Abstract
Background
Several guidelines, including the Japanese Pediatric Guideline for the Treatment and Management of Asthma (JPGL), recommend salmeterol/fluticasone combination therapy (SFC) as step 3 to 4 treatment for moderate to severe asthma. However, the optimal step-down approach to SFC remains unclear. In the current study, we examined step-down approaches in asthmatic children whose symptoms had been stabilized by SFC 100/200 μg/day.
Methods
This randomized, multicenter, open-label, parallel-group study was conducted over 12 weeks. For step-down therapy, subjects aged 5–15 years were randomly assigned to an SFC group (25/50 μg b.i.d.) or an FP group (100 μg b.i.d.), and treated for 12 weeks. Childhood Asthma Control Test (C-ACT) scores, lung function, and exhaled nitric oxide (FeNO) levels were monitored.
Results
Of 131 enrolled subjects, 128 completed the study and were included in the analysis. Decreases in % peak expiratory flow rate and % forced expiratory flow at 50% of vital capacity (V50) were observed in the FP group at each time point. There was a significant difference between the two groups for the change in %V50 from its previous value at each time point. There were no significant changes in FeNO levels (range 15–20 ppb) or C-ACT scores (∼26 points) within or between groups.
Conclusions
A high level of asthma control was maintained with both approaches. The use of SFC step-down resulted in somewhat better respiratory function, with no worsening of airway inflammation. However, halving the dose of SFC and switching to FP alone are both optimal step-down approaches.
Graphical abstract
Keywords
Fluticasone propionate; Moderate to severe asthma; Pediatric asthma; Salmeterol/fluticasone combination therapy; Step-down approach
Abbreviations
ICS, inhaled corticosteroids; SFC, salmeterol/fluticasone combination therapy; FP, fluticasone propionate; FeNO, exhaled nitric oxide
Introduction
The 2008 and 2012 editions of the Japanese Pediatric Guideline for the Treatment and Management of Asthma (JPGL) recommend salmeterol/fluticasone combination therapy (SFC) as step 3 to 4 treatment to control moderate or more severe asthma in children aged 5–15 years.1 The JPGL recommends an SFC dose based on fluticasone 100–200 μg/day (salmeterol/fluticasone 50/100–100/200 μg/day; hereafter, the SFC dose is reported as the fluticasone dose only) for step 3 therapy and 200 μg/day for step 4 therapy. A 2012 report from the Global Initiative for Asthma similarly recommends SFC as a step 3 or 4 therapy.2
Once effective asthma control is achieved with inhaled corticosteroids (ICS), treatment needs to be stepped down to maintain asthma control with the minimum necessary dose. However, the optimal step-down approach following control achieved with SFC remains unclear. In adult asthma patients controlled with SFC 500 μg/day, treatment can be effectively stepped down by changing to SFC 200 μg/day rather than changing to an equivalent dose of ICS [i.e., stopping the long-acting β2 agonist (LABA)].3 Furthermore, previous research has indicated that the anti-asthma effect of fluticasone propionate (FP) 100 μg/day in combination with salmeterol (SFC) is equivalent to treatment with FP 200 μg/day alone.4
Once childhood asthma is stable for 3 months, the JPGL suggests stepping down treatment by stopping the β2 agonist. Therefore, the JPGL recommends a change from SFC to FP alone. This approach might be based in part on the findings of the SMART trial,5 which suggested that long-term use of salmeterol without an ICS could potentially cause increased airway inflammation and consequent worsening of asthma symptoms. In fact, another study found that while asthma control with FP 200 μg/day was superior to SFC 100 μg/day in children, the reverse held true in adults.6 However, there is limited clinical evidence to support the superiority of ICS alone over SFC in pediatric asthma patients.
In the current study, we investigated the optimal step-down approach in asthmatic children whose symptoms had been stabilized with SFC 200 μg/day. We compared changes in respiratory function and extent of airway inflammation between two step-down approaches, halving the dose of SFC to 100 μg/day or switching to monotherapy with FP 200 μg/day.
