Summary
Objective
The purpose of this study was to investigate the expression of glial cell derived neurotrophic factor (GDNF), glypican-1 (GPC-1), and matrix metalloproteinase-9 (MMP-9), and their association with clinicopathologic characteristics as well as prognostic significance in pancreatic cancer.
Methods
Immunohistochemical assessment of GDNF, GPC-1, and MMP-9 was performed in 62 cases of surgically resected pancreatic cancer. Perineural invasion in pancreatic cancer was observed by marking nerve fiber with S-100, while 16 normal pancreatic tissues were used as normal control. Correlations of GDNF, GPC-1 and MMP-9 expressions with clinicopathologic parameters were analyzed. A survival analysis was performed to find the prognostic significance.
Results
The expressions of GDNF, GPC-1 and MMP-9 in pancreatic cancer tissue were significantly higher than of those in normal pancreatic tissues (41/62 vs. 5/16 for GDNF, 35/62 vs. 2/16 for GPC-1, and 37/62 vs. 3/16 for MMP-9; p < 0.01, respectively). The overexpression of GDNF, GPC-1, and MMP-9 in pancreatic cancer tissue was significantly related to the perineural invasion (p < 0.05). Although the overexpression of these genes was related to poor survival, GPC-1 had an independent prognostic effect on overall survival.
Conclusion
GPC-1 is significantly related to the perineural invasion of pancreatic cancer, holding some prognostic significance in patients with pancreatic cancer.
Keywords
GDNF;GPC-1;MMP-9;perineural invasion;pancreatic cancer
1. Introduction
Globally, pancreatic cancer is equivalent to 2.5% of all types of cancer. However, because of its high mortality, it ranks as the fourth or fifth most frequent cause of cancer death in most developed countries.1 The mortality of pancreatic cancer is also equivalent to its incidence per year.1 ; 2 This high mortality is mainly attributed to local invasion and distant metastasis.3 Perineural invasion (PNI) is one of the most important modes of invasion, which happens even in the early stage.4 It limits radical resection and promotes local recurrence, which negatively impacts survival time and life quality of the patients with pancreatic cancer.5 In spite of this, the mechanism of PNI remains unknown. Although research interests have covered a wide range of genetic and epigenetic alterations, recent research6; 7 ; 8 has focused on the roles of glial cell line-derived neurotrophic factor (GDNF), glypican-1 (GPC-1), and matrix metalloproteinase-9 (MMP-9); this is because all of them are highly expressed in various carcinomas, promoting tumor invasion and metastasis. However, little is known about their involvement in PNI in pancreatic cancer. GDNF belongs to the transforming growth factor (TGF)-β superfamily, which is known as HBGFs after combining with heparan.6 GPC-1 can regulate the combination of HBGFs with their high-affinity receptors and enhance tumor growth and invasion.9 ; 10 Okada et al. have revealed that GDNF increases MMP-9 mRNA and protein expression in MIA PaCa-2 cells in a dose-dependent manner.11 Koyama et al12 have showed that the interaction of GPC-1 heparan sulphate chains with MMP-9 on the cell surface is crucial for the migration and invasion of the murine colon adenocarcinoma cells. All these findings suggest some correlation between these factors, yet the key factor to the pancreatic cancer invasion is not known. In the current study, the protein expressions of GDNF, GPC-1, and MMP-9 in pancreatic cancer tissue were investigated, and a correlative analysis of the three factors with the clinical features and survival time of the patients was performed to find out what was the most significant factor among them.
2. Materials and methods
2.1. Patients and tissue sampling
The specimens of pancreatic cancer tissues were taken from 62 patients who underwent radical excision for pancreatic ductal adenocarcinoma between January 2003 and December 2010 at the Department of General Surgery, Xiangya Hospital, Central South University (Changsha, China). All the specimens were ductal adenocarcinoma, and the diagnosis was confirmed by two pathologists at our hospital. Another 16 pancreatic specimens were obtained from the patients of pancreatic injury as normal control samples for the tests. The samples were fixed in 10% formalin immediately after being taken from the patients. A prior informed consent was obtained from the patients for the specimen collection, and the study protocols were approved by the Ethics Committee of Central South University. All specimens were handled and made anonymous according to the ethical and legal standards.
The specimens were fixed with 10% formalin, routinely processed for embedding in paraffin, and cut into 4-μm sections in five randomized choosing sites. Every site was cut down into four pieces (used for PNI, GDNF, GPC-1, and MMP-9 each).
