Highlights
- Naturally occurring HIV-1capsid variants confer HIV-1 resistance to MxB.
- MxB-resistant capsid A116 is a major variant in HIV-1 Subtype C.
- HIV-1 capsid variant A116 is accumulating during expansion of the HIV-1 epidemic in China.
- MxB-resistant HIV-1 capsid variants maintain interaction with MxB.
Interferon (IFN) is a key component of the innate immune response to exogenous pathogens. Human MxB has been identified as a potent inhibitor of HIV-1 induced by interferon. How HIV-1 escapes from MxB inhibition is not clear. This study demonstrates that capsid variations detected in primary HIV-1 isolates can mediate MxB resistance. MxB resistant capsid mutations can accumulate during HIV-1 transmission and are mostly enriched in Clade C HIV-1 that is the most rapidly expanding Clade throughout the world. Identification of the critical role of these capsid mutations in overcoming a host restriction factor may provide opportunities for the development of therapeutic interventions.
Abstract
Recent studies have identified human myxovirus resistance protein 2 (MxB or Mx2) as an interferon induced inhibitor of HIV-1 replication. However, whether HIV-1 can overcome MxB restriction without compromise of viral fitness has been undefined. Here, we have discovered that naturally occurring capsid (CA) variants can render HIV-1 resistant to the activity of MxB without losing viral infectivity or the ability to escape from interferon induction. Moreover, these MxB resistant HIV-1 variants do not lose MxB recognition. Surprisingly, MxB resistant CA variants are most commonly found in the Clade C HIV-1 that is the most rapidly expanding Clade throughout the world. Accumulation of MxB resistant mutations is also observed during HIV-1 spreading in human populations. These findings support a potential role for MxB as a selective force during HIV-1 transmission and evolution.
Keywords
MxB ; HIV-1 ; Capsid variants ; Positive selection
1. Introduction
Human immunodeficiency virus (HIV), the cause of acquired immunodeficiency syndrome (AIDS), has been a major global public health issue for decades. Approximately 35.0 million people were infected with HIV at the end of 2013 globally (http://www.who.int/mediacentre/factsheets/fs360/en/ ). Although aggressive treatment regimens using highly active antiretroviral therapy (HAART) is successful in suppressing HIV viral replication and the progression of HIV disease, the persistence of virus within latently infected cells enables viral rebound to occur once antiretroviral treatment is terminated (Chun et al., 1995 ). The association of many of the currently available antiretroviral agents with adverse side-effects dictates the need for continuing efforts to identify other antiretroviral targets and therapies.
Interferon (IFN), a key component of human innate immunity against invading pathogens acts by inducing expression of hundreds of IFN-stimulated genes (ISGs). Several HIV-1 restriction factors such as APOBEC3G, BST-2 and SAMHD1 can be stimulated by IFN (Malim and Bieniasz, 2012 ) but none of them account for the strong IFN-mediated suppression of HIV-1. Recently, human myxovirus-resistance protein B (MxB) has been identified as a major inhibitor of HIV-1 replication induced by IFN (Kane et al., 2013 , Goujon et al., 2013 and LIU et al., 2013 ).
Like most mammals, humans carry two myxovirus resistance genes, MX1 and MX2, which have arisen by gene duplication (Horisberger et al., 1983 and Aebi et al., 1989 ) and encode the interferon-inducible dynamin-like GTPases MxA and MxB (Aebi et al., 1989 ). Human MxA has been shown to suppress a wide range of pathogenic DNA and RNA viruses (Gordien et al., 2001 ). In contrast, human MxB does not suppress the viruses tested in previous studies (Melen et al. 1996 ). MxB inhibits HIV-1 replication at post-entry steps (Schulte et al., 2015 , Buffone et al., 2015 , Fackler and Keppler, 2013 , LIU et al., 2013 , Kane et al., 2013 , Goujon et al., 2013 , Goujon et al., 2015 and Goujon et al., 2014 ). MxB binding to HIV-1 capsid (CA) has been shown to be important for viral restriction (Fribourgh et al., 2014 , Fricke et al., 2014 and KONG et al., 2014 ).
Unlike APOBEC3, BST-2 and SAMHD1, MxB have not been found to be antagonized by HIV or SIV encoded regulatory proteins. Whether MxB antiviral activity plays an important role in vivo and whether HIV-1 can develop mechanisms to escape MxB activity during viral transmission has not been well characterized. In the present study, we identified a number of capsid variants that render the virus resistant to the activity of MxB. These MxB resistant capsid variants do not alter viral fitness and can still be recognized by MxB. Some of the identified variants are most commonly found in subtype C HIV-1 and are accumulating during expansion of the subtype C epidemic.
2. Materials and Methods
2.1. Ethics Statement
Whole blood was obtained from healthy donors that signed an informed consent. This study has been approved by the Ethics Committee of Institute of Virology and AIDS Research, First Hospital of Jilin University.