Methods
Subjects
This study was conducted at 14 hospitals/clinics in Japan, between October 2010 and March 2013. Subjects were patients who met all of the following inclusion criteria: pediatric asthma patients aged 5–15 years at the start of the study and who had been seen regularly for at least 6 months prior to entering the study; had symptoms stabilized with SFC ≥200 μg/day for at least 12 weeks prior to the start of the study, had a level of asthma control of ≥25 points on the Childhood Asthma Control Test (C-ACT) at the end of the run-in period, had peak expiratory flow (PEF) ≥80% of the predicted value at the end of the run-in period, or were able to undergo spirometry and measurement of exhaled nitric oxide. All subjects were required to stop taking leukotriene receptor antagonists and other controllers before enrollment and allowed using short-acting β2-agonists (SABA) and systemic corticosteroid as reliever medication throughout this study.
Study design
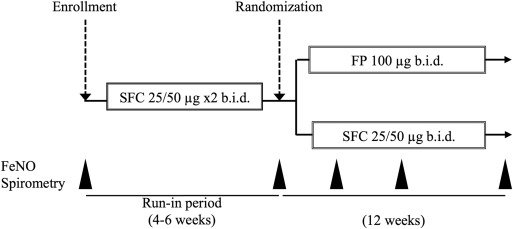
This study was a randomized, multicenter, open-label, parallel-group study. A summary of the study design and the CONSORT flow diagram are shown in Fig. 1 and Fig. 2, respectively. After enrollment, all subjects were administered SFC in two puffs (25/50 μg/puff) b.i.d. via a pressurized metered dose inhaler and with a spacer device during a run-in period of 4–6 weeks. After the run-in period, subjects were randomly assigned to an SFC group (25/50 μg b.i.d.) or an FP group (100 μg b.i.d.). Randomization was performed at the central data center by using a block randomization with a block size of four. After random allocation, subjects were treated continuously for 12 weeks. Subjects were seen every 4 weeks, their asthma diary was checked, and an examination was performed. The subjects C-ACT score was recorded by caregivers and respiratory function was measured using an Autospiro spirometer (Minato Medical, Osaka, Japan). Exhaled nitric oxide (FeNO) was measured with a NIOX MINO device (Aerocrine; Solna, Sweden) every 4 weeks. We didn't require the subjects to stop medicines before the lung function test and the FeNO measuring.
|
|
|
Fig. 1. Study design. |
|
|
|
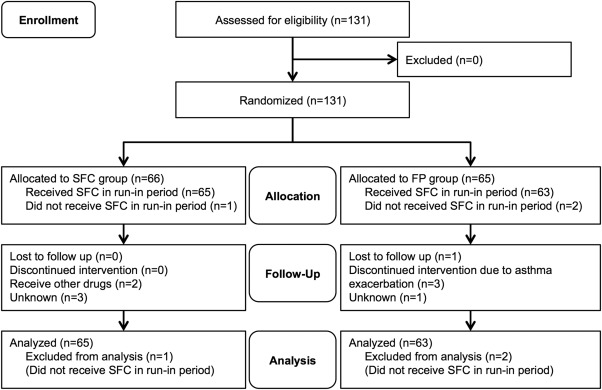
Fig. 2. CONSORT flow diagram. Consort flow diagram for the Optimal step-down approach for pediatric asthma controlled by salmeterol/fluticasone (OSCAR study). A hundred thirty-one patients provided informed consent, of whom 3 patients didn't receive SFC in run-in period. 10 patients dropped out of this study because asthma exacerbation (3 of FP group), other controller use (2 of SFC group), lost to follow-up (1 of FP group) and decision by physician (unknown reason) (3 of SFC group and 1 of FP group). The modified intention-to-treat analysis was performed in 128 of the 131 subjects who received SFC in run-in period. |
Endpoints
The primary endpoint for this study was the extent of changes in the % predicted PEF rate (%PEFR). Secondary endpoints were the extent of changes in respiratory function, FeNO levels, and the C-ACT score.