For immunohistochemical analysis, the sections were stained by streptavidin-peroxidase method with the use of a DAB kit (mouse monoclonal, Santa Cruz Biotechnology, United States of America). After deparaffinization and dehydration, the sections were subjected to microwave oven treatment in 0.01 mol/L sodium citrate buffer (pH 6.0) for 10 minutes to block endogenous peroxidase. All the sections were then immersed in nonimmune serum (blocking reagent) for 5 minutes to block nonspecific immunoglobulin-binding sites. After removal of excess serum, primary antibodies for S-100 (rabbit polyclonal; 1:100; Santa Cruz Biotechnology), GDNF (rabbit polyclonal; 1:50; Santa Cruz Biotechnology), GPC-1 (rabbit polyclonal; 1:50; Santa Cruz Biotechnology), and MMP-9 (rabbit polyclonal; 1:50; Santa Cruz Biotechnology) were added to the sections and incubated overnight at 4°C. Then, the sections were washed 2 × 3 minutes with phosphate buffer solution (PBS), incubated with secondary antibody (mouse anti-rabbit; 1:100; Santa Cruz Biotechnology) for 20 minutes, and with streptavidin-peroxidase complex for 20 minutes. After washing 2 × 3 minutes with PBS, the sections were stained with diaminobenzidine tetrahydrochloride, freshly prepared in trihydroxymethyl aminomethane (TRIS) buffer containing 0.01% H2O2. Nuclei were lightly counterstained with hematoxylin. For negative controls, the sections were incubated with PBS instead of the primary antibody. Finally, the sections were mounted on slides with Permount after dehydrated in alcohol and cleared in xylene.
2.2. Evaluation of positive PNI
PNI is defined as the presence of cancer cells in the perineurium.13 On every case, five sections were used for detecting S-100, which was stained in the area of neural fascicle and its perineurium in brown color; the cases in which cancer cells were present in any medial perineurium were regarded as PNI (+). If no cancer cells were seen in the medial perineurium of any of the five sections, then the case was called as PNI (−).
2.3. Evaluation of immunohistochemical staining
On each section, five randomly chosen fields were used for counting both the positive cells and negative cells; a percentage was calculated for positive cells among the whole cells counted. Fine granular plasma and/or membrane staining was regarded as positive. We classified the results into four grades: (0), positive cells accounted for less than 10%, (1) between 10% and 29%, (2) between 30% and 49%, and (3) more than 50%. The intensity of staining was graded as: 0 = none; 1 = weak brown; 2 = moderate brown; and 3 = strong brown. An overall score for each sample was calculated as grade × intensity. Scores ≥ 2 was considered (+), and scores < 2 were considered (−). One pathologist, blinded to the clinical data, observed and evaluated all the slides.
2.4. Follow-up
Follow-up was either performed by interviewing the patients in our institution on an outpatient basis or by contacting their guardian who took care of them. The cutoff for clinical follow up was December 31, 2011. Survival was calculated from the date of primary resection until the date of death from any cause for overall survival. For patients lost to follow-up, data were censored at the date the patient was last contacted alive.
2.5. Statistical analyses
SPSS version 13.0 for Windows (SPSS Inc, Chicago, IL, USA) was used for the statistical analysis. Patients’ clinicopathologic characteristics were compared between groups using Chi-square or Fishers exact test for categorical variables. Survival estimates were analyzed with Kaplan and Meier survival curves by the log-rank test. Logistic regression analysis was performed to identify variables significantly associated with clinicopathological data. The Cox proportional hazards model was used to identify variables related to overall survival. A value of p < 0.05 was considered statistically significant.
3. Results
3.1. Expression and localization of S-100, GDNF, GPC-1, and MMP-9 in pancreatic tissues
Positive S-100 staining (showing in brown color) was detected in the neural fascicle and its perineurium in almost every section; 32 cases were PNI (+) (32/62, 51.6%). The cancer cells were present in medial perineurium (Fig. 1A). General data (sex, age, tumor lymph node metastasis (TNM) stage of the tumor, the differentiation, location and diameter of the tumor, and lymph node involvement) of the patients are listed in Table 2.
