Abstract
Cochlear implantation is one of the best amongst the various management options available for children and adults with severe to profound sensorineural hearing loss. Inner ear and internal auditory canal (IAC) malformations accounts to approximately 25% of congenital sensorineural hearing loss in children. The primary goal of this report was to evaluate the communication outcomes after cochlear implantation in a child with cystic cochleovestibular anomaly (CCVA). The child was evaluated through various standardized outcome measures at regular intervals to track the progress in terms of auditory and spoken language skills. The scores on Categories of Auditory Perception (CAP), Meaningful Auditory Integration Scale (MAIS), Speech Intelligibility Rating (SIR), Meaningful Use of Speech Scale (MUSS), and listening and spoken language skills showed a significant leap in 12 months duration post implantation. The report thus highlights and correlates the significant progress in auditory and spoken language skills of the child with congenital malformations to appropriate auditory rehabilitation and intensive parental training.
Keywords
Cochlear implants ; Cystic cochleovestibular anomaly ; Inner ear malformation ; Communication outcomes
1. Introduction
Cochlear implant surgery is considered paramount amongst the various rehabilitative choices for various age groups ranging from newborns to adults with severe to profound sensorineural hearing loss (Pakdaman et al., 2011 ). Amongst this group, inner ear and internal auditory canal malformations present a significant challenge even to the most experienced clinicians as they account for approximately 25% of congenital sensorineural hearing loss. Many of these patients have been denied implantation also due to the uncertainty in audiological and communication outcomes post surgery. However, recent researches have reported similar outcomes for children with inner ear malformations in general, mondini dysplasia in specific and those with normal cochlea (Zhou et al., 2014 and Chen et al., 2014 ). Till date, there are many studies reporting the surgical outcomes (Beltrame et al., 2000 , Sennaroglu and Aydin, 2002 and Buchman et al., 2004 ) and a very few reporting the audiological outcomes descriptively (Munro et al., 1996 , Luntz et al., 1997 , Incesulu et al., 2002 and Bauer et al., 2002 ). Although there are many researches reporting the outcomes in general for those with inner ear malformations, there are not any reported till date on cystic cochleovestibular anomaly per se. Herein we are reporting the audiological and communication outcomes following cochlear implantation in one such child with cystic cochleovestibular anomaly (CCVA) in the implanted ear and cochlear aplasia in the other ear, based on various standardized measures.
2. Case report
A four and half year old female child reported with the complaint of delayed speech and language secondary to hearing loss. Baseline assessment with audiological test battery revealed bilateral profound hearing loss on pure tone audiometry, bilateral type A tympanogram on impedance measurement and absent otoacoustic emissions. Findings were correlated with electrophysiological assessment using Auditory Brainstem Response (ABR), which also revealed bilateral profound hearing loss. Radiographic investigations included Magnetic Resonance Imaging and Computerized Tomography. Their findings revealed cystic cochleovestibular anomaly, which is an Incomplete Partition type I (IP-I) in left ear and cochlear aplasia in the right ear. CCVA is defined as a malformation in which the cochlea lacks the entire modiolus and cribriform area, resulting in a cystic appearance, and an accompanying large cystic vestibule. The left ear with CCVA was implanted at the age of 5 years 4 months. The surgical report showed partial insertion with nine electrodes. This child underwent regular speech therapy for around 14 months post implantation with regular mapping. A longitudinal single case study was carried out on this child in order to report the progress made by this child at regular intervals during post implantation. Auditory verbal therapy and structured auditory training were the major treatment strategies employed by the clinician during the therapy sessions and the mother was instructed to train the child with the same target goals during home training. All the assessment tools were administered in a clinical setup by a qualified speech language pathologist with more than ten years of clinical and research experience. A written informed consent was obtained from the parent prior to testing.
The child was evaluated through various standardized outcome measures at 3, 6 and 12 months to track the progress in terms of auditory and spoken language skills. The standardized measures used to track the progress include Categories of Auditory Performance II (CAP), Meaningful Use of Speech Scale (MUSS), Speech Intelligibility Rating (SIR), Meaningful Auditory Integration Scale (MAIS), and other measures assessed were listening and spoken language skills, integration into mainstream school system. CAP II measures the speech perception performance of implanted children, with their scores reflecting everyday auditory performance in a more realistic way. It is a hierarchical scale of auditory perception ranging from 0 for “no awareness of environmental sounds” to 9 for “Use of phone with unknown speaker in unpredictable context”. MAIS is a structured parental questionnaire comprising ten questions assessing three different domains, viz, confidence level of child in using the processor, awareness to different sound stimuli and childs perception and identification of various sounds. Overall, the questionnaire aims to evaluate the functional abilities of a prelingual child after aiding them with hearing aids or cochlear implants from parental view point. MUSS is also a ten item questionnaire, which focuses on assessing the childs potential in using speech meaningfully. This questionnaire is again from the parental perspective. This consists of three subsections, amongst which, questions 1 to 3 assesses the ability of childs effective control on voice, questions 4 to 8 verifies the childs ability to use spontaneous speech and rest of them explores the childs capability in changing various communication strategies contextually. In totem, MAIS and MUSS are validation instruments to track the progress in oral aural skills during the post intervention period for children with hearing impairment. SIR is a tool to evaluate speech intelligibility of children with scores ranging from 1 to 5, quantifying their everyday spontaneous speech. SIR comprises five performance categories ranging from “pre recognizable words in spoken language” to “connected speech is intelligible to all listeners”.
