Abstract
Objective
To determine the outcomes of patients with chest pain (CP) and prior history of coronary artery disease (CAD) managed with observation followed by outpatient stress myocardial perfusion imaging (MPI).
Methods
Retrospective analysis of patients with CP managed with observation followed by outpatient stress MPI, comparing cardiovascular (CV) event rates stratified by CAD history.
Results
375 patients were included: 111 with and 264 without a CAD history. All patients underwent outpatient stress MPI within 72 h of observation. MPI identified patients at risk for CV events. However, while patients with negative MPI and without a CAD history had very low rates of short- and long-term CAD events (0.8%, 0.8%, and 1.3% at 30 days, 1 year, and 3 years, respectively), event rates of those with a negative test but a CAD history were significantly higher (2.6%, 5.3%, and 6.6% at 30 days, 1 year and 3 years, respectively; p = 0.044 and p = 0.034 compared to CAD− patients at 1 year and 3 years, respectively). In a multivariable logistic regression model, a positive MPI proved to be an independent predictor of long-term CV events in patients with CP and prior CAD.
Conclusion
Observation followed by stress MPI can effectively risk stratify CP patients with prior CAD for CV risk. These patients are at increased risk of CV events even after a low-risk stress MPI study. Patients presenting with CP and managed with a strategy of observation followed by a negative stress MPI warrant close short- and long-term monitoring for recurrent events.
Abbreviations
CP, chest pain;CAD, coronary artery disease;MPI, myocardial perfusion imaging;CV, cardiovascular;ACS, acute coronary syndrome;ECG, electrocardiogram;TnI, troponin I
Keywords
Myocardial perfusion imaging;Chest pain;Coronary artery disease;Stress testing
1. Introduction
Chest pain (CP) accounts for greater than 8 million emergency department visits and 2 million hospital admissions per year in the United States [1] ; [2]. As a result, the economic burden of CP management is enormous and methods to reduce the cost of managing chest pain are the subject of a large body of literature. An increasingly popular strategy for the management of CP patients over that past decade has been the use of the emergency department (ED)-based observation unit [3] ; [4]. This strategy typically involves a defined period of observation of less than 24 h, during which time high risk CP features associated with an acute coronary syndrome (ACS) such as changes in the electrocardiogram (ECG) or elevated biomarkers are excluded. Patients are then discharged from the observation unit following arrangement of clinical follow-up. An integral part of this approach is stress testing with or without cardiac imaging to further risk stratify patients, with testing typically performed either immediately or several days after ACS has been ruled out [1].
A growing body of literature has demonstrated the cost-effectiveness and safety of an observation unit strategy in identifying CP patients who can be safely discharged either following stress testing or with plans for early follow-up stress testing [5] ; [6]. Studies have shown that patients managed in a CP unit followed by a non-ischemic outpatient stress test have very low short- and long-term rates of cardiovascular (CV) events. Of note, the vast majority of these studies have been generated using patient cohorts without known CAD. There have been limited studies that have attempted to address the appropriate criteria for CP observation admission [7], and even fewer studies have examined outcomes of patients with known CAD who present with CP and are managed using an observation strategy [8] ; [9].
In the present study we evaluated the use of stress myocardial perfusion imaging in the management of patients with prior documented CAD who present with CP and are triaged to a CP observation unit. Our goal was to determine these patients' short- and long-term outcomes as well as the prognostic value of stress myocardial perfusion imaging (MPI) in predicting adverse CV events.
2. Methods
The study was a retrospective evaluation of a strategy of observation followed by outpatient stress MPI. Patients who met entry criteria and who were entered into the observation program during calendar years 2005–2007 were included in the analysis. The study was approved by the Institutional Review Board of Lehigh Valley Health Network.
