Abstract
Objective
The purpose of this research is to evaluate the ethical aspects of informed consent process of total knee arthroplasty (TKA) patients in Turkey.
Methods
The study included 50 patients undergoing TKA in Gazi Mustafa Kemal State Hospital Orthopedics Clinic. A face to face survey was conducted to determine the ethical appropriateness of the main components of informed consent process such as; disclosure of material information about the disease and alternative treatment options, understanding the disclosed information, comprehending the written consent form and voluntariness in deciding.
Results
The survey revealed that all TKA patients signed informed consent form, 80% of the participants received material information about their disease, 62% were disclosed information about TKA operation, 56% read (in personal or with the assistance of a relative) the written informed consent form, 28% received information regarding possible complications of TKA and 85% were not given any information about the alternative treatments.
Conclusions
Informed consent process in TKA patients have flourished compared to previous years, but still there are some aspects in need of improvement. Using short and understandable language, developing multi-media sources and involving patients to informed consent form development process would contribute to the process.
Keywords
Total knee arthroplasty ; Informed consent ; Respect to autonomy ; Ethical principle
Introduction
The word autonomy , derived from the Greek authos (‘self’) and nomos (‘rule,’ ‘governance’), referred to self-governance of city-states in ancient times. The definition of the term has since been expanded to include concepts such as individual choice, freedom of will, and right to liberty. In the context of medical ethics, autonomy is defined as the patients right and ability to decide on the medical intervention for him- or herself, free from both controlling interference by others and limitations such as inadequate understanding and paternalistic approach of the physician that prevent making an informed rational choice. 1 Respect for the autonomy of the patient is considered as one of the main principles of medical ethics. Informed consent is the practical implementation of respect for the principle of autonomy and is defined as the autonomous authorization of a medical intervention or participation in research.
Informed consent should be regarded with particular interest for total knee arthroplasty (TKA) patients. One reason for this is that patients undergoing TKA tend to be seniors, and old age may augment pre- and postoperative risks and diminish the competency of patients required for autonomous consent.2 Another important aspect of informed consent in TKA patients is the possibility of increased exposure to lawsuits in the absence of proper written informed consent.3 The legal immunity acquired by the orthopedist through proper written informed consent is crucial, as the average settlement against orthopedic surgeons is higher than that of other surgical specialties. In a study by the American Knee and Hip Surgeons Association, it was determined that 78% of orthopedic surgeons face at least one malpractice lawsuit in their careers.4 Studies in the literature propose that enhancing the orthopedic surgeons knowledge and setting the standards for obtaining informed consent from patients may help to diminish the legal problems that may arise as a result of surgical procedures.5 Despite this understanding, very little research has been conducted regarding the legal and ethical appropriateness of the informed consent procedure in TKA patients in Turkey. The purpose of this survey was to evaluate the informed consent procedure for TKA patients in Gazi Mustafa Kemal State Hospital from an ethical perspective. This evaluation serves to identify the ethical problems in the procedure and discuss possible interventions to overcome them.
Patients and methods
The informed consent procedures of 50 patients, selected by simple randomization method among competent patients undergoing TKA, were evaluated between February and April 2015. Five orthopedic surgeons participated and obtained the informed consent forms from the study group.
The survey began by collecting demographic data regarding age, sex, and diagnosis of the patients. This section was followed by questions on the information given to patients through the informed consent procedure about their diagnosis, the surgical treatment, alternative treatments other than TKA, and most probable complications they may face. Participants were asked if they had read and understood the written informed consent form, as well as about their perception about the clarity of the form. Patients who did not read the written informed consent form were asked further about the reason of their avoidance.
Informed consent of each patient was obtained prior to their participation. This study was approved by the local ethical committee.