|
|
|
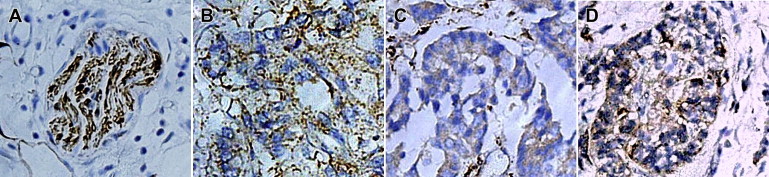
Figure 1. The representative images of immunochemistry (counterstained with hematoxylin). (A) Nerve fibers marked by S-100. Positive staining of (B) GDNF, (C) GPC-1, and (D) MMP-9 in pancreatic cancer tissue. Brown color indicates the positive staining (×400). GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9. |
Immunohistochemical results are summarized in Table 1. In normal pancreatic tissue, there were only traces of GDNF, GPC-1, and MMP-9 staining. In the pancreatic cancer tissue, the targeted GDNF and GPC-1 were highly expressed and mainly located in the cell membrane and cytoplasm and MMP-9 in the cytoplasm (Figs. 1B–D). GDNF was strongly expressed in pancreatic cancer cells and intrapancreatic nerves. Strong GPC-1 immunoreactivity was present in the fibroblasts surrounding the cancer cells. MMP-9 protein expression was mainly seen in the pancreatic cancer cells. The expression of GDNF in pancreatic cancer cases was significantly higher than of those in normal pancreatic tissues (41/62, 5/16; p < 0.01), as well as the GPC-1 and MMP-9 expressions (35/62, 2/16; p < 0.01; 37/62, 3/16; p < 0.01 respectively).
| Pancreatic cancer (n) | Normal pancreatic tissue (n) | |||
|---|---|---|---|---|
| (−) | (+) | (−) | (+) | |
| GDNF | 21 | 41 | 11 | 5 |
| GPC-1 | 27 | 35 | 14 | 2 |
| MMP-9 | 25 | 37 | 13 | 3 |
GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9.
| Clinicopathologic characteristics | N = 62 | GDNF | GPC-1 | MMP-9 | |||
|---|---|---|---|---|---|---|---|
| (+) | p value | (+) | p value | (+) | p value | ||
| Sex | 0.102 | 0.644 | 0.166 | ||||
| Men | 41 | 30 | 24 | 27 | |||
| Women | 21 | 11 | 11 | 10 | |||
| Age (yr) | 0.534 | 0.773 | 0.051 | ||||
| <60 | 38 | 24 | 22 | 19 | |||
| ≥60 | 24 | 17 | 13 | 18 | |||
| Tumor location | 0.800 | 0.564 | 0.219 | ||||
| Head | 43 | 28 | 26 | 25 | |||
| Body-tail | 19 | 13 | 9 | 12 | |||
| Tumor maximum diameter (cm) | 0.854 | 0.518 | 0.185 | ||||
| <2 | 6 | 4 | 4 | 2 | |||
| 2∼5 | 40 | 25 | 23 | 27 | |||
| ≥5 | 16 | 12 | 8 | 8 | |||
| TNM stage | 0.331 | 0.592 | 0.374 | ||||
| I | 11 | 7 | 6 | 7 | |||
| II | 18 | 14 | 10 | 11 | |||
| III | 33 | 20 | 19 | 19 | |||
| Degree of tissue differentiation | 0.658 | 0.482 | 0.719 | ||||
| High | 33 | 21 | 20 | 19 | |||
| Middle-low | 29 | 20 | 15 | 18 | |||
| Lymph node involvement | 0.242 | 0.482 | 0.231 | ||||
| No | 29 | 17 | 15 | 15 | |||
| Yes | 33 | 24 | 20 | 22 | |||
| Perineural invasion | <0.001* | <0.001* | <0.001* | ||||
| (−) | 30 | 14 | 12 | 12 | |||
| (+) | 32 | 27 | 23 | 25 | |||
- p < 0.05 was considered to be statistically significant, Fishers exact test.
GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9; TNM = tumor lymphnode metastasis.