The Lehigh Valley Health Network chest pain observation program utilizes continuous cardiac telemetry beds on a dedicated unit of the hospital. To be admitted to the unit, patients are required to have 3 specific criteria on presentation to the ED: resolution of their CP during initial ED evaluation and treatment, a normal initial cardiac troponin I (TnI), and an initial ECG that is normal or unchanged versus a prior ECG. For the present study patient demographics and history were collected from documentation of the admission assessment. Patients were considered to have a “history of CAD” if they had prior MI or coronary revascularization. Patients whom the ED staff suspected to have alternative diagnoses (such as pulmonary embolism or aortic dissection) were considered for admission to the unit if these alternative diagnoses were definitively ruled out by appropriate imaging studies. Patients were excluded from the unit if they had abnormal levels of TnI and are presenting ECG which was different from prior tracings or recurrent chest pain following admission. Patients were kept on continuous telemetry until at least 2 negative TnI results were obtained on presentation and at least 12 h after admission to the unit. If any of the TnI were abnormal or the patient developed recurrent pain with new ECG changes or arrhythmias they were withdrawn from the observation protocol and treated accordingly. Following the negative observation workup patients were scheduled for an outpatient stress test with myocardial perfusion imaging within 72 hours after discharge. They were given instructions on preparation for the test and a contact number to call if they were unable to comply with the instructions.
Stress testing was carried out using a standard treadmill exercise Bruce protocol. Tc99-Sestamibi was utilized as the resting and post-exercise MPI agent per standard protocol. For patients that were unable to exercise, pharmacologic stressor utilizing either adenosine or dobutamine was performed. Exercise and pharmacologic ECG tests were interpreted as “positive” for ischemia if the ECG demonstrated ≥1 mm flat or slow upsloping ST depression in 2 or more contiguous leads. Exercise ECG responses were termed “indeterminate” if the patient failed to achieve a peak heart rate of 85% maximum predicted heart rate or baseline ECG abnormalities precluded the ability to interpret stress-related changes. Tc99-Sestamibi MPI scans were defined as “positive for ischemia” if the post-exercise or post-adenosine perfusion scan demonstrated reduced tracer uptake in ≥1 myocardial perfusion segment that was not present on the resting scan. Quantitative degrees of ischemia (i.e., ischemic segment models) were not reported, as these are not routinely used in the nuclear reports at our center. Scans were interpreted as “negative for ischemia” if no such areas were detected. The management of patients with positive stress MPI was left to the discretion of the cardiologist who followed up with each patient following the completion of the test.
Patients were assessed for survival status based on review of the national death database. Cardiac events were extracted from the hospital electronic medical record. Adverse cardiac events that were included as endpoints were death, myocardial infarction or the requirement for urgent percutaneous or surgical coronary revascularization. Patients who underwent elective catheterization either with or without percutaneous coronary intervention for positive MPI were not counted as a CV endpoint unless they presented with evidence of an unstable coronary syndrome before or at the time of the procedure.
Continuous data were analyzed using Students t-test and categorical data were interpreted using a chi-squared test. All data analyses were performed using SigmaStat software (Systat, Chicago IL). For all statistical analyses a p value < 0.05 was considered significant.
3. Results
A total of 375 patients completed the observation protocol and outpatient stress testing, and had complete 3 year follow-up data available. It should be noted that these patients were identified after completion of the CP unit protocol: thus, data on the number of patient who “failed” the CP unit protocol and were converted to inpatient status is not available. Of these patients, 111 (29.6%) had a history of CAD. Demographics and clinical characteristics of patients with and without CAD history are summarized in Table 1. Compared to patients without CAD history, patients with a CAD history were older and more likely to be male and have diabetes mellitus, hypercholesterolemia, and hypertension. Not surprisingly, patients with a CAD history were significantly more likely to be taking ASA, clopidogrel (both alone and in combination with ASA), and statins, which would represent appropriate secondary prevention measures for these patients.