2.2. Plasmid Construction
The HIV-1-based expression vector pSCRPSY-MxB was a generous gift from Dr. Paul D. Bieniasz (The Rockefeller University). The MxB expression plasmid Retro-X-MxB and shRNA (TRCN0000056713) targeting MxB were generous gifts from Dr. Chen Liang (McGill University). To generate an expression vector encoding HA-tagged MxB fusion protein, the MxB-HA fragment was PCR amplified using Retro-X-MxB as the template, it was then digested with SalI and XbaI and cloned into VR1012 to generate pVR1012-MxB-HA. Plasmids were generated encoding MxB with an N-terminal truncation: MxB(Δ1–82). This truncated protein was fused with HIV-1 core binding motif sequences derived from PDZD8(MxB(Δ1–82)-sPDZD8), which was constructed by Generay Biotech (Shanghai). The HIV-1 GFP reporting vector (pNL4-3-ΔEnv-EGFP, Cat# 11,100) provided by Dr. Robert Siliciano (Johns Hopkins University) was obtained through the NIH AIDS Research and Reference Reagent Program, NIH. HIV-1 NL4-3 ΔEnv-GFP with capsid mutants was provided by Dr. Christopher Aiken (Vanderbilt University School of Medicine). The NL4-3 CA G116A infectious clone was generated by replacing the BssHII-SpeI DNA fragment from NL4-3 (Cat#114, provided by Dr. Malcolm Martin and obtained through the NIH AIDS Reagent Program, Division of AIDS, NIAID, NIH) with that from NL4-3 ΔEnv-GFP (G116A). The composition of the NL4-3 CA G116A construct was confirmed by DNA sequencing.
2.3. Cells
HEK293T cells (AIDS Research and Reference Reagents Program, Cat #3522) and TZM-bl cells (AIDS Research and Reference Reagents Program, Cat#8129) were maintained in Dulbeccos modified Eagles medium (DMEM, Life Technology) with 10% fetal bovine serum (FBS) and penicillin-streptomycin. The cell lines U937 and K562 (ATCC) were provided by Dr. Donald Small (Johns Hopkins University) and cultured in RPMI medium with 10% FBS. SupT1 cells were grown in RPMI medium supplemented with 10%FBS. Peripheral blood mononuclear cells (PBMC) were obtained from buffy-coat by Ficoll density gradient centrifugation. Monocytes enriched from PBMC by positive selection using CD14 MicroBeads were differentiated into macrophages by culturing in RPMI supplemented with 10% FBS, 50 ng/ml human GM-CSF (R&D Systems) 100 U/ml penicillin, and 100 μg/ml streptomycin. shRNA-silenced cell lines were generated according to the manufacturers instructions (Open biosystem) and selected for resistance to puromycin. All cultured cell lines were maintained at 37 °C in a humidified atmosphere containing 5% CO2 .
2.4. Transfection and Immunoblotting
DNA transfection was carried out using Lipofectamine 2000 (Invitrogen) according to the manufacturers instructions. HEK293T cells were harvested at 48 h after transfection, washed twice with cold PBS, and lysed in lysis buffer (150 mM Tris, pH 7.5, with 150 mM NaCl, 1% Triton X-100, and complete protease inhibitor cocktail tablets [Roche]) at 4 °C for 30 min, then centrifuged at 10,000g for 30 min. The materials were then analyzed by SDS-PAGE and immunoblotting with the appropriate antibodies as previously described (Wei et al., 2012 ). The following antibodies were used: anti-MxB (Novus Biologicals, NBP1-81018), anti-Cyclophilin A (Santa Cruz Biotechology, sc-134,310), anti-HA (Covance, MMS-101R-1000), and anti-β-actin MAb (Sigma, A3853). Monoclonal antibody anti-CAp24 (Cat #1513) was obtained from the AIDS Research and Reference Reagents Program.
2.5. Viruses and Infection
For HIV-1 GFP viral production, HEK293T cells were transfected with 9 μg of HIV-1ΔENV-GFP and 3 μg of pCMV-VSV-G encoding plasmids; for shRNA production, HEK293T cells were transfected with 5 μg of the shRNA construct, 5 μg of the packaging plasmid pΔ8.91, and 2 μg of the VSV-G encoding plasmid. Medium was harvested 48 h later, then filtered at 0.45 μm. Supernatants were then purified, and lentivirus was concentrated by ultracentrifigation at 28 K for 1.5 h with a 20% sucrose cushion. The virus pellet was then dissolved in PBS and stored at − 80 °C. For single infections with the HIV-1-GFP virus, U937, K562, or 293T cells were plated in 24-well plates 12 h before infection, and the efficiency of productive infection was analyzed 48 h later by flow cytometry (FACSCalibur, BD Biosciences). For Transmitted/founder (T/F) of HIV-1 (ZM249M) infection, viruses were generated from transfected HEK293T cells. SupT1 or MxB-SupT1 cells were exposed to equal amount of ZM249M HIV-1 for 2 h and the supernatants were replaced by fresh media. Two days later, the amount of virus that was released into the culture supernatant was determined by infecting the TZM-bl indicator cells. All results are representative of more than three independent experiments.
2.6. Viral Replication Assay
Primary PBMC were separated from whole blood of healthy donors using the Ficoll-Hypaque method. CD4+ cells were isolated using CD4 MicroBeads (Miltenyi, Bergisch Gladbach, Germany). Cells were then cultured in RPMI 1640 medium containing 5 μg/ml PHA and 20 IU/ml human recombinant IL2 for 3 days. HIV-1 NL4-3 and NL4-3 CA G116A viruses were generated by transfecting HEK293T cells. Virus stocks were assessed for CAp24 concentration using an HIV-1 p24 ELISA Assay kit (XpressBio, Frederick, MD). Equal amounts of virus were used to infect activated T cells and infected cells were washed 6 h after infection. Quantitation of newly produced virus in the supernatants of infected cultures was determined by CAp24 ELISA and a viral infectivity assay using TZM-bl cells. Viruses in the supernatants were harvested at 2, 4, and 8 days post infection and determined using the CAp24 ELISA assay. The infectivity of newly produced viruses was assessed by using the same volume of supernatants to infect the indicator TZM-bl cells. Briefly, 2 × 104 TZM-bl cells were placed in 96-well culture plates and cultured overnight. The cells were infected with 50 μl supernatants containing NL4-3 or NL4-3 CA G116A viruses. After 48 h incubation at 37 °C with 5% CO2 , luciferase activity in cell lysates was measured using the Luciferase Assay kit (Promega, Madison, WI).
