Abstract
The world, led by the United States, is hell bent on establishing the absence of choice in addiction, as expressed by the defining statement that addiction is a “chronic relapsing brain disease” (my emphasis). The figure most associated with this model, the director of the American National Institute on Drug Abuse, Nora Volkow, claims that addiction vitiates free will through its effects on the brain. In reality, while by no means a simple task, people regularly quit their substance addictions, often by moderating their consumption, usually through mindfulness-mediated processes (Peele, 2007).
Ironically, the brain disease models ascendance in the U.S. corresponds with epidemic rises in opiate addiction, both painkillers (Brady et al., 2016) and heroin (CDC, n.d.), as well as heroin, painkiller, and tranquilizer poisoning deaths (Rudd et al., 2016). More to the point, the conceptual and treatment goal of eliminating choice in addiction and recovery is not only futile, but iatrogenic. Indeed, the National Institute on Alcohol Abuse and Alcoholisms epidemiological surveys, while finding natural recovery for both drug and alcohol disorders to be typical, has found a decline in natural recovery rates (Dawson et al., 2005) and a sharp increase in AUDs (Grant et al., 2015).
Keywords
Chronic brain disease;Free will;Nora volkow;Harm reduction;Mindfulness;Natural recovery
Nora Volkow, director of the American National Institute on Drug Abuse, the best-known representative of the model of addiction as a chronic brain disease (see Nature, 2014) declared “Addiction as a disease of free will” (Volkow, 2015) for which we as a society need to:
understand that addiction is not just a disease of the brain, but one in which the circuits that enable us to exert free will no longer function as they should. Drugs disrupt these circuits. The person who is addicted does not choose to be addicted; its no longer a choice to take the drug.
The Surgeon Generals first report on smoking (Department of Health, Education, and Welfare, 1964), “Smoking and Health,” definitively linked smoking to cancer, beginning a cultural process over the following decades in which over half of smokers quit. But a substantial minority didn't quit.
The Department of Health and Human Services (2002) published a volume entitled, “Those Who Continue to Smoke.” The investigators imagined those who continued to be addicted as being handicapped in some way. The results were perplexing: “In summary, these trends do not suggest that the population of smokers who remains is more addicted, more resistant to cessation messages, less likely to attempt cessation, or increasingly composed of those with limited activities or poor mental health” (p. 143).
One particularly interesting and surprising finding in the monograph was an interaction between age and degree of dependence in smoking cessation: more dependent younger smokers were less likely to quit than less dependent ones; more dependent older smokers were more likely to do so. Jettisoning all assumptions about addiction, a sensible deduction would be that older heavier smokers, sensing their mortality and wanting to delay death, which they knew was more likely to ensue given the severity of their habit, were more motivated to quit and more often did so.
The whole point in smoking cessation efforts was to recognize smoking as addictive, which is now universally accepted (although the 1964 Surgeon Generals report explicitly rejected the idea; cf. Peele, 2010). Yet these results confound our notion of addiction, and certainly the ironclad, neuroscientific, brain disease model of it.
Despite the consensus around smokings addictiveness, perhaps these results are limited to nicotine/smoking. No, they are not. A contributor to this issue, Gene Heyman (2013), analyzed the most recent NESARC data according to a timeline of likelihood of quitting a drug dependence:
Although varied [according to the specific substance], the remission results were orderly. An exponential growth curve closely approximated the cumulative frequency of remitting for different drugs and different ethnic/racial groups. Thus, each year a constant proportion of those still addicted remitted, independent of the number of years since the onset of dependence.
In summary, addiction as the idea that people are irresistibly, inexorably, irreversibly stuck in a drug dependence so that no effort of will can extricate them is wrong, as proved by research that directly tests this belief. Yet Volkow has no fear of being contradicted while claiming the counterfactual assertion and, moreover, cloaking it with the mantle of science.
1. Reductionism, harm reduction, natural remission
People readily substitute “scientism” for science: that is, being awed by seemingly scientific activity in place of the actual science of testing hypotheses with data.
The New York Times offer one of many examples of a clinician coming to grips with harm reduction, or the idea that total abstinence is not the only beneficial outcome.
Can Nicotine Be Good for You?
