(Created page with " ==Abstract== ====Background==== Extracellular vesicles (EVs) are thought to exert protective effects after ischemic and remote ischemic preconditioning. It is not well und...") |
(No difference)
|
Revision as of 11:44, 19 May 2017
Abstract
Background
Extracellular vesicles (EVs) are thought to exert protective effects after ischemic and remote ischemic preconditioning. It is not well understood which EV content factors are most relevant for protective effects. We hypothesize that ischemic preconditioning leads to qualitative changes in EV mRNA content and quantitative changes in EV size and number.
Methods
Using an in vivo porcine ischemic preconditioning model, EVs were collected from coronary venous blood, and isolated by differential ultracentrifugations. The presence and purity of EV were verified by electron microscopy and Western blot, and EV number was assessed by nanoparticle tracking analysis. The mRNA EV was identified by microarray.
Results
Gene ontology analysis showed enrichment of EV mRNA coding for proteins associated with regulation of transcription, translation, extracellular matrix, morphogenic development and feeding behavior. There were 11,678 different mRNA transcripts detected in EV, where a total of 1103 was significantly increased or decreased after preconditioning, of which 638 mRNA sequences were up-regulated and/or emerged due to preconditioning. Several of them have known association with ischemic preconditioning. There was no significant difference in EV quantity or size before and after preconditioning.
Conclusions
These findings demonstrate in an in vivo model that myocardial ischemic preconditioning influences the composition of mRNA in EV, including gene transcripts for proteins associated with the protective effect of ischemic preconditioning. The finding that preconditioned parental cells release EV containing mRNA that is qualitatively different from those released by non-preconditioned cells shows the importance of the external milieu on parental cell EV production.
Keywords
Extracellular vesicles;mRNA;Transcription;Ischemic preconditioning;Myocardium
1. Introduction
Extracellular vesicles (EVs) are present in all body fluids, and they are known to transport different types of cell contents, including proteins, DNA and RNA [1]; [2] ; [3]. Their biological function is currently not completely understood. The term EV includes different secreted membrane-enclosed vesicles such as exosomes and microvesicles, however there are no specific markers that distinguish subsets of EV from one the other [4]. Most cell types, including cardiomyocytes, actively secrete EV through exocytosis by fusion of multi-vesicular bodies with the plasma membrane or through budding from the cell membrane [5]; [6] ; [7].
Although the functions of EVs are not well understood, they contain markers of conditions of the parent cell. EV from hypoxic cells contain different proteins compared to EV from the same cells before hypoxia [8] ; [9]. When parent cells were exposed to different growth factors, a change in EV messengerRNA (mRNA) composition has been demonstrated [10]. The EV mRNA is presumed to have a functional impact if transferred to a recipient cell, by itself leading to protein synthesis [3] ; [11]. Hence, EV contents can be conveyed to other cells and therefore may be an important signaling mechanism between cells, which can function to confer effects from remote parent cells.
While prolonged myocardial ischemia can lead to permanent injury, there are adaptive protective mechanisms to provide extra resistance to damage. Myocardial ischemic preconditioning (IPC) is a pre-treatment of cardiac tissue where repetitive short exposures to ischemia followed by reperfusion leads to increased cell tolerance for ischemia at a later exposure. This is presumed to be brought about by internal cell mechanisms activated by the short ischemic periods [12] ; [13]. The mechanisms of cellular protections from IPC are not fully known. Recently, EVs were suggested as possible key mediators of protective effects. Extracellular vesicles from the limb muscle and mesenchymal cells exposed to IPC as well as coronary perfusate with EV from IPC hearts, have both in vitro and in vivo, been associated with possible anti-apoptotic effects, limited infarction size and improving cardiac function [14]; [15] ; [16]. Another recent publication has shown both how IPC related changes in EV concentration can occur, as well as the occurrence of EV related proteins that can activate protein kinases already recognized in connection with cardioprotective IPC effects [17]. Findings have also demonstrated that cardiac progenitor cells might stimulate regeneration, and this could lead to functional improvement in the injured myocardium due to EV mediating cardioprotection [18] ; [19].
The specific hypothesis of this study is that IPC leads to qualitative changes in EV mRNA content and quantitative changes in EV size and number. We aimed to study this in EV material collected in vivo in a large animal model through using localized sampling and collection coordinated with a distinct IPC treatment.
2. Materials and methods
Ethical approval for this study (dnr: A182-12) was obtained from the Regional Animal Research Ethics Committee in Umeå, Sweden, and was carried out in accordance with the Guide for the Care and Use of Laboratory Animals (1996, National Academy of Science Institute for Laboratory Animal Research, USA) and the EU Directive 2010/63/EU for animal experiments (http://ec.europa.eu/environment/chemicals/lab_animals/legislation_en.htm). The study material was collected from anesthetized and surgically prepared domestic land-race pigs.
