Abstract
Background
With the publication of the 2014 Focused Update of the Canadian Cardiovascular Society Guidelines for the Management of Atrial Fibrillation, the Canadian Cardiovascular Society Atrial Fibrillation Guidelines Committee has introduced a new triage and management algorithm; the so-called “CCS Algorithm”. The CCS Algorithm is based upon expert opinion of the best available evidence; however, the CCS Algorithm has not yet been validated. Accordingly, the purpose of this study is to evaluate the performance of the CCS Algorithm in a cohort of real world patients.
Methods
We compared the CCS Algorithm with the European Society of Cardiology (ESC) Algorithm in 172 hospital inpatients who are at risk of stroke due to non-valvular atrial fibrillation in whom anticoagulant therapy was being considered.
Results
The CCS Algorithm and the ESC Algorithm were concordant in 170/172 patients (99% of the time). There were two patients (1%) with vascular disease, but no other thromboembolic risk factors, which were classified as requiring oral anticoagulant therapy using the ESC Algorithm, but for whom ASA was recommended by the CCS Algorithm.
Conclusions
The CCS Algorithm appears to be unnecessarily complicated in so far as it does not appear to provide any additional discriminatory value above and beyond the use of the ESC Algorithm, and its use could result in under treatment of patients, specifically female patients with vascular disease, whose real risk of stroke has been understated by the Guidelines.
Keywords
Atrial fibrillation;Stroke prevention;Antithrombotic;Anticoagulation;CCS Algorithm;Guidelines
1. Introduction
The Canadian Cardiovascular Society Guidelines Committee has recently published the 2014 Focused Update of the Canadian Cardiovascular Society Guidelines for the Management of Atrial Fibrillation [1] (the Guidelines). A fundamental element of the Guidelines is a risk stratification and management algorithm, the purpose of which is to recommend an antithrombotic strategy that is accordant with an individual patients risk of stroke.
The development of a triage and management algorithm has been an evolutionary process. The 2010 Canadian Cardiovascular Society Atrial Fibrillation Guidelines [2] initially recommended the use of the CHADS2 Score [3] to estimate stroke risk. This decision was based upon its “simplicity, familiarity and extensive validation” [2]. The Focused 2012 Update of the Canadian Cardiovascular Society Atrial Fibrillation Guidelines [4] subsequently utilized a modified version of the CHA2DS2-VASc Score [5]. These Guidelines recognized that patients with a CHA2DS2-VASc Score of 0 were at very low risk of stroke, and therefore did not require treatment with any antithrombotic therapy. The Guidelines further noted that patients with a CHADS2 Score of 0 were not necessarily at low risk of stroke [6], and those patients with a CHADS2 Score of 0, but a CHA2DS2-VASc Score of 1 or 2 should be treated with ASA or oral anticoagulation (OAC), as appropriate.
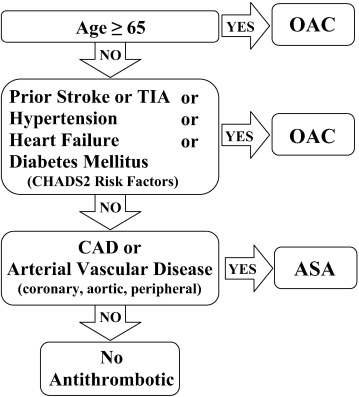
With the publication of the 2014 Focused Update of the Canadian Cardiovascular Society Guidelines for the Management of Atrial Fibrillation [1], the Canadian Cardiovascular Society (CCS) Atrial Fibrillation (AF) Guidelines Committee has introduced a new triage and management algorithm; the so-called “CCS Algorithm” (see Fig. 1). The two key deviations from the previous iteration of the Guidelines are the exclusion of female sex from the CCS Algorithm, and the demotion of vascular disease as a thromboembolic risk factor. The rationale for the decision to modify the algorithm was based upon a review of the Danish National Patient Registry [7], which showed that females with no other thromboembolic risk factors have a 0.9% annual risk of stroke, and that patients with vascular disease, but no other thromboembolic risk factors have a 1.4% annual risk of stroke.
