3 However, various agents including cartilaginous matrix precursors (hyaluronat [HA], chondroitin sulfate [CS], glucosamine [GA]) and cytokine modulators are currently being investigated for their effects on both symptoms and joint structural degradation. These molecules are expected to limit the progression of the disease by affecting the pathological changes in OA and are classified as structure-modifying drugs.4 Due to its positive effects in pain relief and joint functional improvement, the use of viscosupplementation (HA, CS and GA) to treat OA is growing worldwide.5 In addition to HA having potentially chondroprotective effects within the joint, CS and GA play an important role in maintaining joint homeostasis6 and they both have oral and intra-articular injectable forms. Some authors make a point of low bioavailability and potential side effects, including systemic toxicity, impaired glucose tolerance and gastric ulceration of these nutraceuticals when taken orally.7 ; 8 Moreover, the limitations of these drugs, such as protein hypersensitivity of the synovium may have a negative effect on the intra-articular route. Also, the drugs that are injected intra-articularly may be rapidly cleared of the synovial fluid, thus obviating the advantage of direct delivery. Ideally, the drug should be delivered directly inside the affected joint in order to achieve a high intra-articular concentration and have limited systemic toxicity.3
For this purpose, many pharmacologically active drug molecules are under investigation. Recently, an intra-articular injectable hydrogel form of a compound of HA (36 mg/2.25 mL), CS (45 mg/2.25 mL) and N-Acetylglucosamine (NAG) (9 mg/2.25 mL) has been introduced, to achieve long-term drug exposure and low-protein concentration in order to avoid synovial hypersensitivity reaction when delivered intra-articularly.
The purpose of this study was to evaluate the efficacy of this novel intra-articular drug as a structure-modifier and a chondroprotective agent in a papain-induced OA rat model and to compare it to the traditional HA viscosupplementation.
Materials and methods
Study design
All animal experimental research protocols were approved by the Animal Research Committee and the study was supported by our Hospital Research Fund. A total of 44 adult female Sprague-Dawley rats with a mean age of 12 months and weighing between 250 and 350 g were used. Animals were housed (5 rats/cage) under standard management conditions. Room temperature and humidity were maintained at 20–24 °C and at 50–60%, respectively. The light cycle was fixed at 12 h and the animals were fed a standard rat diet with water ad libitum .
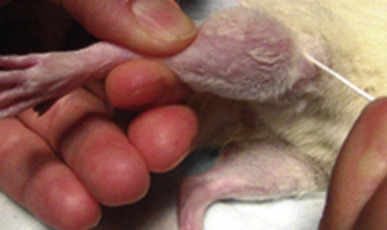
Osteoarthritis was induced by intra-articular injection of papain enzyme (Sigma-P3125; Sigma–Aldrich Corp., St. Louis, MO, USA) at a dose rate of 10 mg in 0.05 M sodium acetate (pH: 4.5) with enzymatic activity of 31 IU/mg in the right knee joints of the 44 Sprague-Dawley rats on the 1st, 4th and 7th days of the study as described by Murat et al9 (Fig. 1 ). On the papain injection days, all rats were injected with 0,2 mL of sterile saline solution (0.9%) in the left knee joints to serve as the control group. On the 35th day, 28 days after the last injection, 11 rats were chosen randomly and sacrificed with high-dose thiopental (200 mg/kg) given intraperitoneally. Both the right (papain group) and the left (control group) knee joints were extra-articularly removed to evaluate the severity of OA according to histological scoring system.10
|
|
|
Fig. 1. Injection to the knee. |
On the 35th day, the remaining experimentally OA-induced rats (n = 33) were randomly divided into three groups, and were given injections in their right knees as follows; 0,2 mL of sterile saline solution (0.9%) in Group 1, 0,2 mL of HA (Ostenil® ; TRB Chemedica AG, Munich, Germany) with a mean molecular weight of 1.2 MDa in Group 2, and 0,2 mL of HA-CS-NAG combination (sodium hyaluronic acid [36 mg/2.25 mL], sodium chondroitin sulfate [45 mg/2.25 mL] and NAG [9 mg/2.25 mL] (Genvisc™ gplus; Phibio GmbH, Frankfurt, Germany)) in Group 3. The injections were given again on the 42nd and 49th days to mimic the clinical use. Two weeks after the last injection, all groups were sacrificed with high dose of intraperitoneal thiopental (200 mg/kg).