Statistical analysis
The rationale for the sample size was a difference in PEF of 7.6 L/min for two groups in a previous study.4 The standard deviation was set at 26.0 L/min. Patient allocation was 1:1, and the α error was 0.05. Statistically calculating the required sample size with a power of 0.8 resulted in a sample size of 65 patients in each group. A one-sample t-test was used to compare changes from previous values at individual measurement points for each group. A two-sample t-test was used to compare the two groups in terms of measurements and the extent of changes. All statistical analysis was performed using SAS version 9.2 software (SAS Institute Inc., Cary, NC, USA).
Ethics
The study protocol was approved by Institutional Review Boards of Jikei University School of Medicine (21-189 [6067]). During enrollment, all patients provided informed consent, and written informed consent was obtained from parents of guardians. The study was conducted in accordance with the principles embodied in the Declaration of Helsinki of 1965. This study was registered as a clinical trial on November 2, 2010 (UMIN000004498).
Results
Of the 131 study subjects, three had not been using SFC regularly prior to enrollment. These three patients were excluded from statistical analysis, resulting in 128 subjects comprising the full analysis set. Baseline characteristics are shown in Table 1. There were no significant differences between the two groups for age, sex, asthma severity, respiratory function, or FeNO levels.
| SFC (n = 65) | FP (n = 63) | |
|---|---|---|
| Age (year) | 9.6 ± 2.0 | 10.0 ± 2.2 |
| Gender (M/F) | 46/19 | 41/22 |
| Height (cm) | 134.1 ± 11.9 | 137.1 ± 13.7 |
| Weight (kg) | 32.2 ± 9.6 | 34.3 ± 10.7 |
| Sensitization for HDM† (%) | 83.1% | 82.5% |
| Comorbidity (AR‡) (%) | 70.8% | 79.4% |
| PEFR (L/s) | 3.9 ± 0.99 | 4.2 ± 1.2 |
| C-ACT§ | 26.1 ± 1.3 | 26.2 ± 0.8 |
| FeNO (ppb) | 23.3 ± 22.8 | 18.0 ± 13.3 |
Results presented in mean ± s.d. or percentage unless stated otherwise.
†. House Dust Mite: Der f1/f2 or Der p1/p2 antigen-specific IgE concentrations of more than 0.69 UA/mL were defined as ‘sensitization’.
‡. Allergic Rhinitis: diagnosed by physician.
§. Childhood Asthma Control Test.
Lung function
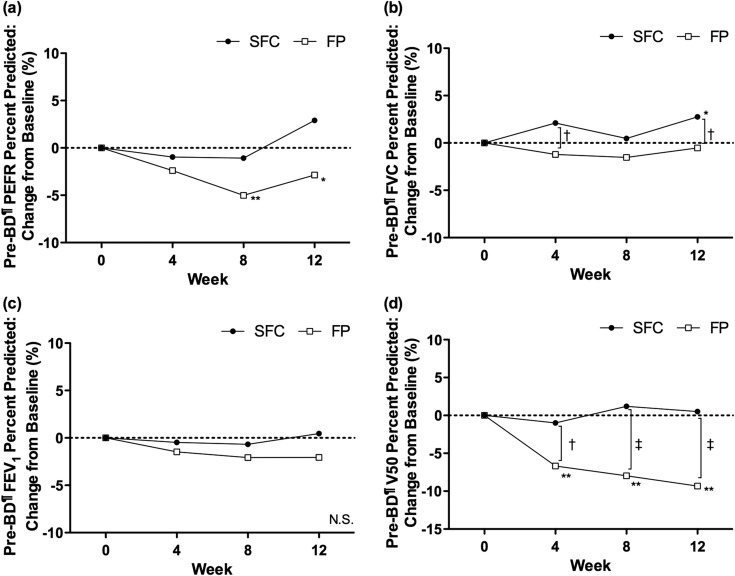
Changes in respiratory function over the study period and results of inter-group comparisons are shown in Figure 3. The FP group had a higher mean value for every parameter prior to the step-down, although the differences between the two groups were not significant at visit 2 (baseline). In the FP group there were significant decreases in the %PEFR and the % predicted forced expiratory flow at 50% of vital capacity (%V50) from previous values at each time point. There was a significant difference between the two groups for the extent of the change in %V50 from its previous value at each time point.
