Abstract
Objectives
The aim of this study was to analyze the changes in hemoglobin level and to determine a suitable timeline for post-operative hemoglobin monitoring in patients undergoing fixation of femoral neck fracture.
Patients and methods
Patients who underwent either dynamic hip screw (DHS) fixation (n = 74, mean age: 80 years) or hip hemiarthroplasty (n = 104, mean age: 84 years) for femoral neck fracture were included into the study. The hemoglobin level of the patients was monitored perioperatively.
Results
Analysis found a statistically and clinically significant mean drop in hemoglobin of 31.1 g/L over time from pre-operatively (D0) to day-5 post-operatively (p < 0.001), with significant reductions from D0 to day-1 and day-1 to day-2 (p < 0.001). At each post-operative time point, DHS patients had lower hemoglobin values over hemiarthroplasty patients (p = 0.046).
Conclusion
The decrease in hemoglobin in the first 24-h post-operative period (D0 to day-1) is an underestimation of the ultimate lowest value in hemoglobin found at day-2. Relying on the day-1 hemoglobin could be detrimental to patient care. We propose a method of predicting patients likely to be transfused, and recommend a protocol for patients undergoing femoral neck fracture surgery to standardize postoperative hemoglobin monitoring.
Level of evidence
Level IV Prognostic study.
Keywords
Fracture ; Hemoglobin ; Neck of femur ; Postoperative
Postoperative hemoglobin analysis for orthopedic patients expected to have lost significant volumes of blood during surgery is part of good medical practice. Therefore, it is often routine care to measure the hemoglobin levels on Day 1 after surgery (D1, [within 24 h of surgery, subsequent 24 h periods are defined as D2, D3 and so forth]). However, the timing of subsequent analyses is not well defined in the literature.
Surgery for fractured neck of femur (NOF) is one of the most common orthopedic procedures performed in hospitals worldwide today.1 ; 2 Generally occurring among elderly,3 fractured NOF is associated with high morbidity (approximately 50%)4 and mortality (33%)5 rates in one year. The guidelines of the National Institute for Health and Care Excellence (NICE) recommend that surgery for fractured NOF be performed between 24 and 48 h after admission following medical optimization and multidisciplinary input, based on the National Hip Fracture Database (NHFD) which suggests a 36-h window.6
Low pre- and postoperative hemoglobin are recognized factors that affect length of stay, transfusion risk, morbidity and mortality.7 ; 8 ; 9 ; 10 ; 11 ; 12 ; 13 ; 14 ; 15 ; 16 However, as of 2014, a review of the peer-reviewed literature revealed that no recommendations exist regarding an optimum perioperative hemoglobin level. In addition, in the UK, there are currently no recommendations regarding the timeframe within which postoperative hemoglobin should be taken.17 A study at our own institution revealed inconsistent postoperative blood sampling practice of hip fracture patients, with some patients having daily blood sampling as default.
An evidence-based protocol could optimize this patient groups recovery and reduce the cost for the National Health Service (NHS, UK). Therefore, we investigated pre- and postoperative hemoglobin to establish a perioperative hemoglobin analysis regime for patients undergoing routine fixation of fractured NOF with a view to efficaciously assess for anemia.
Patients and methods
A prospective study of all NOF fractures surgically managed over an 18-month period was conducted at our institution. The Research and Ethics Committee approved the study and associated protocols (reference: 12/NW/0400). A total of 390 patients were admitted for surgical management of a fractured NOF during this study period. 178 patients (74 dynamic hip screw for intertrochanteric fractures [DHS] and 104 hemiarthroplasty, both monopolar and bipolar hemiarthroplasty for femoral neck fractures) were eligible for analysis after the application of the exclusion criteria described in Table 1 .
| 1. Patients with associated injuries |
|---|
| 2. Patient age ≤50 years |
| 3. Surgical repair other than DHS/hemiarthroplasty |
| 4. >72 h time to surgery |
| 5. <2 Postoperative Hb readings during admission |
| 6. Patients requiring perioperative transfusion |
Sensible assumptions have been made for the purposes of this study. The same technique was used for monopolar and bipolar hemiarthroplasty surgery; only the implant used for each of the two techniques was different. It is therefore reasonable to combine their data. Also, hemoglobin values during the perioperative period are a recognized measure of blood volume and/or blood loss. Blood loss parameter may therefore be used to describe our results. All patients received the same low-molecular weight heparin anticoagulation regimen unless contraindicated. Drains were not routinely inserted.