|
|
|
Fig. 1. The “CCS Algorithm”. Adapted from the 2014 Focused Update of the Canadian Cardiovascular Society Guidelines for the Management of Atrial Fibrillation [1]. |
In contrast, the European Society of Cardiology Guidelines (ESC) for the Management of Atrial Fibrillation [8] continues to endorse the use of the CHA2DS2-VASc Score as the principle determinant in the decision to recommend treatment with OAC therapy. Specifically the ESC Guidelines recommend no antithrombotic therapy (No Therapy) for all patients with a CHA2DS2-VASc Score = 0, and female patients with a CHA2DS2-VASc Score = 1, and OAC therapy for all other patients (i.e. for all patients with a CHA2DS2-VASc Score of ≥ 1, except for female patients with a CHA2DS2-VASc Score of 1). This ESC Algorithm is simple and familiar, and has been extensively validated.
It is important to acknowledge, that while the new CCS Algorithm is based upon expert opinion of the best available evidence, it has not yet been validated prior to publication. Accordingly, the purpose of this study is to evaluate the performance of the CCS Algorithm in real world patients. Specifically, we intend to compare the CCS Algorithm with the ESC Algorithm in a cohort of patients who are at risk of stroke due to non-valvular atrial fibrillation.
2. Methods
2.1. Participants
Hospital inpatients with documented non-valvular atrial fibrillation/flutter (AF) in whom anticoagulant therapy was being considered were recruited from Kingston General Hospital, located at Queens University in Kingston, Ontario. Patients were eligible for the study if they had new onset or known AF that was documented on a 12 Lead ECG. Patients were excluded if they had rheumatic heart disease (moderate or severe mitral stenosis), AF due to a reversible cause (peri-operative, thyrotoxicosis), or conditions other than AF that required anticoagulation (prosthetic heart valves, pulmonary embolism). Patients were also excluded if they had a cognitive impairment that, in the judgment of the investigator, resulted in an inability to follow study procedures, or if they were not fluent in the English language. Ethics approval was obtained from the Research Ethics Board at Queens University.
2.2. Data collection
The following details were abstracted from the patient chart and confirmed through verbal interview with the patient: atrial fibrillation history (new onset versus known), atrial fibrillation type (paroxysmal versus persistent), and warfarin use.
After obtaining written informed consent, we then interviewed patients using an iPad questionnaire, “AFib Patient Kiosk” [9]. Individual patients interacted with the iPad directly, and the research assistant remained at the patients side to answer questions and to provide assistance where necessary. The order of the questionnaire was standardized. Patients first provided demographic information (age, sex, and ethnicity) using a multiple choice question format. Next, a personal health history was obtained in order to determine the CHA2DS2-VASc12 (congestive heart failure, hypertension, age, diabetes, previous stroke/TIA, vascular disease, and sex) Score.
2.2.1. Statistical analysis
Statistical analysis was performed using SPSS (version 17, SPSS Inc., Chicago, IL) and statistical significance was established a-priori at α = 0.05. Descriptive data in addition to the CHA2DS2-VASc Score were tabulated for the study cohort. The sample was further divided based upon the presence or absence of vascular disease and was analyzed with one way ANOVA or Chi-square analysis dependent upon the data type.
