Summary
Adequate colonic cleansing is essential for a high quality colonoscopy. Few studies have investigated the association between patient education and quality of bowel preparation. The control group comprised 165 participants who underwent colonoscopy after a standard bowel preparation protocol during the period September–October 2013 and the study group comprised 251 individuals who underwent colonoscopy after a modified bowel preparation protocol during the period January–February 2014. The modified bowel preparation protocol included an instructional video and leaflet, a dietician-designed 2-day low fiber diet, a follow-up phone message, and information to confirm stool characteristics. The Aronchick Bowel Preparation Scale was used to define the quality of bowel preparation. The endoscopists who performed the procedures were blinded to the preparation protocols. The percentage of participants with excellent bowel preparation quality was significantly higher in the study group than in the control group (35.9% vs. 21.8%, p = 0.002). Also, the percentage of participants with poorly prepared bowels was significantly higher in the control group than in the study group (3% vs. 0.8%, p = 0.042). Moreover, the adenoma detection rate was significantly higher in the study group (35.1% vs. 24.8%, p = 0.028). The results show that the quality of bowel cleansing can be improved by providing patients with a modified bowel preparation protocol.
Keywords
Bowel preparation ; Colonoscopy ; Patient education ; Visual aids
Introduction
Colonoscopy is the preferred modality for colorectal cancer screening and adequate colonic cleansing is essential for high quality colonoscopy [1] . However, approximately 20% of patients present with an inadequately prepared colon during the procedure [2] . Poor bowel preparation has been shown to result in a longer procedure time, a lower adenoma detection rate (ADR), an increased incidence of interval cancer, increased cost, a higher rate of colonoscopy-related complications, and the need for repeated examination [2] ; [3] ; [4] .
Adequate colon preparation can be affected by different bowel-cleansing agents [5] as well as the time between starting bowel preparation and the colonoscopy [6] . Patient factors also influence the adequacy of bowel preparation, such as inpatient status, constipation, use of antidepressants, and compliance with cleansing instructions [3] . Few studies have investigated whether patient education on bowel preparation improves compliance with bowel cleansing protocols. Smith et al [7] found that many patients were unable to comprehend written colonoscopy leaflets. Ibanez et al [8] showed that a low fiber diet for 72 hours improved colon preparation; however, their findings were based on an observational study in patients who received more than one colonoscopic examination. In this study we investigated whether a modified bowel preparation protocol as well as a dietician-designed 2-day low fiber diet improves the quality of bowel preparation for colonoscopy.
Methods
Study group
This study was conducted at the health management center of the Far Eastern Memorial Hospital, New Taipei City, Taiwan. The control group comprised 165 individuals who underwent colonoscopy after a standard bowel preparation protocol during the period September–October 2013. The study group comprised 251 consecutive participants who underwent colonoscopy after a modified bowel preparation protocol during the period January–February 2014. Participants in both groups received information from well-trained nurses on proper bowel cleansing procedures. All participants were Taiwanese and were able to comprehend Mandarin Chinese. The dosage of sodium phosphate (NaP) was two bottles of 45-mL drug in 1-L water both the night before and the morning of the procedure, and the dosage of polyethylene glycol (PEG) was 137.155 g (1 bag of drug) in 2-L water the morning of the procedure. All the procedures were performed in the morning (from 8:30 am to 12:00 pm ). In addition, all of the enrolled participants underwent colonoscopy under general anesthesia. Seven endoscopists who participated in this study were randomly assigned and blinded to the bowel preparation protocols. The colonoscopic system and scope used were the same in both groups (Olympus Evis Lucera Spectrum video system CV-260, Olympus, Tokyo, Japan; colonoscope: Olympus CF-H260AI, Olympus).
Modified bowel preparation
Patients in the control group received a standard bowel preparation protocol, which included a leaflet without illustrations and a diet that did not comprise a dietician-designed 2-day low fiber diet. Patients in the study group received a modified bowel preparation protocol which included: (1) receipt of an instructional video and an illustrated leaflet (Figure 1 ); (2) a dietician-designed 2-day low fiber diet (<4 g/d; Table S1 ); (3) receipt of a cell phone message to remind the patients of their dietary bowel cleansing protocol; and (4) information on how to confirm that stool characteristics were appropriate for colonoscopy, and information that a glycerin ball enema should be used if the characteristics of stool samples did not meet those required before the procedure.