2.1. Preparation
Animals were premedicated with ketamine 10 mg·kg− 1 (Ketalar, Pfizer, Morris Plains, New Jersey, USA) and xylazine 2 mg·kg− 1 (Rompun vet, Bayer AB, Lyngby, Denmark) intramuscularly, and then an ear vein intravenous cannula was used for induction of anesthesia with pentobarbital 10 mg·kg− 1 (Pentobarbitalnatrium, Apoteksbolaget, Stockholm, Sweden). Throughout the experiment anesthesia was maintained with a continuous infusion of pentobarbital 5 mg·kg− 1·h− 1, fentanyl 20 μg·kg− 1·h− 1 (Fentanyl, Braun, Melsungen, Germany) and midazolam 0.3 mg·kg− 1·h− 1 (Dormicum, Roche, Basel, Switzerland). No muscle relaxants were used. Volume-controlled ventilation was used (Evita 4, Dräger, Kiel, Germany) with a mixture of 30% oxygen and adjusted to normocapnia by end-tidal capnometry. Intravenous Ringers acetate was infused at 15 mL·kg−1·h− 1 throughout the protocol. Rectally measured body temperature was maintained at 38–39 °C by cloth covers. At the end of the experiment the animals were euthanized by 40 mmol of potassium chloride after a bolus of pentobarbital (around 200 mg).
Throughout the experiment the heart rate, mean arterial pressure (MAP), ECG and central venous pressure (CVP) were recorded continuously, with all data saved in digital format using a computer based multi-channel acquisition and analysis system (AcqKnowledge, Biopac, California, USA). In dorsal position, a tracheostomy was performed and by surgical dissection neck artery and veins were exposed for cannulation. A triple-lumen central vein catheter (Arrow-Howe Multi-Lumen Central Venous Catheter, Vingmed, Järfälla, Sweden) was inserted for CVP measurements and infusion of drugs and fluids. For invasive blood pressure an arterial catheter was placed in the carotid artery. For selective blood sampling of the blood from coronary veins draining the myocardial ischemic area, a coronary sinus catheter (CCS-7U-90A; Webster Labs, Altadena, California, USA) was placed with the tip optimally positioned using fluoroscopic guidance.
Midline sternotomy and pericardiotomy were performed, followed by placing a patched snare for intermittent occlusion of the middle portion of the left anterior descending artery (LAD), without injury to the corresponding vein. Myocardial ischemia and accurate reperfusion sampling was confirmed by more than doubling of coronary lactate production (Radiometer ABL-5, Copenhagen Denmark).
2.2. Myocardial ischemic preconditioning
The pigs were allowed to rest for 1 h after the surgical preparation before baseline coronary venous samples were collected. Myocardial IPC was created by temporary snare-occlusion for 10 min followed by reperfusion during 20 min, repeated four times [20]. Coronary venous samples (10 mL each) were collected every second minute during a 20 min period, starting 20 min after last LAD snare release. All blood samples were immediately centrifuged for 10 min (at 4 °C and 1800 ×g) to separate the plasma, which was further mixed with an equal amount of phosphate-buffered saline (PBS). Thereafter samples were stored in − 80 °C until EV isolation could be completed.
2.3. Extracellular vesicle isolation
Extracellular vesicles were isolated by differential centrifugations and preparative ultracentrifugation. Plasma samples were thawed in room temperature and centrifuged for 30 min at 4 °C and 3000 ×g, followed by 10,000 ×g for 35 min at 4 °C to remove cellular debris. Supernatants were ultracentrifuged to separate the medium and the EV pellets. All ultracentrifugation steps were conducted at 110,000 ×g for 2 h and 4 °C using a L-90 Beckman centrifuge and the SW-41 rotor (Beckman Instruments, Inc., Fullerton, CA). Pellets were resuspended in PBS to a total volume of 1.5 mL followed by nuclease treatment (Benzonase Nuclease Ultrapure, ≥ 250 units/μL, Sigma-Aldrich, Brøndby, Denmark), for 1 h at 37 °C and 80 rpm (for removal of possible extracellular RNA and DNA). Next, samples were added to the top of a sucrose gradient (prepared by equal amounts of 20% and 40% sucrose solution), followed by immediate ultracentrifugation. Extracellular vesicle fractions were collected by taking 2–3 mL of solution from gradient zone, which were further washed with PBS and once again ultracentrifuged. The pellet was resuspended in PBS before storage in − 80 °C.
2.4. Evaluation of extracellular vesicle preparation
Electron microscopy (EM) and Western blot (described below) were performed as a quality control step to confirm the presence of EV as well as the absence of contaminants such as larger vesicles and cells. Electron microscopy of isolated EV was performed at the electron microscopy unit Emil, Clinical research center, Huddinge, Sweden. Nanoparticle tracking analysis (NTA) (NanoSight N300, Malvern Instruments Ltd. Malvern, United Kingdom) was used for quantification and sizing of EV for isolates from four pigs, before and after IPC, with final samples diluted in PBS (1:500–1:1000).
