Summary
Background/Objective
Core needle biopsy (CNB) was widely used in the diagnosis of ultrasound-detectable breast lesions. We aimed at assessing the diagnostic performance differences between 14- and 16-gauge ultrasound-guided core biopsies.
Methods
This retrospective study enrolled patients receiving CNB from January 2001 to December 2007. The results of 14- and 16-gauge breast CNBs were compared with pathology reports of open surgical biopsy (OSB).
Results
A total of 1024 paired CNB and OSB results were obtained from 1732 CNB procedures in 1630 patients.Those CNB results reached 92.9% sensitivity, 99.7% specificity, 5.96% underestimation, and 94.8% accuracy rates. There was no difference in sensitivity (p = 0.17) or specificity (p = 0.38) between 14- and 16-gauge needles. However, better overall accuracy (p = 0.02), less underestimation (p < 0.001), and lower false-negative (p = 0.02) rates were found for the 14-gauge CNB.
Conclusion
Regarding accuracy and underestimation rates, a 14-gauge needle is preferred to a 16-gauge one in ultrasound-guided biopsies.
Keywords
breast;core needle biopsy;ultrasound guided
1. Introduction
Percutaneous large core needle biopsy (CNB), as first described by Parker et al1 in the early 1990s, has become widely used as an alternative to open surgical biopsy (OSB).1; 2; 3; 4 ; 5 During the past 10 years, with the increasing experience of this procedure, ultrasound-guided CNB has evolved as a highly sensitive, specific, and accurate method for the diagnosis of breast cancer.5; 6; 7 ; 8 Patients with concordant image and CNB results benefit from reduced discomfort and anxiety, as compared with OSB.
Despite a high concordance rate between CNB and histologic results obtained at the subsequent open biopsy,2 ; 5 differences (varying from 0% to 18%)1; 2; 3; 4 ; 9in pathologic findings still existed. The discordant results varied, from initial CNB findings of atypia or ductal carcinoma in situ (DCIS), upgraded to DCIS or invasive carcinoma at surgical excision, 10 to difficulty in distinguishing malignancy from benign papillary lesions.9
Factors affecting the false-negative (FN) and underestimation rates include accurate targeting of the needle, and the number and adequacy of samples obtained.11 ; 12 Recent studies investigating needle core biopsy underestimation rates have pointed to the potential variability associated with the differences in needle gauges.7; 13; 14 ; 15 There are still controversies as to whether the needle size has an impact on the different underestimations among various reported series.7; 14; 15; 16 ; 17
Currently, there is a lack of information about the diagnostic difference between 14- and 16-gauge needles in ultrasound-guided core biopsy for sonogram-detectable breast lesions. Although in 1995, Nath et al18 reported that biopsy samples obtained with a 14-gauge needle, compared with a 16- or 18-gauge needle, provided more accurate diagnostic results. The 16-gauge core needle was still used widely by physicians in many different centers. Studies focusing on the comparison of diagnostic efficacy between 14- and 16-gauge biopsy needles were lacking. Whether 14- and 16-gauge needles resulted in different diagnostic yield in terms of sensitivity, specificity, FN, false-positive (FP), and underestimation rates was still unknown.
The purpose of this study was to examine the diagnostic efficacy and underestimation rates of CNB in a series of breast tumors sampled with 14- versus 16-gauge needles in ultrasound-guided large core biopsies.
2. Methods
2.1. Patients
A retrospective study was conducted in our hospital to determine the accuracy and underestimation rates of CNB, and the difference in results of 14- versus 16-gauge biopsy needles. Data, on patients who received breast CNB during the period of January 2001 to December 2007, were retrospectively collected. The data collected included each patients age, gender, number of samples per CNB procedure, lesion size, and final OSB pathologic report. FN, FP, sensitivity, specificity, underestimation, and overall accuracy rates of CNB, and differences between results from 14- versus 16-gauge needles were compared. Ethical guidelines of the Declaration of Helsinki19 were followed throughout.
2.2. Ultrasound-guided CNBs
Ultrasound-guided procedures were performed with the patient in the supine or supine oblique position. Imaging was performed with a high-resolution 5–12 MHz linear array transducer (Voluson 530D and 730D, Kretz Technik, Zipf, Austria), and recorded according to the Breast Image Reporting and Data System.20 Biopsies were performed using a freehand technique with a 14-gauge automated or 16-gauge Tru-Cut needle and a spring-loaded biopsy gun (Magnum, Bard, Covington, GA, USA) under ultrasound guidance.
