Abstract
Objectives
It is known that the screws of the eight-plate hemiepiphysiodesis construct diverge as growth occurs through the physis. Our objective was to investigate whether there is a correlation between the amount of change of the joint orientation angle (JOA) and that of the interscrew angle (ISA) of the eight-plate hemiepiphysiodesis construct before and after correction.
Patients and methods
After the institutional review board approval, medical charts and X-rays of all patients operated for either genu valgum or genu varum with eight-plate hemiepiphysiodesis were analyzed retrospectively. All consecutive patients at various ages with miscellaneous diagnoses were included. JOA and ISA were measured before and after correction. After review of the X-rays, statistical analyses were performed which included Pearson correlation coefficient and regression analyses.
Results
There were 53 segments of 30 patients included in the study. Eighteen were males, and 12 were females. Mean age at surgery was 9.1 (range 3–17). Mean follow-up time was 21.5 (range, 7–46) months. The diagnoses were diverse. A strong correlation was found between the delta JOA (d-JOA) and delta ISA (d-ISA) of the eight-plate hemiepiphysiodesis construct (r = 0.759 (0.615–0.854, 95%CI), p < 0.001). This correlation was independent of the age and gender of the patient.
Conclusions
There is a strong correlation between the d-ISA and the d-JOA. The d-ISA follows the d-JOA at a predictable amount through formulas which regression analysis yielded. This study confirms the clinical observation of the diverging angle between the screws is in correlation with the correction of the JOA.
Level of evidence
Level IV, Therapeutic study.
Keywords
Hemiepiphysiodesis ; Eight-plate ; Correlation ; Screw divergence ; Joint orientation angle ; Interscrew angle
Introduction
The eight-plate is a tension-band plate and screws construct. It involves a two-hole titanium plate with a figure of eight configuration used with two nonlocking 4.5 mm cannulated cortical screws. It shows its effect by limiting the growth of the hemiphysis over which it is applied, and as the contralateral side of the physis continues to grow and expand, the screws of the eight-plate construct diverge.1 Since it was introduced to the literature by Stevens2 it has become popular in deformity correction in the growing skeleton. The surgeons using this implant observe that the screws diverge as the correction takes place.2 Divergence of the screws represent growth in the related physis.2 ; 3 ; 4 However it has not been studied before whether this divergence of the screws correlates with the amount of correction that takes place in the individual bone segment, femur or tibia. One of the problems that arises in the follow-up of patients who undergo eight-plate hemiepiphysiodesis is that in order to assess the degree of correction the surgeon needs to see the X-rays of the entire individual bone segment; such as AP femur or AP tibia, or the entire lower extremity. At times, those X-rays might be missing the femoral head for the femur, or ankle for the tibia. Sometimes the patients live in areas with limited resources, and would be asked to travel back and forth in order to get proper X-rays. An alternative to that could be not taking X-rays and following patients with clinical judgment, however that could yield imprecise results. The rationale behind this study was that if there is a close enough correlation between the change in the joint orientation angle (JOA) and the change in the interscrew angle (ISA), the patients could be instructed to have only an AP knee X-ray taken instead of a full-length individual bone X-ray until close to full correction. We investigated whether there is a correlation between the delta joint orientation angles (ΔJOA or d-JOA), namely the mLDFA (mechanical lateral distal femoral angle) and MPTA (medial proximal tibial angle),5 and the delta interscrew angles (ΔISA or d-ISA). We aimed to derive formulas through regression analyses that would enable estimation of JOA when one knows the ISA. The hypothesis was that a close correlation exists between d-ISA and d-JOA regardless of the remaining growth potential of the related physis.