A Western blot analysis was performed on lysed EV. CD81 was used as an EV marker and GRP78 to detect potential contamination of cells and apoptotic bodies, and these were compared to crushed porcine myocardial tissue in a cell suspension. Although, this procedure is intended to quantify several proteins in the EV preparation, the limited amount available porcine antibodies restricted us of using only CD81 and GRP78 [4]. Protein concentration was determined using BCA Protein assay (Pierce) and samples of 5–10 μg protein were separated by 10% and 5–14% Mini-PROTEAN TGX gels (Bio-Rad, USA). The separated protein fractions in the gels were then transferred to PVDF membranes (Midi format 0.2 μm, Bio-Rad, USA) using Trans-Blot Turbo (Transfer System, Bio-Rad, USA). The membranes were blocked by Odyssey Blocking Buffer (LI-COR Biosciences, Nebraska, USA) for 1 h at 21 °C, washed with PBS Tween (PBST) and subsequently incubated with an anti-CD81 antibody (Santa Cruz Biotechnology, Texas, USA), diluted 1:200 in 1% PBST and anti GRP-78 antibody (Abcam, UK), and diluted 1:1000 in 1% PBST at 4 °C overnight. The membranes were washed with PBST before they were incubated with secondary goat anti-rabbit antibody (IRDye, 800 CW, LI-COR, USA) and diluted 1:10,000 in 1% PBST for 1 h at 21 °C. After washing with PBST the proteins were visualized using LI-COR ODYSSEY GLx.
2.5. Extracellular vesicle DNA/RNA preparation
The Qiagen Allprep DNA/RNA Mini kit (Qiagen, Alameda, CA, USA) was used to isolate DNA and mRNA from the EV preparation, according to the manufacturers instructions. DNA and mRNA were stored at − 80 °C and the DNA was kept for potential later analysis. mRNA content of the EV pellet was quantified using a nanodrop spectrophotometer (nanoDrop Technologies Inc., Wilmington, Delaware, USA).
2.6. Microarray expression analysis
RNA quality was evaluated using the Agilent 2100 Bioanalyzer system (Agilent Technologies Inc., Palo Alto, CA, USA). Fifty nanograms of total RNA from each sample was used to generate amplified and biotinylated sense-strand cDNA from the entire expressed genome according to the GeneChip® WT PLUS Reagent Kit User Manual (P/N 703174 Rev. 1, Affymetrix Inc., Santa Clara, CA, USA). GeneChip® ST Arrays (GeneChip® Porcine Gene 1.0 ST Array) were hybridized for 16 h in a 45 °C incubator, rotated at 60 rpm. According to the GeneChip® Expression Wash, Stain and Scan Manual (P/N 702731 Rev. 3, Affymetrix Inc., Santa Clara, CA, USA) the arrays were then washed and stained using the Fluidics Station 450 and finally scanned using the GeneChip® Scanner 3000 7G.
2.7. Microarray data
The raw data was normalized in the free software Expression Console provided by Affymetrix (http://www.affymetrix.com) using the robust multi-array average (RMA) method first suggested by Li and Wong in 2001 [21] ; [22]. Subsequent analysis of the gene expression data was carried out in the freely available statistical computing language R (http://www.r-project.org) using packages available from the Bioconductor project (www.bioconductor.org). In order to search for the differentially expressed genes before and after IPC an empirical Bayes moderated t-test was then applied, using the robust version of the lmFit function, from the ‘limma’ package [23] ; [24]. To address the problem with multiple testing, p-values were adjusted using the method of Benjamini and Hochberg [25].
2.8. Ortholog analysis
Since the functions of many Sus scrofa genes are not well known, we chose to identify orthologous genes in the better studied Homo sapiens. Accession numbers for highly expressed genes in the EV of Sus Scrofa, were translated to the corresponding UniProt ID, using the ID mapping tool at www.uniprot.org. The UniProt IDs could further be used to identify human orthologs in the list obtained from InParanoid8 (http://inparanoid.sbc.su.se/cgi-bin/e.cgi) [26].
2.9. Gene ontology
Gene ontology analysis was performed on the 2000 human genes whose orthologs showed the highest expression in all samples, using the functional annotation clustering tool in the web-accessible program DAVID Bioinformatics version 6.7 (http://david.abcc.ncifcrf.gov/home.jsp). Clusters having enrichment score > 1.3 were regarded as significant [27].
