Summary
Parathyroid carcinoma is a rare disease of unknown etiology. This study presents a case of parathyroid carcinoma in a patient with tertiary hyperparathyroidism. Despite a successful kidney transplantation, the intact parathyroid hormone (iPTH) level of the patient was elevated consistently and could not be controlled by medical therapy. Due to the development of tertiary hyperparathyroidism with bone pain and osteoporosis, subtotal parathyroidectomy was performed 4 months after the kidney transplantation. Histological evaluation revealed that one of four parathyroid lesions was a parathyroid carcinoma, while the others were diffuse hyperplasia. Postoperative laboratory studies indicated a decreased level of iPTH. A positron emission tomography–computed tomography performed 6 months after the operation revealed no evidence of local recurrence or distant metastasis.
Keywords
kidney transplantation;parathyroid carcinoma
1. Introduction
Parathyroid carcinoma is a rare disease of unknown etiology.1 Here, we report a case of parathyroid carcinoma in a patient with tertiary hyperparathyroidism.
2. Case report
A 57-year-old man had received long-term hemodialysis (for 11 years) to manage his chronic renal failure caused by polycystic kidney disease. In 2011, he underwent a kidney transplant; since then he has never experienced any complications or rejection reactions.
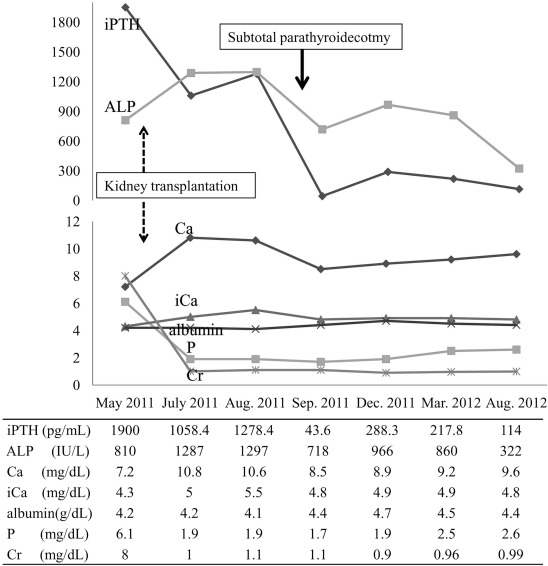
Blood tests performed prior to the kidney transplantation indicated that serum total calcium (Ca) and ionized Ca levels were 7.2 mg/dL (normal, 8.2–10.4 mg/dL) and 4.3 mg/dL (normal, 4.5–5.3 mg/dL), respectively. Serum phosphorus, alkaline phosphatase (ALP), and intact parathyroid hormone (iPTH) levels were found to be 6.1 mg/dL (normal, 1.9–4.4 mg/dL), 810 IU/L (normal, 104–338 IU/L), and above 1900 pg/mL (normal, 14–72 pg/mL), respectively. Postoperative laboratory tests performed 3 months following a kidney transplant surgery showed an elevated level of serum Ca and ALP, which were increased to 10.6 mg/dL and 1297 IU/L, respectively. Blood tests also confirmed a slightly decreased level of iPTH, which was measured to be 1278.4 pg/mL (Fig. 1). The patient took the medication cinacalcet to manage his markedly elevated serum Ca and iPTH levels, but the treatment was ineffective. He complained consistently of knee and ankle pain.