Two breast surgeons with 20 years (D.-R. Chen) and 25 years (S.-T. Chen) of experience, who were also experts in breast sonogram and CNB, conducted the entire biopsy series. Specimens were obtained from each lesion. All CNB specimens were evaluated and diagnosed byan experienced breast pathologist. Determination of concordance between the imaging and histopathologic findings in each case was decided by the breast surgeon who performed the procedure. Benign core biopsy results were considered concordant when there were no imaging features suspicious of malignancy and accurate targeting of the needle and adequate samples had been obtained.
If pathology results revealed mucinous-like lesions, papillary lesions, atypical findings, or discordance between core pathology and imaging, then breast surgeons would recommend OSB of the lesion. For those patients with malignant findings from the CNB, a definite surgical intervention was performed; patients with benign findings, who did not receive surgical excision, were asked to return in 6 months for a follow-up examination. If no changes were seen in the follow-up examination, then the lesions were regarded as likely benign.
2.3. Definition of sensitivity, specificity, accuracy, and underestimation
The histology of final surgical outcomes was compared to the pathology findings of the CNB for assessment of sensitivity, specificity, accuracy, and underestimation rates of the procedure. Only lesions with preoperative CNB results and subsequent OSB were calculated for diagnostic accuracy and underestimation. Results from the CNB and the final surgical outcome were thoroughly reviewed and compared by the breast surgeons for concordance. If the CNB and the final surgical pathologic results were compatible, the CNB was considered concordant.
The positive predictive value for malignancy of each consecutively performed surgical excision was calculated by including DCIS and other invasive breast cancer cases. Underestimation was defined as an initial CNB-revealed atypia, but with final surgical outcome upgraded to DCIS or invasive carcinoma, or DCIS upgraded to infiltrating ductal carcinoma (IDC).9 True negative (TN) was defined as initial CNB showing a benign result, and OSB also revealing benign lesions. True positive (TP) was defined as initial CNB showing a malignant result, and final surgical outcome also confirming malignancy. FN was defined as initial CNB showing a benign result, but OSB revealing malignancy. FP was defined as initial CNB showing a malignant result, but final surgical pathology revealing it to be benign.
Sensitivity was defined as the TPs divided by the sum of TPs and FNs, i.e., sensitivity = TP/(TP + FN). Specificity was defined as the TNs divided by the sum of TNs and FPs, i.e., specificity = TN/(TN + FP). Accuracy was calculated as TP and TN cases diagnosed by CNB at the ratio of total cases, i.e., accuracy = TP + TN/(TP + FN + TN + FP).
2.4. Statistical methods
Data are expressed as mean ± standard deviation (SD) for continuous variables. Independent t tests were used for the comparison of continuous variables. Categorical variables were normally tested with the χ2 test when appropriate. All results with p < 0.05 were considered statistically significant. All statistical analyses were performed with the SAS software, version 9.1.
3. Results
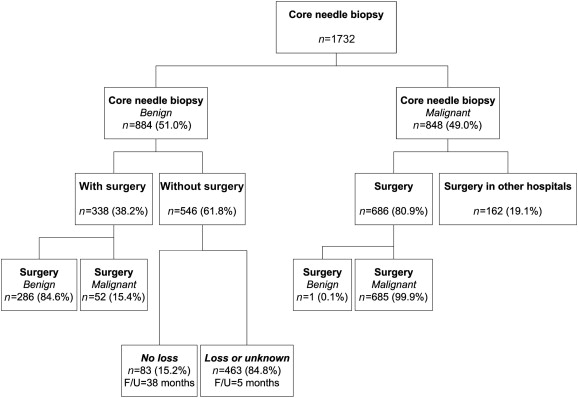
A total of 1732 CNBs were performed on the 1630 patients. The mean age of our patients was 46.4 years (range 13–93 years), with a mean tumor size of 2.8 cm (range 0.1–18 cm). The mean sample number per biopsy procedure was 3.0 (range 1–10) (Table 1). Initial pathologic results were 884 (51.0%) benign and 848 (49.0%) malignant cases. A total of 1024 patients received further surgical procedures due to pathology and imaging discordance, requests on the part of patients, or the presence of malignancy. Of our 884 patients with CNB benign lesions, 546 (61.8%) did not undergo further surgical excision and were followed up in clinic (Fig. 1).