2.10. Analysis of gene expression data from microarray
Average expression of each gene was calculated as the mean value of samples before IPC (n = 5) and the mean of the reperfusion samples (n = 4, one was excluded from this analysis due to the lack of material). To adjust for non-specific hybridization the limit of expression was set as above the background signal (> 1.5). Only these genes were further analyzed. Stating this, an average signal below 1.5 was considered not existing. Therefore, samples before IPC, with average expression < 1.5 increasing to > 1.5 during reperfusion were considered to have emerged as a result of IPC. Vice versa, samples expressed > 1.5 before IPC and declined to < 1.5 after reperfusion were considered to have disappeared due to IPC. When average expression was > 1.5 during baseline and reperfusion, significant up- or downregulated genes were defined as log 2 Fold Change (log 2 FC) ± 0.5. Statistical significance was stated as P < 0.05. The gene expression log 2 FC was calculated as the mean value of reperfusion relative to the mean value before IPC.
3. Results
Five animals were included and completed the protocol for EV sampling before IPC and during reperfusion. The average animal weight was 39.6 ± 4.2 kg (standard deviation). Hemodynamic measurements (all n = 5) before and after (respectively) ischemic preconditioning were as follows: heart rate 89 ± 22 and 82 ± 8.0 beats per minute, mean arterial pressure 92 ± 10.1 and 77 ± 15.7 mm Hg, and central venous pressure 3 ± 0.7 and 4 ± 2.0 mm Hg.
3.1. Purity of EV preparation and EV characterization
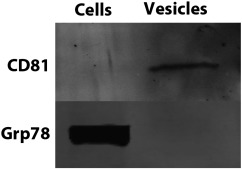
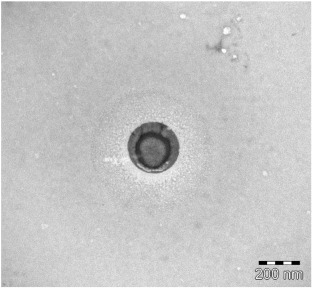
To confirm the presence of EV and estimate the purity of isolation, the EV fractions were evaluated by Western blot, EM and NTA. CD81, a known EV marker, was found in EV samples but not in the porcine cell suspension which indicates that EV preparations were correctly purified (Fig. 1). An endoplasmic reticulum protein, GRP78, was detected in the cell suspension but not in EV; indicating the absence of contaminating apoptotic bodies in the EV preparation (Fig. 1). EM analysis of the EV fractions demonstrated typical morphology of EV and no cell debris (Fig. 2). Nanoparticle tracking analysis showed EV ranging from 30 to 350 nm, the major part between 75 and 200 nm (data not shown). There was no significant difference in plasma EV quantity before and after IPC (data not shown).
|
|
|
Fig. 1. Western blot results. CD81 is present in extracellular vesicle (EV) (labeled Vesicles in the figure) samples and GRP78 in cell suspension (labeled Cells in the figure). The absence of CD81 in cell suspension and GRP78 in EV identifies isolated vesicles as EV with no detectable contamination of apoptotic bodies. |
|
|
|
Fig. 2. Electron microscopy picture of isolated extracellular vesicle. Note the ‘cup-shaped’ appearance. |
3.2. Microarray
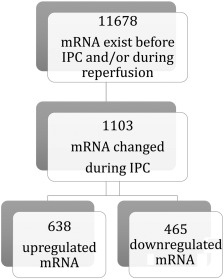
According to settings for expression signal and log 2 FC, microarray assessment detected 11,678 different mRNA transcripts in cardiac EV before IPC and/or during reperfusion. Gene ontology analysis showed an enrichment of mRNA coding for proteins associated with regulation of transcription, translation, extracellular matrix, morphogenic development and feeding behavior. A total of 1103 (9.5%) among the detected 11,678 gene transcripts were significantly increased or decreased after IPC (see Supplemental Table). Also, 638/1103 (57.8%) of the mRNA transcripts were up-regulated, where 634 did not exist before IPC but emerged during reperfusion. There were 465/1103 (42.2%) mRNA sequences that were down-regulated, where 456 existed before IPC but disappeared during reperfusion (Fig. 3). As all porcine genes are not annotated today, biological function of 30% of the induced gene transcripts by IPC (638) could not be assessed.
|
|
|
Fig. 3. Number of distinct mRNA transcripts in extracellular vesicles before ischemic preconditioning (IPC) and after. Both downregulation and upregulation of gene transcription were observed after IPC. |
In this in vivo study we aimed to evaluate whether IPC influenced cardiac EV mRNA content and whether genes with a recognized association to cardioprotection were upregulated. Among 638 transcripts that appeared or increased, the mRNA sequence of transcription factors signal transducer and activator of transcription-3 (STAT3) and T-cell transcription factors/lymphoid-enhancer binding factor (TCF/LEF), the enzymes cyclooxygenase-2 (COX-2) and glycogen synthase kinase 3 beta (GSK-3β), and the receptor ryanodine receptor type 2 (RyR-2) were detected ( Table 1). All these have been, by different pathways, demonstrated to be cardioprotective during I/R and/or IPC [28]; [29]; [30]; [31]; [32] ; [33]. The gene transcript of hypoxia-inducible factor 1 alfa (HIF-1α) was not found [34].
| Gene symbol | UniProtID | Average expression before IPC | Average expression after IPC | Gene description |
|---|---|---|---|---|
| STAT3 | E7CR02Q19550 | Not detected | 1.72 | Signal transducer and activator of transcription 3 |
| TCF/LEF | B3GQS6 | Not detected | 1.66 | Lymphoid enhancer-binding factor 1 |
| RYR2 | NA | Not detected | 1.52 | Ryanodine receptor 2 (cardiac) |
| GSK3B | F1SPD2 | Not detected | 1.51 | Glycogen synthase kinase 3 beta |
| COX2 | Q69GF7 | Not detected | 1.8 | Cytochrome c oxidase subunit II |
IPC = ischemic preconditioning.