Tissue preparation and histological grading
On each scarification day, the tibiofemoral joints of the rats were separated by cutting the tibia and femur, and the attaching ligaments and tendons were removed with a surgical blade. Femoral condyles and tibia samples were fixed at 10% buffered formalin and decalcified in 8% formic acid. After dehydration through a graded series of ethanol solutions, the specimens were embedded in paraffin. The frontal parts were sectioned at 4 μm thickness. Each specimen was evaluated using the modified Mankins histological grading system.11 Hematoxylin and eosin stains were used to evaluate the structure, the chondrocytes, tidemark and pannus formation. Loss of proteoglycan staining intensity was assessed by Toluidine blue staining. Samples were examined and assessed independently by two blinded investigators.
Statistical analysis
Interobserver reliability was evaluated using two-way random, absolute agreement method. Data were evaluated using the SPSS for Windows 21.0 (SPSS Inc., Chicago, IL, USA) software. Before starting the study, a power analysis using pilot data was performed. This analysis determined that with a 95% confidence interval and a power of 80%, 11 animals per group would be required. The Kruskal–Wallis and Dunn tests were used for the comparisons of the parameters. An alpha level of 0.05 was chosen to judge statistical significance.
Results
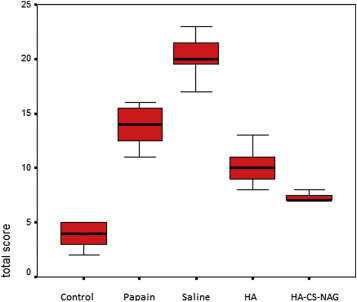
Statistically significant differences were found between the control group (11 left knees) and papain-injected group (11 right knees) regarding total Mankin scores (control: 3.91, papain: 14.0; p < 0.001) (Table 1 ). Representative histological lesions in the cartilage of OA-induced rats were; moderate and severe surface irregularities, cleft formation in the transitional and radial zone, hypercellularity and disrupted columns of chondrocytes and multilayered tidemark. On the 63rd day, lesions were not reduced and got worse in Group 1. Representative histological lesions in Group 1 were; loss of severe matrix loss, moderate pannus formation, all of the above and large patches of cell death and sloughing of layers till mid-zone (Fig. 2 ; Fig. 3 ). On the 63rd day, there was a statistically significant difference between Group 1 and Group 2, between Group 1 and Group 3 regarding total Mankin scores (Group 1: 20.27, Group 2: 10.2, Group 3: 7.18) (Fig. 4 ; Fig. 5 ). Group 3 showed statistically significant improvement in terms of the proteoglycan content of matrix when compared to Group 2 (p < 0.05). Descriptive histological lesions with scores are presented in Table 2 ; Table 3 .
|
|
|
Table 1. Mean and total scores of the groups. |
|
|
|
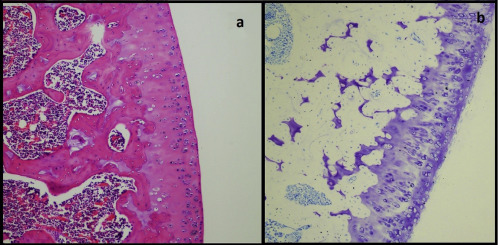
Fig. 2. (a) Characteristics of a normal articular structure: intact surface layer, normal morphology and distribution of chondrocytes and a continuous matrix within them. (b) Proteoglycan matrix showing diffuse staining with accentuation in perichondrial areas (Toluidine blue). |