My new patient explained that in her sophomore year at college she had started smoking. The effect, she said, was like “a key that fit perfectly into a lock.” Her brain felt clearer, her thoughts were more coherent, her mood and energy improved. Not wanting to damage her lungs, she soon switched over to nicotine gum and had been taking the same amount of it for well over a decade. (my emphasis)
She asked me what I thought of her use of the drug. The short answer was that I didn't know what to make of it.
Ultimately, this clinician could only justify allowing her client to persist in this less harmful form of addiction by concluding that her addiction was “in her brain.”
But as I thought about our conversation later, I found her image of a key in a lock particularly striking; it was the very same one that psychiatrists and neurophysiologists use to describe the interactions in the brain between neurotransmitters and their receptors. And in fact, neurons do have receptors into which nicotine neatly fits, mimicking the actions of the brains own molecules. (Fels, 2016)
What if the writer were forced to confront the best data, which shows that people regularly overcome substance addictions, including smoking, even after they are notable for failing to do so for years, even decades? She seemingly wouldn't be able to gather sufficient moral commitment to approve of continuing the addiction in a less harmful form. Her justification for proceeding on this basis is, in my wording, “This woman can't quit her addiction. Its the neurochemical key to her brain.”
But what about all of those people who do quit addictions? At some point in my presentations, I ask the audience, “Have any of you quit a smoking addiction?” A third to a half raise their hands. Virtually none of the people in these exercises relies on the nicotine replacement therapy (NRT) used by this woman. This demonstration doesn't prove that this woman can quit chewing nicotine gum. But it is important to establish scientifically accurate parameters for this possibility.
Using this Times case in a workshop, I said: “Well, of course, this therapist did a brain scan to show that this particular woman has a particular neurochemical reaction proving nicotine has the key to her brain.” No she (the therapist) didn't. She wouldn't know how. Nobody does. There is no such neurochemical key. Nor can a brain scan show that people are able, or on the verge, of quitting or cutting back their addiction. There is some experiential configuration that creates both the addiction and change that can't be broken down into neurochemical, cognitive, and situational components. The residue strongly resembles what might be called free will ( Peele and Thompson, 2015).
Therapy is often directed to lowering a person like this womans anxiety levels and to figuring out her experiential and situational keys—called addictive cues or triggers—for the purpose of assisting her to abstain. But its the womans right to refuse to participate in this process, and our obligation to accept her choice. What is wrong, and immoral, is to tell the woman that such change isn't possible. This phenomenon of mislabeling continued addiction as a biological imperative has been imbedded in harm reduction by Dole and Nyswander (1967), the developers of methadone maintenance, through their claim that former heroin users absolutely require substitute narcotics such as methadone or buprenorphine because they suffer from a permanent “metabolic disease.”
But they don't. Maybe people want that substitute (and who is to say this “want” is not a “need”), either currently, for a long time, or forever. Its their right to choose, without added guilt laid on by therapists or would-be helpers. The parallel is inescapable to observers who justify gay lifestyles on the grounds that peoples sexuality is genetically determined. Would such defenders of gay rights then arrest people who chose a same-sex mate but who were proved not to have a gay gene (one that does not exist)? Of course, when confronted with bisexuality, such well-meaning advocates for tolerance based on biological imperatives are left hemming and hawing.
2. The strange (according to whom?) workings of the human mind
In the area of harm reduction, two landmark studies show that an outcome once claimed by both Alcoholics Anonymous and the journal Science ( Pendery et al., 1982) to be nigh on impossible occurs regularly—as I, along with another contributor to this volume, Nick Heather, have noted for three decades ( Heather and Robertson, 1981; Peele, 1983; Peele, 1987b ; Peele, 2013). Neither study explicitly addresses harm reduction, or what was then called controlled drinking. Yet each offers fundamental insight into its natural occurrence.
A treatment study with alcohol-dependent subjects conducted by the most prestigious pharmacologically-based research center in the United States, at the University of Pennsylvania as led by Charles O′Brien, attempted to establish the benefits of “pharmacogenetic matching” in the case of Naltrexone treatment (NTX) for alcoholism (Oslin et al., 2015). That is, NTX results in alcoholism treatment were often scattered, and the investigators surmised that variants (alleles) of an opioid receptor gene might account for the differences.