Patients and methods
This was a retrospective study to include consecutive patients treated with eight-plate hemiepiphysiodesis at a single university hospital between 2009 and 2013. After the institutional review board approval, patients were identified retrospectively according to the surgery type. Inclusion criteria involved patients operated for genu valgum or genu varum, and treated by eight-plate hemiepiphysiodesis in the distal femur and/or proximal tibia. Patients with all diagnoses at all ages were included. Diagnoses were miscellaneous from congenital, developmental, metabolic, posttraumatic and idiopathic causes. They included Blounts disease, Diamond-Blackfan syndrome, cystinosis, diastematomyelia, fibular hemimelia, Fanconi-Bickel syndrome, Stickler syndrome, rickets, multiple hereditary exostosis, congenital absence of patella, arthrogryposis, coxa vara, mucopolysaccharidosis, and posttraumatic (Cozen phenomenon). Exclusion criteria included double plate hemiepiphysiodesis of the same hemiphysis6 and simultaneous eight-plate applications of both proximal tibia and distal tibia hemiphyses within the same tibia segment. X-rays were obtained before the surgery, at the immediate postoperative period and at the final follow-up. Accompanying surgeries at the same setting were noted. Ipsilateral proximal tibial osteotomies were performed in 5 cases together with distal femoral hemiepiphysiodesis. Middiaphyseal femoral osteotomies were done in two cases together with distal femoral hemiepiphysiodesis and a distal tibial osteotomy was performed in one case together with proximal tibial hemiepiphysiodesis (Table 1 ). The remaining 45 segments had eight-plate hemiepiphysiodesis, only. In three patients where the osteotomy was performed within the same segment, correction through the osteotomy site was acute. The mLDFA or the MPTA in those patients were measured on the immediate postoperative X-ray, instead of a preoperative X-ray. Final follow-up X-ray was determined as the last X-ray with the eight-plate on the bone. Mechanical axis of the lower extremity was not a parameter to be measured at any time during the study. All measurements were made within the same individual bone segment, either femur or tibia. Demographic characteristics of the patients along with the type of the frontal plane deformity present, the treatment modality, if any, accompanying surgeries, and duration of follow up are given in Table 1 . Patients received the same postoperative care. They were allowed to do range of motion exercises, and weight-bear as tolerated immediately. All patients included in the study have completed the follow-up.
| Number | Age | Sex | Bone segment | Frontal plane deformity | Diagnosis | Performed surgery | Side | Additional surgery | Follow-up (mos) |
|---|---|---|---|---|---|---|---|---|---|
| 1 | 11 | M | Femur | Varus | compensatory, adolescent blounts disease | LDFH | L | PTO | 17 |
| 2 | 9 | M | Tibia | Valgus | Diamond-Blackfan syndrome | MPTH | R | – | 46 |
| 2 | 9 | M | Tibia | Valgus | Diamond-Blackfan syndrome | MPTH | L | – | 46 |
| 3 | 17 | M | Femur | Valgus | Cystinosis | MDFH | R | – | 20 |
| 3 | 17 | M | Femur | Valgus | Cystinosis | MDFH | L | MFO | 20 |
| 4 | 5 | M | Tibia | Valgus | Cozen phenomenon | MPTH | L | – | 18 |
| 5 | 7 | F | Tibia | Valgus | Diastematomyelia | MPTH | R | – | 23 |
| 6 | 10 | F | Femur | Valgus | Fibular hemimelia | MDFH | R | – | 27 |
| 7 | 6 | M | Femur | Valgus | Fibular hemimelia | MDFH | L | PTO | 16 |
| 8 | 5 | F | Tibia | Valgus | Cozen phenomenon | MPTH | L | – | 16 |