| + CAD history (n = 111) | − CAD history (n = 264) | p | |
|---|---|---|---|
| Age, years (range) | 65.3 (51–89) | 52.4 (19–86) | < 0.001 |
| Male, % | 69.4 | 52.3 | 0.003 |
| Hypertension, % | 90.1 | 37.9 | < 0.001 |
| Diabetes mellitus, % | 33.3 | 9.5 | < 0.001 |
| Current/prior smoker, % | 6.3 | 12.5 | 0.111 |
| Hypercholesterolemia, % | 95.5 | 33.0 | < 0.001 |
| Family history CAD, % | 5.4 | 10.6 | 0.160 |
| ASA use, % | 81.1 | 16.7 | < 0.001 |
| Clopidogrel use, % | 45.0 | 1.1 | < 0.001 |
| ASA + clopidogrel use, % | 39.6 | 0.4 | < 0.001 |
| Statin use, % | 80.2 | 25.0 | < 0.001 |
Of the patients with a CAD history, 72/111 (64.9%) underwent exercise stress testing and 39 underwent pharmacologic testing. Of the patients without a CAD history, 224/264 (84.8%) underwent exercise stress testing and 40 underwent pharmacologic testing. There were no CV complications during stress testing in our patient population as a whole. Stress testing, MPI results, and early (within 1 week following stress testing) cardiac catheterization data are summarized in Table 2. While there was no significant difference between rates of positive stress ECG between patients with and without a CAD history, significantly more patients with a CAD history had MPI scans interpreted as ischemic (31.5% vs. 10.6%, p < 0.001) and had reduced left ventricular ejection fraction (< 50%) in gated SPECT assessment (17.9% vs. 5.7%, p < 0.001). Based on the results of post-discharge stress myocardial perfusion imaging, significantly more patients with a CAD history were referred for cardiac catheterization and coronary angiography vs. patients without a CAD history (13.5% vs. 5.3%, p = 0.012). A total of 15 patients underwent revascularization (12 PCIs, 3 CABG). Twelve of the 15 patients who underwent revascularization had ischemic MPI; the remaining 3 had positive stress ECG. In patients with history of CAD, 5 PCIs and 1 CABG were performed. While in patients without CAD history, there were 7 PCIs and 2 CABG.
| + CAD history (n = 111) | − CAD history (n = 264) | p | |
|---|---|---|---|
| Stress ECG ischemic (%) | 19 (17.1) | 35 (13.3) | 0.102 |
| SPECT MIBI ischemic (%) | 35 (31.5) | 28 (10.6) | < 0.001 |
| Gated SPECT EF < 0.50 | 20 (17.9) | 18 (5.7) | < 0.001 |
| Cardiac cath (%) | 15 (13.5) | 14 (5.3) | 0.012 |
Cumulative cardiovascular event rates at 30 days, 1 year, and 3 years following ED observation and outpatient stress testing were compared between patients with and without a CAD history (Table 3A). Not surprisingly, patients with documented prior CAD history had higher CV event rates throughout the follow-up period, with a nearly 4-fold increase in CV events by 3 years of follow-up in patients with known CAD. There were 2 deaths in the cohort during the follow-up period — a 72 year old male with prior CAD expired 2 years after a positive stress MPI from a gastrointestinal bleed, and a 50 year old female without prior CAD expired 1 year after an ischemic MPI from sudden cardiac death following non-cardiac surgery. No patients who underwent index revascularization had a CV event during the 3 year follow-up period. Three patients who underwent cardiac cath but no PCI had CV events during the f/u period (1 at 30 days, 2 at 3 years).
| + CAD history (n = 111) | − CAD history (n = 264) | p | |
|---|---|---|---|
| 30 day CV event (%) | 7 (6.3) | 7 (2.7) | 0.169 |
| 1 year CV event (%) | 10 (9.0) | 8 (3.0) | 0.026 |
| 3 year CV event (%) | 13 (11.7) | 10 (3.8) | 0.002 |
We next evaluated the prognostic power of stress myocardial MPI for predicting CV events in patients both with and without a CAD history (Table 3B). In the patient cohort without known CAD, a negative MPI conferred a very low event rate at follow-up (0.8% at 1 year to 1.3% at 3 years). At each of the 3 follow-up time points, patients with inducible ischemia on MPI were significantly more likely to have a CV event. In the patient cohort with known CAD, the results of stress MPI also demonstrated some prognostic value: CAD patients with ischemic MPI were more likely to have a CV event at each follow-up time point, although this difference was only significant at 3 year follow-up.
