Abstract
Objectives
The aims of this study was first to investigate whether the bite size or the bite distance from the tear edge is of primary importance in mattress suture configuration for rotator cuff repair. Secondly, whether the use of a 450 left side bent Arthro-Pierce™ (Smith & Nephew, Andover, USA) during suture passage can be more effective on the strength of the configuration compared to a straight Arthro-Pierce™.
Materials and methods
Twenty-eight bovine infraspinatus muscle tendons were randomized into four groups. Group 1; 5 mm wide ‘bite size’ × 15 mm length ‘distance from the tear edges mattress’; Group 2: 7.5 mm × 10 mm; Group 3: 15 mm × 5 mm ‘using straight Arthro-Pierce™’ and Group 4: 5 mm × 15 mm using left sided 450 bent Arthro-Pierce™. The repair specimens underwent cyclic loading prior to loading the failure testing. Cyclic elongation (mm), peak-to-peak displacement (mm), ultimate load (N), stiffness (N/mm) and failure mode were recorded for each specimen.
Results
The mean ultimate load in Group 1 was higher compared to group 3. The peak to peak displacement was higher in Group 4 compared to Group 1 (p < 0.05). The predominant failure mode in Groups 1, 2 and 4 was suture rupture. The Group 3 most specimens failed due to suture cut through the tendon.
Conclusion
Bite size from the edge of the tendon seems to be more important than the width of the mattress. The curve of the suture passing device may also have an effect on the strength of the suture tendon interface.
Keywords
Rotator cuff tear ; Mattress repair
Introduction
Despite the advances in the arthroscopic repair techniques of rotator cuff tendon tears, the re-tear rates still remain high at 14–25%.1 Suture-tendon interface is still identified as the weakest link of the repair despite the introduction of newly designed anchors and high strength sutures.2 Although various suture configurations have been tested in previous biomechanical studies,3 ; 4 ; 5 the most widely used stitch configurations are simple, mattress or a combination of the two, the massive cuff stitch,6 ; 7 ; 8 since the mattress suture is stronger than a simple suture.6 ; 9 Recent studies have reported that the medial or lateral distance of the stitch from the tear edge2 ; 10 ; 11 and bite size of the horizontal mattress configuration (distance between the limbs passed through the tendon)12 has an effect on the strength of the mattress configuration repair. No study has reported the effect of both parameters though.
Recently, it was also proven that arthroscopic devices, used for suture passage, make bigger holes in the cuff, that result in a weaker suture-tendon interface.10 ; 13
The purpose of this study was to investigate whether the bite size or bite distance from the tear edge is of primary importance in rotator cuff repair and whether using a 45° left-bent ARTHRO-PIERCE™ (Smith & Nephew Inc., Andover, MA, USA) or a straight ARTHRO-PIERCE™ instrument during suture passage would have a greater effect on the strength of the configuration. The hypothesis was that increasing the bite size of the mattress configuration would compensate for the shorter bite distance from the tear edge (that the area of the rectangle covered by the mattress suture ‘bite size times the distance from the tear edge’ is kept constant) and using the 45° bent ARTHRO-PIERCE™ instrument would cause the strength of the configuration to weaken.
Materials and methods
Twenty-eight bovine shoulder specimens were obtained from an abattoir for this study. All specimens were harvested from male calves (age: 16 months) and frozen immediately at −20 °C. Before testing, the specimens were thawed, and the infraspinatus muscle with the tendon attached was dissected from its insertion site at the humerus and removed.
For all specimens, tendon thickness was measured using a digital caliper. The three suture configurations were randomly placed in each set of tendon specimens. Seven tendon specimens were tested for each suture configuration.