|
|
|
Fig. 3. Changes in respiratory function. A significant decrease in the %PEFR (a) and the %V50 (d) from their previous values was shown at each time point in the FP group. Significant differences between the groups were recognized in terms of the extent of the change in %V50 (d) from its previous value at each time point. ∗p < 0.05, compared to baseline (visit 2, week 0), paired t-test. ∗∗p < 0.01, compared to baseline (visit 2, week 0), paired t-test. †p < 0.05, SFC vs FP, t-test. ‡p < 0.01, SFC vs FP, t-test. |
FeNO
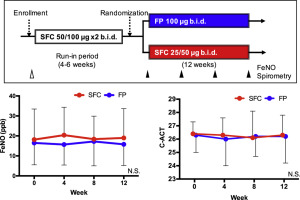
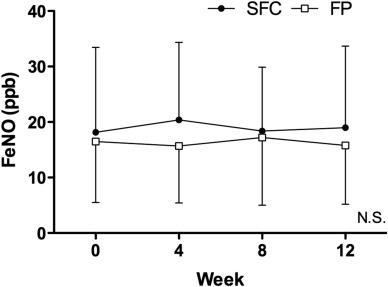
As shown in Figure 4, there were no significant changes in FeNO levels (range 15–20 ppb) in either group during the study and no significant difference between the two groups.
|
|
|
Fig. 4. Changes in FeNO. Significant changes in FeNO levels were not recognized for both 2 groups. Levels ranged from 15 to 20 ppb. |
C-ACT score
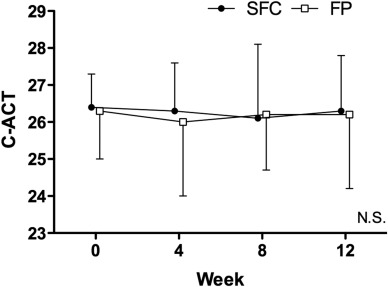
As shown in Figure 5, there were no significant changes in the C-ACT score (∼26) in either group during the study and no significant difference between the two groups.
|
|
|
Fig. 5. Changes in C-ACT. Significant changes in the C-ACT score were not recognized for bothgroup. The score remained around 26 points. |
Adverse events
Two patients in the FP group suffered acute bronchitis during the study period. There were no serious events requiring hospitalization.
Discussion
The current study examined optimal approaches to stepping down treatment in asthmatic children whose symptoms had been stabilized by SFC 200 μg/day. Changes in respiratory function and the extent of airway inflammation were compared between two groups managed with different step-down approaches, halving the dose of SFC (50/25 μg b.i.d.) or switching to FP monotherapy (100 μg b.i.d.). The current results revealed significant decreases in the %PEFR, an indicator of large airway function, and the %V50, an indicator of small airway function, from previous values at each time point in the FP group. In contrast, there were no changes in those indicators in the SFC group with significant differences between the two groups in terms of the extent of the change in %V50 from its previous value at each time point. There are three possible mechanisms to explain this finding. The first is the stimulation of β2 receptors by SFC because the salmeterol component of SFC continued to cause bronchodilation.7 and 8 The second mechanism may be relapsing airway inflammation after step-down in the FP group. However, because FeNO levels did not increase and C-ACT scores did not decrease, this possibility can be ruled out. The third mechanism relates to the finding that the FP group had a higher mean value than the SFC group for every parameter prior to the step-down, although the differences between the two groups were not significant. The possibility that higher values gave way to normal levels cannot be ruled out. However, values for the FP group were the same at visit 1 and visit 2. Switching from SFC to FP is likely to cause some change in stable respiratory function.