2.7. Quantitative Real-time PCR
Cells were collected at 24 h post-infection and washed with PBS. Total RNA was extracted from cells by TRIzol (Invitrogen) and cDNA samples were generated by using the High Capacity cDNA Reverse Transcription Kit (Invitrogen) according to the manufacturers instruction. Samples were then analyzed by quantitative PCR using FastStart Universal SYBR Green Master Mix (Roche) and the ABI 7000 sequence detection system (Applied Biosystems). The sequences of DNA primers for real-time PCR are as follows: Human IFN-β, sense: AGGACAGGATGAACTTTGAC, anti-sense: TGATAGACATTAGCCAGGAG; Human GAPDH, sense: ATGACATCAAGAAGGTGGTG, anti-sense: CATACCAGGAAATGAGCTTG.
2.8. Step Gradient Analyses
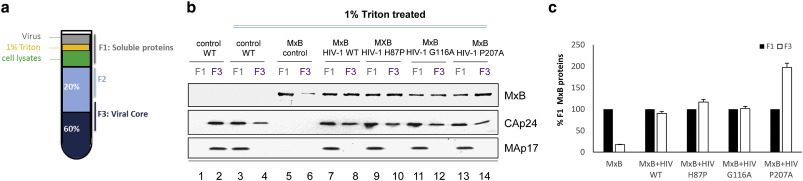
For step sucrose gradient analysis, 2 × 106 MxB-K562 cells were harvested and resuspended in lysis buffer (10 mM Tris, pH 7.4, 1.5 mM MgCl2 , 10 mM KCl, and 0.5 mM DTT). Cells were frozen and thawed twice. Cell lysates were centrifuged at 11,000g for 10 min. The supernatant was collected and immediately used in the binding assay. Purified virus was dissolved in PBS buffer, exposed briefly to 0.1% Triton X-100, and loaded onto soluble MxB containing cell lysates and step sucrose gradient as previously described (Shah and Aiken, 2011 ). Three fractions were harvested: one containing soluble proteins (F1), a buffer fraction (F2), and the virus-core containing fraction (F3). The individual gradient fractions were then subjected to immunoblot analysis.
2.9. Statistical Analysis
Differences among test groups were analyzed by an ANOVA test (Stata Corp, College Station, TX). A value of p < 0.05 was considered to be significant.
3. Results
3.1. Naturally Occurring Capsid Variants That Do Not Reduce Viral Fitness Render HIV-1 Resistant to the Inhibition of MxB
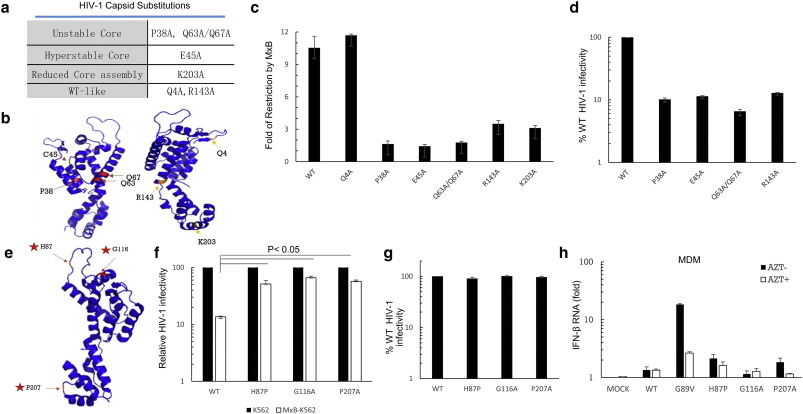
We screened a number of CA variants with single amino acid substitutions that have been shown to decrease (P38A, Q63A/Q67A) or increase (E45A) HIV-1 core stability or to alter host factor binding (G89V) to the HIV-1 core (Shah et al., 2013 and Forshey et al., 2002 ). We observed that certain CA mutations could indeed make mutant HIV-1 resistant to MxB mediated inhibition (Fig. 1 ). These HIV-1 variants can be separated into three classes: (1) resistant to MxB but with reduced viral infectivity (P38A, Q63A/Q67A) (Fig. 1 a–d); (2) resistant to MxB with normal infectivity but enhanced ability to trigger interferon production (CA-G89V) (Fig. S1 and Fig. 1 h); and (3) resistant to MxB with normal infectivity and unaltered ability to trigger interferon production at a level similar to that seen with WT HIV-1 (Fig. 1 e–h).