| Patient characteristics | Total |
|---|---|
| Age (y) | |
| Mean (SD) | 46.4 (12.4) |
| Median | 45 |
| Range | 13–93 |
| Age (y) | |
| <35 (%) | 268/1730 (15.5) |
| 35–45 (%) | 567/1730 (32.8) |
| >45 (%) | 895/1730 (51.7) |
| Sample number | |
| Mean (SD) | 3.0 (1.5) |
| Median | 3 |
| Range | 1–10 |
| Sample number | |
| ≤3 (%) | 1161/1724 (67.3) |
| >3 (%) | 563/1724 (32.7) |
| Tumor size (cm) | |
| Mean (SD) | 2.8 (2.0) |
| Median | 2.2 |
| Range | 0–18 |
| Tumor size (cm) | |
| <2 (%) | 577/1560 (37.0) |
| 2–4 (%) | 701/1560 (44.9) |
| >4 (%) | 282/1560 (18.1) |
| Diagnostic accuracy | |
| Yes (%) | 1 679 (96.9) |
| No (%) | 53 (3.1) |
| Initial core needle biopsy result | |
| Benign | |
| Benign (%) | 865 (49.9) |
| Atypical (%) | 19 (1.1) |
| Malignant | |
| Ductal carcinoma in situ (%) | 75 (4.3) |
| Infiltrating ductal carcinoma (%) | 728 (42.0) |
| Mucinous carcinoma (%) | 13 (0.8) |
| Papillary carcinoma (%) | 7 (0.4) |
| Other malignancies (%) | 25 (1.4) |
SD = standard deviation.
|
|
|
Figure 1. Flow chart of patient allocation. F/U = follow-up. |
Results from the CNB and subsequent surgical procedures were thoroughly reviewed and compared by the breast surgeons for concordance (Table 2). Fifty-two cases with initial CNB of benign lesions turned out to be malignant at the final OSB (Table 3). There was one FP case, with initial CNB indicating a malignant phyllodes tumor that was found to be a benign phyllodes tumor after total excision. The FN and FP rates in our study were, therefore, 5.1% and 0.1%, respectively. Among 61 underestimation cases, 48 were DCIS to IDC and 13 were atypical ductal hyperplasia to DCIS or IDC, with an overall underestimation rate of 5.96%. Our CNB result showed an overall 92.9% sensitivity, 99.7% specificity, and 94.8% accuracy rate.
| Core needle biopsy | Open surgical biopsy | |||
|---|---|---|---|---|
| Total (%) | Total (%) | Benign (%) | Malignant (%) | |
| Benign (%) | 884 (51.0) | 338/884 (38.2) | 286/338 (84.6) | 52/338 (15.4) |
| Malignant (%) | 848 (49.0) | 686/848 (80.9) | 1/686 (0.1) | 685/686 (99.9) |
| Total (%) | 1732 (100) | 1024/1732 (59.1) | 287/1024 (28.0) | 737/1024 (72.0) |
| Total (n = 1024) | Needle gauge used | p | ||
|---|---|---|---|---|
| 14 (n = 470) | 16 (n = 554) | |||
| Sensitivity (%) | 685/737 (92.9) | 277 /293 (94.5) | 408 /444 (91.9) | 0.17 |
| Specificity (%) | 286/287 (99.7) | 177/177 (100) | 109/110 (99.1) | 0.38 |
| Accuracy | ||||
| Yes (%) | 971/1024 (94.8) | 454/470 (96.6) | 517/554 (93.3) | 0.02 |
| No (%) | 53/1024 (5.2) | 16/470 (3.4) | 37/554 (6.7) | |
| Underestimation | ||||
| Yes (%) | 61/1024 (6.0) | 12/470 (2.6) | 49/554 (8.8) | <0.001 |
| No (%) | 962/1024 (94.0) | 457/470 (97.4) | 505/554 (91.2) | |
| False negative | ||||
| Yes (%) | 52/1024 (5.1) | 16/470 (3.4) | 36/554 (6.5) | 0.02 |
| No (%) | 972/1024 (94.9) | 454/470 (96.6) | 518/554 (93.5) | |
| False positive | ||||
| Yes (%) | 1/1024 (0.1) | 0/470 (0) | 1/554 (0.2) | — |
| No (%) | 1023/1024 (99.9) | 470/470 (100) | 553/554 (99.8) | |
Among the 1024 CNB results with further SOB, 470 (45.9%) were performed by 14-gauge needles and 554 (54.1%) by 16-gauge needles. The FN rate of the 14- versus the 16-gauge needle was 3.4% (16/470) versus 6.5% (36/554), respectively (p = 0.02). The only FP result was derived from a 16-gauge needle biopsy. The underestimation rate of the 14- versus the 16-gauge needle was 2.6% (12/470) versus 8.8% (49/554), respectively (p < 0.001). Sensitivity, specificity, and accuracy of the 14- versus the 16-gauge needle was 94.5% versus 91.9% (p = 0.17), 100% versus 99.1% (p = 0.38), and 96.6% versus 93.3% (p = 0.02), respectively ( Table 3).