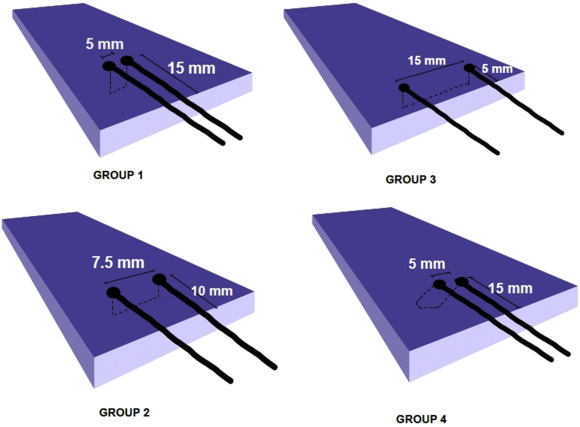
All procedures were performed by a single investigator. There were four test groups. Groups 1,2 and 3 used a straight ARTHRO-PIERCE™ instrument with three different suture configurations (Group 1: 5 mm wide ‘bite size’ × 15 mm length ‘distance from the tear edge’; Group 2: 7.5 mm × 10 mm; Group 3: 15 mm × 5 mm). Group 4 used a left-sided, 45° bent ARTHRO-PIERCE™ instrument with 5 mm × 15 mm suture configuration (Fig. 1 ). Each stitch was created using a no.2 FiberWire® (Arthrex, Inc., Naples, FL, USA) suture.
|
|
|
Fig. 1. Groups tested. |
Biomechanical testing
The tendon repair construct was mounted securely in the jaws of a materials testing system (AG-I 10 kN; Shimadzu Corp., Kyoto, Japan) with free ends of the suture, looped and tied around a bar, leaving 10 cm of the suture from the tendon edge to the bar and 10 cm of tendon protruding from the jaw in every specimen (Fig. 2 ). A 5 N preload was applied to pretension each specimen. The construct was then cyclically loaded under force control from 5 to 30 N at 0.25 Hz for twenty cycles. Force of 30 N was chosen based on previous studies.4 ; 6 ; 14 ; 15
|
|
|
Fig. 2. Test set-up. |
Following cyclic loading, each tendon specimen was loaded to failure at a rate of 1 mm/s.6 Elongation and peak-to-peak displacement were determined during cyclic testing. Elongation is the difference in y displacement between the first cycles peak and the twentieth cycles peak. The average of the peak-to-peak displacement values of the eighteenth, nineteenth and twentieth cycles were defined as peak-to-peak displacement. Load (in Newtons) versus displacement (in millimeters) was recorded until failure. The ultimate tensile load was considered to be the peak force. Stiffness was calculated by determining the slope of the load–displacement curve using a best-fit line on the load versus displacement curve. Cyclic elongation (mm), peak-to-peak displacement (mm), ultimate load (N), stiffness (N/mm) and failure mode were recorded for each specimen.
Statistical analysis
The null hypothesis was that increasing the bite size of the mattress configuration would not compensate for the shorter bite distance from the tear edge and that the use of 45° bent ARTHRO-PIERCE™ instrument would not cause the strength of the configuration to weaken. Kruskal–Wallis' one-way analysis of variance was used to analyze the groups and evaluate overall differences. When an overall group difference was observed, a Mann–Whitney U test was used to identify the specific location of the statistically significant difference with the significance level set at p < 0.05.
Results
The specimen data are summarized in Table 1 . The mean tendon thickness was higher in Group 3 in comparison to Group 1. The mean ultimate load in Group 1 was higher in comparison to Group 3 and the peak-to-peak displacement was significantly higher in Group 4 than Group 1 (p < 0.05). Further comparisons between groups including cyclic elongation, peak-to-peak displacement, ultimate load, and tendon thickness were not different.