|
|
|
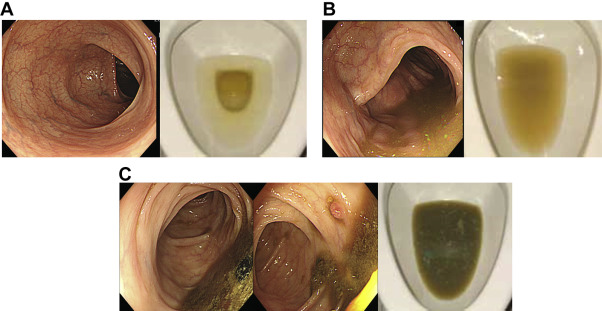
Figure 1. Bowel preparation: (A) shows excellent or good bowel preparation (left panel) and clear liquid stool (right panel). Excellent or good bowel preparation is essential for correct diagnosis and further endoscopic management; (B) turbid fluid in colon is indicative of a fair colon preparation (left panel), and stool was turbid (right panel). The appearance of colonic mucosa is difficult to evaluate, and some lesions may be obscured; and (C) shows poor colon preparation (left panel). A polyp was detected after repeated water flush (middle panel). Some formed or soft stools are noted (right panel). |
Measure of the adequacy of bowel preparation
We used the Aronchick Bowel Preparation Scale to define the quality of bowel preparation as previously reported: a small volume of clear liquid or > 95% of surface seen was defined as “excellent”; clear liquid covering 5–25% of the surface and some semisolid stool suctioned or washed away but > 90% of surface seen were defined as “good” and “fair”; semisolid stool that could not be suctioned or washed away and < 90% of the surface seen was defined as “poor” [9] . The right-sided colon was defined as comprising the ascending and transverse colons and the left-sided colon was defined as comprising the descending and sigmoid colons and the rectum.
Statistical analysis
All data are presented as mean ± standard deviation for continuous variables. Differences in means of continuous measurements were analyzed with the unpaired t test for normally distributed variables and the Wilcoxon test for non-normally distributed variables. The Chi-square test was used for comparison of categorical variables, including bowel preparation quality, ADR, and right- versus left-sided colonic polyps.
Results
The two groups were similar with respect to age (mean ± standard deviation, 49.04 ± 10.84 years vs. 49.31 ± 12.65 years, p = 0.819), sex ratio (male:female, 103:62 participants vs. 137:114 participants, p = 0.113), and regimens used for bowel cleansing (NaP:PEG, 60:105 participants vs. 86:165 participants, p = 0.661; Table 1 ). All the participants had good compliance to the bowel preparation protocols. No complications such as bowel perforation, intestinal bleeding, dehydration, or neurologic changes were noticed in the participants. The percentage of individuals with excellent bowel preparation quality was significantly higher in the study group than in the control group (35.9% vs. 21.8%, p = 0.002). Also, the percentage of individuals with poorly prepared bowels was significantly higher in the control group than in the study group (3% vs. 0.8%, p = 0.042). In total, 61 colonic adenomas were detected in 41 participants in the control group and 120 colonic adenomas were detected in 88 participants in the study group. The ADR in participants with at least one detected adenoma was higher in individuals who underwent the modified bowel preparation protocol (35.1% vs. 24.8%, p = 0.028). In addition, the whole procedure time was shorter in the study group than in the control group (15.5 ± 4.4 minutes vs. 14.6 ± 4.1 minutes, p = 0.032). However, the modified bowel preparation protocol did not significantly affect the cecal intubation time and cecal intubation rate (3.8 ± 2.2 minutes vs. 4.1 ± 2.8 minutes, p = 0.242; 98.8% vs. 100%, p = 0.08). There were no differences in the location of adenomatous polyps between the two groups.
| Control group (n = 165) | Study group (n = 251) | p | |
|---|---|---|---|
| Demographic characteristics | |||
| Age (y) | 49.04 ± 10.84 | 49.31 ± 12.65 | 0.819 |
| Sex (male:female) | 103:62 | 137:114 | 0.113 |
| Bowel preparation regimen (NaP:PEG) | 60:105 | 86:165 | 0.661 |
| Cecal intubation time (min) | 3.8 ± 2.2 | 4.1 ± 2.8 | 0.242 |
| Whole procedure time (min) | 15.0 ± 4.4 | 14.6 ± 4.1 | 0.032 |
| Cecal intubation rate | 98.8 | 100 | 0.080 |
| Bowel preparation quality | |||
| Excellent | 36 (21.8) | 90 (35.9) | 0.002 |
| Good | 94 (57.0) | 120 (47.8) | 0.067 |
| Fair | 30 (18.2) | 40 (15.9) | 0.549 |
| Poor | 5 (3.0) | 2 (0.8) | 0.042 |
| ADR | 41 (24.8) | 88 (35.1) | 0.028 |
| Right:left-sided colonic polyps | 45:16 | 84:36 | 0.596 |
Data are presented as n , n (%) or mean ± standard deviation, unless otherwise indicated.
ADR = adenoma detection rate; NaP = sodium phosphate; PEG = polyethylene glycol; QC = quality control.
