Abstract
Objective
The role of plate configuration was found inconclusive on the biomechanical effects of the plate size and hole number for dual plate constructions in humeral shaft fractures. The purpose of this study was to test the biomechanical stability of various dual plate constructions.
Methods
Twenty-four left humeri (4th Generation Composite Humerus, Sawbones, Malmö, Sweden) with comminuted midshaft humeral fracture were used. Four groups of plate constructs were tested: laterally fixed 8-hole locking plate and screws were combined with anteriorly locking plates containing 0, 4, 6, or 8 holes in groups I, II, III, and IV, respectively. The alterations in axial, bending, and torsional angles were recorded.
Results
There were no fixation failures during axial, bending, or torsional stiffness testing within the elastic behavior limits. Axial stiffness was highest in Group IV. Torsional stiffness, posterior-to-anterior bending stiffness, lateral-to-medial bending stiffness, and medial-to-lateral bending stiffness were lowest in Group I.
Conclusion
The similar stiffness values for the 8-to-4 hole and 8-to-6 hole plate constructions indicate that the 8-to-4 hole construction is an option in young adults, while the stiffest 8-to-8 hole combination may be an option for osteoporotic patients.
Keywords
Humeral shaft fractures ; Dual plate ; Fixation
Introduction
Diaphyseal humeral fractures are seen relatively more frequently in the elderly population.1 Even though nonoperative treatment is preferable, osteopenia as a result of lack of use leads to the need for options for internal fixation to avoid high levels of disability associated with humeral shaft nonunion.2
In humeral shaft fractures managed by surgery, the conventional manner for internal fixation is the use of large fragment plates. However, the variable size and shape of the humerus creates difficulties during the procedure in determining the appropriate combination of plate size and screw number.3 The recent literature indicates that the use of dual plate yields better results in terms of mechanical properties than does the use of large fragment plate.4 In the use of dual plate, the layout angles of the plates relative to the humeral shaft is controversial. Placement of the anterior and lateral plates at 90° was found to be best configuration for dual plating.5
Despite the increased usage of locking plates in osteoporotic humeral shaft fractures, the few studies on the plate configuration were inconclusive regarding the biomechanical effects of plate size and hole number in dual plate constructions. The purpose of this study was to test the biomechanical stability of various dual plate constructions.
Patients and methods
Twenty-four left humeri (4th Generation Composite Humerus, Sawbones, Malmö, Sweden) were used in the present study. The specimens were embedded in cement at both ends, which were cut into a cylindrical shape to facilitate insertion into the testing grips. The center of the bone was determined by vernier calipers, and a comminuted midshaft humeral fracture was modeled with a 1-cm midshaft gap created with a surgical reciprocating saw.6 ; 7 ; 8 All specimens were prepared by the same 2 orthopedic surgeons. Standard technique for plate fixation was performed, placing all of the screws bicortically. The osteotomy provided a noncontact situation, allowing for isolated testing of the plate constructs.
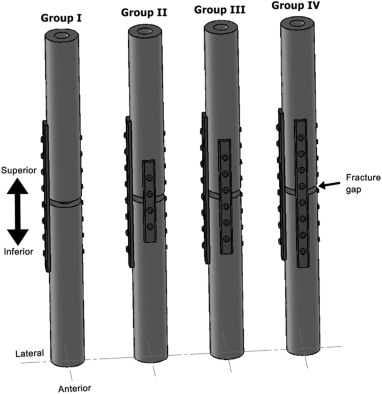
Four groups of plate constructs were tested. Group I specimens were fixed laterally by an 8-hole 3.5-mm locking plate (8hLP) (all locking plates used in this study were produced by Med Tıp Medical Device Company A.S., Izmir, Turkey), Group II specimens were fixed laterally with an 8hLP and anteriorly with a 4hLP, Group III were fixed laterally with an 8hLP and anteriorly with a 6hLP, and Group IV were fixed both laterally and anteriorly with an 8hLP (Fig. 1 ).
|
|
|
Fig. 1. Schematic illustration of the plate configurations. |
All tests were performed with a mechanical test machine (AG-IS 10 kN, Shimadzu, Kyoto, Japan). The humeral bone models were fixed to the load cell of the test machine. The axial load was applied to the cylindrical embedded end (Fig. 2 ). In all tests, the alterations in axial, bending, and torsional angles were recorded both in loaded and unloaded states.
