Keywords
QRS duration;Ventricular arrhythmias;30 day mortality;ST elevation myocardial infarction
Studies have demonstrated an association between QRS duration and long term mortality after myocardial infarction [1] ; [2].
However, there remains a scarcity of data on QRS duration after ST elevation myocardial infarction (STEMI) and its association with mortality. We investigated whether QRS duration during STEMI hospitalization could predict 30-day and one year mortality. A secondary objective was to determine the relationship between prolonged QRS and occurrence of inpatient ventricular arrhythmias.
Five hundred and fifty three patients admitted to Einstein Medical Center, Philadelphia from August 1, 2006 to August 31, 2011 with a diagnosis of STEMI were screened. The study protocol was approved by our Institutional Review Board. The author(s) of this manuscript have certified that they comply with the principles of ethical publishing in the International Journal of Cardiology.
STEMI was diagnosed on the basis of cardiac symptoms and electrocardiographic changes consisting of ST elevation in two contiguous leads in accordance with the guidelines [3].
Patients with any of the following were excluded:
- Known prior QRS duration ≥ 100 ms
- Bundle branch block
- Paced rhythm on admission
- Patients with incomplete data set.
All EKGs from the time of presentation to the time of discharge/death of the patient, as well as telemetry data, were reviewed to determine the QRS duration on admission and the development of inpatient ventricular arrhythmias (ventricular tachycardia (VT) and ventricular fibrillation (VF)) during that hospital stay.
QRS durations from fifty random EKGs were measured by both manual and electronic means and then compared to ascertain accuracy and reliability of the electronic method of collection which was eventually used for EKG measurements (R2 = 0.96, P < 0.0001).
Data on patient demographics and clinical characteristics, baseline hemodynamic parameters, ejection fraction, obtained from transthoracic echocardiogram reports, and type of intervention done (percutaneous coronary intervention (PCI) or coronary artery bypass graft (CABG)) were collected.
Mortality at 30 days and one year was determined from hospital records and the publically accessed social security death index website.
The study population was divided into two groups; QRS < 100 ms and QRS ≥ 100 ms. The cut-off of 100 ms was used because it yielded the highest accuracy on analysis. Baseline characteristics of each group were compared using independent-sample t tests for continuous variables and chi-square or Fishers exact test for discrete variables. Multivariate Cox proportional hazards regression models were used to evaluate independent predictors of mortality. Kaplan–Meier method was used for generating survival curves and compared using the log-rank test. The effect of each variable was expressed as an odds ratio (OR) and confidence interval (CI). A p value < 0.05 was considered statistically significant. Statistical analyses were performed using SPSS, version 22.
The final cohort consisted of 449 patients with mean age of 61 ± 14 years, 41% were female and the average QRS duration was 96 ± 23 ms. During hospitalization, 13.3% of patients with QRS ≥ 100 ms on admission had an episode of VT compared to 4.9% of those with a QRS < 100 ms (p = 0.01). Likewise those with a QRS ≥ 100 ms had slightly more episodes of VF compared to those with a QRS < 100 ms though it was not statistically significant (17.1% and 16.0% respectively; p = 0.760).
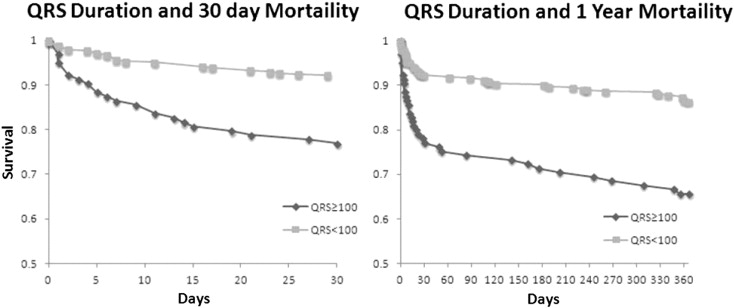
Multivariate analysis revealed that patients with a QRS duration ≥ 100 ms had increased 30-day mortality (HR = 2.30, 95% CI 1.2–4.3; p < 0.01) and 1 year mortality (HR = 2.28, 95% CI 1.4–3.8; p < 0.01) (Table 1) compared to patients with QRS duration < 100 ms (TIMI score variables, ejection fraction, chronic kidney disease, hypotension and tachycardia on presentation were adjusted). They also had an increased occurrence of VT (OR = 3.49, 95% CI 1.6–7.5; p < 0.01) but not VF (OR = 1.01, 95% CI 0.5–1.9; p = 0.97). Kaplan–Meier curve stratified by QRS duration ≥ 100 ms versus QRS duration < 100 ms showed that there was an increase in 30 day and one year mortality in patients that had prolonged QRS duration (Fig. 1).
| HR (95% CI) | P value | |
|---|---|---|
| 30 day mortality | ||
| QRS duration on admission | 2.29 (1.23–4.29) | < 0.01 |
| Age | 1.04 (1.02–1.07) | < 0.01 |
| Percutaneous coronary intervention | 0.44 (0.24–0.81) | < 0.01 |
| Tachycardia | 2.64 (1.39–5.04) | < 0.00 |
| 1 year mortality | ||
| QRS duration on admission | 2.28 (1.38–3.76) | < 0.01 |
| Age | 1.03 (1.01–1.05) | < 0.01 |
| Hypertension | 2.39 (1.14–5.02) | 0.02 |
| Percutaneous coronary intervention | 0.43 (0.26–0.69) | < 0.01 |
| Tachycardia | 1.90 (1.11–3.25) | 0.00 |
| Hypotension | 2.77 (1.43–5.36) | < 0.01 |
|
|
|
Fig. 1. Kaplan–Meier survival estimates of 30 day mortality and 1 year mortality. |
The QRS duration which has recently found its place in determining those patients with heart failure that might benefit from cardiac resynchronization therapy [4], has been underutilized in the prognostication of patients that might do poorly post-MI.