3.2. Relationship between the expression of GDNF, GPC-1, MMP-9, and clinicopathologic characteristics
The expressions of GDNF, GPC-1, and MMP-9 were significantly linked to PNI (p = 0.002, 0.011, 0.002; Table 2), but not to sex, age, TNM stage, tumor location, size, degree of differentiation, or lymph node involvement in pancreatic cancer. The multiple logistic regression analysis showed that GPC-1 was the most dangerous factor among the three to predict PNI (Table 3).
| Factors | Odds ratio | 95% confidence interval | p value |
|---|---|---|---|
| GDNF [(−) vs. (+)] | 1.424 | 1.264–1.604 | <0.001* |
| GPC-1 [(−) vs. (+)] | 1.925 | 1.755–2.112 | <0.001* |
| MMP-9 [(−) vs. (+)] | 1.509 | 1.356–1.680 | <0.001* |
- p < 0.05 was considered to be statistically significant.
GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9.
3.3. Survival analysis
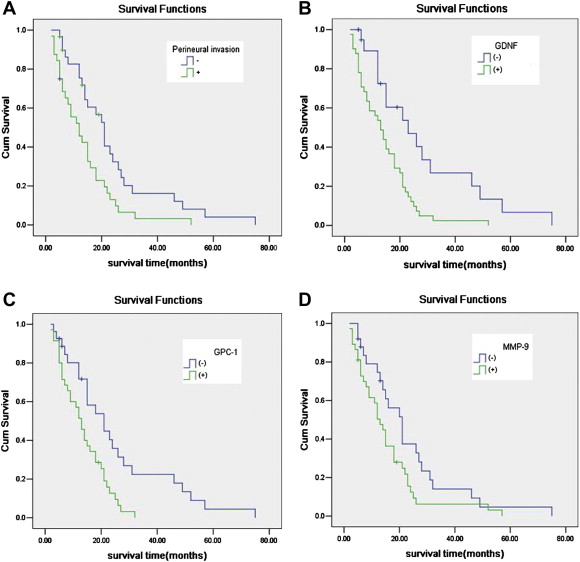
All of the pancreatic cancer patients had been followed 2–75 months (17.2 ± 14.2 months) until their death. There were five patients still alive, and the median survival time after resection was 14 months. Patient survival was associated with PNI (Fig. 2A, log-rank = 7.174, p = 0.007), but not to the sex, age, tumor location, size, degree of differentiation, or lymph node involvement. Even though the log-rank test (Figs. 2B–D) showed that the expression of GDNF, GPC-1, and MMP-9 were all significantly related to the survival rate after resection (log-rank = 9.696, p = 0.002; log-rank = 8.975, p = 0.003; log-rank = 3.899, p = 0.048; respectively), Cox regression analysis of the above four co-variates further confirmed that only the expression of GPC-1 was significantly related to the survival rate after resection (Table 4).
|
|
|
Figure 2. Kaplan-Meier survival curves for the four covariates in pancreatic cancer patients. (A) When PNI is the covariate, the survival time between PNI (+) and PNI (−) is significantly different (p = 0.007, log-rank test); (B) when GDNF is the covariate, survival time between GDNF (+) and (−) is significantly different (p = 0.002, log-rank test); (C) when GPC-1 is the covariate, survival time between GPC-1 (+) and (−) is significantly different (p = 0.003, log-rank test); (D) when MMP-9 is the covariate, survival time between MMP-9 (+) and (−) is significantly different (p = 0.048, log-rank test). GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9; PNI = perineural invasion. |
| Variables | Odds ratio | 95% confidence interval | p value |
|---|---|---|---|
| PNI [(−) vs. (+)] | 1.189 | 0.640–2.209 | 0.584 |
| GDNF [(−) vs. (+)] | 1.237 | 0.836–1.829 | 0.287 |
| GPC-1 [(−) vs. (+)] | 1.584 | 1.055–2.378 | 0.026* |
| MMP-9 [(−) vs. (+)] | 1.159 | 0.850–1.582 | 0.351 |
- p < 0.05 was considered to be statistically significant.
GDNF = glial cell derived neurotrophic factor; GPC-1 = glypican-1; MMP-9 = matrix metalloproteinase-9; PNI = perineural invasion.
4. Discussion
The peripheral nerve system is covered by three membranes: the endoneurium, perineurium, and epineurium. PNI is defined as the presence of cancer cells in the perineurium.13 In this study, we labeled the nerve tissue by S-100 through immunohistochemical staining, which made the detection of nerve tissue easier than through HE staining, and it helped us accurately determine the infiltration of nerve fibers by cancer cells. Furthermore, we stained five sections taken from different locations in each specimen to detect PNI in pancreatic cancer. The expressions of GDNF, GPC-1, and MMP-9 in pancreatic ductal adenocarcinoma tissues were found upregulated. They were positively related with PNI and a worse prognosis postsurgery. Furthermore, GPC-1 was found to be the most significant factor that was related to the degree of PNI and a worse prognosis.