Forty-three female and 7 male patients participated in the study. The average ages of female and male participants were 66.1 years and 81.8 years, respectively. Twenty-seven patients (54%) had right knee gonarthrosis, 16 (32%) left knee gonarthrosis, and 7 (14%) bilateral gonarthrosis. Twenty-nine patients (58%) had undergone prior surgery, and 21 revealed that they were not presented with an informed consent form (Table 1 ).
| Age (years) | N | % | |
|---|---|---|---|
| 51–60 | 8 | 16 | |
| 61–70 | 26 | 52 | |
| 71–80 | 15 | 30 | |
| 81–90 | 1 | 2 | |
| Gender | N | % | |
| Female | 43 | 86 | |
| Male | 7 | 14 | |
| Education | N | % | |
| Illiterate | 13 | 26 | |
| Literate (without graduation from primary school) | 14 | 28 | |
| Primary school | 21 | 42 | |
| Secondary school | 2 | 4 | |
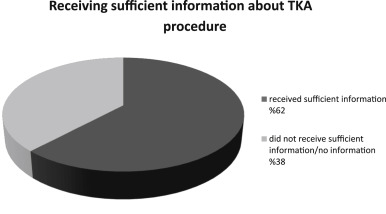
Written and signed informed consent was taken from all patents. Forty patients (80%) stated that they had received sufficient information about their disease, while 10 (20%) were not satisfied with the amount of information given. The dissatisfied patients explained that they would like to learn more about the etiology, course, and severity of the disease, as well as the duration of treatment. Thirty-one participants (62%) revealed that they were given sufficient information about the TKA procedure, while 19 (38%) said the information was insufficient or deficient, or that they received no information. The dissatisfied group was asked about the information they would like to have. Feedback from the group indicated that duration of hospitalization and time until return to routine activities of daily living were of primary concern (Table 2 ).
| Right knee gonarthrosis | 27 (54%) |
|---|---|
| Left knee gonarthrosis | 16 (32%) |
| Bilateral gonarthrosis | 7 (14%) |
Most participants were not satisfied with the disclosed information about possible complications of TKA. Only 14 participants (28%) said they received enough information about complications, and 36 (72%) said they wished to have obtained more comprehensive information. The questions on information disclosure on alternative treatment options—an essential component of informed consent, with the utmost importance—were answered positively by 15 participants (30%), who stated the information they were given on this issue was sufficient. Furthermore, 2 of these 15 participants revealed that they had tried alternative medical and physical treatments but did not benefit from them, leading them to elect TKA after consultation with their physicians. Thirty-one participants (62%) were not content with the information they were given regarding alternative treatment options, and 4 (8%) said they were completely ignorant of the possibility of treatment options besides TKA (Graph 1 ).
Graph 1.
Satisfaction by the disclosed information.
Participants were asked if they read the informed consent form; 15 participants (30%) said that they had read the informed consent form. Twelve participants (24%) said their relatives read the form to them, the reasons for this mainly being because these patients were illiterate or possessed inadequate reading skills to independently comprehend the form. Twenty-three participants (43%) did not read the form or did not have it read to them. The reasons for not reading the form were as follows:
- There were too many foreign words which they did not understand.
- The font of the letters was too small to see and read.
- They were already told by their physicians what was written in the form.
- They believed they would not comprehend the form even if they read it.
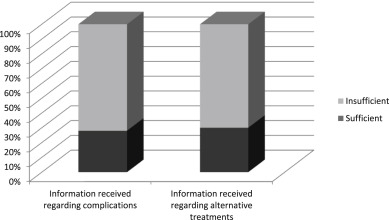
This data is presented in Graph 2 and Table 3 .
Graph 2.
Information received about complications and alternative treatments.
| Patients satisfied with disclosed information | Patients unsatisfied with disclosed information | |
|---|---|---|
| About the disease | 40 (80%) | 10 (20%) |
| About TKA procedure | 31 (62%) | 19 (38%) |
| About alternative treatment options | 15 (30%) | 35 (70%) |
| About TKA complications | 14 (28%) | 36 (72%) |
Twenty-two participants who read the informed consent form or had a relative read the form to them said that they understood the content. Five participants revealed that they did not understand what they read. The reasons for not being able to understand were as follows:
- There were too many words which they were not familiar with.
- The form was too long to read and follow.
- The sentences were too complicated.
This data is presented in Table 4 .
| Read independently by patient | Read to patient by relative | Did not read |
|---|---|---|
| 15 (30%) | 12 (24%) | 23 (46%) |
The limitations of the study are the relatively small sample size (n = 50) and the fact that the samples were taken from a single hospital. Therefore, more research is needed in different hospitals and settings in Turkey before generalizing the results. Another limitation is the female gender dominance of the participants. This might have affected the results, since literacy and level of education is significantly lower in women than men in Turkey. The demographic data of the participants is compatible with this fact. All illiterate participants (n = 13) were women. Moreover, 12 participants who could read and write but had not completed primary school (n = 14) were women. This increased the number of participants who did not read the informed consent by herself.