| 9 | 8 | M | Femur | Valgus | Fanconi-Bickel syndrome | MDFH | R | – | 25 |
| 9 | 8 | M | Femur | Valgus | Fanconi-Bickel syndrome | MDFH | L | – | 25 |
| 9 | 8 | M | Tibia | Valgus | Fanconi-Bickel syndrome | MPTH | R | – | 25 |
| 9 | 8 | M | Tibia | Valgus | Fanconi-Bickel syndrome | MPTH | L | – | 25 |
| 10 | 15 | M | Femur | Valgus | Status post liver transplantation | MDFH | R | MFO | 17 |
| 11 | 11 | M | Tibia | Valgus | Stickler syndrome | MPTH | L | – | 25 |
| 12 | 7 | F | Femur | Varus | Rickets | LDFH | L | – | 16 |
| 12 | 8 | F | Tibia | Valgus | Rickets | MPTH | L | – | 15 |
| 13 | 12 | M | Femur | Valgus | Cystinosis | MDFH | R | – | 23 |
| 13 | 12 | M | Femur | Valgus | Cystinosis | MDFH | L | – | 33 |
| 13 | 12 | M | Tibia | Valgus | Cystinosis | MPTH | R | – | 23 |
| 13 | 12 | M | Tibia | Valgus | Cystinosis | MPTH | L | – | 33 |
| 14 | 14 | M | Femur | Valgus | Idiopathic | MDFH | R | – | 8 |
| 14 | 14 | M | Femur | Valgus | Idiopathic | MDFH | L | – | 8 |
| 15 | 11 | M | Femur | Valgus | Compensatory, Proximal tibia growth arrest | MDFH | R | PTO | 16 |
| 16 | 10 | F | Femur | Valgus | Cerebral palsy | MDFH | R | – | 33 |
| 16 | 10 | F | Femur | Valgus | Cerebral palsy | MDFH | L | – | 33 |
| 17 | 7 | F | Femur | Valgus | Multiple hereditary exostosis | MDFH | L | – | 15 |
| 17 | 7 | F | Tibia | Valgus | Multiple hereditary exostosis | MPTH | L | – | 23 |
| 18 | 13 | M | Femur | Valgus | Congenital absence of patella | MDFH | R | – | 25 |
| 19 | 8 | F | Femur | Valgus | Fibular hemimelia | MDFH | R | PTO | 16 |
| 20 | 13 | F | Tibia | Valgus | Arthrogryposis | MPTH | R | – | 26 |
| 21 | 8 | F | Femur | Valgus | Fanconi-Bickel syndrome | MDFH | R | – | 24 |
| 21 | 8 | F | Femur | Valgus | Fanconi-Bickel syndrome | MDFH | L | – | 24 |
| 21 | 9 | F | Tibia | Valgus | Fanconi-Bickel syndrome | MPTH | R | – | 28 |
| 21 | 8 | F | Tibia | Valgus | Fanconi-Bickel syndrome | MPTH | L | – | 24 |
| 22 | 5 | M | Femur | Valgus | Fibular hemimelia | MDFH | R | – | 12 |
| 22 | 5 | M | Tibia | Valgus | Fibular hemimelia | MPTH | R | – | 12 |
| 23 | 11 | M | Femur | Valgus | Multiple Hereditary Exostosis | MDFH | R | – | 10 |
| 23 | 11 | M | Tibia | Valgus | Multiple hereditary exostosis | MPTH | L | – | 10 |
| 24 | 4 | M | Femur | Valgus | Fibular hemimelia | MDFH | R | PTO | 10 |
| 25 | 13 | M | Femur | Valgus | Idiopathic | MDFH | R | – | 12 |
| 25 | 13 | M | Tibia | Valgus | Idiopathic | MPTH | R | – | 12 |
| 26 | 6 | F | Femur | Valgus | Rickets | MDFH | R | – | 7 |
| 27 | 4 | F | Tibia | Valgus | Coxa vara | MPTH | R | – | 15 |
| 28 | 7 | F | Tibia | Varus | Blounts disease | LPTH | R | – | 16 |
| 28 | 7 | F | Tibia | Varus | Blounts disease | LPTH | L | – | 16 |
| 29 | 8 | M | Femur | Valgus | Fibular hemimelia | MDFH | L | – | 17 |
| 29 | 8 | M | Tibia | Valgus | Fibular hemimelia | MPTH | L | DTO | 17 |
| 30 | 6 | M | Femur | Valgus | Mucopolysaccharidosis | MDFH | R | – | 32 |
| 30 | 6 | M | Femur | Valgus | Mucopolysaccharidosis | MDFH | L | – | 32 |
| 30 | 6 | M | Tibia | Valgus | Mucopolysaccharidosis | MPTH | R | – | 32 |
| 30 | 6 | M | Tibia | Valgus | Mucopolysaccharidosis | MPTH | L | – | 32 |
LDFH: Lateral distal femoral hemiepiphysiodesis.
MDFH: Medial distal femoral hemiepiphysiodesis.
LPTH: Lateral proximal tibial hemiepiphysiodesis.
MPTH: Medial proximal tibial hemiepiphysiodesis.
PTO: Proximal tibial osteotomy, fixation with frame.
DTO: Distal tibial osteotomy, fixation with frame.
MFO: Middiaphyseal femoral osteotomy, fixation with plate.
