Abstract
Background
Both Takotsubo cardiomyopathy (TTC) and reverse TTC (r-TTC) are characterized by reversible regional wall motion abnormalities of the heart unrelated to coronary artery pathology. It remains unclear whether and/or how r-TTC differs from TTC. Subarachnoid hemorrhage (SAH) is occasionally causative of TTC/r-TTC, and this study was conducted to detect possible differences between TTC and r-TTC associated with SAH.
Methods
A single-center retrospective study was conducted on 328 consecutive SAH patients. They routinely underwent transthoracic echocardiography (TTE), ECG, and measurements of plasma catecholamines and other cardiac biomarkers within 24 h of admission. Demographic, echocardiographic, electrocardiographic and neurochemical profiles were compared between patients with TTC and r-TTC. The diagnosis of TTC/r-TTC was based on the revised Mayo Clinic Criteria.
Results
Data of 21 SAH-induced TTC and 10 SAH-induced r-TTC patients admitted between January 2009 and December 2014 were analyzed. The patients with r-TTC were significantly younger than those with TTC (51.8 ± 10.9 vs. 63.5 ± 14.4 years, p = 0.04). The former exhibited significantly higher plasma epinephrine levels than the latter (809 ± 710 vs. 380 ± 391 pg/mL, p = 0.04). Plasma norepinephrine levels did not differ significantly (2421 ± 1374 vs. 1724 ± 1591 pg/mL, p = 0.25). No significant differences were observed in other demographic/physiologic variables, echocardiographic parameters, frequency of ECG abnormalities, and 90-day mortality. Moreover, none of the patients who underwent a follow-up TTE exhibited morphologic change from one type to the other.
Conclusions
The pathomechanisms in TTC and r-TTC may not be identical: however, distinguishing the two conditions may not have great importance from the standpoint of clinical management and prognostication.
Keywords
Subarachnoid hemorrhage;Takotsubo cardiomyopathy;Reverse Takotsubo cardiomyopathy;Transthoracic echocardiography
1. Introduction
Takotsubo cardiomyopathy (TTC) is characterized by transient regional wall motion abnormalities (WMA) of the cardiac ventricle(s), and is causally unrelated to coronary artery pathology [1]. Although there is no universally accepted definition of TTC, the revised Mayo Clinic Criteria have been used most commonly [1]. Those criteria state that TTC is transient hypokinesis, akinesis or dyskinesis of the left mid-ventricular segments with or without apical involvement [1]. Meanwhile, a TTC variant, characterized by hypocontractile mid-ventricular segments and a hypercontractile apex, is known and designated as either reverse TTC (r-TTC) or inverted TTC [2]; [3] ; [4]. Plasma catecholamine (epinephrine/norepinephrine) levels are highly elevated in patients with both TTC and r-TTC, and sympathetic nervous system over-activity has been implicated as a common etiological mechanism [2]; [3] ; [4]. Several authors have attempted to identify potential differences between TTC and r-TTC unrelated to neurological diseases, and reported several differences [3] ; [4]. Meanwhile, other authors have argued that TTC and r-TTC may be a temporal evolution of the same disease, based on patients who developed r-TTC several weeks to months after an episode of typical TTC [5]; [6]; [7] ; [8]. Therefore, the question of whether TTC is different from r-TTC has not been answered fully. Reverse TTC is also known to develop in patients with severe brain damage, particularly in those with aneurysmal subarachnoid hemorrhage (SAH) [9]; [10]; [11]; [12] ; [13]. However, only a few case reports of SAH-induced r-TTC are available in the literature [9]; [10]; [11]; [12] ; [13]. This study was conducted to identify possible demographic, physiologic, echocardiographic, electrocardiographic, and neurochemical differences between TTC and r-TTC associated with SAH.
