Abstract
Background
Minimal persistent inflammation (MPI) contributes to hyperreactivity in allergic rhinitis. However, little is known regarding whether pre-onset activation of eosinophils and mast cells is present or not in Japanese cedar pollinosis (JCP). Furthermore, a prophylactic effect of intranasal corticosteroids on such MPI in JCP has not been investigated.
Methods
We designed a double-blinded, randomized, placebo-controlled, crossover trial. Twenty patients with JCP were examined outside the pollen season (UMIN000008410). Nasal provocation with paper discs containing extracts of Japanese cedar pollen was performed once a day for 3 consecutive days. Onset of nasal symptoms was monitored over 15 min after each provocation. The levels of eosinophil cationic protein (ECP) and tryptase in nasal secretions were examined. Fluticasone furoate nasal spray or placebo treatment was started one day before the first provocation.
Results
In the placebo group, 25% of the patients showed onset of nasal symptoms following provocation on the first day. In addition, 75% and 68% of the patients showed symptom onset on the second and third day of provocation, respectively. After the first provocation, the levels of ECP and tryptase in nasal secretions were significantly increased. These increases were seen not only in symptomatic but also in asymptomatic subjects in response to provocation, and the levels were similar between these subjects. Prophylactic treatment with fluticasone significantly suppressed the increase in nasal ECP and tryptase associated with repeated provocations.
Conclusions
These results suggest that pre-onset activation of eosinophils and mast cells is present in experimental JCP, and that prophylactic treatment with intranasal corticosteroids has the potential to control such activation.
Keywords
Eosinophil cationic protein; Intranasal corticosteroids; Japanese cedar pollinosis; Minimal persistent inflammation; Tryptase
Abbreviations
AR, allergic rhinitis; ECP, eosinophil cationic protein; FFNS, fluticasone furoate nasal spray; INS, intranasal corticosteroids; JCP, Japanese cedar pollinosis; MPI, minimal persistent inflammation
Introduction
In allergic rhinitis (AR), minimal persistent inflammation (MPI) is characterized by an influx of inflammatory cells such as eosinophils and neutrophils into the nasal mucosa without the onset of nasal symptoms following exposure to low levels of allergen.1 MPI was originally described after the end of symptoms in both perennial and seasonal allergic rhinitis.2 and 3 It has been suggested that MPI is also present in the initial dispersion of pollen prior to onset of symptoms, which contributes to hyperreactivity and subsequently to onset of full-scale symptoms; however, the precise characterization and clinical implication of this “pre-onset” MPI remains to be elucidated.1, 3 and 4
Prophylactic, in other words early interventional or initial, treatment starting immediately after pollen release or the onset of symptoms is recommended in patients who annually experience substantial symptoms of pollen-induced seasonal allergic rhinitis.5 Placebo-controlled studies confirmed that anti-histamines, anti-leukotrienes and intranasal corticosteroids (INS) are effective for prophylactic treatment in pollinosis.6, 7 and 8 Of these medications, prophylactic treatment with INS has been shown to delay onset and reduce symptom severity.1, 7, 8, 9 and 10 For example, we reported that prophylactic treatment with mometasone furoate nasal spray did not induce the substantial onset of pollinosis, whereas placebo treatment did, in the relatively low pollen dispersal season in Japanese cedar pollinosis (JCP), the most prevalent seasonal allergic rhinitis in Japan.9 In addition, we have recently demonstrated that this prophylactic treatment significantly delayed the onset of symptoms and alleviated symptom severity compared not only with placebo but also with post-onset treatment with mometasone in the relatively high pollen dispersal season.10 One of the bases of prophylactic treatment is the control of pre-onset MPI; however, little is known regarding how INS controls pre-onset MPI.
In the present study, we sought to determine whether pre-onset activation of eosinophils and mast cells exists in experimental JCP. In addition, the efficacy of INS for this pre-onset activation was investigated. These results provide a basis for understanding the clinical implications of INS for prophylactic treatment in seasonal AR.