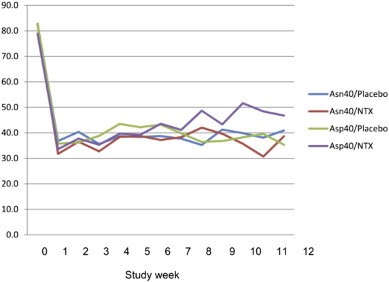
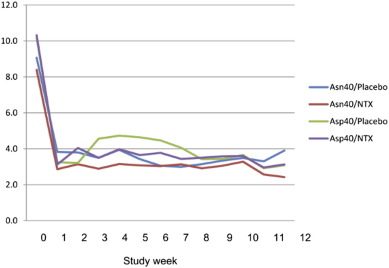
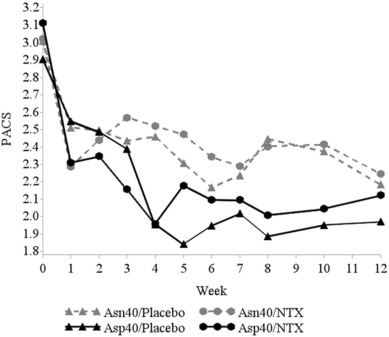
But no such matching appeared. In fact, placebo outcomes for reduced drinking were virtually identical to those created by NTX in two opioid receptor allele conditions over an experimental period of 12 weeks—remarkably so, as shown in Fig. 1 ; Fig. 2. For craving assessments (Fig. 3), the lowest measurement occurred for a placebo group by the end of the trial. This is not to say that benefits in reduced drinking weren't noted. Indeed, they were distinct and across-the-board. Moreover, these benefits appeared almost instantly, at the very outset of the trial.
|
|
|
Fig. 1. Percent days of any drinking during the course of treatment. |
|
|
|
Fig. 2. Drinks per drinking day during the course of treatment. |
|
|
|
Fig. 3. Weekly craving measure during the course of treatment. |
These results strongly resemble those from the landmark clinical trial of psychotherapy for alcoholism treatment—Project MATCH. In fact, the massive MATCH operation produced no usable results in re matching, to which the director of the NIAAA, Enoch Gordis, responded by claiming: “The good news is that treatment works. All three treatments evaluated in Project MATCH produced excellent overall outcomes.”
In order to make such a statement, however, Gordis and MATCH investigators had to overlook the relative paucity of abstinence by subjects (who were highly selected to be socially stable and not burdened with mental illness or criminal problems), and instead to emphasize harm reduction outcomes: “During the year after treatment, 1 in 4 clients remained continuously abstinent on average, and an additional 1 in 10 used alcohol moderately and without problems. The remaining clients, as a group, showed substantial improvement, abstaining on 3 days out of 4 and reducing their overall alcohol consumption by 87%, on average. Alcohol-related problems also decreased by 60%” (Miller et al., 2001).
This was not the final word on MATCH, however. As I summarized the MATCH results, (Peele, 1997), combined with the NIAAAs NLAES project: “(1) minimal or no treatment produces outcomes that are equal to/better than those from longer/standard treatments; (2) patient traits and initiative are far more important than treatment type or intensity for recovery; (3) reduced drinking is the most common outcome for alcohol-dependent individuals.” Some years later Cutler and Fishbain (2005) re-analyzed the MATCH data, with the conclusions: “Overall, a median of only 3% of the drinking outcome at follow-up could be attributed to treatment. However this effect appeared to be present at week one before most of the treatment had been delivered.” (emphasis added).
As with the NTX/genetics trial, the main deduction to be taken from Project MATCH is that something identifiable as treatment has little to do with recovery, relative to the persons own ability to come to grips with and to eliminate their addiction.
3. What if you remove choice from people?
The goal of the brain disease model of addiction is to remove any idea of the drinker or drug user as an active participant in their recovery, as someone capable of enacting an intention to quit in line with their values (see Peele, 1987a). Instead, this model sees humans as biological automatons who must rely on—can only be passive recipients of—some modern medical miracle, a la NTX, that isolates and removes the neurochemical source of their addiction.
Nicotine replacement therapy (NRT) is the most widespread form of chemical treatment for addiction. In clinical trials, NRT produces a slight but distinct advantage over peoples quitting cold turkey. But, as to maintaining abstinence, researchers at Harvards Center for Global Tobacco Control compared people who quit smoking either cold turkey, or with NRT, three times at interims of two years each (Alpert et al., 2012).