For 68% of the patients, hemoglobin levels were measured preoperatively (D0) and on at least two consecutive postoperative days while the other 32% had their hemoglobin levels monitored on at least two non-consecutive postoperative days. No protocol was in place to instruct clinicians on when to monitor hemoglobin levels. The decrease in hemoglobin was calculated by subtracting the hemoglobin level on the studied postoperative day from the level on the preoperative day.
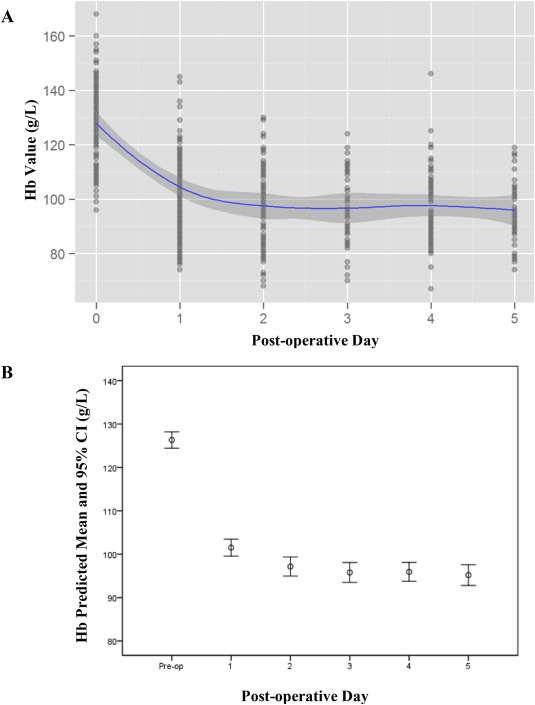
A repeated measures General Estimation Equation (GEE) model was employed for any omitted hemoglobin values with day (D) as the factor to assess for the overall trend in hemoglobin levels over time (Fig. 1 ). Pairwise comparisons between days were assessed and significances were adjusted using a quasi-Bonferroni correction for multiple testing by applying a lower critical value of 0.01 (1% significance level) for pairwise p values. Adjusted means were comparable between time points despite variance in numbers of non-missing outcome measures due to use of the GEE model.
|
|
|
Fig. 1. (A ) Scatter plot of hemoglobin values with locally weighted scatterplot smoothing best-fit curve. (B ) Average hemoglobin values with 95% confidence intervals. |
Dynamic hip screw and hemiarthroplasty patients were compared for hemoglobin values over time. In addition, hemoglobin levels were compared between patients undergoing prompt surgery (surgery commenced within 36 h of admission) with patients who had delayed surgery for a non-medical cause (between 36 and 72 h from admission).
The GEE models investigated the differences between surgical procedures fitted with factors including numbers of days since admission, type of surgical procedure and interaction, and influence of delay to commencing surgery and those fitted with factors including numbers of days since admission, type of surgical procedure and surgery delay.
Additionally, hemoglobin blood loss by D2 was assessed using analysis of covariance (ANCOVA) models. The analyses of D2 hemoglobin values included predictors for D0 hemoglobin, type of surgical procedure, and surgery delay. Changes in hemoglobin from D0 to D2 were calculated from the adjusted means from the ANCOVA model.
Overall analysis used a conventional two-sided 5% significance level, and pairwise comparisons were adjusted for multiple comparisons using a two-sided 1% significance level. All analyses were produced using SPSS Statistics (Version 20.0, IBM Corp).
Results
The mean age of the patient cohort was 83 years (DHS 80.5, hemiarthroplasty 84.4; range: 58–98 years, standard deviation [SD]: 10 years) and preoperative hemoglobin was 126.3 g/L (range: 93–168 g/L, SD: 12.9 g/L).