|
|
|
Fig. 2. Axial load was applied to the cylindrical potted end. |
The bone-plate constructs were tested under axial loading with the embedded humeral head. While simultaneously recording the vertical displacement and strain, 500 N for 5000 cycles at 3 Hz were applied. Displacement was recorded.4
A 4-point bending model was used for the anterior-posterior, posterior-anterior (sagittal plane), medial-lateral, and lateral-medial (coronal plane) testing. In each bending test, a maximal load of 250 N was applied at 10 mm/min. Bending moment was applied to the same point by centering the device on the midpoint of the fracture gap. Load versus displacement values were recorded to calculate the bending stiffness and flexibility.
Torsion test was performed with a servo sync torque machine (SQM132, 245 Nm 100 rpm, ELSIM Elektroteknik A.S, Istanbul, Turkey). The torsion tests were conducted in the displacement control mode with a maximum moment of 4.5 Nm in both directions; the premoment was 0 Nm, and the test velocity was 0.3°/second. The testing cycle was applied from 0 to 4.5 Nm. Torque versus the degree of angle deformation values were recorded.7 ; 8 ; 9
Each specimen was tested 3 times in bending and torsion tests to ensure reproducibility of the results. All tests were performed within the elastic behavior limits of the construct; the load–deflection data did not show any sign of plastic or permanent deformation for any of the constructs in any orientation. The testing was performed in the same order for each sample. Statistical analysis was conducted with Mann–Whitney U test by using SPSS software (version 15.0, SPSS Inc., Chicago, IL, USA). The level for significance was defined as p < 0.05.
Results
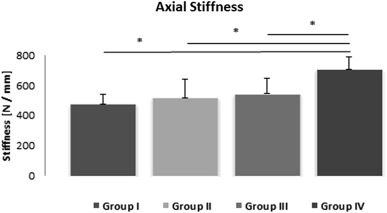
There were no fixation failures during axial, bending, or torsional stiffness testing within the elastic behavior limits. Mean stiffness values of all groups are presented in Table 1 . Axial stiffness in Group IV was 706.2 N/mm, which was significantly higher than in Group I (475.6 N/mm, p = 0.004), Group II (516.6 N/mm, p = 0.025), and Group III (543.5 N/mm, p = 0.006) (Fig. 3 ).
| Axial stiffness (N/mm) | Bending stiffness (N/mm) | Rotational stiffness (N/º) | ||||
|---|---|---|---|---|---|---|
| A-P | P-A | L-M | M-L | |||
| Group I | 475,6 ± 63 | 340,4 ± 37 | 285,8 ± 24 | 134,5 ± 4 | 196,55 ± 28 | 6,3 ± 2 |
| Group II | 516,6 ± 124 | 372,7 ± 41 | 424,8 ± 39 | 413,1 ± 23 | 382,3 ± 17 | 12,1 ± 3,9 |
| Group III | 543,5 ± 102 | 330,4 ± 39 | 430,8 ± 125 | 373,3 ± 46 | 411,9 ± 100 | 11,5 ± 4,3 |
| Group IV | 706,2 ± 78 | 414,6 ± 96 | 509,1 ± 135 | 410,3 ± 69 | 496,9 ± 174 | 15,1 ± 5,7 |
|
|
|
Fig. 3. Axial stiffness according to groups. |
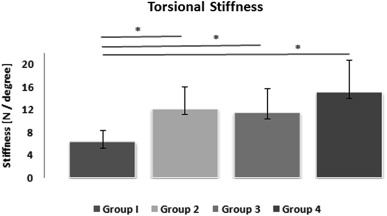
For torsional stiffness measurements, stiffness in Group I was 6.31 N/degree, which was significantly lower than in Group II (12.16 N/degree, p = 0.01), Group III (11.51 N/degree, p = 0.01), and Group IV (15.10 N/degree, p = 0.006) (Fig. 4 ).
|
|
|
Fig. 4. Torsional stiffness according to groups. |
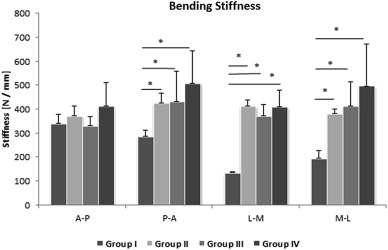
Bending stiffness was also compatible with the previously described results. By all of the measured parameters of stiffness (posterior-anterior bending, lateral-medial bending, medial-lateral bending) results for Group I were significantly lower than for all of the other groups (Fig. 5 ).