The study found no advantage in smoking cessation from using NRT. Moreover, for the most dependent smokers, NRT use significantly more often led to relapse. This typically happened when the smokers abandoned their NRT regimen, and then quickly relapsed. Dr. Gregory N. Connolly, director of Harvards Center and co-author of the study, regretted their discovery: “We were hoping for a very different story. I ran a treatment program for years, and we invested millions in treatment services” (Carey, 2012).
Why did highly dependent smokers relapse so readily after receiving NRT? The most important ingredients in quitting addictions are the persons belief that they can, and their commitment to doing so. These elements represent a basic life shift; they are inescapable aspects of overcoming addiction in the long run. And these essential ingredients to recovery cannot be injected or ingested in drug form. Instead, telling yourself that you can't quit your addiction without the drug undercuts the self-efficacy required to achieve freedom from addiction. And, not recognizing this truth, a massive, well-intentioned program produced more negative outcomes, and presumably death.
This remarkable finding about addiction as experienced “in the flesh” won't impact those who espouse chemical remedies for addiction, and who detest self-cure, just as their results had no effect on the O′Brien team (which concluded: “Despite the results of this trial, pharmacogenetics continues to hold promise as a way to improve the targeting of medications to improve treatment response,” p. E6). Dr. Richard Hurt, director of the Nicotine Dependence Center at the Mayo Clinic, who was not involved in the Harvard study, said products like nicotine gum and patches “are absolutely essential, but we use them in combinations and doses that match treatment to what the individual patient needs, unlike smokers who are self-treating.”
The Times itself continues to drumbeat chemical cures for smoking in its Well column, including now in addition to NRT, Chantix. Meanwhile, in a workshop I led (March 3, 2016) at Adelphi Universitys School of Social Work comprising 85 people, I asked how many had quit smoking. Thirty to 35 people raised their hands. When I asked how many used any form of medication in order to quit, one person raised her hand.
I then asked another woman what had enabled her to quit. “I tried for years, and I was sick with worry. I would go to bed at night, vowing not to smoke in the morning, and then I picked it right up again.” This story is identical to those told by smokers who finally quit smoking, they say, due to Chantix, stories frequently advertised on television by the drugs manufacturer. Only this womans story, almost universally typical for the smokers in my informal sample, a group unheard from in the media, in which she ultimately quit on her own after a tortuous journey, and didn't relapse, fundamentally contradicts the advertisement.
4. What does this tell us about addiction, therapy and change?
4.1. Iatrogenic conceptions and treatment
What may be the most obvious result of our cultural conceptions and therapeutic efforts in re addiction is our ability to create addiction and to retard remission. I have cited the sharp increase in overdose deaths (more accurately labeled drug-related-deaths, cf. Rudd et al., 2016) and reported addiction (Brady et al., 2016; although the leap from DRD to addiction is, by itself, speculative and tangential) concurrent with the ascendance of the brain disease movement (Peele, 2016). This backward trend is also evident in the U.S. governments survey of lifetime histories of drug and alcohol dependence, referred to as NLAES and NESARC. Both NLAES and NESARC (which included waves of surveying of subjects) have found natural remission to be the dominant outcome category, including a majority of formerly-dependent drinkers who now drink without problems (Peele, 2007)
While it isn't possible to compare the exact remission rates across the decades between NLAES (1992, see Dawson, 1996), NESARC I (2001–2002, see Dawson et al., 2005), and NESARC III (2012–2103, see Grant et al., 2015), we detect that (a) Dawson et al. (2005) noted a decline in natural remission between NLAES and NESARC I, while (b) Grant et al. (2015) found a 50% increase (!) in past-year AUDs, from 8.5% to 14% retaining the DSM-IV categorization of subjects, between 2001–02 and 2012–13.
4.2. Mindfulness, meaning the ability to separate oneself from ones addicted state, is an essential therapeutic tool
What accounts for apparently simultaneously increasing painkiller and heroin addiction rates in the early part of this century, along with the sharp increase in measured alcohol use disorders? It is certainly not a good sign for current conceptions of addiction and therapy for it, but rather the reverse (Peele, 2015). In Recover! ( Peele and Thompson, 2015), I argue for therapy that (a) separates peoples identities from their addictions by making clear the latter are changeable, and (b) the use of mindfulness, derived from Buddhism, that presents cognitive techniques that allow people to detach themselves from the ongoing rush of their experience.
We issue a call in Recover!: "So, hear this: you are not a passive spectator to your brains functioning or an unfortunate victim of it. You are the primary generator of how your brain functions—of how you function—both in the here and now, and certainly over the long run."