Methods
Patients
Twenty patients with JCP, between the ages of 22 and 52 years (mean 35.3 ± 10.4 years; 6 males and 14 females) were enrolled. All the patients had at least a 2-year history of JCP and were asymptomatic out of the pollen season. Sensitization to Japanese cedar pollen was assessed by a skin prick test. Patients were excluded from the study if they had: (a) sensitization to house dust mite assessed by a skin prick test, (b) concomitant sinonasal disease that could potentially affect the outcome of the trial (e.g., nasal polyps, rhinosinusitis, nasal septum deviation); (c) rhinitis medicamentosa and non-infectious, non-allergic rhinitis; (d) cedar pollen-specific immunotherapy; (e) sinonasal surgery including laser vaporization of inferior turbinates within 1 year; (f) medication with anti-allergic drugs including antihistamines, chromones, glucocorticoids and decongestants within 2 weeks of study initiation; (g) hypersensitivity to fluticasone furoate nasal spray; (h) systemic infection including mycosis; or (i) were pregnant and breastfeeding. Prior to the study initiation, we estimated the sample size that would be required based on the mean and standard deviation in the groups reported in our previous studies.9 and 10
Study design
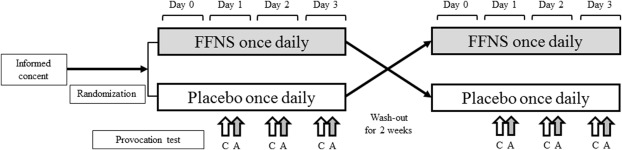
The study was a single-center, double-blinded, randomized, placebo-controlled, crossover trial that was carried out in August, outside the Japanese cedar pollen season (Fig. 1). Allocation concealment was granted by the central registry and computer-generated block randomization. The control nasal provocation, followed by active allergen provocation with a 15 min interval, was given for 3 consecutive days. The allergen provocation test was performed by placing two paper discs (Torii Pharmaceutical, Tokyo, Japan) containing the Japanese cedar pollen extract that is used for skin scratch tests (14.7 μg in 5 μl per disc, Torii), to the surface of the bilateral inferior turbinates for 5 min. Control discs contained 5 μl of the control solution used for the scratch test (Torii Pharmaceutical). After 5 min, the discs with adsorbed nasal secretions were removed, placed into a 1.5 ml micro test tube (Eppendorf AG, Hamburg, Germany), and stored at −80 °C until assayed. The subjects were monitored for 15 min as to whether they showed an onset of nasal symptoms such as sneezing, itching, rhinorrhea and nasal congestion in response to nasal provocation. Fluticasone furoate nasal spray (FFNS: 55 μg per nostril once a day in the morning) or the placebo spray was administered to the subjects starting from one day prior to the first provocation. The placebo spray provided by GlaxoSmithKline K.K. had a white-colored lid and trigger. The lid and trigger of the FFNS bottle, which were initially cyan-colored, were changed to white to ensure that both FFNP and placebo spray appeared the same. This treatment was continued until the third provocation (4 days in total). Wash-out periods of 2 weeks were instituted between the treatments (Fig. 1). The study was approved by the Institutional Review Board of Okayama University Graduate School of Medicine, Dentistry and Pharmaceutical Sciences (Rinri-1436), and is registered in UMIN (UMIN000008410). Prior to participation in the study, all patients provided written informed consent.
|
|
|
Fig. 1. Study design. Subjects received a nasal provocation test with control discs (C) followed by allergen discs (A) for 3 consecutive days. Fluticasone furoate nasal spray (FFNS) or a placebo spray was given to the subjects starting from one day prior to the first provocation. After wash-out for 2 weeks, a crossover trial was performed. |
Measurement of nasal ECP and tryptase
The discs were soaked overnight at 4 °C in 0.8 ml of Dulbeccos phosphate buffered saline (Invitrogen, Grand Island, NY, USA) with gentle rotation. Levels of ECP and tryptase were determined by ImmunoCAP ECP and ImmunoCAP tryptase, respectively (Phadia, Uppsala, Sweden). The detection limit of the assay for ECP and tryptase was 2 ng/ml and 1 ng/ml, respectively.
Statistical analysis
Values are expressed as the median value. A non-parametric Mann–Whitney U test and Fishers exact probability test were used to compare the data between groups, while the Wilcoxon signed rank test was used for analysis within the groups. Statistical analyses were performed using SAS (Statistical Analysis System) version 9.2, with P < 0.0.5 considered to be significant.