|
|
|
Fig. 5. Bending stiffness according to groups. |
Discussion
Plate fixation is the gold standard for treatment of humeral nonunion. It enables compression, correction of malalignment, and stimulation of osteogenesis (grafting) in a single procedure.10 Humeral nonunion can be severely disabling. Although several authors have recommended plate fixation for the management of nonunion at midshaft level, inappropriate plate fixation techniques are one of the main reasons that fractures fail to heal.11 ; 12 ; 13 ; 14 ; 15 ; 16 Foster et al reported that the most common indication for surgical management of a humeral shaft fracture is a concurrent multiple injury, and the second is nonunion of humeral shaft fracture. They reported a 96% success rate for union in their study, using both single- and dual-plate constructs either with or without lag screws.11 Murray et al pioneered the use of double-plate constructs for nonunion in 1964. Using an anterolateral approach, they placed 1 plate on the lateral side of the humerus and the other on the posterior aspect. They suggested that this method provides a more stable construct than that achieved with single plates because of the biplanar control provided by dual plates at right angles to each other.14
In our study, we investigated the in vitro mechanical stability of different dual plate constructs. It is apparent in the literature that use of the dual plate construct in the treatment of humeral fractures has a significantly higher mechanical stability compared to the single plate application.6 Similar to the published results, our study confirmed that the dual plate construct had a significantly higher stability than single plate fixation.
In the treatment of nonunions, which arise from simple transverse fractures of long bones like the humerus and ulna, the increased stability with dual plates may lead to union.17 Egol et al suggested a theoretical concern for the amount of soft-tissue dissection and revascularization needed to place a second plate at a 90° angle to the first.18 ; 19 Although this is a concern in the treatment of acute fractures, in the case of nonunions, the dissection needed to correct the deformity and debride the fibrous tissue allows application of the second plate without additional exposure. Furthermore, a study by Rubel et al showed that the addition of a second plate did not increase the rate of treatment failure.20 The results of our biomechanical tests in the gap model suggest that higher axial and rotational stiffness is achieved with a dual plate construct. It has been shown that a dual plate construct is sometimes helpful when bone quality is poor and pseudoarthrosis is present or when the stability achieved by the first plate is not clinically sufficient.11 The use of dual plate provided healing in nonunion patients in such situations. In our study, performed on the humerus transverse fracture model, 8-hole single plate fixation (Group I) showed statistically significant lower stiffness than the dual plate (Group II, Group III, Group IV) constructions. There were no statistical differences between the 8-hole lateral plate fixation combined with a second 90 ̊ anterior plate with 4 holes (Group II) or with 6 holes (Group III). The plate combinations with 8-hole plate lateral and 8-hole plate anterior construct (Group IV) had significantly higher axial stiffness. However, Group IV showed excessive stiffness, in which the fixation construct reduces stress and strain on the bone and may lead to bone resorption.20