|
|
|
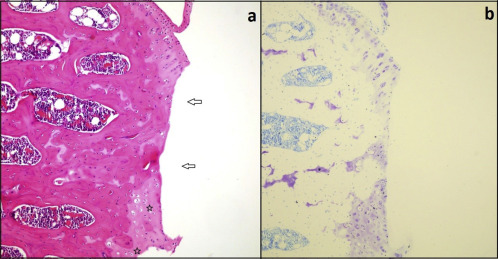
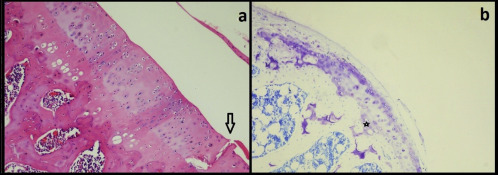
Fig. 3. Images from Group 1 (saline-treated knees) (a) Extensive loss of the transitional and radial zone (arrows) as well as hypocellularity in the residual chondroid structure (asterisk) and cell deaths. (b) Prominent loss of proteoglycan matrix manifesting as pale areas in Toluidine blue staining. |
|
|
|
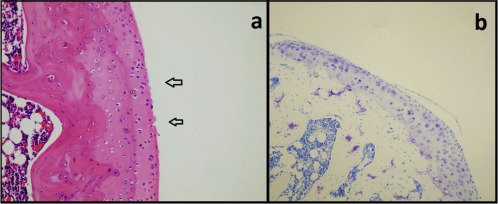
Fig. 4. (a) A vertical cleft extends through the transitional and radial zone (arrow), slightly irregular surface layer, cluster of cells focally as well as hypocellularity and cell deaths. (b) Moderate loss of proteoglycan matrix in Group 2 stained with Toluidine blue (asterisk). |
|
|
|
Fig. 5. (a) Mild to moderate degree of surface irregularity (arrows). Hypercellularity due to chondrocyte proliferation with minimal clustering. (b) Minimal loss of proteoglycan matrix in Group 3 stained with Toluidine blue. |
| Sacrification at 28th day | Sacrification at 63rd day | ||||
|---|---|---|---|---|---|
| Control | Papain induced | Saline treatment | HA treatment | HA-CS-NAG treatment | |
| Cartilage structure | 2.45 ± 0.93 | 5.27 ± 0.65 | 6.27 ± 0.65 | 3.64 ± 0.67 | 2.18 ± 0.40 |
| Cells distribution and density | 0.91 ± 0.54 | 4.09 ± 0.54 | 6.91 ± 0.94 | 2.55 ± 0.82 | 2.00 ± 0.77 |
| Toluidine blue staining | 0.55 ± 0.52 | 2.36 ± 0.67 | 3.09 ± 0.54 | 1.55 ± 0.52 | 1.09 ± 0.30 |
| Tidemark integrity | – | 1.00 ± 0.63 | 2.09 ± 0.54 | 1.45 ± 0.52 | 1.36 ± 0.50 |
| Pannus formation | – | 1.27 ± 0.65 | 1.91 ± 0.54 | 0.82 ± 0.40 | 0.55 ± 0.52 |
| Total Mankin score | 3.91 ± 1.04 | 14.0 ± 1.79 | 20.27 ± 1.79 | 10.02 ± 1.54 | 7.18 ± 0.98 |
| Total Mankin score | Cartilage structure | Cells distribution and density | Toluidine blue staining | Tidemark integrity | Pannus | |
|---|---|---|---|---|---|---|
| Papain/control | p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | p > 0.05 | p < 0.05 |
| HA/saline | p < 0.05 | p < 0.05 | p < 0.05 | p < 0.05 | p > 0.05 | p < 0.05 |
| HA-CS-NAG/saline | p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | p > 0.05 | p < 0.05 |
| HA-CS-NAG/HA | p > 0.05 | p > 0.05 | p > 0.05 | p < 0.05 | p > 0.05 | p > 0.05 |
Discussion
Structure-modifying drugs including HA, CS and GAs are thought to be potentially effective as chondroprotectives by altering the catabolic and anabolic balance of the joint.11 These drugs are candidates for intra-articular use, due to either their poor oral bioavailability or concern for systemic toxicity.3 Despite the presence of many studies on the intra-articular use of HA, oral NAG and CS combination, there is limited experimental data to evaluate the intra-articular application and its effects on hyaline cartilage of these drugs.
The purpose of this experimental study was to evaluate the structure-modifying and chondroprotective effect of an intra-articular injectable hydrogel form of a compound of HA, NAG and CS, through histopathological parameters.