Results
Release of ECP and tryptase in nasal secretions following allergen provocation in the placebo treatment group
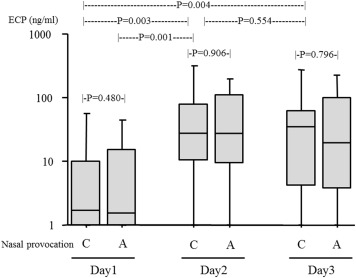
In the groups treated with placebo, the levels of ECP in nasal secretions extracted from the paper discs remained unchanged 5 min after each provocation. However, the baseline levels of ECP determined in the control disc of the second day (P = 0.003) and third day (P = 0.004) provocations were significantly increased compared to the baseline ECP on the first day of provocation, suggesting that exposure to Japanese cedar pollen induced release of ECP ( Fig. 2).
|
|
|
Fig. 2. Levels of nasal ECP following repeated nasal provocation with Japanese cedar pollen extract in subjects treated with placebo. Control discs (C) followed by allergen discs (A) were placed on the surface of the bilateral inferior turbinates for 5 min with a 15 min interval. This provocation was given for 3 consecutive days. Levels of ECP in nasal secretions adsorbed to the discs were determined. The rectangle includes the range from the 25th to the 75th percentiles; the horizontal line indicates the median, and the vertical line indicates the range from the 10th to the 90th percentiles. P values were determined using the Wilcoxon signed rank test. |
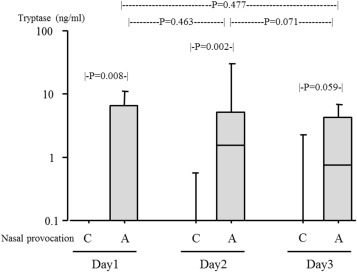
A significant increase in the levels of tryptase was seen 5 min after the first day provocation (P = 0.008). However, unlike the ECP response, the tryptase levels returned to the baseline prior to the active provocation on the second day. The tryptase response on the second and third day provocations was similar to that on the first day of provocation ( Fig. 3).
|
|
|
Fig. 3. Levels of nasal tryptase following repeated nasal provocation with Japanese cedar pollen extract in subjects treated with placebo. Control discs (C) followed by allergen discs (A) were placed on the surface of the bilateral inferior turbinates for 5 min with a 15 min interval. This provocation was given for 3 consecutive days. Levels of tryptase in nasal secretions adsorbed to the discs were determined. The rectangle includes the range from the 25th to the 75th percentiles; the horizontal line indicates the median, and the vertical line indicates the range from the 10th to the 90th percentiles. P values were determined using the Wilcoxon signed rank test. |
Onset of nasal symptoms after allergen provocation for 3 consecutive days in the placebo treatment group
Fifteen minutes after the first provocation, 5 out of 20 (25%) patients treated with placebo showed an onset of nasal symptoms. In addition, 15 (75%) and 14 (68%) patients showed symptom onset after the second and third day provocation, respectively. No significant differences in age, sex, a history of smoking or complications including bronchial asthma, aspirin intolerance, perennial rhinitis, atopic dermatitis, food allergy and drug allergies were found between patients showing positive (symptomatic, group A, n = 5) and negative (asymptomatic, group B, n = 15) response to the first allergen provocation (Table 1).
| Group A | Group B | ||
|---|---|---|---|
| Number | 5 | 15 | |
| Age (mean ± SD) | 33.8 ± 6.6 | 35.4 ± 11.3 | |
| Sex (male/female) | 1/4 | 5/10 | |
| History of smoking | 0/5 | 0/15 | |
| Complications | Bronchial asthma | 0/5 | 0/15 |
| Aspirin intolerance | 0/5 | 0/15 | |
| Perennial rhinitis | 0/5 | 1/15 | |
| Atopic dermatitis | 2/5 | 4/15 | |
| Food allergy | 0/5 | 0/15 | |
| Drug allergies | 1/5 | 0/15 | |
Results were shown as mean ± standard deviation.