Discussion
Studies in Turkey show an upwards trend in the rate of obtaining informed consent from patients.6 The rate of taking written consent from patients was 71% in 1996, whereas it increased to 89.9% in 2005 in a range of surveys.7 This improvement is verified by the present study, which shows 100% of patients were given written informed consent before TKA. This improvement may be attributed to the following:
- The force of legislative obligations to obtain written informed consent from each and every patient.
- The positive effect of proper informed consent on number of malpractice lawsuits and administrative complaints.
- Considering informed consent as an essential component of quality assessments of health facilities.
- The wide acceptance of the informed consent concept in the medical literature.
Informed consent has greater legal and ethical importance in major surgeries such as TKA. Thus, disclosing proper information regarding risks of the operation and discussing pros and cons of alternative treatment options are crucial. Additionally, studies have shown the desire of patients to receive information regarding the general risks of the operation, alternative treatment options, and probable limitations in quality of life postoperatively.2
The results of our survey show that informed consent was obtained from all study participants. However, some issues arose regarding the disclosed information about the course of gonarthrosis, TKA procedure, and alternative treatments options, as well as the context, letter font, and wording of the written consent form.
The results of the survey reveal that 38% of the participants were not satisfied with the amount of information they received regarding their disease and TKA. This finding constitutes a significant problem, as it is crucial for the patient to be aware of the course of their disease, the surgical procedure they will undergo, the expected duration of hospitalization, and the expected duration until return to their daily routines in order to make a rational decision and give full consent. Informed consent is the decision of the patient to consent or decline a medical intervention by processing objective data rationally and reaching a decision in compliance with his or her ethical values.8 Therefore, dissatisfaction with the disclosed information on these issues indicates a deficiency of respect to autonomy of the patients in the discourse of informed consent.
The amount of information to be disclosed is a subjective benchmark which varies widely among diseases and patients. While studies in the literature report that most patients would like to be briefed on the possible consequences they would face if they decline the proposed surgery and the impact of the surgery on their work and routine daily lives,9 ; 10 ; 11 there is data which demonstrates that not only patients undergoing TKA but also other major surgeries such as cardiovascular and cancer surgery face insufficient information disclosure regarding their disease and surgical procedure.12 ; 13 In this context, surgeons who perform major surgery, such as orthopedic surgeons, should be mindful to disclose sufficient information—including the course of the surgery, with special attention to pre- and postoperative consequences of the surgery and expected quality of life—to their patients, so that the patients may consent or decline the surgery on a rational basis.
Discussion of alternative treatments is both an essential process for ensuring adherence to the principle of autonomy and a requirement of patient rights in the context of the right to have access to less risky treatment options. Our survey shows that 70% of patients did not receive content information on alternative treatment options to TKA. Our results support those of Braddock et al, who in 2008 revealed that 62% of orthopedic surgeons gave limited or no information on alternative treatments.14
On the other hand, some participants reported being in regular contact with their orthopedists and having tried conservative treatment options, which, having failed, led them to elect to undergo TKA. This indicates that chronic diseases such as gonarthrosis should involve long-term patient–physician relationship and that disclosure of information and informed consent procedure should begin long before the discussion of major surgery such as TKA. An ongoing interaction between the patient and physician reduces the need to formally discuss alternative conservative treatments to TKA.15 Therefore, the particular nature of the patient–physician relationship in cases of chronic diseases such as gonarthrosis should be taken into consideration while assessing the informed consent process in an ethical context.