There were significant reductions in hemoglobin over time (p < 0.001). Specifically, the drop in hemoglobin values between the preoperative period and the lowest adjusted mean value on D5 was 31.1 g/L.
The D0 hemoglobin values had a highly significant influence on hemoglobin changes by D2 (p < 0.001), after adjusting for type of surgery and surgical delay. Hemoglobin values dropped significantly from D0 (mean 126.3 g/L) to D1 (101.5 g/L) by 24.8 g/L (p < 0.001). Postoperatively, a further significant fall of 4.4 g/L in hemoglobin (p < 0.001) was also noted between D1 and D2 (97.1 g/L). However, there were no statistically significant changes from D2 to D3 (p = 0.131), D3 to D4 (p = 0.881), and D4 to D5 (p = 0.483) (Table 2 ).
| Predicted Hb values from GEE model over time | |||
|---|---|---|---|
| Day | n-value | Hb adjusted mean (g/L) | 95% confidence interval (g/L) |
| Pre-op (Day 0) | 178 | 126.3 | 124.4, 128.2 |
| Day 1 | 166 | 101.5 | 99.6, 103.5 |
| Day 2 | 114 | 97.1 | 95.0, 99.3 |
| Day 3 | 69 | 95.8 | 93.5, 98.1 |
| Day 4 | 76 | 95.9 | 93.8, 98.1 |
| Day 5 | 49 | 95.2 | 92.8, 97.6 |
Comparison between surgical procedures showed statistically significant differences in hemoglobin between types of surgeries (p = 0.046) over all time points. DHS patients consistently had lower average hemoglobin values than hemiarthroplasty patients (Table 3 ). The average changes from D0 to D5 were 31.7 g/L for DHS and 30.6 g/L for hemiarthroplasty.
| Hb results from GEE model for surgery type grouping | ||||
|---|---|---|---|---|
| Surgery type grouping | Day | n-value | Hb adjusted mean (g/L) | 95% confidence interval (g/L) |
| DHS | Pre-op | 74 | 125.0 | 121.9, 128.1 |
| Day 1 | 68 | 99.5 | 96.4, 102.6 | |
| Day 2 | 49 | 93.9 | 90.6, 97.2 | |
| Day 3 | 32 | 93.9 | 90.3, 97.5 | |
| Day 4 | 28 | 94.0 | 90.1, 97.8 | |
| Day 5 | 23 | 93.3 | 89.9, 96.7 | |
| Hemiarthroplasty | Pre-op | 104 | 127.3 | 124.9, 129.6 |
| Day 1 | 98 | 102.9 | 100.4, 105.4 | |
| Day 2 | 65 | 99.6 | 96.7, 102.4 | |
| Day 3 | 37 | 96.9 | 94.1, 99.8 | |
| Day 4 | 48 | 97.3 | 94.7, 99.8 | |
| Day 5 | 26 | 96.7 | 93.4, 99.9 | |
For both DHS and hemiarthroplasty, the drop was greatest on the first two postoperative days, after adjusting for D0 values and surgical delay (Table 5 ). DHS patients had 4.6 g/L greater mean hemoglobin reduction compared to hemiarthroplasty patients (p = 0.043, 95% confidence interval [CI] −9.12, −0.15 g/L), with the hemoglobin values decreased the most from D0 to D1.
