Summary
We report a case of delayed presentation of a small bowel perforation following blunt abdominal trauma (BAT). An initial computed tomography (CT) scan revealed that the patient (a 32-year-old man) had a mesenteric hematoma, which was managed conservatively. Four weeks later, he returned to the hospital complaining of abdominal pain. A CT scan of the abdomen showed a thickened loop of the small bowel adjacent to the mesenteric hematoma at the level of the ileum. He was discharged home, but re-presented with acute abdomen 6 weeks post-trauma. An exploratory laparotomy was performed, which showed a perforated thickened loop of the ileum forming a phlegmon in the lower abdomen. In the English medical literature, only eight other reports of delayed post-traumatic presentation of ileal/jejunal perforation following BAT have been reported. We propose that post-traumatic intestinal perforation be considered in the differential diagnosis even in patients who experience a delayed small bowel perforation following BAT.
Keywords
blunt abdominal trauma;bowel perforation;delayed presentation;mesenteric hematoma;small bowel
1. Introduction
A small bowel perforation due to blunt abdominal trauma (BAT) is relatively uncommon,1; 2 ; 3 and the exact mechanism remains controversial. Delayed presentation of small bowel perforation following BAT is extremely rare. The delayed onset of symptoms following the trauma often makes the diagnosis difficult. In the English-language medical literature, eight other reports (10 cases) of delayed post-traumatic presentation of ileum perforation (3 cases) or jejunum perforation (7 cases) following BAT have been reported.4; 5; 6; 7; 8; 9; 10 ; 11 The underlying pathophysiologic mechanism has not been described well. Characteristics of the patients from the previous reports who had a delayed presentation of small bowel perforation following BAT are summarized in Table 1.
| Age (y) | Sex | Reference | Mechanism of injury | Presentation delay (d) | Perforation site | Mesenteric injurya | Postoperative findings |
|---|---|---|---|---|---|---|---|
| 28 | M | How et al4 | MVC | 56 | Ileum | NM | Mucosal necrosis, transmural edema in keeping with ischemic changes in the involved segment |
| 37 | M | Subramanian et al5 | MVC | 77 | Jejunum | MH (+) | Mucosal necrosis, transmural congestion, hemorrhage, and serositis in the involved segment |
| 32 | M | Subramanian et al5 | MVC | 49 | Jejunum | NM | Ulceration, transmural congestion, submucosal infiltration, and granulation tissue in the involved SB |
| 36 | M | Coats6 | MVC | 26 | Ileum | MT (+) | Histological evidence of bowel ischemia in the involved segment |
| 36 | F | Maull and Rozycki7 | MVC | 4 | Jejunum | NM | Antimesenteric SB perforation |
| 7 | M | Winton et al8 | MVC | 6 | Jejunum | MH (+) | Seromuscular tears proximal and distal to the SB perforation |
| 29 | M | Winton et al8 | MVC | 6 | Jejunum | MH (+) | SB perforation and ischemic sigmoid colon |
| 13 | M | Ross and Bickerstaff9 | Fall from bicycle | 6 | Jejunum | NM | SB perforation with necrotic area at the edge of perforation |
| 32 | M | Fleishman et al10 | MVC | 35 | Ileum | NM | Total disruption of the terminal ileum associated with tissue loss |
| 30 | M | Burrell et al11 | MVC | 11 | Jejunum | NM | SB perforation secondary to bowel infarction |
F = female; M = male; MH = mesenteric hematoma; MT = mesenteric tear; MVC = motor vehicle crash; NM = not mentioned; SB = small bowel.
a. Presence and type of the reported mesenteric injuries are in bold.
This report presents a rare case of delayed bowel perforation in a patient who developed a mesenteric hematoma following BAT. We discuss the possible mechanism underlying this delayed presentation and propose that post-traumatic intestinal perforation be considered in the differential diagnosis of patients who experience a delayed presentation of small bowel perforation following BAT.