Levels of ECP and tryptase after the first day provocation in symptomatic and asymptomatic patients
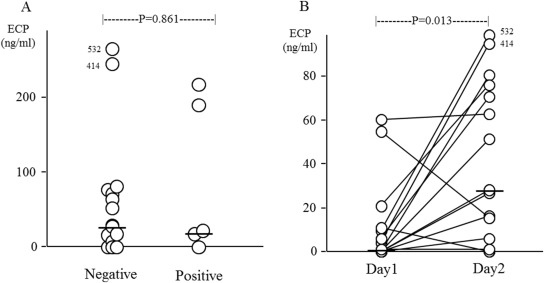
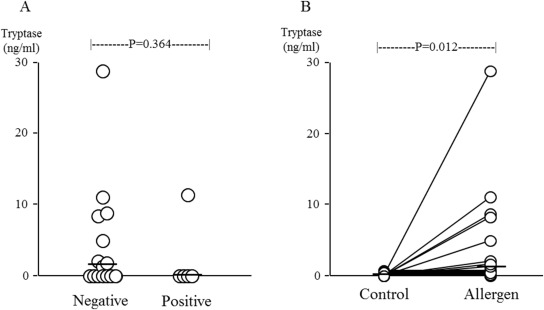
We next focused on analysis of ECP and tryptase levels in the patients that showed a negative or a positive response to the first day provocation. Nasal ECP and tryptase levels in the control and active (pollen) disc on the first, second, and third day in each group were shown in Table 2. Levels of ECP in the control disc on the second day were similar between the groups (Fig. 4A, P = 0.861). In addition, significant elevation in the levels of ECP was seen in asymptomatic patients on day 2 compared to day 1 ( Fig. 4B, P = 0.013). Levels of tryptase in the allergen disc on the first day were also similar between symptomatic and asymptomatic patients ( Fig. 5A, P = 0.364). In addition, significant elevation in the levels of tryptase was seen in the allergen discs of asymptomatic patients compared to the control discs ( Fig. 5B, P = 0.012).
| Day 1 | Day 2 | Day 3 | ||||||
|---|---|---|---|---|---|---|---|---|
| C | A | C | A | C | A | |||
| ECP (ng/ml) | Group A (n = 5) | Placebo | 2.46 | 0 | 20.43 | 18.32 | 28.38 | 12.04 |
| FFNS | 0 | 0 | 4.65 | 0 | 0 | 1.07 | ||
| P value | 0.109 | 0.180 | 0.068 | 0.465 | 0.109 | 0.109 | ||
| Group B (n = 15) | Placebo | 0 | 2.24 | 28.27 | 28.20 | 40.99 | 26.84 | |
| FFNS | 0 | 3.00 | 4.00 | 3.20 | 0 | 3.33 | ||
| P value | 0.441 | 0.059 | 0.023 | 0.023 | 0.001 | 0.015 | ||
| Typtase (ng/ml) | Group A (n = 5) | Placebo | 0 | 0 | 0 | 0 | 0 | 0 |
| FFNS | 0 | 0 | 0 | 0 | 0 | 1.31 | ||
| P value | – | 0.180 | – | 0.180 | 0.317 | 0.285 | ||
| Group B (n = 15) | Placebo | 0 | 1.35 | 0 | 2.42 | 0 | 1.40 | |
| FFNS | 0 | 0 | 0 | 0 | 0 | 0 | ||
| P value | – | 0.038 | 0.180 | 0.074 | 0.655 | 0.009 | ||
Effect of the treatment with FFNS was also shown. P values were determined using Wilcoxons signed rank test.
|
|
|
Fig. 4. Nasal ECP levels following a single allergen provocation. (A) Nasal ECP levels in the control disc on the second day in patients with negative (n = 15) or positive (n = 5) response to the first provocation were compared. The bar represents the median value. P values were determined using the Mann–Whitney U test. (B) Changes in nasal ECP levels in the control disc between the first and second day were determined in patients with a negative response to the first provocation. The bar represents the median value. P values were determined using Wilcoxons signed rank test. |
|
|
|
Fig. 5. Nasal tryptase levels following a single allergen provocation. (A) Nasal tryptase levels in the allergen disc on the first day were compared between patients with a negative (n = 15) or a positive (n = 5) response to the first provocation. The bar represents the median value. P values were determined using the Mann–Whitney U test. (B) Changes in nasal tryptase levels between the control and allergen discs on the first day were determined in asymptomatic patients in response to a single provocation. The bar represents the median value. P values were determined using Wilcoxons signed rank test. |
Effect of prophylactic treatment of FFNS on ECP and tryptase release
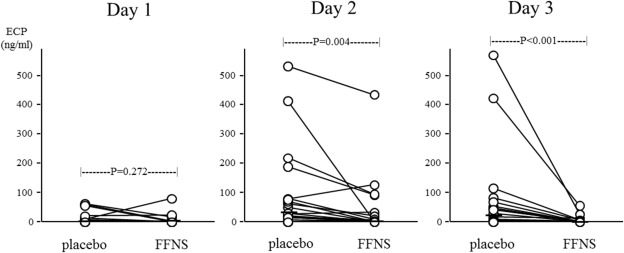
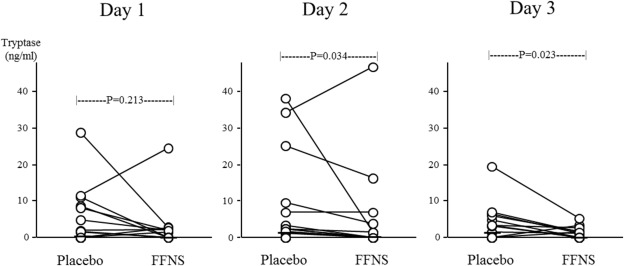
Prophylactic treatment with FFNS did not inhibit the release of ECP on the first day provocation as compared with the placebo treatment due to a small release even in the placebo treatment. However, a significant decrease in ECP levels was seen in control discs on the second (P = 0.004) and third (P < 0.001) day provocation in FFNS treatment as compared with the placebo treatment ( Fig. 6). Significant inhibition of tryptase levels by FFNS treatment was also seen in allergen discs on the second (P = 0.034) and third (P = 0.023) day provocation ( Fig. 7). The effect of the treatment with FFNS on ECP and tryptase levels after the first, second, and third provocation in each group (A and B) was shown in Table 2. The onset rate of nasal symptoms was not significantly different between placebo and FFNS treatment in the group of patients (n = 5) showing positive response to the first provocation (P = 0.083, P = 0.222 and P = 0.444 at the first, second and third provocation, respectively). Similar findings were seen in the group of patients (n = 15) showing negative response to the first provocation (P = 0.112, P = 0.231 and P = 0.233 at the first, second and third provocation, respectively).