| Hb results from GEE main effects model | |||||
|---|---|---|---|---|---|
| Surgery type grouping | Surgery delay | Day | n-value | Hb adjusted mean (g/L) | 95% confidence interval (g/L) |
| DHS | 0–1 day | Pre-op | 54 | 124.0 | 120.9, 127.1 |
| Day 1 | 50 | 99.2 | 96.1, 102.3 | ||
| Day 2 | 35 | 94.8 | 91.6, 98.1 | ||
| Day 3 | 20 | 93.5 | 90.2, 96.8 | ||
| Day 4 | 20 | 93.6 | 90.2, 97.0 | ||
| Day 5 | 17 | 93.0 | 89.7, 96.3 | ||
| 2–3 days | Pre-op | 20 | 125.5 | 122.1, 128.9 | |
| Day 1 | 18 | 100.7 | 97.4, 104.0 | ||
| Day 2 | 14 | 96.3 | 92.8, 99.8 | ||
| Day 3 | 12 | 95.0 | 91.2, 98.7 | ||
| Day 4 | 8 | 95.1 | 91.4, 98.7 | ||
| Day 5 | 6 | 94.5 | 90.7, 98.3 | ||
| Hemiarthroplasty | 0–1 day | Pre-op | 71 | 127.2 | 124.7, 129.7 |
| Day 1 | 66 | 102.4 | 99.8, 105.0 | ||
| Day 2 | 45 | 98.0 | 95.3, 100.8 | ||
| Day 3 | 26 | 96.7 | 93.9, 99.4 | ||
| Day 4 | 29 | 96.8 | 94.2, 99.4 | ||
| Day 5 | 20 | 96.2 | 93.3, 99.0 | ||
| 2–3 days | Pre-op | 33 | 128.7 | 125.5, 131.8 | |
| Day 1 | 32 | 103.8 | 100.7, 107.0 | ||
| Day 2 | 20 | 99.5 | 96.2, 102.7 | ||
| Day 3 | 11 | 98.1 | 94.6, 101.7 | ||
| Day 4 | 19 | 98.3 | 95.1, 101.5 | ||
| Day 5 | 6 | 97.6 | 94.0, 101.3 | ||
| Surgery type grouping | Day | n-value | Hb adjusted mean (g/L) | 95% confidence interval (g/L) |
|---|---|---|---|---|
| DHS | Day 2 | 49 | 93.73 | 90.21, 97.25 |
| Change from pre-op | −32.70 | −36.22, −29.18 | ||
| Hemiarthroplasty | Day 2 | 65 | 98.36 | 95.27, 101.45 |
| Change from pre-op | −28.07 | −31.16, −24.98 |
The trend of hemoglobin changes over time showed no statistically significant differences between either forms of surgery (p = 0.414). Therefore, although the decrease in hemoglobin was greater from D0 for DHS, the pattern of change was similar between types of surgery.
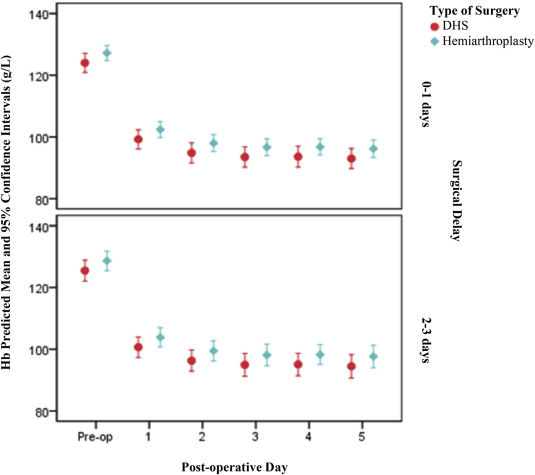
There were no statistically significant differences in hemoglobin levels for surgical delay (p = 0.389) (Table 4 ), after adjusting the number of days since admission and type of surgery (Fig. 2 ).
|
|
|
Fig. 2. A graphical representation of hemoglobin levels in the perioperative period divided by type of surgery and surgical delay. |
The decrease in hemoglobin from D0 values was greatest until D2; hence further detailed analysis was conducted for this time period.
Discussion
Although expeditious surgery for patients with hip fractures has benefits for patient recovery and return to function, we are unable to benefit from postoperative hemoglobin values. Patients with dynamic hip screw fixation lose more blood overall (and certainly within the first two days postoperatively) but this is not affected by prompt surgery. If surgery occurs within 72 h of the first hemoglobin reading, then repeating this preoperatively is unnecessary.