2. Methods
2.1. Patients
This was a retrospective analysis using data acquired prospectively between January 2009 and December 2014. We prospectively performed the following examinations on aneurysmal SAH patients: transthoracic echocardiography (TTE), 12-lead ECG, and measurements of plasma epinephrine/norepinephrine levels and those of other cardiac biomarkers. All three examinations were completed within 24 h of admission. Follow-up TTEs were performed in selected patients, mostly within 7 days of admission. The decision to perform a follow-up TTE was at the discretion of the attending neuro-intensivist. All TTE images were reviewed by a board-certified cardiologist (EW) and an experienced ultrasound technician (KS). The diagnosis of TTC/r-TTC was based on the revised Mayo Clinic Criteria [1] and dichotomization was done jointly by the two authors (EW and KS). SAH severity was evaluated using the World Federation of Neurosurgical Societies (WFNS) SAH score [14]. Concomitant pulmonary edema was diagnosed clinically [13]. Clinical outcomes are represented by 90-day mortality. This study was approved by the internal review board of our institution, and informed consent was obtained from patients or more often, from their surrogates.
2.2. Echocardiographic/electrocardiographic evaluations
For acquisition of TTE, General Electric Vivid 7 (GE Healthcare, Tokyo, Japan) was used. Experienced ultrasound technicians performed all TTE procedures. Left ventricular (LV) dimensions, LV wall thickness, and LV mass were measured according to the recommendations of the American Society of Echocardiography, and LV mass was indexed to body surface area [15] ; [16]. A standard Doppler assessment of diastolic function was performed according to the guidelines of the American Society of Echocardiography [15] ; [16]. Early diastolic (E) wave velocities and atrial (A) wave velocities, and the E wave deceleration time were measured using a pulse wave Doppler recording. Septal and lateral mitral annular early diastolic velocities (E′) were measured from an apical four-chamber view using off-line color tissue Doppler images. The E = velocities from the lateral and septal annuli were averaged (E′), and E/E′ was calculated to assess LV filling pressure. The following images were obtained routinely to evaluate WMA: parasternal long axis; parasternal short axis at the level of the mitral valve, papillary muscles, and apex; apical two-, three-, and four-chamber; subcostal four-chamber; and subcostal short axis. The 16 segment model of the American Society of Echocardiography and the Regional Wall Motion Score Index (RWMSI) were used for analysis [15] ; [16]. The RWMSI was calculated by averaging the scores for all 16 segments, and WMA was defined as a RWMSI ≥ 1.0 [15] ; [16]. The frequencies of WMA were illustrated using the 16 segment model in the patients with TTC and r-TTC. A board-certified cardiologist (EW) determined the presence or absence of ST-segment changes, T-wave inversion, and the mean QTc interval for the ECG evaluation. The frequencies of ST-segment change and T-wave inversion, and mean QTc interval were compared between the two groups.
2.3. Catecholamine/biomarker measurement
Plasma epinephrine and norepinephrine levels were measured by high-performance liquid chromatography. The other cardiac biomarkers measured were troponin I, B-type natriuretic peptide, white blood cell count, and blood glucose levels.
2.4. Statistical analysis
Fishers exact test was used to compare categorical variables, and Students t-test was used to compare continuous variables. Linear regression analysis was performed to evaluate the correlation between plasma epinephrine and norepinephrine levels. JMP software (SAS Institute, Cary, NC, USA) was used for all statistical analyses. Numerical data are expressed as mean ± SD, and p < 0.05 was considered statistically significant.