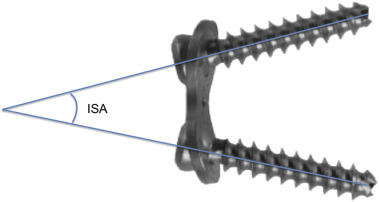
Joint orientation angles, namely, the mLDFA and MPTA were measured on preoperative and postoperative AP X-rays of femur or tibia, respectively. Interobserver and intraobserver reliability of these angles were tested previously, and it was stated as good to very good.7 Two of the investigators who were trained in limb deformity analysis reviewed the X-rays on two separate occasions. Intraclass correlation coefficient was used in testing agreement. We described ‘Interscrew angle’ (ISA) as the angle between the long axes of the screws of the eight-plate on each side of the physis (Fig. 1 ). Because most of the segments were valgus and few were varus, instead of the joint orientation angles themselves, the difference between the before and after measurements were obtained. So a delta value for each JOA was calculated. Immediate postoperative and final follow-up ISAs were measured and the difference was analyzed in comparison to the preoperative and final follow-up JOAs in order to find a correlation using Pearson correlation coefficient. Regression analyses were performed while investigating the effect of ISA on the JOA. Statistical analysis was performed with IBM SPSS Version 21.0 for Windows (SPSS Inc., Chicago, IL, USA). Continuous variables in this study were given with mean ± standard deviation or median [min − max] as appropriate. Categorical variables were summarized as frequencies and percentages. Correlation between the changes in angles was determined by Pearson correlation coefficient. Stepwise multiple linear regression analysis was used to verify the relation between JOA and ISA. Significance level was determined as p < 0.05. Confidence intervals at 95% were noted, as well. The resultant data were reviewed and analyzed by a biostatistician.
|
|
|
Fig. 1. Graphic illustration of interscrew angle (ISA). |
Results
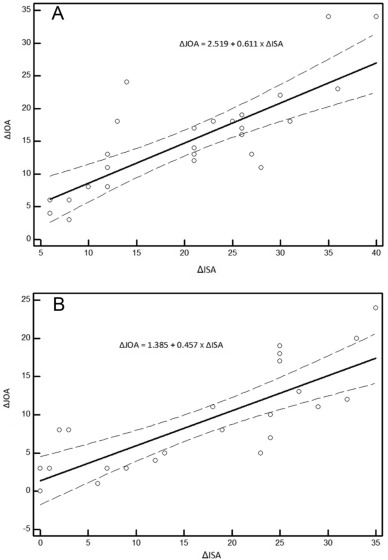
There were 53 segments of 30 patients included in the study. Eighteen were males, and 12 were females. Mean age at surgery was 9.1 (range 3–17). There are 29 femurs, and 24 tibias included in the study. Four patients had all four segments operated. Fifteen patients had single segment operated, femur or tibia. The remainder had two segments operated horizontally or vertically. Thirty-three segments (18 femur and 15 tibia) were operated using eight-plate (Orthofix, Verona, Italy), and 20 segments (11 femur and 9 tibia) were operated using eight-plate (Ortopro, Istanbul, Turkey). Both products have same material properties and implant design. The two different brands did not show any significant difference in terms of correlation between the d-JOA and d-ISA (p = 0.994). Mean follow-up time was 21.5 (range, 7–46) months. Intraclass correlation coefficient (ICC) yielded very good interobserver and intraobserver reliability (ICC was 0.950 for JOA and 0.993 for ISA for the interobserver reliability, and 0.980 for JOA and 0.997 for ISA for the intraobserver reliability). The ISA in the femur changed from 12.1 ± 10.1° at the immediate postoperative period to 32.3 ± 14.3° at the final follow-up and in the tibia it changed from 8.3 ± 8.0° at the immediate postoperative period to 25.4 ± 12.8° at the final follow-up. The d-ISA in the femur was 20.2 ± 9.8° and in the tibia it was 17.1 ± 11.4°. The d-JOA in the femur was 14.9 ± 7.9° and in the tibia it was 9.2 ± 6.6°. Scatter Plots have been created for evaluating the correlation between the d-JOA and the d-ISA, which revealed linear correlation. Using Pearson correlation coefficient, strong correlation was found between d-JOA and d-ISA. (r = 0.759 (0.615–0.854, 95%CI), p < 0.001). Because strong correlation was found between the d-JOA and d-ISA, stepwise multiple linear regression analyses were carried out in order to create formulas that will allow us to make some predictions. Age, gender and d-ISA were considered as independent factors to predict d-JOA. As a result of the analysis, only d-ISA was found significant. Following are such formulas: For femurs (ΔJOA = 2.519 + 0.611 × ΔISA) and for tibias (ΔJOA = 1.385 + 0.457 × ΔISA). 95% Confidence Intervals were given along with these scatter plots that described strong correlation (Fig. 2 A and B).