Another finding of the present study is the deficiency of patient information regarding the complications of TKA, which is in agreement with previous reports in the literature. In 2005, Bhattacharyya et al conducted a survey which showed that 13 of 28 malpractice law suits against orthopedic surgeons hinged on the claim that the patients were not informed before surgery about potential complications which were later experienced.16 A study by Egri et al revealed an average rate of information disclosure regarding surgical complications by orthopedists and other specialists who perform major surgery of 42%.17 It has been stated that informing patients comprehensively regarding the most common complications of the surgical operation reduces the risk of exposure to lawsuits and administrative complaints.5 ; 18
There is discussion regarding which complications should be addressed and the extent of information that should be given during the informed consent procedure. In the guide published by the National Institute of Health in the UK, it is stated that “complications which appear at a scientifically significant rate should be discussed prior to surgery.”19 The American Association of Orthopedic Surgeons advises informing patients about common complications as well as rare but severe complications. Patient attitude is another determining factor in the extent to which complications should be discussed. Some patients request as much information as possible, while others may be contented with little information, with trust in their physicians to follow the best course of action.19 ; 20 Despite these differing attitudes of patients, studies on various patient groups in the literature demonstrate that patient groups consider major complications as an important piece of information.9 ; 12 ; 21
Consequently, these reports illustrate that major surgery such as TKA requires a well-established patient–physician relationship. Legal obligations, risks, and ethical imperatives require orthopedists to develop a rational attitude rather than a conservative paternalistic approach to their patients. Deliberative attitude positions the orthopedist in a hierarchically equal position with the patient and asks him or her to disclose sufficient information to his or her patient and respect the patients ethical values and prospects of life at the same time. This approach protects the dignity and respects the autonomy of the patient, as well as supports the patient to develop insight to make the proper choice for him- or herself as a rational ethical subject. The deliberative attitude can help fulfill the legal and ethical obligations of proper informed consent and meet the expectations of the patient.
The results of the survey reveal that although 100% of participants gave written informed consent for TKA, more than half of the participants did not comprehend the content of the informed consent form. The predominance of female participants in the present study could have an effect on this result, since the level of education and literacy is lower in females than males in Turkey. This result indicates that the level of comprehension is affected by the education level and comprehensive capacity of the patients.22 Refining the consent procedure to stimulate communication and adopting health literacy-based informed consent process would promote obtaining ethically sound informed consent from patients.23
The survey results showed that some patients avoid reading the consent form. The belief of not being able to comprehend the documents contents and the presence of many words that are unfamiliar to the patients were reported as the main reasons of this avoidance. Similar negative assessments regarding informed consent forms are found in the literature.3 Some recommendations have been put forth in the literature to improve the readability and comprehensibility of informed consent forms. Expanding the form to take education and health literacy levels of patients into consideration, using concise and easily understandable simple sentences, and choosing a letter type and font size suitable for all are the most common recommendations for producing reader-friendly consent forms.23 ; 24 Furthermore, using multimedia sources to provide additional supplementary information has been found to have positive impact on the informed consent procedure.25 Patients should be involved in the informed consent form development process, so as to most effectively develop an easily understandable document in plain language.
Conclusion
Informed consent procedure is an essential part of medical intervention, with legal and ethical obligations. To have a signed informed consent form in the dossier of the patient is enough to meet the legal requirements but it is not sufficient to fulfill the ethical obligations. In the ethical context, informed consent is a procedure which can be accomplished only with the fulfillment of all components. TKA is among major surgeries with significant impact on the quality of life and future life prospects of the patients. Therefore, the informed consent procedure should be performed properly with TKA patients to safeguard the respect to autonomy principle and dignity of the patient. The results of this survey show that while the informed consent process of TKA patients in Turkey has improved, further development is required.
Conflict of interest
None declared.
References
- 1 T.L. Beauchamp, J.F. Childress; Principles of Biomedical Ethics; (5th ed.)Oxford University Press, New York (2001), pp. 57–103
- 2 American Association of Orthopedic Surgeons. Code of Ethics and Professionalism for Orthopedic Surgeons. http://www.aaos.org/about/papers/ethics/code.asp erişim 08.04.15.