3. Results
3.1. Background data
A total of 328 consecutive patients with aneurysmal SAH underwent TTE during the 6-year study period. Among them, 21 patients with TTC and 10 with r-TTC were identified. All patients with TTC/r-TTC were ethnic Japanese. The demographic variables compared between the two groups were: age, sex ratio, frequency of WFNS grade IV/V SAH and presence of co-morbid diseases. Patients with r-TTC were significantly younger than those with TTC (51.8 ± 10.9 vs. 63.5 ± 14.4 years, p = 0.04) (Table 1). No significant differences were observed in the other demographic variables (Table 1). The physiological variables measured in the emergency department, including systolic/diastolic blood pressures, heart rates, and the frequency of pulmonary edema were compared, but no significant intergroup differences were observed (Table 1). Similarly, no significant difference was observed in the frequency of patients who required the use of inotropics to maintain systemic circulation (38% in TTC vs. 50% in r-TTC, p = 0.70). No significant difference was detected in 90-day mortality between the TTC and r-TTC groups (33% vs. 50%, p = 0.45).
| TTC (n = 21) | r-TTC (n = 10) | p-Value | |
|---|---|---|---|
| Age (y) | 63.5 ± 14.4 | 51.8 ± 10.9 | 0.04⁎ |
| Male:female | 7:14 | 7:3 | 0.12 |
| Aneurysm locations | MCA 7, ACoA 5, ICA 5, VA 3, BA 1 | VA 5, ACoA 4, MCA 1 | N/A |
| Grade IV/V SAH | 18 (86%) | 10 (100%) | 0.53 |
| Hypertension | 11 (52%) | 6 (60%) | 1.00 |
| Hyperlipidemia | 2 (10%) | 1 (10%) | 1.00 |
| Diabetes mellitus | 1 (5%) | 0 | 1.00 |
| Current smoking | 4 (19%) | 4 (40%) | 0.38 |
| Systolic BP (mm Hg) | 163 ± 57 | 131 ± 42 | 0.12 |
| Diastolic BP (mm Hg) | 96 ± 31 | 79 ± 20 | 0.13 |
| Heart rate (bpm) | 97 ± 29 | 95 ± 20 | 0.86 |
| Pulmonary edema | 5 (24%) | 5 (50%) | 0.22 |
| Need for inotropic agents | 8 (38%) | 5 (50%) | 0.70 |
| 90-day mortality | 7 (33%) | 5 (50%) | 0.45 |
ACoA: anterior communicating artery; BA: basilar artery; BP: blood pressure; GCS: Glasgow Coma Scale; ICA: internal carotid artery; MCA: middle cerebral artery; NA: not applicable; r-TTC: reverse Takotsubo cardiomyopathy; TTC: Takotsubo cardiomyopathy; VA: vertebral artery.
⁎. Statistically significant.
3.2. Echocardiographic/electrocardiographic findings
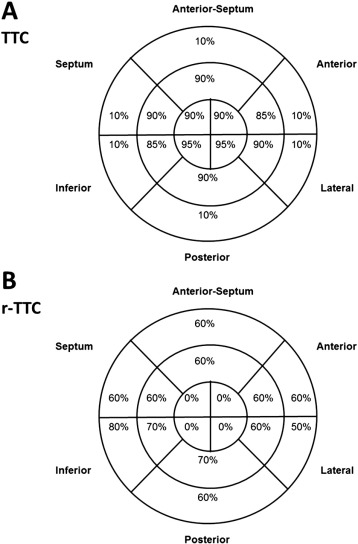
Marked differences in the frequencies of regional WMAs were revealed in basal and apical segments by comparing the 16 segment model between the patients with TTC and r-TTC (Fig. 1A, B). In contrast, no significant intergroup differences were detected in the echocardiographic parameters for systolic/diastolic functions, including LV ejection fraction, E value, E/A ratio or the E/E′ ratio (Table 2). Similarly, no significant intergroup difference was detected in mean RWMSI (Table 2). The frequencies of ECG abnormalities were similar between the two groups (Table 2).
