Dear Editor,
Allergic diseases are manifested in various forms, such as atopic dermatitis (AD), bronchial asthma (BA) and allergic rhinitis (AR). Dermatitis research, such as that on Netherton syndrome, has progressed to the stage where it is now thought that lesions in the epithelial barrier predispose people to eczema, and that atopy might be a secondary disease.1
Filaggrin (FLG) has been known as a natural moisturizing factor and barrier-related protein. Mutation in the human FLG gene has been reported to be the most significant risk factor for AD. It has also been demonstrated that FLG gene mutations increased the risk of bronchial asthma in patients with atopic dermatitis. These findings have brought a breakthrough, where AD may be now considered as a barrier disorder disease.2
In contrast, FLG in the nose has not been well studied directly, although there are abundant mentions of FLG in relation to allergic rhinitis.3 In this study, for the first time, we attempted to evaluate FLG expression in human nasal mucosa through real time RT-PCR and demonstrated those alterations after various stimulations. Moreover, we also attempted to confirm the immunohistochemical localization of FLG in nasal mucosa, as presented previously in a preliminary study.4
Primary human nasal epithelial cells culture was performed in an air-liquid interface, as described by Gruenert et al.5 Human nasal epithelial cells were purchased from PromoCell GmbH (Heidelberg, Germany). The cell suspension of nasal epithelial cells was placed on a collagen-coated (Cellmatrix Type I-P, Nitta Gelatin, Japan) membrane filter (Millicel-CM, Millipore, MA, USA).
Quantitative PCR analysis was performed, as described by Kinoshita et al., 6 after stimulation of the lipopolysaccharides with Escherichia coli (LPS, 1 μg/ml), Polyinosinic–polycytidylic acid potassium salt (Poly I: C 1 μg/ml), TNFα (20 ng/ml), and TNFα (20 ng/ml) + Poly I: C 1 μg/ml for 24 h, respectively.
The immunohistochemistry study was performed using biopsies from three Japanese nonatopic patients. The anti-filaggrin primary antibody employed was an affinity-purified rabbit polyclonal IgG antibody (1/500 dilution; ab24584; Abcam PLC, Cambridge, UK). Staining was achieved with a Simple Stain kit (Nichirei, Tokyo, Japan) and developed with 3, 3-diaminobenzidine tetrahydrochloride (DAB) and hydrogen peroxide (Nichirei). The sections were counterstained with hematoxylin. The ethics committee of Dokkyo Medical University Koshigaya Hospital approved the study.
An unpaired Student t test (2-tailed) or 1-way ANOVA with the Tukey multiple comparison test was used. P values of less than .05 were regarded as statistically significant.
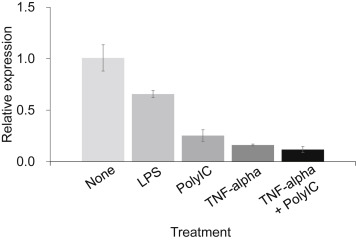
After stimulation of LPS, Poly I: C, TNFα and TNFα + Poly I: C for 24 h, respectively, FLG expressions were diminished significantly (Fig. 1). We have already demonstrated that LPS and poly I: C diminish transepithelial resistance (TER), respectively, which may reflect the down-regulation of airway epithelia.7 Measurements of TER of these conditions will be necessary for direct analysis. Kim et al.8 reported that TNF-α downregulates FLG expression in skin. In this study, the effect was maximal after stimulation with TNFα + Poly I: C. Poly I: C and TNF-alpha have might have different mechanisms for the expression of FLG in human nasal mucosa.