And this is free will.
5. Conclusion
People regularly quit addictions, including often by cutting down their consumption in the case of alcohol. Yet these phenomena—self-cure and moderation—are little noted in the dominant neuroscientific paradigm of addiction. Indeed, it may be impossible for this paradigm to accommodate these phenomena, which dominate both our lived experience and epidemiological data (Peele, 2015).
To form a realistic, useful scientific and policy approach to addiction we must instead recognize:
- Change in addictive behavior is usually self-initiated and self-propelled—i.e., mindful.
- Convincing people that they are not able to control their behavior is counterproductive.
- The dominant model of addiction, viewing people as passive victims, fuels addiction.
References
- Alpert et al., 2012 H.R. Alpert, G.N. Connolly, L. Biener; A prospective cohort study challenging the effectiveness of population-based medical intervention for smoking cessation; Tobacco Control (2012) http://dx.doi.org/10.1136/tobaccocontrol-2011-050129
- Brady et al., 2016 K.T. Brady, J.L. McCauley, S.E. Back; Prescription opioid misuse, abuse, and treatment in the United States: An update; American Journal of Psychiatry, 173 (2016), p. 1 (Available at http://ajp.psychiatryonline.org/doi/abs/10.1176/appi.ajp.2015.15020262)
- Carey, 2012 B. Carey; Nicotine gum and skin patch face new doubt: Nicotine replacement doesn't help smokers quit, study finds; New York Times (2012) (Available at http://mobile.nytimes.com/2012/01/10/health/study-finds-nicotine-gum-and-patches-dont-help-smokers-quit.html?, January 9)
- Centers for Disease Control and Prevention, N.d Centers for Disease Control and Prevention. (n.d.). Todays heroin epidemic. Vital Signs. (Accessed March 8, 2016. Available at http://www.cdc.gov/vitalsigns/heroin/).
- Cutler and Fishbain, 2005 R.B. Cutler, D.A. Fishbain; Are alcoholism treatments effective? The project MATCH data; BMC Public Health, 5 (2005), pp. 75–85 http://dx.doi.org/10.1186/1471-2458-5-75
- Dawson, 1996 D.A. Dawson; Correlates of past-year status among treated and untreated persons with former alcohol dependence: United States, 1992; Alcoholism: Clinical and Experimental Research, 20 (1996), pp. 771–779
- Dawson et al., 2005 D.A. Dawson, B.F. Grant, F.S. Stinson, P.S. Chou, B. Huang, W.J. Ruan; Recovery from DSM-IV alcohol dependence, United States, 2001–2002; Addiction, 100 (2005), pp. 281–292
- Department of Health, Education, and Welfare, 1964 Department of Health, Education, and Welfare; Smoking and health (public health service publication no. 1103); USGPO, Washington, DC (1964)
- Department of Health and Human Services, 2002 Department of Health and Human Services; Those who continue to smoke (monograph 15); Smoking and Tobacco Control Series, Rockville, MD (2002)
- Dole and Nyswander, 1967 V.P. Dole, M.E. Nyswander; Heroin addiction—A metabolic disease; Archives of Internal Medicine, 120 (1) (1967), pp. 19–24
- Fels, 2016 A. Fels; Can nicotine be good for you? New York Times (2016) (Available at http://www.nytimes.com/2016/03/06/opinion/sunday/can-nicotine-be-good-for-you.html, March 5)
- Grant et al., 2015 B.F. Grant, R.B. Goldstein, T.D. Saha, S.P. Chou, J. Jung, H. Zhang, ... D.S. Hasin; Epidemiology of DSM-5 alcohol use disorder: Results from the national epidemiologic survey on alcohol and related conditions III; JAMA Psychiatry, 72 (8) (2015), pp. 757–766 http://dx.doi.org/10.1001/jamapsychiatry.2015.0584
- Heather and Robertson, 1981 N. Heather, I. Robertson; Controlled drinking; Methuen, London (1981)
- Heyman, 2013 G.H. Heyman; Quitting drugs: Quantitative and qualitative features; Annual Review of Clinical Psychology, 9 (2013), pp. 29–59 http://dx.doi.org/10.1146/annurev-clinpsy-032511-143041