|
|
|
Fig. 1. Comparison of the 16 segment model between Takotsubo cardiomyopathy (TTC, A) and reverse Takotsubo cardiomyopathy (r-TTC, B) associated with subarachnoid hemorrhage revealing that there were marked differences in the frequency of regional wall motion abnormality in the apical and basal segments. |
| TTC (n = 21) | r-TTC (n = 10) | p-value | |
|---|---|---|---|
| LVEF (%) | 43.7 ± 9.7 | 39.8 ± 11.3 | 0.33 |
| LVIDd (mm) | 44.5 ± 7.8 | 47.1 ± 5.1 | 0.36 |
| LVIDs (mm) | 33.3 ± 9.6 | 38.6 ± 4.8 | 0.14 |
| LVMI (g/m2) | 116.1 ± 41.8 | 83.8 ± 14.2 | 0.16 |
| E (m/s) | 69.5 ± 19.2 | 64.1 ± 18.2 | 0.48 |
| A (m/s) | 73.2 ± 24.8 | 65.9 ± 22.7 | 0.46 |
| E/A | 1.07 ± 0.51 | 1.04 ± 0.38 | 0.86 |
| E′ (m/s) | 5.52 ± 1.90 | 6.22 ± 1.78 | 0.35 |
| E/E′ | 13.7 ± 5.6 | 10.9 ± 4.5 | 0.19 |
| DcT (ms) | 189.7 ± 70.5 | 192.2 ± 61.5 | 0.93 |
| RWMSI | 1.77 ± 0.35 | 1.71 ± 0.38 | 0.65 |
| ST segment change | 13/21 (62%) | 7/10 (70%) | 1.00 |
| T-wave inversion | 6/21 (29%) | 1/10 (10%) | 0.38 |
| QTc (ms) | 476 ± 5 | 463 ± 4 | 0.48 |
DcT: deceleration time; LVEF: left ventricular ejection fraction; LVIDd: left ventricular internal dimension, diastole; LVIDs: left ventricular internal dimension, systole; LVMI: left ventricular mass index; RWMSI: Regional Wall Motion Score Index; TTC: Takotsubo cardiomyopathy; r-TTC: reverse Takotsubo cardiomyopathy.
Follow-up TTEs were obtained in 11 (52%) patients with TTC and in five (50%) with r-TTC at a mean interval of 96 ± 43 h in the TTC and 91 ± 46 h in the r-TTC groups. As a result, residual WMAs were observed in eight of the 11 patients with TTC and two of the five with r-TTC (Table 3). The frequencies of residual WMAs did not differ significantly (73% vs. 40%, p = 0.30). None of the 16 patients who underwent follow-up TTE exhibited a morphological change from one type to the other.
| TTC (n = 21) | r-TTC (n = 10) | p-value | |
|---|---|---|---|
| Follow-up TTE available | 11/21 (52%) | 5/10 (50%) | 1.00 |
| Interval between 1st and 2nd TTE (h) | 96 ± 43 | 91 ± 46 | 0.84 |
| Residual TCM/r-TCM in 2nd TTE | 8/11 (73%) | 2/5 (40%) | 0.30 |
r-TTC: reverse Takotsubo cardiomyopathy; TTC: Takotsubo cardiomyopathy; TTE: transthoracic echocardiography.