Construct stiffness is highly important. It governs the performance of the fixation system, using the other interrelated outcomes measures reported (bone stress shielding, hardware stress, and interfragmentary strain),4 ; 7 which eventually causes screw loosening and construct failure.21 ; 22 ; 23 However, excessive reductions in stiffness may lead to increased screw and plate stress and early fatigue failure of the construct.22 ; 23 ; 24 Stiffness resulting from the compressive loading simulations of the humerus may be especially important during crutch weight-bearing.8 ; 22 Moreover, torsional loading also is of interest in the analysis of humeral fracture fixation constructs because it has been reported as a predominant loading mode and possible cause for nonunion of humeral fractures.22 ; 24 ; 25 Hertel et al recommended obtaining a minimum of 3 cortices per segment.26 In good quality bone, Gautier and Sommer recommended using a minimum of 2 screws per segment, with at least 3 cortices for simple fractures and 4 cortices for comminuted fractures. In other cases such as osteoporotic bone, they recommended a minimum of 3 screws per segment.22 Stoffel et al found that axial stiffness and torsional rigidity were mainly influenced by the distance between the fracture site and the closest screw. After moving the screw 1 hole farther from the fracture, the construct became almost twice as flexible in compression and torsion.23 The development of locking plates has provided an alternative to standard compression plates. Locking plates can provide fracture fixation without the undesirable effects on periosteal vascularization and mechanical drawbacks that are encountered with standard compression plates.24
Biomechanics of the fixation device is only one of many factors to be considered in the operative treatment of humeral fractures. Although numerous factors affect operative treatment decisions, it is helpful for the orthopedic surgeon to have comparative biomechanical information of different plating constructs. Because the amount of motion at the fracture site influences the biologic reaction of bone, the biomechanical stability of a fracture fixation implant plays an important role in fracture healing.21 ; 27 ; 28 ; 29
This biomechanical study might have a critical role in determining the appropriate construction in the treatment of humeral shaft nonunion. Our results suggest that, depending on the fracture type, in young adult patients, lateral 8-hole and anterior 4-hole plate constructions may be used, while in osteoporotic patients, lateral 8-hole and anterior 6-hole plate constructions may be utilized. Aziz et al reported that the strengths of the cortical screws are significantly lower according to their pullout tests on osteoporotic bone.30 In osteoporotic bone, insufficient screw purchase leads to loosening of nonlocking screws and levering of the plate away from the bone. Loosening of nonlocking screws in osteoporotic bone is an important factor in implant failure in humeral shaft fracture fixation.31 The stability of the fixation system is influenced by hardware factors including the number of screws, type of screws (i.e., bicortical, unicortical), working length, plate offset from the bone cortex, and placement of the hardware.8 ; 22 ; 32 Ideal plate fixation in shaft fractures should have at least 6 (or preferably 8) cortex fixations above and below the fracture line.33 In addition to plate placement, the hardware variables were controlled in this study based on recommendations from the literature.17 ; 21 In our study, all of the lateral locked plates used 4 screws per fragment, based on the literature findings that additional screws did not show a significant increase in torsional stiffness.5 ; 23
In conclusion, in the treatment of nonunion or pseudoarthrosis of humeral fractures, dual plate fixation is a technique that increases the stability and healing rates. As shown in our results of similar stiffness values for the 8-to-4 hole and 8-to-6 hole plate construction, an 8-to-4 hole construction may be suggested as an option in young adults, while an 8-to-8 hole combination, the overall stiffest combination, may be an option for osteoporotic patients. Further studies are required to understand the biomechanical behavior of osteoporotic bones on dual plate fixation.
Conflict of interest
None declared.
References
- 1 J.A. Baron, M. Karagas, J. Barrett, et al.; Basic epidemiology of fractures of the upper end and lower limb among Americans over 65 years of age; Epidemiology, 7 (1996), pp. 612–618