2. Case report
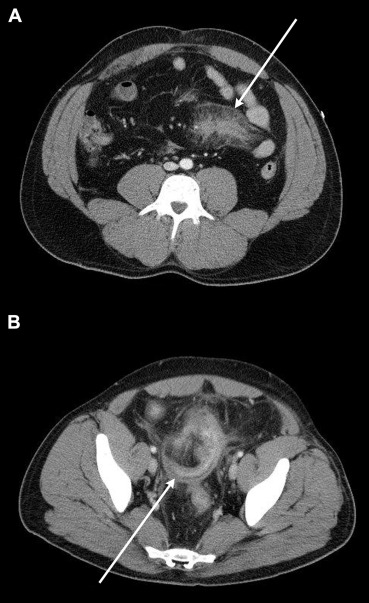
A 32-year-old male presented to our trauma center following a motorcycle accident. He was found to have a closed head injury, rib fractures, left shoulder dislocation, humerus fracture, and open fracture of the left tibia and fibula. A computed tomography (CT) scan of the abdomen with contrast showed a 7 × 4 cm2 mesenteric hematoma (Fig. 1A). A closed reduction of the shoulder dislocation, and an open reduction and internal fixation of his tibia and fibula fractures were performed. He was discharged from the hospital after 1 week of observation. As the patient had open fractures on admission, he received a 10-day course of antibiotics (7 days during the hospital stay and 3 days after his discharge). At the time of discharge, the patient had no fever and was tolerating a regular diet. His abdomen was soft and nontender on examination. His complete blood count showed a normal white blood cell count of 9.03 k/μL (k/μL = thousands per cubic milliliter) (normal range = 4.0–11.0 k/μL). The patient returned to the hospital 4 weeks after discharge (5 weeks post-trauma), complaining of abdominal pain on sitting up and in a standing position. He did not have a fever, was tolerating regular food, and had normal bowel movements. There was no evidence of peritoneal signs on abdominal physical examination. A repeat CT scan of the abdomen with contrast was performed, which showed a thickened narrowed loop of the small bowel adjacent to a mesenteric hematoma at the level of the distal ileum (Fig. 1B). His white blood cell count was 7.59 k/μL (normal range = 4.0–11.0 k/μL). He was discharged home but re-presented 1 week later (6 weeks post-trauma) with signs of acute abdomen. His white blood cell count was measured at 18.94 k/μL (normal range 4.0–11.0 k/μL). An exploratory laparotomy was performed. Intraoperative findings included a phlegmon in the mid lower abdomen with a perforated thickened loop of the small bowel and about 300 mL of purulent material in the abdomen (Fig. 2). He underwent resection and anastomosis of the small bowel.
|
|
|
Figure 1. (A) Abdominal computed tomography immediately after trauma and (B) 5 weeks post-trauma, showing the mesenteric hematoma (white arrow in Fig. 1A) and the stenotic loop of the small bowel adjacent to the hematoma (white arrow in Fig. 1B). |
|
|
|
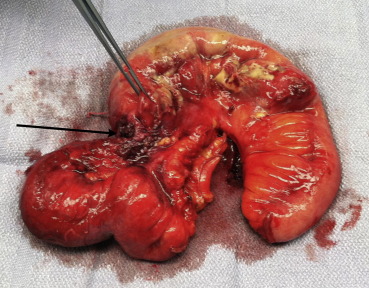
Figure 2. Postoperative specimen of the resected segment of the small bowel showing its thickened, inflamed, and perforated loop. The site of perforation is indicated with a black arrow. |
3. Discussion
Various pathophysiological mechanisms (deceleration, crushing, and rupture phenomena) are responsible for small bowel perforations following BAT.1 These mechanisms are generally responsible for small bowel injury in cases where perforations of the small bowel from BAT present soon after the initial trauma. Direct injury mechanisms described by Vertruyen et al1 do not explain the situations where the small bowel perforation develops a few weeks after the blunt abdominal trauma.
Post-traumatic mesenteric injury is a potentially life-threatening complication of BAT and can cause severe hemorrhage and/or bowel ischemia. Many cases with minor and isolated mesenteric injuries may remain subclinical and go undiagnosed for a period of time.12 Delayed intestinal stenosis resulting in small bowel obstruction after BAT has been reported by our group and other authors.13 ; 14 We reviewed the literature and discussed the possible mechanism for this feared complication in our previous report.13
In situations where the post-traumatic mesenteric injury is not severe and consists of only minor tears and contusions, the clinical presentation would follow a period of normal bowel function and may be delayed by a time period ranging from 2 weeks to 3 months.13
Patients with such injuries need to be followed closely with repeated physical examinations to detect any signs of peritonitis, and if necessary with serial X-ray investigations (abdominal X-rays and/or abdominal CT scans).
The clinical presentation is normally a consequence of a mesenteric tear or hematoma formation, which can affect progressively blood supply to the small bowel and cause partial ischemia of the adjacent bowel segment, partial- or full-thickness intestinal wall ischemia, mucosal ulceration, and submucosal inflammation.13 Severe steatorrhea and profound weight loss are other presentations of ischemic small bowel stricture and blind loop syndrome, which have also been reported in association with a partial mesenteric tear.15
The subsequent occurrences depend to a great extent on the dominance of progressive ischemia or takeover by a healing process. It is possible to have a dominant healing process with continuous fibrosis formation, ultimately leading to stricture and bowel obstruction, as well as a progressive ischemia and ulceration resulting in bowel perforation (the current case). These two pathophysiologic scenarios can occur simultaneously with synergistic effects. The presence of stricture and bowel obstruction would lead to an increase in intraluminal pressure in the affected small bowel segment, which affects the intestinal wall circulation even further.5 The increase in intraluminal pressure would expedite the process of ulcer formation, resulting in bowel perforation.