3. Results and discussion
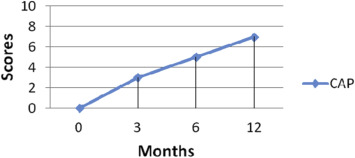
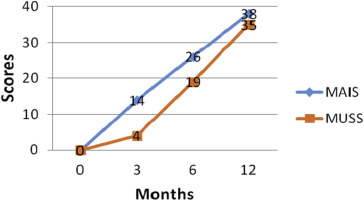
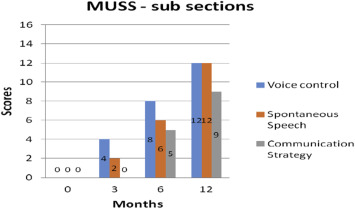
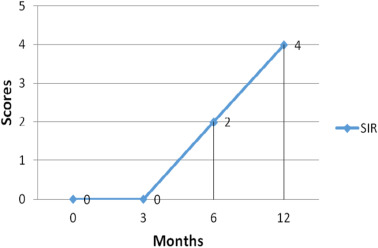
The child was assessed with various standardized measures mentioned above at regular intervals and results are summarized in this section. The baseline assessment was done immediately after switch on and this is depicted as ‘0’ months. The child achieved a score of 7 (Use of phone with familiar speaker) for a maximum score of 9 on Categories of Auditory Performance II by 12 months of post implantation as seen from Fig. 1 . MAIS scores progressed from 0 to 38 and MUSS scores moved to 35 from baseline score of 0 as evident from Fig. 2 . The MAIS and MUSS questionnaires have a maximum score of 40 and these tools enable us to assess the progress in childrens early auditory perception skills and their correlation to speech production skills relative to perception. The results reveal a proportional raise in MAIS and MUSS scores. This parallel progress in scores is suggestive of the childs ability to use spontaneous speech and different communication strategies relative to the auditory perception skills. MUSS comprised of 3 subsections, viz, the voice control, use of spontaneous speech and communication strategy, which is clearly shown in Fig. 3 . The scores for voice control and spontaneous speech ranged from 0 at baseline to 12 by 1 year post implantation, while the scores progressed from 0 to 9 for use of communication strategy. These scores reveal that the progressive control in terms of voice and use of spontaneous speech precedes the use of various communication strategies. The parallel growth in MAIS and MUSS scores suggest that the better the perception of auditory information through implants, the higher the progress in terms of speech production skills (Umat et al., 2010 ). The scores on voice control shows that a childs effective listening, and control of their own voice follows a quality auditory feedback offered by their implants. This enables them to use spontaneous speech for communication although intelligibility can be expected to improve a little later. The SIR scores progressed from 2 to 4 for a maximum score of 5 by 6–12 months (See Fig. 4 ). The aided audiogram had thresholds within the speech spectrum at the speech frequencies, 0.5, 1, 2 and 4 KHz, by 9–12 months post implantation. The child was able to use simple 3 words phrases for spontaneous interaction. The child was integrated in to a mainstream school system after 5 months of intervention, wherein she attains ‘A’ to ‘A+ ’ grades in both curricular and co-curricular activities.
|
|
|
Fig. 1. Scores on Categories of Auditory Performance (CAP) at regular intervals post implantation. |
|
|
|
Fig. 2. Progress in MAIS and MUSS scores at regular intervals post implantation. |
|
|
|
Fig. 3. Scores obtained in various subsections of MUSS. |
|
|
|
Fig. 4. Scores obtained on Speech Intelligibility Rating (SIR) at regular intervals post implantation. |
Research in the past reveals that active parental involvement in childrens progress, i.e, vigorous home training was directly related to increase in phonological awareness and vocabulary (Foy and Mann, 2003 ). Parents' involvement in terms of intensive speech and language stimulation through auditory modality predominantly in the post implantation period has been documented as a significant feature in enhancing auditory perception in an implanted or aided child (DesJardin and Eisenberg, 2007 ). There is always a positive correlation reported in relationship between mothers linguistic input and childs progress in receptive and expressive language skills (Umat et al., 2010 ). The results of the study by Umat et al. (2010) partially supported the above-mentioned studies stating that amount of quality time spent by parents outside the clinical sessions had a significant correlation with MAIS scores during post intervention assessment. MUSS scores also showed a similar trend, however, the parental input did not show a significant correlation with MUSS scores in their study. The current report also goes to prove that acquisition of speech and language skills after cochlear implantation is promising even in children with congenital cochlear anomalies. Although the cochlear implantation was performed above 5 years of chronological age of the child, with partial insertion and limited number of electrodes, the significant progress in auditory, speech and language skills can be correlated to appropriate auditory rehabilitation and intensive parental training. This showcases the importance of these factors, which play a vital role for the development of auditory and spoken language skills, not only in challenging cases but also for every child undergoing implantation irrespective of the anomalies involved. When the performance of this child was compared to other implanted children with radiologically normal inner ears, this child was a star performer as her performance was at par or most of the times ahead of those children. This childs video performance was in fact used as a motivating factor during counseling for other prospective parents considering cochlear implantation and for those with poor home training. As there was only one child with CCVA and the rest were radiologically normal ears in the authors clinic, a comparison was not possible objectively and hence this paper reports the significant outcomes of a single child. These findings further emphasizes on the importance of professionals' involvement in counseling and working with the parents and immediate members of the family, very intimately thereby augmenting their participation in post implantation therapy to facilitate speech, language and listening skills in very young children undergoing implantation.