- 2 D. Ring, B.H. Perey, J.B. Jupiter; The functional outcome of ununited fractures of the humeral diaphysis in older patients; J Bone Jt Surg Am, 81 (1999), pp. 177–190
- 3 R. Patel, C.P. Neu, S. Curtiss, D.P. Fyhrie, B. Yoo; Crutch weightbearing on comminuted humeral shaft fractures: a biomechanical comparison of large versus small fragment fixation for humeral shaft fractures; J Orthop Trauma, 25 (2011), pp. 300–305
- 4 A. Watts, P. Weinhold, W. Kesler, L. Dahners; A biomechanical comparison of short segment long bone fracture fixation techniques: single large fragment plate versus 2 small fragment plates; J Orthop Trauma, 26 (2012), pp. 528–532
- 5 V. Kosmopoulos, A.D. Nana; Dual plating of humeral shaft fractures: orthogonal plates biomechanically outperform side-by-side plates; Clin Orthop Relat Res, 472 (4) (2014 Apr), pp. 1310–1317 http://dx.doi.org/10.1007/s11999-013-3379-7 Epub 2013 Nov 12. PubMed PMID: 24218163; PubMed Central PMCID: PMC3940765
- 6 N.C.1 Tejwani, A. Murthy, J. Park, T.M. McLaurin, K.A. Egol, F.J. Kummer; Fixation of extra-articular distal humerus fractures using one locking plate versus two reconstruction plates: a laboratory study; J Trauma, 66 (3) (2009 Mar), pp. 795–799 http://dx.doi.org/10.1097/TA.0b013e318181e53c
- 7 D.C. Fitzpatrick, J. Doornink, S.M. Madey, M. Bottlang; Relative stability of conventional and locked plating fixation in a model of the osteoporotic femoral diaphysis; Clin Biomech, 24 (2009), pp. 203–209
- 8 R.V. O'Toole, R.C. Andersen, O. Vesnovsky, et al.; Are locking screws advantageous with plate fixation of humeral shaft fractures? a biomechanical analysis of synthetic and cadaveric bone; J Orthop Trauma, 22 (10) (2008 Nov–Dec), pp. 709–715 http://dx.doi.org/10.1097/BOT.0b013e31818df8cb)
- 9 J. Blum, H. Machemer, F. Baumgart, U. Schlegel, D. Wahl, P.M. Rommens; Biomechanical comparison of bending and torsional properties in retrograde intramedullary nailing of humeral shaft fractures; J Orthop Trauma, 13 (5) (1999 Jun-Jul), pp. 344–350 PubMed PMID: 10406701
- 10 K.P. Padhye, V.S. Kulkarni, G.S. Kulkarni, et al.; Plating, nailing, external fixation, and fibular strut grafting for non-union of humeral shaft fractures; J Orthop Surg (Hong Kong), 21 (3) (2013 Dec), pp. 327–331 PubMed PMID: 24366794
- 11 R.J. Foster, G.L. Dixon Jr., A.W. Bach, R.W. Appleyard, T.M. Green; Internal fixation of fractures and non-unions of the humeral shaft. Indications and results in a multi-center study; J Bone Jt Surg Am, 67 (6) (1985 Jul), pp. 857–864 PubMed PMID:4019533
- 12 C.L. Lin, C.K. Fang, F.Y. Chiu, C.M. Chen, T.H. Chen; Revision with dynamic compression plate and cancellous bone graft for aseptic nonunion after surgical treatment of humeral shaft fracture; J Trauma, 67 (6) (2009 Dec), pp. 1393–1396 http://dx.doi.org/10.1097/TA.0b013e31818c1595 PubMed PMID: 20009693
- 13 R.K. Marti, C.C. Verheyen, P.P. Besselaar; Humeral shaft nonunion: evaluation of uniform surgical repair in fifty-one patients; J Orthop Trauma, 16 (2) (2002 Feb), pp. 108–115 PubMed PMID: 11818806
- 14 W.R. Murray, D.B. Lucas, VTi Inman; Treatment of non-union of fractures of the long bones by the two plate method; J Bone Jt Surg Am, 46 (1964 Jul), pp. 1027–1048 PubMed PMID: 14192498
- 15 A.B. Spitzer, R.I. Davidovitch, K.A. Egol; Use of a “hybrid” locking plate for complex metaphyseal fractures and nonunions about the humerus; Injury, 40 (3) (2009 Mar), pp. 240–244 http://dx.doi.org/10.1016/j.injury.2008.07.019 Epub 2009 Feb 4. PubMed PMID:19195653
- 16 A.P. Van Houwelingen, M.D. McKee; Treatment of osteopenic humeral shaft nonunion with compression plating, humeral cortical allograft struts, and bone grafting; J Orthop Trauma, 19 (1) (2005 Jan), pp. 36–42 PubMed PMID: 15668582
- 17 K.A. Egol, E.N. Kubiak, E. Fulkerson, F.J. Kummer, K.J. Koval; Biomechanics of locked plates and screws; J Orthop Trauma, 18 (8) (2004 Sep), pp. 488–493 Review. PubMed PMID:15475843