In the absence of a direct bowel injury, a patient may initially tolerate a diet and display normal bowel function. In the current patient, we believe that the perforation was a complication of the mesenteric hematoma, which compromised blood flow to this bowel segment. This mechanism may explain the situation in the cases reported by other authors as well.5; 6 ; 8
4. Conclusion
Based on our experience and following a review of the reported cases in the literature, we propose that post-traumatic intestinal perforation be considered in the differential diagnosis of patients who experience a delayed presentation of small bowel perforation following BAT. While we agree that hemodynamically stable and asymptomatic post-trauma patients with a mesenteric tear and/or hematoma following BAT can be managed conservatively, the surgical team should be aware of possible delayed complications of such injuries. These concerns should be shared with the patient when planning the management, and the patient should be followed closely so that such complications can be detected very early during the course of follow-up.
Consent
Written informed consent was obtained from the patient whose case is discussed in this paper regarding the publication of this case report and accompanying images.
Acknowledgments
The authors would like to thank Mr John Cyrus for his editorial assistance and Ms Lory Tubbs, Graphic Designer at the Louisiana State University Health Sciences Center, for her help with the preparation of the images.
References
- 1 M. Vertruyen, J. Nardini, J. Bruyns; Isolated perforations of the small bowel from blunt abdominal trauma. Report of two cases and review of the literature; Acta Chir Belg, 95 (1995), pp. 76–80
- 2 W. Ceelen, U. Hesse, B. De Hemptinne; Small bowel perforation following blunt abdominal trauma; Acta Chir Belg, 95 (4 suppl.) (1995), pp. 187–189
- 3 G.R. Faria, A.B. Almeida, H. Moreira, E. Barbosa, P. Correia-da-Silva, J. Costa-Maia; Prognostic factors for traumatic bowel injuries: killing time; World J Surg, 36 (2012), pp. 807–812
- 4 P.D. How, H. Feddo, E. Woo, A. Huang; Delayed ileal perforation secondary to traumatic stricture presenting as pyrexia of unknown origin; Ulus Travma Acil Cerrahi Derg, 15 (2009), pp. 185–187
- 5 V. Subramanian, R.S. Raju, F.L. Vyas, P. Joseph, V. Sitaram; Delayed jejunal perforation following blunt abdominal trauma; Ann R Coll Surg Engl, 92 (2010), pp. W23–W24
- 6 T.J. Coats; Delayed presentation of perforation of the ileum following seat belt trauma; Arch Emerg Med, 8 (1991), pp. 144–146
- 7 K.I. Maull, G.S. Rozycki; Delayed presentation of traumatic blunt small bowel perforation; J Tenn Med Assoc, 79 (1986), pp. 287–288
- 8 T.L. Winton, M.J. Girotti, P.N. Manley, E.E. Sterns; Delayed intestinal perforation after nonpenetrating abdominal trauma; Can J Surg, 28 (1985), pp. 437–439
- 9 W.B. Ross, D.R. Bickerstaff; Late jejunal perforation following blunt injury; Injury, 16 (1985), p. 481
- 10 H.A. Fleishman, G.L. Griffith, B.A. Bivins; Delayed perforation of small bowel following blunt abdominal trauma; J Ky Med Assoc, 77 (1979), pp. 294–295
- 11 M. Burrell, R. Toffler, R. Lowman; Blunt trauma to the abdomen and gastrointestinal tract. Plain film and contrast study; Radiol Clin North Am, 11 (1973), pp. 561–578
- 12 B.W. Nolan, S.G. Gabram, R.J. Schwartz, L.M. Jacobs; Mesenteric injury from blunt abdominal trauma; Am Surg, 61 (1995), pp. 501–506
- 13 A. Northcutt, A. Hamidian Jahromi, L. Johnson, A.M. Youssef; Unusual late occurrence of bowel obstruction following blunt abdominal trauma; J La State Med Soc, 163 (2011), pp. 305–307
- 14 G. Kaban, R.A. Somani, J. Carter; Delayed presentation of small bowel injury after blunt abdominal trauma: case report; J Trauma, 56 (2004), pp. 1144–1145
- 15 P. Isaacs, M. Rendall, E.O. Hoskins, G.A. Missen, G.E. Sladen; Ischemic jejunal stenosis and blind loop syndrome after blunt abdominal trauma; J Clin Gastroenterol, 9 (1987), pp. 96–98
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?