Summary
Follicular thyroid carcinoma (FTC) with sternum metastasis is rarely reported. Conservative treatments always result in a poor prognosis. We report two cases of FTC presenting with a large symptomatic solitary metastatic lesion in the sternum. Surgical intervention included total thyroidectomy, combined with wide composite resection of the sternal manubrium, as well as the adjacent clavicular head and ribs. A large defect with exposed pericardium and great vessels was found post resection in both cases. Because the ipsilateral vessels were sacrificed, a contralateral extended pedicled pectoralis major adipofascial flap was designed and transposed to cover the underlying vital organs. The patients received both adjuvant I-131 and radiotherapy postoperatively. The treatment was uneventful, and the patients are well and asymptomatic 5 years after the treatment. Wide composite resection and appropriate adjuvant therapies may offer a survival benefit in patients with advanced FTC with sternum metastasis.
Keywords
follicular thyroid carcinoma;pectoralis major myoadipofascial flap;sternum metastasis
1. Introduction
Well-differentiated thyroid carcinoma with direct invasion or bone metastasis to the sternum is uncommon. Patients with metastatic disease, in general, have a poorer prognosis. However, additional treatments may reduce the burden of tumor for some of these patients and thus offer them a survival or palliative benefit. Treatment modalities for patients with metastatic thyroid cancer include surgical excision, radioactive iodine (RAI) therapy with I-131, external-beam radiotherapy, and recruitment to clinical trials. Large tumors and bone metastases are factors that predict a poor response to RAI therapy.1 Complete surgical resection of isolated symptomatic metastases has been associated with improved survival and should be considered, especially, for patients <45 years old with slowly progressive diseases. For skeletal metastases in particular, surgery is recommended for symptomatic or asymptomatic tumors in weight-bearing extremities. However, metastasis of thyroid carcinoma to the sternum is uncommon and has been reported only rarely. Herein, we present two cases of thyroid follicular carcinoma with metastases to the sternum and demonstrate how surgical intervention, together with appropriate adjuvant therapy, can result in long-term survival.
2. Case reports
2.1. Case 1
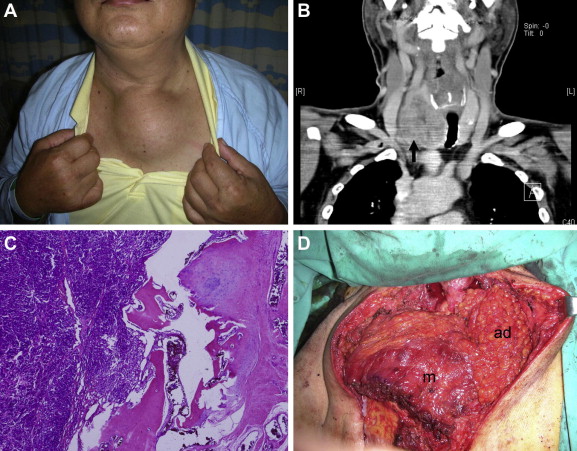
A 56-year-old male patient presented to our center with a painful, progressively enlarging mass over his anterior chest that had been present for the previous 6 months (Fig. 1A). On physical examination, an 8 × 6 cm2 sized mass was noted in the sternal manubrium, involving the left clavicle head. A computed tomography scan revealed the presence of a right thyroid tumor with bone metastases to his sternum as well as the T9 and L2 vertebral bodies (Fig. 1B). There was also a palpable right thyroid nodule. The sternal mass biopsy revealed metastatic follicular carcinoma (Fig. 1C). Total thyroidectomy and a wide composite resection of his sternum, including the bilateral sternoclavicular joint and partial resection of bilateral second and left third ribs, were performed. No surgery was performed for his other bone metastases, as he was asymptomatic. The wide composite resection revealed a large soft-tissue defect with exposed pericardium, great vessels, and a pleural apex. Because of the absence of the pedicle of the ipsilateral pectoralis major (PM) flap after tumor composite ablation, we harvested the extended PM myoadipofascial flap from the contralateral side. This flap included PM muscle (18 × 20 cm2) with adjoining adipofascial tissue (15 × 10 cm2) and was about 18 × 25 cm2 in total size. The flap was used to abolish the dead space next to the pericardium and apex of the left lung (Fig. 1D). A combination of three courses of RAI (I-131) ablation therapy and external-beam radiotherapy was administered postoperatively. The patient recovered uneventfully, and has been well and pain free for the 5 years since surgery.