| Group 1 (5 × 15 mm) (Mean ± SD) | Group 2 (7.5 × 10 mm) (Mean ± SD) | Group 3 (15 × 5 mm) (Mean ± SD) | Group 4 (5 × 15 mm) (Mean ± SD) | |
|---|---|---|---|---|
| Tendon thickness (mm) | 3 ± 0.5 | 3 ± 0.6 | 3.6 ± 0.4 | 3.4 ± 0.5 |
| Cyclic elongation (mm) | 0.9 ± 0.3 | 0.9 ± 0.3 | 0.8 ± 0.2 | 1.1 ± 0.2 |
| Peak-to-peak displacement (mm) | 3.4 ± 1.2 | 3.5 ± 1.2 | 3.4 ± 0.6 | 5 ± 0.9 |
| Ultimate load (N) | 301 ± 16 | 225 ± 91 | 209 ± 62 | 305 ± 100 |
| Stiffness (N/mm) | 11 ± 5 | 12 ± 2 | 11 ± 3 | 9 ± 5 |
N: Newton, SD: standard deviation.
The predominant failure mode in Group 1, 2 and 4 was suture rupture (Group 1 had six suture ruptures and one suture cut through the tendon; Group 2 had four suture ruptures and three suture cut-throughs; Group 4 had seven suture ruptures). In Group 3, most of the specimens failed due to suture cuts through the tendon; two specimens failed due to suture rupture.
Discussion
The main finding of the present study was that an increase in the bite size of the mattress configuration did not compensate for a more lateral localization of the suture. In addition, a left-bent suture passing device resulted in higher peak-to-peak displacement than a straight device.
Recent biomechanical studies have reported that medial placement of sutures at the tendon can increase the suture retention properties of the construct.2 ; 10 ; 11 Wang et al11 reported that sutures placed at the myotendinous junction were stronger than sutures placed laterally close to the free tendon edge in torn specimens. The authors claimed that this was due to the smaller fibril diameter and fibril fraction area at the lateral edge of the tendon. In another study, Wieser et al reported that suture positioning lateral to the rotator cable led to significantly lower suture retention properties compared to positioning the suture medial to the cable.2 Similarly, Ponce et al reported that a 10 mm bite from the tear edge resulted in a higher failure load compared to a 5 mm bite.10 It is possible that the longer distance the suture has to slide through the tendon, compared to lateral positioning, contributed to the mechanical advantage of the medial positioning of the stitch. Although the results presented in this study reveal that the medially bit cuff has a higher tendency to re-tear, recent literature suggests paying more attention to Type 2 failures and musculotendinous junction failures with the suture bridge and double-row repair techniques, driving the debate on the strength or failure risk.12 ; 13 ; 14 ; 16
In one clinical scenario, it is not always possible to pass the sutures medially due to different tear configurations and/or tear degeneration. Recently, Tamboli et al demonstrated that increasing the bite size of the mattress suture increased the ultimate strength of the configuration and prevented the suture-tendon interface failure.17 Based on these, the hypothesis of the study was that lateral placement of the sutures can be compensated by an increase in the suture bite of the mattress configuration. In other words, if the area of the tendon covered by the suture is kept constant (bite size of mattress × distance from the edge of the tendon), the strength of the configuration will not change significantly.
This hypothesis was not totally confirmed in the present study. The ultimate load of Group 3 was lower than Group 1 with most failure at the suture-tendon interface instead of suture rupture. There was no difference between Group 1 and 2. In contrast to recent studies, reporting less gap formation and strain with a 4-mm wide mattress compared to a 10-mm wide mattress, we found no difference between the groups in terms of cyclic loading parameters.17 However, the distance from the tendon edge was kept constant and anchor fixation with knot-tying over the tendon was incorporated in this study, precluding the opportunity to purely test the holding capacity of the tendon.17
Ponce et al10 recently outlined the variables within the control of the surgeon, in order of increasing importance; 1) type of instrument used 2) size of the tissue bite taken, and 3) type of stitch placed with a higher failure load associated with a 10-mm bite compared to a 5-mm bite. As the size of the suture passing device increased, the failure load decreased with no effect on cyclic elongation or displacement. In another study,18 it was reported that a SutureLasso™ (Arthrex Inc., Naples, FL, USA) and a tapered needle failed at higher loads after cyclic loading, compared to a straight BirdBeak® (Arthrex Inc., Naples, FL, USA) or Viper™ (Arthrex Inc., Naples, FL, USA) instrument.3 Contrary to both studies, the present study sought to determine whether the curvature of the same device (straight or 45° bent) had any effect on the strength, which could only be demonstrated at peak-to-peak displacement.10 ; 18
One limitation of this study was the use of the bovine model. Animal models allow a more predictable and uniform tendon quality, unlike human cadaver specimens which have a great deal of variability. Bovine infraspinatus have also been validated in previous biomechanical studies.19 ; 20 ; 21 Moreover, this study did not evaluate the behavior of a long-term rotator cuff repair and only addressed the initial security of the suture-tendon interface, thus removing potentially confounding variables related to the tendon-bone and bone-anchor interfaces.