| + CAD history (n = 111) | − CAD history (n = 264) | |||||
|---|---|---|---|---|---|---|
| MPI + (n = 35) | MPI− (n = 76) | p | MPI + (n = 28) | MPI − (n = 236) | p | |
| 30 day CV events (%) | 5 (14.3) | 2 (2.6) | 0.053 | 5 (17.9) | 2 (0.8) | < 0.001 |
| 1 year CV events (%) | 6 (17.1) | 4 (5.3) | 0.097 | 6 (21.4) | 2 (0.8) | < 0.001 |
| 3 year CV events (%) | 8 (22.9) | 5 (6.6) | 0.031 | 7 (25.0) | 3 (1.3) | < 0.001 |
A negative post-discharge stress MPI is known to confer a very low risk of adverse CV events at both short- and long-term follow-up periods in patients with low-risk chest pain [1] ; [10]. To determine if a negative stress test confers a similar low rate of CV events in patients with a CAD history, we examined the predictive value of a negative stress ECG and MPI in patients with vs. without prior CAD. Patients without a CAD history and normal stress ECG had extremely low CV event rates (0.5% at 30 days, 1 year, and 3 years). In contrast, patients with ischemic stress ECG tests had 30 day, 1 year, and 3 year event rates of 3.1%, 6.2%, and 10.7%, respectively (p = 0.297, p = 0.016, and p < 0.001 vs. event rates of patients without CAD history).
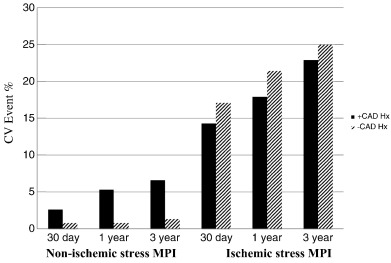
Comparison of event rates following a negative MPI in patients with vs. without a CAD history is summarized in Fig. 1. Patients without prior CAD diagnosis and with a non-ischemic stress MPI had very low cumulative event rates up to 3 years of follow-up (0.8%, 0.8%, and 1.3% at 30 days, 1 year, and 3 years, respectively). In comparison, patients with known CAD and negative MPI had significantly higher event rates throughout the follow-up period (2.6%, 5.3%, and 6.6% at 30 days, 1 year, and 3 years, respectively). In contrast, while as expected patients with abnormal MPI results had higher rates of CV events vs. those with normal MPI, there was no significant difference in follow-up CV event rates after an abnormal MPI when comparing the patient cohorts with and without a CAD history.
|
|
|
Fig. 1. Follow-up event rates after ischemic and non-ischemic stress MPI, comparing patients with and without CAD history (black bars = + CAD history; striped bars = − CAD history). |
Patients in our cohort with a CAD history were noted to have significantly greater rates of several key risk factors, including older age and greater prevalence of hypertension, diabetes mellitus, hypercholesterolemia, and reduced ejection fraction. It would be theoretically possible that the higher long-term rates of CAD events in this population were due entirely to accumulated effects of these risk factors, and positive MPI testing simply identified patients with the greatest risk factor burden and thus did not have independent prognostic value in this population. For this reason we performed multivariate logistic regression to determine the independent predictive value of an ischemic MPI in a model that included previously identified risk factors that were more prevalent in the cohort with a CAD history (Table 4). We did not include ejection fraction as we did not find increased rates of 3 year adverse events in patients with reduced ejection fraction in our raw data. In this model, a positive stress MPI was in fact the only independent predictor of long term (3 year) adverse CV events (OR 5.00, 95% CI 1.41–17.80, p = 0.013). Thus, a positive stress MPI following a period of observation was a powerful independent predictor of long-term CV events in patients with CP and prior CAD history. Furthermore, in this model unlike MPI, the stress ECG result was not an independent predictor of 3 year outcomes. Thus, MPI added significant prognostic power to routine ECG stress testing in our patient population.
| Variable | Odds ratio | 95% CI | p |
|---|---|---|---|
| Age | 0.96 | 0.90–1.01 | 0.138 |
| Sex (M) | 1.21 | 0.26–5.65 | 0.813 |
| Hypertension | 0.95 | 0.12–7.40 | 0.959 |
| Diabetes mellitus | 0.75 | 0.16–3.62 | 0.722 |
| Hypercholesterolemia | 0.18 | 0.02–3.62 | 0.134 |
| Stress ECG positive | 0.89 | 0.40–1.97 | 0.777 |
| MPI positive | 5.00 | 1.41–17.80 | 0.013 |
4. Discussion
The use of an observation unit has become an increasingly popular modality for the management of CP in US emergency departments [1] ; [2]. These units allow efficient and rapid identification and disposition of low-risk chest pain patients to outpatient follow-up and risk stratification without the need for inpatient hospitalization. Moderate-sized studies have supported the safety of this strategy [4] ; [5]. In general, patients who have immediate or early follow-up stress tests that do not reveal inducible ischemia have very low follow-up CV event rates [10]. In the present study we evaluated the diagnostic utility of expanding the chest pain observation strategy to patients with known CAD and history of prior CV events. Our results demonstrate that while these patients can be effectively risk stratified with a strategy of observation followed by early outpatient stress testing, the overall risk of future CV events and the prognostic implications of an ischemic stress MPI study are very different in these patients compared to those who present with low-risk CP but without a CAD history.