|
|
|
Fig. 2. Scatter plots in femurs (A) and in tibias (B) for evaluating the change in interscrew angle (ISA) versus joint orientation angle (JOA) with 95% confidence interval marked. |
Discussion
Tension band hemiepiphysiodesis is a well-established technique that corrects deformities through the contralateral growing hemiphysis by tethering the ipsilateral hemiphysis after the application of the eight-plate. The screws are inserted at an angle below and above the physis, which never stay at the same angle, as long as the physis continues to grow. For frontal plane deformities after the eight-plate is implanted, the patient needs to be followed-up with X-rays including individual bone in its full-length, preferably every four months due to unpredictability associated with guided growth.8 At times, in order to avoid traveling, the patient has a knee X-ray taken locally and sends it by mail. Before this study, it was not anticipatory to make a decision just by anteroposterior (AP) knee X-rays. We hypothesized that there would be a close correlation between the amount of divergence of the screws of eight-plate and the amount of correction of the deformity, and the latter could be estimated by using certain formulae. Our results showed that the hypothesis was correct and there is correlation, between the delta joint orientation angle and the delta interscrew angle. This correlation is not related to the growth rate of the physis. It is a purely mathematical correlation, independent of the age and sex of the patient. However there is no one to one correlation. In other words 10 degrees of change in interscrew angle does not yield 10 degrees of change in the joint orientation angle. An explanation to this could be the slack of the screws within the plate construct when placed in situ.9 ; 10 The implant configuration described in this article that revealed a correlation between the d-JOA and d-ISA applies to constructs, screws of which did not reach maximum divergent angle. In a situation where screws diverged at maximum, screws would theoretically impinge on the plate and the interscrew angle would not change anymore, while the change in the joint orientation angle could still occur. However this is rather unseen. In fact, Ballal et al speculated that due to the flexible nature of the implant, even after the screws reached at their maximal divergence there is facility within the flexible plate to bend.11 This can also be seen in Figure 5c of the paper by Boero et al.12 One case in our study who was treated for bilateral genu valgum didn't come to his follow-up visits. And when he showed up he developed varus deformity in the distal femur. Interestingly the ISA were found to be 43 and 78° on right and left femur, respectively. His immediate postoperative ISA values were found to be 8 and 38°, respectively. The differences between the interscrew angles were 35 and 40°, whereas the differences between the mLDFA angles were 34° in both sides. With careful analysis of the X–rays it was obvious that the divergence continued even after the screws reached their maximum at the expense of bending the plate. So the authors agree with Ballal et al11 that the titanium plate could bend being unable to resist the forces created by the physeal growth potential. This observation could falsify the assumption that the screws would stop diverging after they reach maximum divergence. We observed that the plate configuration facing the bone changed from being concave to convex after the bend due to its flexible nature.
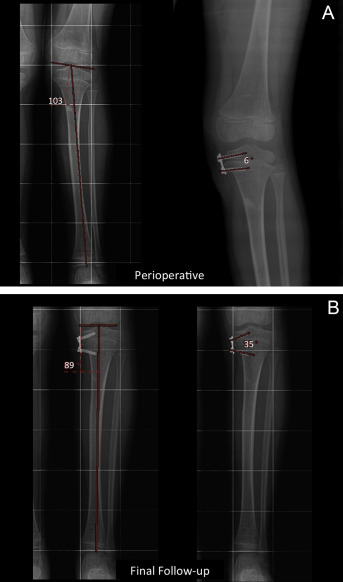
An application of the formulas to estimate d-JOA from d-ISA is depicted in Fig. 3 A and B. This is a case of Cozen phenomenon. The values are as follows: MPTA perioperative 103°, MPTA final follow-up 89°. ISA perioperative 6° and ISA final follow-up is 35°. By taking an AP knee X-ray only, one would be able to estimate the difference in the joint orientation angle (MPTA). For that purpose the following formula for tibias should be chosen (ΔJOA = 1.385 + 0.457 × ΔISA).
|
|
|
Fig. 3. A 5-year-old female patient who developed Cozen phenomenon after a proximal metaphyseal fracture. Her left medial proximal tibial angle (MPTA) was 103°, and the ISA was 6° when the eight plate was first applied (A - Perioperative). In 16 months the MPTA changed to 89° and the ISA changed to 35° (B – Final Follow-up). |
d-ISA in this case is 35–6 = 29°.
|
|
14.6° is the amount that is estimated by this formula using the difference between the ISAs before and after correction at the time of the X-ray.