The results show a mean hemoglobin decrease of 31.1 g/L for all patients over five days from surgery. Interestingly, our study showed that the drop in hemoglobin continues until D5, however, decreases between consecutive days were only significant until D2. Thus, we recommend D2 for the most timely analysis and subsequent management of postoperative hemoglobin. Our analysis in bleeding kinetics within acute fractured NOF patients is in parallel to the findings of Irisson et al who investigated the fall in hemoglobin in elective lower limb arthroplasty.18 The group also showed that the most significant bleeding loss occurred between the end of surgery and D1; however, the fall in hemoglobin ceased by D3. It is reasonable to assume that the observed decrease in hemoglobin is caused by varying contributions from bleeding from the wound site, bleeding into soft tissues, loss in drains and the dilutive effect of postoperative fluids. More complex pathological processes such as decreased erythropoiesis secondary to a large inflammatory response from surgery, and decreased intestinal absorption and mobilization of iron also contribute to the postoperative hemoglobin drop.19 ; 20
Based on the findings within this study, surgeons should be aware that the patients preoperative hemoglobin should be able to withstand a minimum of 31.1 g/L drop. When considering the upper and lower limits of the 95% confidence intervals of D0 and D2 respectively, a preoperative hemoglobin level of 40 g/L above the institutions transfusion trigger value (TTV) is recommended to allow for predicted drop in hemoglobin and to avoid transfusion. This level can be achieved by preoperative transfusion and iron replacement (with or without erythropoietin) with decisions made on a case-by-case basis.
Further justification for the surgical prerequisite stems from previous studies, which suggest that a low D0 hemoglobin increases the necessity of transfusion (and its associated risks),12 in addition to increased morbidity and mortality. Halm et al showed that patients with higher preoperative hemoglobin had a shorter length of stay, lower morbidity and readmission within 60 days of discharge.7 Gruson et al followed 395 patients above the age of 65, and similarly found that hospital length of stay and mortality at six months and twelve months postoperatively were higher for patients with a preoperative anemia.8 In fact, it was shown that patients were twice as likely to die in hospital compared to non-anemic patients (odds ratio: 2.0, p = 0.3). This trend is echoed by a study by Ho et al who found that a preoperative hemoglobin of less than 110 g/L was associated with increased mortality at 12 months.9 Importantly, one of the most commonly used and reliable predictors of mortality post hip fracture fixation surgery,21 the Nottingham Hip Fracture Score specifically includes preoperative hemoglobin in its mortality predicting score due to the high association with mortality.10
This study demonstrated that a hemoglobin value taken on D2 postoperatively represents the largest drop in a patients circulating hemoglobin with statistical and also clinical significance. We can conclude that D1 postoperative hemoglobin values may provide false reassurance to clinicians monitoring patients who have undergone a fractured NOF procedure. The evidence shows that the hemoglobin value might be above the TTV on D1, but may fall below TTV due to the continued and significant fall in hemoglobin. In effect, a hemoglobin value measured on D1 might provide false assurance to the clinician and will have fallen further on D2.
Within the study cohort of n = 178, we detected 14 patients (7.9%) who had a ‘falsely high’ hemoglobin value on D1, which subsequently fell further on D2 to below the TTV value. However, 7.9% is probably fairly conservative considering that these 14 patients were within the 102 patients who had both their blood samples taken on D1 and D2.