|
|
|
Fig. 1. Effects of microbial derivatives for filaggrin expression in primary cultured human nasal epithelial cells. After stimulation of lipopolysaccharides from E. coli (LPS, 1 μg/ml), Polyinosinic–polycytidylic acid potassium salt (Poly I: C 1 μg/ml), TNFα(20 ng/ml), TNFα(20 ng/ml) + Poly I: C 1 μg/ml for 24 h respectively. Each experiment was performed 5 times and representative data was shown. Data shown are the means ± SDs. |
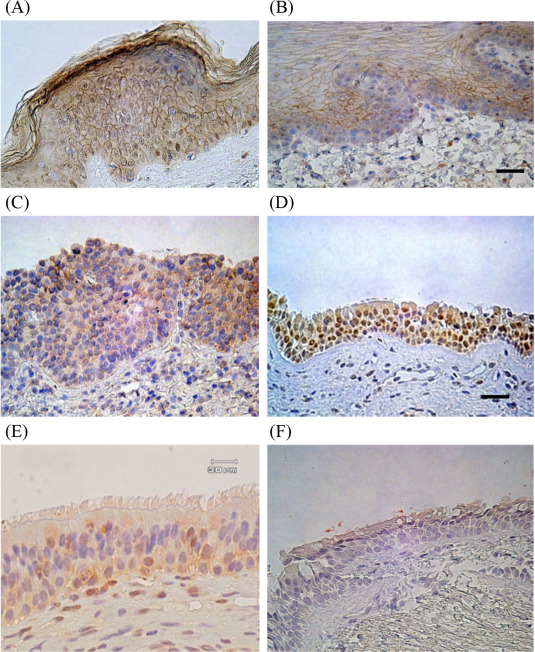
We also tried to confirm the localization of FLG in various tissues. Our immunohistochemical study showed that, FLG was expressed in the nose in human nasal epithelial cells of the inferior turbinate, not only in the stratified squamous epithelium in the anterior portion, but also in the pseudo-stratified ciliated epithelium in the posterior portion, as well as the maxillary sinus mucosa (Fig. 2).
|
|
|
Fig. 2. Immunohistochemical analysis of filaggrin was evaluated under a microscope at 100× magnification. Scale bar: 30 μM. Epidermis (A), oral mucosa (B), anterior portion of inferior turbinate (stratified squamous epithelium) (C), posterior portion of inferior turbinate (pseudostratified ciliated epithelium) (D), maxillary sinus mucosa (E) were demonstrated filaggrin positive cells immunohistochemically. Filaggrin positive cells were not detected in bronchial mucosa (F). Non-specific staining of FLG was observed in a number of infiltrating inflammatory cells, as well as in the nucleus and the cell membranes of some epithelial cells. |
Palmer et al., 2 Ying et al.9 and De Benedetto10et al. demonstrated a lack of FLG expression in the human airway. In contrast to those previous reports, in this study, for the first time, we confirmed that FLG exists in the human nose through both real time PCR and immunohistochemical procedures. Under Th2 dominated circumstances, it has been reported that FLG expression is down-regulated in vitro. 11 From this study, we demonstrated that bacterial and viral infections can alter FLG gene expression in human nasal mucosa for the first time.
Pseudostratified ciliated columnar epithelium is the main respiratory epithelium in the human upper airway; however, the anterior portion of the inferior turbinate consists of stratified squamous epithelium. Weidinger et al.3 reported that nasal biopsies demonstrated FLG expression only in the cornfield epithelium of the nasal vestibular lining. It is well recognized that airway ciliated mucosa has keratin related proteins. In a immunohistochemical study, we demonstrated that FLG is located in the human nasal epithelial cells of the inferior turbinate, not only in the stratified squamous epithelium in the anterior portion, but also in the pseudostratified ciliated epithelium in the posterior portion, as well as in the maxillary sinus mucosa.
In conclusion, for the first time, we demonstrated that precise localization of FLG in human nasal mucosa and TLR-3 and -4 signaling altered the amount of FLG gene expression in human nasal mucosa. A possible new therapeutic strategy to regulate atopic dermatitis through upregulating expression has been reported.12 On the other hand, from the viewpoint of our study, this control has not been demonstrated in the airway at al. It may be expected that further studies including western blotting will lead to a fix for the epithelial barrier in order to treat and prevent AR as a barrier disorder.
Conflict of interest
The authors have no conflict of interest to declare.
Acknowledgments
We would like to express our thanks to Nobukazu Kano, Noriyuki Nakajima, Shintaro Yamaguchi, Takashi Hirose and Toshio Ichiwata for their help related to the immunohistochemical study, Hiroko Ushio, Toshiro Takai and Ko Okumura for their valuable comments, and finally, Aki Nakayama for arranging the figures.