|
|
|
Fig. 1. The intrinsic features of the HIV-1 core that critically affect sensitivity to MxB restriction. (A) Table of HIV-1 capsid variants which alter viral core stability (either decreased or increased) or have no effect (wild type-like). (B) Location of indicated CA mutations on the structural model of the CA monomer (PDB: 3GV2 ). (C) Folds of restriction to of indicated HIV-1 infectivity by MxB in the presence or absence of MxB expression in K562 cells. The infectivity was measured 48 h after viral infection by using flow cytometry to detect GFP positive cells. Results are representative of four independent experiments. Each bar is the average of three replicates from the same experiment (error bars indicate standard deviations). (D) Relative infectivity of HIV-1 containing the indicated capsid mutants in Hela cells. (E) Location of amino acid residues important for HIV-1 resistance to MxB on the structural model of the CA monomer (PDB: 3GV2 ). (F) Relative infectivity of HIV-1 containing CA mutants H87P, G116 A or P207A in the presence or absence of MxB expression in K562 cells. The infectivity was measured 48 h after viral infection using flow cytometry to detect GFP positive cells. Results are representative of four independent experiments. Each bar is the average of three replicates from the same experiment (error bars indicate standard deviations). The p values were calculated using ANOVA test. (G) Relative infectivity of HIV-1 with the indicated CA mutants compared to the infectivity of the same quantity of wild type virus. The viruses were generated by transfecting HEK293T cells. The same quantity of each virus, measured by viral mRNA, was used to infect the Hela cells. (H) IFN-β mRNA induction after HIV-1 infection in the presence or absence of AZT. Monocyte-derived macrophages isolated from healthy donors were challenged with HIV-1 wild-type viruses, viruses containing MxB-resistant CA mutations (H87P, or G116A, or P207A), or the CypA binding- defective mutant G89V, respectively. The figure shows the effect of CA mutations on IFN-β mRNA expression in macrophages after infection with HIV-1 viruses containing the indicated CA mutations. Cells were harvested 24 h after infection for total RNA extraction, cDNA generation and quantitation by RT-PCR assay. mRNA of interferon beta (IFN-β) was normalized by expression of human GAPDH mRNA. |
Interestingly, we identified three CA surface mutants (H87P, G116A, P207A) that could significantly restore viral infection levels even in the presence of MxB expression (Fig. 1 f). By investigating the effects of these capsid mutants on the HIV-1 life cycle, we confirmed that these capsid mutants maintained similar viral infectivity as wild type HIV-1 (Fig. 1 g). cDNA encoding capsid generated during reverse transcription of viral RNA can potentially interact with host cell proteins and trigger an IFN response that inhibits viral replication. For example, the cDNA encoding the G89V capsid mutant does not binds host CypA resulting in immune activation that prevents viral replication. The CA mutants we have generated did not trigger such immune activation in primary monocyte-derived macrophages (Fig. 1 h).
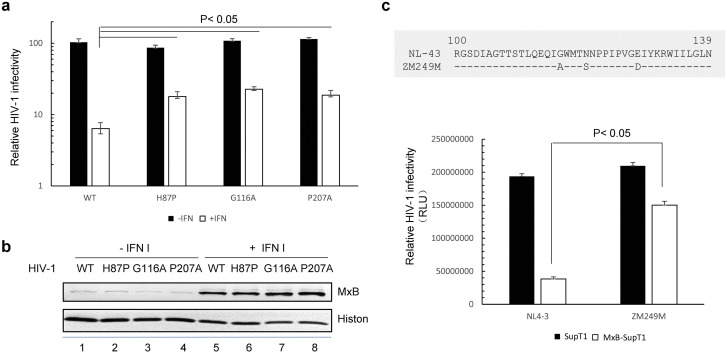
To investigate the infectivity of HIV-1 viruses containing these MxB-resistance CA mutations in interferon (IFN)-treated primary macrophages, we isolated macrophages from healthy donors as previously described (Yu et al., 1991 ). IFN pre-treated and untreated cells were challenged with equal amounts of the indicated GFP-reporter viruses. 48 h after infection, GFP positive cells were analyzed using flow cytometry. HIV-1 mutants (H87P, G116A, P207A) maintained similar infectivity to wild-type virus in primary macrophages (Fig. 2 a). As expected, interferon treatment significantly increased MxB expression in primary macrophages (Fig. 2 b). More importantly, these MxB resistant viruses (H87P, G116A, P207A) became more resistant (2.64–3.40 fold) to interferon-mediated anti-viral activity than the wild-type HIV-1 virus in primary macrophages (Fig. 2 a).
|
|
|
Fig. 2. Certain CAp24 variants confer HIV-1 resisitance to MxB. (a) CAp24 mutations render HIV-1 partially insensitive to inhibition by Interferon in primary macrophages. 24 h before viral infection, macrophages were cultured with or without 500 U ml− 1 IFN-α. Treated cells were challenged by HIV-1 wild-type viruses or viruses containing MxB-resistance CA mutations (H87P, or G116A, or P207A) respectively. The infectivity was measured 48 h after viral infection by using flow cytometry to detect GFP positive cells. Results are representative of three independent experiments. The p values were calculated using ANOVA test with the Bonferroni correction. The expression of endogenous MxB in macrophages was detected by immunoblotting using the indicated antibodies (b). (c) Transmitted/founder (T/F) of HIV-1 subtype C resistant to MxB. Transmitted/founder virus (ZM249M) was used to infect control SupT1 and MxB expressing SupT1 cells. Levels of HIV-1 replication were determined by infecting the TZM-bl reporter cells. Fold-inhibition by MxB was calculated by dividing the amount of HIV-1 produced from MxB- SupT1 cells by that from control SupT1 cells. Results are representative of three independent experiments. Each bar is the average of three replicates from the same experiment (error bars indicate standard deviations). The p values were calculated using ANOVA test with the Bonferroni correction. |
Transmitted/founder (T/F) of HIV-1 subtype C ZM249M containing the G116A mutation was also evaluated for MxB sensitivity. Similar infectivity was detected for NL4-3 and ZM249M viruses in K562 cells (Fig. 2 c). Compared to NL4-3 virus, ZM249M virus was more resistant to MxB-mediated viral inhibition in MxB transduced SupT1 cells (Fig. 2 c). In addition, the virus replication assay confirmed that HIV-1 NL4-3 CA G116A maintained a replication capacity similar to the parental NL4-3 virus in primary T cells (Fig.S1). Together, these data indicate that the G116A mutation in CA can reduce HIV-1 sensitivity to MxB restriction.