Two notable prior studies suggested higher rates of positive stress tests and resultant coronary revascularization in patients with prior CAD who were managed in a chest pain observation unit [8] ; [9]. Madsen et al. retrospectively examined the rate of failure of observation status in 531 patients at a single center [8]. Patients with a CAD history were significantly more likely to require inpatient admission and catheterization and revascularization vs. those patients without a CAD history. Nabi et al. prospectively followed 1576 consecutive patients who were seen in a single emergency room for CP and followed for CV events over an average 7 month period [9]. The 189 patients in the cohort with a CAD history had significantly higher event rates vs. the patients without a CAD history. It should be noted that the majority of events in this study (56 of 77 or 72.3%) occurred during the index hospitalization; thus further information is needed regarding the long-term event rate in patients with known CAD and prior CV events managed with a CP observation strategy. The present study confirms the findings of these studies and adds important additional data regarding long-term event rates in patients with CP and prior CAD diagnoses. To the best of our knowledge the present study is the largest study examining long term (up to 3 year) outcomes of patients with a CAD history managed with a chest pain unit strategy. Specifically, we demonstrate that patients with prior CAD but a negative MPI continue to accrue CAD events compared to those without a CAD history at longer term follow-up. Thus, the increased rate of events in this population is not accounted for only by increased rates of revascularization during or shortly after the index hospitalization.
The finding that patients with known CAD and a negative stress MPI have higher event rates vs. those without CAD and a negative test is not surprising. The finding of a negative stress test in a patient without known CAD very likely indicates that the patient indeed is free of hemodynamically significant coronary stenoses, and such a patient would be expected to have a low risk of CV events at follow-up. Additionally, in this study we considered abnormal MPI based completely on the presence of ischemia on post-stress images, and we did not assess the prognostic effect of the finding of fixed defect/scar on MPI. It is likely that fixed defects were more common in our cohort with a CAD history, and this finding is known to be associated with higher rates of subsequent CV events [11].
Recently, the appropriateness of the practice of performing early stress testing on chest pain patients following a period of observation has been questioned, given the lack of data regarding the impact of this strategy on patient outcomes and the lack of a clear-cut benefit of invasive procedures on patients found to have ischemia on follow-up noninvasive testing [12] ; [13]. Furthermore, recent studies have offered evidence for the use of alternative strategies for risk stratifying chest pain patients, including CT angiography [14]; [15] ; [16] and positron emission tomography MPI [17]. The present study does not attempt to address either of these controversies, although it does identify a subset of patients who are often managed using an observation strategy and are at particularly high risk of subsequent CV events. As such, this subset of chest pain observation patients need to be a focus of future studies evaluating the benefit of any post-observation imaging strategy on patient outcomes.
Our study has several weaknesses. Because it is retrospective, we do not have data available on the number or characteristics of patients who dropped out of the observation protocol due to recurrent pain or high risk findings such as positive TnI, as these patients would not have met criteria for entry into our database. A prior study documented a significantly higher rate of observation status “failure” among patients with known CAD [7]. Knowledge of the rate at which patients with prior CAD “fail” an observation protocol is critical to the determination of the optimal method for triaging chest pain in this subset of patients. Additionally, because our medical center is not a “closed” hospital system, we were unable to assess follow-up CV events that may have been managed at hospitals not linked to our electronic medical record.
In conclusion, our study confirms the safety of a strategy of observation followed by outpatient stress testing in CP patients who have a prior CAD history. Our data also clearly supports the need for additional caution in managing these patients, and in particular highlights the need to follow these patients particularly closely, even after the reassurance of a low risk post-discharge stress test.