Discussion
Few studies have investigated the effect of educational interventions as a tool to improve the quality of bowel preparation. Studies have shown that visual aids and educational pamphlets or photographs are more informative and result in better patient compliance than simple visual aids and conventional education programs [10] ; [11] ; [12] . Beside better colon preparation, educational pamphlets could reduce the patients’ anxiety levels and lower the dosage of sedatives [10] . However, Modi et al [13] showed that educational intervention had no impact on the overall quality of bowel preparation. But the intervention was an additional explanation of the preparation process without vivid pictures. In this study, we found that an intensive education program combined with a low fiber diet improved the quality of bowel preparation and resulted in a shorter whole procedure time and a higher ADR. In addition, better bowel preparations resulting from intensive participant education had no inference on cecal intubation time. The result suggested that endoscopists wasted less time on washing uncleaned colon under better bowel preparation.
The results were similar in the subgroup analysis, which evaluated whether differences in bowel preparation regimen (NaP or PEG) had an effect on the quality of bowel preparation (data not shown). However, there were a few limitations in our study. Firstly, this was a single-center study with a small sample size. Secondly, it was not a randomized study and a historical control was used for analysis. Thirdly, we did not have detailed characteristics of the participants, such as body mass index and smoking habits, or other risk factors for colorectal cancer.
In summary, a modified bowel preparation protocol comprising easy-to-understand pictures and videos as well as a dietician-designed 2-day low fiber diet improves the adequacy of bowel cleansing for colonoscopy.
Conflicts of interest
All authors declare no conflicts of interest.
Appendix A. Supplementary data
The following is the supplementary data related to this article:
References
- [1] D.J. Robertson, M.F. Kaminski, M. Bretthauer; Effectiveness, training and quality assurance of colonoscopy screening for colorectal cancer; Gut, 64 (2015), pp. 982–990
- [2] D.K. Rex, T.F. Imperiale, D.R. Latinovich, L.L. Bratcher; Impact of bowel preparation on efficiency and cost of colonoscopy; Am J Gastroenterol, 97 (2002), pp. 1696–1700
- [3] F. Froehlich, V. Wietlisbach, J.J. Gonvers, B. Burnand, J.P. Vader; Impact of colonic cleansing on quality and diagnostic yield of colonoscopy: the European Panel of Appropriateness of Gastrointestinal Endoscopy European multicenter study; Gastrointest Endosc, 61 (2005), pp. 378–384
- [4] C.H. Oh, C.K. Lee, J.W. Kim, J.J. Shim, J.Y. Jang; Suboptimal bowel preparation significantly impairs colonoscopic detection of non-polypoid colorectal neoplasms; Dig Dis Sci, 60 (2015), pp. 2294–2303
- [5] P.O. Katz, D.K. Rex, M. Epstein, N.K. Grandhi, S. Vanner, L.C. Hookey, et al.; A dual-action, low-volume bowel cleanser administered the day before colonoscopy: results from the SEE CLEAR II study; Am J Gastroenterol, 108 (2013), pp. 401–409
- [6] T. Reilly, G. Walker; Reasons for poor colonic preparation with inpatients; Gastroenterol Nurs, 27 (2004), pp. 115–117
- [7] S.G. Smith, C. von Wagner, L.M. McGregor, L.M. Curtis, E.A. Wilson, M. Serper, et al.; The influence of health literacy on comprehension of a colonoscopy preparation information leaflet; Dis Colon Rectum, 55 (2012), pp. 1074–1080
- [8] M. Ibanez, A. Parra-Blanco, P. Zaballa, A. Jimenez, R. Fernandez-Velazquez, J.O. Fernandez-Sordo, et al.; Usefulness of an intensive bowel cleansing strategy for repeat colonoscopy after preparation failure; Dis Colon Rectum, 54 (2011), pp. 1578–1584
- [9] C.A. Aronchick, W.H. Lipshutz, S.H. Wright, F. Dufrayne, G. Bergman; A novel tableted purgative for colonoscopic preparation: efficacy and safety comparisons with Colyte and Fleet Phospho-soda; Gastrointest Endosc, 52 (2000), pp. 346–352
- [10] A.A. Shaikh, S.M. Hussain, S. Rahn, D.J. Desilets; Effect of an educational pamphlet on colon cancer screening: a randomized, prospective trial; Eur J Gastroenterol Hepatol, 22 (2010), pp. 444–449
- [11] A.H. Calderwood, E.J. Lai, O.K. Fix, B.C. Jacobson; An endoscopist-blinded, randomized, controlled trial of a simple visual aid to improve bowel preparation for screening colonoscopy; Gastrointest Endosc, 73 (2011), pp. 307–314
- [12] J.W. Tae, J.C. Lee, S.J. Hong, J.P. Han, Y.H. Lee, J.H. Chung, et al.; Impact of patient education with cartoon visual aids on the quality of bowel preparation for colonoscopy; Gastrointest Endosc, 76 (2012), pp. 804–811
- [13] C. Modi, J.R. Depasquale, W.S. Digiacomo, J.E. Malinowski, K. Engelhardt, S.N. Shaikh, et al.; Impact of patient education on quality of bowel preparation in outpatient colonoscopies; Qual Prim Care, 17 (2009), pp. 397–404
Document information
Published on 15/05/17
Submitted on 15/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?