|
|
|
Fig. 6. Effect of prophylactic treatment with fluticasone furoate on nasal ECP levels following repeated allergen provocations. One day prior to the first provocation, the subjects received the fluticasone furoate nasal spray (FFNS) or the placebo spray. ECP levels in nasal secretion adsorbed to the control discs were compared between FFNS and placebo treatment. The bar represents the median value. P values were determined using Wilcoxons signed rank test. |
|
|
|
Fig. 7. Effect of prophylactic treatment with fluticasone furoate on nasal tryptase levels following repeated allergen provocations. The subjects received FFNS or the placebo spray one day prior to the first provocation. Tryptase levels in nasal secretions adsorbed to the allergen discs were compared between FFNS and placebo treatment. The bar represents the median value. P values were determined using Wilcoxons signed rank test. |
Discussion
In the present study, we demonstrated that ECP and tryptase were released into nasal secretions not only in symptomatic but also in asymptomatic patients with JCP following a single allergen provocation outside the pollen season. In addition, treatment with fluticasone that was started one day prior to the first provocation significantly suppressed the increase in nasal ECP and tryptase that occurred with repeated provocations. We and others have reported that prophylactic treatment with INS is effective for pollinosis.7, 9 and 10 The present results suggest that the prophylactic effect of INS on pollinosis is mediated by the suppression of pre-onset activation of eosinophils and mast cells.
In contrast to the originally described MPI that is seen after the end of symptoms, little is known about “pre-onset” MPI and its regulation. Ricca et al. were the first to demonstrate increases in eosinophils, neutrophils and ICAM-1 expression prior to the initial onset of nasal symptoms, which were clinically evident in patients with birch pollinosis only after pollen counts increased dramatically. 3 Several studies investigated MPI in seasonal allergic rhinitis using a nasal provocation test with allergen. 4 and 11 Juliusson et al. demonstrated an increase in eosinophils and mast cells in asymptomatic patients with strictly seasonal allergic rhinitis to timothy pollen following a single allergen provocation; however, all patients displayed nasal symptoms following the provocation. 11 Roquet et al. demonstrated that although 7 days of exposure to birch pollen allergen at low doses outside the pollen season caused few symptoms, it produced increased ECP but not histamine in lavage fluid from patients with seasonal allergic rhinitis. 4 Our results were consistent with this report by Roquet et al. in terms of ECP release by asymptomatic patients, and further demonstrated that pre-onset activation of eosinophils and mast cells can be induced even after a single allergen provocation.
On the other hand, unlike the observation by Roquet et al. in which no or minimal symptoms were observed, we found that 25% of the patients showed an onset of nasal symptoms after a single provocation. These different results may be due to the difference in the allergen dose used for provocation. The allergen dose set by Rousquet et al. was approximately 1/100 of the cumulative dose until symptoms of itching and sneezing occurred for each individual. 4 We used two paper discs containing a Japanese cedar pollen extract that is used for skin scratch tests (14.7 μg of protein in 5 μl per disc) for provocation. Our dose may be higher than that set by Roquet et al.