3. Results
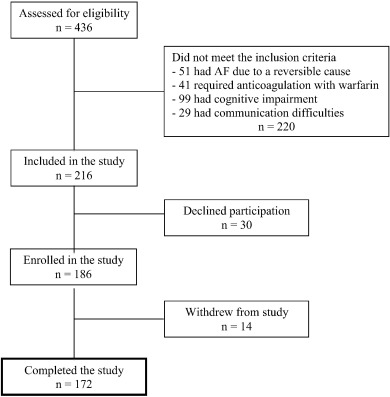
Fig. 2 represents a schematic of the study design. A total of 436 consecutive hospital inpatients were screened for entry into the study between May, 2012 and August, 2012. Of those, 220 patients did not meet eligibility criteria and were excluded, leaving 216 patients who were eligible for inclusion in the study. Reasons for exclusion included AF due to a reversible cause (n = 51), presence of other conditions that required anticoagulation with warfarin (n = 41), cognitive impairment (n = 99) and communication difficulties (n = 29). Thirty patients declined to participate in the study, and 14 patients withdrew from the study part way through completing the questionnaire, leaving 172 patients on whom the primary analysis was performed.
|
|
|
Fig. 2. Schematic representation of patient enrollment. |
3.1. Patient characteristics
The patient characteristics of the study participants are reported in Table 1. The average age of the study participants was 73 ± 12 years. 78% of patients had a known history of AF, and 59% of patients were already on warfarin. The mean CHA2DS2-VASc Score was 3.5 ± 2.0, representing an annual absolute risk of stroke of 6.3%.
| Demographics | n = 172 |
| Age (years) | 73 ± 12 |
| Ethnicity | |
| Caucasian | 164 (95%) |
| Atrial fibrillation history | |
| New onset | 38 (22%) |
| Known | 134 (78%) |
| Atrial fibrillation type | |
| Paroxsymal | 62 (36%) |
| Persistent | 72 (42%) |
| Permanent | 52 (30%) |
| Warfarin | 102 (59%) |
| CHA2DS2-VASc score mean | 3.5 ± 2.0 |
| Congestive heart failure | 37 (22%) |
| Hypertension | 102 (59%) |
| Age ≥ 75 | 81 (47%) |
| Diabetes mellitus | 49 (29%) |
| Stroke, TIA or thromboembolism | 38 (22%) |
| Vascular disease | 79 (46%) |
| Coronary artery disease | 70 (41%) |
| Angina | 32 (19%) |
| Previous myocardial infarction | 42 (24%) |
| Previous PCI | 20 (12%) |
| Previous CABG | 22 (13%) |
| Peripheral arterial disease | 26 (15%) |
| Age 65–74 | 50 (29%) |
| Female sex | 56 (34%) |
3.2. Patient classification
Table 2 illustrates the classification of patients using either the ESC Algorithm or the CCS Algorithm. 10 out of 172 patients (5.8%) had a CHA2DS2-VASc Score of 0, while there was one female patient (0.6%) with a CHA2DS2-VASc Score of 1. Accordingly 11 out of 172 patients (6%) were allocated to No Therapy using the ESC Algorithm. Conversely, 161 out of 172 patients (94%) have a CHA2DS2-VASc Score ≥ 1 (excepting the single female patient with a CHA2DS2-VASc Score of 1), and were therefore allocated to therapy with OAC. Progressing through the CCS Algorithm, 131 out of 172 patients (76%) were aged ≥ 65 years of age, while 28 out of the remaining 40 patients (16%) had one or more of the following “CHDS” risk factors: prior stroke or TIA, hypertension, heart failure or diabetes mellitus. Accordingly 159 out of 172 patients (92%) were allocated to therapy with OAC using the CCS Algorithm. 2 out of 172 patients (1%) had vascular disease as their sole thromboembolic risk factor, and these two patients were allocated to therapy with ASA using the CCS Algorithm. 11 patients (6%) were allocated to No Therapy using the CCS Algorithm, of which one patient was female.