3.3. Catecholamine/biomarker measurement
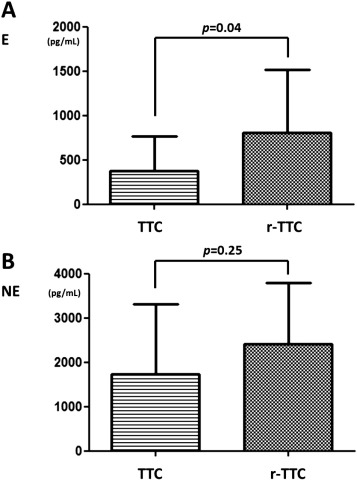
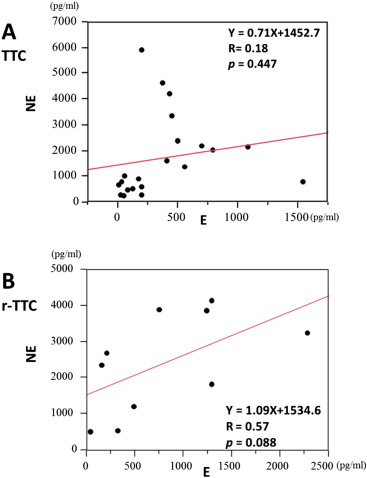
Plasma epinephrine levels (pg/mL) were 380 ± 391 in the patients with TTC and 809 ± 710 in those with r-TTC (p = 0.04, Fig. 2A). Plasma norepinephrine levels (pg/mL) were 1724 ± 1591 in TTC and 2421 ± 1374 in r-TTC, and there was no significant difference (p = 0.25, Fig. 2B). The linear regression analysis showed that plasma epinephrine and norepinephrine levels were not correlated in the patients with TTC (R = 0.18, p = 0.447) (Fig. 3A) and weakly correlated in those with r-TTC (R = 0.57, p = 0.09) (Fig. 3B). No significant differences were detected in the levels of the other biomarkers (Table 4).
|
|
|
Fig. 2. Plasma epinephrine levels (pg/mL) were 380 ± 391 in Takotsubo cardiomyopathy (TTC) and 809 ± 710 in reverse Takotsubo cardiomyopathy (r-TTC) patients (A). The difference was statistically significant (p = 0.04). Plasma norepinephrine levels (pg/mL) were 1724 ± 1591 for TTC and 2421 ± 1374 for r-TTC patients (B). The difference was not statistically significant (p = 0.25). |
|
|
|
Fig. 3. Linear regression analysis showing that the plasma epinephrine and norepinephrine levels were not correlated in the 21 TTC patients (0.18, p = 0.447) (A). The plasma epinephrine and norepinephrine levels were weakly correlated in the 10 r-TTC patients (R = 0.57, p = 0.09) (B). |
| TTC (n = 21) | r-TTC (n = 10) | p-Value | |
|---|---|---|---|
| Troponin I (ng/mL) | 2.21 ± 3.28 | 0.87 ± 0.97 | 0.28 |
| BNP (pg/mL) | 214.8 ± 306.8 | 157.2 ± 192.6 | 0.71 |
| WBC (× 109/L) | 13.6 ± 5.3 | 14.3 ± 5.9 | 0.77 |
| Blood glucose (mg/dL) | 198.5 ± 56.6 | 183.2 ± 69.5 | 0.53 |
BNP: B-type natriuretic peptide; r-TTC: reverse Takotsubo cardiomyopathy; TTC: Takotsubo cardiomyopathy; WBC: white blood cells.
4. Discussion
It is widely accepted that TTC and r-TTC share many characteristics. However, it remains controversial whether r-TTC actually differs demographically, prognostically and neurochemically from TTC. Several authors have reported that patients with r-TTC are significantly younger and have a higher prevalence of triggering stress [3] ; [4]. In contrast, there are patients who experienced two separate episodes of TTC and r-TTC, suggesting that TTC and r-TTC may be a temporal evolution of the same disease [5]; [6]; [7] ; [8]. Most of those studies were performed on patients with idiopathic TTC, i.e., those without neurological disease or pheochromocytoma. However, virtually no study has evaluated the potential differences between TTC and r-TTC in patients with SAH. In this regard, our study may be one of the first to report the presence of substantial differences between these two conditions. This study is also unique in that a team of cardiologists, ultrasound technicians and neurosurgeons jointly evaluated the differences between TTC and r-TTC. The frequency of r-TTC in patients without neurological disease seems to be low; Song et al. reported that the ratio of r-TTC vs. other TTC is approximately 1:4. [3]. In contrast, r-TTC in patients with SAH may occur more commonly, considering a higher r-TTC:TTC ratio of approximately 1:2 in our cohort.