|
|
|
Figure 1. (A) A 56-year-old male patient presenting with a painful enlarged mass over his upper part of sternum. (B) Computed tomography of head and neck revealed right thyroid tumor with sternum and parasternal tissue metastases. (C) Histological examination illustrated sternal metastases from follicular thyroid carcinoma. (D) After wide composite resection, large sternum and chest wall soft-tissue defect was reconstruction by pectoralis major myoadipofascial flap, 18 × 25 cm2 in size. ad = distal adipofascial tissue; m = pectoralis major muscle. |
2.2. Case 2
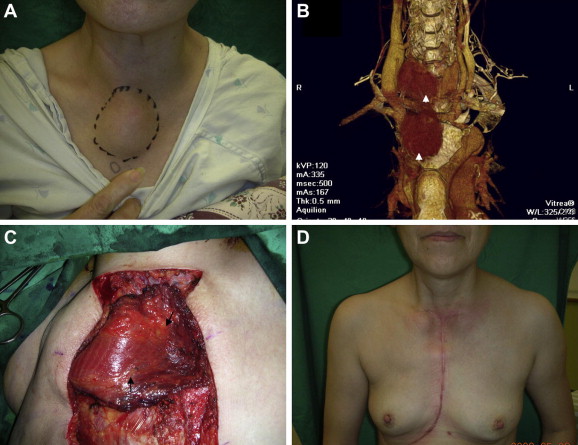
A 55-year-old lady presented to our center with a large painful solitary tumor over the upper part of her sternum, which had been present for 2 months. She also has a history of a thyroid goiter. A physical examination revealed a 4 × 5 cm2 mass located in the sternum and right clavicle head (Fig. 2A). Fine-needle aspiration cytology of the sternal masses revealed metastatic follicular carcinoma. The head and neck computed tomography revealed a 4.3 × 2.5 × 5.5 cm3 tumor in the right thyroid gland and another 5.0 × 4.0 cm2 upper sternal osteolytic mass (Fig. 2B). The patient received a total thyroidectomy and underwent a wide composite resection of the anterior mediastinal tumor as well as of the manubrium, sternum, and bilateral partial first and second ribs. After the wide resection, a large soft-tissue defect exposing the pericardium and the great vessels was found. As the pedicle of the ipsilateral PM flap had already been sacrificed during the composite wide resection, we used a contralateral PM muscle flap (12 × 18 cm2) with adjoining adipofascial flap tissue (10 × 8 cm2), which was about 12 × 22 cm2 in total size, to abolish the dead space and cover the soft-tissue defect adjacent to the pericardium (Fig. 2C). After the operation, the patient received RAI (I-131) therapy and radiotherapy. The aesthetic result was good except for mild breast asymmetry (Fig. 2D). No paradoxical chest wall movement or impaired ventilation was observed. No evidence of cancer recurrence or distant metastasis was detected during the follow-up over the last 5 years.
|
|
|
Figure 2. (A) A 55-year-old lady presenting with a painful solitary mass over the upper part of her sternum. (B) Computed tomography angiogram revealed a 4.3 × 2.5 × 5.5 cm3 tumor in right thyroid gland and another 5 × 4 cm2 upper sternal mass with osteolytic feature (arrowheads). (C) After wide composite resection, a huge soft-tissue defect with pericardium, and great vessel exposure was found. The defect was reconstructed by a pectoralis major myoadipofascial flap 10 × 22 cm2 in size (arrow). (D) Patient showed good results without recurrence postoperatively. |
3. Discussion
Distant metastases are the principal cause of death from papillary and follicular carcinomas. Almost 10% of patients with papillary carcinoma and up to 25% of those with follicular carcinoma develop distant metastases. About 50% of these metastases are present at the time of diagnosis. In managing patients with bone metastases, the key criteria for therapeutic decisions include the following: (1) the presence of or the risk for pathologic fracture, particularly in a weight-bearing structure; (2) the risk of neurologic compromise from vertebral lesions; (3) the presence of pain; (4) the avidity of RAI uptake; and (5) the potential for significant marrow exposure from radiation arising from RAI-avid pelvic metastases. Surgical palliation is recommended for symptomatic bone metastases or asymptomatic tumors in weight-bearing extremities. Other therapeutic options include 131-I treatment (if the whole-body scan is positive), considering dosimetry to maximize dosing and/or external-beam radiotherapy. However, patients with large metastases and bone metastases are unlikely to benefit from RAI treatment.1
Metastasis of thyroid carcinoma to the sternum is rarely reported.2 To date, we found only 10 such cases reported in English when we conducted a search on PubMed. Table 11; 2; 3; 4; 5; 6; 7 ; 8 presents a summary of these cases, including the two patients from our center. Consequences of large sternal metastases include pain, ulceration, and dyspnea. In addition to these morbidities, large sternal metastases have been specifically documented as a cause of immediate death because of the compression of the superior vena cava and circulatory arrest.1 As large metastases and bone metastases are unlikely to benefit from RAI treatment, sternal resection is an important palliative option for patients with large thyroid cancer metastases to the sternum.1 In our series, the patients suffered significant pain from the sternal metastases. To achieve optimal results, total thyroidectomy with a composite resection of the metastatic sternal lesion is warranted. Radical removal of the metastatic sternum, including the adjacent clavicle and ribs, is necessary to obtain clear margins.