| Therapy | n (%) | Male | Female | |
|---|---|---|---|---|
| ESC Algorithm | ||||
| CHA2DS2-VASc Score ≥ 1a | OAC | 161 (94%) | 106 | 55 |
| CHA2DS2-VASc Score = 0b | No therapy | 11 (6%) | 10 | 1 |
| CCS Algorithm (progressing through algorithm) | ||||
| Age ≥ 65 | OAC | 131 (76%) | 82 | 49 |
| CHDS | OAC | 28 (16%) | 22 | 6 |
| Vascular disease | ASA | 2 (1%) | 2 | 0 |
| No therapy | No therapy | 11 (6%) | 10 | 1 |
- OAC = oral anticoagulant therapy. CHDS = CHF, Htn, diabetes, stroke/TIA.
a. Excluding female patients with a CHA2DS2-VASc Score of 1.
b. Including female patients with a CHA2DS2-VASc Score of 1.
Table 3 presents the contingency table results. 159 out of 172 patients (92%) were recommended OAC therapy by both the ESC Algorithm and the CCS Algorithm. 11 out of 172 patients (6%) were recommended No Therapy by both the ESC Algorithm and the CCS Algorithm. In total, the ESC Algorithm and the CCS Algorithm were concordant in 170/172 patients (99% of the time). There were two patients (male sex with CHA2DS2-VASc Score = 1 due to the presence of vascular disease, but no other thromboembolic risk factors) who were classified as requiring OAC therapy using the ESC Algorithm, but for whom ASA was recommended by the CCS Algorithm.
| CCS Algorithm | Total | ||||
|---|---|---|---|---|---|
| No therapy | ASA | OAC | |||
| ESC algorithm | No therapy | 11 | 0 | 0 | 11 |
| OAC | 0 | 2 | 159 | 161 | |
| Total: | 11 | 2 | 159 | N = 172 | |
- OAC = Oral anticoagulant therapy.
The patient characteristics were then analyzed by vascular disease status (see Table 4). Patients with vascular disease were older (75 ± 10 versus 70 ± 13 years, p = 0.007) than patients without vascular disease, and there was a trend towards a greater proportion of patients with vascular disease being aged ≥ 75 years (54% versus 41%, p = 0.076). Patients with vascular disease were more likely to have a history of heart failure (33% versus 12%, p = 0.001), and the mean CHA2DS2-VASc Score was significantly higher in patients with vascular disease than in patients without vascular disease (4.4 ± 1.9 versus 2.8 ± 1.7, p < 0.001).
| Vascular disease | |||
|---|---|---|---|
| Absent | Present | p Value | |
| (n = 93) | (n = 79) | ||
| Demographics | |||
| Age (years) | 70 ± 13 | 75 ± 10 | 0.007* |
| Ethnicity | |||
| Caucasian | 88 (95%) | 76 (96%) | 0.624 |
| Atrial fibrillation history | |||
| New onset | 19 (20%) | 19 (24%) | 0.568 |
| Known | 74 (80%) | 60 (76%) | |
| Atrial fibrillation type | |||
| Paroxysmal | 41 (44%) | 21 (27%) | 0.027* |
| Persistent | 13 (14%) | 7 (9%) | |
| Permanent | 20 (22%) | 32 (41%) | |
| Warfarin | 52 (56%) | 50 (63%) | 0.326 |
| CHA2DS2-VASc score mean | 2.8 ± 1.7 | 4.4 ± 1.9 | < 0.001* |
| Congestive heart failure | 11 (12%) | 26 (33%) | 0.001* |
| Hypertension | 51 (55%) | 51 (65%) | 0.196 |
| Age ≥ 75 | 38 (41%) | 43 (54%) | 0.076 |
| Diabetes mellitus | 24 (26%) | 25 (32%) | 0.398 |
| Stroke, TIA or thromboembolism | 20 (22%) | 18 (23%) | 0.840 |
| Vascular disease | 79 (100%) | ||
| Coronary artery disease | 70 (89%) | ||
| Angina | 32 (41%) | ||
| Previous myocardial infarction | – | 42 (53%) | – |
| Previous PCI | 20 (25%) | ||
| Previous CABG | 22 (28%) | ||
| Peripheral arterial disease | 26 (33%) | ||
| Age 65–74 | 27 (29%) | 23 (30%) | 0.991 |
| Female sex | 31 (33%) | 25 (32%) | 0.814 |
4. Discussion
The Canadian Cardiovascular Society Atrial Fibrillation Guidelines Committee has introduced the “CCS Algorithm” in the 2014 Focused Update of the Canadian Cardiovascular Society Guidelines for the Management of Atrial Fibrillation. This represents an attempt to further refine the risk stratification, and treatment of patients with non-valvular atrial fibrillation. The CCS Algorithm has not yet been validated prior to publication, and as such, we set out to evaluate the performance of the CCS Algorithm in real world patients by comparing the CCS Algorithm with the ESC Algorithm in a cohort of patients who are at risk of stroke due to non-valvular atrial fibrillation. The results of our study show that, for the vast majority (99%) of patients, there is no difference in recommended therapy between the CCS Algorithm and the ESC Algorithm.