GPC-1, a ubiquitous protein that is attached to the extracytoplasmic surface of the cell membrane, may play a role in the control of cell division and growth.14 Multiple signaling pathways, including the ERK MAPK and c-Myc signaling, are stimulated by GPC-1,15 and it is overexpressed in pancreatic cancer cells and the adjacent fibroblasts.16 Down-regulation of GPC-1in the human pancreatic cancer cell line PANC-1 leads to a prolonged doubling time, and attenuates tumor growth, angiogenesis, and metastasis when these cells are transplanted into athymic mice.7 GDNF, a member of the neurotrophic factor family that is necessary for the growth, development, and reparation of a variety of neural cell types, is found to be associated with the pathogenesis of malignant melanoma, and it is related to the prognosis of patients with pancreatic cancer and also involved in squamous non-small-cell carcinoma.6; 17 ; 18 MMP-9 is a member of the MMP family, which is involved in the breakdown of extracellular matrix in both normal physiologic processes (such as embryonic development, reproduction, and tissue remodeling), and disease processes (such as arthritis and metastasis).19 MMP-9 is also overexpressed in pancreatic cancer and correlated with a worse prognosis.20
Our results are basically in line with above mentioned others findings, with slightly more features being revealed in this study: (1) The overexpression of GPC-1, GDNF, and MMP-9 in pancreatic tumor tissue is linked mainly to PNI, not to other clinical characteristics, (2) GPC-1 is the most dangerous factor among the three in predicting PNI, and (3) even the expression of GDNF, GPC-1, and MMP-9 would prognose a worse survival, only the expression of GPC-1 was significantly related to the survival rate of the patient and it may be used as an independent prognostic factor for pancreatic ductal adenocarcinoma. More interestingly, we found that GPC-1 was significantly related to the survival independent of PNI, which does not contradict our immunohistochemical results, showing various aspects of the involvement of GPC-1 in the cancer other than PNI. The carcinogenetic role of GPC-1 in pancreatic cancer is also further highlighted in recent studies: Whipple et al.21 have found that pancreatic ductal adenocarcinoma growth, angiogenesis, and invasion are enhanced by GPC-1 in a mouse model. Furthermore, the suppression of GPC-1 is suggested to be an important component of therapeutic strategies in pancreatic ductal adenocarcinoma. Di Norcia et al.22 have also found that the loss of RAGE (the receptor for advanced glycation end-products) function inhibits the development of pancreatic intraepithelial neoplasia and its progression to adenocarcinoma, significantly prolonging survival time in mouse models. It is reasonable that among these three pancreatic cancer-related genes, GPC-1 is the one needs further investigation.
In conclusion, we have found through this study that GPC-1 is significantly related to PNI of pancreatic cancer, and that it is with some prognostic significance in patients with pancreatic cancer. Further studies on the molecular mechanisms of PNI and on the prognostic significance of GPC-1 in pancreatic cancer will be required, which may contribute to the establishment of effective pancreatic cancer therapy and may lead to better management of the patients.
Acknowledgments
This study was supported by grants from Sci-Tech Project of Hunan Province of China (S2006F223) and Hunan Provincial Natural Science Foundation (08JJ3071). The authors thank the patients who participated in this study and all the staff members who assisted with the sample collection and pretreatment in the operation room.
