Summary
This case concerns a 10-year-old boy with a history of behavioral abnormality that arrived at our surgical emergency room with acute abdominal discomfort. The boy had acute colitis-like clinical symptoms resulting from ingested and retained foreign bodies in the colon. These foreign bodies (gravel and stones) had accumulated in the entire colon over a period of 1 year. Attempts to dislodge the foreign bodies from the rectum by mechanical means failed; therefore the possibility of surgical intervention was considered in view of the worsening colitis. However, the problem was finally resolved by repeated basketting by colonoscopy, antibiotics and later laxatives. The case is noteworthy because of the extent of the condition, difficulty of the decision-making, and the relative success of watchful conservative measures.
Keywords
colitis;foreign body
1. Case report
A 10-year-old male child, a native of the Lakshadweep islands, now a Kerala resident for the purpose of education, presented to the emergency department with a history of constipation followed by abdominal distension and foul smelling brownish stools mixed with gravel stones, and tenesmus lasting for a duration of 4 days. There was no associated vomiting, oliguria, bleeding from the rectum or features of peritonitis.
His development history revealed a mild delay in attaining speech. He had multiple episodes of inconsolable crying, breath holding, fainting and seizure-like episodes in childhood. His academic performance was poor and was associated with a poor social rapport. A history of multiple episodes of earth-eating since the age of 1.5 years was present.
On presentation his vital signs were stable. His abdomen was tense and distended. There was a palpable lump in the right iliac fossa (6 × 6 cm). Its lower border was not palpable. Bowel sounds were audible, with no hyperperistalitic character. There was mild generalized tenderness over the abdomen. Gravel stones were palpable rectally. Other systems were normal on clinical examination. The attending surgeon attempted to wash out the gravel by giving an enema, which enabled a few gravel stones to come out.
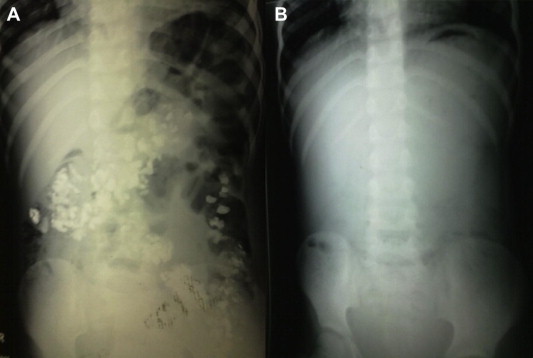
Detailed clinical examination revealed mild pallor. His body mass index (BMI) was 20.5, hemoglobin (Hb) 8.02 g (%) and packed cell volume (PCV) 30.2%. Anemia was corrected by packed cell transfusion. His total leucocyte count (TLC) was elevated (15,600 cells/mm3) with a neutrophilic image (74.5% neutrophils). His electrolyte status and urine output were normal. An erect view X-ray of the abdomen revealed multiple opacities along the line of colon (Fig. 1A). No gas was visualized under the diaphragm. Proctoscopy only was possible, which revealed gravel loaded in the rectum. The stones were difficult to dislodge as they were embedded in crypts of mucosa. Mucosa was ulcerated and edematous. Some of the stones were retrieved with a wire-guided basket (Fig. 2A). The patient was put on antibiotics and was given a high fiber diet. To relieve pain, analgesics were given and the boy was observed for any complications.
|
|
|
Figure 1. (A) Erect X-ray of the abdomen showing gravel inside the large and small bowel; (B) post-treatment erect X-ray of the abdomen showing clearance of the bowel of gravel. |
|
|
|
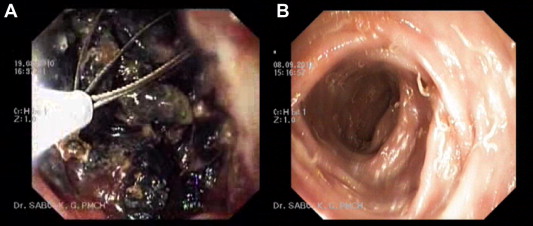
Figure 2. (A) Sigmoidoscopy showing gravel inside the rectum. Ulcerated mucosa and impaction of stones and the wire basket are visible; (B) colonoscopy image after the treatment. Mucosa had reverted back to normal except for worms. |
An ultrasonography (USG) of the abdomen, which was undertaken because of persistence of abdominal distension, revealed a distended colon and rectum. Colonoscopy was attempted again but the scope couldn’t be passed beyond the anal canal due to the stones. Stones were seen embedded in the crypts of mucosa and mucosa was ulcerated. Hence basketting of stones after dislodging from their crypts was attempted, following which he started passing gravel in his stools. This was repeated 3 times and he passed gravel in stools for the next 5 days. From the 2nd to 5th day of hospital stay he had low-grade continuous fever. He was treated with antibiotics and laxatives. A urine culture was sent for examination, which revealed no growth. After the 5th day when the gravel extrusion was minimal the fever stopped and the child regained appetite. An X-ray on the 6th day of hospital stay showed no radio opaque bodies and was consistent with the history of stoppage of extrusion of gravel (Fig. 1B).