Looking at specific values, the data shows that the statistically significant fall in hemoglobin between D1 and D2 is on average from 101.5 g/L (95% CI 99.6, 103.5 g/L) to 97.1 g/L (95% CI 95.0, 99.3 g/L) for all fixations of NOF fractures. This decrease traverses the value of 100 g/L which is typically the threshold for anemia.22 This threshold was also historically relevant for transfusions,23 however, with increased awareness of risks associated with transfusion, more restrictive transfusion policies are now favored. Despite this, patients with symptomatic anemia with a hemoglobin of less than 100 g/L are still recommended to have a transfusion.24
Furthermore, it can be concluded that the average patient undergoing NOF fracture fixation becomes anemic on D2 and not D1. This adds further weight behind the idea of routinely testing the patients on D2 postoperatively and not D1. If D2 hemoglobin level is more sensitive for anemia, affected patients can be reliably identified and commenced on appropriate measures to restore their hemoglobin to acceptable levels. This is important because anemic patients are more likely to require a transfusion if their hemoglobin is not managed well.25 ; 26
Orthopedic surgeons should highly consider the importance of the limitations anemic patients might have when working with rehabilitation services. Young et al described that patients feeling the lethargic effect of anemia may well have a reduced functional status resulting in an increased time to discharge and potentially a higher infection rate postoperatively.27 Lawrence et al showed that higher hemoglobin levels postoperatively were associated with increased functional status as measured by walking distance.28 Dunne et al found that patients who were anemic postoperatively (defined by a hematocrit less than 36) had increased mortality, incidence of pneumonia and length of hospital stay.29
A hemoglobin level of less than 100 g/L has been shown to be associated with the increased likelihood of wound infection rates in vascular surgery30 and this trend has also been confirmed in total joint arthroplasty.31 Early intervention in treating low hemoglobin was shown to reduce postoperative transfusion frequency and number of units in addition to postoperative infection rates in orthopedic patients.19 ; 32 Collectively, this research adds significant justification to the argument for timely hemoglobin monitoring in order to predict, detect and treat anemia promptly.7 ; 8 ; 9 ; 10 ; 11 ; 12 ; 13 ; 14 ; 15 ; 16
Jointly, the resource and subsequent financial burden of hip fracture surgery is significant. The estimated cost of collecting, transporting and processing a single full blood count sample is £633 – individually this may appear to be an insignificant sum, however when considering the number of patients undergoing hip fracture surgery (currently approximately 70,000 per year projected to increase to 101,000 in 2020) in the context of an ageing population, the financial burden runs into thousands of pounds per year per center and this value is set to increase.34 Moreover, after consideration of the risks associated with the practice of phlebotomy, including, but not limited to, bruising/hematoma, phlebitis/bacteremia and needle stick injuries, a greater evidence base should be employed to make decisions about postoperative blood testing.
Therefore, a protocol for efficacious blood sampling would reduce the number of samples required for hemoglobin analysis, in turn reducing the risk on patient and practitioner.
Evidence has shown that certain groups will require close -daily- monitoring of hemoglobin levels. Carson et al have previously shown that surgical patients with cardiovascular disease have a greater incidence of morbidity and mortality if they had a hemoglobin level of 100 g/L or less.35 With regards to chronic disease in the elderly population, patients with chronic renal impairment have been shown to have an increased incidence of transfusion in the perioperative period36 and so this group should also be given special consideration. With regards to this study, patients taking some form of anticoagulation were excluded due to the fact that this subpopulation will intrinsically have significant comorbidities and should therefore be monitored on an individual basis. Moreover, anticoagulation has been shown to facilitate blood loss37 and, therefore, levels of hemoglobin should be monitored more closely starting D1. The aforementioned ‘at risk’ patient groups (as defined in Table 6 ) require closer observation due to greater variance in physiology (such as patients with renal or cardiovascular disease) and coagulation (patients taking anticoagulation therapy).
| ‘At Risk’ groups: |
|---|
| 1. Patients with a pre-operative Hb level of <32 g/L above the centres TTV |
| 2. Patients taking any form of anticoagulation |
| 3. Patients with underlying chronic renal, cardiac disease |
Declaration
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Author contributions
NSN performed data collection, analysis and authored the manuscript. DvP performed data collection, analysis and authored the manuscript. SW performed statistical analysis and reviewed the manuscript. EMH provided study design and technical assistance and reviewed the manuscript.
References
- 1 J.A. Kanis, A. Odén, E.V. McCloskey, H. Johansson, D.A. Wahl, C. Cooper; A systematic review of hip fracture incidence and probability of fracture worldwide; Osteoporos Int, 23 (9) (2012), pp. 2239–2256
- 2 P. Kannus, J. Parkkari, H. Sievänen, A. Heinonen, I. Vuori, M. Järvinen; Epidemiology of hip fractures; Bone, 18 (1996), pp. 57–63
- 3 K.E. Ensrud; Epidemiology of fracture risk with advancing age; J Gerontol A Biol Sci Med Sci, 68 (10) (2013), pp. 1236–1242
- 4 R.S. Morrison; The medical Consultants role in caring for patients with hip fracture; Ann Intern Med, 130 (1) (1999), p. 76
- 5 J.J.W. Roche, R.T. Wenn, O. Sahota, C.G. Moran; Effect of comorbidities and postoperative complications on mortality after hip fracture in elderly people: prospective observational cohort study; BMJ, 331 (7529) (2005), p. 1374
- 6 National Institute for Health and Clinical Excellence. Quality Standard for Hip Fracture. Available from: http://www.nice.org.uk/guidance/qs16/chapter/about-this-quality-standard . Accessed 16 May 2015.