References
- 1 P. Maisonneuve, A.B. Lowenfels; Epidemiology of pancreatic cancer: an update; Dig Dis, 28 (2010), pp. 645–656
- 2 A. Jemal, R. Siegel, E. Ward, Y. Hao, J. Xu, M.J. Thun; Cancer statistics, 2009; CA Cancer J Clin, 59 (2009), pp. 225–249
- 3 D. Li, K. Xie, R. Wolff, J.L. Abbruzzese; Pancreatic cancer; Lancet, 363 (2004), pp. 1049–1057
- 4 P.M. Pour, R.H. Bell, S.K. Batra; Neural invasion in the staging of pancreatic cancer; Pancreas, 26 (2003), pp. 322–325
- 5 I. Hirai, W. Kimura, K. Ozawa, et al.; Perineural invasion in pancreatic cancer; Pancreas, 24 (2002), pp. 15–25
- 6 H. Liu, Q. Ma, J. Li; High glucose promotes cell proliferation and enhances GDNF and RET expression in pancreatic cancer cells; Mol Cell Biochem, 347 (2011), pp. 95–101
- 7 T. Aikawa, C.A. Whipple, M.E. Lopez, et al.; Glypican-1 modulates the angiogenic and metastatic potential of human and mouse cancer cells; J Clin Invest, 118 (2008), pp. 89–99
- 8 D. Bausch, T. Pausch, T. Krauss, et al.; Neutrophil granulocyte derived MMP-9 is a VEGF independent functional component of the angiogenic switch in pancreatic ductal adenocarcinoma; Angiogenesis, 14 (2011), pp. 235–243
- 9 Y. Ohshima, I. Yajima, K. Takeda, et al.; c-RET molecule in malignant melanoma from oncogenic RET-carrying transgenic mice and human cell lines; PLoS One, 5 (2010), p. e10279
- 10 Q.W. Ben, J.C. Wang, J. Liu, et al.; Positive expression of L1-CAM is associated with perineural invasion and poor outcome in pancreatic ductal adenocarcinoma; Ann Surg Oncol, 17 (2010), pp. 2213–2221
- 11 Y. Okada, G. Eibl, J.P. Duffy, H.A. Reber, O.J. Hines; Glial cell-derived neurotrophic factor upregulates the expression and activation of matrix metalloproteinase-9 in human pancreatic cancer; Surgery, 134 (2003), pp. 293–299
- 12 Y. Koyama, H. Naruo, Y. Yoshitomi, et al.; Matrix metalloproteinase-9 associated with heparan sulphate chains of GPI-anchored cell surface proteoglycans mediates motility of murine colon adenocarcinoma cells; J Biochem, 143 (2008), pp. 581–592
- 13 M. Kayahara, H. Nakagawara, H. Kitagawa, T. Ohta; The nature of neural invasion by pancreatic cancer; Pancreas, 35 (2007), pp. 218–223
- 14 J.R. Vermeesch, G. Mertens, G. David, P. Marynen; Assignment of the human glypican gene (GPC1) to 2q35-q37 by fluorescence in situ hybridization; Genomics, 25 (1995), pp. 327–329
- 15 H. Kayed, J. Kleeff, S. Keleg, et al.; Correlation of glypican-1 expression with TGF-beta, BMP, and activin receptors in pancreatic ductal adenocarcinoma; Int J Oncol, 29 (2006), pp. 1139–1148
- 16 C. Garnis, J.J. Davies, T.P. Buys, et al.; Chromosome 5p aberrations are early events in lung cancer: implication of glial cell line-derived neurotrophic factor in disease progression; Oncogene, 24 (2005), pp. 4806–4812
- 17 L.F. Lin, D.H. Doherty, J.D. Lile, S. Bektesh, F. Collins; GDNF: a glial cell line-derived neurotrophic factor for midbrain dopaminergic neurons; Science, 260 (1993), pp. 1130–1132
- 18 T. Iwase, C.G. Jung, H. Bae, M. Zhang, B. Soliven; Glial cell line-derived neurotrophic factor-induced signaling in Schwann cells; J Neurochem, 94 (2005), pp. 1488–1499
- 19 P. Huhtala, R.L. Eddy, Y.S. Fan, M.G. Byers, T.B. Shows, K. Tryggvason; Completion of the primary structure of the human type IV collagenase preproenzyme and assignment of the gene (CLG4) to the q21 region of chromosome 16; Genomics, 6 (1990), pp. 554–559
- 20 A. Pryczynicz, K. Guzińska-Ustymowicz, V. Dymicka-Piekarska, J. Czyzewska, A. Kemona; Expression of matrix metalloproteinase 9 in pancreatic ductal carcinoma is associated with tumor metastasis formation; Folia Histochem Cytobiol, 45 (2007), pp. 37–40
- 21 C.A. Whipple, A.L. Young, M. Korc; A Kras(G12D)-driven genetic mouse model of pancreatic cancer requires glypican-1 for efficient proliferation and angiogenesis; Oncogene, 31 (2012), pp. 2535–2544
- 22 J. DiNorcia, M.K. Lee, D.N. Moroziewicz, et al.; RAGE gene deletion inhibits the development and progression of ductal neoplasia and prolongs survival in a murine model of pancreatic cancer; J Gastrointest Surg, 16 (2012), pp. 104–112
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?