We found that patients with r-TTC were significantly younger than those with TTC (Table 1), which is consistent with previous studies on idiopathic TTC [3] ; [4]. The neurochemical profiles also differed between the patients with TTC and r-TTC (Fig. 2 ; Fig. 3). No cases of crossover, i.e., morphological changes from one type to the other, were found on the second follow-up TTE study. Therefore, TTC and r-TTC may not be identical neurochemically, at least in patients with SAH. From the viewpoint of clinical management, however, there may be few differences between TTC and r-TTC, except that the latter tend to be more hypotensive (Table 1): neither 90-day mortality nor the need for inotropic agents differed significantly. Similarly, few differences were found in the TTE parameters or ECG findings (Table 2), despite marked morphological differences on TTE. Therefore, distinguishing TTC from r-TTC may not be very important to neurosurgeons, cardiologists or intensivists for planning the treatment strategy or predicting outcomes in SAH patients. The follow-up TTE study results indicated that r-TTC may resolve more rapidly than TTC, as WMA had resolved in 60% of r-TTC patients on the second TTE performed 4 days after the first. In contrast, only 27% of TTC patients exhibited normalized cardiac wall motion. No significant differences were observed because of the small number of patients, and it remains to be seen whether speed of recovery truly differs between patients with TTC and r-TTC.
Among many neurochemical substances etiologically associated with cardiac WMA, epinephrine and norepinephrine may be the most important [12]. As plasma levels of both catecholamines are highly elevated after stressful events, such as aneurysm rupture, it is difficult to determine which catecholamine plays a more active role in the pathogenesis of TTC and/or r-TTC. Unintentional (frequently iatrogenic) epinephrine administration may provide unique insight, because many cases of iatrogenic r-TTC have been associated with exogenous epinephrine administration in the literature [17]; [18]; [19]; [20]; [21]; [22]; [23] ; [24]. Our finding of extremely elevated epinephrine levels in patients with r-TTC may also support its etiological role. The higher epinephrine–norepinephrine correlation coefficient in patients with r-TTC compared to those with TTC (Fig. 3A, B) is also reasonable. However, our findings may not be explained by the working hypothesis that a difference in the distribution of β1/β2-adrenoceptors between the apex and base, with denser β2-adrenoceptor distribution in the apex, is the reason for the greater contractile response to epinephrine in the apical myocardium with subsequent apical stunning [25]: according to this hypothesis, higher epinephrine levels would lead to typical TTC rather than to r-TTC [25]. Further clinical and experimental studies are warranted to elucidate the role of each catecholamine and its adrenoceptor in the pathogenesis of TTC and r-TTC [26].
Several limitations of this study should be mentioned. First, this was a retrospective observational study; thus, it is impossible to prove the causality of elevated epinephrine in the pathogenesis of r-TTC. Second, dichotomization into TTC and r-TTC may have been too simplistic, considering that as many as four TTC variants have been proposed [27]. Although this dichotomization has been adopted by several authors, categorical overlap might have occurred, particularly involving the mid-ventricular segments. Third, the number of patients was small: given that both conditions have low incidences making it difficult to accumulate an adequate number of samples, it may be important to establish national/international TTC registries [28]. Fourth, because of the short half-life of epinephrine, the epinephrine/norepinephrine coefficient can vary substantially with the timing of blood sample collection [29]. Finally, the follow-up TTEs were conducted in only half of the patients, and the interval between the first and second TTEs may have been too short; therefore, it may be too early to conclude that a morphological change from one type to the other does not occur in patients with SAH.
5. Conclusion
Patients with SAH-induced r-TTC were significantly younger and exhibited higher plasma epinephrine levels than those with SAH-induced TTC. These results suggest that the pathomechanisms of the two conditions may not be identical. However, distinguishing between TTC and r-TTC in patients with SAH may not have great importance from the standpoint of clinical management and prognostication.
Conflict of interest
The authors declare that there is no conflict of interest regarding this manuscript.