3.2. MXB Resistant Capsid Variations Are Detected Among Primary HIV-1 Isolates
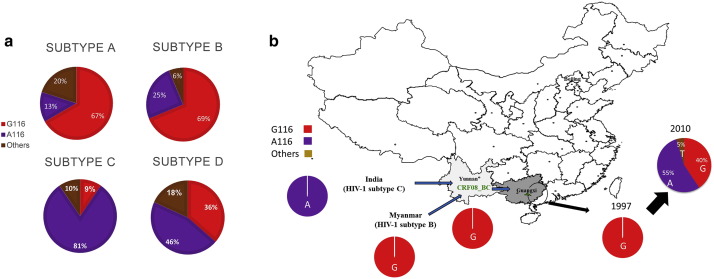
HIV-1 variants (H87P, G116A, P207A) were less sensitive to MxB and still maintained viral infectivity. More importantly, these HIV-1 variants carrying MxB-resistance mutations could be detected among primary HIV-1 isolates from different subtypes. For example, the 2013 HIV sequence compendium reveals that A116 variants are detected among subtypes A, C, and D, which are prevalent in Africa and Asia as well subtype B which is the prevalent strain in Europe and North America. In fact, in subtype C, the A116 variant is the dominant genotype (Fig. 3 a). The accumulation of P87 and A207 variants among HIV-1 subtypes A, B, C and D was also detected but less prevalent than A116 (Fig. S2).
|
|
|
Fig. 3. Detection of MxB resistant CA variations among primary HIV-1 strains from different subtypes. (a) The distribution of CA 116 variants in global HIV-1 group M subtypes A, B, C and D. (b) Paths (arrows) of HIV-1 transmission to and within China. The HIV-1 B/C recombinant CRF08 was generated in Yunnan Province due to recombination between subtype B from Myanmar and subtype C from India. CRF08 was subsequently transmitted to Guangxi Province. The pie charts show the proportion of viral capsid variants at amino acid 116 in south China, colored in red (G116), purple (A116) and brown (others). |
To further evaluate the accumulation of MxB-resistance mutations during HIV-1 transmission in human populations, we analyzed the sequences of circulating HIV-1 stains collected in China since the beginning of the epidemic (1997–2010). A unique subtype B/C recombinant (CRF08) was generated in Yunnan Province (Mcclutchan et al., 2002 , Yu et al., 1998 and Piyasirisilp et al., 2000 ). This recombinant arose from HIV-1 subtype B from Myanmar and subtype C from India in association with drug trafficking patterns between those two countries (Beyrer et al., 2000 ). The majority of the gag gene of CRF08 is subtype C but contains a fragment of CA gene from subtype B (Fig. S3). CRF08 was then transmitted to the neighboring Guangxi Province from Yunnan Province in 1997. The Guangxi founder CRF08 viruses in 1997 all carried the G116 genotype (Fig. 3 b). However, 55% of the circulating CRF08-BC strains detected in 2010 carried the A116 genotype and the G116 viral strains decreased to 40% (Fig. 3 b).
Accumulation of MxB resistance mutations at position 207 of CA during HIV-1 transmission in Southern China was observed (Fig. S4). While the parental subtypes B, C and original CRF08 BC recombinant HIV-1 strains all contained the MxB-sensitive P207 genotype, more recent CRF08 BC recombinant HIV-1 strains carried the A207 MxB-resistant genotype (Fig. S4). Similar accumulation of CA mutation at position 208, which was identified in a recent report (Liu et al., 2015 ), was also observed (Fig. S5). These findings all suggest possible selection for MxB resistant HIV-1 variants.
3.3. Capsid Variants Render HIV-1 Resistant to the Inhibiton of MxB Without Affecting Capsid Binding
MxB has been shown to recognize HIV-1 capsid and this interaction is important for MxB-mediated HIV-1 inhibition (Fribourgh et al., 2014 , KONG et al., 2014 , Fricke et al., 2014 and Matreyek et al., 2014 ). Surprisingly, amino acid variations at positions 87, 116 and 207 of CA influenced the sensitivity of these mutant HIV-1 to MxB activity but did not enhance the interaction of the mutant core with MxB (Fig. 4 ). We next used a different CA-MxB binding assay recently reported by others to investigate the interaction between CAp24 (WT and mutants) and MxB (Liu et al., 2015 ). All tested CAp24 variants maintained MxB binding (Fig.S6). Deletion of the amino-terminal region of MxB (MxB ∆ 1–82) resulted in reduced HIV-1 core binding and impaired ability to inhibit HIV-1 (Fig. S7A–C). Addition of a CA binding motif from PDZD8 (Guth and Sodroski, 2014 and Henning et al., 2010 ) restored HIV-1 core binding but could not enhance the anti -HIV activity of chimeric MxB (∆ 1–82)-PDZD8 (Fig. S7B, C). HIV-1 CA mutants lacking CypA interaction became resistant to MxB restriction ( LIU et al., 2013 , Kane et al., 2013 , Goujon et al., 2013 and Busnadiego et al., 2014 ) but these mutations had no effect on MxB binding ( Liu et al., 2015 and Fricke et al., 2014 ). CsA treatment which disrupts CyPA and CA interaction also impaired MxB mediated HIV-1 inhibition (Fig. S8).
|
|
|
Fig. 4. Capsids of HIV-1 variants resistant to MxB inhibition still interact with MxB. (A) Schematic of MxB-viral core binding assay: HIV-1 viruses were exposed briefly to 0.1% Triton X-100, mixed with soluble MxB containing cell lysates and subsequently loaded onto step sucrose gradients. (B) and (C) The individual gradient fractions representing soluble MxB (F1) and core-associated MxB (F3) were subjected to immunoblot analysis. Antibodies against HIV-1 CAp24 and MAp17 were used as controls. |
HIV-2 is less sensitive to MxB mediated restriction (Fricke et al., 2014 and Goujon et al., 2013 ) and its CA is known to interact poorly with CypA (Lahaye et al., 2013 ). Interestingly, enhancement of CypA binding to HIV-2 CA (Lahaye et al., 2013 ) (Fig. S9A, B) did not increase HIV-2 sensitivity to MxB mediated restriction (Fig. S9C). These data again suggest that MxB binding to HIV-1 CA is necessary but not sufficient for MxB-mediated restriction.