4. Discussion
The main findings are that the mRNA contents in EVs changed after myocardial IPC in vivo. To our knowledge, this is the first demonstration of an alteration of EV mRNA content related to preconditioning in vivo. The fact that the preconditioned parental cells release EV containing mRNA that is qualitatively different from those released by non-preconditioned cells, not only shows the importance of the external milieu of parental cells, but also strongly indicates that the EV contents of mRNA are biologically relevant. While these EVs were harvested from coronary venous effluent, there is no direct identification of the parent cells for these EVs. Hence these vesicles may derive from cardio-myocytes, fibroblasts or endothelial cells, even though the sampling was highly localized. Still, in this design we can assume that EVs containing gene transcripts that changed after myocardial IPC originate from the heart, and that transcription of approximately 1000 mRNA sequences was affected by IPC.
Gene ontology analysis, on the 2000 genes with highest expression, showed an enrichment of mRNA coding for proteins associated with regulation of transcription, translation, extracellular matrix, morphogenic development and feeding behavior. This is consistent with the enrichment of ribosomal mRNA that we identified in EV/exosomes/cardiosomes from cultured cardiomyocytes [10]. These findings suggest that the EV content at least partly is destined for supporting target cells and their protein synthesis and cellular remodeling. Several of the identified mRNA sequences that emerged due to IPC are from previous studies known to have associations to cardioprotective phenomena. Five mRNAs translate cell proteins with strong association to IPC: STAT3, TCF/LEF, COX-2, GSK-3β and RyR2. The cardioprotective effects by IPC are associated with two phases, one early phase lasting for about 2 h after IPC, followed by a later phase starting some hours later and lasting for a couple of days [13]. Protective signals of EV mRNA may contribute more to the later phase of cardioprotection, although it is still possible that some aspects of the early phase are mediated in part by EV mRNA. The transcription factors STAT3 and TCF/LEF have each revealed to be cardioprotective. Activation of STAT3 has demonstrated cardioprotection by improved mitochondrial function and upregulation of anti-apoptotic proteins [29] ; [31]. TCF/LEF is known to protect the myocardium during IPC by regulating genes important for anti-apoptosis and angiogenesis [32]. In addition, these transcription factors have in common to initiate the expression of COX-2; an enzyme recognized to become induced by IPC and mediate cardioprotection [35]; [36]; [37] ; [38]. Myocardial tissue levels of COX-2 mRNA have been shown to increase at 1 h after IPC and COX-2 protein and its specific cardioprotective prostanoid metabolites (PGE2 and PGI2) at 24 h after IPC [27]; [36]; [37] ; [38]. In concordance with a previous study where it was shown that EV/prostasomes contain ribosomes [39], it is suggested that IPC increases the expression of TCF/LEF and STAT3 in the cardiac EVs, firstly to obtain their direct cardioprotective effects and secondly, to guarantee further COX-2 protein synthesis in recipient cells. In addition, mRNA transcripts of COX-2 were induced in cardiac EVs after IPC, which may demonstrate an alternative pathway to obtain the cardioprotective mechanisms of COX-2 in target cells. These two ways of transferring an increase of COX-2 effect in recipient cells could indicate that the COX-2 effect of IPC is transferred by EV.
It is well recognized that HIF-1α is induced under hypoxic conditions, but still it was not detected in our cardiac EVs. HIF-1α has been suggested necessary for cardioprotection in IPC and induces expression of various cardioprotective genes such as COX-2 [40] ; [41] consistent with the present results.
Even mRNA of GSK-3β, an enzyme being important in cardiomyocyte apoptosis, was increased due to IPC. The enzyme in its phosphorylated state has been associated to cardioprotection during myocardial IPC by inhibiting opening of mitochondrial permeability transition pores [30]. The amount of RyR2 mRNA (a well recognized myocardial Ca2 + channel receptor) increased in cardiac EVs after IPC. Cytosolic Ca2 + overload is one important pathophysiological mechanism of myocardial damage during ischemia/reperfusion (I/R), and IPC improves Ca2 + homeostasis during reperfusion [42]. Studies have presented Ca2 + overload to be caused by defect Ca2 + release through ischemically impaired RyR2. It has been suggested that pharmacological modulation restoring and preventing RyR2 dysfunction may be cardioprotective during myocardial I/R, explaining at least some of the infarct sparing effects of IPC [33]; [43] ; [44].