In our study, an early-stage OA model was produced by intra-articular application of papain which is a proteolytic enzyme. Papain impairs the collagen integration by affecting on the proteoglycans in the extracellular matrix (ECM)12 ; it does not have a direct impact on collagen and chondrocytes.13 It has been reported that papain also did not impair the regeneration mechanisms of the cartilage and that the regeneration potential was inversely proportional with the applied dose.12 ; 14 Quantification of the papain-induced OA in rodent models was developed in relation to progression of lesions with days. Thus, it is possible to grade OA and evaluate the available treatment options in these grades. This model has been well accepted and demonstrated that, on Day 28, the observed lesions were consistent with early osteoarthritic changes in humans.9 ; 15
In our experimental model of OA, the scores in each subcategory of Mankin scoring system, including articular cartilage surface, cell distribution and density, Toluidine blue staining (proteoglycan content of matrix), integrity of tidemark and pannus formation were statistically significant when compared to the control group and consistent with those of early-stage OA, similar to literature.9 ; 15 ; 16
Again in our early-stage OA model, HA and HA-CS-NAG compound have provided a statistically significant improvement in the articular surface and matrix proteoglycan content. HA is a critical glycosaminoglycan for the maintenance of functional and structural integrity of the joint cartilage. It is one of the main components of the synovial fluid; it maintains the viscosity and elasticity in the knee joint. The comparison of HA and HA-CS-NAG compound revealed that the proteoglycan content of the matrix in Mankin subtypes were statistically significant in favor of the HA-CS-NAG. We believe that this is due to NAG and CS content of this new hydrogel product. CS and NAG are naturally found in the cartilage matrix, synovial fluid and major components of ECM where they constitute an important part of proteoglycans. They are primarily thought to provide building blocks for the biosynthesis of cartilage ECM by chondrocytes.17
In many in vitro studies, endogenous HA has been shown to increase proteoglycan and collagen synthesis, reduce chondrocytes apoptosis and stimulate the metalloproteinase tissue inhibitor. 18 Some investigators suggest that HA exerts this effect with inhibiting nitric oxide production and this might be a mechanism for the therapeutic effect of HA.19 In addition to chondroprotective effect of HA, it has been shown that NAG inhibits nitric oxide, cyclooxygenase-2, and IL-6 production which in turn reduce apoptosis in cultured human chondrocytes.20 CS can also reduce apoptosis of chondrocytes via mitochondrial pathway.21
In our study, histopathological evaluation revealed statistically significant healing of cellular abnormality in the HA and HA-CS-NAG groups when compared to the saline group, similar to the literature. Although the HA-CS-NAG group had better results in healing cellular abnormality, no significant difference was found when compared to the HA group. At the junction of the hyaline cartilage and adjacent subchondral bone, in the area which is called ‘tidemark’, a remnant of calcified cartilage is present. As OA progresses, vascular invasion and advancement of this zone of calcified cartilage into the articular cartilage occur and this process further contributes to a decrease in the articular thickness.22 The effects of synovial inflammation likely contribute to the dysregulation of chondrocyte function in an analogous fashion, favoring a disequilibrium between the catabolic and anabolic activities of the chondrocyte in remodeling the cartilage ECM.23 With regards to the tidemark and synovial membrane, there were no statistically significant differences between the treatment and saline groups. Since the study was conducted in an early model of OA, this was probably due to the fact that both tidemarks (indistinctly and vascular invasion) and moderate or severe synovial membrane inflammatory changes are present at the advanced steps of OA. Many clinical and experimental studies have demonstrated the efficacy of CS and GA in treating cartilage degeneration and OA in both animals and humans. However, in almost all of these studies, CS and GA have been administered orally.8 ; 24 ; 25 Some authors and guidelines make a point of low bioavailability of GA and CS when taken orally. CS has a very low bioavailability; typically 10–15% in the body.24 When taken orally, most of the GA and CS are lost in the digestive track. This is why it may take a long time to benefit from capsules, tablets and liquids. Therefore, oral GA carries the risk of ‘excess gastric acidity’ leading to what is now known as ‘glucosamine allergy’ (gastric irritation, wheezing, constipation and gastric ulceration).26
Moreover, it is demonstrated that dietary supplement of GA has side effects such as acute liver injury, insulin resistance and impaired glucose tolerance, and increased intra-orbital pressure.7 ; 8 ; 27 There are studies concerning more effective and practical administration of these molecules that have chondroprotective effects as demonstrated in numerous studies. These studies are also aimed at increasing the bioavailability and avoiding side effects. Currently, it has been shown that intra-articular HA, NAG and CS administration is safe and efficacious in OA trials, experimental animal models and in vitro studies. 28 ; 29 ; 30 Overall, our microscopic evaluation revealed the chondroprotective effect of intra-articular HA-CS-NAG compound in hydrogel form in an experimental OA model, with respect to preserving and healing articular surfaces, cellular abnormality and proteoglycan content when compared to the groups treated with saline or HA.
The main drawback of our study which precludes reaching a more definite judgement was that the Mankin scoring system is a semi-quantitative histomorphometric assessment method and its results are subjective. Further studies investigating the quantification of proteoglycan or Type 2 collagen are essential and should be required.
In conclusion, HA-CS-NAG compound in hydrogel form is more chondroprotective to rats' cartilage when compared to HA during the early stages of OA. The HA-CS-NAG compound group showed statistically significant difference regarding the proteoglycan content of ECM.
Conflicts of interest
No conflicts declared.