There were no significant changes in FeNO levels within or between the SFC and FP groups. Sorkness et al.6 compared the long-term (48 weeks) control of mild to moderate persistent asthma in children aged 6–14 years treated with one of three regimens: montelukast (5 mg/day); FP (200 μg/day); or SFC (100/100 μg/day). The authors reported a significant increase in forced expiratory volume in 1 s (FEV1)/forced vital capacity (FVC) and a significant decrease in FeNO levels in patients given FP. FEV1/FVC also increased in patients given SFC; however, the extent of that increase was significantly lesser than that in patients given FP. The authors also noted a significant decrease in FeNO levels; however, the patients given SFC had a significantly smaller percent change compared with patients given FP.6 Based on these findings, the authors concluded that FP 200 μg/day was superior to SFC 100 μg/day for the long-term control of mild to moderate persistent asthma in children. There are several reasons to explain why those results appear to conflict with the current findings. The first relates to differences in the study subjects. Sorkness et al.6 studied children with unstable asthma symptoms, whereas the children enrolled in the current study had been stabilized by SFC. In other words, the current study examined children with sufficiently reduced airway inflammation. This could mean that a relapse in airway inflammation that was already well controlled was not noted even when the SFC dose was halved or the patient was switched to an equivalent dose of FP. The second reason relates to the method of administration of SFC. In the current study, SFC 50/25 μg was administered twice daily whereas Sorkness et al.6 administered SFC in a double dummy fashion (SFC 100/50 μg in the morning and salmeterol 50 μg in the evening). Therefore, in the previous study, SFC in the morning treated inflammation while therapy in the evening was an LABA (bronchodilator) alone. Long-term use of an LABA alone is reported to exacerbate airway inflammation. 9 and 10 Therefore, SFC in the study by Sorkness et al.6 may have had weaker anti-inflammatory action than FP.
There were no significant differences in the C-ACT score within or between the two groups. A high level of control was maintained over 12 weeks in both the SFC group and the FP group. As mentioned earlier, slight differences between the two groups were recognized in terms of changes in respiratory function; however, there were no differences in asthmatic symptoms as indicated by C-ACT scores. Moreover, the C-ACT score remained high throughout the 12 weeks of step-down. These findings indicate that halving the dose of SFC and switching to FP may both be optimal step-down approaches to asthma therapy in practice.
There are three limitations to the current study that warrant mention. First, the study was an open trial. The intervention and assessment were not blinded, so bias may have affected the assessment. Respiratory function and FeNO levels were the primary endpoints of the study; however, there are limits to the extent by which these parameters can be affected. The effects of bias on FeNO levels can probably be ignored because the subjects were allocated randomly. In addition, both groups had consistently high C-ACT scores; hence, there is no need to overestimate the effects of bias. The second limitation is that medication was not stopped before the respiratory function tests. Nevertheless, the guidelines on the Standardization of Spirometry from the American Thoracic Society makes no specific mention of stopping medication prior to testing.11 When the current study was devised, the decision was made to not stop medication in light of the feasibility of study. As a result, the data on respiratory function from the current study may reflect residual effects of salmeterol, particularly in the SFC group. However, the effect on FeNO or C-ACT can be ignored. The third limitation concerns the C-ACT. The C-ACT with a maximum score of 27 points, is intended for children aged 4–11 years.12 The adult version of the test, the Asthma Control Test (ACT), with a maximum score of 25 points, should be used for children aged 12 years and older.13 However, in the current study, the C-ACT was used for children aged 12–15 years because differing scores would complicate the analysis, particularly of children who turned 12 during the study.
In summary, we compared two step-down approaches in asthmatic children whose symptoms had been stabilized by SFC 200 μg/day, halving the dose of SFC and switching to FP monotherapy. Both approaches resulted in excellent control of asthmatic symptoms (as indicated by the C-ACT score) for 12 weeks. When the approaches were assessed based on changes in respiratory function, halving the dose of SFC proved slightly better. Furthermore, there was no worsening of airway inflammation following step down to half the dose of SFC. Our findings suggest that halving the dose of SFC and switching to FP alone are both optimal step-down approaches.
Conflict of interest
YA received lecture fees from GlaxoSmithKline, MSD. TF received lecture fees from GlaxoSmithKline, MSD, and research grants from Kaketsuken, Pfizer. TKa received research grants from GlaxoSmithKline, Boehringer Ingelheim, Ono Pharmaceutical, Sanofi, MSD. The rest of the authors have no conflict of interest.