It has been reported that U937 cells express significant level of endogenous MxB proteins but do not suppress HIV-1 infection even in the presence of interferon (Kane et al., 2013 ). We have observed that interferon treatment could significantly enhance MxB expression in Jurkat cells (Fig. S10B). However, enhanced MxB expression had little effect on HIV-1 infection when compared to untreated Jurkat cells (Fig. S10A). The cell type dependent differences in HIV-1 sensitivity to MxB suggest the potential existence of a co-factor required for MxB mediated HIV-1 restriction.
4. Discussion
Interferon (IFN) is a key component of the innate immune response to exogenous pathogens. Interferon increases the mRNA levels of interferon-stimulated genes (ISGs) in vivo which is thought to account for its antiviral activity. Recent studies have identified that human myxovirus resistance protein B, one of the ISGs, contributes to the inhibition of HIV-1 replication by interferon. However, whether HIV-1 could evolve to counteract against MxB restriction has been undefined. In the present study, we identified and characterized a number of capsid variants that render the mutant HIV-1 viruses resistant to the inhibition of MxB without altering viral fitness. These mutant viruses maintained viral infectivity that is comparable to the wild-type virus in human cell lines as well as in primary macrophages (Fig. 1 ). Furthermore, like wild-type virus, they do not trigger type I interferon production during infection of primary macrophages (Fig. 1 h). This is in sharp contrast to the HIV-1 mutant (G89V) that lost the ability to bind CyPA and became resistant to MxB inhibition but could not prevent interferon production (Fig. 1 h).
The capsid mutations that could render HIV-1 less sensitive to MxB restriction are detected among primary HIV-1 isolates. Of particular interest is the finding that MxB resistant variants containing A116 are most commonly found in the Clade C HIV-1 viruses that are the most rapidly expanding clade throughout the world. Furthermore, as the HIV-1 epidemic spreads in China, there is a clear positive selection for those MxB resistance variants that do not alter viral fitness. These findings support a critical role for MxB as a selective force during HIV-1 transmission and evolution. It is not clear why the A116 mutation that has become predominant in subtype C HIV-1 viruses has not attained the same dominance in other HIV-1 subtypes such as A, B, and D, which still primarily carry G116. One possibility is that these HIV-1 subtypes do not encounter MxB inhibition during HIV-1 transmission when compared to subtype C HIV-1. Alternatively, A116 in CA is less fit than G116 in certain HIV-1 subtypes and is only selected when they encounter MXB selection. Another possibility is that HIV-1 subtypes A, B, and D use other strategies to overcome MxB restriction.
MxB targets HIV-1 capsid to mediate its anti-viral function. We have observed that HIV-1 resistant variants maintained the ability to be recognized by MxB, suggesting the existence of MxB co-factor(s) required for MxB mediated viral restriction. Consistent with this idea, Jurkat cells express high level of endogenous MxB proteins after interferon treatment (Fig. S10). However, interferon induced MxB expression did not alter HIV-1 infectivity in these Jurkat cells compared to the untreated Jurkat cells (Fig. S10). It has been reported that U937 cells express MxB, but this expression has limited impact on HIV-1 infection (Kane et al., 2013 ). CypA has been reported to be a critical factor for MxB mediated HIV-1 restriction. We have observed that addition of CypA binding to HIV-2 capsid did not alter HIV-2 sensitivity to MxB (Fig. S9). Factor(s) in addition to CypA may be required for MxB mediated HIV-1 restriction. Interestingly, the three MxB-resistant HIV-1 capsid variants are all located on the raised surface region formed by two subunits of the capsid hexamer (Fig. S11), suggesting that these sites could influence the putative MxB cofactor binding but may not alter intrinsic features of the viral core (Fig. 5 ). Identification of the critical role of these HIV-1 capsid mutations in overcoming a host restriction factor may provide opportunities for the development of therapeutic interventions.
|
|
|
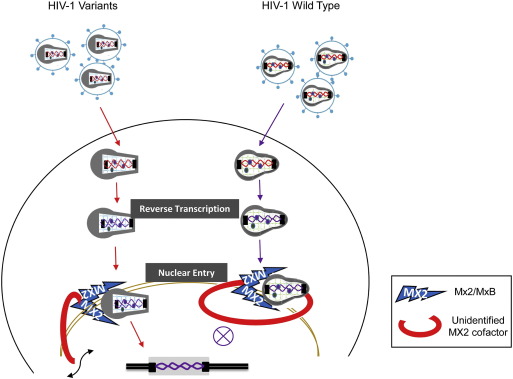
Fig. 5. Diagram of proposed models for HIV-1 evasion of the antiviral activity of MxB. MxB as an endogenous lentiviral infection sensor is located at the nuclear pore. After HIV-1 entry, MxB recognizes and binds to the core, which allows the attachment of a MxB cofactor to bind to the complex, thereby inhibiting viral infection. HIV-2 or HIV-1 with certain CA surface residue mutations avoid the putative MxB cofactor binding and are resistant to MxB mediated viral restriction. |
Funding Sources
This work was supported in part by funding from the Chinese Ministry of Science and Technology (No 2012CB911100 ), the Chinese Ministry of Education (No IRT1016 ). The funding sources had no role in the writing of the manuscript or the decision to submit for publication. We would like to acknowledge support for the statistical analysis from the National Center for Research Resources and the National Center for Advancing Translational Sciences (NCATS) of the National Institutes of Health through Grant Number 1UL1TR001079 . The authors were not paid to write this article by any pharmaceutical company or agency.