References
- 1 R.F. Loeser, S.R. Goldring, C.R. Scanzello, M.B. Goldring; Osteoarthritis: a disease of the joint as an organ; Arthritis Rheum, 64 (2012), pp. 1697–1707 PMID: 22392533
- 2 X. Chevalier; Intraarticular treatments for osteoarthritis: new perspectives; Curr Drug Targets, 11 (5) (2010 May), pp. 546–560 PMID: 20199394
- 3 S. Abramson; Drug delivery in degenerative joint disease: where we are and where to go?; Adv Drug Deliv Rev, 58 (2) (2006 May 20), pp. 125–127 Epub 2006 May 2. PMID: 16631277
- 4 P. Qvist, A.C. Bay-Jensen, C. Christiansen, E.B. Dam, P. Pastoureau, M.A. Karsdal; The disease modifying osteoarthritis drug (DMOAD): is it in the horizon?; Pharmacol Res, 58 (1) (2008), pp. 1–7 PMID: 18590824
- 5 B. Gallagher, F.P. Tjoumakaris, M.I. Harwood, R.P. Good, M.G. Ciccotti, K.B. Freedman; Chondroprotection and the prevention of osteoarthritis progression of the knee: a systematic review of treatment agents; Am J Sports Med, 43 (3) (2015 Mar), pp. 734–744 http://dx.doi.org/10.1177/0363546514533777 Epub 2014 May 27. PMID: 24866892
- 6 Yves Henrotina, Marc Marty, Ali Mobasheri; What is the current status of chondroitin sulfate and glucosamine for the treatment of knee osteoarthritis?; Review Maturitas, 78 (3) (2014 Jul), pp. 184–187 http://dx.doi.org/10.1016/j.maturitas.2014.04.015 Epub 2014 May 1. PMID: 24861964
- 7 J.S. Hwang, J.W. Park, M.S. Nam, H. Cho, I.O. Han; Glucosamine enhances body weight gain and reduces insulin response in mice fed chow diet but mitigates obesity, insulin resistance and impaired glucose tolerance in mice high-fat diet; Metabolism, 64 (3) (2015 Mar), pp. 368–379 http://dx.doi.org/10.1016/j.metabol.2014.11.005 Epub 2014 Nov 20. PMID: 25516476
- 8 D.O. Clegg, D.J. Reda, C.L. Harris, et al.; Glucosamine, chondroitin sulfate, and the two in combination for painful knee osteoarthritis; New Engl J Med, 354 (8) (2006 Feb 23), pp. 795–808 PMID: 16495392
- 9 N. Murat, B. Karadam, S. Ozkal, V. Karatosun, S. Gidener; Quantification of papain-induced rat osteoarthritis in relation to time with the Mankin score; Acta Orthop Traumatol Turc, 41 (3) (2007), pp. 233–237 PMID: 17876125
- 10 Y. Sakakibara, T. Miura, H. Iwata, T. Kikuchi, T. Yamaguchi, T. Yoshimi; Effect of high molecular weight sodium hyaluronate on immobilized rabbit knee; Clin Orthop Relat Res, 299 (1994 Feb), pp. 282–292 PMID: 8119031
- 11 Y.S. Park, S.W. Lim, I.H. Lee, et al.; Intra-articular injection of a nutritive mixture solution protects articular cartilage from osteoarthritic progression induced anterior cruciate ligament transection in mature rabbits: a randomized controlled trial; Arthritis Res Ther, 9 (1) (2007), p. R8 PMID: 17257416
- 12 T. Havdrup, A. Henricson, H. Telhag; Papain-induced mitosis of chondrocytes in adult joint cartilage: an experimental study in full-grown rabbits; Acta Orthop Scand, 53 (1982), pp. 119–124 PMID: 7039216
- 13 K.P. Pritzker; Animal models for osteoarthritis: processes, problems and prospects; Ann Rheum Dis, 53 (6) (1994 Jun), pp. 406–420 PMID: 8037500
- 14 T. Kikuchi, T. Sakuta, T. Yamaguchi; Intra-articular injection of collagenase induces experimental osteoarthritis in mature rabbits; Osteoarthr Cartil, 6 (1998), pp. 177–186 PMID: 9682784
- 15 H.M. Khan, M. Ashraf, A.S. Hashmi, M.U.D. Ahmad, A.A. Anjum; Papain induced progressive degenerative changes in articular cartilage of rat femorotibial joint and its histopathological grading; J Anim Plant Sci, 23 (2) (2013), pp. 350–358