The mean weight of sample harvested per core was 12.7 mg (range 9.4–15.4 mg, SD 2.1) in the 14-gauge automated gun needle and 5.3 mg (range 3.5–7.1 mg, SD 1.2) in the 16-gauge Tru-Cut core needle (p = 0.002).
4. Discussion
The FN and underestimation rates of pathological findings of CNB compared to those of OSB remain an issue in the diagnosis of breast disease.1; 2; 3; 4; 5 ; 9 Our CNB results, which achieved 92.9% sensitivity, 99.7% specificity, 94.8% accuracy, and 5.96% underestimation rates, are compatible with the current reported series.5; 7; 11 ; 14 Of special note is that among our 52 “FN” cases, 13 had CNB atypical ductal hyperplasia and 17 CNB papillary lesions (Table 3). In our institution, atypical ductal hyperplasia and papillary lesions were viewed as indications for further OSB. If we excluded these 30 patients from the so-called “FN” results, the sensitivity would reach 97%. Our current result supported the fact that CNB is a sensitive, highly specific, and well-accepted tool for the diagnosis of breast cancer in Taiwanese women.
Although some studies7; 16; 17 ; 18 discussed the different results obtained by different gauge needle sizes, currently limited information was available focusing on the comparison of diagnostic yield between 14- and 16-gauge needle core biopsy. Nath et al18 conducted a study on biopsy of surgically removed specimens with three different gauges (14, 16, and 18) of core needles. One satisfied core specimen was obtained with each of the three different sizes of needles, which was then compared the diagnosis obtained with surgical excision biopsy result for diagnostic sensitivity and specificity. The authors concluded that biopsy samples obtained with a 14-gauge needle compared with a 16- or 18-gauge needle provide the most accurate diagnosis, which correlates with the diagnosis made with the surgical excision biopsy technique. However, Nath et als18 study was limited by the fact that the CNB was not performed under ultrasound guidance, and only one core of specimen was obtained and compared. Furthermore, that study was conducted at a time when the technique and instrument of large core biopsy were still in the developmental phases, and high-resolution ultrasound was still not available. In our study, compared with the 16-gauge, the 14-gauge needle had higher sensitivity (94.5% vs. 91.9%) and specificity (100% vs. 99.1%); however, both were not statistically significant (p values were 0.17 and 0.38, separately). Higher FN rate (6.5% vs. 3.4%) and underestimation rate (8.8% vs. 2.6%) were found in case of the 16-gauge than the 14-gauge needle. Overall, a 14-gauge core needle is more accurate than a 16-gauge needle (96.6% vs. 93.3%, p = 0.02; Table 3).
The main influence of the various needle gauges selected was the difference of volume retrieval from CNB. The amount of tissue obtained varied with different gauges of automated gun or vacuum-assisted biopsy device. In the vacuum-assisted breast biopsy, 34–40 mg and 94–96 mg per core tissue could be obtained with a 14- and an 11-gauge needle,13; 15 ; 21 respectively, and an eight-gauge vacuum-assisted needle results in a 39% increase in tissue harvesting compared to an 11-gauge needle.14 Nath et al18 revealed that although 14-, 16-, and 18-gauge needles all had the same capacity to hold a 12-mm-long core tissue sample, biopsy sample obtained with the 14-gauge needle is wider and longer compared with the specimens obtained with the 16- and 18-gauge needles. However, in that study, no detailed information about the weight or volume of tissue was revealed per core of different gauges of biopsy. In our breast center, the mean weight of sample harvested per core was 12.7 mg with the 14-gauge automated gun needle and 5.3 mg with the 16-gauge Tru-Cut core needle. A 139.6% increase of tumor volume retrieval was found with the 14-gauge automated core needle than with the 16-gauge Tru-Cut needle per core specimen. A larger core needle obtained more tissue, theoretically creating more chance of correct tissue diagnosis. It is very likely that the larger tumor volume retrieval by the 14-gauge core needle may result in a more accurate diagnostic concordance than that obtained by the smaller 16-gauge needle.