Conflicts of Interest
The authors have no conflict of interest to declare.
Author Contributions
W.W., H.G. and M.M. performed experiments. W.W., R.M., and XF.Y. analyzed the data. W.W., R.M., and XF.Y. wrote the paper with help from all authors. W.W., and XF.Y. directed the project.
Acknowledgments
We thank Guoqiang Zhou, Jingliang Li and Chunyan Dai for technical assistance; Yajuan Rui and Dr. Carol Thompson for data analysis; Drs. C. Aiken, P. Bieniasz, C. Liang, R. Siliciano and D. Small for critical reagents. pAM249M cat#12416 was obtained through the NIH AIDS Reagent Program, Division of AIDS, NIAID, NIH from Dr. Beatrice Hahn.
Appendix A. Supplementary data
Supplementary figures.
References
- Aebi et al., 1989 M. Aebi, J. Fah, N. Hurt, C.E. Samuel, D. Thomis, L. Bazzigher, J. Pavlovic, O. Haller, P. Staeheli; cDNA structures and regulation of two interferon-induced human Mx proteins; Mol. Cell. Biol., 9 (1989), pp. 5062–5072
- Beyrer et al., 2000 C. Beyrer, M.H. Razak, K. Lisam, J. Chen, W. Lui, X.F. Yu; Overland heroin trafficking routes and HIV-1 spread in south and south-east Asia; AIDS, 14 (2000), pp. 75–83
- Buffone et al., 2015 C. Buffone, B. Schulte, S. Opp, F. Diaz-Griffero; Contribution of MxB oligomerization to HIV-1 capsid binding and restriction; J. Virol., 89 (2015), pp. 3285–3294
- Busnadiego et al., 2014 I. Busnadiego, M. Kane, S.J. Rihn, H.F. Preugschas, J. Hughes, D. Blanco-Melo, V.P. Strouvelle, T.M. Zang, B.J. Willett, C. Boutell, P.D. Bieniasz, S.J. Wilson; Host and viral determinants of Mx2 antiretroviral activity; J. Virol., 88 (2014), pp. 7738–7752
- Chun et al., 1995 T.W. Chun, D. Finzi, J. Margolick, K. Chadwick, D. Schwartz, R.F. Siliciano; In vivo fate of HIV-1-infected T cells: quantitative analysis of the transition to stable latency; Nat. Med., 1 (1995), pp. 1284–1290
- Fackler and Keppler, 2013 O.T. Fackler, O.T. Keppler; MxB/Mx2: the latest piece in HIVs interferon puzzle; EMBO Rep., 14 (2013), pp. 1028–1029
- Forshey et al., 2002 B.M. Forshey, U. von Schwedler, W.I. Sundquist, C. Aiken; Formation of a human immunodeficiency virus type 1 core of optimal stability is crucial for viral replication; J. Virol., 76 (2002), pp. 5667–5677
- Fribourgh et al., 2014 J.L. Fribourgh, H.C. Nguyen, K.A. Matreyek, F.J. Alvarez, B.J. Summers, T.G. Dewdney, C. Aiken, P. Zhang, A. Engelman, Y. Xiong; Structural insight into HIV-1 restriction by MxB; Cell Host Microbe, 16 (2014), pp. 627–638
- Fricke et al., 2014 T. Fricke, T.E. White, B. Schulte, D.A. de Souza Aranha Vieira, A. Dharan, E.M. Campbell, A. Brandariz-Nunez, F. Diaz-Griffero; MxB binds to the HIV-1 core and prevents the uncoating process of HIV-1; Retrovirology, 11 (2014), p. 68
- Gordien et al., 2001 E. Gordien, O. Rosmorduc, C. Peltekian, F. Garreau, C. Brechot, D. Kremsdorf; Inhibition of hepatitis B virus replication by the interferon-inducible MxA protein; J. Virol., 75 (2001), pp. 2684–2691
- Goujon et al., 2013 C. Goujon, O. Moncorge, H. Bauby, T. Doyle, C.C. Ward, T. Schaller, S. Hue, W.S. Barclay, R. Schulz, M.H. Malim; Human MX2 is an interferon-induced post-entry inhibitor of HIV-1 infection; Nature, 502 (2013), pp. 559–562
- Goujon et al., 2014 C. Goujon, O. Moncorge, H. Bauby, T. Doyle, W.S. Barclay, M.H. Malim; Transfer of the amino-terminal nuclear envelope targeting domain of human MX2 converts MX1 into an HIV-1 resistance factor; J. Virol., 88 (2014), pp. 9017–9026
- Goujon et al., 2015 C. Goujon, R.A. Greenbury, S. Papaioannou, T. Doyle, M.H. Malim; A triple-arginine motif in the amino-terminal domain and oligomerization are required for HIV-1 inhibition by human MX2; J. Virol., 89 (2015), pp. 4676–4680
- Guth and Sodroski, 2014 C.A. Guth, J. Sodroski; Contribution of PDZD8 to stabilization of the human immunodeficiency virus type 1 capsid; J. Virol., 88 (2014), pp. 4612–4623
- Henning et al., 2010 M.S. Henning, S.G. Morham, S.P. Goff, M.H. Naghavi; PDZD8 is a novel Gag-interacting factor that promotes retroviral infection; J. Virol., 84 (2010), pp. 8990–8995