This study was confined to explore cardiac EV mRNA. We can therefore only presume that altered gene transcripts will further result in a biological function of a translated protein. In this explorative study, microRNA, DNA, and protein content in recipient cells were not investigated. We and others have previously shown in vitro that the transferred EV mRNA was functional by inducing gene expression changes and becoming translated to proteins in the target cell [3] ; [11]. The co-existence of miR, mRNA and DNA fragments in EV, and the observation that they are all qualitatively changed by the external milieu, support the idea of a hierarchically organized signal system exerting protective actions on recipient cells. MicroRNA appears as the fastest signal from parental cells, followed by mRNA, which has a more sustained biological signal, and also DNA fragment signals.
Concerning limitations of the study design, gene function of the porcine genome is less known and few antibodies are available for more specific functional studies. Still, a large animal model is needed for collecting enough EVs, and is more suitable for conclusions concerning the human situation. In future studies, unique identifiers on EV, representative of the parent cells, will facilitate more specific analysis of EV contents in in vivo models. Mechanisms of EV packaging needs to be better understood as well as the time relationship of stimulus and EV release from parent cells. In this study, EVs were collected subsequent to the ischemic stimulus, since it is well established that IPC has induced cardiac protection by then. However, it is possible that EV production and EV contents change over time after the stimulus, which is the reason why it would be relevant to study the signal of cardioprotection over time.
In summary, these findings demonstrate for the first time in an in vivo model that IPC in the heart muscle influences the composition of mRNA in EVs harvested from the coronary venous blood. We also show that EVs from cardiac cells exposed to IPC contain gene transcripts for proteins which are associated with cardioprotective effects of IPC. Hence, EVs contain transcription material, which we suggest is relevant for the protective effects of IPC in the heart muscle.
Acknowledgement of grant support
This work was supported by grants from the Swedish Heart-Lung Foundation [grant numbers 2012-0469 and 2013-0690]; the University of Gothenburg; Umeå University; the County Councils of Västra Götaland and Västerbotten, Göteborgs Läkarsällskap (GLS-326401), Elsa och Gustav Lindhs fond, and the Kungliga och Hvitfeldtska stiftelsen.
Conflict of interest
There are no conflicts of interest for any authors to declare.
Acknowledgements
The authors acknowledge the expert help of research engineer Göran Johansson, M.S.
Appendix A. Supplementary data
Supplementary table. All detected gene transcripts.
References
- [1] M. Simons, G. Raposo; Exosomes—vesicular carriers for intercellular communication; Curr Opin Cell Biol, 21 (4) (2009), pp. 575–581
- [2] X. Loyer, A.C. Vion, A. Tedgui, C.M. Boulanger; Microvesicles as cell–cell messengers in cardiovascular diseases; Circ Res, 114 (2) (2014), pp. 345–353
- [3] A. Waldenström, N. Gennebäck, U. Hellman, G. Ronquist; Cardiomyocyte microvesicles contain DNA/RNA and convey biological messages to target cells; PLoS One, 7 (4) (2012), p. e34653
- [4] J. Lötvall, A.F. Hill, F. Hochberg, E.I. Buzás, D. Di Vizio, C. Gardiner, et al.; Minimal experimental requirements for definition of extracellular vesicles and their functions: a position statement from the International Society for Extracellular Vesicles; J Extracell Vesicles, 3 (2014), p. 26913
- [5] S. Keller, M.P. Sanderson, A. Stoeck, P. Altevogt; Exosomes: from biogenesis and secretion to biological function; Immunol Lett, 107 (2) (2006), pp. 102–108
- [6] S. Gupta, A.A. Knowlton; HSP60 trafficking in adult cardiac myocytes: role of the exosomal pathway; Am J Physiol Heart Circ Physiol, 292 (6) (2007), pp. H3052–H3056
- [7] S. Mathivanan, R.J. Simpson; ExoCarta: a compendium of exosomal proteins and RNA; Proteomics, 9 (21) (2009), pp. 4997–5000