During his hospital stay psychiatric consultation was prescribed for his abnormal behavior. He was diagnosed to have an oppositional defiant disorder. His IQ test revealed that he was mildly mentally retarded. After a number of sessions with the caregivers the boy admitted to having eaten gravel. According to the account given by the boy he had been intermittently eating gravel since 1 year of age. His peripheral smear revealed microcytic hypochromic anemia.
He was completely asymptomatic when discharged from hospital and was only taking fluoxetine, which was prescribed by the psychiatrist for oppositional defiant disorder. After 1 week a repeat colonoscopy was undertaken which was normal except for worms, for which deworming was implemented (Fig. 2B). His abdominal mass and distension had disappeared and pica was absent.
2. Discussion
Ingestion of foreign bodies is common among children.1 About 1% of foreign bodies are associated with perforation. About 37% of children less than 5 years old eat earth at least occasionally.2 Psychiatric illness compounding an eating disorder and pica is a frequent association.3 Ingestion of lithobezoar is quite uncommon among children when compared to the incidence of foreign body ingestion in children of this age group.4 As this patient had lithobezoar ingestion over a prolonged period (no similar case encountered in the previous literature), he therefore showed a rare presentation, which makes this case reportable.5 The patient had a history of gravel eating since he was 1 year old and he had developed constipation before presenting to the emergency room (ER). By the time he presented to the ER he had developed foul smelling brownish stools with tenesmus, abdominal distension and generalized tenderness over the abdomen. These features suggested a developing colitis and the clinical inference was reinforced by development of fever on the 2nd day of hospital admission and elevated blood counts with neutrophilia. Erect X-rays of the abdomen ruled out a perforation and USG of the abdomen suggested colonic obstruction.6; 7 ; 8 The colonic foreign bodies visualized by the X-ray were massive enough in quantity to cause obstruction. Since clinically there was colitis with the obstructive features, the differential diagnoses were confined to the varied etiologies of enterocolitis and colonic obstruction. As the amount of foreign body was massive and filled almost up to the proximal colon, surgical intervention was always expected at any stage of hospital stay. The child was managed conservatively as he continued to pass the gravel in feces without any worsening of his condition. Within 6 days of hospital admission he stopped passing gravel in feces and repeat X-ray confirmed the absence of gravel in the gut. The follow-up colonoscopy confirmed complete resolution of the mucosal pathology.
3. Conclusion
An unusual case of retained ingested foreign bodies in the colon as a result of psychiatric illness in a 10-year-old boy is described. The case was of particular interest in two respects: (a) the unusual situation could be treated by appropriate therapy; (b) no surgical intervention was needed despite evidence of obstruction as revealed by the distended colon and rectum in USG and clinical evidence of enterocolitis supported by elevated blood counts and appearance of mucosa in colonoscopy and proctoscopy.
Declaration about financial interests
This is to declare that all the authors of this article do not have any financial interest associated with the material presented herein.
References
- 1 K.M. Cross, A.J. Holland; Gravel gut: small bowel perforation due to a blunt ingested foreign body; Pediatr Emerg Care, 23 (2007), pp. 106–108
- 2 W.A. Shivoga, W.N. Moturi; Geophagia as a risk factor for diarrhoea; J Infect Dev Ctries, 3 (2009), pp. 94–98
- 3 F. Serour, M. Witzling, D. Frenkel-Laufer, A. Gorenstein; Intestinal obstruction in an autistic adolescent; Pediatr Emerg Care, 24 (2008), pp. 688–690
- 4 S.K. Narayanan, V.S. Akbar Sherif, P.R. Babu, T.K. Nandakumar; Intestinal obstruction secondary to a colonic lithobezoar; J Pediatr Surg, 43 (2008), pp. e9–e10
- 5 W. Cheng, P.K. Tam; Foreign-body ingestion in children: experience with 1265 cases; J Pediatr Surg, 34 (1999), pp. 1472–1476
- 6 V. Selivanov, G.F. Sheldon, J.P. Cello, R.A. Crass; Management of foreign body ingestion; Ann Surg, 199 (1984), pp. 187–191
- 7 M. Dahiya, J.S. Denton; Esophagoaortic perforation by foreign body (coin) causing sudden death in a 3-year-old child; Am J Forensic Med Pathol, 20 (1999), pp. 184–188
- 8 K. Renner, B. Holzer, G. Hochwarter, E. Weihsbeck, R. Schiessel; Needle perforation of the appendix; Dig Surg, 17 (2000), pp. 413–414
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?