Authors' contributions
KA collected data, analyzed and wrote the manuscript; HMe managed data collection; YT, JA, RT, YK, TKi, HMu, MT, KS, SS and HN collected data; MF and KM monitored data and safety; HA and YA designed the study; SY and TF designed the study and collected data; TKa designed the study, collected data and finalized the manuscript.
Acknowledgments
The authors wish to thank Kazuki Sato, Kouji Hashimoto, Hiroyasu Okahata, and Rieko Masuda for collecting the data, and Mitsuyoshi Urashima for data management.
This work was partly supported by unrestricted grants, which TKa received from GlaxoSmithKline, Boehringer Ingelheim, Ono Pharmaceutical, Sanofi-Aventis and MSD.
References
- 1 Y. Hamasaki, Y. Kohno, M. Ebisawa, N. Kondo, S. Nishima, T. Nishimuta, et al.; Japanese guideline for childhood asthma 2014; Allergol Int, 63 (2014), pp. 335–356
- 2 Global Initiative for Asthma (GINA). Global Strategy for Asthma Management and Prevention. Updated 2014. Available at: http://www.ginasthma.org. [accessed 13.09.14].
- 3 E.D. Bateman, L. Jacques, C. Goldfrad, T. Atienza, T. Mihaescu, M. Duggan; Asthma control can be maintained when fluticasone propionate/salmeterol in a single inhaler is stepped down; J Allergy Clin Immunol, 117 (2006), pp. 563–570
- 4 American Lung Association Asthma Clinical Research Centers, S.P. Peters, N. Anthonisen, M. Castro, J.T. Holbrook, C.G. Irvin, et al.; Randomized comparison of strategies for reducing treatment in mild persistent asthma; N Engl J Med, 356 (2007), pp. 2027–2039
- 5 H.S. Nelson, S.T. Weiss, E.K. Bleecker, S.W. Yancey, P.M. Dorinsky, SMART Study Group; The salmeterol multicenter asthma research trial: a comparison of usual pharmacotherapy for asthma or usual pharmacotherapy plus salmeterol; Chest, 129 (2006), pp. 15–16
- 6 C.A. Sorkness, R.F. Lemanske, D.T. Mauger, S.J. Boehmer, V.M. Chinchilli, F.D. Martinez, et al.; Long-term comparison of 3 controller regimens for mild-moderate persistent childhood asthma: the Pediatric Asthma Controller Trial; J Allergy Clin Immunol, 119 (2007), pp. 64–72
- 7 M. Johnson; Salmeterol: a novel drug for the treatment of asthma; Agents Actions Suppl, 34 (1991), pp. 79–95
- 8 F.E. Simons, N.R. Soni, W.T. Watson, A.B. Becker; Bronchodilator and bronchoprotective effects of salmeterol in young patients with asthma; J Allergy Clin Immunol, 90 (1992), pp. 840–846
- 9 S.C. Lazarus, H.A. Boushey, J.V. Fahy, V.M. Chinchilli, R.F. Lemanske Jr., C.A. Sorkness, et al.; Long-acting beta2-agonist monotherapy vs continued therapy with inhaled corticosteroids in patients with persistent asthma: a randomized controlled trial; JAMA, 285 (2001), pp. 2583–2593
- 10 R.A. McIvor, E. Pizzichini, M.O. Turner, P. Hussack, F.E. Hargreave, M.R. Sears; Potential masking effects of salmeterol on airway inflammation in asthma; Am J Respir Crit Care Med, 158 (1998), pp. 924–930
- 11 Standardization of Spirometry, 1994 Update. American Thoracic Society; Am J Respir Crit Care Med, 152 (1995), pp. 1107–1136
- 12 A.H. Liu, R. Zeiger, C. Sorkness, T. Mahr, N. Ostrom, S. Burgess, et al.; Development and cross-sectional validation of the Childhood Asthma Control Test; J Allergy Clin Immunol, 119 (2007), pp. 817–825
- 13 R.A. Nathan, C.A. Sorkness, M. Kosinski, M. Schatz, J.T. Li, P. Marcus, et al.; Development of the Asthma Control Test: a survey for assessing asthma control; J Allergy Clin Immunol, 113 (2004), pp. 59–65
Document information
Published on 05/04/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?