- 16 F.U. Ozkan, K. Ozkan, S. Ramadan, Z. Guven; Chondroprotective effect of N-acetylglucosamine and hyaluronate in early stages of osteoarthritis–an experimental study in rabbits; Bull NYU Hosp Jt Dis, 67 (4) (2009), pp. 352–357 PMID: 20001938
- 17 Y. Henrotin, M. Marty, A. Mobasheri; What is the current status of chondroitin sulfate and glucosamine for the treatment of knee osteoarthritis?; Maturitas, 78 (3) (2014), pp. 184–187 maturitas.2014.04.015 http://dx.doi.org/10.1016/j. maturitas.2014.04.015 PMID: 24861964
- 18 A. Ando, Y. Hagiwara, E. Chimoto, K. Hatori, Y. Onoda, E. Itoi; Intra-articular injection of hyaluronan diminishes loss of chondrocytes in a rat immobilized-knee model; Tohoku J Exp Med, 215 (4) (2008 Aug), pp. 321–331 PMID: 18679006
- 19 H. Peng, J.L. Zhou, S.Q. Liu, et al.; Hyaluronic acid inhibits nitric oxide-induced apoptosis and dedifferentiation of articular chondrocytes in vitro; Inflamm Res, 59 (2010), pp. 519–530 PMID: 20077126
- 20 A.R. Shikhman, K. Kuhn, N. Alaaeddine, M. Lotz; N-acetylglucosamine prevents IL-1 beta mediated activation of human chondrocytes; J Immunol, 166 (2001), pp. 5155–5160 PMID: 11290798
- 21 X.L. Yue, S. Lehri, V. Barbier-Chassefiere, et al.; Insights on a new path of pre-mitochondrial apoptosis regulation by a glycosaminoglycan mimetic; Cell Death Differ, 16 (2009), pp. 770–781 PMID: 19229249
- 22 D.B. Burr, M.B. Schaffler; The involvement of subchondral mineralized tissues in osteoarthrosis: quantitative microscopic evidence; Microsc Res Tech, 37 (1997), pp. 343–357 PMID: 9185156
- 23 S.R. Goldring, M.B. Goldring; The role of cytokines in cartilage matrix degeneration in osteoarthritis; Clin Orthop Relat Res, 427S (2004), pp. 27–36 PMID: 15480070
- 24 N. Volpi; Oral absorption and bioavailability of ichthyic origin chondroitin sulfate in healthy male volunteers; Osteoarthr Cartil, 11 (6) (2003 Jun), pp. 433–441 PMID: 12801483
- 25 J. Martel-Pelletier, C. Roubille, F. Abram, et al.; First-line analysis of the effects of treatment on progression of structural changes in knee osteoarthritis over 24 months: data from the osteoarthritis initiative progression cohort; Ann Rheum Ther Nat Rev Rheumatol, 9 (2013), pp. 68–70 PMID: 24336337
- 26 John N. Hathcock, Andrew Shao; Risk assessment for glucosamine and chondroitin sulfate; Regul Toxicol Pharmacol, 47 (2007), pp. 78–83 http://dx.doi.org/10.1016/j.yrtph.2006.07.004 PMID: 16942821
- 27 R.K. Murphy, L. Ketzler, R.D. Rice, S.M. Johnson, M.S. Doss, E.H. Jaccoma; Oral glucosamine supplements as a possible ocular hypertensive agent; JAMA Ophthalmol, 131 (7) (2013 Jul), pp. 955–957 http://dx.doi.org/10.1001/jamaophthalmol.2013.227 PMID: 23702812
- 28 T. Conrozier, X. Chevalier; Long-term experience with hylan GF-20 in the treatment of knee osteoarthritis; Expert Opin Pharmacother, 9 (2008), pp. 1797–1804 PMID: 18570611
- 29 T. Conrozier, J. Jerosch, P. Beks, et al.; Prospective, multi-centre, randomised evaluation of the safety and efficacy of five dosing regimens of viscosupplementation with hylan G-F 20 in patients with symptomatic tibio-femoral osteoarthritis: a pilot study; Arch Orthop Trauma Surg, 129 (2009), pp. 417–423 PMID: 18365224
- 30 A.R. Shikhman, D. Amiel, D. D'Lima, et al.; Chondroprotective activity of N-acetylglucosamine in rabbits with experimental osteoarthritis; Ann Rheum Dis, 64 (2005), pp. 89–94 PMID: 15608304
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?