There has been controversy over whether QRS duration alone can predict the development of arrhythmias post-infarction. One study concluded that QRS duration cannot be used as a standalone predictor of arrhythmias post-infarction, however most patients in this study had MI that occurred more than six months prior to the time of enrollment into the study [5]. On literature review there was no study found that specifically addressed the relationship between QRS prolongation at the time of MI hospitalization and short term mortality or in-patient ventricular arrhythmias after STEMI.
In this study, multivariate analysis demonstrated that patients with QRS duration ≥ 100 ms admitted with STEMI have a 2.3 fold increase in 30 day mortality compared to those with a QRS duration < 100 ms.
Several studies have hypothesized that post-MI QRS prolongation might be due to scar tissue formation affecting the conduction system, which could predispose to reentry and ultimately dangerous ventricular arrhythmias [6]; [7] ; [8]. Another study hypothesized that the association of QRS prolongation post-STEMI and increased long-term mortality might be due to late potentials that are large enough to affect the surface EKG, suggesting extensive infarcts and involvement of the interventricular conduction system [9]. The ability of the QRS duration to predict 30 day mortality, found in the present study, may be useful in stratifying patients into a group that requires more aggressive care; for example, being discharged with a life vest to protect against ventricular arrhythmias post-STEMI and hence sudden death, versus those that may only require routine monitoring.
The limitations we had included difficulty to determine cause of death after a patient leaves the hospital hence 30 day mortality was all cause mortality which is less reliable in demonstrating a direct cause and effect relationship. STEMI patients were placed on guideline directed therapy that may have affected the QRS duration. Finally, our subject population was predominantly black which might limit generalizing our results to other populations.
QRS duration ≥ 100 ms is an independent predictor of 30-day and one year mortality and in-patient ventricular tachycardia after STEMI. QRS duration should be considered in further STEMI risk stratification and aggressive arrhythmia management.
Disclosures
No conflicts of interest.
References
- [1] F. Baslaib, S. Alkaabi, A.T. Yan, R.T. Yan, P. Dorian, K. Nanthakumar, et al.; QRS prolongation in patients with acute coronary syndrome; Am Heart J, 159 (4) (Apr 2010), pp. 593–598
- [2] V. Kalahasti, V. Nambi, D.O. Martin, C.T. Lam, D. Yamada, B.L. Wilkoff, et al.; QRS duration and prediction of mortality in patients undergoing risk stratification for ventricular arrhythmias; Am J Cardiol, 92 (7) (Oct 2003), pp. 798–803
- [3] P.T. O'Gara, et al.; ACCF/AHA Guideline for the Management of ST-Elevation Myocardial Infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines; Circulation, 127 (2013), pp. e362–e425 [December 2012]
- [4] A.J. Moss, M.W. Brown, D.S. Cannom, J.P. Daubert, M. Estes, E. Foster, et al.; Multicenter Automatic Defibrillator Implantation Trial-Cardiac Resynchronization Therapy (MADIT-CRT): design and clinical protocol; Ann Noninvasive Electrocardiol, 10 (Oct 2005), pp. 34–43
- [5] A.E. Buxton, M.O. Sweeney, M.S. Wathen, M.E. Josephson, M.F. Otterness, E. Hogan-miller, et al.; QRS duration does not predict occurrence of ventricular tachyarrhythmias in patients with implantable cardioverter-defibrillators; J Am Coll Cardiol, 46 (2005), pp. 310–316
- [6] M.C. Tjandrawidjaja, Y. Fu, C.M. Westerhout, G.S. Wagner, C.B. Granger, P.W. Armstrong, et al.; Usefulness of QRS score as a strong prognostic marker in patients discharged after undergoing primary PCI for STEMI; Am J Cardiol, 106 (5) (Sep 1 2010), pp. 630–634
- [7] T. Horwich, S.J. Lee, L. Saxon; Usefulness of QRS prolongation in predicting risk of inducible monomorphic ventricular tachycardia in patients referred for electrophysiologic studies; Am J Cardiol, 92 (7) (Oct 1 2003), pp. 804–809
- [8] D.P. Zipes; Cardiac electrophysiology: promises and contributions; J Am Coll Cardiol, 13 (1989), pp. 1329–1352
- [9] W.R. Hathaway, D.E. Peterson, G.S. Wagner, C.B. Granger, K.M. Zabel, K.S. Pieper, et al.; Prognostic significance of the initial electrocardiogram in patients with acute myocardial infarction; JAMA, 279 (1998), pp. 387–391
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?