Conflict of interest
The authors report no relationships that could be construed as a conflict of interest.
References
- [1] E.A. Amsterdam, J.D. Kirk, D.B. Diercks, W.R. Lewis, S.D. Turnipseed; Exercise testing in chest pain units: rationale, implementation, and results; Cardiol Clin, 23 (2005), pp. 503–516
- [2] E.P. Hess, D.M. Nestler; Transforming the emergency department observation unit: a look into the future; Clin Cardiol, 30 (2012), pp. 501–521
- [3] A.K. Venkatesh, B.P. Geisler, J.J. Gibson Chambers, et al.; Use of observation care in US emergency departments, 2001–2008; PLoS One, 6 (9) (2011), p. e24326
- [4] W.R. Lewis, E.A. Amsterdam, S. Turnipseed, J.D. Kirk; Immediate exercise testing of low risk patients with known coronary artery disease presenting to the emergency department with chest pain; J Am Coll Cardiol, 33 (1999), pp. 1843–1847
- [5] E.A. Amsterdam, J.D. Kirk, D.B. Diercks, W.R. Lewis, S.D. Turnipseed; Immediate exercise testing to evaluate low-risk patients presenting to the emergency department with chest pain; J Am Coll Cardiol, 40 (2002), pp. 251–256
- [6] S.W. Goodacre, F.M. Morris, S. Campbell, K. Angelini; A prospective, observational study of a chest pain observation unit in a British hospital; Emerg Med J, 19 (2002), pp. 117–121
- [7] K. Wilkinson, H. Severance; Identification of chest pain patients appropriate for an emergency department observation unit; Emerg Med Clin North Am, 19 (1) (2001), pp. 35–66
- [8] T. Madsen, P. Bossart, J. Bledsoe, et al.; Patients with coronary artery disease fail observation status at higher rates than patients without coronary disease; Am J Emerg Med, 28 (2010), pp. 19–22
- [9] F. Nabi, S.M. Chang, J. Xu, E. Gigliotti, J.J. Mahmarian; Assessing risk in acute chest pain: the value of stress myocardial perfusion imaging in patients admitted through the emergency department; J Nucl Cardiol, 19 (2) (2012), pp. 233–243
- [10] L.D. Metz, M. Beattie, R. Hom, R.F. Redberg, D. Grady, K.E. Fleischmann; The prognostic value of normal stress myocardial perfusion imaging and exercise echocardiography: a meta-analysis; J Am Coll Cardiol, 49 (2007), pp. 227–237
- [11] E. Braunwald, R.H. Jones, D.B. Mark, et al.; Diagnosing and managing unstable angina. Agency for health care policy and research; Circulation, 90 (1994), pp. 613–622
- [12] S.C. Penumetsa, J. Mallidi, J.L. Friderici, W. Hiser, M.B. Rothberg; Outcomes of patients admitted for observation of chest pain; Arch Intern Med, 172 (11) (2012), pp. 873–877
- [13] V. Prasad, M. Cheung, A. Cifu; Chest pain in the emergency department: the case against our current practice of routine noninvasive testing; Arch Intern Med, 172 (19) (2012), pp. 1506–1509
- [14] U. Hoffmann, Q.A. Truong, D.A. Schoenfeld, et al.; Coronary CT angiography versus standard evaluation in acute chest pain; N Engl J Med, 367 (4) (2012), pp. 299–308
- [15] H.I. Litt, C. Gatsonis, B. Snyder, et al.; CT angiography for safe discharge of patients with possible acute coronary syndromes; N Engl J Med, 366 (15) (2012), pp. 1393–1403
- [16] V.L. Priest, P.A. Scuffham, R. Hachamovitch, T.H. Marwick; Cost-effectiveness of coronary computed tomography and cardiac stress imaging in the emergency department; J Am Coll Cardiol Img, 4 (5) (2011), pp. 549–556
- [17] S. Dorbala, M.F. Di Carli, R.S. Beanlands, et al.; Prognostic value of stress myocardial perfusion positron emission tomography: results from a multicenter observational registry; J Am Coll Cardiol, 61 (2) (2013), pp. 176–184
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?