In conclusion, the bite size from the edge of the tendon seems to be more important than the width of the mattress in rotator cuff repair. The curve of the suture passing device may also have an effect on the strength of the suture-tendon interface.
Conflict of interest
None.
References
- 1 P.J. Millett, R.J. Warth, G.J. Dornan, J.T. Lee, U.J. Spiegl; Clinical and structural outcomes after arthroscopic single-row versus double-row rotator cuff repair: a systematic review and meta-analysis of level I randomized clinical trials; J Shoulder Elb Surg, 23 (4) (2014), pp. 586–597 http://dx.doi.org/10.1016/j.jse.2013.10.006
- 2 K. Wieser, S. Rahm, M. Farshad, E.T. Ek, C. Gerber, D.C. Meyer; Stitch positioning influences the suture hold in supraspinatus tendon repair; Knee Surg Sports Traumatol Arthrosc, 21 (7) (2013), pp. 1587–1592 http://dx.doi.org/10.1007/s00167-012-2103-6
- 3 S. Frosch, G. Buchhorn, A. Hoffmann, et al.; Novel single-loop and double-loop knot stitch in comparison with the modified Mason-Allen stitch for rotator cuff repair; Knee Surg Sports Traumatol Arthrosc (2014) http://dx.doi.org/10.1007/s00167-014-2976-7 5
- 4 O. Hapa, F.A. Barber, E. Sünbüloğlu, Y. Kocabey, N. Sarkalkan, G. Baysal; Tendon-grasping strength of various suture configurations for rotator cuff repair; Knee Surg Sports Traumatol Arthrosc, 19 (10) (2011), pp. 1749–1754 http://dx.doi.org/10.1007/s00167-010-1322-y
- 5 B.A. Ponce, C.D. Hosemann, P. Raghava, J.P. Tate, A.W. Eberhardt, L. Lafosse; Biomechanical evaluation of 3 arthroscopic self-cinching stitches for shoulder arthroscopy: the lasso-loop, lasso-mattress, and double-cinch stitches; Am J Sports Med, 39 (1) (2011), pp. 188–194 http://dx.doi.org/10.1177/0363546510383394
- 6 C.B. Ma, J.D. Macgillivray, J. Clabeaux, S. Lee, J.C. Otis; Biomechanical evaluation of arthroscopic rotator cuff stitches; J Bone Jt Surg Am, 86 (6) (2004), pp. 1211–1216
- 7 J.D. MacGillivray, C.B. Ma; An arthroscopic stitch for massive rotator cuff tears: the Mac stitch; Arthroscopy, 20 (6) (2004), pp. 669–671
- 8 M.J. Sileo, C.R. Ruotolo, C.O. Nelson, F. Serra-Hsu, A.P. Panchal; A biomechanical comparison of the modified Mason-Allen stitch and massive cuff stitch in vitro; Arthroscopy, 23 (3) (2007), pp. 235–240
- 9 C. Gerber, A.G. Schneeberger, M. Beck, U. Schlegel; Mechanical strength of repairs of the rotator cuff; J Bone Jt Surg Br, 76 (1994), pp. 371–380
- 10 B.A. Ponce, C.D. Hosemann, P. Raghava, J.P. Tate, E.D. Sheppard, A.W. Eberhardt; A biomechanical analysis of controllable intraoperative variables affecting the strength of rotator cuff repairs at the suture-tendon interface; Am J Sports Med, 41 (10) (2013), pp. 2256–2261 http://dx.doi.org/10.1177/0363546513499228