- Horisberger et al., 1983 M.A. Horisberger, P. Staeheli, O. Haller; Interferon induces a unique protein in mouse cells bearing a gene for resistance to influenza virus; Proc. Natl. Acad. Sci. U. S. A., 80 (1983), pp. 1910–1914
- Yu et al., 1991 X.F. Yu, Q.C. Yu, M. Essex, T.H. Lee; The vpx gene of simian immunodeficiency virus facilitates efficient viral replication in fresh lymphocytes and macrophage; J. Virol., 65 (1991), pp. 5088–5091
- Kane et al., 2013 M. Kane, S.S. Yadav, J. Bitzegeio, S.B. Kutluay, T. Zang, S.J. Wilson, J.W. Schoggins, C.M. Rice, M. Yamashita, T. Hatziioannou, P.D. Bieniasz; MX2 is an interferon-induced inhibitor of HIV-1 infection; Nature, 502 (2013), pp. 563–566
- KONG et al., 2014 J. KONG, B. Xu, W. Wei, X. Wang, W. Xie, X.F. Yu; Characterization of the amino-terminal domain of Mx2/MxB-dependent interaction with the HIV-1 capsid; Protein Cell, 5 (2014), pp. 954–957
- Lahaye et al., 2013 X. Lahaye, T. Satoh, M. Gentili, S. Cerboni, C. Conrad, I. Hurbain, A. EL Marjou, C. Lacabaratz, J.D. Lelievre, N. Manel; The capsids of HIV-1 and HIV-2 determine immune detection of the viral cDNA by the innate sensor cGAS in dendritic cells; Immunity, 39 (2013), pp. 1132–1142
- Yu et al., 1998 X.F. Yu, J. Chen, Y. Shao, C. Beyrer, S. Lai; Two subtypes of HIV-1 among injection-drug users in southern China; Lancet, 351 (1998), p. 1250
- LIU et al., 2013 Z. LIU, Q. PAN, S. DING, J. QIAN, F. Xu, J. Zhou, S. Cen, F. Guo, C. Liang; The interferon-inducible MxB protein inhibits HIV-1 infection; Cell Host Microbe, 14 (2013), pp. 398–410
- Liu et al., 2015 Z. Liu, Q. Pan, Z. Liang, W. Qiao, S. Cen, C. Liang; The highly polymorphic cyclophilin A-binding loop in HIV-1 capsid modulates viral resistance to MxB; Retrovirology, 12 (2015), p. 1
- Malim and Bieniasz, 2012 M.H. Malim, P.D. Bieniasz; HIV restriction factors and mechanisms of evasion; Cold Spring Harb Perspect Med, 2 (2012), p. a006940
- Matreyek et al., 2014 K.A. Matreyek, W. Wang, E. Serrao, P.K. Singh, H.L. Levin, A. Engelman; Host and viral determinants for MxB restriction of HIV-1 infection; Retrovirology, 11 (2014), p. 90
- Mcclutchan et al., 2002 F.E. Mcclutchan, J.K. Carr, D. Murphy, S. Piyasirisilp, F. Gao, B. HAHN, X.F. Yu, C. Beyrer, D.L. Birx; Precise mapping of recombination breakpoints suggests a common parent of two BC recombinant HIV type 1 strains circulating in China; AIDS Res. Hum. Retrovir., 18 (2002), pp. 1135–1140
- Melen et al., 1996 K. Melen, P. Keskinen, T. Ronni, T. Sareneva, K. Lounatmaa, I. Julkunen; Human MxB protein, an interferon-alpha-inducible GTPase, contains a nuclear targeting signal and is localized in the heterochromatin region beneath the nuclear envelope; J. Biol. Chem., 271 (1996), pp. 23478–23486
- Piyasirisilp et al., 2000 S. Piyasirisilp, F.E. McCutchan, J.K. Carr, E. Sanders-Buell, W. Liu, J. Chen, R. Wagner, H. Wolf, Y. Shao, S. LAI, C. Beyrer, X.F. Yu; A recent outbreak of human immunodeficiency virus type 1 infection in southern China was initiated by two highly homogeneous, geographically separated strains, circulating recombinant form AE and a novel BC recombinant; J. Virol., 74 (2000), pp. 11286–11295
- Schulte et al., 2015 B. Schulte, C. Buffone, S. Opp, F. DI Nunzio, D.A. de Souza Aranha Vieira, A. Brandariz-Nunez, F. Diaz-Griffero; Restriction of HIV-1 requires the N-terminal region of MxB as a capsid-binding motif but not as a nuclear localization signal; J. Virol., 89 (2015), pp. 8599–8610
- Shah and Aiken, 2011 V.B. Shah, C. Aiken; In vitro uncoating of HIV-1 cores; J Vis Exp. (2011)
- Shah et al., 2013 V.B. Shah, J. Shi, D.R. Hout, I. Oztop, L. Krishnan, J. Ahn, M.S. Shotwell, A. Engelman, C. Aiken; The host proteins transportin SR2/TNPO3 and cyclophilin A exert opposing effects on HIV-1 uncoating; J. Virol., 87 (2013), pp. 422–432
- Wei et al., 2012 W. Wei, H. Guo, X. Han, X. Liu, X. Zhou, W. Zhang, X.F. Yu; A novel DCAF1-binding motif required for Vpx-mediated degradation of nuclear SAMHD1 and Vpr-induced G2 arrest; Cell. Microbiol., 14 (2012), pp. 1745–1756
Document information
Published on 06/04/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?