|
|
|
Figure 1. Serum iPTH, ALP, Ca, iCa, albumin, P, and Cr levels from kidney transplantation to subtotal parathyroidectomy. ALP = alkaline phosphatase; Ca = calcium; Cr = creatinine; iCa = ionized calcium; iPTH = intact parathyroid hormone; P = phosphorus. |
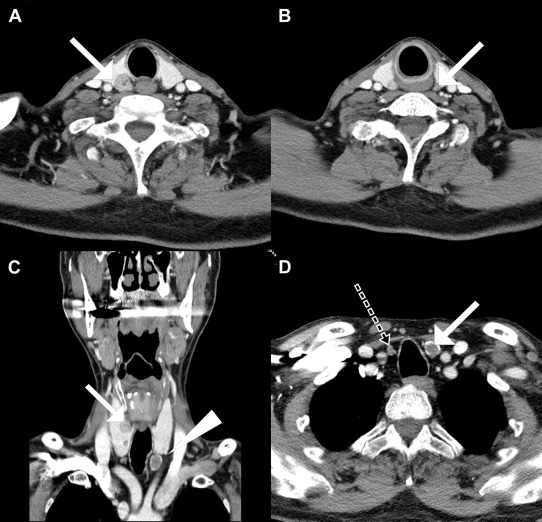
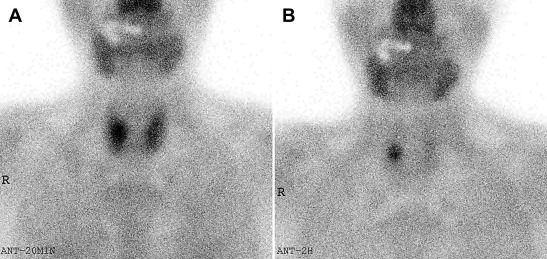
To treat symptomatic tertiary hyperparathyroidism with osteoporosis, the patient was referred to endocrine surgeon. The mean T-score of the lumbar spine (L1–L4), measured by dual-energy X-ray absorptiometry, was –3.1. Computed tomography of the neck showed three enlarged parathyroid glands (Fig. 2). Fig. 3 represents a 2-hour delayed 99mTc-sestamibi scintigraphy (MIBI scan) showing an increased uptake in the right inferior parathyroid gland. During the neck exploration, four enlarged, soft, oval, and yellowish parathyroid glands were observed (right superior: 1.8 × 1.5 cm2; right inferior: 1 × 1 cm2; left superior: 1 × 0.7 cm2; left inferior: 2.5 × 1.8 cm2). Frozen biopsy performed intraoperatively on the left superior parathyroid revealed parathyroid hyperplasia. Left superior parathyroid gland was preserved partially, while other lesions were removed completely.
|
|
|
Figure 2. Enlarged parathyroid glands in computed tomography. (A) Right superior parathyroid (arrow); (B) left superior parathyroid (arrow); (C) right superior parathyroid (arrow) and left inferior parathyroid (arrowhead); and (D) left inferior parathyroid (white arrow) and right inferior parathyroid (dotted arrow). Right inferior parathyroid was mistakenly identified as a lymph node on initial computed tomography. Intraoperative findings confirmed it to be a right inferior parathyroid. |
|
|
|
Figure 3. MIBI scintigraphy. (A) MIBI uptake in both thyroid areas 20 minutes after MIBI injection and (B) MIBI uptake in the right inferior parathyroid 2 hours after MIBI injection. Uptake lesion was identified intraoperatively as a migrated right superior parathyroid. MIBI = 99mTc-sestamibi. |
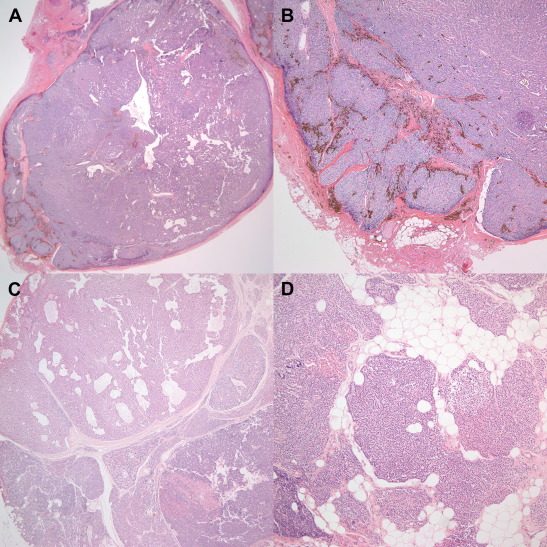
Histological findings revealed a parathyroid carcinoma on a 1.7 × 1.5 × 1.0 cm3 mass of the right superior parathyroid gland; its capsular penetration was present and vascular or perineural invasion was absent. Its surgical resection margin was clear. Histological evaluation confirmed all other resected tissues to be diffuse parathyroid hyperplasia (Fig. 4).