Acknowledgement
The corresponding author (JI) received a research grant from the Japan Society for the Promotion of Science (JSPS KAKENHI Grant Number 26462173).
References
- [1] D.C. Scantlebury, A. Prasad; Diagnosis of Takotsubo cardiomyopathy; Circ. J., 78 (2014), pp. 2129–2139
- [2] P. Angelini; Reverse, or inverted, transient Takotsubo cardiomyopathy: terms and status of an open discussion; Tex. Heart Inst. J., 40 (2013), pp. 60–63
- [3] B.G. Song, W.J. Chun, Y.H. Park, et al.; The clinical characteristics, laboratory parameters, electrocardiographic, and echocardiographic findings of reverse or inverted Takotsubo cardiomyopathy: comparison with mid or apical variant; Clin. Cardiol., 34 (2011), pp. 693–699
- [4] R. Ramaraj, M.R. Movahed; Reverse or inverted Takotsubo cardiomyopathy (reverse left ventricular apical ballooning syndrome) presents at a younger age compared with the mid or apical variant and is always associated with triggering stress; Congest. Heart Fail., 16 (2010), pp. 284–286
- [5] S. Chattopadhyay, J. John; Tako-tsubo and reverse Tako-tsubo cardiomyopathy: temporal evolution of the same disease?; Eur. Heart J., 30 (2009), p. 2837
- [6] N.F. Ehl, M. Zurek, H. Rickli, M.T. Maeder; “Double Takotsubo”: first description of the sequence of classical followed by inverted type in a young woman; Int. J. Cardiol., 174 (2014), pp. e36–e37
- [7] O. Wever-Pinzon, J. Wever-Pinzon, L. Tami; Recurrent Takotsubo cardiomyopathy presenting with different morphologic patterns; Int. J. Cardiol., 148 (2011), pp. 379–381
- [8] F. Migliore, A. Zorzi, M. Perazzolo Marra, et al.; Typical and atypical Takotsubo syndrome in the same patient; Int. J. Cardiol., 162 (2013), pp. e28–e30
- [9] C.J. Waller, B. Vandenberg, D. Hasan, A.B. Kumar; Stress cardiomyopathy with an “inverse” Takotsubo pattern in a patient with acute aneurysmal subarachnoid hemorrhage; Echocardiography, 30 (2013), pp. E224–E226
- [10] P.V. Ennezat, D. Pesenti-Rossi, J.M. Aubert, et al.; Transient left ventricular basal dysfunction without coronary stenosis in acute cerebral disorders: a novel heart syndrome (inverted Takotsubo); Echocardiography, 22 (2005), pp. 599–602
- [11] S. Shoukat, A. Awad, D.K. Nam, et al.; Cardiomyopathy with inverted Tako-tsubo pattern in the setting of subarachnoid hemorrhage: a series of four cases; Neurocrit. Care., 18 (2013), pp. 257–260
- [12] K. Sugimoto, J. Inamasu, Y. Hirose, et al.; The role of norepinephrine and estradiol in the pathogenesis of cardiac wall motion abnormality associated with subarachnoid hemorrhage; Stroke, 43 (2012), pp. 1897–1903
- [13] J. Inamasu, M. Nakatsukasa, K. Mayanagi, et al.; Subarachnoid hemorrhage complicated with neurogenic pulmonary edema and Takotsubo-like cardiomyopathy; Neurol. Med. Chir. (Tokyo), 52 (2012), pp. 49–55
- [14] H. Sano, A. Satoh, Y. Murayama, et al.; Modified World Federation of Neurosurgical Societies subarachnoid hemorrhage grading system; World Neurosurg., 83 (2015), pp. 801–807
- [15] M. Hravnak, J.M. Frangiskakis, E.A. Crago, et al.; Elevated cardiac troponin I and relationship to persistence of electrocardiographic and echocardiographic abnormalities after aneurysmal subarachnoid hemorrhage; Stroke, 40 (2009), pp. 3478–3484