False positivity is the most erroneous result of CNB, which may cause an unnecessary mastectomy and lead to a possible legal problem. Compared with fine needle aspiration cytology with an FP rate of <1%,22 false positivity in CNB is a rarely reported issue. The only one FP result in our series was obtained using a 16-gauge CNB, with an initial diagnosis of a malignant phyllodes tumor, which turned out to be a benign phyllodes tumor in the final surgical pathology report. Fortunately, the patient received a breast conservative surgery, without losing the whole breast. This occurred at an earlier time when CNB was initially used as an alternative diagnosis to OSB, and the pathologist was not familiar with the pathologic results from small core specimen. Since then, the pathologist became more experienced with CNB specimen, and no more FP results were found.
Here, we present our retrospective analysis of 1024 paired CNB and OSB results, derived from 1732 CNB procedures from 1630 patients during a recent study period (2001–2007) when high-resolution ultrasound was available. We tried to delineate the diagnostic yield between 14- and 16-gauge needles of ultrasound-guided CNB by comparison of different parameters, and diagnostic yields in terms of sensitivity, specificity, FP, FN, underestimation, and overall diagnostic accuracy rates. The data presented here were relatively homogeneous with all CNBs being performed under ultrasound guidance, without any mammogram-guided or MRI-guided procedures to interfere the current results. There was less variability in imaging interpretation, biopsy methodology, and number of samples obtained due to the fact that only two experienced breast surgeons completed all the biopsies; this may have eliminated the bias of a learning curve. Of interest, one breast surgeon performed the CNB procedures using 14-gauge needles, while the other preferred using 16-gauge needles. Although this study is retrospective and not randomized, the data were rather homogenous and without the selection bias of needle gauges. However, there were still limitations in this study; about 62% of the benign CNB lesions did not undergo further surgical excision to confirm concordance between CNB and OSB. Furthermore, the average number of tissue specimens retrieved during a 14-gauge biopsy was 3.9 and that during a 16-gauge biopsy was 2.1. This could have resulted in bias in the interpretation of the results comparing the two different gauges in the CNB.
As a whole, our current analysis demonstrated a good diagnostic agreement between ultrasound-guided CNB and subsequent surgical procedures. We also demonstrated that the gauge of the needle influenced the accuracy of pathology findings at CNB. In this analysis, both 14- and 16-gauge needle core biopsies were associated with a more than 90% sensitivity and accuracy rates for malignancy, and a higher than 99% rate of specificity. In terms of accuracy and underestimation rates, 14-gauge needles are a preferred option, as compared with ultrasound-guided biopsies that use 16-gauge needles.
Acknowledgments
Editorial support was provided by Ms Yu-Fen Wang, MS.