- 11 V.M. Wang, F.C. Wang, A.G. McNickle, et al.; Medial versus lateral supraspinatus tendon properties: implications for double-row rotator cuff repair; Am J Sports Med, 38 (12) (2010), pp. 2456–2463 http://dx.doi.org/10.1177/0363546510376817
- 12 K. Hayashida, M. Tanaka, K. Koizumi, M. Kakiuchi; Characteristic retear patterns assessed by magnetic resonance imaging after arthroscopic double-row rotator cuff repair; Arthroscopy, 28 (4) (2012 Apr), pp. 458–464
- 13 S.S. Burkhart, P.J. Denard, J. Konicek, B.T. Hanypsiak; Biomechanical validation of load-sharing rip-stop fixation for the repair of tissue-deficient rotator cuff tears; Am J Sports Med, 42 (2) (2014), pp. 457–462
- 14 G.E. Awwad, K. Eng, G.I. Bain, D. McGuire, C.F. Jones; Medial grasping sutures significantly improve load to failure of the rotator cuff suture bridge repair; J Shoulder Elb Surg, 23 (5) (2014), pp. 720–728
- 15 M.V. Wlk, A. Abdelkafy, M. Hexel, et al.; Biomechanical evaluation of suture-tendon interface and tissue holding of three suture configurations in torn and degenerated versus intact human rotator cuffs; Knee Surg Sports Traumatol Arthrosc (2014) http://dx.doi.org/10.1007/s00167-014-2988-3
- 16 R.S. Kullar, J.M. Reagan, C.W. Kolz, R.T. Burks, H.B. Henninger; Suture placement near the musculotendinous junction in the supraspinatus: implications for rotator cuff repair; Am J Sports Med, 43 (1) (2015), pp. 57–62
- 17 M. Tamboli, T. Mihata, J. Hwang, M.H. McGarry, Y. Kang, T.Q. Lee; Biomechanical characteristics of the horizontal mattress stitch: implication for double-row and suture-bridge rotator cuff repair; J Orthop Sci, 19 (2) (2014), pp. 235–241 http://dx.doi.org/10.1007/s00776-013-0504-0
- 18 B.V. Chokshi, E.N. Kubiak, L.M. Jazrawi, et al.; The effect of arthroscopic suture passing instruments on rotator cuff damage and repair strength; Bull Hosp Jt Dis, 63 (3-4) (2006), pp. 123–125
- 19 W. Anderl, P.R. Heuberer, B. Laky, B. Kriegleder, R. Reihsner, J. Eberhardsteiner; Superiority of bridging techniques with medial fixation on initial strength; Knee Surg Sports Traumatol Arthrosc, 20 (12) (2012), pp. 2559–2566 http://dx.doi.org/10.1007/s00167-012-1922-9
- 20 L.J. Bisson, L.M. Manohar, R.D. Wilkins, J. Gurske-Deperio, M.T. Ehrensberger; Influence of suture material on the biomechanical behavior of suture-tendon specimens: a controlled study in bovine rotator cuff; Am J Sports Med, 36 (5) (2008), pp. 907–912 http://dx.doi.org/10.1177/0363546508314793
- 21 A.K. Koganti, G.J. Adamson, C.S. Gregersen, M.M. Pink, J.A. Shankwiler; Biomechanical comparison of traditional and locked suture configurations for arthroscopic repairs of the rotator cuff; Am J Sports Med, 34 (11) (2006), pp. 1832–1838 http://dx.doi.org/10.1177/0363546506289701
Document information
Published on 31/03/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?