In the present study, nasal ECP and tryptase were monitored as specific markers for the activation of eosinophils and mast cells, respectively.12 Previous studies reported that elevation of nasal ECP levels is mainly seen in the late-phase response and is sometimes seen in the early-phase response following allergen provocation.13, 14, 15 and 16 The present study showed that a significant elevation of nasal ECP was seen at 24 h but not at 5 min after a single allergen provocation, suggesting that ECP release is mainly seen in the late-phase response in this experimental model. This result is similar to the report by Raulf-Meimsoth et al.15 They measured nasal ECP at 30 min, 2, 6 and 24 h after nasal provocation and found a significant elevation of nasal ECP that started at 2 h after provocation and lasted for 24 h. Together with the finding that the elevation of nasal ECP was seen not only in symptomatic but also in asymptomatic subjects, these results suggest a pre-onset activation of eosinophils following exposure to Japanese cedar pollen.
On the other hand, despite it can be speculated that the accumulation of eosinophils is enhanced by repeated stimulation with allergen, the reason why the baseline levels of ECP between the second day and the third day was not significant (P = 0.554) is not clear. Future evidences should be provided whether not only the activation but also the accumulation of eosinophils in nasal secretions is induced in this experimental model.
Tryptase is a neutral protease that is selectively released from mast cells.17 Previous studies demonstrated that nasal tryptase in nasal secretions or lavages are increased in the early phase but not in the late phase response following nasal provocation with allergens.14, 15 and 16 The present study showed that a significant elevation of nasal tryptase was seen at 5 min but not at 24 h after a single allergen provocation. This result is consistent with the previous reports.14, 15 and 16 Similar to ECP, the elevation of nasal tryptase was seen not only in symptomatic but also in asymptomatic subjects, suggesting that an induction of early-phase minimal inflammation with mast cells occurs following exposure to Japanese cedar pollen. Mast cells also contribute to late-phase responses through upregulation of cytokines and chemokines including GM-CSF, RANTES, eotaxins and TRAC.18 Although a specific marker of mast cell activation in late-phase responses has not been available, future investigation should determine whether mast cells contribute to “pre-onset” persistent inflammation in pollinosis.
The present study demonstrated that repeated nasal allergen provocations increased the rate of onset of nasal symptoms. This result is consistent with previous reports that demonstrated that repeated allergen provocations during out of pollen season decrease the threshold for nasal symptoms in pollinosis.19 and 20 On the other hand, the present study may be the first report to show the existence of MPI characterized by the activation of eosinophils and mast cells prior to the onset of nasal symptoms in repeated allergen provocation tests. Priming effect was originally called by Connell that the number of allergen required to elicit a positive nasal symptom was reduced by 10- to 100-fold when a second challenge was repeated to the following day.21 Strictly speaking, although priming effect and pre-onset activation of eosinophils and mast cells share common pathological characteristics, they are different in terms of the presence or absence of nasal symptoms.
Intranasal glucocorticosteroids (INS) are the most effective drugs for controlling AR-caused inflammation.22 It is well known that INS suppress the release of ECP and tryptase into nasal secretions.23 and 24 For example, Di Lorenzo et al. showed that treatment with fluticasone propionate aqueous nasal spray significantly reduces the levels of ECP and tryptase in nasal lavage whereas placebo treatment does not. 23 In terms of prophylactic treatment with INS, Ahlstrom-Emanuelsson et al. showed that prophylactic treatment with budesonide significantly suppresses histamine-induced release of ECP and tryptase in nasal saline lavage. 24 We also reported that prophylactic treatment with mometasone furoate suppressed the levels of ECP in nasal secretion as compared with placebo treatment during the peak season of Japanese cedar pollen in patients with JCP.9 The anti-inflammatory effect of glucocorticoids is due to the down-regulation of pro-inflammatory genes via several mechanisms including an effect on the protein–protein interactions that sequester protein kinase A and CREB-binding protein from NF-κB. 25 and 26 The interaction between NF-κB, CREB, and the CREB-binding protein leads to the acetylation of chromatin and the subsequent transcription of proinflammatory genes, such as the genes encoding cytokines, inflammatory enzymes, adhesion molecules and inflammatory receptors.27 Thus prophylactic use of INS may be more effective than post-onset use in controlling inflammation where the activity of NF-κB is relatively lower than that in the peak pollen season. In fact, Table 2 showed that significant reductions in the levels of ECP and tryptase were seen by the treatment with FFNS as compared with placebo in asymptomatic patients (Group B) but not symptomatic patients (Group A). However, this may be due to the small number of patients in Group A (n = 5).