- 7 E.A. Halm, J.J. Wang, K. Boockvar, et al.; The effect of perioperative anemia on clinical and functional outcomes in patients with hip fracture; J Orthop Trauma, 18 (6) (2004), pp. 369–374
- 8 K.I. Gruson, G.B. Aharonoff, K.A. Egol, J.D. Zuckerman, K.J. Koval; The relationship between admission hemoglobin level and outcome after hip fracture; J Orthop Trauma, 16 (1) (2002), pp. 39–44
- 9 C.-A. Ho, C.-Y. Li, K.-S. Hsieh, H.-F. Chen; Factors determining the 1-year survival after operated hip fracture: a hospital-based analysis; J Orthop Sci, 15 (1) (2010), pp. 30–37
- 10 M.J. Maxwell, C.G. Moran, I.K. Moppett; Development and validation of a preoperative scoring system to predict 30 day mortality in patients undergoing hip fracture surgery; Br J Anaesth, 101 (4) (2008), pp. 511–517
- 11 A. Shander, K. Knight, R. Thurer, J. Adamson, R. Spence; Prevalence and outcomes of anemia in surgery: a systematic review of the literature; Am J Med, 116 (2004), pp. 58–69
- 12 D. Enko, F. Wallner, A. von-Goedecke, C. Hirschmugl, V. Auersperg, G. Halwachs-Baumann; The impact of an algorithm-guided management of preoperative anemia in perioperative hemoglobin level and transfusion of major orthopedic surgery patients; Anemia, 2013 (2013), p. 641876
- 13 K.B. Björkelund, A. Hommel, K.-G. Thorngren, D. Lundberg, S. Larsson; Factors at admission associated with 4 months outcome in elderly patients with hip fracture; AANA J, 77 (1) (2009), pp. 49–58
- 14 A. Oztürk, Y. Ozkan, S. Akgöz, N. Yalçin, R.M. Ozdemir, S. Aykut; The risk factors for mortality in elderly patients with hip fractures: postoperative one-year results; Singap Med J, 51 (2) (2010), pp. 137–143
- 15 A. Shokoohi, S. Stanworth, D. Mistry, S. Lamb, J. Staves, M.F. Murphy; The risks of red cell transfusion for hip fracture surgery in the elderly; Vox Sang, 103 (3) (2012), pp. 223–230
- 16 J.M. Willems, A.J.M. de Craen, R.G.H.H. Nelissen, P.A. van Luijt, R.G.J. Westendorp, G.J. Blauw; Hemoglobin predicts length of hospital stay after hip fracture surgery in older patients; Maturitas, 72 (3) (2012), pp. 225–228
- 17 Hip fracture overview - NICE Pathways. Available from: http://pathways.nice.org.uk/pathways/hip-fracture/hip-fracture-overview#content=view-node:nodes-multidisciplinary-rehabilitation . Accessed 13 May 2015.