- 18 A. Zhiquan, Z. Bingfang, W. Yeming, Z. Chi, H. Peiyan; Minimally invasive plating osteosynthesis (MIPO) of middle and distal third humeral shaft fractures; J Orthop Trauma, 21 (9) (2007 Oct), pp. 628–633 PubMed PMID: 17921838
- 19 H.J. Lee, C.W. Oh, J.K. Oh, et al.; Minimally invasive plate osteosynthesis for humeral shaft fracture: a reproducible technique with the assistance of an external fixator; Arch Orthop Trauma Surg, 133 (5) (2013 May), pp. 649–657 http://dx.doi.org/10.1007/s00402-013-1708-7 Epub 2013 Mar 5. PubMed PMID: 23463256
- 20 S.L. Woo, W.H. Akeson, R.D. Coutts, et al.; A comparison of cortical bone atrophy secondary to fixation with plates with large differences in bending stiffness; J Bone Jt Surg Am, 58 (2) (1976 Mar), pp. 190–195
- 21 I.F. Rubel, P. Kloen, D. Campbell, et al.; Open reduction and internal fixation of humeral nonunions : a biomechanical and clinical study; J Bone Jt Surg Am, 84-A (8) (2002 Aug), pp. 1315–1322 PubMed PMID: 12177259
- 22 E. Gautier, C. Sommer; Guidelines for the clinical application of the LCP; Injury, 34 (Suppl 2) (2003 Nov), pp. B63–B76 Review. PubMed PMID: 14580987
- 23 K. Stoffel, U. Dieter, G. Stachowiak, A. Gächter, M.S. Kuster; Biomechanical testing of the LCP–how can stability in locked internal fixators be controlled?; Injury, 34 (Suppl 2) (2003 Nov), pp. B11–B19 PubMed PMID: 14580982
- 24 S.L. Tan, Z.J. Balogh; Indications and limitations of locked plating; Injury, 40 (7) (2009 Jul), pp. 683–691 http://dx.doi.org/10.1016/j.injury.2009.01.003 Epub 2009 May 22. Review. PubMed PMID: 19464682
- 25 J.P. Verbruggen, W. Sternstein, J. Blum, P.M. Rommens, J.W. Stapert; Compression-locked nailing of the humerus: a mechanical analysis; Acta Orthop, 78 (1) (2007 Feb), pp. 143–150 PubMed PMID: 17453406
- 26 R. Hertel, H. Eijer, A. Meisser, C. Hauke, S.M. Perren; Biomechanical and biological considerations relating to the clinical use of the Point Contact-Fixator–evaluation of the device handling test in the treatment of diaphyseal fractures of the radius and/or ulna; Injury, 32 (Suppl 2) (2001 Sep), pp. B10–B14 PubMed PMID: 11718734
- 27 I. Mehling, K. Schmidt-Horlohé, L.P. Müller, W. Sternstein, J. Korner, P.M. Rommens; Locking reconstruction double plating of distal humeral fractures: how many screws in the distal ulnar column segment in A3 fracture provide superior stability? A comparative biomechanical in vitro study; J Orthop Trauma, 23 (8) (2009 Sep), pp. 581–587 http://dx.doi.org/10.1097/BOT.0b013e3181a87725 PubMed PMID: 19704274
- 28 D.J. Hak, P. Althausen, S.J. Hazelwood; Locked plate fixation of osteoporotic humeral shaft fractures: are two locking screws per segment enough?; J Orthop Trauma, 24 (4) (2010 Apr), pp. 207–211 http://dx.doi.org/10.1097/BOT.0b013e3181bdd1da PubMed PMID:20335752
- 29 M.L. Prasarn, J. Ahn, O. Paul, et al.; Dual plating for fractures of the distal third of the humeral shaft; J Orthop Trauma, 25 (1) (2011 Jan), pp. 57–63 http://dx.doi.org/10.1097/BOT.0b013e3181df96a7 Erratum in: J Orthop Trauma. 2013 Sep;27(9):541. PubMed PMID: 21085023
- 30 M.S. Aziz, B. Nicayenzi, M.C. Crookshank, H. Bougherara, E.H. Schemitsch, R. Zdero; Biomechanical measurements of cortical screw purchase in five types of human and artificial humeri; J Mech Behav Biomed Mater, 30 (2014 Feb), pp. 159–167 http://dx.doi.org/10.1016/j.jmbbm.2013.11.007 Epub 2013 Nov 19. PubMed PMID: 24295967
- 31 R. Frigg; Locking compression plate (LCP). An osteosynthesis plate based on the dynamic compression plate and the point contact fixator (PC-Fix); Injury, 32 (Suppl 2) (2001 Sep), pp. 63–66 PubMed PMID: 11718740
- 32 M. Wagner; General principles for the clinical use of the LCP; Injury, 34 (Suppl 2) (2003 Nov), pp. B31–B42 Review. PubMed PMID: 14580984
- 33 M. Walker, B. Palumbo, B. Badman, J. Brooks, J. Van Gelderen, M. Mighell; Humeral shaft fractures: a review; J Shoulder Elb Surg, 20 (5) (2011 Jul), pp. 833–844 http://dx.doi.org/10.1016/j.jse.2010.11.030 Epub 2011 Mar 9. Review. PubMed PMID: 21393016
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?