References
- 1 S.H. Parker, J.D. Lovin, W.E. Jobe, et al.; Stereotactic breast biopsy with a biopsy gun; Radiology, 176 (1990), pp. 741–747
- 2 S.H. Parker, J.D. Lovin, W.E. Jobe, B.J. Burke, K.D. Hopper, W.F. Yakes; Nonpalpable breast lesions: stereotactic automated large-core biopsies; Radiology, 180 (1991), pp. 403–407
- 3 S.H. Parker, F. Burbank, R.J. Jackman, et al.; Percutaneous large-core breast biopsy: a multi-institutional study; Radiology, 193 (1994), pp. 359–364
- 4 S.H. Parker, F. Burbank; A practical approach to minimally invasive breast biopsy; Radiology, 200 (1996), pp. 11–20
- 5 Y.C. Wu, D.R. Chen, S.J. Kuo; Personal experience of ultrasound-guided 14-gauge core biopsy of breast tumor; Eur J Surg Oncol, 32 (2006), pp. 715–718
- 6 X. Wei, Y. Li, S. Zhang, Y. Zhu, Y. Fan; Experience in large-core needle biopsy in the diagnosis of 1431 breast lesions; Med Oncol, 28 (2011), pp. 429–433
- 7 S. Destounis, M.N. Skolny, R. Morgan, et al.; Rates of pathological underestimation for 9 and 12 gauge breast needle core biopsies at surgical excision; Breast Cancer, 18 (2011), pp. 42–50
- 8 M. Bilous; Breast core needle biopsy: issues and controversies; Mod Pathol, 23 (Suppl. 2) (2010), pp. S36–S45
- 9 H.S. Tseng, Y.L. Chen, S.T. Chen, et al.; The management of papillary lesion of the breast by core needle biopsy; Eur J Surg Oncol, 35 (2009), pp. 21–24
- 10 R.J. Jackman, F. Burbank, S.H. Parker, et al.; Stereotactic breast biopsy of nonpalpable lesions: determinants of ductal carcinoma in situ underestimation rates; Radiology, 218 (2001), pp. 497–502
- 11 G.M. Tse, P.H. Tan; Diagnosing breast lesions by fine needle aspiration cytology or core biopsy: which is better?; Breast Cancer Res Treat, 123 (2010), pp. 1–8
- 12 J.E. Fishman, C. Milikowski, R. Ramsinghani, M.V. Velasquez, G. Aviram; US-guided core-needle biopsy of the breast: how many specimens are necessary?; Radiology, 226 (2003), pp. 779–782
- 13 W.A. Berg, T.L. Krebs, C. Campassi, L.S. Magder, C.C. Sun; Evaluation of 14- and 11-gauge directional, vacuum-assisted biopsy probes and 14-gauge biopsy guns in a breast parenchymal model; Radiology, 205 (1997), pp. 203–208
- 14 R.F. Brem, J.M. Schoonjans, S.N. Goodman, A. Nolten, F.B. Askin, O.M. Gatewood; Nonpalpable breast cancer: percutaneous diagnosis with 11- and 8-gauge stereotactic vacuum-assisted biopsy devices; Radiology, 219 (2001), pp. 793–796
- 15 F. Burbank; Stereotactic breast biopsy: comparison of 14- and 11-gauge Mammotome probe performance and complication rates; Am Surg, 63 (1997), pp. 988–995
- 16 A.P. Lourenco, M.B. Mainiero, E. Lazarus, D. Giri, B. Schepps; Stereotactic breast biopsy: comparison of histologic underestimation rates with 11- and 9-gauge vacuum-assisted breast biopsy; AJR Am J Roentgenol, 189 (2007), pp. W275–W279
- 17 M.L. Darling, D.N. Smith, S.C. Lester, et al.; Atypical ductal hyperplasia and ductal carcinoma in situ as revealed by large-core needle breast biopsy: results of surgical excision; AJR Am J Roentgenol, 175 (2000), pp. 1341–1346
- 18 M.E. Nath, T.M. Robinson, H. Tobon, D.M. Chough, J.H. Sumkin; Automated large-core needle biopsy of surgically removed breast lesions: comparison of samples obtained with 14-, 16-, and 18-gauge needles; Radiology, 197 (1995), pp. 739–742
- 19 Declaration of Helsinki. Ethical principles for medical research involving human subjects. First adopted in Helsinki, Finland, 1964. Revised at the 52nd World Medical Association Assembly in Edinburgh, Scotland, 2000. Note of clarification on Paragraph 29 added by the World Medical Association Assembly, Washington, 2002.
- 20 C.J. D'Orsi, American College of Radiology; BI-RADS: mammography; C.J. D'Orsi (Ed.), American College of Radiology. Breast Imaging Reporting and Data System: ACR BI-RADS-Breast Imaging Atlas (4th ed.), American College of Radiology, Reston, VA (2003)
- 21 F. Burbank, S.H. Parker, T.J. Fogarty; Stereotactic breast biopsy: improved tissue harvesting with the Mammotome; Am Surg, 62 (1996), pp. 738–744
- 22 C.A. Wells, I.O. Ellis, H.D. Zakhour, A.R. Wilson; Guidelines for cytology procedures and reporting on fine needle aspirates of the breast. Cytology Subgroup of the National Coordinating Committee for Breast Cancer Screening Pathology; Cytopathology, 5 (1994), pp. 316–334
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?