- 18 E. Irisson, F. Kerbaul, S. Parratte, et al.; Perioperative management based on kinetics of bleeding during total primary arthroplasty; Ann Fr Anesth Reanim, 32 (3) (2013), pp. 170–174
- 19 M. Muñoz, J.A. García-Erce, J. Cuenca, E. Bisbe, E. Naveira; On the role of iron therapy for reducing allogeneic blood transfusion in orthopedic surgery; Blood Transfus, 10 (1) (2012), pp. 8–22
- 20 M. Muñoz, J.A. García-Erce, Á.F. Remacha; Disorders of iron metabolism. Part II: iron deficiency and iron overload; J Clin Pathol, 64 (4) (2011), pp. 287–296
- 21 I.K. Moppett, M. Parker, R. Griffiths, T. Bowers, S.M. White, C.G. Moran; Nottingham hip fracture score: longitudinal and multi-assessment; Br J Anaesth, 109 (4) (2012), pp. 546–550
- 22 J.N. Lunn, P.C. Elwood; Anaemia and surgery; Br Med J, 3 (5714) (1970), pp. 71–73
- 23 J.K. Wang, H.G. Klein; Red blood cell transfusion in the treatment and management of anaemia: the search for the elusive transfusion trigger; Vox Sang, 98 (1) (2010), pp. 2–11
- 24 J.L. Carson, B.J. Grossman, S. Kleinman, et al.; Red blood cell transfusion: a clinical practice guideline from the AABB; Ann Intern Med, 157 (1) (2012), pp. 49–58
- 25 C.S. Colón-Emeric; Postoperative management of hip fractures: interventions associated with improved outcomes; Bonekey Rep, 1 (2012), p. 241
- 26 J.L. Vincent, J.-F. Baron, K. Reinhart, et al.; Anemia and blood transfusion in critically ill patients; JAMA, 288 (12) (2002), pp. 1499–1507
- 27 S.W. Young, D.J. Marsh, M.A. Akhavani, C.G. Walker, J.A. Skinner; Attitudes to blood transfusion post arthroplasty surgery in the United Kingdom: a national survey; Int Orthop, 32 (3) (2008), pp. 325–329
- 28 V.A. Lawrence, J.H. Silverstein, J.E. Cornell, T. Pederson, H. Noveck, J.L. Carson; Higher Hb level is associated with better early functional recovery after hip fracture repair; Transfusion, 43 (12) (2003), pp. 1717–1722
- 29 J.R. Dunne, D. Malone, J.K. Tracy, C. Gannon, L.M. Napolitano; Perioperative anemia: an independent risk factor for infection, mortality, and resource utilization in surgery; J Surg Res, 102 (2) (2002), pp. 237–244
- 30 P. Kougias, S. Orcutt, T. Pak, et al.; Impact of postoperative nadir hemoglobin and blood transfusion on outcomes after operations for atherosclerotic vascular disease; J Vasc Surg, 57 (5) (2013), pp. 1331–1337
- 31 M.J. Dunbar, G. Richardson; Minimizing infection risk: fortune favors the prepared mind; Orthopedics, 34 (9) (2011), pp. 467–469
- 32 J.A. García-Erce, J. Cuenca, M. Muñoz, et al.; Perioperative stimulation of erythropoiesis with intravenous iron and erythropoietin reduces transfusion requirements in patients with hip fracture. A prospective observational study; Vox Sang, 88 (4) (2005), pp. 235–243
- 33 C. Czoski-Murray, M. Lloyd Jones, C. McCabe, et al.; What is the value of routinely testing full blood count, electrolytes and urea, and pulmonary function tests before elective surgery in patients with no apparent clinical indication and in subgroups of patients with common comorbidities: a systematic revi; Health Technol Assess, 16 (50) (2012), pp. 1–159
- 34 M. Stoneham, D. Murray, N. Foss; Emergency surgery: the big three–abdominal aortic aneurysm, laparotomy and hip fracture; Anaesthesia, 69 (2014), pp. 70–80
- 35 J.L. Carson, A. Duff, R.M. Poses, et al.; Effect of anaemia and cardiovascular disease on surgical mortality and morbidity; Lancet, 348 (9034) (1996), pp. 1055–1060
- 36 C. Lejus, A. Desdoits, C. Lambert, et al.; Preoperative moderate renal impairment is an independent risk factor of transfusion in elderly patients undergoing hip fracture surgery and receiving low-molecular-weight heparin for thromboprophylaxis; J Clin Anesth, 24 (5) (2012), pp. 378–384
- 37 G.A. Nuttall, P.J. Santrach, W.C. Oliver, et al.; The predictors of red cell transfusions in total hip arthroplasties; Transfusion, 36 (2) (1996), pp. 144–149
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?