- [8] X. Yu, L. Deng, D. Wang, N. Li, X. Chen, X. Cheng, et al.; Mechanism of TNF-α autocrine effects in hypoxic cardiomyocytes: initiated by hypoxia inducible factor 1α, presented by exosomes; J Mol Cell Cardiol, 53 (6) (2012), pp. 848–857
- [9] Z.A. Malik, K.S. Kott, A.J. Poe, T. Kuo, L. Chen, K.W. Ferrara, et al.; Cardiac myocyte exosomes: stability, HSP60, and proteomics; Am J Physiol Heart Circ Physiol, 304 (7) (2013), pp. H954–H965
- [10] N. Gennebäck, U. Hellman, L. Malm, G. Larsson, G. Ronquist, A. Waldenström, et al.; Growth factor stimulation of cardiomyocytes induces changes in the transcriptional contents of secreted exosomes; J Extracell Vesicles, 2 (2013) https://doi.org/10.3402/jev.v2i0.20167
- [11] H. Valadi, K. Ekström, A. Bossios, M. Sjöstrand, J.J. Lee, J.O. Lötvall; Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells; Nat Cell Biol, 9 (6) (2007), pp. 654–659
- [12] C.E. Murry, R.B. Jennings, K.A. Reimer; Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium; Circulation, 74 (5) (1986), pp. 1124–1136
- [13] D.M. Yellon, J.M. Downey; Preconditioning the myocardium: from cellular physiology to clinical cardiology; Physiol Rev, 83 (4) (2003), pp. 1113–1151
- [14] Z. Giricz, Z.V. Varga, T. Baranyai, P. Sipos, K. Pálóczi, Á Kittel, et al.; Cardioprotection by remote ischemic preconditioning of the rat heart is mediated by extracellular vesicles; J Mol Cell Cardiol, 68 (2014), pp. 75–78
- [15] Y. Feng, W. Huang, M. Wani, X. Yu, M. Ashraf; Ischemic preconditioning potentiates the protective effect of stem cells through secretion of exosomes by targeting Mecp2 via miR-22; PLoS One, 9 (2) (2014), p. e88685
- [16] T. Yamaguchi, Y. Izumi, Y. Nakamura, T. Yamazaki, M. Shiota, S. Sano, et al.; Repeated remote ischemic conditioning attenuates left ventricular remodeling via exosome-mediated intercellular communication on chronic heart failure after myocardial infarction; Int J Cardiol, 178C (2014), pp. 239–246
- [17] J.M. Vicencio, D.M. Yellon, V. Sivaraman, D. Das, C. Boi-Doku, S. Arjun, et al.; Plasma exosomes protect the myocardium from ischemia–reperfusion injury; J Am Coll Cardiol, 65 (15) (2015), pp. 1525–1536
- [18] A.G. Ibrahim, K. Cheng, E. Marbán; Exosomes as critical agents of cardiac regeneration triggered by cell therapy; Stem Cell Rep., 2 (5) (2014), pp. 606–619
- [19] L. Barile, V. Lionetti, E. Cervio, M. Matteucci, M. Gherghiceanu, L.M. Popescu, et al.; Extracellular vesicles from human cardiac progenitor cells inhibit cardiomyocyte apoptosis and improve cardiac function after myocardial infarction; Cardiovasc Res, 103 (4) (2014), pp. 530–541
- [20] M. Kavianipour, G. Ronquist, G. Wikström, A. Waldenström; Ischaemic preconditioning alters the energy metabolism and protects the ischaemic myocardium in a stepwise fashion; Acta Physiol Scand, 178 (2) (2003), pp. 129–137
- [21] R.A. Irizarry, B. Hobbs, F. Collin, Y.D. Beazer-Barclay, K.J. Antonellis, U. Scherf, et al.; Exploration, normalization, and summaries of high density oligonucleotide array probe level data; Biostatistics, 4 (2) (2003), pp. 249–264
- [22] C. Li, W.H. Wong; Model-based analysis of oligonucleotide arrays: expression index computation and outlier detection; Proc Natl Acad Sci U S A, 98 (1) (2001), pp. 31–36
- [23] G.K. Smyth; Linear models and empirical Bayes methods for assessing differential expression in microarray experiments; Stat Appl Genet Mol Biol, 3 (2004) [Article3]
- [24] G.K. Smyth; Limma: linear models for microarray data; R. Gentleman, V. Carey, S. Dudoit, R. Irizarry, W. Huber (Eds.), Bioinformatics and Computational Biology Solutions using R and Bioconductor, Springer, New York (2005), pp. 397–420
- [25] Y. Benjamini, Y. Hochberg; Controlling the false discovery rate: a practical and powerful approach to multiple testing; J R Stat Soc Ser B (57) (1995), pp. 289–300
- [26] K.P. O'Brien, M. Remm, E.L. Sonnhammer; Inparanoid: a comprehensive database of eukaryotic orthologs; Nucleic Acids Res, 33 (Database issue) (2005), pp. D476–D480
- [27] W. Huang da, B.T. Sherman, R.A. Lempicki; Systematic and integrative analysis of large gene lists using DAVID bioinformatics resources; Nat Protoc, 4 (1) (2009), pp. 44–57