In conclusion, activation of eosinophils and mast cells was seen in asymptomatic patients with JCP after a single allergen provocation, and prophylactic use of INS was effective in inhibiting this activation. These results suggest that the prophylactic effect of INS on JCP is mediated by the suppression of pre-onset activation of eosinophils and mast cells. Future investigation should consider whether other inflammatory cells including lymphocytes and dendritic cells, as well as constitutive cells including epithelial cells and fibroblasts, contribute to pre-onset activation of eosinophils and mast cells.
Conflict of interest
MO has received lecture fees from GSK and MSD. The rest of the authors have no conflict of interest.
Authors' contributions
YN, MO and KN designed the study and wrote the manuscript. TF, SK, SM and THa contributed to data collection. KK and THi performed the statistical analysis and interpretation of the results.
Acknowledgments
The authors would like to thank Yuko Okano for her editorial assistance. This work was supported in part by grants from Ministry of Education, Culture, Sports, Science and Technology of Japan (25861563).
References
- 1 G.W. Canonica, E. Compalati; Minimal persistent inflammation in allergic rhinitis: implications for current treatment strategies; Clin Exp Immunol, 158 (2009), pp. 260–271
- 2 G. Ciprandi, S. Buscaglia, G. Pesce, C. Gronzato, V. Ricca, S. Pamiani, et al.; Minimal persistent inflammation is present at mucosal level in patients with asymptomatic rhinitis and mite allergy; J Allergy Clin Immunol, 96 (1995), pp. 971–979
- 3 V. Ricca, M. Landi, P. Ferrero, A. Bairo, C. Tazzer, G.W. Canonica, et al.; Minimal persistent inflammation is also present in patients with seasonal allergic rhinitis; J Allergy Clin Immunol, 104 (1999), pp. 54–57
- 4 A. Roquet, M. van Hage-Hamsten, G. Hallden, O. Zetterstrom; Allergen-induced inflammation in the nose: a comparison of acute and repeated low-dose allergen exposure; Allergy, 51 (1996), pp. 42–48
- 5 K. Okubo, Y. Kurono, S. Fujieda, S. Ogino, E. Uchio, H. Odajima, et al.; Japanese guideline for allergic rhinitis 2014; Allergol Int, 63 (2014), pp. 357–375
- 6 T. Yamada, H. Saito, S. Fujieda; Present state of Japanese cedar pollinosis: the national affliction; J Allergy Clin Immunol, 133 (2014), pp. 632–639
- 7 D. Graft, D. Aaronson, P. Chervinsky, H. Kaiser, J. Melamed, A. Pedinoff, et al.; A placebo– and active-controlled randomized trial of prophylactic treatment of seasonal allergic rhinitis with mometasone furoate aqueous nasal spray; J Allergy Clin Immunol, 98 (1996), pp. 724–731
- 8 M.C. Morelli, S. Bordonaro, L. Hedbys, S. Romagnani, the Italian Study Group; Effect of pre-seasonal and seasonal treatment with budesonide topical nasal powder in patients with seasonal allergic rhinitis; Allergol Int, 45 (1996), pp. 151–157
- 9 S. Makihara, M. Okano, T. Fujiwara, M. Kimura, T. Higaki, T. Haruna, et al.; Early interventional treatment with intranasal mometasone furoate in Japanese cedar/cypress pollinosis: a randomized placebo-controlled trial; Allergol Int, 61 (2012), pp. 295–330
- 10 T. Higaki, M. Okano, S. Makihara, T. Fujiwara, T. Haruna, Y. Noda, et al.; Early interventional treatment with intranasal corticosteroids compared with postonset treatment in pollinonsis; Ann Allergy Asthma Immunol, 109 (2012), pp. 458–464
- 11 S. Juliusson, U. Pipkorn, G. Karlsson, L. Enerback; Mast cells and eosinophils in the allergic mucosal response to allergen challenge: changes in distribution and signs of activation in relation to symptoms; J Allergy Clin Immunol, 90 (1992), pp. 898–909
- 12 P. Venge; Monitoring the allergic inflammation; Allergy, 59 (2004), pp. 26–32
- 13 K. Nishioka, C. Saito, T. Nagano, M. Okano, Y. Masuda, T. Kuriyama; Eosinophil cationic protein in the nasal secretions of patients with mite allergic rhinitis; Laryngoscope, 103 (1993), pp. 189–192