There are, however, two key patient populations that distinguish the CCS Algorithm from the ESC Algorithm; patients with vascular disease but no other thromboembolic risk factors (CHA2DS2-VASc Score = 1), and female patients with vascular disease, but no other thromboembolic risk factors (CHA2DS2-VASc Score = 2).
In our cohort of patients, there were only two patients (1%) with vascular disease but no other thromboembolic risk factors. We found that patients with vascular disease were older, and were more likely to have a history of heart failure than patients without vascular disease. These results are concordant with the Danish National Patient Registry [10], where only 508 out of the 87,202 patients (0.6%) were identified as having vascular disease without any other thromboembolic risk factors. In this same study, patients with vascular disease were found to be older, and were more likely to have heart failure, hypertension, diabetes, and previous thromboembolism. As a result, in patients with atrial fibrillation, it is very unlikely that vascular disease will occur in isolation of other thromboembolic risk factors.
The Guidelines Committee authors recommended the use of ASA for patients with vascular disease without any other thromboembolic risk factors, citing a 1.4% annual risk of stroke for patients with vascular disease but no other thromboembolic risk factors. It is important to note, that this figure that was quoted was for male patients with vascular disease but no other thromboembolic risk factors [7]. The annual stroke rate for female patients with vascular disease but no other thromboembolic risk factors is actually 2.0–2.9% [7]. This is higher than the risk of a patient with hypertension as their sole thromboembolic risk factor (1.6% annual stroke risk [7]), for which OAC is currently recommended by the Guidelines. Arguably these female patients are at sufficiently high risk to justify the use of OAC in preference to ASA. This position is supported by the results of the AVERROES Study [11], which showed that apixaban reduced the risk of stroke by 54% compared to ASA with no increase in major bleeding. As such the routine use of apixaban, in preference to ASA, in female patients with vascular disease, but no other thromboembolic risk factors, would be expected to reduce the annual absolute risk of stroke by 1.1–1.6% with a number needed to treat (NNT) of 13–19 female patients over five years.
As noted by the Canadian Cardiovascular Society Atrial Fibrillation Guideline committee authors, utilizing a simple algorithm is of paramount importance, since the limiting factor to an algorithms success is adoption by clinicians. The simple reality is that if a physician is not able to remember the algorithm, they are not likely to use it. In this regard, it would appear that the CCS Algorithm is unnecessarily complicated in so far as it does not appear to provide any additional discriminatory value above and beyond the use of the dichotomous ESC Algorithm, which is simple, and easily remembered. Further, use of the CCS Algorithm could result in under treatment of patients, specifically female patients with vascular disease, whose real risk of stroke has been understated by the Guidelines.