(95% Confidence interval 0.615–0.854)
103–14.6 = 88.4° is the estimate for the current MPTA with the help of the formula and the difference of ISAs. The real MPTA was 89°.
Thus, this example shows that by knowing the change in the ISA, which was 29° in this case, it might be possible to predict the amount of change in joint orientation angle that is around 14 degrees of change in MPTA in this case.
The outliers have been shown in the scatterplot graphs. The outliers do not belong to a specific sex, age or disease. They are also not associated with an accompanying osteotomy. There are some underestimates and overestimates in using the formula. The formulas that the regression model yielded have been validated using bootstrap sampling in our dataset. The formulas need to be tested in other datasets for further validation. This study has some limitations. The number of participants included in the study were 30 involving their 53 segments. This does not jeopardize the results, since statistically this number is enough to investigate the correlation, run regression analyses and create formulas. However, further validating studies are needed to be performed in larger series of patient populations with eight-plates. Twenty of the 53 segments were operated using a different brand of the eight-plate implant. However both brands were composed of the same material. And there were no differences in the statistical analysis of the two groups (p = 0.994).
In our study, the angular divergence between the screws of the eight-plate construct was found to be correlated with change in the joint orientation angle, mLDFA or MPTA. Regression analyses yielded formulas that enabled us make estimations for the change in interscrew angle if the change in joint orientation angle was known. The formulas depicted in this paper are applicable to constructs composed of a titanium two-hole nonlocking plate with a figure of eight, and two cannulated 4.5 mm cortical screws. The formulas might or might not apply in other configurations of tension-band plates available in the market.
This study is important to confirm that there is close correlation between d-ISA and d-JOA. This correlation exists in all patients with varying degrees of growth potential.
References
- 1 D.M. Eastwood, A.P. Sanghrajka; Guided growth: recent advances in a deep-rooted concept; J Bone Jt Surg Br, 93 (2011), pp. 12–18
- 2 P.M. Stevens; Guided growth for angular correction: a preliminary series using a tension band plate; J Pediatr Orthop, 27 (2007), pp. 253–259
- 3 P.M. Stevens, F. Pease; Hemiepiphysiodesis for posttraumatic tibial valgus; J Pediatr Orthop, 26 (2006), pp. 385–392
- 4 J. Klatt, P.M. Stevens; Guided growth for fixed knee flexion deformity; J Pediatr Orthop, 28 (2008), pp. 626–631
- 5 D. Paley; Principles of deformity correction; Springer – Verlag, Berlin (2002), p. 8
- 6 R.D. Burghardt, S.C. Specht, J.E. Herzenberg; Mechanical failures of eight-plate guided growth system for temporary hemiepiphysiodesis; J Pediatr Orthop, 30 (2010), pp. 594–597
- 7 D.S. Feldman, E.R. Henderson, H.B. Levine, et al.; Interobserver and intraobserver reliability in lower-limb deformity correction measurements; J Pediatr Orthop, 27 (2007), pp. 204–208
- 8 N. Saran, K.E. Rathjen; Guided growth for the correction of pediatric lower limb angular deformity; J Am Acad Orthop Surg, 18 (2010), pp. 528–536
- 9 R.D. Burghardt, A.D. Kanellopoulos, J.E. Herzenberg; Hemiepiphyseal arrest in a porcine model; J Pediatr Orthop, 31 (2011), pp. e25–e29
- 10 J.J. Masquijo, L. Lanfranchi, A. Torres-Gomez, V. Allende; Guided growth with the tension band plate construct: a prospective comparison of 2 methods of implant placement; J Pediatr Orthop, 35 (2015), pp. e20–e25
- 11 M.S. Ballal, C.E. Bruce, S. Nayagam; Correcting genu varum and genu valgum in children by guided growth: temporary hemiepiphysiodesis using tension band plates; J Bone Jt Surg Br, 92 (2010), pp. 273–276
- 12 S. Boero, M.B. Michelis, S. Riganti; Use of the eight-Plate for angular correction of knee deformities due to idiopathic and pathologic physis: initiating treatment according to etiology; J Child Orthop, 5 (2011), pp. 209–216
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?