|
|
|
Figure 4. (A) Microscopic finding shows infiltrative parathyroid carcinoma with growth into adjacent fatty tissue (H&E stain, 12.5×). (B) Another microscopic finding displays confluent solid nodules penetrating into fibrofatty tissue adjacent to parathyroid carcinoma (H&E stain, 40×). (C) Diffuse parathyroid hyperplasia (H&E stain, 40×). (D) Parathyroid hyperplasia with sheets of chief cells and scattered fat cells (H&E stain, 100×). H&E = hematoxylin and eosin. |
During follow-up, the patient did not have any serious postoperative complications. Postoperative blood tests performed a day after the operation showed decreased levels of serum Ca and iPTH, which were 8.5 mg/dL and 43.6 pg/mL, respectively. However, a slightly increased value was noted for iPTH level on the follow-up after 3 months of the operation. No evidence of local recurrence or distant metastasis was noted on the positron emission tomography–computed tomography scan, and neck ultrasonography was performed 6 months after the operation. One year postoperatively, his iPTH level continued to decrease to 114.1 pg/mL, and Ca and ALP levels were within normal range (9.6 mg/dL and 322 IU/L, respectively). In addition, the T-score of L4 spine improved markedly (from −3.1 to −1.2).
3. Discussion
Tertiary hyperparathyroidism is defined as persistent parathyroid hyperfunction developing from the secondary hyperplasia that occurs after restoration of renal function.2 Parathyroid pathology in patients with tertiary hyperparathyroidism mostly reveals marked hyperplasia.3 The patient in our study underwent subtotal parathyroidectomy for uncontrolled hyperparathyroidism after kidney transplantation. Subsequent histological findings confirmed one of four parathyroid lesions to be an unexpected parathyroid carcinoma and the others as diffuse parathyroid hyperplasia. On the basis of the histological confirmation of a parathyroid carcinoma and the finding of high iPTH level, we diagnosed this case as parathyroid carcinoma in tertiary hyperparathyroidism.
Considering that the operation was performed only 4 months after the kidney transplantation, it is unclear when the parathyroid carcinoma developed. Some reports have suggested that chronic renal failure is associated with the development of parathyroid carcinoma.4 ; 5 Therefore, parathyroid carcinoma may develop during secondary hyperparathyroidism. Some studies showed that the incidence of endocrinologic cancer was increased more after kidney transplantation than prior to the transplantation.6 ; 7 A study reported that cumulative incidence of nonskin malignancy after kidney transplantation was 1.2% at Month 3.7 Immunosuppressive agents such as azathioprine and calcineurin inhibitors are most linked with post-transplant malignancies.8 However, there was no report on the occurrence of parathyroid carcinoma. Further studies are necessary to clarify the underlying mechanism for the development of parathyroid carcinoma.
Some studies have suggested that significantly high level of serum Ca is a positive predictive factor for parathyroid carcinoma in patients with primary hyperparathyroidism.1; 9 ; 10 However, it should be noted that the Ca level is not a useful indicator of parathyroid carcinoma in patients with end-stage renal disease, as the kidney does not respond to parathyroid hormone in such patients. Although parathyroid carcinoma and hyperplasia can be expected to increase serum Ca level significantly once renal function recovers in response to high iPTH, only a slight increase in its level was observed in our case. Therefore, Ca level do not seem to be useful indicator of parathyroid carcinoma in secondary or tertiary hyperparathyroidism.
MIBI scanning is a useful modality for localization of abnormal parathyroid lesions in hyperparathyroidism.11 However, the role of a MIBI scan in diagnosing parathyroid carcinoma in secondary or tertiary hyperparathyroidism is, as yet, not clear.12 The MIBI scan can be used as an indicator of proliferative parathyroid gland activity.13 Parathyroid carcinoma can be assumed to have higher proliferative activity than parathyroid hyperplasia. Therefore, when a lesion of parathyroid carcinoma coexists with other lesions of parathyroid hyperplasia, an increased uptake in the MIBI scan is suggestive of parathyroid carcinoma.
In our case, a 2-hour delayed MIBI scan showed an increased uptake in the right inferior gland. However, parathyroid carcinoma was later found in the right superior parathyroid gland. This discordance can be due to the fact that the superior parathyroids, when tumorous, may migrate posteriorly and inferiorly, and often appear as higher uptake in the inferior location on MIBI scan.14 In fact, we identified migrated right superior parathyroid tumors in posterior and inferior positions, intraoperatively. Single-photon emission computed tomography MIBI scan is helpful in differentiating between superior and inferior parathyroid lesions.15 ; 16
Postoperative laboratory findings for iPTH level were dynamic: it decreased to 43.6 pg/mL on postoperative Day 1, increased to 288.3 pg/mL 3 months following the operation, and then decreased again to 114 pg/mL. Such findings may be explained by the recurrence of tumor. However, its possibility was considered minimal, because iPTH level decreased without any treatment and imaging studies were inconsistent. We assumed that the remaining hyperplastic parathyroid tissues were impaired transiently in the immediate postoperative period and regained their function afterward. Some studies showed that 24–35% patients with parathyroid adenoma had increased levels of iPTH 8 weeks after parathyroidectomy,17 ; 18 which implied diminished Ca absorption and increased bone turnover with cortical bone remineralization.18 Therefore, in our case, an increased iPTH level after parathyroidectomy may be attributed to bone remineralization.