- Miller et al., 2001 W.R. Miller, S.T. Walters, M.E. Bennett; How effective is alcoholism treatment in the United States?; Journal of Studies on Alcohol, 62 (2) (2001), pp. 211–220 (Available at http://www.ncbi.nlm.nih.gov/pubmed/11327187)
- Nature (Editorial), 2014 Nature (Editorial); Animal farm: Europes policy-makers must not buy animal-rights activists' arguments that addiction is a social, rather than a medical, problem; Nature (2014) (Available at http://www.nature.com/news/animal-farm-1.14660, February 5)
- Oslin et al., 2015 D.W. Oslin, S.H. Leong, K.G. Lynch, W. Berrettini, C.P. O'Brien, A. Gordon, M. Rukstalis; Naltrexone vs placebo for the treatment of alcohol dependence: A randomized clinical trial; JAMA Psychiatry, 72 (5) (2015), pp. 430–437 http://dx.doi.org/10.1001/jamapsychiatry.2014.3053
- Peele, 1983 S. Peele; Through a glass darkly: Can some alcoholics learn to drink in moderation? The answer, at least in this country, may be more political than scientific; Psychology Today (1983), pp. 38–42 (Available at http://www.peele.net/lib/glass.html, April)
- Peele, 1987a S. Peele; A moral vision of addiction: How peoples values determine whether they become and remain addicts; Journal of Drug Issues, 17 (2) (1987), pp. 187–215 (Available at http://www.peele.net/lib/vision.html)
- Peele, 1987b S. Peele; Why do controlled-drinking outcomes vary by investigator, by country and by era? Cultural conceptions of relapse and remission in alcoholism; Drug and Alcohol Dependence, 20 (1987), pp. 173–201 (Available at http://www.peele.net/lib/cdoutcomes.html)
- Peele, 1997 S. Peele; Bait and switch in project MATCH: What NIAAA research actually shows about alcohol treatment; PsychNews International (1997) (Available at http://www.peele.net/lib/projmach.html, May-June)
- Peele, 2007 S. Peele; Addiction as disease: Policy, epidemiology, and treatment consequences of a bad idea; J. Henningfield, W. Bickel, P. Santora (Eds.), Addiction treatment in the 21st Century: Science and policy issues, Johns Hopkins, Baltimore (2007), pp. 153–163 (Available at http://www.peele.net/lib/consequences.html)
- Peele, 2010 S. Peele; The fluid concept of smoking addiction; C.V. Phillips, P.L. Bergen (Eds.), Tobacco harm reduction 2010: A yearbook of recent research and analysis. TobaccoHarmReduction.org (2010) (Available at http://www.peele.net/lib/fluid.html)
- Peele, 2013 S. Peele; Truth and reconciliation for alcoholism: Retract anti-harm reduction article in science; (2013) (Available at http://www.huffingtonpost.com/stanton-peele/alcoholism_b_3559263.html, September 11)
- Peele, 2015 S. Peele; Why neurobiological models can't contain mental disorder and addiction; The Behavior Therapist, 38 (7) (2015), pp. 218–222
- Peele, 2016 S. Peele; Why pretty much the only reasonable voice on drug policy in the federal government is Obama; The Alternet (2016) (Available at http://www.alternet.org/drugs/only-reasonable-voice-drug-policy-government-obama, May 5)
- Peele and Thompson, 2015 S. Peele, I. Thompson; Recover!: An empowering program to help you stop thinking like an addict and reclaim your life; (Paperback ed.) Da Capo, Berkeley (2015)
- Pendery et al., 1982 M.L. Pendery, I.M. Maltzman, L.J. West; Controlled drinking by alcoholics? New findings and a reevaluation of a major affirmative study; Science, 217 (4555) (1982), pp. 169–175 (Available at http://www.ncbi.nlm.nih.gov/pubmed/7089552)
- Rudd et al., 2016 R.A. Rudd, N. Aleshire, J.E. Zibbell, R.M. Gladden; Increases in drug and opioid overdose deaths — United States, 2000–2014; Morbidity and Mortality Weekly Report, 64 (50) (2016), pp. 1378–1382 (Available at http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6450a3.htm?s_cid = mm6450a3_w, January 1)
- Volkow, 2015 N. Volkow; Addiction is a disease of free will; Huffington Post (2015) (Available at http://www.huffingtonpost.com/nora-volkow/addiction-is-a-disease-of_b_7561200.html, June 12)
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?