This work was supported by JSPS KAKENHI Grant Number 24592580 and in part by a Grant-in-Aid (S1311011) from the Foundation of Strategic Research Projects in Private Universities from the MEXT, Japan.
References
- 1 A. Hovnanian; Netherton syndrome: skin inflammation and allergy by loss of protease inhibition; Cell Tissue Res, 351 (2013), pp. 289–300
- 2 C.N. Palmer, A.D. Irvine, A. Terron-Kwiatkowski, Y. Zhao, H. Liao, S.P. Lee, et al.; Common loss-of-function variants of the epidermal barrier protein filaggrin are a major predisposing factor for atopic dermatitis; Nat Genet, 38 (2006), pp. 441–446
- 3 S. Weidinger, M. O'Sullivan, T. Illig, H. Baurecht, M. Depner, E. Rodriguez, et al.; Filaggrin mutations, atopic eczema, hay fever, and asthma in children; J Allergy Clin Immunol, 121 (2008), pp. 1203–1209
- 4 M. Miwa, N. Kano, N. Nakajima, S. Yamaguchi, T. Hirose, Y. Iwasaki, et al.; [Immunohistochemical detection of filaggrin in human upper airway mucosa]; Arerugi, 58 (2009), p. 359 [abstract] (in Japanese)
- 5 D.C. Gruenert, W.E. Finkbeiner, J.H. Widdicombe; Culture and transformation of human airway epithelial cells; Am J Physiol, 268 (3 Pt 1) (1995), pp. L347–L360
- 6 H. Kinoshita, T. Takai, T.A. Le, S. Kamijo, X.L. Wang, H. Ushio, et al.; Cytokine milieu modulates release of thymic stromal lymphopoietin from human keratinocytes stimulated with double-stranded RNA; J Allergy Clin Immunol, 123 (2009), pp. 179–186
- 7 M. Miwa, K. Ohmori, K. Fukuda, K. Kohyama, N. Kanoh, Y. Iwasaki, et al.; Control of transepithelial electrical resistance on primary cultured airway tracheal cells excised from guinea pig; Proc Airway Sec Res, 11 (2009), pp. 1–4
- 8 B.E. Kim, M.D. Howell, E. Guttman-Yassky, P.M. Gilleaudeau, I.R. Cardinale, M. Boguniewicz, et al.; TNF-α downregulates filaggrin and loricrin through c-Jun N-terminal kinase: role for TNF-α antagonists to improve skin barrier; J Invest Dermatol, 131 (2011), pp. 1272–1279
- 9 S. Ying, Q. Meng, C.J. Corrigan, T.H. Lee; Lack of filaggrin expression in the human bronchial mucosa; J Allergy Clin Immunol, 118 (2006), pp. 1386–1388
- 10 A. De Benedetto, C.M. Qualia, F.M. Baroody, L.A. Beck; Filaggrin expression in oral, nasal, and esophageal mucosa; J Invest Dermatol, 128 (2008), pp. 1594–1597
- 11 G.M. O'Regan, A. Sandilands, W.H. McLean, A.D. Irvine; Filaggrin in atopic dermatitis; J Allergy Clin Immunol, 122 (2008), pp. 689–693
- 12 A. Otsuka, H. Doi, G. Egawa, A. Maekawa, T. Fujita, S. Nakamizo, et al.; A possible new therapeutic strategy to regulate atopic dermatitis through upregulating filaggrin expression; J Allergy Clin Immunol, 133 (2014), pp. 139–146
Note to users: Corrected proofs are Articles in Press that contain the authors' corrections. Final citation details, e.g., volume and/or issue number, publication year and page numbers, still need to be added and the text might change before final publication.
Although corrected proofs do not have all bibliographic details available yet, they can already be cited using the year of online publication and the DOI , as follows: author(s), article title, Publication (year), DOI. Please consult the journals reference style for the exact appearance of these elements, abbreviation of journal names and use of punctuation.
When the final article is assigned to volumes/issues of the Publication, the Article in Press version will be removed and the final version will appear in the associated published volumes/issues of the Publication. The date the article was first made available online will be carried over.
Document information
Published on 05/04/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?