- 3 A. Upadhyay, S. York, W. Macaulay, B. McGrory, J. Robbennolt, B.S. Bal; Medical malpractice in hip and knee arthroplasty; J Arthroplast, 22 (6 suppl 2) (2007), pp. 2–7
- 4 M.R. Johnson, J.A. Singh, T. Stewart, T.J. Gioe; Patient understanding and satisfaction in informed consent for total knee arthroplasty: a randomized study; Arthritis Care Res (Hoboken), 63 (2011), pp. 1048–1054
- 5 N. Beresford-Cleary, J. Halliday, L. Biant, S. Breusch; Consent process for elective total hip and knee arthroplasty; J Orthop Surg, 19 (2011), pp. 274–278
- 6 E.R. Aydın, Ö.M. Şenses, A. Akpınar, N. Ersoy; Ortopedide Aydınlatılmış Onama Ait Etik Sorunlar: Kocaeli’den Bir Örnek Turkiye Klinikleri; J Med Sci, 31 (2011), pp. 455–463
- 7 F. Ağalar, M. Çakmakçı, K. Yorgancı, G. Ergör, İ. Sayek; Hasta memnuniyeti-aydınlatma ve aydınlatılmış onam sorunu; Toplum Hekim Bülteni (1996), pp. 11–12
- 8 M. David; Clarke autonomy, rationality and the wish to die; J Med Ethics, 25 (1999), pp. 457–462
- 9 H. El-Wakeel, G.J. Taylor, J.J. Tate; What do patients really want to know in an informed consent procedure? A questionnaire-based survey of patients in the bath area; U. K. J Med Ethics, 32 (2006), pp. 612–616
- 10 P.A. Newton-Howes, N.D. Bedford, B.R. Dobbs, et al.; Informed consent: what do patients want to know?; N. Z. Med J, 111 (1998), pp. 340–342
- 11 E. Aunan; Writing information and consent prior to orthopedic surgery; Tidsskr Nor Laegeforen, 123 (2003;25), pp. 2594–2596
- 12 H.A. Vohra, J. Ledsham, H. Vohra, R.L. Patel; Issues concerning consent in patients undergoing cardiac surgery-the need for patient-directed improvements: a UK perspective; Cardiovasc Surg, 11 (2003), pp. 64–69
- 13 D. Feldman-Stewart, S. Chammas, C. Hayter, J. Pater, W.J. Mackillop; An empirical approach to informed consent in ovarian cancer; J Clin Epidemiol, 49 (1996), pp. 1259–1269
- 14 C. Braddock, P.L. Hudak, J.J. Feldman, S. Bereknyei, R.M. Frankel, W. Levinson; Surgery is certainly one good option: quality and time-efficiency of informed decision-making in surgery; J Bone Jt Surg Am, 90 (2008), pp. 1830–1838
- 15 A. Atrey, I. Leslie, J. Carvell, et al.; Standardised consent forms on the website of the British Orthopaedic Association; J Bone Jt Surg Br, 90-B (2008), pp. 422–423
- 16 T. Bhattacharyya, H. Yeon, M.B. Harris; The medical-legal aspects of informed consent in orthopaedic surgery; J Bone Jt Surg Am, 87 (2005), pp. 2395–2400
- 17 M. Hassan; Informed consent and the law—an English legal perspective; Dig Dis, 26 (2008), pp. 23–27
- 18 M. Egri, O. Celbis, M. Karaca, B. Ozdemir, A.N. Kok; The informed consent status for surgery patients in eastern Turkey: a cross-sectional study; Indian J Med Ethics, 5 (2008), pp. 26–28
- 19 Department of Health; Good Practice in Consent Implementation Guide: Consent to Examination or Treatment; Department of Health Publications, London (2001) http://www.health.wa.gov.au/mhareview/resources/documents/UK_DOH_implementation_guide.pdf Accessed 01.04.15.
- 20 W. Holt; Informed Consent: A Process, Not a Piece of Paper. American Academy of Orthopaedic Surgeons; (2007) http://www.aaos.org/news/bulletin/sep07/managing5.asp erişim 08.04.15.
- 21 K. Degerliyurt, J.C. Gunsolley, D.M. Laskin; Informed consent: what do patients really want to know?; J Oral Maxillofac Surg, 68 (2010), pp. 1849–1852
- 22 R.F. Ittenbach, E.C. Senft, G. Huang, J.J. Corsmo, J.E. Sieber; Readability and understanding of informed consent among participants with low incomes: a preliminary report; J Empir Res Hum Res Ethics, 10 (2015), pp. 444–448
- 23 M.J. Miller, M.A. Abrams, B. Earles, K. Phillips, E.M. McCleeary; Improving patient-provider communication for patients having surgery: patient perceptions of a revised health literacy-based consent process; J Patient Saf, 7 (2011), pp. 30–38
- 24 S. Kusec, S. Oresković, M. Skegro, D. Korolija, Z. Busić, M. Horzić; Improving comprehension of informed consent; Patient Educ Couns, 60 (2006), pp. 294–300
- 25 E. Bollschweiler, J. Apitzsch, R. Obliers, et al.; Improving informed consent of surgical patients using a multimedia-based program? Results of a prospective randomized multicenter study of patients before cholecystectomy; Ann Surg, 248 (2008), pp. 205–211
Document information
Published on 31/03/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?