5. Conclusion
The CCS Algorithm, as proposed by the CCS AF Guideline Committee, does not appear to be any better in the real world setting than simply using the ECS Algorithm. Unlike the CCS Algorithm, the ESC Algorithm is familiar to most clinicians, and can be easily remembered and employed to dichotomize patients into Low Risk (CHA2DS2-VASc Score = 0, and female patients with a CHA2DS2-VASc Score = 1) for thromboembolism, who require No Therapy, or High Risk (CHA2DS2-VASc Score of ≥ 1, except for female patients with a CHA2DS2-VASc Score of 1) for thromboembolism, who do require OAC Therapy. In the opinion of the authors, it is ill advised to recommend ASA in preference to apixaban for patients (male or female, but especially female) with vascular disease as their sole thromboembolic risk factor.
Limitations
This study was conducted on hospital inpatients. As such the findings of this study may not be able to be extrapolated to the outpatient setting. However, the results of the Danish National Patient Registry [7] appear to be concordant with the results of the present study, and therefore, the results of this study can likely be extrapolated to the entire atrial fibrillation population.
Funding
This project was not funded.
Conflict of interest
LaHaye: Has received speaker fees from Bristol-Myers Squibb and Pfizer.
Olesen: Has received speaker fees from Bristol-Myers Squibb and Boehringer Ingelheim, and funding for research from the Lundbeck Foundation, Bristol-Myers Squibb, and The Capital Region of Denmark, Foundation for Health Research.
Lacombe: None declared.
References
- [1] A. Verma, J.A. Cairns, L.B. Mitchell, et al.; 2014 focused update of the Canadian Cardiovascular Society Guidelines for the management of atrial fibrillation; Can J Cardiol, 30 (2014), pp. 1114–1130
- [2] J.A. Cairns, S. Connolly, S. McMurty, et al.; Canadian Cardiovascular Society atrial fibrillation Guidelines 2010: prevention of stroke and systemic thromboembolism in atrial fibrillation and flutter; Can J Cardiol, 27 (2011), pp. 74–90
- [3] B.F. Gage, A.D. Waterman, W. Shannon, M. Boechler, M.W. Rich, M.J. Radford; Validation of clinical classification schemes for predicting stroke; JAMA, 285 (2001), pp. 2864–2870
- [4] A.C. Skanes, J.S. Healey, J.A. Cairns, et al.; Focused 2012 update of the Canadian Cardiovascular Society atrial fibrillation guidelines: recommendations for stroke prevention and rate/rhythm control; Can J Cardiol, 28 (2012), pp. 125–136
- [5] G.Y.H. Lip, R. Nieuwlaat, R. Pisters, D.A. Lane, H.J.G.M. Crijns; Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach; Chest, 137 (2010), pp. 263–272
- [6] J.B. Olesen, C. Torp-Pedersen, M.L. Hansen, G.Y.H. Lip; The value of the CHA2DS2-VASc score for refining stroke risk stratification in patients with atrial fibrillation with a CHADS2 score 0–1: a nationwide cohort study; Thromb Haemost, 107 (2012), pp. 1072–1079
- [7] J.B. Olesen, G.Y. Lip, M.L. Hansen, et al.; Validation of risk stratification schemes for predicting stroke and thromboembolism in patients with atrial fibrillation: nationwide cohort study; BMJ, 342 (2011), p. d124
- [8] A.J. Camm, G.Y.H. Lip, R. De Caterina, et al.; 2012 focused update of the ESC Guidelines for the management of atrial fibrillation; Eur Heart J, 33 (2012), pp. 2719–2747
- [9] Clinical Support Systems; ‘AFib Patient Kiosk’ iPad application available in the iTunes App Store; (February 23, 2012)
- [10] J.B. Olesen, G.Y.H. Lip, D.A. Lane, et al.; Vascular disease and stroke risk in atrial fibrillation: a nationwide cohort study; Am J Med, 125 (2012), pp. e13–e23
- [11] S.J. Connolly, J. Eikelboom, C. Joyner, et al.; Apixaban in patients with atrial fibrillation; N Engl J Med, 364 (2011), pp. 806–817
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?