- [16] M. Tanabe, E.A. Crago, M.S. Suffoletto, et al.; Relation of elevation in cardiac troponin I to clinical severity, cardiac dysfunction, and pulmonary congestion in patients with subarachnoid hemorrhage; Am. J. Cardiol., 102 (2008), pp. 1545–1550
- [17] P. Esnault, L. Née, T. Signouret, N. Jaussaud, F. Kerbaul; Reverse Takotsubo cardiomyopathy after iatrogenic epinephrine injection requiring percutaneous extracorporeal membrane oxygenation; Can. J. Anaesth., 61 (2014), pp. 1093–1097
- [18] G. Khoueiry, N. Abi Rafeh, B. Azab, et al.; Reverse Takotsubo cardiomyopathy in the setting of anaphylaxis treated with high-dose intravenous epinephrine; J. Emerg. Med., 44 (2013), pp. 96–99
- [19] I.V. Litvinov, M.A. Kotowycz, S. Wassmann; Iatrogenic epinephrine-induced reverse Takotsubo cardiomyopathy: direct evidence supporting the role of catecholamines in the pathophysiology of the “broken heart syndrome”; Clin. Res. Cardiol., 98 (2009), pp. 457–462
- [20] J. Tomcsányi, H. Arabadzisz, T. Frész, et al.; Reverse Takotsubo syndrome pattern induced by local anaesthesia; Orv. Hetil., 149 (2008), pp. 2387–2389
- [21] O.A. Kajander, M.P. Virtanen, S. Sclarovsky, K.C. Nikus; Iatrogenic inverted Takotsubo syndrome following intravenous adrenaline injections for an allergic reaction; Int. J. Cardiol., 165 (2013), pp. e3–e5
- [22] T. Härle, K. Kronberg, H. Nef, H. Möllmann, A. Elsässer; Inverted Takotsubo cardiomyopathy following accidental intravenous administration of epinephrine in a young woman; Clin. Res. Cardiol., 100 (2011), pp. 471–473
- [23] C.J. Magri, S. Fava, H. Felice; Inverted Takotsubo cardiomyopathy secondary to adrenaline injection; Br. J. Hosp. Med. (Lond), 72 (2011), pp. 646–647
- [24] A. Manzanal, L. Ruiz, J. Madrazo, M. Makan, J. Perez; Inverted Takotsubo cardiomyopathy and the fundamental diagnostic role of echocardiography; Tex. Heart Inst. J., 40 (2013), pp. 56–59
- [25] A.R. Lyon, P.S. Rees, S. Prasad, P.A. Poole-Wilson, S.E. Harding; Stress (Takotsubo) cardiomyopathy—a novel pathophysiological hypothesis to explain catecholamine-induced acute myocardial stunning; Nat. Clin. Pract. Cardiovasc. Med., 5 (2008), pp. 22–29
- [26] B. Redfors, A. Ali, Y. Shao, J. Lundgren, L.M. Gan, E. Omerovic; Different catecholamines induce different patterns of Takotsubo-like cardiac dysfunction in an apparently afterload dependent manner; Int. J. Cardiol., 174 (2014), pp. 330–336
- [27] E. Kazakauskaitė, A. Jankauskas, T. Lapinskas, R. Ordienė, E. Ereminienė; Takotsubo cardiomyopathy: the challenging diagnosis in clinical routine; Medicina (Kaunas), 50 (2014), pp. 1–7
- [28] J.R. Ghadri, F. Ruschitzka, T.F. Lüscher, C. Templin; Takotsubo cardiomyopathy: still much more to learn; Heart, 100 (2014), pp. 1804–1812
- [29] D.S. Goldstein, G. Eisenhofer, I.J. Kopin; Sources and significance of plasma levels of catechols and their metabolites in humans; J. Pharmacol. Exp. Ther., 305 (2003), pp. 800–811
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?