To the Editor,
We read with interest the article by Ng and Cheong.1 The authors reported a rare case of spontaneous sigmoid perforation in a 17-year-old man with Ehlers–Danlos syndrome. Spontaneous perforation of the colon is rare and can represent rare entities. Here, we present a rare case of spontaneous perforation of the colon in end colostomy.
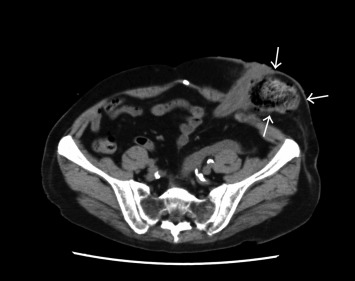
A 78-year-old man with severe chronic constipation presented with a 1-day history of fever, lower abdominal pain, and watery colostomy output. He underwent abdominoperitoneal resection for rectal cancer 14 years prior, and a colostomy on his left lower abdomen. Physical examination revealed redness and tenderness around the colostomy site. Computed tomography of the abdomen revealed an aberration of feces under the skin from the proximal end of the colostomy site, in addition to fecal impaction; the inflammation extended along the subdermal fascia toward his back (Figure 1). A diagnosis of perforation of the colon proximal to the colostomy stoma was established. The patient immediately underwent fenestration drainage. A perforation of 3 cm in diameter in the wall of the colon was found and subsequently repaired. The patient recovered with daily cleaning of the wound and antimicrobial therapy. Given his chronic constipation, this perforation was considered a stercoral perforation (perforation of the bowel due to pressure necrosis from fecal masses),2 and a laxative agent was given on discharge.
|
|
|
Figure 1. An aberration of feces under the skin from the proximal end of the colostomy site (arrows) and fecal impaction. |
Perforation of the colon in end colostomy is rare and reportedly develops most often in patients with trauma or in those in the early postoperative phase of colostomy. It is rare in patients whose stoma was made a long time ago; only two cases have been reported, both of which were considered a stercoral perforation.3 Only 137 cases of stercoral perforation have been reported.4 The most common sites are the sigmoid colon (50%) followed by the rectosigmoid junction (24%).4 Stercoral perforation is potentially life-threatening, with an overall mortality rate of 34%.4 Maurer et al5 presented the criteria of stercoral perforation, which includes the following: (1) round or ovoid perforation, >1 cm in diameter; (2) fecalomas present within the colon, protruding through the perforation site or lying within the abdominal cavity; and (3) pressure necrosis or ulcer and chronic inflammatory reaction around the perforation site are present microscopically. In our case, at least three of these criteria were met, and thus stercoral perforation was highly suspected. Risk factors for stercoral perforation include chronic constipation, old age, evidence of fecal impaction, and increasing abdominal pain unexplained by constipation alone.4 Computed tomography might be recommended in patients with a colostomy presenting with these risk factors.4
Colostomy is sometimes created with the sigmoid colon, which is susceptible to stercoral perforation, and patients who undergo this procedure take on the risk of constipation. Although rare, our case illustrates the importance of considering stercoral perforation of the colon in colostomy patients with chronic constipation, as a potential reason of spontaneous perforation of the colon.
Acknowledgments
The authors would like to thank Ms Ryoko Yoshida for editing the pictures. Written consent to publish the article and figures was obtained from the patient.
References
- 1 K.L. Ng, W.K. Cheong; Surgical pitfalls in patients with Ehlers–Danlos type IV: a case of spontaneous sigmoid perforation in a 17-year-old male; As J Surg, 34 (2011), pp. 143–145
- 2 J.W. Serpell, R.J. Nicholls; Stercoral perforation of the colon; Br J Surg, 77 (1990), pp. 1325–1329
- 3 Y.W. Kim, H.J. Kwon, I.Y. Kim; Stercoral perforation of the colon in sigmoid colostomy patients: two case reports; Int J Surg Case Rep, 4 (2013), pp. 1038–1040
- 4 S. Chakravartty, A. Chang, J. Nunoo-Mensah; A systematic review of stercoral perforation; Colorectal Dis, 15 (2013), pp. 930–935
- 5 C.A. Maurer, P. Renzulli, L. Mazzucchelli, B. Egger, C.A. Seiler, M.W. Buchler; Use of accurate diagnostic criteria may increase incidence of stercoral perforation of the colon; Dis Colon Rectum, 43 (2000), pp. 991–998
Further reading
Reply to Editor re: Perforation of the colon in end colostomy
Summary
We would like to heartily congratulate the authors Akira Kuriyama and Tetsunori Ikegami for the successful publication of their case report on Perforation of the colon in end colostomy. 1 We read with interest about their experience regarding that of a stercoral perforation occurring proximal to a colostomy in an elderly patient secondary to pressure necrosis from fecal masses. This has enhanced our overall understanding of this rare cause of spontaneous colonic perforation, and we humbly thank them for their citation of our article Surgical pitfalls in patients with Ehlers–Danlos type IV: a case of spontaneous sigmoid perforation in a 17-year-old male.
Furthering the rare causes of spontaneous colonic perforation, this is indeed a good opportunity to remind ourselves of the need to consider various differential diagnoses in patients who present as such in our clinical encounters. J.A. Berry in 1984 first classified spontaneous colonic perforations into stercoral versus idiopathic perforations based on etiological and pathophysiological bases, with the former classification being attributed to impacted feces resulting in ischemia (as excellently expounded upon in Kuriyama and Ikegamis article), and the latter being known to be linear types with corresponding normal histology.
Other than the highlighted issues of chronic constipation occurring particularly in the elderly and underlying connective tissue disorders (e.g. Ehlers–Danlos type IV, Marfan syndrome, etc.) being causative factors, another less common cause to consider may include hypothyroidism resulting in intestinal hypomotility.2
We would like to round off with a word of caution: common things do happen commonly, and it remains imperative that surgeons take into consideration frequently occurring phenomenon in patients who present with acute peritonitis; as Maurer et al3 rightly pointed out, organic causes such as external injury, obstruction, tumors (both gastrointestinal in origin and otherwise, e.g. lymphoma), and diverticulosis must first be excluded. Within our Asian context, tuberculosis is an often-missed diagnosis. Either way, spontaneous colonic perforation remains a rare and interesting subset of all colonic perforations, for which we eagerly await publication of further literature to lend a greater understanding to this uncommon but significantly morbid clinical entity.
Conflicts of interest
The authors declare no conflicts of interest.
References
- 1 T. Ikegami, A. Kuriyama; Perforation of the colon in end colostomy; Asian J Surg, 39 (2016), pp. 262–263
- 2 S.K. Zachariah, N. Raja; Spontaneous perforation of the colon and hypothyroidism: report of a case and review of literature; Gastroenterol Res, 3 (2010), pp. 147–149
- 3 C.A. Maurer, P. Renzulli, L. Mazzucchelli, B. Egger, C.A. Seiler, M.W. Büchler; Use of accurate diagnostic criteria may increase incidence of stercoral perforation of the colon; Dis Colon Rectum, 43 (2000), pp. 991–998
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?