- 14 C. de Graaf-in't Veld, I.M. Garrelds, A.W. van Toorenenbergen, R. Gerth van Wijk; Nasal responsiveness to allergen and histamine in patients with perennial rhinitis with and without late phase response; Thorax, 52 (1997), pp. 143–148
- 15 M. Raulf-Heimsoth, C. Wirtz, F. Papenfuss, X. Baur; Nasal lavage mediator profile and cellular composition of nasal brushing material during latex challenge test; Clin Exp Allergy, 30 (2000), pp. 110–121
- 16 J.D. Boot, P. Chandoesing, M.L. de Kam, M.A. Mascelli, A.M. Das, R. Gerth van Wijk, et al.; Applicability and reproducibility of biomarkers for the evaluation of anti-inflammatory therapy in allergic rhinitis; J Inventig Allergol Clin Immunol, 18 (2008), pp. 433–442
- 17 K. Amin; The role of mast cells in allergic inflammation; Respir Med, 106 (2012), pp. 9–14
- 18 R. Pawankar, S. Mori, C. Ozu, S. Kimura; Overview on the pathomechanisms of allergic rhinitis; Asia Pac Allergy, 1 (2011), pp. 186–193
- 19 J.R. Bacon, J.A. McLean, K.P. Mathews, J.M. Banas; Priming of the nasal mucosa by ragweed extract or by an irritant (ammonia); J Allergy Clin Immunol, 67 (1981), pp. 111–116
- 20 H. Yoshida, H. Shimizu, S. Fukami; [Relation between symptom and count of scattering Japanese cedar pollen – examination of clinical observation and repeated provocation]; Arerugi, 45 (1996), pp. 49–61 (in Japanese)
- 21 J. Connell; Quantitative intranasal pollen challenges. II. Efficacy of daily pollen challenge, environmental pollen exposure and placebo challenge on the nasal membrane; J Allergy, 41 (1968), pp. 123–129
- 22 M. Okano; Mechanisms and clinical implications of glucocorticoids in the treatment of allergic rhinitis; Clin Exp Immunol, 158 (2009), pp. 164–173
- 23 G. Di Lorenzo, F. Gervasi, A. Drago, M. Esposito Pellitteri, A. Di Salvo, D. Cosentino, et al.; Comparison of the effects of fluticasone propionate, aqueous nasal spray and levocabastine on inflammatory cells in nasal lavage and clinical activity during the pollen season in seasonal rhinitics; Clin Exp Allergy, 29 (1999), pp. 1367–1377
- 24 C. Ahlstrom-Emanuelsson, M. Andersson, C.G.A. Persson, L. Thorsson, L. Greiff; Effects of topical formoterol alone and in combination with budesonide in a pollen season model of allergic rhinitis; Respir Med, 101 (2007), pp. 1106–1112
- 25 M. Saitoh, R. Takayanagi, K. Goto, A. Fukamizu, A. Tomura, T. Yanase, et al.; The presence of both the amino- and carboxyl-terminal domains in the AR is essential for the completion of a transcriptionally active form with coactivators and intranuclear compartmentalization common to the steroid hormone receptors: a three-dimensional imaging study; Mol Endocrinol, 16 (2002), pp. 694–706
- 26 G. Pascual, C.K. Glass; Nuclear receptors versus inflammation: mechanisms of treasrepression; Trends Endocrinol Metab, 17 (2006), pp. 321–327
- 27 I.M. Adcock, K. Ito, P.J. Barnes; Glucocorticoids: effects on gene transcription; Proc Am Thorac Soc, 1 (2004), pp. 247–254
Note to users: Corrected proofs are Articles in Press that contain the authors' corrections. Final citation details, e.g., volume and/or issue number, publication year and page numbers, still need to be added and the text might change before final publication.
Although corrected proofs do not have all bibliographic details available yet, they can already be cited using the year of online publication and the DOI , as follows: author(s), article title, Publication (year), DOI. Please consult the journals reference style for the exact appearance of these elements, abbreviation of journal names and use of punctuation.
When the final article is assigned to volumes/issues of the Publication, the Article in Press version will be removed and the final version will appear in the associated published volumes/issues of the Publication. The date the article was first made available online will be carried over.
Document information
Published on 05/04/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?