References
- 1 E. Shane; Clinical review 122: parathyroid carcinoma; J Clin Endocrinol Metab, 86 (2001), pp. 485–493
- 2 M.W. Krause, C.E. Hedinger; Pathologic study of parathyroid glands in tertiary hyperparathyroidism; Hum Pathol, 16 (1985), pp. 772–784
- 3 E. Kebebew, Q.Y. Duh, O.H. Clark; Tertiary hyperparathyroidism: histologic patterns of disease and results of parathyroidectomy; Arch Surg, 139 (2004), pp. 974–977
- 4 M. Bossola, L. Tazza, A. Ferrante, et al.; Parathyroid carcinoma in a chronic hemodialysis patient: case report and review of the literature; Tumori, 91 (2005), pp. 558–562
- 5 Y. Tominaga; Mechanism of parathyroid tumourigenesis in uraemia; Nephrol Dial Transplant, 14 (1999), pp. 63–65
- 6 C.M. Vajdic, S.P. McDonald, M.R. McCredie, et al.; Cancer incidence before and after kidney transplantation; JAMA, 296 (2006), pp. 2823–2831
- 7 B.L. Kasiske, J.J. Snyder, D.T. Gilbertson, C. Wang; Cancer after kidney transplantation in the United States; Am J Transplant, 4 (2004), pp. 905–913
- 8 R. Marcén; Immunosuppressive drugs in kidney transplantation: impact on patient survival, and incidence of cardiovascular disease, malignancy and infection; Drugs, 69 (2009), pp. 2227–2243
- 9 A.C. Cordeiro, F.L. Montenegro, M.A. Kulcsar, et al.; Parathyroid carcinoma; Am J Surg, 175 (1998), pp. 52–55
- 10 J.B. Koea, J.H. Shaw; Parathyroid cancer: biology and management; Surg Oncol, 8 (1999), pp. 155–165
- 11 M. McBiles, A.T. Lambert, M.G. Cote, S.Y. Kim; Sestamibi parathyroid imaging; Semin Nucl Med, 25 (1995), pp. 221–234
- 12 C. Lomonte, N. Buonvino, M. Selvaggiolo, et al.; Sestamibi scintigraphy, topography, and histopathology of parathyroid glands in secondary hyperparathyroidism; Am J Kidney Dis, 48 (2006), pp. 638–644
- 13 M.R. Custódio, F. Montenegro, A.F.P. Costa, et al.; MIBI scintigraphy, indicators of cell proliferation and histology of parathyroid glands in uraemic patients; Nephrol Dial Transplant, 20 (2005), pp. 1898–1903
- 14 G.W. Randolph; Surgery of the Thyroid and Parathyroid Glands; Saunders, Philadelphia (2003) 517
- 15 B. Shafiei, S. Hoseinzadeh, F. Fotouhi, et al.; Preoperative 99mTc-sestamibi scintigraphy in patients with primary hyperparathyroidism and concomitant nodular goiter: comparison of SPECT-CT, SPECT, and planar imaging; Nucl Med Commun, 33 (2012), pp. 1070–1076
- 16 H.K. Eslamy, H.A. Ziessman; Parathyroid scintigraphy in patients with primary hyperparathyroidism: 99mTc sestamibi SPECT and SPECT/CT; Radiographics, 28 (2008), pp. 1461–1476
- 17 A. Bergenfelz, S. Valdemarsson, S. Tibblin; Persistent elevated serum levels of intact parathyroid hormone after operation for sporadic parathyroid adenoma: evidence of detrimental effects of severe parathyroid disease; Surgery, 119 (1996), pp. 624–633
- 18 J. Westerdahl, S. Valdemarsson, P. Lindblom, A. Bergenfelz; Postoperative elevated serum levels of intact parathyroid hormone after surgery for parathyroid adenoma: sign of bone remineralization and decreased calcium absorption; World J Surg, 24 (2000), pp. 1323–1329
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?