4. Conclusion
This report supports the existing evidences that cochlear implant significantly improves the auditory and spoken language skills in severe to profound hearing loss children. In addition the current report stresses on the significant progress shown by a child with cystic cochleovestibular anomaly in one ear and cochlear aplasia in the other ear, wherein only a partial insertion with limited number of electrodes has brought about the drastic progress in auditory, speech and language skills. The better the auditory integration, the higher the communicative intent and use of spontaneous speech, which is evident from the parallel growth of MAIS and MUSS scores. These positive aspects can be well correlated to the intensive parental training at home beyond the clinical sessions in an auditory verbal mode.
References
- Bauer et al., 2002 P.W. Bauer, F.J. Wippold, J. Goldin, R.P. Lusk; Cochlear implantation in children with CHARGE association; Arch. Otolaryngol. Head Neck Surg., 128 (2002), pp. 1013–1017
- Beltrame et al., 2000 M.A. Beltrame, Bonfioloi, G.N. Frau; Cochlear implant in inner ear malformation; Adv. Otorhinolaryngol., 57 (2000), pp. 113–119
- Buchman et al., 2004 C.A. Buchman, B.J. Copeland, C.J. Brown, V.N. Carrasco, H.C. Pillsbury; Cochlear implantation in children with congenital inner ear malformations; Laryngoscope, 114 (2004), pp. 309–316
- Chen et al., 2014 X. Chen, F. Yan, B. Liu, S. Liu, Y. Kong, J. Zheng, Y. Li, S. Gong, D. Han, L. Zhang; The development of auditory skills in young children with Mondini dysplasia after cochlear implantation; PLoS One, 9 (9) (2014), pp. 3–17
- DesJardin and Eisenberg, 2007 J.L. DesJardin, L.S. Eisenberg; Maternal contributions: supporting language development in young children with cochlear implants; Ear Hear., 28 (2007), pp. 456–469
- Foy and Mann, 2003 J.G. Foy, V. Mann; Home literacy environment and phonological awareness in preschool children: differential effects for rhyme and phoneme awareness; Appl. Psycholinguist., 24 (2003), pp. 59–88
- Incesulu et al., 2002 A. Incesulu, M. Vural, U. Erkam, S. Kocaturk; Cochlear implantation in children with inner ear malformations; Int. J. Pediatr. Otorhinolaryngol. (2002), pp. 171–179
- Luntz et al., 1997 M. Luntz, T. Balkany, A.V. Hodges, F.F. Telischi; Cochlear implants in children with congenital inner ear malformations; Arch. Otolaryngol. Head Neck Surg., 123 (1997), pp. 974–977
- Munro et al., 1996 K.J. Munro, C.R. George, N.P. Haacke; Audiological findings after multichannel cochlear implantation in patients with Mondini dysplasia; Br. J. Audiol., 30 (1996), pp. 369–379
- Pakdaman et al., 2011 M.N. Pakdaman, B.S. Herrmann, H.D. Curtin, J.V. Beek-King, D.J. Lee; Cochlear implantation in children with anomalous cochleovestibular anatomy: a systematic review; Otolaryngol. Head Neck Surg., 146 (2) (2011), pp. 180–190
- Sennaroglu and Aydin, 2002 L. Sennaroglu, E. Aydin; Anteroposterior approach with split ear canal for cochlear implantation in severe malformations; Otol. Neurotol., 23 (2002), pp. 39–43
- Umat et al., 2010 C. Umat, K.S. Hufaidah, A.R. Azlizawati; Auditory functionality and early use of speech in a group of pediatric cochlear implant users; Med. J. Malays., 65 (1) (2010), pp. 7–13
- Zhou et al., 2014 H. Zhou, X. Sun, Z. Chen, H. Shi, Y. Wu, W. Zhang, S. Yin; Evaluation of cochlear implantation in children with inner ear malformation; B-ENT, 10 (4) (2014), pp. 265–269
Document information
Published on 10/10/16
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?