- [28] R. Bolli, K. Shinmura, X.L. Tang, E. Kodani, Y.T. Xuan, Y. Guo, et al.; Discovery of a new function of cyclooxygenase (COX)-2: COX-2 is a cardioprotective protein that alleviates ischemia/reperfusion injury and mediates the late phase of preconditioning; Cardiovasc Res, 55 (3) (2002), pp. 506–519
- [29] R. Bolli, A.B. Stein, Y. Guo, O.L. Wang, G. Rokosh, B. Dawn, et al.; A murine model of inducible, cardiac-specific deletion of STAT3: its use to determine the role of STAT3 in the upregulation of cardioprotective proteins by ischemic preconditioning; J Mol Cell Cardiol, 50 (4) (2011), pp. 589–597
- [30] T. Miura, M. Tanno; Mitochondria and GSK-3beta in cardioprotection against ischemia/reperfusion injury; Cardiovasc Drugs Ther, 24 (3) (2010), pp. 255–263
- [31] G. Heusch, J. Musiolik, N. Gedik, A. Skyschally; Mitochondrial STAT3 activation and cardioprotection by ischemic postconditioning in pigs with regional myocardial ischemia/reperfusion; Circ Res, 109 (11) (2011), pp. 1302–1308
- [32] S. Kaga, L. Zhan, E. Altaf, N. Maulik; Glycogen synthase kinase-3beta/beta-catenin promotes angiogenic and anti-apoptotic signaling through the induction of VEGF, Bcl-2 and survivin expression in rat ischemic preconditioned myocardium; J Mol Cell Cardiol, 40 (1) (2006), pp. 138–147
- [33] J. Fauconnier, S. Roberge, N. Saint, A. Lacampagne; Type 2 ryanodine receptor: a novel therapeutic target in myocardial ischemia/reperfusion; Pharmacol Ther, 138 (3) (2013), pp. 323–332
- [34] Q. Ke, M. Costa; Hypoxia-inducible factor-1 (HIF-1); Mol Pharmacol, 70 (5) (2006), pp. 1469–1480
- [35] R. Bolli, B. Dawn, Y.T. Xuan; Role of the JAK–STAT pathway in protection against myocardial ischemia/reperfusion injury; Trends Cardiovasc Med, 13 (2) (2003), pp. 72–79
- [36] D.A. Rodriguez, J.C. Tapia, J.G. Fernandez, V.A. Torres, N. Muñoz, D. Galleguillos, et al.; Caveolin-1-mediated suppression of cyclooxygenase-2 via a beta-catenin-Tcf/Lef-dependent transcriptional mechanism reduced prostaglandin E2 production and survivin expression; Mol Biol Cell, 20 (8) (2009), pp. 2297–2310
- [37] K. Shinmura, X.L. Tang, Y. Wang, Y.T. Xuan, S.Q. Liu, H. Takano, et al.; Cyclooxygenase-2 mediates the cardioprotective effects of the late phase of ischemic preconditioning in conscious rabbits; Proc Natl Acad Sci U S A, 97 (18) (2000), pp. 10197–10202
- [38] Y. Guo, D.N. Tukaye, W.J. Wu, X. Zhu, M. Book, W. Tan, et al.; The COX-2/PGI2 receptor axis plays an obligatory role in mediating the cardioprotection conferred by the late phase of ischemic preconditioning; PLoS One, 7 (7) (2012), p. e41178
- [39] G.E. Sahlén, L. Egevad, A. Ahlander, B.J. Norlén, G. Ronquist, B.O. Nilsson; Ultrastructure of the secretion of prostasomes from benign and malignant epithelial cells in the prostate; Prostate, 53 (3) (2002), pp. 192–199
- [40] G. Loor, P.T. Schumacker; Role of hypoxia-inducible factor in cell survival during myocardial ischemia-reperfusion; Cell Death Differ, 15 (4) (2008), pp. 686–690
- [41] Z. Cai, H. Zhong, M. Bosch-Marce, K. Fox-Talbot, L. Wang, C. Wei, et al.; Complete loss of ischaemic preconditioning-induced cardioprotection in mice with partial deficiency of HIF-1 alpha; Cardiovasc Res, 77 (3) (2008), pp. 463–470
- [42] A. Waldenström, G. Ronquist, A.M. Aberg, K. Ahlström, P. Hauck, P. Abrahamsson, et al.; Ischaemic preconditioning reduces myocardial calcium overload in coronary-occluded pig hearts shown by continuous in vivo assessment using microdialysis; Clin Physiol Funct Imaging, 32 (2) (2012), pp. 133–138
- [43] J. Fauconnier, A.C. Meli, J. Thireau, S. Roberge, J. Shan, Y. Sassi, et al.; Ryanodine receptor leak mediated by caspase-8 activation leads to left ventricular injury after myocardial ischemia–reperfusion; Proc Natl Acad Sci U S A, 108 (32) (2011), pp. 13258–13263
- [44] R. Zucchi, F. Ronca, S. Ronca-Testoni; Modulation of sarcoplasmic reticulum function: a new strategy in cardioprotection?; Pharmacol Ther, 89 (1) (2001), pp. 47–65
Document information
Published on 19/05/17
Submitted on 19/05/17
Licence: Other
Share this document
Keywords
claim authorship
Are you one of the authors of this document?