| Case no. | Age (y) | Sex | Size (cm) | Histology | Symptom | Other metastases | Year reported | References |
|---|---|---|---|---|---|---|---|---|
| 1. | 75 | F | 14 × 8 × 7 | Poorly Differentiated | Pain | Pulmonary | 2008 | Yanagawa et al1 |
| 2. | 35 | F | 7 × 7 | Poorly Differentiated | Pain | None | 2000 | Mishra et al2 |
| 3. | 43 | M | 7 × 10 | Follicular | None | Pulmonary, vertebral | 2000 | Mishra et al2 |
| 4. | 61 | F | 6 × 5 × 4.5 | Follicular | Pain | None | 2006 | Eroglu et al3 |
| 5. | 69 | F | 8 × 4.5 | Papillary | Pain | None | 2004 | Haraguchi et al4 |
| 6. | 54 | F | 4 × 4 | Follicular | Pain | Pulmonary | 1995 | Ozaki et al5 |
| 7. | 48 | F | 8 6 | Papillary | Pain | None | 1995 | Ozaki et al5 |
| 8. | 59 | F | NR | Follicular | NR | Neck | 2005 | Meyer and Behrend6 |
| 9. | 62 | F | NR | Poorly differentiated | NR | Lymph nodes | 2001 | Kinoglou et al7 |
| 10. | 75 | F | 12 × 9 | Follicular | None | None | 1998 | Muthuphei and Mabua8 |
| 11. | 57 | M | 6 × 7 × 7 | Follicular | Pain | Vertebral | ||
| 12. | 55 | F | 5 × 4 | Follicular | Pain | None |
F = female; M = male; NR = not reported.
Nevertheless, exposed pericardium, great vessels, and existence of a pleural apex after the wide composite resection always pose a challenge. For soft-tissue reconstruction, loco-regional flaps, such as the PM muscle flap, are most commonly used because they provide adequate soft-tissue volume and are easy to harvest. However, in our series, the main pedicle of the ipsilateral PM flap was sacrificed during wide composite resection, and no other local flaps were suitable for reconstruction. The contralateral traditional PM muscle flap could not completely cover the distal part of the pericardium and lung apex. Nevertheless, we designed and used the contralateral PM muscle flap with distal adjoining adipofascial tissue as a myoadipofascial flap to increase the distal flap length and volume for coverage of the pericardium and lung apex. Postoperatively, both patients received adjuvant I-131 therapy and radiotherapy. Since the completing treatment 5 years ago, these patients have remained asymptomatic and well. Moreover, there have been no respiratory complications or chest wall instability related to our reconstruction.
In summary, wide composite resection with appropriate reconstruction for patients with advanced follicular thyroid cancer with sternal metastases can be performed safely and may offer these patients a palliative or survival benefit.
References
- 1 J. Yanagawa, F. Abtin, C.K. Lai, et al.; Resection of thyroid cancer metastases to the sternum; J Thorac Oncol, 4 (2009), pp. 1022–1025
- 2 A. Mishra, S.K. Mishra, A. Agarwal, et al.; Surgical treatment of sternal metastases from thyroid carcinoma: report of two cases; Surg Today, 31 (2001), pp. 799–802
- 3 A. Eroglu, N. Karaoglanglu, H. Bilen, et al.; Follicular thyroid carcinoma: metastasis to the sternum, 13 years after total thyroidectomy; Int J Clin Pract, 60 (2006), pp. 1506–1508
- 4 S. Haraguchi, Y. Yamashita, K. Yamashita, et al.; Sternal resection for metastasis from thyroid carcinoma and reconstruction with the sandwiched Marlex and stainless steel mesh; Jpn J Thorac Cardiovasc Surg, 52 (2004), pp. 209–212
- 5 O. Ozaki, W. Kitagawa, H. Koshiishi, et al.; Thyroid carcinoma metastasized to the sternum: resection of the sternum and reconstruction with acrylic resin; J Surg Oncol, 60 (1995), pp. 282–285
- 6 A. Meyer, M. Behrend; Partial resection of the sternum for osseous metastasis of differentiated thyroid cancer: case report; Anticancer Res, 25 (2005), pp. 4389–4392
- 7 G. Kinoglou, E. Vandeweyer, P. Lothaire, et al.; Thyroid carcinoma metastasis to the sternum: resection and reconstruction; Acta Chir Belg, 101 (2001), pp. 253–255
- 8 M.N. Muthuphei, M.P. Mabua; Retrosternal thyroid carcinoma metastatic to the sternum: a case report; Cent Afr J Med, 44 (1998), pp. 292–293
Document information
Published on 26/05/17
Submitted on 26/05/17
Licence: Other
Share this document
claim authorship
Are you one of the authors of this document?